- 1Department of Anatomy, New York Institute of Technology, College of Osteopathic Medicine, Old Westbury, NY, United States
- 2Center for Biomedical Innovation, New York Institute of Technology, College of Osteopathic Medicine, Old Westbury, NY, United States
- 3Department of Occupational Therapy, New York Institute of Technology, School of Health Professions, Old Westbury, NY, United States
- 4Department of Biomedical Sciences, New York Institute of Technology, College of Osteopathic Medicine, Old Westbury, NY, United States
- 5Inclusive Sports and Fitness, Holbrook, NY, United States
Introduction: Children and adolescents with Autism Spectrum Disorder face challenges throughout their development. Autism Spectrum Disorder can affect a multitude of areas, including social, cognitive, and physical. Due to delays in development, poor motor coordination, hypersensitivities, and difficulties with motivation and focus, these individuals are uninspired and discouraged to partake in physical activity. This lack of interest can lead to further impairments in health and developing social skills. This study evaluated the effect of virtual reality on exercise, specifically the effects on actual energetic output and perceived energetic output.
Methods: Eleven participants aged 8–19 with Level 1 Autism Spectrum Disorder completed two walking trials on a treadmill. The control trial did not have participants wear a virtual reality headset or interact with any games. The virtual reality trial allowed participants to play an interactive virtual reality game while walking on the treadmill. To measure actual metabolic output, energetic costs were measured by calculating cost of locomotion, cost of transport, and youth metabolic equivalents via open flow respirometry. To measure perceived levels of exertion, participants were asked to rate their exertion level using the Borg Rating of Perceived Exertion scale throughout the duration of the trials.
Results: A statistically significant increase was observed in all energetic measures during the virtual reality walking trials compared to the control trials (all p-values <0.020). Differences in perceived exertion were not statistically significant between the two experimental conditions.
Discussion: These findings suggest that in this patient population, virtual reality can help promote more intense and energetically costly physical activity, while having no effect on perceived exertion levels. These findings may be explained by multiple factors, including virtual reality acting as a distractor, the novelty aspect, or the effects of dual-task cognitive and motor activity.
Introduction
Autism Spectrum Disorder (ASD) is a developmental condition primarily known for its impact on social interaction, communication, and repetitive patterns of communication, interests, and activities (American Psychiatric Association, 2022; Kangarani-Farahani et al., 2023). A less discussed, but prevalent impact of ASD is neuromuscular impairments, leading to difficulties in motor skills, gait, and sensory processing. (Fournier et al., 2010; Abdel Karim and Mohammed, 2015; Kindregan et al., 2015; Dufek et al., 2017; Bennett and Haegele, 2021; Kangarani-Farahani et al., 2023). The range of motor and social impairments, social alienation and marginalization, inaccessible programs and facilities, contributes to diminished engagement, active participation, and physical activity as compared to neurotypical (non-ASD) individuals (Pan, 2008; Bauman, 2010; Bandini et al., 2013; Ma et al., 2024).
Recently, there has been a broader effort to increase modalities and forms of structured exercise in the ASD population (Sowa and Meulenbroek, 2012; Arslan et al., 2022). Physical exercise in the ASD population has been shown to improve two of the major symptom domains in the ASD population: motor and social deficits (Sowa and Meulenbroek, 2012; Ferreira et al., 2019). Additionally, physical exercise has been shown to improve aspects of cognitive function, more specifically executive functioning and working memory (Anderson-Hanley et al., 2011). Overall, physical activity has been shown to be a promising intervention in improving function and promoting overall wellbeing (Peng et al., 2022).
Despite the benefits of exercise in the population, many individuals with ASD do not engage in any voluntary rigorous activity (Finkelstein et al., 2010; Lang et al., 2010). This can be attributed to a variety of difficulties, ranging from motor coordination to difficulties in social interaction (Lang et al., 2010). Children with ASD can experience reduced motivation to partake in physical activity due to increased sensitivity to new and unfamiliar environments, as these children prefer structured and predictable routines (Wong et al., 2024). Pan et al. (2016) posited that children with ASD may be reluctant to participate in physical activities because of their perceived awareness of impaired social skills, motor skill deficits, and athletic incompetence. These challenges hinder their ability to connect with peers and perform activities effectively, leading to reduced enjoyment, diminished initiation, and limited intrinsic motivation to engage in physical activities. Exergaming, utilizing virtual reality (VR), has been shown to motivate neurotypical individuals to participate in exercise more often (Finkelstein et al., 2010). The motivation and intense focus in children engaged in gaming can be attributed to a sense of psychological flow, in which they become fully immersed in an activity that matches their skill level with the right level of challenge (Csikszentmihalyi, 2008). This deep engagement fosters enjoyment, sustained attention, and a desire to persist. Exergaming not only increases motivation but can create favorable differences between perceived and actual energy expenditure, allowing participants to play for longer and at high intensities without the associated perceptions of exhaustion and fatigue (Stewart et al., 2022; Yamamoto et al., 2024).
In the ASD population, exergaming can improve motor skills and has been shown to be a suitable method for therapeutic intervention (Caro et al., 2017). The augmentation of VR during physical activity allows individuals with ASD to achieve higher levels of activity while reporting increased levels of enjoyment (Finkelstein et al., 2010; 2013). VR can help decrease ratings of perceived effort, increasing tolerance for more strenuous exercise (Yamamoto et al., 2024). These benefits, combined with the increased motivation of individuals with ASD to exercise using VR, highlights the effectiveness of VR therapy and exercise in this population. While the therapeutic effect of exergaming has been proven for this population, there have been no comparisons on energetic output and perceived intensity in the ASD patient population. In this study, we intend to compare actual metabolic output and exertion levels, measured by indirect respirometry, to perceived exertion levels in both VR and non-VR environments, to determine the effects of VR on actual and perceived exertion.
Methods
Study design
This was a prospective, repeated-measures, single-site study design to measure the effects of VR on energy expenditure and rating of perceived exertion (RPE) during treadmill walking. All trials were conducted at Inclusive Sports and Fitness (ISF; 5,004 Veterans Memorial Hwy, Holbrook, NY, 11741), an outpatient rehabilitation facility for neurodivergent individuals. The study adhered to ethical guidelines and was approved by the New York Institute of Technology College of Osteopathic Medicine Internal Review Board (Protocol: BHS–1932_2024-21).
