- College of Pharmacy, QU Health, Qatar University, Doha, Qatar
Introduction: Academic institutions have a duty to equip health professional students with the requisite research skills to ensure the implementation of evidence-based practice. This study aims to determine the perceptions of pharmacy students and alumni toward research after completing Undergraduate Research in Pharmacy Courses (URPCs) at the College of Pharmacy–Qatar University (CPH–QU).
Methods: A cross-sectional survey was conducted. All CPH-QU alumni (n = 238), and all third- and fourth-year professional students who had completed at least one URPC at the time of conducting the study (n = 42) were approached. The questionnaire contained items relating to research experience and perceptions of significance, confidence in conducting research, actual and anticipated outcomes, and motivation for future research. A Theoretical Domains Framework informed the development of selected items.
Results: The response rate was 72.1% (202/280); however, the usable rate was 95.5% (193/202). The participants gave positive responses relating to their perceptions of research significance {Median = 5.0 [Interquartile range (IQR) = 1.0], Minimum–Maximum = 1–5}, confidence in conducting research [Median = 4.0 (IQR = 1.0), Minimum–Maximum = 1–5], actual and anticipated outcomes [Median = 4.0 (IQR = 1.0), Minimum–Maximum = 1–5], and motivation for future research plans [Median = 4.0 (IQR = 1.0), Minimum–Maximum = 1–5]. The majority of participants perceived non-confidence in using data analysis software [72 (39.4% non-confidence)] and a high proportion of participants were non-confident in conducting data analysis [45 (24.6% non-confidence)]. More than half reported publishing at least one peer-reviewed article [99 (54.4% agreement)] from their courses and were highly motivated to consider post-graduate degrees in pharmacy [132 (73.3% agreement)].
Conclusions: Incorporating URPCs into CPH–QU curriculum has potentially improved students and alumni's perceptions of research. Action is needed to improve confidence in different aspects of research.
Introduction
Continuous advancement in healthcare requires the development of healthcare professionals committed to Evidence-Based Practice (EBP) (1). However, the successful integration of EBP into clinical practice is hindered by inadequate research knowledge, skills, experience, and confidence among healthcare professionals (2, 3). Therefore, research is a priority for many healthcare professional education programs (4).
Research is fundamental to evidence-based pharmacy practice (5), generating knowledge and advancing practices, establishing innovative roles and services, and improving health outcomes (6, 7). Given the significance of pharmacy research, it is critical to prepare pharmacy students and graduates with the requisite knowledge, skills, and willingness to conduct research and apply the findings to clinical practice (8, 9).
In the last few decades, pharmacy education around the globe has evolved significantly, with substantial advancements in curriculum, pedagogical methods, and instructional strategies (10, 11). The accreditation standards for the 2016 Accreditation Council for Pharmacy Education (ACPE) (12) and the 2018 Canadian Council for Accreditation of Pharmacy Programs (CCAPP) (13) highlight the importance of the achievement of specific research competencies by pharmacy students. These are outlined by the Task Force for the American College of Clinical Pharmacy (ACCP) on Research in the Professional Curriculum who emphasize eight key curricular competencies linked to research for students in pharmacy schools: identifying relevant problems; generating a hypothesis; designing a study; analyzing data; interpreting and applying findings; disseminating research findings; and applying regulatory and ethical principles (14).
Pharmacy colleges worldwide offer designated research tracks (15, 16), or directed research courses as core or elective requirements (17–19). In several studies, students indicated improved confidence when conducting research after completing a one-semester research course (17), and in applying knowledge in practice after completing an independent research elective course (20). Likewise, health professional students' early immersion in health-related research provides them with an opportunity to improve their knowledge, expertise, attitudes, and self-efficacy demonstrated by being able to define a problem, systematically gather data, think critically and analytically, and become lifelong learners (21). Furthermore, previous studies have found that health professional students' research experience is related to future professional and academic research endeavors (22, 23). The provision of adequate research facilities and supervision are also key requirements in preparing students for future practice (24).
There is a scarcity of research investigating pharmacists and pharmacy students' perspectives into research and the significance of research courses in the likely implementation of EBP in the Middle East. In Qatar, pharmacy practice is developing in all healthcare settings (25, 26), with a comparable advancement in pharmacists' engagement in health-related research as per the national requirement of pharmacy education (27). The College of Pharmacy at Qatar University (CPH–QU), accredited by the CCAPP, was founded in 2006 and represents its first and only pharmacy college. The focus at CPH–QU during their 5-year undergraduate degree program is on equipping students with research competencies via six Pharmacy Research Evaluation and Presentation Skills (PREP) courses, and two Undergraduate Research in Pharmacy Courses (URPCs). The two URPC courses are PHAR 445 (elective) and PHAR 545 (mandatory) in the third (P3) and the fourth (P4) professional years (28).
