- Cancer Research UK Centre, MRC Institute of Genetics and Molecular Medicine, University of Edinburgh, Edinburgh, UK
Introduction
Only two new drugs have been licensed for the treatment of epithelial ovarian cancer in the last 5 years (bevacizumab and olaparib). These are also the only two molecularly targeted agents licensed in this disease. As we continue to move into the genomic era of cancer therapy, it is clear that optimal therapy is going to depend on molecular stratification and that the stratification itself is going to need to contend with tumor heterogeneity. In this article, we discuss molecular stratification and tumor heterogeneity in the context of high-grade serous ovarian cancer.
The development of bevacizumab and olaparib has provided contrasting examples of stratification in molecularly targeted agents. Bevacizumab is licensed as an unselected agent, currently without molecular (or indeed histological) stratification. However, emerging data may be able to help us refine which patients may benefit the most from this agent (and which may not require it). Any such refinement can be expected to increase the median benefit in the selected population and reinforce the cost:benefit advantage. Conversely, olaparib is licensed as a highly selected agent, currently by genomic or somatic BRCA1/BRCA2 mutation in high-grade serous cancer. However, emerging data may be able to help us expand its role into tumors with other homologous recombination deficits (while also determining if all BRCA1/BRCA2 mutations respond equally). For both agents, however, cancers progress even on continuous therapy and targeting the resistant clones that have emerged from tumor heterogeneity will be key to extending benefit for these patients.
Bevacizumab
Bevacizumab is the first vascular endothelial growth factor (VEGF)-targeted therapy to have been licensed in ovarian cancer; by the European Medicines Agency (EMA) in 2011 and the United States Food and Drug Administration (FDA) in 2014. These licenses differ although in both cases the bevacizumab is given in combination with chemotherapy. The EMA license was the result of first line data from the GOG 218 (1) and ICON7 (2) studies, second line platinum sensitive data from OCEANS (3) and second line platinum resistant data from AURELIA (4) all of which demonstrated a statistically significant increase in progression free survival compared to chemotherapy alone. The FDA license relates to the platinum resistant setting only and was dependent on the data from the AURELIA study. The optimal setting for this treatment is unknown (5), as is the value of treating through progression or utilizing combinations of anti-angiogenic therapies. VEGF-targeted therapy is clearly an active approach in ovarian cancer (at least in combination with chemotherapy) and other anti-angiogenic agents have been investigated in this setting including pazopanib (6), cedirinib (7), nintedanib (8), aflibercept (9), trebananib (10), sunitinib (11), sorafenib (12), and (PDGFR) imatinib (13).
Given the mode of action, it was not unreasonable to seek potential broad activity for bevacizumab and, as with all previous agents in ovarian cancer, these trials had no molecularly or histological stratification. However, potential biomarkers are now emerging for benefit from bevacizumab (14), building on the extensive translational work incorporated in ICON7. For blood biomarkers, a link is evident between circulating Ang1 plus Tie2 levels and progression free survival (15), with most of the benefit from bevacizumab in the high Ang1-low Tie2 group (HR 0.27), no significant effect in the low Ang1 group and a detriment in the high Ang1-high Tie2 group (HR 3.6). A possible link noted with plasma VEGF-A in other tumor types (16), was not seen in this ovarian dataset. For tissue biomarkers, a signature made up of tissue mesothelin, FLT4 and AGP and blood CA125 also has potential to strongly differentiate between benefit and harm from bevacizumab but was limited by patient numbers in the analysis (17). Recently, a transcriptomic signature has been presented (18), which identifies distinct molecular subgroups of high-grade serous ovarian cancer that respond very differently to bevacizumab. In this analysis, the two proangiogenic subgroups had a poorer overall survival but appeared to contain all the benefit from bevacizumab. The other, immune subgroup had a superior prognosis but had a detriment (HR 2.0) from bevacizumab. This data will need confirmation in further datasets but the above examples suggest that we are getting closer to a molecular biomarker for bevacizumab benefit (and resistance). The next step will of course be identifying if these molecular signals also emerge in acquired resistance and if they indicate a druggable pathway to improve or extend the activity of VEGF-directed therapies to resistant tumors (or resistant clonal subpopulations). The story may be complicated by the fixed duration of bevacizumab in some studies (such as ICON7) but continuous maintenance therapy is the expected direction of travel for the future.
