- 1Department of Burn and Plastic Surgery, Children’s Hospital of Nanjing Medical University, Nanjing, China
- 2The First Clinical Medicine College, Nanjing Medical University, Nanjing, China
- 3Department of Biomedical Engineering, College of Medicine, Tianjin University, Tianjin, China
- 4Department of Cardiology, The First Affiliated Hospital of Nanjing Medical University, Nanjing, China
- 5Department of Anatomy, Histology, and Embryology, Nanjing Medical University, Nanjing, China
- 6Nanjing Pukou Central Hospital, Pukou Branch Hospital of Jiangsu Province Hospital, Nanjing, China
Background: Nutritionally unhealthy obesity is a newly introduced phenotype characterized by a combined condition of malnutrition and obesity. This study aims to explore the combined influence of obesity and nutritional status on the prevalence and outcome of hypertension.
Methods: Participants collected from the National Health and Nutrition Examination Survey (NHANES) database were divided into four subgroups according to their obesity and nutritional conditions, as defined by waist circumference and serum albumin concentration. The lean-well-nourished was set as the reference group. Logistic regression models were applied to evaluate the hypertension risk. Kaplan–Meier analysis and Cox proportional hazard regression models were used to assess the survival curve and outcome risk of participants with hypertension.
Results: A total of 28,554 participants with 10,625 hypertension patients were included in the analysis. The lean-malnourished group showed a lower hypertension risk (odds ratio [OR] 0.85, 95% confidence interval [CI]: 0.77–0.94), while the obese-well-nourished condition elevated the risk (OR 1.47, 95% CI: 1.3–1.67). Two malnourished groups had higher mortality risks (HR 1.42, 95% CI: 1.12–1.80 and HR 1.31, 95% CI: 1.03–1.69 for the lean and obese, respectively) than the reference group. The outcome risk of the obese-well-nourished group (HR 1.02, 95% CI: 0.76–1.36) was similar to the lean-well-nourished.
Conclusion: Malnutrition was associated with a lower risk of developing hypertension in both lean and obese participants, but it was associated with a worse outcome once the hypertension is present. The lean-malnourished hypertension patients had the highest all-cause mortality risk followed by the obese-malnourished. The obese-well-nourished hypertension patients showed a similar mortality risk to the lean-well-nourished hypertension patients.
1. Introduction
Arterial hypertension is a leading risk factor for multiple cardiovascular diseases (CVDs) and renal disability (1). About 10 million deaths globally can be attributed to hypertension each year (2, 3). Despite the relatively stable global average blood pressure in these decades, the prevalence of hypertension is continuously increasing in various low- and middle-income regions (1, 4).
Due to the unhealthy diet and behavior patterns, obesity, a condition strongly associated with type 2 diabetes and CVDs, has become a growing worldwide health problem (5). However, obesity is a phenomenon of high heterogeneity and can occur under a broad spectrum of metabolic situations (6). Interestingly, malnutrition and obesity can be observed simultaneously in individuals as part of the so-called “double burden of malnutrition” (7, 8). This hybrid condition of malnutrition and obesity is recognized to be highly implicated with the inflammatory state and the risk of non-communicable diseases (7).
Recently, an intriguing research on heart failure patients revealed that the obese-malnourished participants had significantly higher comorbidity burden and less favorable cardiac outcomes compared with other nutrition and obesity statuses (9). This result led to our speculation about the potential influence of this phenotype on hypertension. Although obesity has long been identified as an important risk factor for hypertension (10), the relationship between nutrition status and blood pressure remains vague (11, 12). To our knowledge, no previous research has investigated the combined effect of nutrition and obesity status on hypertension. In this study, we aim to explore the association of nutrition status defined by serum albumin (SA) levels and abdominal obesity with the prevalence and outcomes of clinical hypertension.
2. Methods
2.1. Data source and study population
The National Health and Nutrition Examination Survey (NHANES) is a multistage health survey based on interviews and physical/laboratory examinations of the civilian US population. The National Death Index (NDI) is a centralized death record information database collecting the follow-up information from the date of medical examination to either death or censoring (December 31, 2015). This study was based on the publicly available data of 7 consecutive NHANES cycles (2001–2002, 2003–2004, 2005–2006, 2007–2008, 2009–2010, 2011–2012, 2013–2014) and the NDI database. The demographic data, body measurements, blood pressure, CVD, smoking/drinking status, medical conditions, standard biochemistry profiles, income, and education levels of participants were extracted. The race of participants was categorized as non-Hispanic white, non-Hispanic black, Mexican American, other Hispanic, and Other. The exclusion criteria were as follows: (1) participants aged <18 or > 80 years, (2) without body mass index (BMI) or waist circumference records, (3) without blood pressure records, (4) pregnant individuals, (5) diagnosed with cancer, (6) deceased within 3 months. After selecting patients with hypertension, 10,625 participants were finally enrolled. National Center for Health Statistics Research Ethics Review Board approved the analysis, and informed consent was acquired from all individuals.
2.2. Study definitions
Abdominal obesity was defined by waist circumference, with a cut-off value of 102/88 cm for males and females, respectively, as proposed by the National Cholesterol Education Program-Adult Treatment Panel III (NCEP-ATP III) (13). Nutrition status was defined by the serum albumin concentration as in the previous study (9). Participants with SA < 45 g/L or ≥ 45 g/L were recognized as malnourished or well-nourished.
Each participant’s blood pressure was measured following the American Heart Association standardized protocol three times after resting 5 minutes in a seated position. Hypertension was defined as previously described (14, 15): (1) average systolic blood pressure ≥ 130 mmHg or diastolic blood pressure ≥ 80 mmHg, (2) self-reported hypertension, or (3) self-reported administration of anti-hypertensive medications.