This study aims to examine the perceptions of pharmacy students and alumni of research following the completion of at least one of the URPCs. The specific objectives are to determine: (1) research experiences and perceptions of research significance; (2) perceptions of confidence in conducting pharmacy-related research; and (3) perceptions of the impact of participating in the URPCs on anticipated and actual outcomes, and their motivation for future research.
Materials and methods
Design and setting
The study was a cross-sectional design conducted at CPH–QU from August to December 2021. Ethics approval was obtained from the QU Institutional Review Board (QU-IRB 1562-EA/21).
Study population
“The total number of CPH–QU alumni [i.e., from the first batch of graduates (2011) to the most recent batch of graduates (2021)], and all third- and fourth-year professional students who had completed at least one URPC was 287 (n = 244 alumni and 43 students). Raosoft® online calculator was used to determine the minimum sample size of participants, excluding the 6 alumni and 1 student who conducted the face validity, and taking into consideration a 5% margin of error and confidence level of 95%. A sample of 162 participants was needed. However, the total eligible population (n = 280) was approached considering the possible non-response.“
Undergraduate research in pharmacy courses
URPCs are two-credit 1-h courses [PHAR 445 (elective) and PHAR 545 (mandatory)] in P3 and P4 professional years, respectively (28). The courses provide students with an opportunity to conduct research under the supervision of a faculty member. Students are taught in the URPCs to comprehend and apply conceptual, theoretical, and empirical components of various research types within a wide area of pharmacy research. In addition to enhancing research skills, students are tutored in other scholarly-related activities such as scientific writing and presentation skills (i.e., poster and oral presentations), and are offered the opportunity to participate in research seminars, forums and conferences.
Questionnaire development and validation
A self-administered questionnaire was developed and informed by previous studies (6, 17, 24, 29–34). Specific items were guided by the Theoretical Domains Framework (TDF), an integrated framework of 33 behavior change theories described in 14 domains of behavior determinants (influences) (35). Specific domains of interest were knowledge, skills, belief in capabilities, professional role/identity, emotions, beliefs in consequences, intentions, and goals. Incorporating theory into research improves the robustness, relevance, and impact of findings (36).
To determine the likely content validity, the first draft was shared with 15 local, regional, and international pharmacy education and practice experts, and the questionnaire was developed over two stages. The first involved a qualitative evaluation and review of the content relevance, representativeness, and technical quality of each item. The second round involved utilizing an item Content Validity Index (i-CVI) and Scale-Content Validity/Average (S-CVI/Ave) for item-reduction purposes, which revealed acceptable scores and, hence, no item was removed. Face validity was conducted by purposefully selecting seven participants (6 CPH–QU alumni and 1 current student who had completed at least one URPC. These were then requested to consider the representativeness of each item to the actual experience of the target population. This led to the removal of three questionnaire items to reduce redundancy, and the rephrasing of several items to enhance readability and understandability.
The final version of the questionnaire comprised 68 items, divided into four sections: demographics and professional characteristics (11 items); research experience (5 items) and perceptions of research significance (11 items; 5-point Likert scale [1 = strongly disagree to 5 = strongly agree] based on knowledge, professional role/identity, and emotion domains of TDF); confidence in conducting research (19 items; 5-point Likert scale [1 = not confident at all to 5 = extremely confident] based on self-efficacy and skills domains of TDF); perceptions of impact (7 items and an open-ended item) and anticipated outcomes (4 items based on belief in consequences domain of TDF; 5-point Likert scale and an open-ended item); and motivation for future research (9 items; 5-point Likert scale, based on intentions and goals domain of TDF) (See Supplementary material 1 for the mapping of questionnaire items to TDF).
Data collection procedure
The personal e-mail addresses of the study population were retrieved from a CPH–QU database, with each invited to complete an anonymous, self-administered questionnaire through a web-link at SurveyMonkey® (Survey Monkey Inc., San Mateo, California, USA). A detailed description of the study (e.g., objectives, data collection procedure, confidentiality and anonymity measures, and voluntary nature of participation) was provided. The completion of the questionnaire implied an informed consent to participate. The questionnaire link was open from early November to late December 2021, and three reminders were sent.
Statistical analysis
Descriptive and inferential statistics were performed using IBM Statistical Package for Social Sciences (IBM SPSS® 27 software). Non-parametric statistics were used to compare different subgroups in terms of the overall perceptions of research significance, confidence in research, research outcomes, and motivation for future research. Sub-group analyses targeted having a post-graduate degree (yes or no), practice setting (hospital-based, non-hospital based or not practicing), years of work experience (0, <1, 1–5, 6–10 or >10 years), URPC research discipline (clinical pharmacy, pharmaceutical sciences or both), additional research projects undertaken (yes or no), and whether participating in publication and/or poster/oral presentations (yes or no). Mann-Whitney U and Kruskal-Wallis H tests were used to compare variables with two and more than two categories, respectively. The level of statistical significance was set a priori at p < 0.05. The questionnaire scales were tested for internal consistency reliability (Cronbach's alpha), considering α ≥ 0.7 as the minimum satisfactory value.