Subjects
We recruited eleven individuals who were already participants in structured exercise programs at ISF. All participants have been diagnosed with Level One Autism Spectrum Disorder (American Psychiatric Association, 2022), confirmed by the patient’s own healthcare providers. Level One severity is the least severe diagnosis of ASD, where individuals with this diagnosis need minimal support (American Psychiatric Association, 2022). Individuals with this diagnosis still have deficits in communication and rigid behavioral routines (American Psychiatric Association, 2022). We excluded individuals with strength or mobility pathologies, as well as any preexisting metabolic and cardiorespiratory pathologies. Participants with a past history of severe motion sickness during VR activities were excluded. Additionally, participants who were unable to wear the respirometry mask or the VR headset were excluded.
Energetics protocol
We used the COSMED K5 respirometry system (COSMED, Concord, CA) for all metabolic energetics testing. Before all tests, we instructed participants not to consume any food or drink 2 hours before their scheduled appointment. Prior to treadmill walking, we fitted participants with an appropriate respirometry mask and asked them to sit or lie down (self-selected) in a quiet room for 15–20 minutes to measure resting metabolic rate (RMR). Within the same visit, each subject was required to complete two trials of continuous walking on a Tuff Tread Sports Performance Treadmill (Tuff Tread, Conroe, TX) at a pre-determined velocity (see below), one trial with the VR headset (VR trial) and one trial without (control trial). The trial concluded once the subject reached a steady state of oxygen consumption, which has been shown to occur by 6 minutes of exercise (Chernik et al., 2025). A minimum rest period of 5 minutes was given between each session to ensure the subject returned to baseline metabolic rates. During all trials, participants were monitored by trained occupational therapists. Participants wore a safety harness to mitigate the risk of fall. The treadmill used was wide enough to allow forward, lateral, and backward motion of the arms, without the risk of injury. Figure 1 depicts the experimental setup during VR trials. Throughout the protocol, participants were screened for any balance or sensory disturbances due to the respirometry system or the VR headset.

Figure 1. Experimental setup during VR walking trials. Participants wore a VR headset and K5 respirometry mask. To mitigate risk of injury, each participant wore a safety harness during all walking trials.
The velocity differed between participants as we set the treadmill speed to a constant Froude number (0.515) (Alexander, 1996; Delattre et al., 2009) to control for differences in metabolic costs associated with body mass and speed (Heglund and Taylor, 1988; Lighton, 2008; Halsey and White, 2019). This speed equated to a moderate walking speed (mean velocity 1.52 ± 0.10 m/s). For each participant, the treadmill speed remained constant for both the VR and control trials.
Rate of perceived exertion
Prior to any metabolic testing, participants were educated on the Borg Rating of Perceived Exertion to assess exertion levels accurately. Participants were informed they would be asked to rate their exertion on the Borg Scale (6–20) just prior to the test (minute 0), during the test at minutes 2 and 4, at the end of the test (minute 6). Participants rated their exertion level by interacting with the treadmill screen.
Virtual reality gaming
During the VR trial, participants played the popular VR exergame called Beat Saber (Reality Labs, Menlo Park, CA), an exergame equated energetically to other upper body active video games, such as the Wii (Nintendo, Kyoto, Japan) (Butte et al., 2017; Godfrey et al., 2025). Participants wore a Meta Quest Pro VR (Meta Platforms, Menlo Park, CA) headset, and held a VR controller in each hand. Beat Saber was selected as it did not require participants to walk or laterally shift, mitigating the risk for injury during treadmill walking, and is a popular VR game accessible for purchase to any individual with the Meta Quest VR.
Prior to starting the study, participants were offered an acclimation period for VR exergaming. This acclimation period included wearing the VR headset and then playing Beat Saber while standing still in an open space. Once participants felt comfortable with VR, they were moved to the motionless treadmill belt, where they played the Beat Saber in the safety harness. During the acclimation period and VR walking trial, Beat Saber was configured in the “No Fail” mode, ensuring the game would not stop mid-trial. A difficulty level of easy was selected, as this was the first time participants would be using VR while walking on a treadmill.
Data analysis
We analyzed all energetics data using custom-written MATLAB (MathWorks, Natick, MA) with previously published formulas (Heglund and Taylor, 1988; Schuna et al., 2016). Briefly, using VO2 (L), we determined the timestamps when steady state occurred (i.e., the point at which VO2 consumption per minute plateaued). We averaged the raw metabolic rate (kcal/min) within those timestamps. We converted metabolic rate (MR) into J·s-1 and subtracted RMR from MR to yield the net metabolic rate (MRnet). We calculated the net cost of locomotion (COLnet, in units of J·s-1·kg-1 or W·kg-1) by dividing MRnet by the participant’s mass (kg). To normalize energetic cost by the average speed (m·s-1) at which participants ran, we derived the net cost of transport (COTnet in units of J·kg-1·m-1). To relate energy expenditure to resting metabolic rates, we calculated the youth metabolic equivalent (youth MET) of each trial. To calculate, we averaged the mass-specific VO2 (mL·kg-1·min-1) during steady state exercise and RMR trials. Youth METs (exercise mass-specific VO2 / resting mass-specific VO2) was then calculated (Schuna et al., 2016). Youth METs were used, as this metric has been shown to provide balance in attenuating the age and sex dependence of youth energy expenditure estimates (McMurray et al., 2015; Schuna et al., 2016).
Statistical analyses
We conducted all statistical analyses in R (R Core Team, 2021) using the packages “lmerTest” (Kuznetsova et al., 2017) and “effectsize” (Ben-Shachar et al., 2020). VR and no VR trials were compared using paired t-tests (p = 0.05) for both energetics and perceived exertion metrics. Effect size was calculated for statistically significant differences using Cohen’s d. We follow the standard guidelines on qualitative interpretation of Cohen’s d effect sizes, as follows: small effects = 0.2; medium effects = 0.5; large effects = 0.8.