The income levels of participants were evaluated by family income-to-poverty ratios (PIRs), which was calculated as the ratio of family income to the federal poverty level. PIR was categorized as <1.33, 1.33–<3.50, and ≥ 3.50, following the qualification criterion for the US federal Supplemental Nutrition Assistance Program (16).
2.3. Covariates
Multiple covariates related to hypertension were assessed in this study to minimize bias. To be specific, age, sex, body mass index (BMI), race (non-Hispanic white, non-Hispanic Black, Mexican American, other Hispanic, and other races), diabetes, taking prescriptions for hypertension, smoking, alcohol drinking, and education level of the participants were collected from the NHANES and were adjusted in the statistical analysis.
2.4. Statistical analysis
The statistical reporting recommendations by the American Heart Association were followed in the study (17). Participants were categorized into four groups according to their waist circumference and nutrition status. The group with low waist circumference and fine nutrition status was selected as the reference group (the lean-well-nourished group). Kolmogorov–Smirnov test was used to assess the normality. Continuous variables with normal distribution were provided as mean ± standard deviation, while skewed distributed variables were provided as median with interquartile range. Categorical variables were reported as percentages. ANOVA test, Kruskal-Wallis test, and chi-square test were adapted for comparing the baseline characteristics of continuous variables with normal and skewed distribution, and categorical variables, as appropriate.
Logistic regression models were applied to evaluate the association of obesity and malnutrition with the prevalence of hypertension, and Cox proportional hazard regression models were used to assess the association of obesity and malnutrition with all-cause death in participants with hypertension. Odds ratios (ORs) and hazard ratios (HRs) with 95% confidence intervals (CIs) were calculated in the logistic and Cox regression analyses, respectively. In either logistic or Cox regression analysis, unadjusted analysis was performed at first. Then two different adjusted models were performed to minimize the bias caused by covariates. Model 1 was adjusted for age, sex, race, diabetes, having CVDs, taking prescriptions for hypertension, smoking/drinking status, and education level. Model 2 was adjusted for model 1 covariates plus BMI. An additional age-stratified analysis for the young (below 45 years old) and the elder (above 45 years old) were then conducted with the same method.
Moreover, we further assessed the association between obesity and nutrition status with the prognosis of hypertension by Kaplan–Meier survival analysis. Pairwise comparisons of the survival rates in different groups were performed by the log-rank test. A two-tail value of p < 0.05 was considered statically significant. All statistical analyses were performed using the R software (version 3.6.1; R Foundation for Statistical Computing, Vienna). An additional age-stratified analysis for the young (below 45 years old) and the elder (above 45 years old) were then conducted with the same method.
3. Results
3.1. Baseline characteristics
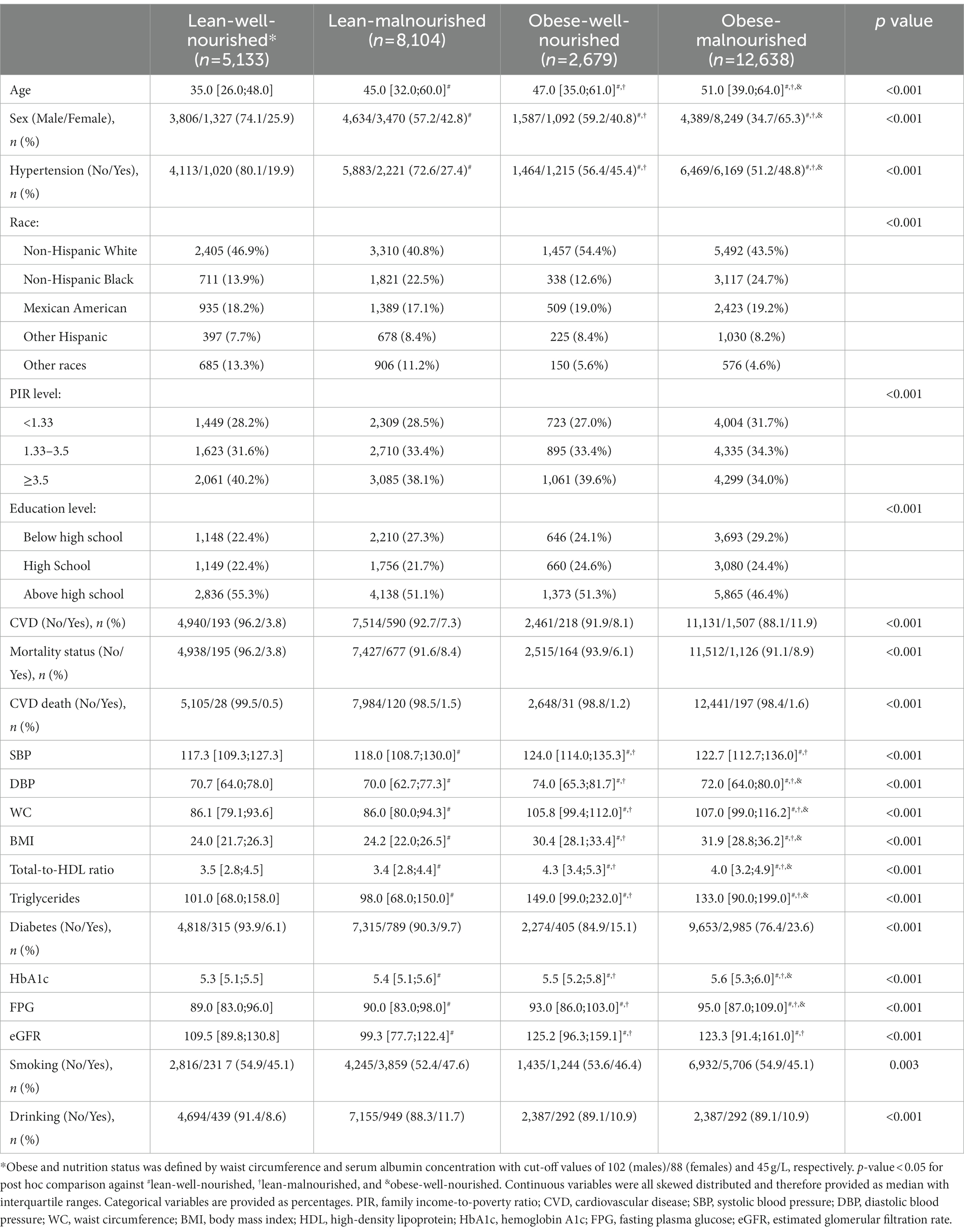
The demographics, cardiovascular health status, cardiovascular risk factors, and behavioral factors of the participants were provided in Table 1. A total of 28,554 participants were included in the study, including 10,625 (37.2%) participants diagnosed with hypertension. During a median follow-up of 6.8 years, 2,162 (7.6%) deaths were observed, including 376 (17.3%) CVD deaths.