Results
Demographics and professional characteristics
The response rate was 72.1% (n = 202 of 280); however, the usable rate was 95.5% (n = 193 of 202), after removing respondents who filled the demographic section only. The questionnaire sections were not filled completely by all the 193 participants; hence, each section was analyzed separately to maintain the adequacy of responses. Therefore, different numbers of participants were reported in each section. Participants' demographic and professional characteristics are presented in Table 1. The majority were CPH–QU alumni [151 (78.2%)] who graduated between 2014 and 2019 [90 (60.4%]), acquired a post-graduate degree [95 (62.9%)], predominantly from the CPH–QU PharmD program [66 (69.5%)]. The majority of the CPH–QU alumni were full-time employees [100 (85.5%)], working in governmental hospitals [56 (37.33%)] for 1–5 years [65 (43.0%)].
Participants' perceptions of research after completing the undergraduate research in pharmacy courses
Perceptions of research experience and significance
Table 2 presents the participants' research experience and background. Almost half [101 (52.3%)] were involved in both URPCs (i.e., PHAR 445 and PHAR 545). The majority [118 (61.1%)] had participated in additional research projects (other than URPCs) during their undergraduate pharmacy degree, primarily via the Undergraduate Research Experience Program (UREP) of the Qatar National Research Fund [107 (91.5%)].
Participants' perceptions regarding the significance of, and interest in, pharmacy-related research are presented in Table 3 {Median = 5.0 [Interquartile range (IQR) = 1.0], Minimum–Maximum = 1–5}. The internal consistency of this scale was = 0.898 (Supplementary material 2). The majority expressed agreement levels of more than 80% with the significance of URPCs and their interest in research, as indicated by responses to most items. A Mann-Whitney U test identified that those who participated in projects additional to URPC showed a significantly statistically higher perception of research importance and interest than those who did not (U = 3,103.50, p = 0.013) (Supplementary material 3).
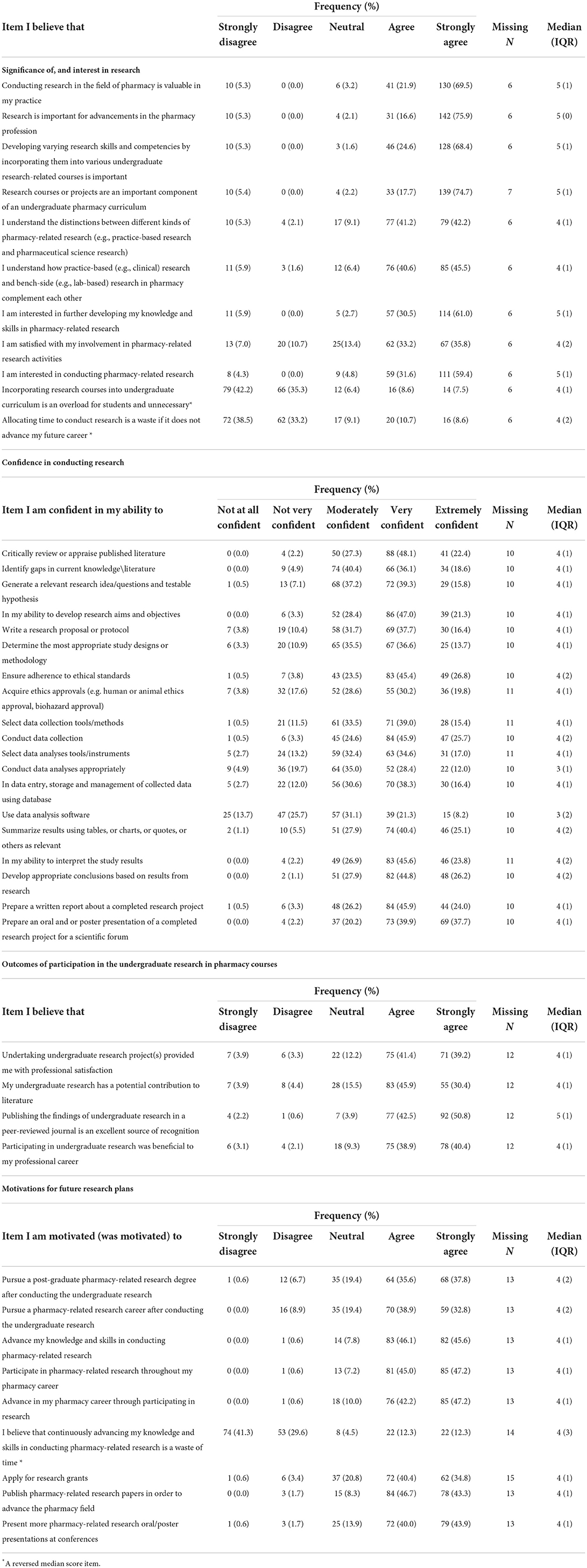
Table 3. Participants' perceptions of research after completing the undergraduate research in pharmacy courses.