Results
Descriptive characteristics
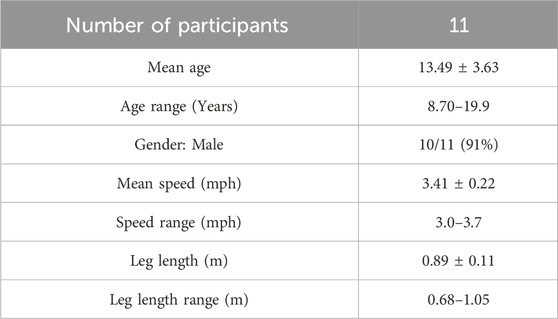
Demographic characteristics are presented in Table 1. All 11 participants were included in data analysis. Ten participants were male, one participant was female. Participant age ranged from 8 to 19 years (13.49 ± 3.63; Table 1). Participants’ activity levels prior to this study were limited, as many did not partake in any organized sports or extracurricular exercise outside of the twice weekly 50-min sessions occurring at ISF. As the participants were recruited from ISF, they all had some previous interactions with VR.
Energetics
Energetically, the use of VR was more costly compared to the non-VR walking trial. The COLnet was 7.82 ± 1.53 J·s-1 kg-1 when playing the VR game. Without the VR game, COLnet was 6.91 ± 1.24 J·s-1·kg-1 (Table 2; Figure 2). This 0.91 J·s-1·kg-1 increase while playing VR was statistically significant (p = 0.014, Cohen’s d = 0.63; 13% more costly with VR; Table 2).
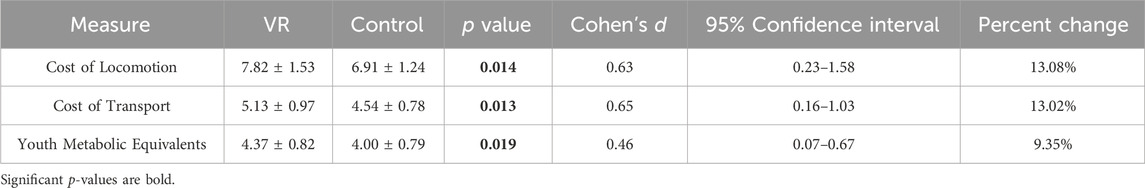
Table 2. Paired t-test analysis analyzing the differences in energy expenditure in the VR and non-VR trials: Cost of locomotion (J·s-1·kg-1), Cost of Transport (J·kg-1·m-1), and Youth Metabolic Equivalents. VR denotes treadmill walking while using the VR headset. Control denotes treadmill walking without using the VR headset. Percent change represents the change in energy expenditure between the control and VR trials, with an increase representing more costly exercise in the VR trials.
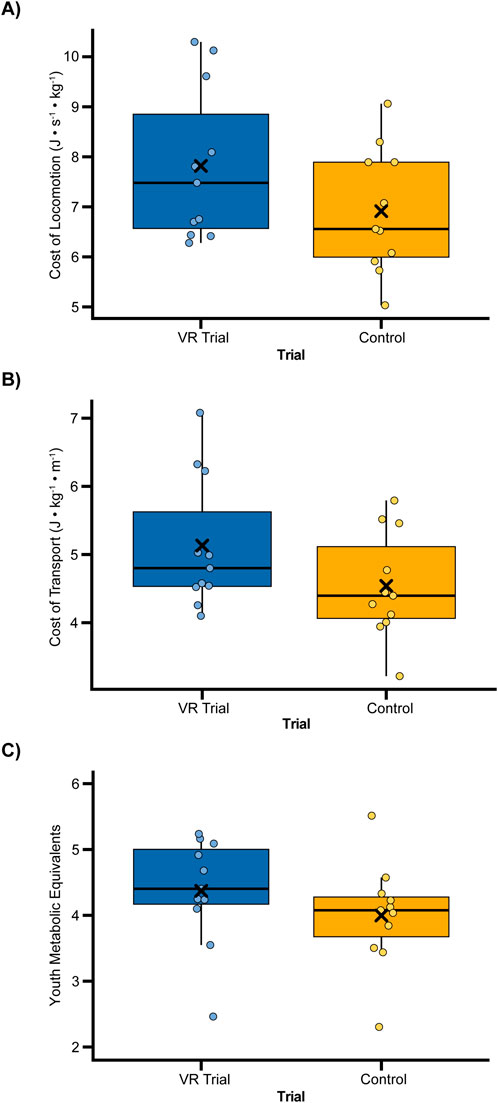
Figure 2. Box plots showing energetic variables: (A) Cost of Locomotion (J·s-1·kg-1), (B) Cost of Transport (J·kg-1·m-1), and (C) Youth Metabolic Equivalents. Each graph depicts the two trial types: VR Trial, where the participant is playing the VR game while walking, and Control, where the participant is not wearing the VR headset while walking. The black “X” denotes the mean.
Accounting for the variation in speed, the COTnet was 5.13 ± 0.97 J·kg-1·m-1 when playing the VR game. Without the VR game, the COTnet was 4.54 ± 0.78 J·kg-1·m-1 (Table 2; Figure 2). This 0.59 J·kg-1·m-1 increase while playing VR was statistically significant (p = 0.013, Cohen’s d = 0.65; 13% more costly with VR; Table 2).
When examining energy in terms of metabolic equivalents, the youth METs were 4.37 ± 0.82 while playing the VR game. Without the VR game, the youth METs were 4.00 ± 0.79 (Table 2; Figure 2). This 0.37 increase while playing VR was statistically significant (p = 0.019, Cohen’s d = 0.46; 9% more costly with VR; Table 2).
Rate of perceived exertion
In the control walking trials, participants began the trial at a rating of “no intensity at all” (Borg RPE = 6.73 ± 1.42; Table 3) and concluded the trial at rating of “light intensity” (Borg RPE = 11.64 ± 4.27; Table 3). Similar ratings were seen in the VR trial; participants began the trial at a rating of “no intensity at all” (Borg RPE = 6.73 ± 1.85; Table 3) and concluded the trial at a rating of “light intensity” (Borg RPE = 11.64 ± 4.18; Table 3) (Williams, 2017). Examining the changes in RPE at 0, 2, 4, and 6 min, no statistically significant differences were seen between the VR trials and the non-VR trials (all p-values >0.768; Table 3; Figure 3).
