- 1Centre for Host–Microbiome Interactions, Faculty of Dentistry, Oral & Craniofacial Sciences, Kings College London, London, United Kingdom
- 2Eastman Dental Institute, Paediatric Dentistry Department, University College London, London, United Kingdom
Innovation has always been part of dentistry and with that comes thinking outside the box to produce guidelines for implementation of new approaches. Regenerative dentistry (RD) is a young specialty within the profession, which gathers knowledge from stem cells, molecular biology, and tissue and material engineering to produce and apply novel biologically based therapies. Since RD is an emerging branch of dentistry, it is not yet understood whether active clinicians are aware of this field and know exactly what it does. The aim of this study is to explore the awareness, understanding, and beliefs about RD of active dentists. A random selection of active dentists in the UK was approached via e-mail and face-to-face and asked to fill in a questionnaire. A total of 45 responses were received and analyzed. The results showed that active dentists in the UK are aware of the field but are not prepared to apply personalized biologically based therapies and feel a desire to educate themselves about RD further. Also, the results shine a light on the opportunities for regulatory and educational bodies to work together to prepare the clinicians for this novel field. Our research suggests that active dentists are ill-prepared for an era of personalized biologically based dental treatments. Further thinking of how to implement basic and more advanced biological knowledge and their application in dentistry is needed, and suggestions are made here.
Introduction
Regenerative dentistry (RD) is an up and coming dental specialty that works toward the birthing of innovative treatments that are fully based on the biology of the body. Novel biologically based tools (biomarkers, genetic screening, and stem cell-based treatments) are available to the public (1–4), and any dental practitioner may face the request to have these biologically based options in his or her treatment plan. Explaining biomarker results to patients or providing these novel therapy options requires a deep understanding of molecular biology, stem cells, and tissue engineering. Nevertheless, dental education is still highly focused on technical hand abilities and the materials that will be placed in the patient rather than understanding the biological potential of patients themselves.
Real-life examples of these new biological tools currently available in the market diagnostic tools such as PerioPredict®, Celsus One™, OMNIgene®. Likewise, treatments based on growth factors and stem cells are readily available in the market [recombinant human Insulin-like growth factor-1 (rhIGFs), recombinant human bone morphogenetic protein (rhBMPs), human recombinant basic fibroblast growth factor (rhFGF) REGROTH® Dental Kit, recombinant human platelet-derived growth factor (rhPDGFs), platelet-rich plasma (PRP), platelet-rich fibrin (PRF), ZenBio®, The Regenerative Clinic®]. In addition, biological therapies using stem cells [third molar dental pulp and stem cells from exfoliated deciduous teeth (SHED)] to regenerate whole dental pulps in patients who underwent pulpectomy have already been shown to be successful (5, 6), and soon these therapies will reach the market. The question is, are dentists equipped to offer such biologically based therapeutic tools to patients?
We hypothesized that active dentists in the United Kingdom (UK) are not ready for RD; therefore, further understanding of the knowledge level, expectations, and beliefs dentists hold about biologically based therapies is needed. To achieve that, a questionnaire was generated to understand the percentage of dentists who are exposed and believe that they understand the topics of basic biology that comprises RD. This study adds pilot evidence on how prepared dentists are to apply biologically based treatment options. This questionnaire research investigated the UK-based dentists' levels of RD awareness, exploring their understanding and beliefs about this area of the profession. This pilot research raises major points on how ill-prepared dentists seem to be for applying personalized biologically based therapies and suggests potential strategies to improve the motivation of learning in the field and policy making. The result of this questionnaire adds information to educators and policy makers for the appropriate changes to be set up in support of dentistry evolution, this way decreasing the potential of future biological iatrogenesis.
Methods
This was a single-centered quantitative study. A questionnaire was created with questions that could show awareness, understanding, and beliefs about RD (Supplementary Data). Participants were approached online or in person. In this pilot study, we aimed to collect data from 10% of the ideal sample size of the UK dentist's representation [38 participants (95% confidence level and 5% margin error)]. The questionnaire was cascaded to a King's College London Dental Faculty mailing list on February 2019. The survey was open for 8 weeks, until April 2019. During this time, respondents were sent two e-mail reminders. The participants were a random selection of dentists in the UK from different backgrounds and specialties who were involved in National Health Service (NHS) and/or private practice (n = 45). The inclusion criterion was to be an active dentist working in the UK; the exclusion criterion was any other dental professional who was not a dentist. If they agreed to undertake the study, the submission of a completed online survey/printed questionnaire/online app data was implied consent. Missing responses were not added to the analysis.