Among four groups classified by abdominal obesity and nutrition status, the obese-malnourished group had the most participants (12,638, 44.3%), much higher than the obese-well-nourished group (2,679). The obese-malnourished group was generally the oldest (median 51 years) and had the highest BMI (median 31.9), drinking percentage (16.2%), and crude prevalence of diabetes (23.6%). The obese-malnourished group also presented the highest crude prevalence of hypertension (48.8%). The obese-malnourished group had the largest absolute number (8,249) and proportion (65.3%) of females. Being the opposite of the obese-malnourished, the lean-well-nourished group presented the youngest age (median 35 years), lowest alcohol drinking proportion (8.6%), and lowest crude prevalence of diabetes (6.1%) and hypertension (19.9%).
3.2. The association of obesity and malnutrition with the prevalence of hypertension
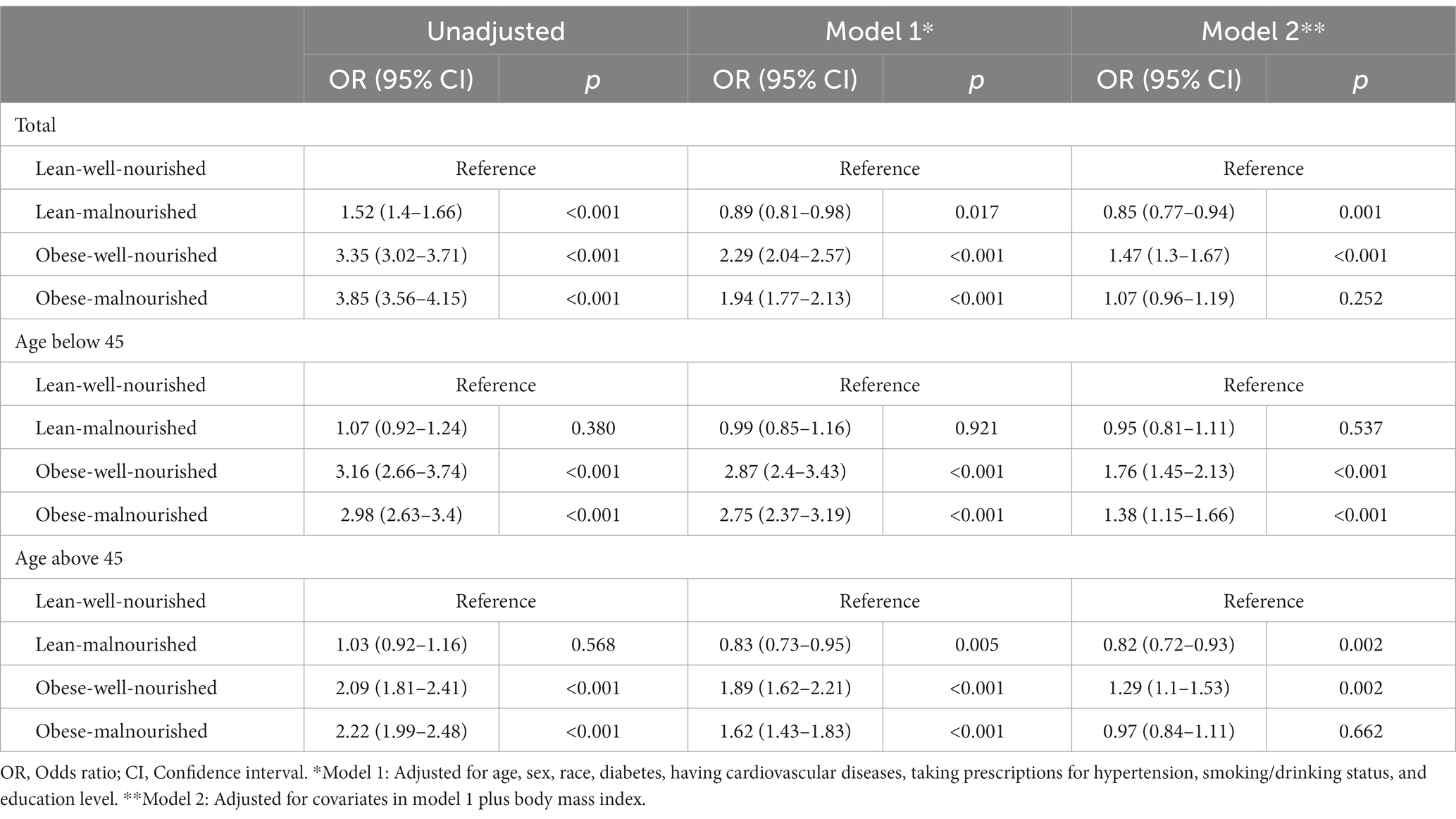
Table 2 shows the results of the logistic regression models assessing the association of obesity and malnutrition with the prevalence of hypertension. In the multivariable-adjusted model 1, compared with the lean-well-nourished group, both two obese groups showed a significantly higher risk of hypertension, with ORs of 2.29 (95% CI: 2.04–2.57) and 1.94 (95% CI, 1.77–2.13) respectively for the well−/malnourished. Interestingly, the old lean-malnourished group had a significantly lower risk for hypertension (OR 0.83, 95% CI: 0.73–0.95) compared with the reference group, but the significance was not observed in the younger participants.