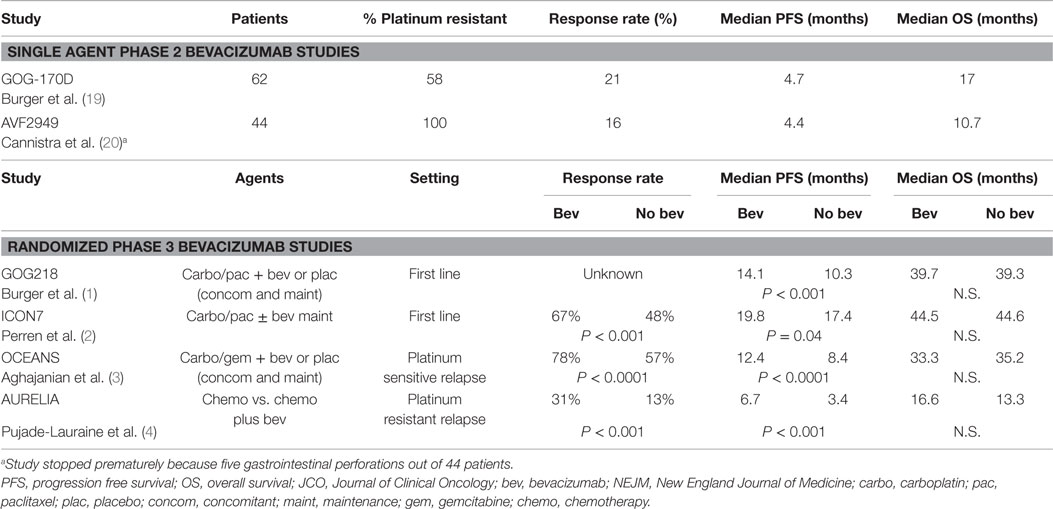
Hopefully, the above approaches can help address the mystery of why VEGF-directed therapy does not yet seem to be living up to its clear potential. In the phase 2 single agent studies (19, 20), bevacizumab had a roughly 20% objective response rate (ORR), a figure matched by the additional ORR benefit seen compared to chemotherapy alone in phase 2 and phase 3 combination studies, regardless of setting (Table 1). It is unclear why this clear ORR benefit has not translated into more impressive PFS or OS benefits in the phase 3 first line studies (PFS benefit 3.8m in GOG 218 and 2 months in ICON7, with updated analysis of the latter non-significant and no OS benefit in the ITT population). It seems likely that there is a subset benefiting greatly from therapy (and this subset will be evident when response rate is the primary endpoint, as in some phase 2 studies) but that the effect is being diluted by the current lack of a selection biomarker and is therefore harder to detect when PFS is the primary endpoint (as in the phase 3 studies). Identifying this subset may be the key to widening its licensed indications. Identifying the tumor heterogeneity that leads to resistance to VEGF-directed therapy may be the key to improving and prolonging the benefit.
Olaparib
Olaparib is the first poly ADP ribose polymerase (PARP)-inhibitor to have been licensed in ovarian cancer (2014). The EMA license is as post-chemotherapy maintenance in patients with germline or somatic BRCA1 or BRCA2 mutations. This was as a result of the subgroup analysis (21) of BRCA1/2 mutant cancers (germline or somatic), in the molecularly unselected Study 19 of relapsed platinum sensitive high-grade serous ovarian cancer (22). The FDA license is as monotherapy in patients with deleterious or suspected deleterious germline BRCA mutated advanced ovarian cancer who have been treated with three or more prior lines of chemotherapy. PARP inhibitors have demonstrated strong activity in molecularly selected populations and other agents include rucaparib (23), niraparib (24), veliparib (25), and talazoparib (26).