To give context, the term “regenerative dentistry” was defined in the information sheet as “a new field of dentistry that gathers knowledge about stem cells, molecular biology, and tissue and material engineering aiming to create and apply new clinical treatments based on the biology of the body.”
This study was given ethics clearance by King's College London ethics committee (MRA-18/19-10479) and was conducted in line with usual guidelines pertaining to participants' rights to anonymity, confidentially, and withdraw. All information obtained was treated as strictly confidential, under General Data Protection Regulation (GDPR) rules, and the participants cannot be indefinable.
Data Analysis
Data were explored using SPSS for descriptive statistics. The questions were checked for consistency using Cronbach alpha, and questions >0.7 were excluded. One open-ended question was analyzed using a free word cloud generation (https://www.wordclouds.com/).
Results
Demographics
A balanced ratio of male/female individuals participated in the questionnaire (female, n = 20; male, n = 24; prefer not to say, n = 1) (Figure 1A). The participants were predominantly aged between 18 and 40 years of age (77.7%), with 57.8% having graduated from their Bachelor in Dental Surgery (BDS) in the last decade (2010–2018), and 62.2% had a postgraduate degree. Those who replied “other” (n = 6) had the following degrees: Master of Business Administration (MBA), Postgraduate Diploma (PgDip) (n = 2), Doctor of Dental Medicine (DMD), Dental Residency, Master of Philosophy (MPhil).
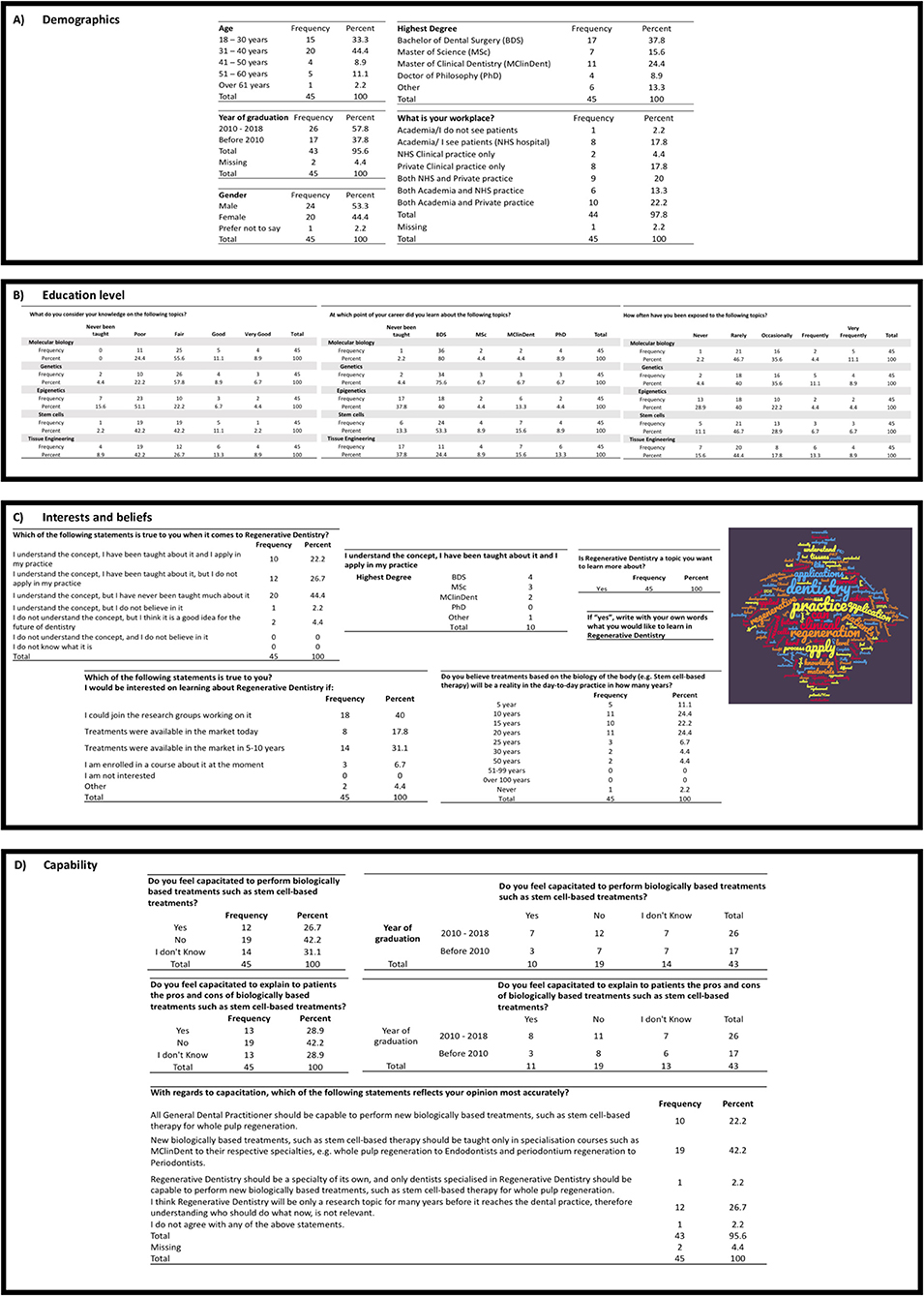
Figure 1. Questions and answers about demographics, education level, interests and beliefs, and capability.