In model 2, which adjusted covariates in model 1 plus BMI, a significant elevation of hypertension risk was still observed in the obese-well-nourished group (OR 1.47, 95% CI: 1.3–1.67). The older lean-malnourished group still showed a lower risk (OR 0.82, 95% CI: 0.72–0.93) comparing with participants with normal waist circumference and nutrition status. However, the significant rise in hypertension risk in the obese-malnourished group was only observed in younger participants (OR 1.38, 95% CI: 1.15–1.66) in model 2.
3.3. The association of obesity and malnutrition with the outcome of hypertension patients
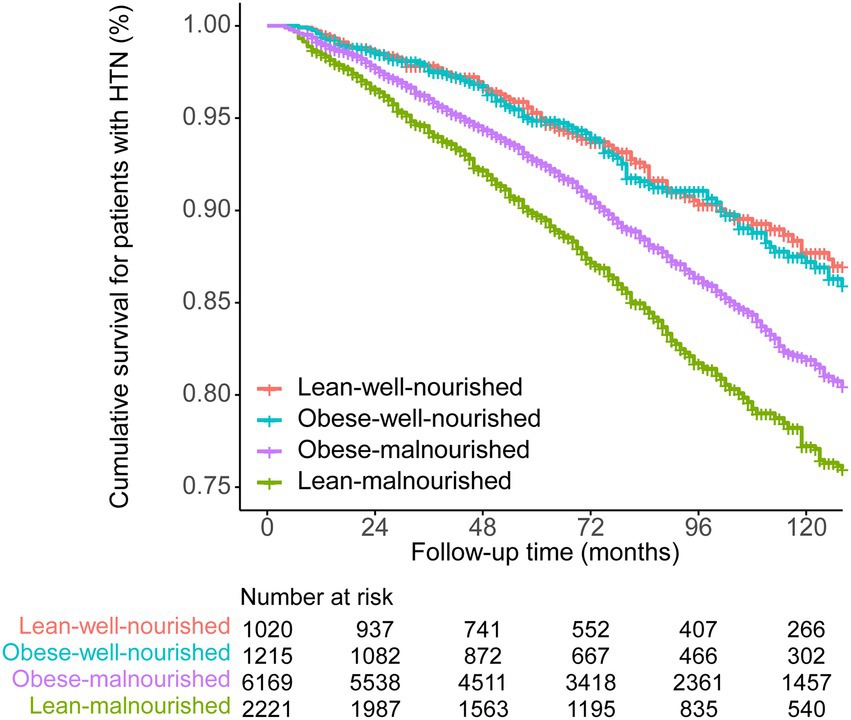
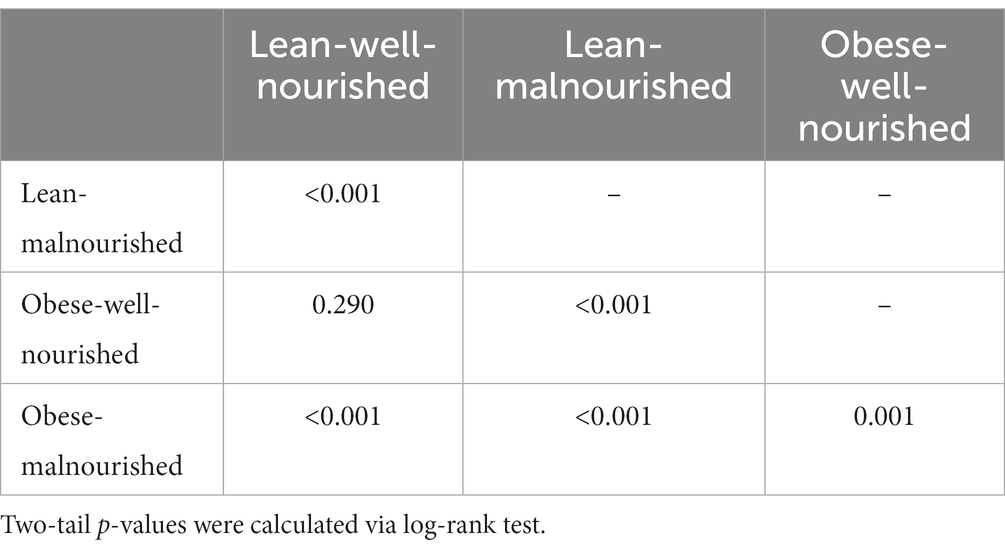
Among 10,625 participants with hypertension, 1,370 (12.9%) deaths were observed during the follow-up. Figure 1 and Table 3 show the results of the Kaplan–Meier analysis for evaluating the association of obesity and malnutrition with the risk of all-cause death in hypertension patients. Compared with the lean-well-nourished group, both malnourished groups showed significantly elevated death risk. Interestingly, the difference between the two malnourished groups is also statistically significant, with the lean-malnourished having a higher mortality risk. However, no significant difference was observed between the lean-well-nourished and the obese-well-nourished groups.