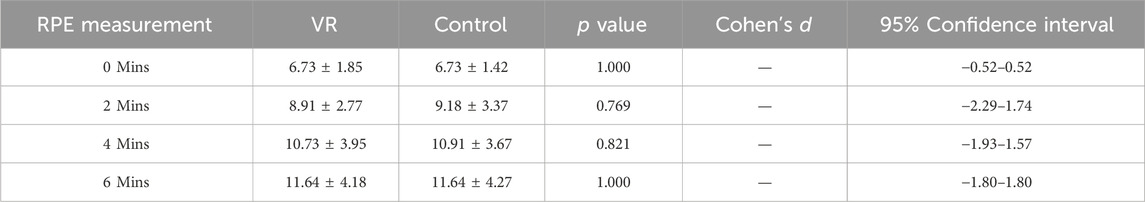
Table 3. Paired t-test analysis analyzing the differences in perceived exertion levels using the Borg Rating of Perceived Exertion Scale (6–20). A higher value represents a greater rating of perceived exertion. VR denotes treadmill walking while using the VR headset. Control denotes treadmill walking without using the VR headset. There is no statistically significant differences in perceived exertion between control and VR settings.
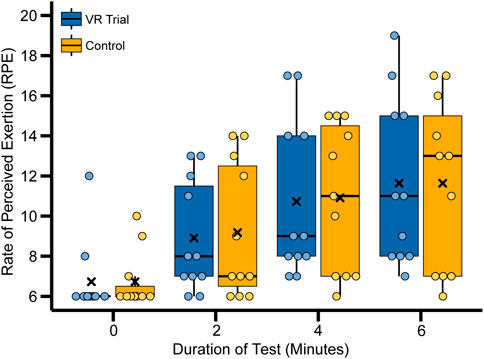
Figure 3. Box plots showing the Rating of Perceived Exertion. Participants were prompted to evaluate their exertion levels at: 0 (before starting trial), 2, 4, and 6 (immediately after trial conclusion). Values are separated by trial type, with VR Trial representing trials where the participant is playing the VR game while walking, and Control representing trials where the participant is not wearing the VR headset while walking. The black “X” denotes the mean.
Discussion
We aimed to explore how virtual reality influences the perception of and motivation to participate in physical activity among children with ASD. The subjects included in this study had a documented history of sedentary behaviors, characterized by minimal engagement in mainstream physical activities and limited participation in organized sports. Their daily routines typically involved prolonged periods of inactivity, preferring passive leisure activities such as screen time or other non-physical hobbies. Additionally, these participants had limited exposure to structured physical environments, further contributing to their reduced physical activity levels and overall fitness. This sedentary lifestyle of individuals with ASD highlights the necessity of investigating innovative interventions, such as virtual reality, to promote increased physical engagement and motivation (Finkelstein et al., 2010).
This study aimed to evaluate how virtual reality influences perceptions of physical activity and compare these perceived levels of physical activity to actual measured energetic consumption. Energy expenditure, measured by cost of locomotion, cost of transport, and youth metabolic equivalents, were all increased during the VR walking trial. This observation aligns with our predictions, as previous studies have examined the effects of playing VR games such as Beat Saber (Godfrey et al., 2025). Using this data, we can calculate the youth METs of Beat Saber around 2.1, which corresponds with other forms of active video games (Butte et al., 2017). While nearly half the energetic cost of walking (youth METs 4.07), the additional exertion of VR increased overall energetic costs during exercise. These findings correspond with previous research examining the use of VR during exercise and the reported increase in energy expenditure during VR exercise (Barbour et al., 2024; Merola et al., 2025). Our findings of energy expenditure during walking correspond with previous values in the literature, especially when comparing youth METs (Schuna et al., 2016).
While energy expenditure increased during the VR trials, we found no statistically significant difference in perceived exertion levels. Participants demonstrated a greater tolerance for increasingly demanding physical activities when immersed in VR, while still reporting similar feelings of exertion compared to performing the same activities without VR. Using VR, participants were able to sustain higher levels of energic output and physical activity, while reporting no changes in perceived effort levels. These findings highlight the potential benefits of VR exergaming to increase the tolerance of exercise intensity. Particularly, our findings support previous studies, which found despite similar or increased levels of energy expenditure and actual exertion during VR exercise, participants did not report any perceived differences in exertion levels (Finkelstein et al., 2013; McDonough et al., 2020; Yamamoto et al., 2024). These results can be explained through VR’s effect on limiting pain and discomfort while increasing motivation (Mesa-Gresa et al., 2018; Matsangidou et al., 2019).
A lower perceived exertion level paired with higher physiologic metabolic costs can help further motivate participants to continue exercising beyond their typical tolerance levels when using immersive VR (Kilpatrick et al., 2020). Virtual environments may effectively enhance physical engagement, advancing cardiorespiratory performance and health and wellness among children with ASD. The subjects exhibited significantly improved tolerance to moderate exercise during the VR game, as indicated by an increased cost of locomotion, transport, and METs in the VR trials. Although the locomotor costs were noticeably higher, subjects reported a lower perceived rate of exertion and showed greater tolerance for the activities, demonstrating the ability to push themselves beyond their usual point of fatigue. This disconnect between RPE and energy exertion may be explained by the VR intervention. Our findings may be explained by a multitude of factors, which may include the effects of VR as a distractor during exercise, dual-task cognitive and motor activity, and the novelty of VR.
Previous studies have shown the effects of VR as a distractor during physical exertion, limiting any perceived increases in physical exertion (Runswick et al., 2024). Virtual reality has also been shown to reduce levels of discomfort and pain (Gromala et al., 2015; Sharar et al., 2016). Instead of focusing on their exertion levels, participants are preoccupied with a new and exciting task in front of them. VR has been shown to promote disassociation and avoidance of body sensation (Baños et al., 2016; Runswick et al., 2024). As discussed above, the energetic costs of Beat Saber are not negligible (2.1 youth METs) (Godfrey et al., 2025), and therefore we would expect some increase in perceived exertion levels. Our findings align with (Runswick et al., 2024), who examined the effects of VR creating incongruent exercise (actual vs. perceived incline while cycling), and demonstrated VR’s ability to manipulate perceived exertion levels. This effect can help prolong exercise duration and increase exercise adherence in populations who are traditionally averse to exercise, such as ASD.