Among the participants, 24.4% had clinical speciality training (n = 11), and 8.9% were Doctors of Philosophy (PhDs) (n = 4). The participants' workplaces were varied; however, the participants were predominantly dentists who work in private practice (60%).
Education Level
The results of the questionnaire showed that active dentists think their knowledge in molecular biology, genetics, epigenetics, tissue engineering, and stem cells ranges predominantly from fair to poor, averaging 79.32% of all respondents in that scale (Figure 1B). Moreover, exposure to RD topics, such as molecular biology, genetics, epigenetics, and stem cells, took place majorly in their BDS. Tissue engineering and epigenetics, however, are topics that the majority has never been taught (37.8%). Finally, 84.02% of the active dentists occasionally to never get exposed to these topics during their careers (average between all topics).
Interest and Beliefs
Next, the questionnaire probed the dentists' interests and beliefs about RD (Figure 1C). When asked to correlate their feelings about RD to sentences, 93.3% of the responses said that they understand the concept of RD. However, the majority (44%, n = 20) felt that they have never been taught the subject. However, 22.2% of the respondents felt that they have been taught about it and apply the concept in their practice.
To understand who feels comfortable with their level of knowledge and application of such approaches in practice, a cross tabulation of the results was performed. The results showed that dentists with different levels of education answered positively. Interestingly, no PhD-holding dentist felt comfortable with their level of knowledge and application of such approaches in practice.
Further, the questionnaire showed that all participants want to learn more about RD, and when asked what they would like to learn, the most common theme on the open answers was “application,” appearing 12 times (apply, n = 4; application, n = 3; applications, n = 3; applied, n = 2). Examples of the answers were: “how to apply it in clinics,” “how can we apply the researches and lab work done on clinical practice,” “Viable applications in dentistry.”
The questionnaire also probed how the participants wanted to be involved in learning about RD. Most participants would be interested in learning about RD if they could be part of a research group on the topic (40%). Those who replied “other” felt that they would be interested in learning about RD if (1) they “could attend lectures and study discussions,” (2) “It was accessible, achieved CPD, and broadened my knowledge.”
Finally, it was also essential to understand when the participants believe that treatments based on the biology of the body would be available in day-to-day practice. The majority of the participants thought that in the next 5–15 years (57.7%), these treatments would be a reality in day-to-day practice.
Capability
Given that dentists are, and will be, in charge of treating patients with translational RD techniques, in this section, the questionnaire explored whether this dentist sample felt capable of both explaining the pros and cons of and performing biologically based treatments such as stem cell-based treatment (Figure 1D).
The results showed that dentists were not confident that they could perform and explain the pros and cons of biologically based therapies such as stem cell-based therapies (73.3 and 71.1% of “No” and “I don't know” answers, respectively).
Interestingly, a small demographic felt that they were capable to perform and explain (26.7 and 28.9% of “Yes” answers, respectively). To understand who felt they were capable, a cross tabulation was performed, showing that the majority of those who feel capable have graduated in the past decade. However, those who graduated in the last decade also represent the majority of those who do not feel capable.