Perceptions of confidence in conducting research
Perceptions of their confidence in conducting research are presented in Table 3 [Median = 4.0 (IQR = 1.0), Minimum–Maximum = 1–5]. The internal consistency of this scale was 0.948 (Supplementary material 2). Over three-quarters were confident (i.e., very confident or extremely confident) in their ability to prepare an oral or poster presentation [142 (77.6%)] and in ensuring adherence to ethical standards [132 (72.2%)]. More than a quarter of the participants indicated moderate confidence in almost all items (16/19 items). Conversely, a large proportion reported a lack of confidence (i.e., not confident at all and not very confident) in using data analysis software [72 (39.4%)], and in conducting data analyses [45 (24.6%)]. Kruskal Wallis H test showed a statistically significant difference in confidence in conducting research between those alumni who worked in hospital-based practices and those in non-hospital-based practices (H = 6.783, p = 0.034) (Supplementary material 3).
Perceptions of research outcomes
Reported research outcomes following completion of URPCs are provided in Table 4. Many indicated publish at least one peer-reviewed article (99 [54.4%]). Mann-Whitney U test indicated that participants who had published at least one peer-reviewed article had a significantly higher perception of their confidence in conducting research than those who did not (U = 3209.0, p = 0.025) (Supplementary material 3). Presenting a poster from the URPCs at an international conference was associated with a significantly higher level of confidence in conducting research (U = 2982.0, p = 0.007) (Supplementary material 3).
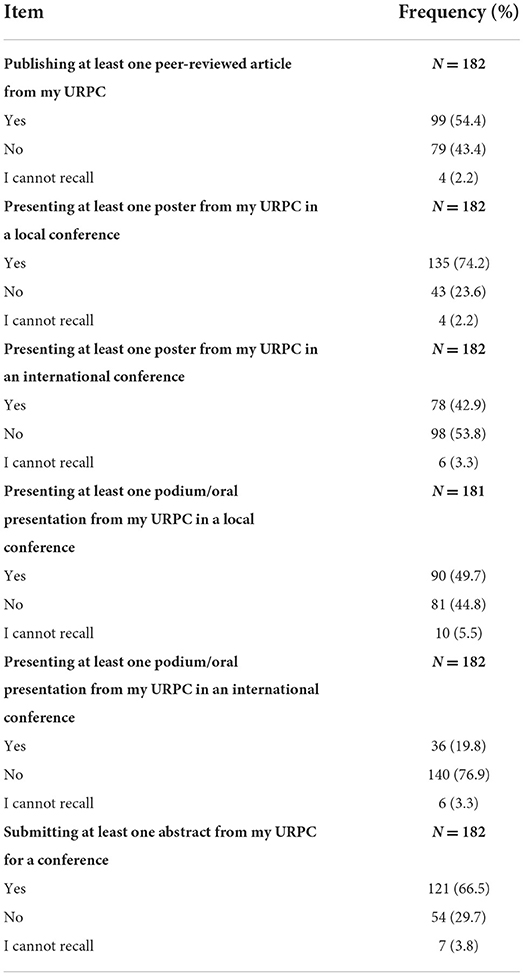
Table 4. Participants' reported outcomes after taking the undergraduate research in pharmacy courses (URPC)s.
Table 3 gives participants' perceptions of the actual and anticipated outcomes of participation in URPCs [Median = 4.0 (IQR = 1.0), Minimum–Maximum = 1–5]. The internal consistency of this scale was 0.857 (Supplementary material 2). The majority [169 (93.3%)] considered the publication of URPCs findings in a peer-reviewed journal as an excellent source of recognition. Mann-Whitney U demonstrated that undertaking other research projects in addition to the URPCs was associated with a significantly higher perception of outcomes of participating in URPCs (U = 2740.0, p = 0.006) (Supplementary material 3).
Perceptions of the motivations for future research plans
Participants' perceptions toward motivations for future research plans are presented in Table 3 [Median = 4.0 (IQR = 1.0), Minimum–Maximum = 1–5]. The internal consistency of this scale was 0.832 (Supplementary material 2). The majority of participants reported agreement with items related to participants' motivations for future research (i.e., agree and strongly agree, ranging from 71.7 to 92.2%). The largest proportion of participants reported agreements with motivation to participate in pharmacy-related research [166 (92.2%)] and with motivation to advance knowledge and skills in conducting research [165 (91.7%)]. A Mann-Whitney U identified a statistically significant association between those undertaking other research projects in addition to URPCs and higher perceptions of motivation for future career plans (U = 2,727.5, p = 0.004) (Supplementary material 3).
Discussion
The majority of participants expressed agreement with the significance of conducting pharmacy profession research, and the importance of its incorporation into undergraduate pharmacy curricula. This is similar to results obtained by Kritikos et al. (6) who noted that around three-quarters of pharmacy students at the University of Sydney recognized the significance of incorporating research-related activities in their undergraduate curriculum (6). A lack of formal research courses in the curriculum was largely considered a barrier to research activity engagement among dental hygiene students (37). Several factors negatively impact health professional students' perceptions of research significance, such as the probability of research projects yielding insignificant results despite the time and effort invested in them (30, 38). Contrary to a Saudi Arabian study (30), the majority of participants believed research to be essential and not a waste of time regardless of career advancement.