The idea of VR acting as a distractor does conflict with the association between exergaming and dual-task cognitive and motor activity. Virtual reality has been used to encourage dual-task cognitive and motor activity in Parkinson’s patients (Killane et al., 2015) and older individuals (Gallou-Guyot et al., 2020). Previous studies have shown an increase in perceived exertion levels when dual-task exercise and cognitive effort occurs (Condello et al., 2019; Maeneja et al., 2023). In contrast, during the VR trial participants reported non-statistically significant lower or equal levels of exertion through the entire duration of the trial (Table 3). However, it is important to note cognitive effort was not measured in this study, so it is difficult to quantify the level of cognitive difficulty subjects faced during VR trials. This measurement is an area for future research.
Along similar lines, the novelty effect of a “new” stimulus could be contributing to our results. Mestre et al. (2011) demonstrated decreased interaction with virtual reality as participants spent more time with the virtual reality system. While this is a concerning fact, as VR augmented exercise therapy should be a continuous tool, the study above used identical VR environments across trials, limiting any “new” stimulus. Beat Saber, along with many other VR games, can create new and different stimuli between each game, meaning no two games of Beat Saber are identical. VR has been shown to be an effective rehabilitative tool well past the “novelty effect” window (Elor et al., 2022). Future work in this area should include longitudinal studies, where the novelty effect of VR exercise can be better explored.
A possible underlying mechanism for our results, and area for future research, is flow state. Flow state is a mental state marked by intense motivation, deep focus, and engagement during enjoyable and challenging activities (Csikszentmihalyi, 2008). Virtual reality can help modulate effort and attention levels to achieve an appropriate, “just right” distracting challenge for individuals with limited physical capabilities (Tatla et al., 2013). Participants, focused on the VR task at hand, may have a limited perception of effort levels. While this theory is plausible, this study did not include any measurements of flow and is merely speculative. This idea is an area for further research.
Traditional occupational and physical therapy interventions often face challenges in engaging children with ASD in exercise due to the difficulty with sensory-motor control or performance, reliance on verbal instruction and communication disorders, and monotonous repetitive delivery methods that may not align with the child’s sensory preferences or motivation (Ashburner et al., 2014; Bumin et al., 2015; Simonyan and Harutyunyan, 2022). These approaches can feel demanding or unappealing, leading to reduced participation and effort. Wong et al. (2024) found motivation for physical activity in the ASD population is largely influenced by their sensory environment. Traditional interventions can appear overwhelming and overstimulating, limiting the motivation of the participants. In contrast, immersive VR exergaming offers an interactive and visually stimulating environment that naturally captures attention and promotes self-directed engagement (Farrow et al., 2019). By integrating movement with play and allowing individualized pacing, VR exergaming transforms physical activity into a motivating, enjoyable experience that encourages greater engagement and sustained participation among children with ASD (Finkelstein et al., 2010; Rose et al., 2021; Stewart et al., 2022). By modulating the game and tasks given to each individual, VR’s ability to distract users from physical effort while promoting engagement offers a unique opportunity to design more effective and enjoyable therapeutic interventions, especially for the pediatric population. Future studies with larger and more diverse populations can expand on the understanding of how VR-based interventions can be optimized for various therapeutic goals.
Limitations
The experimental design and recruitment for this study faced several challenges. Recruiting participants proved difficult due to the protected nature of this patient population, and recruitment was limited to word-of-mouth and social media. Inclusion criteria, such as verbal consent capability, absence of any strength, mobility, and cardiorespiratory pathology, and tolerance of wearing both a VR headset and a tight fitting respirometry mask further narrowed the pool. Those who are unable to remain calm during resting metabolic rate measurements or exercise with the mask and VR headset were excluded. Additionally, our capacity to test participants was constrained by the necessity of one-to-one observation and coaching. Regarding assessments, this study did not implement any measures of cognitive function or measures of flow state. Future studies should implement established testing protocols to assess the changes in cognitive function during VR and non-VR exercise training. Additionally, examining the accuracy and performance of gameplay during walking and standing is an area of future research.
When considering internal validity, the use of paired t-tests minimizes the influence of between-subject confounding variables. Randomization of trial order, along with sufficient rest between trials, limited the fatigue experienced by participants. However, the novelty of VR, along with the potential increases in stress that using VR can create, even with an acclimation period, must be acknowledged as a potential confounding variable. While all participants had some baseline level of activity, we did not collect or control for varying levels and history of activity. Future studies should address this limitation to better assess how this intervention applies to individuals with different levels of activity. Recruitment of subjects was conducted via convenience sampling, as participants were already enrolled in structured exercise programs at ISF, and almost all had past interactions with VR. As participants were already enrolled in structured exercise, our sample may not reflect the abilities or tolerance of the broader pediatric ASD patient population, who may be naïve to structured exercise and VR exergaming, as our participants had previous exposure to VR. However, the intervention used in this study is intended to help augment therapy and structured exercise, and proper supervision and structure is still necessary.
Conclusion
This study examined the effects of VR augmented exercise in the ASD patient population. We found that using VR during exercise increased energy expenditure while having no effect on perceived exertion levels. These findings highlight the benefits of including VR in exercise and therapy programs for children with ASD. Virtual reality and other exergaming experiences can enhance participation and outcomes by aligning with the everyday experiences and interests of those with ASD. The use of VR in exercise can encourage individuals with ASD to sustain higher levels of exertion at similar levels of perceived exertion, allowing for prolonged physical activity. The use of technology that provides meaningful and pleasurable experiences can lead to greater therapeutic compliance and improve health and wellness among individuals with ASD.
Data availability statement
The original contributions presented in the study are included in the article/Supplementary Material, further inquiries can be directed to the corresponding authors.
Ethics statement
The studies involving humans were approved by New York Institute of Technology College of Osteopathic Medicine Institutional Review Board. The studies were conducted in accordance with the local legislation and institutional requirements. Written informed consent for participation in this study was provided by the participant’s; legal guardians/next of kin.