The final section on capability probed what the participants believed with regard to the necessary capability for performing RD approaches in practice. The results showed that the participants believe that the training for these techniques should be taught in clinical speciality training of their respective specialities, for example, whole pulp regeneration to endodontists and periodontium regeneration to periodontists (42.2%). Interestingly, 26.7% of the participants thought that who could perform these new treatments was not a relevant topic to discuss, and only one participant thought it should be a specialty of its own.
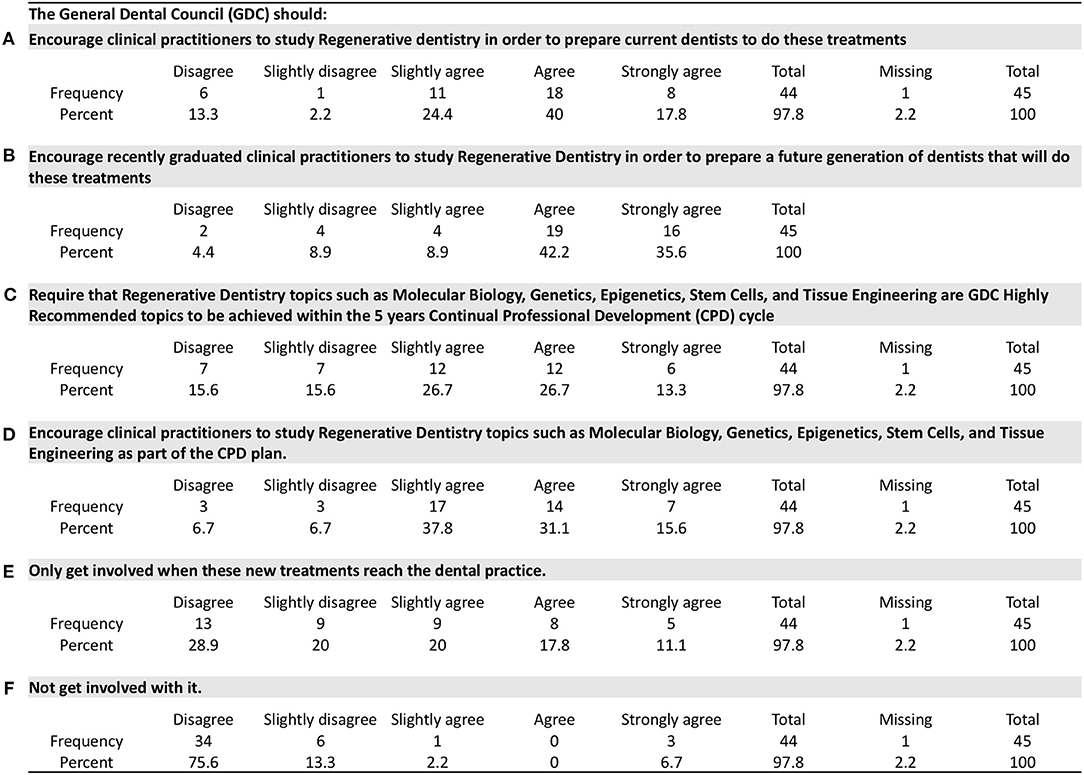
General Dental Council Policy Suggestion
In the UK, the General Dental Council (GDC) is responsible for implementing strategies to protect the patients. In order to add safe novel RD therapies in practice, the participants were asked how the GDC should approach such a case. The suggestions of how to implement regenerative knowledge in the dentists' day-to-day showed that the majority agreed that it is important for both current and future practitioners to study RD (Figures 2A,B). Moreover, the participants agreed that a Continuing Professional Development (CPD) course should be encouraged by the GDC on the RD topics such as molecular biology, genetics, epigenetics, tissue engineering, and stem cells (Figures 2C,D). However, they do not support the idea for it to be a recommended topic, that is, to be required in the CPD 5-year cycle.
Moreover, 48.9% of the participants believe that the GDC should take action prior to new biologically based treatments to be implemented in dental practice as a marketable product, and predominantly (88.9%) the participants suggested that the GDC should get involved in regulating it (Figures 2E,F).
Discussion
Novel biologically based therapies for humans' oral health improvement are in the making around the world. Dentists will be the “applicants” of such novel therapies, and to provide the correct treatment to patients and avoid iatrogenesis, this professional class must develop a deeper biological knowledge to apply these novel techniques, namely (but not limited to), stem cell-based therapies.