An important finding of this study, consistent with results found in other studies (6, 32) was the considerable proportion (>25%) of participants who reported moderate confidence to various aspects of research surveyed in the questionnaire items. Moreover, the present study also found that the majority of participants perceived non-confidence in their ability to use data analysis software and a high proportion of participants were non-confident in conducting data analysis. aligning with results reported from a number of previous studies on pharmacy students (32, 39), and students of other health professions (40, 41). Improving students' comprehension and application of statistical tests is an area for improvement. Participants showed more confidence in their ability to prepare oral or poster presentations of a completed research project, a result which may be attributed to URPC-based orientation sessions around these skills, in addition to being exposed to a variety of research evaluations and presentation skills in several courses and journal clubs within the curriculum. Similarly, pharmacy students in the United States indicated that participation in elective research courses resulted in their improved engagement with research-related activities, such as poster and podium presentations and peer-reviewed publications (42).
CPH–QU alumni working in hospital settings perceived themselves to have a significantly lower rate of confidence in conducting research than those who worked in non-hospital settings (e.g., academia and research institutes). This finding is in concordance with studies by Awaisu et al. (27) investigating hospital pharmacists in Qatar, who lacked competence and confidence in several aspects of research, such as developing research protocols, critically appraising literature, determining sample size, and interpreting research findings. Conducting research is neither part of the job description of a hospital pharmacist, nor a requirement for preregistration in Qatar or many other countries (32); hence, engagement in research activities is not considered a priority.
The current study found that participants placed a high value on publishing their undergraduate research in peer-reviewed journals, which they considered to be an excellent source of recognition. A similar finding was reported in a study conducted in the United States where more than 90% of PharmD students believed that publications provided a sense of recognition and excellence, with the authors noting that research participation facilitates career advancement (43). A study conducted among research advisors at Ambo University, Ethiopia, demonstrated that there is an absence of knowledge transfer through publication and presentation which was a potential outcome of poor undergraduate pharmacy students' research projects (44). It has also been reported that inadequate research mentoring can hinder student research activity and associated outputs (45).
This study showed that the majority of participants were motivated to pursue a post-graduate pharmacy-related research degree and to work in a research-related career, similar to a recent study in Saudi Arabia (30). Conversely, a study conducted in Canada demonstrated that few pharmacy students were interested in pursuing postgraduate research due to a lack of interest in a research career (46). In that regard, Johnson et al. (47) suggested that early exposure to research during the undergraduate study is necessary for pharmacy graduates to show a preference for a research-related career (47). In a cross-sectional study of medical and allied health professional students, Bovijn et al. (23) found there to be greater interest in future research among those who had previous or current research experience (23). Furthermore, Overholser et al. (48) and Surratt et al. (15) argued that enhancing pharmacy students' perception of research significantly improves their motivation to conduct research studies in their professional practices (15, 48).
TDF was used in this study to provide a focus on potential research behavior influences. Although participants self-reported high levels of knowledge and understanding regarding the significance of research to the pharmacy, their beliefs about capabilities (i.e., lack of confidence in their abilities to perform different research processes) might benefit from tailored behavior change interventions. Indeed, others have suggested teaching strategies that increase student conviction in their ability to successfully perform research tasks (49). Moreover, it has been shown that inadequate training in several research competencies (e.g., research methodology, and data analysis) is the most significant obstacle to undertaking high-quality research in developing countries (50). This suggests that teaching research as a mandatory course would eliminate this challenge. Cailor et al. (17) claimed that research courses offered as electives might only be taken by students who were already interested in pursuing a research-based career (17). As today's healthcare practice is an integral aspect of evidence-based health care, research education and training should be mandatory in undergraduate health professions education, including pharmacy.
Strengths and limitations
The strengths of this study include the steps taken in pretesting the questionnaire, and the inclusion of TDF in several items with the aim of enhancing internal validity. The response rate was relatively high, minimizing the potential for non-response bias (51). Nevertheless, the findings of the current study should be interpreted with caution due to the relatively small population size and the potential for underpowered statistical comparisons. Also, the questionnaire evaluation did not include other types of validity tests (e.g., construct validity). There may have been an element of recall bias, particularly for the batch of alumni who graduated the earliest. While the findings may not be generalizable to other settings and populations, many of the findings do resonate with the literature.
Further research
There would be merit in conducting longitudinal studies with similar populations and colleges in other similar Arab countries while comparing perceptions of students who participated in elective research courses and those who did not participate. Moreover, it might be useful to compare how students perceive research from the alumni population, which was not feasible in this study due to the small sample student population. Furthermore, qualitative research would provide an in-depth understanding of the key findings. Additional psychometric tests (e.g., construct and criterion validities) may be warranted to provide further validation of the designed questionnaire.