Author contributions
NC: Data curation, Formal Analysis, Methodology, Project administration, Resources, Software, Supervision, Validation, Visualization, Writing – original draft, Writing – review and editing. SG: Conceptualization, Methodology, Project administration, Supervision, Writing – original draft, Writing – review and editing. RS: Conceptualization, Funding acquisition, Project administration, Resources, Writing – review and editing, Software. AL: Conceptualization, Funding acquisition, Investigation, Methodology, Project administration, Resources, Supervision, Writing – original draft, Writing – review and editing.
Funding
The author(s) declare that financial support was received for the research and/or publication of this article. This study was funded in part by the Center for Biomedical Innovation at New York Institute of Technology and Inclusive Sports and Fitness.
Conflict of interest
The authors declare that AL, who oversaw the safety supervision of participants during data collection, is the founder of ISF. AL did not participate in the analysis of the data.
The remaining authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Generative AI statement
The author(s) declare that no Generative AI was used in the creation of this manuscript.
Any alternative text (alt text) provided alongside figures in this article has been generated by Frontiers with the support of artificial intelligence and reasonable efforts have been made to ensure accuracy, including review by the authors wherever possible. If you identify any issues, please contact us.
Publisher’s note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
Supplementary material
The Supplementary Material for this article can be found online at: https://www.frontiersin.org/articles/10.3389/frvir.2025.1629297/full#supplementary-material
References
Abdel Karim, A. E., and Mohammed, A. H. (2015). Effectiveness of sensory integration program in motor skills in children with autism. Egypt. J. Med. Hum. Genet. 16, 375–380. doi:10.1016/j.ejmhg.2014.12.008
American Psychiatric Association (2022). “Diagnostic and statistical manual of mental disorders: DSM-5-TRTM,” in Text revision. Fifth edition (Washington, DC: American Psychiatric Association Publishing).
Anderson-Hanley, C., Tureck, K., and Schneiderman, R. L. (2011). Autism and exergaming: effects on repetitive behaviors and cognition. Psychol. Res. Behav. Manag. 4, 129–137. doi:10.2147/PRBM.S24016
Arslan, E., Ince, G., and Akyüz, M. (2022). Effects of a 12-week structured circuit exercise program on physical fitness levels of children with autism spectrum condition and typically developing children. Int. J. Dev. Disabil. 68, 500–510. doi:10.1080/20473869.2020.1819943
Ashburner, J., Rodger, S., Ziviani, J., and Jones, J. (2014). Occupational therapy services for people with autism spectrum disorders: current state of play, use of evidence and future learning priorities. Aust. Occup. Ther. J. 61, 110–120. doi:10.1111/1440-1630.12083
Bandini, L. G., Gleason, J., Curtin, C., Lividini, K., Anderson, S. E., Cermak, S. A., et al. (2013). Comparison of physical activity between children with autism spectrum disorders and typically developing children. Autism 17, 44–54. doi:10.1177/1362361312437416
Baños, R. M., Escobar, P., Cebolla, A., Guixeres, J., Alvarez Pitti, J., Lisón, J. F., et al. (2016). Using virtual reality to distract overweight children from bodily sensations during exercise. Cyberpsychology, Behav. Soc. Netw. 19, 115–119. doi:10.1089/cyber.2015.0283
Barbour, B., Sefton, L., Bruce, R. M., Valmaggia, L., and Runswick, O. R. (2024). Acute psychological and physiological benefits of exercising with virtual reality. PLOS ONE 19, e0314331. doi:10.1371/journal.pone.0314331
Bauman, M. L. (2010). Medical comorbidities in autism: challenges to diagnosis and treatment. Neurotherapeutics 7, 320–327. doi:10.1016/j.nurt.2010.06.001
Ben-Shachar, M. S., Lüdecke, D., and Makowski, D. (2020). Effectsize: estimation of effect size indices and standardized parameters. J. Open Source Softw. 5, 2815. doi:10.21105/joss.02815
Bennett, H. J., and Haegele, J. A. (2021). Running biomechanics of adolescents with autism spectrum disorder. J. Biomechanical Eng. 143, 111005. doi:10.1115/1.4051346
Bumin, G., Huri, M., Salar, S., Kayihan, H., Bumin, G., Huri, M., et al. (2015). “Occupational therapy in autism,” in Autism spectrum disorder - recent advances. (IntechOpen). doi:10.5772/59168
Butte, N. F., Watson, K. B., Ridley, K., Zakeri, I. F., McMurray, R. G., Pfeiffer, K. A., et al. (2017). A youth compendium of physical activities: activity codes and metabolic intensities. Med. Sci. sports Exerc. 50, 246–256. doi:10.1249/mss.0000000000001430
Caro, K., Tentori, M., Martinez-Garcia, A. I., and Zavala-Ibarra, I. (2017). FroggyBobby: an exergame to support children with motor problems practicing motor coordination exercises during therapeutic interventions. Comput. Hum. Behav. 71, 479–498. doi:10.1016/j.chb.2015.05.055
Chernik, N. D., Young, M. W., Jacobson, R. N., Kantounis, S. J., Lynch, S. K., Virga, J. Q., et al. (2025). Pilot study: effects of high-intensity training on gait symmetry and locomotor performance in neurodivergent children. Symmetry 17, 1073. doi:10.3390/sym17071073
Condello, G., Forte, R., Monteagudo, P., Ghinassi, B., Di Baldassarre, A., Capranica, L., et al. (2019). Autonomic stress response and perceived effort jointly inform on dual tasking in aging. Brain Sci. 9, 290. doi:10.3390/brainsci9110290
Csikszentmihalyi, M. (2008). Flow: the psychology of optimal experience, 1. New York, NY London Toronto Sydney New Delhi Auckland: Harper Perennial Modern Classics edition. HarperPerennial.