We then examined the survival of hypertension participants in each group by multi-adjusted Cox models to eliminate the bias caused by cardiovascular covariates (Table 4). In model 1, compared with the lean-well-nourished, only the elevation of mortality risk in the lean-malnourished group reached significance (HR 1.42, 95% CI: 1.12–1.79). After further adjustment of BMI in model 2, the unstratified analysis found a significantly higher risk in the lean-malnourished group (HR 1.42, 95% CI: 1.12–1.80) and obese-malnourished group (HR 1.31, 95% CI: 1.03–1.69). In the age-stratified model 2, the lean-malnourished group had higher outcome risks (HR 2.61, 95% CI 1.10–6.18 and HR 1.36, 95% CI 1.06–1.74 for the young and the elder, respectively), and the risk elevation of the obese-malnourished group also nearly reached statistical significance (HR 1.29, 95% CI 1.00–1.67).
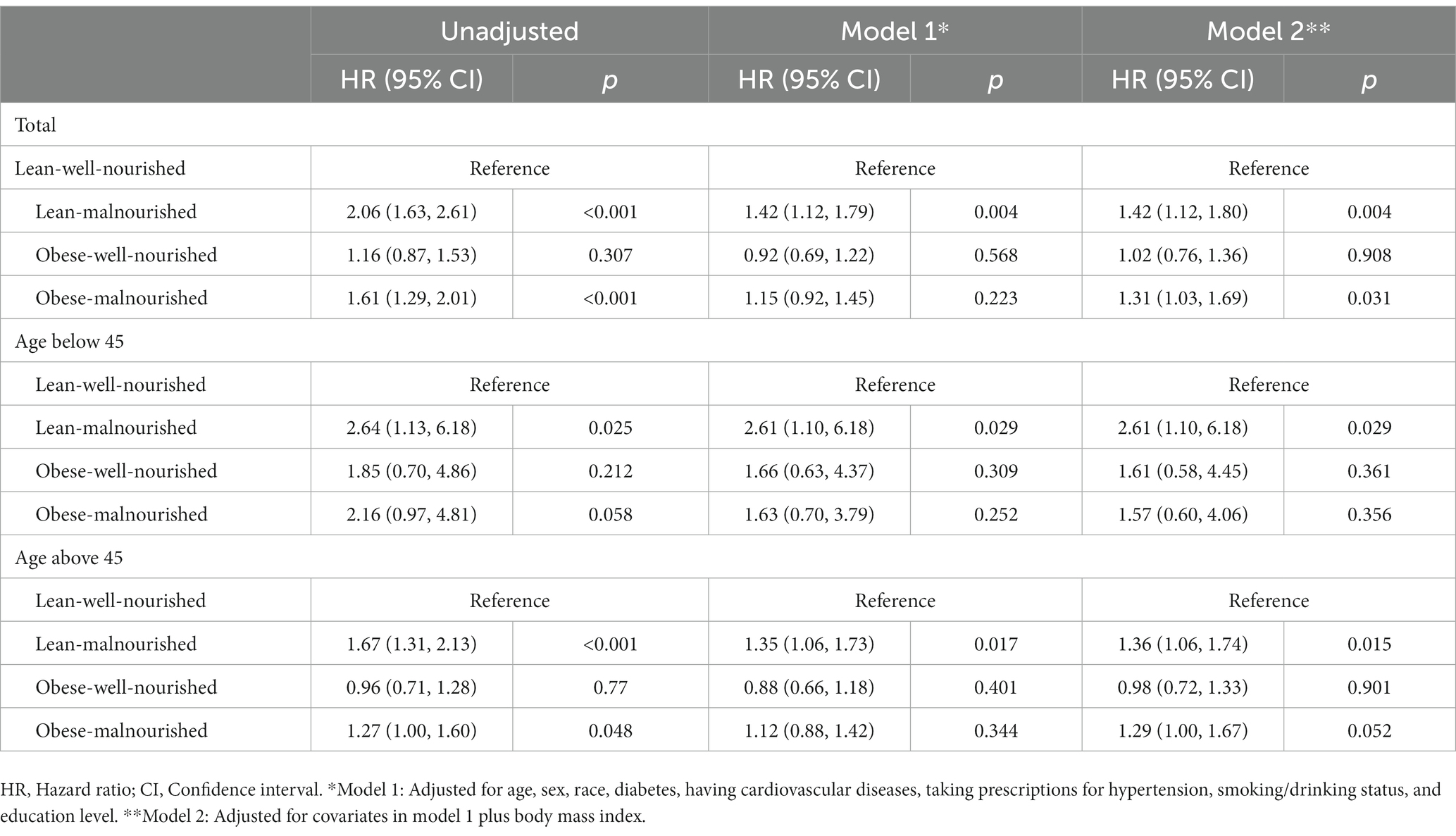
Table 4. The association of obesity and malnutrition with all-cause death in participants with hypertension.
4. Discussion
Nutritionally unhealthy obesity, or the individual-level double burden of malnutrition, is a newly introduced phenotype characterized by a combined condition of malnutrition and obesity, caused mainly by poor food quality and inadequate micronutrient consumption (9, 18). Traditionally, the double burden of malnutrition is thought to affect primarily low- to middle-income countries (7, 8). However, our study observed an individual-level double burden of malnutrition (low SA levels plus high waist circumference) in a considerable proportion of US participants, suggesting the long-standing importance of promoting favorable diet and health behaviors not only in developing countries but still in developed ones. We found that the demographic distribution of the obese-malnourished was typically older and often women, which is generally consistent with a recent study on Asian participants (9). This demographic distribution pattern is similar to that of malnutrition alone, the underlying mechanisms of which may include socioeconomic burden and metabolic features of aging (19).
Our results suggested that the association between obesity and the all-cause mortality risk of hypertension patients is modified by nutrition status. The obese-malnourished hypertension patients have a significantly higher mortality risk than the lean-well-nourished, whereas the risk of the obese-well-nourished is comparable with that of the reference group. This result implies that malnutrition may be an outcome indicator of hypertension which is independent of obesity. Similarly, a newly published study on heart failure patients reported that compared with the obese-well-nourished, the obese-malnourished status has a higher outcome risk, higher likelihood of comorbidities, and notable cardiac remodeling (9). Malnutrition in obese individuals is often overlooked in clinical practice, but recent evidence, including our study, suggested the significant association between this phenotype and the prognosis of CVDs and other diseases (20, 21).