Conclusions
Incorporating research courses into the undergraduate pharmacy curriculum at CPH–QU has potentially improved students and alumni's perceptions of research significance, their interest and confidence in conducting pharmacy-related research, and their motivation for perusing a research-related career. Further action is needed to improve confidence in different aspects of pharmacy-related research.
Data availability statement
The raw data supporting the conclusions of this article will be made available by the authors, without undue reservation.
Ethics statement
Ethics approval was obtained from the QU Institutional Review Board (QU-IRB 1562-EA/21). The patients/participants provided their written informed consent to participate in this study.
Author contributions
All authors listed have made a substantial, direct, and intellectual contribution to the work and approved it for publication.
Funding
This research was supported by the (Qatar University internal grant) under Grant (QUST-2- CPH -2021-213). Open access funding is provided by Early Career Researcher Award (ECRA03-001-3-001) and Qatar National Research Fund.
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
Supplementary material
The Supplementary Material for this article can be found online at: https://www.frontiersin.org/articles/10.3389/fmed.2022.988908/full#supplementary-material
References
1. Moraes DW, Jotz M, Menegazzo WR, Menegazzo MS, Veloso S, Machry MC, et al. Interest in research among medical students: challenges for the undergraduate education. Revista da Associação Médica Brasileira. (2016) 62:652–8. doi: 10.1590/1806-9282.62.07.652
2. Sadeghi-Bazargani H, Tabrizi JS, Azami-Aghdash S. Barriers to evidence-based medicine: a systematic review. J Eval Clin Pract. (2014) 20:793–802. doi: 10.1111/jep.12222
3. da Silva TM, Costa LdCM, Garcia AN, Costa LOP. What do physical therapists think about evidence-based practice? A systematic review. Man Ther. (2015) 20:388–401. doi: 10.1016/j.math.2014.10.009
4. Salmond SW. Advancing evidence-based practice: a primer. Orthop Nurs. (2007) 26:114–23. doi: 10.1097/01.NOR.0000265869.72265.0a
5. Peterson G, Jackson S, Fitzmaurice K, Gee P. Attitudes of Australian pharmacists towards practice-based research. J Clin Pharm Ther. (2009) 34:397–405. doi: 10.1111/j.1365-2710.2008.01020.x
6. Kritikos VS, Carter S, Moles RJ, Krass I. Undergraduate pharmacy students' perceptions of research in general and attitudes towards pharmacy practice research. Int J Pharm Pract. (2013) 21:192–201. doi: 10.1111/j.2042-7174.2012.00241.x
7. Badowski M, Mazur JE, Lam SW, Miyares M, Schulz L, Michienzi S. Engaging in collaborative research: focus on the pharmacy practitioner. Hosp Pharm. (2017) 52:33–43. doi: 10.1310/hpj5201-33
8. Poloyac SM, Empey KM, Rohan LC, Skledar SJ, Empey PE, Nolin TD, et al. Core competencies for research training in the clinical pharmaceutical sciences. Am J Pharm Educ. (2011) 75:27. doi: 10.5688/ajpe75227
9. Slack MK, Martin J, Worede L, Islam S. A systematic review of extramural presentations and publications from pharmacy student research programs. Am J Pharm Educ. (2016) 80:100. doi: 10.5688/ajpe806100
10. Accreditation Council for Pharmacy Education. Accreditation Standards and Guidelines for the Professional Program in Pharmacy Leading to the Doctor of Pharmacy Degree. Chicago, IL: Accreditation Council for Pharmacy Education (2006).
11. Brazeau GA, Meyer SM, Belsey M, Bednarczyk EM, Bilic S, Bullock J, et al. Preparing pharmacy graduates for traditional and emerging career opportunities. Am J Pharm Educ. (2009) 73:157. doi: 10.5688/aj7308157
12. Medina MS, Plaza CM, Stowe CD, Robinson ET, DeLander G, Beck DE, et al. Center for the Advancement of Pharmacy Education 2013 educational outcomes. Am J Pharm Educ. (2013) 77:162. doi: 10.5688/ajpe778162
13. Canadian Council for Accreditation of Pharmacy P. Accreditation standards for Canadian first professional degree in pharmacy programs. Toronto, ON: CCAPP Toronto (2018).