Recently, the authors published opinion pieces on how dentistry should focus on biology advance development of novel therapies and the need to expose young dentists to RD topics (7, 8). Here, questionnaire data were presented to illustrate the level of RD awareness, beliefs, and possible strategies to implement further clinical–biological knowledge in the education of dentists.
The results of this questionnaire showed that although dentists have learned the topics necessary to apply new biologically based techniques in their BDS, following their BDS, the participants lose touch with these subjects, with the majority expressing that they rarely encounter these topics in their careers. Additionally, given that the majority of dentists do not feel capacitated to provide and explain biologically based treatments, it is suggested that dentists' knowledge levels are lower than necessary for such therapies to be applied with safety. Therefore, further professional development in the field is needed.
According to the participants, there is a high interest in further education and research in RD, showing the desire to learn and contribute to the development of cutting-edge techniques. Interestingly, what would help dentists to further educate themselves in this field is to be presented with opportunities to be involved with research and learn about the applications of such approaches in clinical practice. Further, the participants of this questionnaire believed that whoever should apply such approaches must apply within their specialty. However, this questionnaire does not have the power to answer whether specialty training programs are preparing the specialists for such approaches.
A surprise in this questionnaire was to see that a small demographic felt that they were capable to perform and explain RD techniques. These results raise a red flag on the possibility of application of techniques without adequate training, leading to iatrogenesis, which, in the case of biologically based techniques, may be more detrimental to the patient than a misplaced dental implant. Therefore, it is important to strategize how training for these techniques should take place.
One could infer that in order to learn a novel technique in dentistry at application level, one ought to experience it from the basics to the application, as in the case of, for example, placing a denture. In this case, the education strategy relies on the dentist in training learning/experiencing how to do all the laboratorial steps before the denture can be fitted in the mouth, working its way up to fitting and adjustments in the mouth. If a dentist would like to provide, for example, cell transplants in his practice, we would argue that they would have to be trained in all the cell culture technical steps. However, in dentistry, the thought of having dentists in training, both undergrad and specialties, learning how to do cell culture, seems far-fetched, and changing a whole system to focus on that also seems difficult. Yet, that does not mean that our argument is destined to fail. Through the years, different dental materials have been created, and current dental education requires that in-depth chemical and physical properties of these materials must be understood by the active clinician. Therefore, we suggest further education, exposure, and research incentives for dentists to pursue in-depth knowledge of the biology of the human body.
Many novel approaches in the history of dentistry have faced intense criticism and disbelief before being established as part of basic routine care in the profession. The amalgam filling, for example, which is now righteously in phasing, was a revolutionary idea and material (9); however, dentists firstly opposed to the newly developed mercury paste (10). Further, about 70 years ago when toothbrushing was suggested as an absolute good for oral health, there was a backlash from the profession suggesting that oral hygiene was purely an esthetic choice (11). These examples illustrate the amount of trouble novelty must face in the eyes of a close-minded profession. Nevertheless, today, such approaches are used routinely. These examples spark hope for RD approaches to be 1 day in routine care.
However, the sheer desire of the authors and the dental community to make this a reality is not enough. In the UK, for RD to find a place within the ordinary and specialist dental practices, the GDC must take a stance. This regulatory body oversees the quality of education for dentists in training, specialties, and CPDs, and yet, the GDC fails to mention the importance of simple novel techniques in RD, such as stem cells and their clinical application and current market options. The participants of this questionnaire believe that the GDC should be part of regulating RD and promoting CPD to the professionals in the UK.
Finally, it is crucial to think how the market/professional model for RD will be implemented; thus here, some strategies for the case of cell therapies will be suggested: (1) Dentists have their own cell laboratory and storage in their dental practice (same as those practices with a prosthesis laboratory), (2) Dentists outsource the laboratory phase from a partner laboratory (same as those practices that do not have a prosthesis laboratory), and 3) Do not implement cell therapy in the dental practice. It is noteworthy that further analysis and thought must be given to this topic; however, due to lack of space, we will not develop these strategies here.
This unique pilot study lays the grounds and initiates a debate pointing that action should be taken to equip the dentist with the knowledge necessary for RD and be able to apply it in their dental practice. The current dental curriculum does not seem to be preparing the professional for this new biological era; therefore, a larger global study is required to gather data and evaluate dentists' attitude toward RD education.