This study further enhanced the understanding of the value of the SA test in clinical practice. Our results suggested that SA test can be an easy and inexpensive test in clinical practice to assist in evaluating the prognosis of hypertension patients. Beyond our findings, low SA levels have also been found to be an indicator of the emergence and worsening of some CVDs (22), and an independent predictor of ischemic heart disease and ischemic stroke even after adjustments for BMI, liver functions, and kidney functions (23). The underlying mechanisms of the association of low SA levels and cardiovascular dysfunctions are ambiguous. Speculations are that it is related to the inflammatory condition in malnutritional status with low SA. As human albumin is the most copious antioxidant in the whole blood, the insufficiency of SA will initialize oxidative stress and inflammation, which play a key role in the pathogenesis of hypertension and multiple CVDs (22, 24). At the same time, low SA levels can be the result of various causes including kidney diseases and general organ dysfunction due to CVDs (25), which may directly affect or reflect the cardiovascular health condition.
Among the malnourished hypertension participants, we found that obese individuals had a better outcome than the lean. This phenomenon is related to the so-called obesity paradox, i.e., obesity is associated with a higher risk for developing CVDs, but a better prognosis if the disease is present (26). Recent evidence argued that this paradox might stem more from the poorer catabolic reserve and more cachexia of the lean group rather than the potential benefit of the obesity itself, as studies have confirmed that low body fat percentage and low BMI are independent predictors of worse outcomes of CVDs (27, 28). Other possible causes for the better outcome of obese individuals may include younger age at presentation, lower prevalence of smoking, lower levels of atria natriuretic peptide, and more usage of cardiac medications (26).
Our study suggested that malnutrition may reduce the prevalence of hypertension. After being stratified by obesity status, the two malnourished groups presented a lower risk for developing hypertension than their well-nourished counterparts. This result is partly in line with earlier observations that SA level is positively associated with blood pressure (12, 29). However, this result does not imply that weakening nutritional condition is a desirable way to prevent hypertension since malnutrition is a harmful state associated with various comorbidities and remarkably higher mortality risk (30, 31). We speculate that this result is related to the SA’s function of maintaining colloid osmotic pressure, but precise underlying causes are worthy of further research.
Body mass index remains hitherto the most widely used measure to report obesity and related cardiovascular risk. However, since only weight and height are considered, BMI cannot comprehensively describe the heterogeneous composition of body weight and fat distribution within the obese population (32). Compared with BMI, waist circumference can better indicate visceral adiposity and provide additive information (33, 34), and was therefore recommended as a vital sign in clinical practice according to a recent consensus (35). Previous studies have reported that when analyzed in the same model, waist circumference was a risk factor for CVDs, but BMI was usually found to be a neutral or even protective factor (36–38). It is a strength that we used waist circumference to define obesity and adjusted for BMI in the analysis to fully investigate the potential value of obesity and nutrition status in evaluating the risk of hypertension.
4.1. Limitations
First, on the association between obesity and nutrition status with the prognosis of hypertension, this study only explored the risk of all-cause mortality without confirmation of the causal relationship. There remains the possible existence of multiple confounding factors that should not be ignored. Low SA levels may result from different causes such as chronic diseases and inflammatory conditions, many of which are directly related to worse cardiac outcomes, so the precise causal chain still needs to be further identified. Second, the baseline waist circumference and SA level of participants may change during the follow-up, but we cannot analyze the possible influence of these changes on the outcome. Third, the nutritional status was only evaluated by SA levels in this study. However, SA levels were affected by concurrent health issues apart from nutrition status. Therefore, further validation based on other nutritional indicators should be performed in the following study. Fourth, hypertension defined by both examination and self-report, may affect the robustness of the results. Lastly, due to the limitation of the data source, this study could not distinguish between primary and secondary hypertension.
5. Conclusion
This study based on NHANES observed the existence of an individual-level double burden of malnutrition in US citizens. We found that the association between obesity and the prognosis of hypertension is altered by nutrition status. Malnutrition defined by SA was associated with a lower risk of developing hypertension in both lean and obese participants, but it was associated with a worse outcome if the hypertension is present. The lean-malnourished hypertension patients had the highest all-cause death risk followed by the obese-malnourished. The obese- and lean-well-nourished hypertension patients showed a similar mortality risk lower than the mal-nourished.
Data availability statement
The original contributions presented in the study are included in the article/supplementary material, further inquiries can be directed to the corresponding authors.
Author contributions
H-ZZ, J-YS, SS, and YS conceived and designed the study. Y-LG, S-YW, J-YS, and L-LC analyzed the data. H-ZZ, Y-HW, and Y-LG wrote the paper. All authors provided critical revisions of the manuscript and approved the final manuscript.
Funding
This study was supported in part by the Natural Science Foundation of Jiangsu Province (No. 21KJB320006) and the College Students Innovation and Entrepreneurship Training Program of Jiangsu Province (No. 202110312006Z and No. 202210312010Z).