14. Lee MW, Clay PG, Kennedy WK, Kennedy MJ, Sifontis NM, Simonson D, et al. The essential research curriculum for doctor of pharmacy degree programs. Pharmacotherapy. (2010) 30:966. doi: 10.1592/phco.30.9.966
15. Surratt CK, Drennen Iii JK, Douglas Bricker J. The” Research Track“ concentration, a new PharmD elective option. Am J Pharm Educ. (2005) 691–5. doi: 10.5688/aj690590
16. Wiley TL, Rowe JM, Hammond DA. Making the most of advanced pharmacy practice experiences. Am J Health Syst Pharm. (2017) 74:648–51. doi: 10.2146/ajhp160202
17. Cailor SM, Chen AMH, Kiersma ME, Keib CN. The impact of a research course on pharmacy students' perceptions of research and evidence-based practice. Curr Pharm Teach Learn. (2017) 9:28–36. doi: 10.1016/j.cptl.2016.08.031
18. Perez A, Rabionet S, Bleidt B. Teaching research skills to student pharmacists in one semester: an applied research elective. Am J Pharm Educ. (2017) 81:16. doi: 10.5688/ajpe81116
19. Gebremariam ET, Gadisa DA. Evaluation of the undergraduate pharmacy student research projects in Ambo University, Ethiopia: retrospective review. Adv Med Educ Pract. (2021) 12:205–13. doi: 10.2147/AMEP.S297038
20. Islam MA, Gunaseelan S, Khan SA. A research elective course on dietary supplements to engage doctor of pharmacy students in primary literature evaluation and scholarly activity. J Pharm Pract. (2015) 28:577–84. doi: 10.1177/0897190013516510
21. Leach MJ, Hofmeyer A, Bobridge A. The impact of research education on student nurse attitude, skill and uptake of evidence-based practice: a descriptive longitudinal survey. J Clin Nurs. (2016) 25:194–203. doi: 10.1111/jocn.13103
22. Dong T, Durning SJ, Gilliland WR, Waechter DM, Cruess DF, DeZee KJ, et al. Exploring the relationship between self-reported research experience and performance in medical school and internship. Mil Med. (2012) 177(Suppl. 9):11–5. doi: 10.7205/MILMED-D-12-00232
23. Bovijn J, Kajee N, Esterhuizen TM, Van Schalkwyk SC. Research involvement among undergraduate health sciences students: a cross-sectional study. BMC Med Educ. (2017) 17:1–10. doi: 10.1186/s12909-017-1025-x
24. Bhagavathula AS, Bandari DK, Tefera YG, Jamshed SQ, Elnour AA, Shehab A. The attitude of medical and pharmacy students towards research activities: a multicenter approach. Pharmacy. (2017) 5:55. doi: 10.3390/pharmacy5040055
25. Zaidan M, Singh R, Wazaify M, Tahaineh L. Physicians' perceptions, expectations, and experience with pharmacists at Hamad Medical Corporation in Qatar. J Multidiscip Healthc. (2011) 4:85. doi: 10.2147/JMDH.S14326
26. Kheir N, Fahey M. Pharmacy practice in Qatar: challenges and opportunities. South Med Rev. (2011) 4:92. doi: 10.5655/smr.v4i2.1007
27. Awaisu A, Kheir N, Alrowashdeh HA, Allouch SN, Jebara T, Zaidan M, et al. Impact of a pharmacy practice research capacity-building programme on improving the research abilities of pharmacists at two specialised tertiary care hospitals in Qatar: a preliminary study. J Pharm Health Serv Res. (2015) 6:155–64. doi: 10.1111/jphs.12101
28. CPH-QU. BSc in Pharmacy. Available online at: http://www.qu.edu.qa/pharmacy/departments/programs/bachelor-Pharmacy (accessed May 27, 2022).
29. Alhomoud FK. Pharmacists' background, interests, barriers, self-perceived competence and confidence to design and undertake pharmacy practice-based research in the GCC geographic area. BMC Med Educ. (2020) 20:1–12. doi: 10.1186/s12909-020-02346-4
30. Al-Arifi MN. Attitudes of pharmacy students towards scientific research and academic career in Saudi Arabia. Saudi Pharm J. (2019) 27:517–20. doi: 10.1016/j.jsps.2019.01.015
31. Kritikos VS, Saini B, Carter S, Moles RJ, Krass I. Factors influencing pharmacy students' attitudes towards pharmacy practice research and strategies for promoting research interest in pharmacy practice. Pharm Pract. (2015) 13:587. doi: 10.18549/PharmPract.2015.03.587
32. Awaisu A, Bakdach D, Elajez RH, Zaidan M. Hospital pharmacists' self-evaluation of their competence and confidence in conducting pharmacy practice research. Saudi Pharm J. (2015) 23:257–65. doi: 10.1016/j.jsps.2014.10.002
33. Stewart D, Paudyal V, Cadogan C, Hazen A, Okuyan B, Lutters M, et al. A survey of the European Society of Clinical Pharmacy members' research involvement, and associated enablers and barriers. Int J Clin Pharm. (2020) 42:1073–87. doi: 10.1007/s11096-020-01054-9
34. Keib CN, Cailor SM, Kiersma ME, Chen AMH. Changes in nursing students' perceptions of research and evidence-based practice after completing a research course. Nurse Educ Today. (2017) 54:37–43. doi: 10.1016/j.nedt.2017.04.007
35. Michie S, Johnston M, Abraham C, Lawton R, Parker D, Walker A. Making psychological theory useful for implementing evidence based practice: a consensus approach. BMJ Qual Saf. (2005) 14:26–33. doi: 10.1136/qshc.2004.011155
36. Stewart D, Klein S. The use of theory in research. Int J Clin Pharm. (2016) 38:615–9. doi: 10.1007/s11096-015-0216-y
37. Partido BB, Colón M. Motivations and challenges towards research activities among undergraduate dental hygiene students. Am Dent Hyg Assoc. (2019) 93:23.