The target population was a clear priority from the original phase 1 study, where BRCA1/BRCA2 mutation carriers were the predominant responders, leading to a BRCA1/BRCA2 expansion (27), with promising activity in ovarian cancer (28), which was subsequently confirmed in phase 2 (29). However, BRCA1/BRCA2 mutation is known not to be an absolute biomarker for sensitivity and other homologous recombination defects have been strongly implicated as additional predictive biomarkers (30). Study 19 represented a pragmatic approach to enrich for this whole group without genetic testing by looking at a platinum-sensitive, high-grade serous histopathology, ovarian population (22), given the known link between platinum sensitivity, high-grade serous histopathology and BRCA1/2 or wider homologous recombination gene defects (31, 32), even in non-hereditary cases (33, 34). However, although this study did identify activity in the non-BRCA mutant subgroup (HR 0.54), the dramatic effect was really in the BRCA1/2 mutant subgroup (HR 0.18), and the diluted overall signal risked being a barrier to licensing of these important, active agents. Therefore, olaparib is now licensed for BRCA1/2 mutant cancers and steps are being taken to identify additional predictive biomarkers, including other known homologous recombination defects. However, predictive biomarkers are seldom binary and olaparib provides a good example where molecular heterogeneity between patients and within tumors leads to significant variation in activity and resistance.
When comparing different patients with different homologous recombination deficient tumors, we are beginning to realize that all BRCA molecular deficits are not equal – epigenetic changes are clearly a different biology to genetic (30, 32, 35) but what about different specific mutations or the difference between germline and somatic? Today, it is generally accepted that the different histological subgroups of epithelial ovarian cancer represent different diseases (36). However, as with other cancers, it is also clear that different molecular subgroups (30) of high-grade serous ovarian cancer can have different phenotypes (37) and outcomes (38, 39), with homologous recombination defects a clear example. It is natural to extend this to specific homologous recombination proteins and, even further, to specific mutations/defects of individual proteins.
Molecular heterogeneity within an individual’s cancer may be just as important. While adaptive epigenetic changes have been implicated in platinum resistance (40), a more striking mechanism of resistance may underlie some of the cross-resistance of platinum therapy and PARP inhibition that has lead to the focus on platinum sensitive disease in the clinic (28, 41). This is the phenomenon where inactivating mutations within the BRCA1/BRCA2 genes revert to functional genes (41–45), clearly demonstrating the strong selection pressures, which drive outgrowth of a resistant subclone that lacks the one main feature that defined, or even induced, the original cancer but which subsequently had become its Achilles heel. In effect, the tumor is doing whatever it can to evade the agents used against it, even if that means re-expressing the gene that it had to lose in order to become a cancer cell in the first place.
Of course, not every individual’s tumor will contain the resistant subclones that drive this response and much can be learned from the super-responders (28, 46) who give an example of what we might hope to achieve if we could overcome that heterogeneity.
The Future
Clearly, future optimal therapy for high-grade serous ovarian cancer will depend on optimal molecular stratification and this is just as true for bevacizumab and olaparib as it will be for future agents. While this will help rise to the challenge of optimizing therapy for inter-patient molecular heterogeneity, monotherapy may never overcome intra-patient heterogeneity. If we want to improve the durability of responses, that pool of resistant clones may need to be narrowed by using combination therapies. Indeed, recent clinical data for the addition of the VEGFR inhibitor, cedirinib, to olaparib have shown a significant increase in response rate and a near-doubling of progression free survival (47). The majority of this benefit was in the BRCA1/BRCA2 wild-type (or unknown) group, perhaps demonstrating that combinations can overcome monotherapy dependencies but also highlighting that there is still a lot to learn about biomarkers for anti-angiogenic and PARP inhibitor agents in ovarian cancer.
