- 1 Jean-Pierre Aubert Research Center, Inserm, U837, F-59000, Lille, France
- 2 Laboratory of Anatomy, Université Lille Nord de France, Lille, France
- 3 School of Medicine, UDSL, Lille, France
- 4 Department of Neurosurgery, CHULille, Lille, France
Over the past four decades it has become clear that prostaglandin E2 (PGE2), a phospholipid-derived signaling molecule, plays a fundamental role in modulating the gonadotropin-releasing hormone (GnRH) neuroendocrine system and in shaping the hypothalamus. In this review, after a brief historical overview, we highlight studies revealing that PGE2 released by glial cells such as astrocytes and tanycytes is intimately involved in the active control of GnRH neuronal activity and neurosecretion. Recent evidence suggests that hypothalamic astrocytes surrounding GnRH neuronal cell bodies may respond to neuronal activity with an activation of the erbB receptor tyrosine kinase signaling, triggering the release of PGE2 as a chemical transmitter from the glia themselves, and, in turn, leading to the feedback regulation of GnRH neuronal activity. At the GnRH neurohemal junction, in the median eminence of the hypothalamus, PGE2 is released by tanycytes in response to cell–cell signaling initiated by glial cells and vascular endothelial cells. Upon its release, PGE2 causes the retraction of the tanycyte end-feet enwrapping the GnRH nerve terminals, enabling them to approach the adjacent pericapillary space and thus likely facilitating neurohormone diffusion from these nerve terminals into the pituitary portal blood. In view of these new insights, we suggest that synaptically associated astrocytes and perijunctional tanycytes are integral modulatory elements of GnRH neuronal function at the cell soma/dendrite and nerve terminal levels, respectively.
Introduction
Sexual development, puberty, and adult fertility are achieved by events that are initiated within the central nervous system and require the maturation and function of a neural network that transmits both homeostatic and external cues to the discrete hypothalamic neuronal population that releases gonadotropin-releasing hormone (GnRH) from neuroendocrine terminals within the median eminence into the pituitary portal vessels to control gonadotropins (luteinizing hormone, LH and follicle stimulating hormone, FSH) secretion (Terasawa and Fernandez, 2001; Herbison and Neill, 2006; Malpaux, 2006; Ojeda and Skinner, 2006; Plant, 2006; Donato et al., 2011). In turn, these gonadotropins act on the ovaries and testis to regulate the secretion of sex steroids and the production of eggs and sperm.
In addition to neurons, accumulating evidence over the past two decades indicates that glial cells, and in particular astrocytes and tanycytes, also contribute to the neural network that converges onto GnRH neurons to control reproduction. Both the neuronal and glial elements of this GnRH neural network are subject to the direct modulatory influence of gonadal steroids (Garcia-Segura and McCarthy, 2004; Ronnekleiv and Kelly, 2005; Mong and Blutstein, 2006; Wintermantel et al., 2006; Christian and Moenter, 2010; Prevot et al., 2010a; Bellefontaine et al., 2011). Although neuronal elements regulate the activity of GnRH neurons through a complex array of excitatory and inhibitory synaptic inputs, glial cells communicate with GnRH neurons via the activation of specific growth-factor-dependent signaling pathways (reviewed in Melcangi et al., 2002; Herbison and Neill, 2006; Mahesh et al., 2006; Ojeda and Skinner, 2006; Sharif and Prevot, 2010).
The main glial population in the brain consists of astrocytes that ensheathe synapses and are in contact with blood vessels. They regulate blood flow, provide much-needed energy to neurons, and supply the building blocks for neurotransmitters at the synapses, in addition to dynamically contributing to information processing within the central nervous system (Haydon and Carmignoto, 2006; Martineau et al., 2006; Iadecola and Nedergaard, 2007; Eroglu and Barres, 2010; Halassa and Haydon, 2010; Pfrieger, 2010; Di Castro et al., 2011; Panatier et al., 2011), including the hypothalamus (Hatton and Wang, 2008; Theodosis et al., 2008; Gordon et al., 2009; Panatier, 2009; Oliet and Bonfardin, 2010). Tanycytes are elongated radial glial cells that have many features in common with astrocytes and are closely associated with neuroendocrine terminals in the median eminence of the hypothalamus (Theodosis et al., 2008; Prevot et al., 2010a,b; Dale, 2011; Sild and Ruthazer, 2011). As integrative hubs, astrocytes and tanycytes likely play a fundamental role in shaping and regulating the GnRH system.
Here, we will review recent findings that illustrate the remarkable interplay between glia and neurons within the hypothalamo-hypophyseal–gonadal axis, and show that different glial cell types regulate different aspects of the architecture, function, and plasticity of the GnRH system through dynamic and often multidirectional interactions with specialized neuronal junctions, such as synapses and neurohemal junctions. We will mainly restrict our focus to the roles of hypothalamic astrocytes and tanycytes subserved by the release of prostaglandin E2 (PGE2), a molecule that has long been known to regulate GnRH neuronal function and has recently been identified as a gliotransmitter.