38. Park SJ, McGhee CN, Sherwin T. Medical students' attitudes towards research and a career in research: an Auckland, New Zealand study. NZ Med J. (2010) 123:34–42.
39. Sheehan AH, Wagner LE, Sowinski KM. Student pharmacists' knowledge of biostatistical and literature evaluation concepts. Curr Pharm Teach Learn. (2016) 8:622–8. doi: 10.1016/j.cptl.2016.06.013
40. Munabi IG, Katabira ET, Konde-Lule J. Early undergraduate research experience at Makerere University Faculty of Medicine: a tool for promoting medical research. Afr Health Sci. (2006) 6:182–6. doi: 10.5555/afhs.2006.6.3.182
41. Sánchez-García I. Molina MdPU, López-Medina IM, Pancorbo-Hidalgo PL. Knowledge, skills and attitudes related to evidence-based practice among undergraduate nursing students: a survey at three universities in Colombia, Chile and Spain. Nurse Edu Pract. (2019) 39:117–23. doi: 10.1016/j.nepr.2019.08.009
42. Harirforoosh S, Stewart DW. A descriptive investigation of the impact of student research projects arising from elective research courses. BMC Res Notes. (2016) 9:1–5. doi: 10.1186/s13104-016-1865-1
43. Nykamp D, Murphy JE, Marshall LL, Bell A. Pharmacy students' participation in a research experience culminating in journal publication. Am J Pharm Educ. (2010) 74:47. doi: 10.5688/aj740347
44. Gebremariam ET, Gadisa DA. Factors affecting the quality of undergraduate pharmacy students' researches in Ambo University, Ethiopia: a qualitative study from advisors' perspective. Adv Med Educ Pract. (2021) 12:745. doi: 10.2147/AMEP.S316201
45. Mugabo E, Velin L, Nduwayezu R. Exploring factors associated with research involvement of undergraduate students at the College of Medicine and Health Sciences, University of Rwanda. BMC Med Educ. (2021) 21:1–9. doi: 10.1186/s12909-021-02662-3
46. Taylor JG, Szmukier Z. Graduate studies as part of a career path for saskatchewan pharmacy students: current high salaries for practitioners cited as one deterrent to graduate work. Can Pharm J. (2005) 138:43–9. doi: 10.1177/171516350513800706
47. Johnson JA, Moore MJ, Shin J, Frye RF. A summer research training program to foster PharmD students' interest in research. Am J Pharm Educ. (2008) 72:23. doi: 10.5688/aj720223
48. Overholser BR, Foster DR, Henry JR, Plake KS, Sowinski KM. The influence of an elective introductory clinical research course on pharmacy student interest in pursuing research-based careers. Am J Pharm Educ. (2010) 74:165. doi: 10.5688/aj7409165
49. Heffernan CJ. Social foundations of thought and action: a social cognitive theory, Albert Bandura Englewood Cliffs, New Jersey: Prentice Hall, 1986, xiii+ 617 pp. Hardback US $3950 Behav Change. (1988) 5:37–8. doi: 10.1017/S0813483900008238
50. Vujaklija A, Hren D, Sambunjak D, Vodopivec I, Ivaniš A, Marušić A, et al. Can teaching research methodology influence students' attitude toward science? Cohort study and nonrandomized trial in a single medical school. J Investig Med. (2010) 58:282–6. doi: 10.2310/JIM.0b013e3181cb42d9
Keywords: pharmacy, research courses, significance, interest, confidence, outcomes, motivation, Theoretical Domains Framework (TDF)
Citation: Mukhalalati B, Elshami S, Adlan O, Elshazly M, Awaisu A, Stewart D, Al-Badriyeh D and Alali F (2022) Perceptions and experiences of undergraduate pharmacy students and alumni toward research after exposure to undergraduate research courses. Front. Med. 9:988908. doi: 10.3389/fmed.2022.988908
Received: 07 July 2022; Accepted: 22 August 2022;
Published: 08 September 2022.
Edited by:
Kathryn Toy Knecht, Loma Linda University, United StatesReviewed by:
Diriba Gadisa, Ambo University, EthiopiaKatharina Brandl, University of California, San Diego, United States
Copyright © 2022 Mukhalalati, Elshami, Adlan, Elshazly, Awaisu, Stewart, Al-Badriyeh and Alali. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Banan Mukhalalati, YmFuYW4ubUBxdS5lZHUucWE=
†These authors have contributed equally to this work
 Banan Mukhalalati
Banan Mukhalalati Sara Elshami
Sara Elshami Ola Adlan†
Ola Adlan† Ahmed Awaisu
Ahmed Awaisu Derek Stewart
Derek Stewart Feras Alali
Feras Alali