Conflict of Interest Statement
Charlie Gourley has sat on advisory boards for AstraZeneca, Roche, and Nucana. He has also received lecture fees from AstraZeneca and Roche. Through his institution he has received research funding from AstraZeneca, Aprea, and Novartis. Stefan Symeonides declares that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
References
1. Burger RA, Brady MF, Bookman MA, Fleming GF, Monk BJ, Huang H, et al. Incorporation of bevacizumab in the primary treatment of ovarian cancer. N Engl J Med (2011) 365(26):2473–83. doi: 10.1056/NEJMoa1104390
2. Perren TJ, Swart AM, Pfisterer J, Ledermann JA, Pujade-Lauraine E, Kristensen G, et al. A phase 3 trial of bevacizumab in ovarian cancer. N Engl J Med (2011) 365(26):2484–96. doi:10.1056/NEJMoa1103799
3. Aghajanian C, Blank SV, Goff BA, Judson PL, Teneriello MG, Husain A, et al. OCEANS: a randomized, double-blind, placebo-controlled phase III trial of chemotherapy with or without bevacizumab in patients with platinum-sensitive recurrent epithelial ovarian, primary peritoneal, or fallopian tube cancer. J Clin Oncol (2012) 30(17):2039–45. doi:10.1200/JCO.2012.42.0505
4. Pujade-Lauraine E, Hilpert F, Weber B, Reuss A, Poveda A, Kristensen G, et al. Bevacizumab combined with chemotherapy for platinum-resistant recurrent ovarian cancer: the AURELIA open-label randomized phase III trial. J Clin Oncol (2014) 32(13):1302–8. doi:10.1200/JCO.2013.51.4489
5. Monk BJ, Pujade-Lauraine E, Burger RA. Integrating bevacizumab into the management of epithelial ovarian cancer: the controversy of front-line versus recurrent disease. Ann Oncol (2013) 24(Suppl 10):x53–8. doi:10.1093/annonc/mdt472
6. du Bois A, Floquet A, Kim JW, Rau J, del Campo JM, Friedlander M, et al. Incorporation of pazopanib in maintenance therapy of ovarian cancer. J Clin Oncol (2014) 32(30):3374–82. doi:10.1200/JCO.2014.55.7348
7. Matulonis UA, Berlin S, Ivy P, Tyburski K, Krasner C, Zarwan C, et al. Cediranib, an oral inhibitor of vascular endothelial growth factor receptor kinases, is an active drug in recurrent epithelial ovarian, fallopian tube, and peritoneal cancer. J Clin Oncol (2009) 27(33):5601–6. doi:10.1200/JCO.2009.23.2777
8. Ledermann JA, Hackshaw A, Kaye S, Jayson G, Gabra H, McNeish I, et al. Randomized phase II placebo-controlled trial of maintenance therapy using the oral triple angiokinase inhibitor BIBF 1120 after chemotherapy for relapsed ovarian cancer. J Clin Oncol (2011) 29(28):3798–804. doi:10.1200/JCO.2010.33.5208
9. Coleman RL, Duska LR, Ramirez PT, Heymach JV, Kamat AA, Modesitt SC, et al. Phase 1-2 study of docetaxel plus aflibercept in patients with recurrent ovarian, primary peritoneal, or fallopian tube cancer. Lancet Oncol (2011) 12(12):1109–17. doi:10.1016/S1470-2045(11)70244-3
10. Karlan BY, Oza AM, Richardson GE, Provencher DM, Hansen VL, Buck M, et al. Randomized, double-blind, placebo-controlled phase II study of AMG 386 combined with weekly paclitaxel in patients with recurrent ovarian cancer. J Clin Oncol (2012) 30(4):362–71. doi:10.1200/JCO.2010.34.3178
11. Baumann KH, du Bois A, Meier W, Rau J, Wimberger P, Sehouli J, et al. A phase II trial (AGO 2.11) in platinum-resistant ovarian cancer: a randomized multicenter trial with sunitinib (SU11248) to evaluate dosage, schedule, tolerability, toxicity and effectiveness of a multitargeted receptor tyrosine kinase inhibitor monotherapy. Ann Oncol (2012) 23(9):2265–71. doi:10.1093/annonc/mds003
12. Hainsworth JD, Thompson DS, Bismayer JA, Gian VG, Merritt WM, Whorf RC, et al. Paclitaxel/carboplatin with or without sorafenib in the first-line treatment of patients with stage III/IV epithelial ovarian cancer: a randomized phase II study of the Sarah Cannon Research Institute. Cancer Med (2015) 4(5):673–81. doi:10.1002/cam4.376
13. Safra T, Andreopoulou E, Levinson B, Borgato L, Pothuri B, Blank S, et al. Weekly paclitaxel with intermittent imatinib mesylate (Gleevec): tolerance and activity in recurrent epithelial ovarian cancer. Anticancer Res (2010) 30(9):3243–7.