Conclusion
This questionnaire raises major points on how ill-prepared dentists seem to be for applying personalized biologically based therapies. The majority of dentists believe that their knowledge on, and frequency of exposure to, RD subjects is poor, shedding light on the need for change. Moreover, it highlights how regulatory bodies and educational bodies could work together to prepare clinicians for this novel field.
Limitations
Although this is a study with a little n-number and the location where the active dentists were graduated is not taken in consideration, this research is unique and unprecedented in the world.
The major drawback from this quantitative research is that misinterpretation of the question or related topics may have led to unsure answers. Moreover, there was a bias of the questionnaire maker, who knows the subject better than the participants. Therefore, a non-biased qualitative research with open questions is crucial for eliciting the perceptions and dentist's current understanding of what biologically based diagnostic tools and treatments are and their potential in clinical practice.
Data Availability Statement
The original contributions presented in the study are included in the article/Supplementary Material, further inquiries can be directed to the corresponding author/s.
Ethics Statement
The studies involving human participants were reviewed and approved by King's College London ethics committee (MRA-18/19-10479). The patients/participants provided their written informed consent to participate in this study.
Author Contributions
VN contributed to the conception, design, data acquisition, interpretation, and analysis and drafted and critically revised the manuscript. HJ contributed to drafting and critically revising the manuscript. Both authors gave final approval and agree to be accountable for all aspects of the work.
Conflict of Interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Acknowledgments
The authors would like to thank Faye Kilgour for reviewing and correcting this manuscript. Also, Paul Sharpe and Professor Jennifer Gallagher for their valuable insights into the questionnaire. Finally, I would like to thank the participants who spent their valuable time to contribute to this research.
Supplementary Material
The Supplementary Material for this article can be found online at: https://www.frontiersin.org/articles/10.3389/fdmed.2021.630546/full#supplementary-material
References
1. Celsus OneTM. Available online at: https://www.oraldna.com/test/mpid/ (accessed 8, June 2020).
2. 23andMe®. Available online at: https://www.23andme.com/en-gb/ (accessed 8, June 2020).
3. Zen-Bio® Stem-cell based treatments off shelf. Available online at: https://www.zen-bio.com/ (accessed 8, June 2020).
4. The Regenerative Clinic® provides Medical stem cell treatment. Available online at: https://www.theregenerativeclinic.co.uk/the-procedure/ (accessed 8, June 2020).
5. Nakashima M, Iohara K, Murakami M, Nakamura H, Sato Y, Ariji Y, et al. Pulp regeneration by transplantation of dental pulp stem cells in pulpitis: a pilot clinical study. Stem Cell Res Ther. (2017) 8:61. https://doi.org/10.1186/s13287-017-0506-5
6. Xuan K, Li B, Guo H, Sun W, Kou X, He X, Zhang Y, et al. Deciduous autologous tooth stem cells regenerate dental pulp after implantation into injured teeth. Sci Transl Med. (2018) 10:eaaf3227. https://doi.org/10.1126/scitranslmed.aaf3227
7. Neves VCM. A new perspective to push forward a stagnated dental world. Br Dent J. (2019) 227:85–7. doi: 10.1038/s41415-019-0518-x
8. Jamal H, and Elhussein M. Integration of regenerative dentistry into the dental undergraduate curriculum. Front Dent Med. (2020) 1:596189. doi: 10.3389/fdmed.2020.596189
9. FDI Amalgam phasing plans. Available online at: https://www.fdiworlddental.org/minamata-convention-mercury (accessed 8, June 2020)
Keywords: regenerative dentistry, education, dental education, stem cells, translation, policymaking
Citation: Neves VCM and Jamal H (2021) A Pilot Epidemiological Exploration of Regenerative Dentistry From the Perspective of Active Clinicians Working in the UK. Front. Dent. Med. 2:630546. doi: 10.3389/fdmed.2021.630546
Received: 17 November 2020; Accepted: 02 February 2021;
Published: 10 March 2021.
Edited by:
Alastair James Sloan, University of Melbourne, AustraliaReviewed by:
Mohammed El-Awady Grawish, Mansoura University, EgyptWaruna Lakmal Dissanayaka, The University of Hong Kong, Hong Kong
Copyright © 2021 Neves and Jamal. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Vitor C. M. Neves, dml0b3IubmV2ZXNAa2NsLmFjLnVr
 Vitor C. M. Neves
Vitor C. M. Neves Hasan Jamal
Hasan Jamal