Delattre, N., Lafortune, M. A., and Moretto, P. (2009). Dynamic similarity during human running: about froude and Strouhal dimensionless numbers. J. Biomechanics 42, 312–318. doi:10.1016/j.jbiomech.2008.11.010
Dufek, J. S., Eggleston, J. D., Harry, J. R., and Hickman, R. A. (2017). A comparative evaluation of gait between children with autism and typically developing matched controls. Med. Sci. 5, 1. doi:10.3390/medsci5010001
Elor, A., Powell, M., Mahmoodi, E., Teodorescu, M., and Kurniawan, S. (2022). Gaming beyond the novelty effect of immersive virtual reality for physical rehabilitation. IEEE Trans. Games 14, 107–115. doi:10.1109/TG.2021.3069445
Farrow, M., Lutteroth, C., Rouse, P. C., and Bilzon, J. L. J. (2019). Virtual-reality exergaming improves performance during high-intensity interval training. Eur. J. Sport Sci. 19, 719–727. doi:10.1080/17461391.2018.1542459
Ferreira, J. P., Ghiarone, T., Cabral Júnior, C. R., Furtado, G. E., Moreira Carvalho, H., Machado-Rodrigues, A. M., et al. (2019). Effects of physical exercise on the stereotyped behavior of children with autism spectrum disorders. Medicina 55, 685. doi:10.3390/medicina55100685
Finkelstein, S., Nickel, A., Barnes, T., and Suma, E. A. (2010). “Astrojumper: motivating children with autism to exercise using a VR game,” in CHI ’10 extended abstracts on human factors in computing systems (Atlanta Georgia USA), 4189–4194. doi:10.1145/1753846.1754124ACM
Finkelstein, S., Barnes, T., Wartell, Z., and Suma, E. A. (2013). “Evaluation of the exertion and motivation factors of a virtual reality exercise game for children with autism,” in 2013 1st workshop on virtual and augmented assistive technology (VAAT) (USA: Lake Buena Vista, FL), 11–16. doi:10.1109/VAAT.2013.6786186
Fournier, K. A., Hass, C. J., Naik, S. K., Lodha, N., and Cauraugh, J. H. (2010). Motor coordination in autism spectrum disorders: a synthesis and meta-analysis. J. Autism Dev. Disord. 40, 1227–1240. doi:10.1007/s10803-010-0981-3
Gallou-Guyot, M., Mandigout, S., Bherer, L., and Perrochon, A. (2020). Effects of exergames and cognitive-motor dual-task training on cognitive, physical and dual-task functions in cognitively healthy older adults: an overview. Ageing Res. Rev. 63, 101135. doi:10.1016/j.arr.2020.101135
Godfrey, C. A., Oody, J. F., Conger, S. A., and Steeves, J. A. (2025). Active virtual reality games: comparing energy expenditure, game experience, and cybersickness to traditional gaming and exercise in youth aged 8–12. Games Health J. 14, 42–48. doi:10.1089/g4h.2024.0034
Gromala, D., Tong, X., Choo, A., Karamnejad, M., and Shaw, C. D. (2015). “The virtual meditative walk: virtual reality therapy for chronic pain management,” in Proceedings of the 33rd annual ACM conference on human factors in computing systems (New York, NY, USA: Association for Computing Machinery), 521–524. doi:10.1145/2702123.2702344
Halsey, L. G., and White, C. R. (2019). Terrestrial locomotion energy costs vary considerably between species: no evidence that this is explained by rate of leg force production or ecology. Sci. Rep. 9, 656–13. doi:10.1038/s41598-018-36565-z
Heglund, N. C., and Taylor, C. R. (1988). Speed, stride frequency and energy cost per stride: how do they change with body size and gait? J. Exp. Biol. 138, 301–318. doi:10.1242/jeb.138.1.301
Kangarani-Farahani, M., Malik, M. A., and Zwicker, J. G. (2023). Motor impairments in children with autism spectrum disorder: a systematic review and meta-analysis. J. Autism Dev. Disord. 54, 1977–1997. doi:10.1007/s10803-023-05948-1
Killane, I., Fearon, C., Newman, L., McDonnell, C., Waechter, S. M., Sons, K., et al. (2015). Dual motor-cognitive virtual reality training impacts dual-task performance in freezing of gait. IEEE J. Biomed. Health Inf. 19, 1855–1861. doi:10.1109/JBHI.2015.2479625
Kilpatrick, M., Newsome, A., Foster, C., Robertson, R., and Green, M. (2020). Scientific rationale for RPE use in fitness assessment and exercise participation. ACSM’s Health & Fit. J. 24, 24–30. doi:10.1249/FIT.0000000000000587
Kindregan, D., Gallagher, L., and Gormley, J. (2015). Gait deviations in children with autism spectrum disorders: a review. Autism Res. Treat. 2015, 1–8. doi:10.1155/2015/741480
Kuznetsova, A., Brockhoff, P. B., and Christensen, R. H. B. (2017). lmerTest package: tests in linear mixed effects models. J. Stat. Softw. 82, 1–26. doi:10.18637/jss.v082.i13
Lang, R., Koegel, L. K., Ashbaugh, K., Regester, A., Ence, W., and Smith, W. (2010). Physical exercise and individuals with autism spectrum disorders: a systematic review. Res. Autism Spectr. Disord. 4, 565–576. doi:10.1016/j.rasd.2010.01.006
Ma, Y., Liu, M., Liu, Y., Liu, D., and Hou, M. (2024). Exploring physical activity in children and adolescents with disabilities: a bibliometric review of current status, guidelines, perceived barriers, and facilitators and future directions. Healthc. (Basel) 12, 934. doi:10.3390/healthcare12090934
Maeneja, R., Silva, C. R., Ferreira, I. S., and Abreu, A. M. (2023). Aerobic physical exercise versus dual-task cognitive walking in cognitive rehabilitation of people with stroke: a randomized clinical trial. Front. Psychol. 14, 1258262. doi:10.3389/fpsyg.2023.1258262
Matsangidou, M., Ang, C. S., Mauger, A. R., Intarasirisawat, J., Otkhmezuri, B., and Avraamides, M. N. (2019). Is your virtual self as sensational as your real? Virtual reality: the effect of body consciousness on the experience of exercise sensations. Psychol. Sport Exerc. 41, 218–224. doi:10.1016/j.psychsport.2018.07.004