14. Lambrechts D, Lenz HJ, de Haas S, Carmeliet P, Scherer SJ. Markers of response for the antiangiogenic agent bevacizumab. J Clin Oncol (2013) 31(9):1219–30. doi:10.1200/JCO.2012.46.2762
15. Backen A, Renehan AG, Clamp AR, Berzuini C, Zhou C, Oza A, et al. The combination of circulating Ang1 and Tie2 levels predicts progression-free survival advantage in bevacizumab-treated patients with ovarian cancer. Clin Cancer Res (2014) 20(17):4549–58. doi:10.1158/1078-0432.CCR-13-3248
16. Jayson GC, de Haas S, Delmar P, Miles DW, Shah MA, Van Cutsem E, et al. Evaluation of plasma VEGFA as a potential predictive pan-tumour biomarker for bevacizumab. Eur J Cancer (2011) 47(Suppl 1):S96. doi:10.1016/S0959-8049(11)70641-4
17. Collinson F, Hutchinson M, Craven RA, Cairns DA, Zougman A, Wind TC, et al. Predicting response to bevacizumab in ovarian cancer: a panel of potential biomarkers informing treatment selection. Clin Cancer Res (2013) 19(18):5227–39. doi:10.1158/1078-0432.CCR-13-0489
18. Gourley C, McCavigan A, Perren T, Paul J, Michie CO, Churchman M, et al. Molecular subgroup of high-grade serous ovarian cancer (HGSOC) as a predictor of outcome following bevacizumab. J Clin Oncol (2014) 32(5s):abstr 5502.
19. Burger RA, Sill MW, Monk BJ, Greer BE, Sorosky JI. Phase II trial of bevacizumab in persistent or recurrent epithelial ovarian cancer or primary peritoneal cancer: a Gynecologic Oncology Group Study. J Clin Oncol (2007) 25(33):5165–71. doi:10.1200/JCO.2007.11.5345
20. Cannistra SA, Matulonis UA, Penson RT, Hambleton J, Dupont J, Mackey H, et al. Phase II study of bevacizumab in patients with platinum-resistant ovarian cancer or peritoneal serous cancer. J Clin Oncol (2007) 25(33):5180–6. doi:10.1200/JCO.2007.12.0782
21. Ledermann J, Harter P, Gourley C, Friedlander M, Vergote I, Rustin G, et al. Olaparib maintenance therapy in patients with platinum-sensitive relapsed serous ovarian cancer: a preplanned retrospective analysis of outcomes by BRCA status in a randomised phase 2 trial. Lancet Oncol (2014) 15(8):852–61. doi:10.1016/S1470-2045(14)70228-1
22. Ledermann J, Harter P, Gourley C, Friedlander M, Vergote I, Rustin G, et al. Olaparib maintenance therapy in platinum-sensitive relapsed ovarian cancer. N Engl J Med (2012) 366(15):1382–92. doi:10.1056/NEJMoa1105535
23. Ihnen M, zu Eulenburg C, Kolarova T, Qi JW, Manivong K, Chalukya M, et al. Therapeutic potential of the poly(ADP-ribose) polymerase inhibitor rucaparib for the treatment of sporadic human ovarian cancer. Mol Cancer Ther (2013) 12(6):1002–15. doi:10.1158/1535-7163.MCT-12-0813
24. Jones P, Wilcoxen K, Rowley M, Toniatti C. Niraparib: a Poly(ADP-ribose) polymerase (PARP) inhibitor for the treatment of tumors with defective homologous recombination. J Med Chem (2015) 58(8):3302–14. doi:10.1021/jm5018237
25. Coleman RL, Sill M, Aghajanian C, Gray HJ, Tewari KS, Rubin SC, et al. A phase II evaluation of the potent, highly selective PARP inhibitor veliparib in the treatment of persistent or recurrent epithelial ovarian, fallopian tube, or primary peritoneal cancer in patients who carry a germline BRCA1 or BRCA2 mutation – a Gynecologic Oncology Group study. Gynecol Oncol (2014) 133(s1):56. doi:10.1016/j.ygyno.2015.03.042