Prostaglandin E2 and the Central Control of Reproduction
Prostaglandin E2 is one of a number of prostanoids synthesized from arachidonic acid, which is produced from membrane phospholipids by a phospholipase A2. Arachidonic acid is converted to bioactive prostanoids by the cyclooxygenases (COX-1 and COX-2) and a class of terminal synthases (see for review Bosetti, 2007; Figure 1). Several studies suggest that PGE2 is mainly derived from the COX-2 pathway (Brock et al., 1999; Vidensky et al., 2003; Sang et al., 2005). PGE2 signaling is propagated by four G-protein-coupled receptors, EP1–EP4 (see for review Coleman et al., 1994; Figure 1).
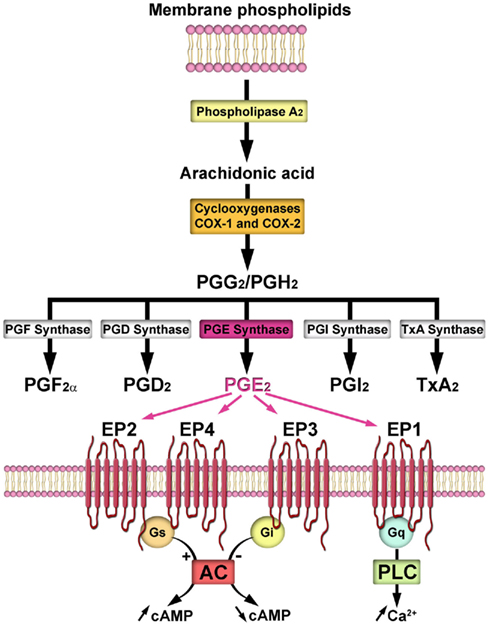
Figure 1. Prostaglandin E2 (PGE2) biosynthesis and signaling. Upon its release from plasma membrane phospholipids by phospholipase A2, arachidonic acid is converted to the unstable endoperoxide intermediates, prostaglandin G2 (PGG2), and prostaglandin H2 (PGH2) by the cyclooxygenases (COX-1 and COX-2, encoded by separate genes). Both COX isoforms catalyze the same reactions, but while COX-1 is constitutively expressed, COX-2 is rapidly and transiently upregulated by cytokines and growth factors. Terminal synthases convert both PGG2 and PGH2 into prostaglandins [PGE2, PGD2, PGF2α, prostacyclin (PGI2)], and thromboxane (TxA2). Once synthesized, PGE2 immediately diffuses away and activates its specific E-prostanoid receptors (EP1–4), which belong to the family of seven-transmembrane G-protein-coupled receptors. EP2 and EP4 are coupled to Gs and stimulate the adenylyl cyclase (AC)–cyclic adenosine monophosphate (cAMP)–protein kinase A (PKA) pathway. In contrast, EP3 is coupled to Gi and inhibits AC activation, resulting in decreased cAMP concentrations. EP1 is thought to be coupled to the Gq-phospholipase C (PLC) pathway, leading to an elevation of free cytosolic calcium concentrations (Milatovic et al., 2011). Notably, an examination of the capacity of the hypothalamus to metabolize arachidonic acid through the COX pathway has revealed a pubertal increase in the formation of PGE2, particularly during the first proestrus (Ojeda and Campbell, 1982). Intriguingly, the increase in PGE2 synthesis is not associated with changes in the formation of PGF2α, PGI2, PGD2, or thromboxane A2 from exogenous arachidonic acid, suggesting that it is a specific event directly associated with the peripubertal activation of the reproductive hypothalamus (Ojeda and Campbell, 1982). Such a selective synthesis of PGE2 has also been shown to be triggered by estrogens during early postnatal development (Amateau and McCarthy, 2002).