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Publisher’s note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
References
1. Zhou, B, Perel, P, Mensah, GA, and Ezzati, M. Global epidemiology, health burden and effective interventions for elevated blood pressure and hypertension. Nat Rev Cardiol. (2021) 18:785–802. doi: 10.1038/s41569-021-00559-8
2. Stanaway, JD, Afshin, A, Gakidou, E, Lim, SS, Abate, D, Abate, KH, et al. Global, regional, and national comparative risk assessment of 84 behavioural, environmental and occupational, and metabolic risks or clusters of risks for 195 countries and territories, 1990–2017: a systematic analysis for the global burden of disease study 2017. Lancet. (2018) 392:1923–94. doi: 10.1016/s0140-6736(18)32225-6
3. Olsen, MH, Angell, SY, Asma, S, Boutouyrie, P, Burger, D, Chirinos, JA, et al. A call to action and a lifecourse strategy to address the global burden of raised blood pressure on current and future generations: the lancet commission on hypertension. Lancet. (2016) 388:2665–712. doi: 10.1016/S0140-6736(16)31134-5
4. Collaboration NCDRF. Worldwide trends in hypertension prevalence and progress in treatment and control from 1990 to 2019: a pooled analysis of 1201 population-representative studies with 104 million participants. Lancet. (2021) 398:957–80. doi: 10.1016/S0140-6736(21)01330-1
5. Collaboration NCDRF. Worldwide trends in body-mass index, underweight, overweight, and obesity from 1975 to 2016: a pooled analysis of 2416 population-based measurement studies in 128.9 million children, adolescents, and adults. Lancet. (2017) 390:2627–42. doi: 10.1016/S0140-6736(17)32129-3
6. Samocha-Bonet, D, Dixit, VD, Kahn, CR, Leibel, RL, Lin, X, Nieuwdorp, M, et al. Metabolically healthy and unhealthy obese--the 2013 stock conference report. Obes Rev. (2014) 15:697–708. doi: 10.1111/obr.12199
7. Wells, JC, Sawaya, AL, Wibaek, R, Mwangome, M, Poullas, MS, Yajnik, CS, et al. The double burden of malnutrition: aetiological pathways and consequences for health. Lancet. (2020) 395:75–88. doi: 10.1016/S0140-6736(19)32472-9
8. Popkin, BM, Corvalan, C, and Grummer-Strawn, LM. Dynamics of the double burden of malnutrition and the changing nutrition reality. Lancet. (2020) 395:65–74. doi: 10.1016/S0140-6736(19)32497-3
9. Chien, SC, Chandramouli, C, Lo, CI, Lin, CF, Sung, KT, Huang, WH, et al. Associations of obesity and malnutrition with cardiac remodeling and cardiovascular outcomes in Asian adults: a cohort study. PLoS Med. (2021) 18:e1003661. doi: 10.1371/journal.pmed.1003661
10. Stamler, R, Stamler, J, Riedlinger, WF, Algera, G, and Roberts, RH. Weight and blood pressure. Findings in hypertension screening of 1 million Americans. JAMA. (1978) 240:1607–10. doi: 10.1001/jama.1978.03290150053024
11. Oda, E. Decreased serum albumin predicts hypertension in a Japanese health screening population. Intern Med. (2014) 53:655–60. doi: 10.2169/internalmedicine.53.1894
12. Vargas, CM, Obisesan, T, and Gillum, RF. Association of serum albumin concentration, serum ionized calcium concentration, and blood pressure in the third National Health and nutrition examination survey. J Clin Epidemiol. (1998) 51:739–46. doi: 10.1016/S0895-4356(98)00047-X
13. Executive summary of the third report of the National Cholesterol Education Program (NCEP) expert panel on detection, evaluation, and treatment of high blood cholesterol in adults (adult treatment panel III). JAMA. (2001) 285:2486–97. doi: 10.1001/jama.285.19.2486
14. Bakris, G, Ali, W, and Parati, G. ACC/AHA versus ESC/ESH on hypertension guidelines: JACC guideline comparison. J Am Coll Cardiol. (2019) 73:3018–26. doi: 10.1016/j.jacc.2019.03.507
15. Whelton, PK, Carey, RM, Aronow, WS, Casey, DE Jr, Collins, KJ, Dennison Himmelfarb, C, et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA guideline for the prevention, detection, evaluation, and Management of High Blood Pressure in adults: executive summary: a report of the American College of Cardiology/American Heart Association task force on clinical practice guidelines. J Am Coll Cardiol. (2018) 71:2199–269. doi: 10.1016/j.jacc.2017.11.005
16. Saydah, SH, Siegel, KR, Imperatore, G, Mercado, C, and Gregg, EW. The Cardiometabolic risk profile of young adults with diabetes in the U.S. Diabetes Care. (2019) 42:1895–902. doi: 10.2337/dc19-0707
17. Althouse, AD, Below, JE, Claggett, BL, Cox, NJ, de Lemos, JA, Deo, RC, et al. Recommendations for statistical reporting in cardiovascular medicine: a special report from the American Heart Association. Circulation. (2021) 144:e70–91. doi: 10.1161/CIRCULATIONAHA.121.055393
18. Freeman, AM, and Aggarwal, M. Malnutrition in the obese: commonly overlooked but with serious consequences. J Am Coll Cardiol. (2020) 76:841–3. doi: 10.1016/j.jacc.2020.06.059
19. O'Keeffe, M, Kelly, M, O'Herlihy, E, O'Toole, PW, Kearney, PM, Timmons, S, et al. Potentially modifiable determinants of malnutrition in older adults: a systematic review. Clin Nutr. (2019) 38:2477–98. doi: 10.1016/j.clnu.2018.12.007
20. Chien, SC, Chen, CY, Lin, CF, and Yeh, HI. Critical appraisal of the role of serum albumin in cardiovascular disease. Biomark Res. (2017) 5:31. doi: 10.1186/s40364-017-0111-x