26. Roche H, Blum J, Eiermann W, Im YH, Martin M, Mina L, et al. P1.01A phase 3 study of the oral PARP inhibitor talazoparib (BMN 673) in BRCA mutation subjects with advanced breast cancer (EMBRACA). Ann Oncol (2015) 26(Suppl 2):ii16. doi:10.1093/annonc/mdv090.1
27. Fong PC, Boss DS, Yap TA, Tutt A, Wu P, Mergui-Roelvink M, et al. Inhibition of poly(ADP-ribose) polymerase in tumors from BRCA mutation carriers. N Engl J Med (2009) 361(2):123–34. doi:10.1056/NEJMoa0900212
28. Fong PC, Yap TA, Boss DS, Carden CP, Mergui-Roelvink M, Gourley C, et al. Poly(ADP)-ribose polymerase inhibition: frequent durable responses in BRCA carrier ovarian cancer correlating with platinum-free interval. J Clin Oncol (2010) 28(15):2512–9. doi:10.1200/JCO.2009.26.9589
29. Audeh MW, Carmichael J, Penson RT, Friedlander M, Powell B, Bell-McGuinn KM, et al. Oral poly(ADP-ribose) polymerase inhibitor olaparib in patients with BRCA1 or BRCA2 mutations and recurrent ovarian cancer: a proof-of-concept trial. Lancet (2010) 376(9737):245–51. doi:10.1016/S0140-6736(10)60893-8
30. Cancer Genome Atlas Research Network. Integrated genomic analyses of ovarian carcinoma. Nature (2011) 474(7353):609–15. doi:10.1038/nature10166
31. Tan DS, Rothermundt C, Thomas K, Bancroft E, Eeles R, Shanley S, et al. “BRCAness” syndrome in ovarian cancer: a case-control study describing the clinical features and outcome of patients with epithelial ovarian cancer associated with BRCA1 and BRCA2 mutations. J Clin Oncol (2008) 26(34):5530–6. doi:10.1200/JCO.2008.16.1703
32. Yang D, Khan S, Sun Y, Hess K, Shmulevich I, Sood AK, et al. Association of BRCA1 and BRCA2 mutations with survival, chemotherapy sensitivity, and gene mutator phenotype in patients with ovarian cancer. JAMA (2011) 306(14):1557–65. doi:10.1001/jama.2011.1456
33. Carser JE, Quinn JE, Michie CO, O’Brien EJ, McCluggage WG, Maxwell P, et al. BRCA1 is both a prognostic and predictive biomarker of response to chemotherapy in sporadic epithelial ovarian cancer. Gynecol Oncol (2011) 123(3):492–8. doi:10.1016/j.ygyno.2011.08.017
34. Hennessy BT, Timms KM, Carey MS, Gutin A, Meyer LA, Flake DD II, et al. Somatic mutations in BRCA1 and BRCA2 could expand the number of patients that benefit from poly (ADP ribose) polymerase inhibitors in ovarian cancer. J Clin Oncol (2010) 28(22):3570–6. doi:10.1200/JCO.2009.27.2997
35. Press JZ, De Luca A, Boyd N, Young S, Troussard A, Ridge Y, et al. Ovarian carcinomas with genetic and epigenetic BRCA1 loss have distinct molecular abnormalities. BMC Cancer (2008) 8:17. doi:10.1186/1471-2407-8-17
36. Bowtell DD. The genesis and evolution of high-grade serous ovarian cancer. Nat Rev Cancer (2010) 10(11):803–8. doi:10.1038/nrc2946