McDonough, D. J., Pope, Z. C., Zeng, N., Liu, W., and Gao, Z. (2020). Comparison of college students’ blood pressure, perceived exertion, and psychosocial outcomes during virtual reality, exergaming, and traditional exercise: an exploratory study. Games Health J. 9, 290–296. doi:10.1089/g4h.2019.0196
McMurray, R. G., Butte, N. F., Crouter, S. E., Trost, S. G., Pfeiffer, K. A., Bassett, D. R., et al. (2015). Exploring metrics to express energy expenditure of physical activity in youth. PLOS ONE 10, e0130869. doi:10.1371/journal.pone.0130869
Merola, P., Cardoso, M. B., Barreto, G., Chagas, M. C., Saunders, L. F. O., Saunders, B., et al. (2025). Virtual reality high-intensity interval training exergaming compared to traditional high-intensity circuit training among medical students: pilot crossover study. JMIR Serious Games 13, e63461. doi:10.2196/63461
Mesa-Gresa, P., Gil-Gómez, H., Lozano-Quilis, J.-A., and Gil-Gómez, J.-A. (2018). Effectiveness of virtual reality for children and adolescents with autism spectrum disorder: an evidence-based systematic review. Sensors 18, 2486. doi:10.3390/s18082486
Mestre, D. R., Dagonneau, V., and Mercier, C.-S. (2011). Does virtual reality enhance exercise performance, enjoyment, and dissociation? An exploratory study on a stationary bike apparatus. Presence Teleoperators Virtual Environ. 20, 1–14. doi:10.1162/pres_a_00031
Pan, C.-Y. (2008). Objectively measured physical activity between children with autism spectrum disorders and children without disabilities during inclusive recess settings in Taiwan. J. Autism Dev. Disord. 38, 1292–1301. doi:10.1007/s10803-007-0518-6
Pan, C.-Y., Tsai, C.-L., Chu, C.-H., Sung, M.-C., Ma, W.-Y., and Huang, C.-Y. (2016). Objectively measured physical activity and health-related physical fitness in secondary school-aged Male students with autism spectrum disorders. Phys. Ther. 96, 511–520. doi:10.2522/ptj.20140353
Peng, S., Fang, Y., Othman, A. T., and Liang, J. (2022). Meta-analysis and systematic review of physical activity on neurodevelopment disorders, depression, and obesity among children and adolescents. Front. Psychol. 13, 940977. doi:10.3389/fpsyg.2022.940977
R Core Team (2021). R: a language and environment for statistical computing. Vienna, Austria: R Foundation for Statistical Computing. Available online at: https://www.R-project.org/.
Rose, V., Stewart, I., Jenkins, K. G., Tabbaa, L., Ang, C. S., and Matsangidou, M. (2021). Bringing the outside in: the feasibility of virtual reality with people with dementia in an inpatient psychiatric care setting. Dement. Lond. 20, 106–129. doi:10.1177/1471301219868036
Runswick, O. R., Siegel, L., Rafferty, G. F., Knudsen, H. S., Sefton, L., Taylor, S., et al. (2024). The effects of congruent and incongruent immersive virtual reality modulated exercise environments in healthy individuals: a pilot study. Int. J. Human–Computer Interact. 40, 7864–7874. doi:10.1080/10447318.2023.2276524
Schuna, J. M., Barreria, T. V., Hsia, D. S., Johnson, W. D., and Tudor-Locke, C. (2016). Youth energy expenditure during common free-living activities and treadmill walking. J. Phys. Act. Health 13, S29–S34. doi:10.1123/jpah.2015-0728
Sharar, S. R., Alamdari, A., Hoffer, C., Hoffman, H. G., Jensen, M. P., and Patterson, D. R. (2016). Circumplex model of affect: a measure of pleasure and arousal during virtual reality distraction analgesia. Games Health J. 5, 197–202. doi:10.1089/g4h.2015.0046
Simonyan, T., and Harutyunyan, Z. (2022). The challenges of occupational therapy intervention in supporting adolescents with autism to accomplish self-care activities. AJSE 6, 69–83. doi:10.24234/se.v6i2.300
Sowa, M., and Meulenbroek, R. (2012). Effects of physical exercise on autism spectrum disorders: a meta-analysis. Res. Autism Spectr. Disord. 6, 46–57. doi:10.1016/j.rasd.2011.09.001
Stewart, T. H., Villaneuva, K., Hahn, A., Ortiz-Delatorre, J., Wolf, C., Nguyen, R., et al. (2022). Actual vs. perceived exertion during active virtual reality game exercise. Front. Rehabil. Sci. 3, 887740. doi:10.3389/fresc.2022.887740
Tatla, S. K., Sauve, K., Virji-Babul, N., Holsti, L., Butler, C., and Van Der Loos, H. F. M. (2013). Evidence for outcomes of motivational rehabilitation interventions for children and adolescents with cerebral palsy: an American academy for cerebral palsy and developmental medicine systematic review. Dev. Med. & Child Neurology 55, 593–601. doi:10.1111/dmcn.12147
Williams, N. (2017). The borg rating of perceived exertion (RPE) scale. Occup. Med. 67, 404–405. doi:10.1093/occmed/kqx063
Wong, M. L., Girdler, S., Afsharnejad, B., Ntoumanis, N., Milbourn, B., Kebble, P., et al. (2024). Motivation to participate in structured physical activity for autistic youth: a systematic scoping review. Autism 28, 2430–2444. doi:10.1177/13623613241240603
Keywords: virtual reality, Autism Spectrum Disorder, energetics, exergaming, occupational therapy
Citation: Chernik ND, Gonzalez S, Stout R and Lopez A (2025) Energy expenditure during virtual reality exergaming in adolescents with Autism Spectrum Disorder. Front. Virtual Real. 6:1629297. doi: 10.3389/frvir.2025.1629297
Received: 15 May 2025; Accepted: 14 October 2025;
Published: 19 November 2025.
Edited by:
Derek Ham, Carnegie Mellon University, United StatesReviewed by:
Arnav Jhala, North Carolina State University, United StatesSarah Anderson, The Ohio State University, United States
Copyright © 2025 Chernik, Gonzalez, Stout and Lopez. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: N. D. Chernik, bmNoZXJuaWtAbnlpdC5lZHU=; A. Lopez, YWxvcGV6QG55aXQuZWR1
 N. D. Chernik
N. D. Chernik S. Gonzalez3
S. Gonzalez3 R. Stout
R. Stout A. Lopez
A. Lopez