21. Robinson, MK, Mogensen, KM, Casey, JD, McKane, CK, Moromizato, T, Rawn, JD, et al. The relationship among obesity, nutritional status, and mortality in the critically ill. Crit Care Med. (2015) 43:87–100. doi: 10.1097/CCM.0000000000000602
22. Arques, S. Human serum albumin in cardiovascular diseases. Eur J Intern Med. (2018) 52:8–12. doi: 10.1016/j.ejim.2018.04.014
23. Ronit, A, Kirkegaard-Klitbo, DM, Dohlmann, TL, Lundgren, J, Sabin, CA, Phillips, AN, et al. Plasma albumin and incident cardiovascular disease: results from the CGPS and an updated meta-analysis. Arterioscler Thromb Vasc Biol. (2020) 40:473–82. doi: 10.1161/ATVBAHA.119.313681
24. Rodrigo, R, Gonzalez, J, and Paoletto, F. The role of oxidative stress in the pathophysiology of hypertension. Hypertens Res. (2011) 34:431–40. doi: 10.1038/hr.2010.264
25. Levitt, DG, and Levitt, MD. Human serum albumin homeostasis: a new look at the roles of synthesis, catabolism, renal and gastrointestinal excretion, and the clinical value of serum albumin measurements. Int J Gen Med. (2016) 9:229–55. doi: 10.2147/IJGM.S102819
26. Ortega, FB, Lavie, CJ, and Blair, SN. Obesity and cardiovascular disease. Circ Res. (2016) 118:1752–70. doi: 10.1161/CIRCRESAHA.115.306883
27. Lavie, CJ, De Schutter, A, Patel, D, Artham, SM, and Milani, RV. Body composition and coronary heart disease mortality--an obesity or a lean paradox? Mayo Clin Proc. (2011) 86:857–64. doi: 10.4065/mcp.2011.0092
28. Lavie, CJ, McAuley, PA, Church, TS, Milani, RV, and Blair, SN. Obesity and cardiovascular diseases: implications regarding fitness, fatness, and severity in the obesity paradox. J Am Coll Cardiol. (2014) 63:1345–54. doi: 10.1016/j.jacc.2014.01.022
29. Hostmark, AT, Tomten, SE, and Berg, JE. Serum albumin and blood pressure: a population-based, cross-sectional study. J Hypertens. (2005) 23:725–30. doi: 10.1097/01.hjh.0000163139.44094.1d
30. Correia, MI, and Waitzberg, DL. The impact of malnutrition on morbidity, mortality, length of hospital stay and costs evaluated through a multivariate model analysis. Clin Nutr. (2003) 22:235–9. doi: 10.1016/S0261-5614(02)00215-7
31. Dziedzic, T, Slowik, A, and Szczudlik, A. Serum albumin level as a predictor of ischemic stroke outcome. Stroke. (2004) 35:e156–8. doi: 10.1161/01.STR.0000126609.18735.be
32. Neeland, IJ, Poirier, P, and Despres, JP. Cardiovascular and metabolic heterogeneity of obesity: clinical challenges and implications for management. Circulation. (2018) 137:1391–406. doi: 10.1161/CIRCULATIONAHA.117.029617
33. Pischon, T, Boeing, H, Hoffmann, K, Bergmann, M, Schulze, MB, Overvad, K, et al. General and abdominal adiposity and risk of death in Europe. N Engl J Med. (2008) 359:2105–20. doi: 10.1056/NEJMoa0801891
34. Poirier, P. Adiposity and cardiovascular disease: are we using the right definition of obesity? Eur Heart J. (2007) 28:2047–8. doi: 10.1093/eurheartj/ehm321
35. Ross, R, Neeland, IJ, Yamashita, S, Shai, I, Seidell, J, Magni, P, et al. Waist circumference as a vital sign in clinical practice: a consensus statement from the IAS and ICCR working group on visceral obesity. Nat Rev Endocrinol. (2020) 16:177–89. doi: 10.1038/s41574-019-0310-7
36. Garvey, WT, and Mechanick, JI. Proposal for a scientifically correct and medically actionable disease classification system (ICD) for obesity. Obesity (Silver Spring). (2020) 28:484–92. doi: 10.1002/oby.22727
37. de Hollander, EL, Bemelmans, WJ, Boshuizen, HC, Friedrich, N, Wallaschofski, H, Guallar-Castillon, P, et al. The association between waist circumference and risk of mortality considering body mass index in 65- to 74-year-olds: a meta-analysis of 29 cohorts involving more than 58 000 elderly persons. Int J Epidemiol. (2012) 41:805–17. doi: 10.1093/ije/dys008
38. Coutinho, T, Goel, K, Correa de Sa, D, Kragelund, C, Kanaya, AM, Zeller, M, et al. Central obesity and survival in subjects with coronary artery disease: a systematic review of the literature and collaborative analysis with individual subject data. J Am Coll Cardiol. (2011) 57:1877–86. doi: 10.1016/j.jacc.2010.11.058
Keywords: hypertension, obesity, malnutrition, waist circumference, double burden of malnutrition
Citation: Zhang H-Z, Wang Y-H, Ge Y-L, Wang S-Y, Sun J-Y, Chen L-L, Su S and Sun Y (2023) Obesity, malnutrition, and the prevalence and outcome of hypertension: Evidence from the National Health and Nutrition Examination Survey. Front. Cardiovasc. Med. 10:1043491. doi: 10.3389/fcvm.2023.1043491
Edited by:
Elise Peery Gomez-Sanchez, University of Mississippi Medical Center, United StatesReviewed by:
Diego Arauna, University of Talca, ChileAlexandre A. da Silva, University of Mississippi Medical Center, United States
Copyright © 2023 Zhang, Wang, Ge, Wang, Sun, Chen, Su and Sun. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Ying Sun, c3VueWluZzg3MTAxNEAxNjMuY29t; Shuang Su, MzUwMzQxNTAyQHFxLmNvbQ==; Heng-Zhi Zhang, aGVuZ3poaXpoYW5nQG5qbXUuZWR1LmNu
†These authors have contributed equally to this work and share first authorship
 Heng-Zhi Zhang
Heng-Zhi Zhang Yi-Han Wang1,2†
Yi-Han Wang1,2† Shu-Yu Wang
Shu-Yu Wang Jin-Yu Sun
Jin-Yu Sun Ying Sun
Ying Sun