37. Gourley C, Michie CO, Roxburgh P, Yap TA, Harden S, Paul J, et al. Increased incidence of visceral metastases in Scottish patients with BRCA1/2-defective ovarian cancer: an extension of the ovarian BRCAness phenotype. J Clin Oncol (2010) 28(15):2505–11. doi:10.1200/JCO.2009.25.1082
38. Bolton KL, Chenevix-Trench G, Goh C, Sadetzki S, Ramus SJ, Karlan BY, et al. Association between BRCA1 and BRCA2 mutations and survival in women with invasive epithelial ovarian cancer. JAMA (2012) 307(4):382–90. doi:10.1001/jama.2012.20
39. Candido-dos-Reis FJ, Song H, Goode EL, Cunningham JM, Fridley BL, Larson MC, et al. Germline mutation in BRCA1 or BRCA2 and ten-year survival for women diagnosed with epithelial ovarian cancer. Clin Cancer Res (2015) 21(3):652–7. doi:10.1158/1078-0432.CCR-14-2497
40. Zeller C, Dai W, Steele NL, Siddiq A, Walley AJ, Wilhelm-Benartzi CS, et al. Candidate DNA methylation drivers of acquired cisplatin resistance in ovarian cancer identified by methylome and expression profiling. Oncogene (2012) 31(42):4567–76. doi:10.1038/onc.2011.611
41. Sakai W, Swisher EM, Jacquemont C, Chandramohan KV, Couch FJ, Langdon SP, et al. Functional restoration of BRCA2 protein by secondary BRCA2 mutations in BRCA2-mutated ovarian carcinoma. Cancer Res (2009) 69(16):6381–6. doi:10.1158/0008-5472.CAN-09-1178
42. Edwards SL, Brough R, Lord CJ, Natrajan R, Vatcheva R, Levine DA, et al. Resistance to therapy caused by intragenic deletion in BRCA2. Nature (2008) 451(7182):1111–5. doi:10.1038/nature06548
43. Swisher EM, Sakai W, Karlan BY, Wurz K, Urban N, Taniguchi T. Secondary BRCA1 mutations in BRCA1-mutated ovarian carcinomas with platinum resistance. Cancer Res (2008) 68(8):2581–6. doi:10.1158/0008-5472.CAN-08-0088
44. Norquist B, Wurz KA, Pennil CC, Garcia R, Gross J, Sakai W, et al. Secondary somatic mutations restoring BRCA1/2 predict chemotherapy resistance in hereditary ovarian carcinomas. J Clin Oncol (2011) 29(22):3008–15. doi:10.1200/JCO.2010.34.2980
45. Sakai W, Swisher EM, Karlan BY, Agarwal MK, Higgins J, Friedman C, et al. Secondary mutations as a mechanism of cisplatin resistance in BRCA2-mutated cancers. Nature (2008) 451(7182):1116–20. doi:10.1038/nature06633
46. Lheureux S, Ledermann JA, Kaye SB, Gourley C, Friedlander M, Bowtell D, et al. Characterization of ovarian cancer long-term responders on olaparib. J Clin Oncol (2014) 32(5s):abstr 5534.
Keywords: ovarian cancer, olaparib, bevacizumab, heterogeneity, stratification
Citation: Symeonides S and Gourley C (2015) Ovarian cancer molecular stratification and tumor heterogeneity: a necessity and a challenge. Front. Oncol. 5:229. doi: 10.3389/fonc.2015.00229
Received: 14 July 2015; Accepted: 01 October 2015;
Published: 21 October 2015
Edited by:
Euan Alexander Stronach, Imperial College London, UKReviewed by:
Jozien Helleman, Erasmus MC, NetherlandsCopyright: © 2015 Symeonides and Gourley. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) or licensor are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Charlie Gourley, Y2hhcmxpZWdvdXJsZXlAZWQuYWMudWs=
 Stefan Symeonides
Stefan Symeonides Charlie Gourley
Charlie Gourley