Prostaglandin E2 has been known to play a role in the central control of reproduction for more than 35 years. The first indication that PGE2 was involved in the process of GnRH secretion was provided by experiments showing that PGE2 injected into the third ventricle of the rat brain induced the release of LH into the general circulation (Harms et al., 1973) and of GnRH into the pituitary portal blood vessels (Eskay et al., 1975; Ojeda et al., 1975b). A similar stimulatory effect of PGE2 on GnRH release has also been documented in monkeys using push–pull perfusion in conscious animals (Gearing and Terasawa, 1991). To bring about the activation of the GnRH axis, PGE2 acts at two main hypothalamic sites: the preoptic-anterior hypothalamic region in which GnRH cell bodies reside, and the tuberal region of the hypothalamus, which contains the median eminence and GnRH-releasing neuroendocrine terminals (Ojeda et al., 1977). The use of COX inhibitors such as indomethacin has provided further support for a physiological role of the prostaglandins in the control of GnRH release. Indomethacin administration suppresses the LH surge induced by estradiol during anestrus in ewes (Carlson et al., 1974) and during the early follicular phase in rhesus monkeys (Carlson et al., 1977). In rats, the intraventricular or intrahypothalamic administration of indomethacin inhibits both pulsatile LH release and the LH discharge induced by ovarian steroids (Ojeda et al., 1975a). Other studies have demonstrated that the microinjection of either aspirin, a non-steroidal COX inhibitor, or N-0164, a prostaglandin and thromboxane antagonist, into the tuberal region of the rat hypothalamus results in the suppression of ovulation (Labhsetwar and Zolovick, 1973; Botting et al., 1977). Finally, experiments conducted using hypothalamic explants in vitro have revealed that PGE2 is an effective stimulator of GnRH release from median eminence nerve terminals (Gallardo and Ramirez, 1977; Ojeda et al., 1979, 1986b).
A sizable body of evidence also implicates PGE2 as a physiological component of the GnRH system during postnatal development. For instance, PGE2 can induce the release of GnRH long before puberty in both mice and rats (Ojeda et al., 1986a; Prevot et al., 2003b). As puberty approaches, the increasing output of estradiol from the developing ovaries induces a preovulatory surge of GnRH/LH. Biochemical analyses at this last phase of sexual maturation have demonstrated that the capacity of the reproductive hypothalamus to metabolize arachidonic acid through the COX pathway leads to a specific increase in PGE2 synthesis (Figure 1), particularly during the first proestrus (Ojeda and Campbell, 1982). This effect appears to be estrogen-dependent since it is mimicked by the treatment of juvenile animals (early post-weaning period) with estradiol at doses capable of inducing a preovulatory surge of LH (Ojeda and Campbell, 1982). More recent studies have shown that an estradiol-induced increase in hypothalamic PGE2 levels can be seen even in newborn rats (Amateau and McCarthy, 2002). Intriguingly, experiments showing that estradiol treatment upregulates both COX-2 mRNA and protein synthesis in the hypothalamus of female rats during postnatal development (Amateau and McCarthy, 2004) raise the possibility that estrogens may act on COX-2 expression to promote PGE2 synthesis at puberty.
Since the levels of arachidonic acid in tissue phospholipids are to some degree influenced by the dietary intake of different polyunsaturated fatty acids (e.g., linoleic acid), malnutrition during early life could cause deficits in arachidonic acid synthesis (de Souza et al., 2011; Lauritzen and Carlson, 2011), which in turn could lead to changes in the production of prostaglandins and thus interfere with the maturation of the GnRH system. Indeed, a diet-related deficiency of essential fatty acids initiated before fertilization in female rats has been shown to significantly delay the onset of reproductive capacity in female offspring without affecting the progression of gestation or the delivery of healthy litters by the dams (Smith et al., 1989). In this study, delayed puberty was associated with reduced PGE2 synthesis within the hypothalamus. The deficit did not appear to be due to the impairment of COX activity, but to diminished arachidonic acid bioavailability (Smith et al., 1989).
Glia, the Main Source of Prostaglandin E2 within the GnRH Neurosecretory System
Although PGE2 was initially postulated to be an intracellular messenger produced by the binding of neurotransmitters to receptors located on GnRH neurons and acting within these neurons (Ojeda et al., 1982; Gearing and Terasawa, 1991; Rettori et al., 1992), this concept has been revisited following studies showing that the actions of PGE2 on GnRH release are initiated by its binding to specific membrane receptors (Coleman et al., 1994) expressed by GnRH neurons (Rage et al., 1997) and the recognition that astrocytes represent a major source of PGE2 in the brain (Ma et al., 1997; Bezzi et al., 1998; Hirst et al., 1999). Two decades ago, seminal studies by Ojeda and colleagues revealed that the PGE2-mediated activation of GnRH neuronal secretory activity triggered by estrogen at the time of puberty required the activation of growth-factor-dependent glial signaling pathways involving receptor tyrosine kinases of the erbB family (Ojeda et al., 1990; Junier et al., 1991; Ma et al., 1992).
Of the four known members of the erbB family (Figure 2), three of them, erbB1, erbB3, and erbB4, bind and are activated by cognate ligands. In contrast, erbB2 has no known ligand, and functions primarily as a modulator of the other members of the family (Hynes and Lane, 2005). While erbB receptors do not appear to be expressed in GnRH neurons (Ma et al., 1994b, 1999; Voigt et al., 1996; Prevot et al., 2003b), erbB1, erbB2, and erbB4, but not erbB3, are expressed in hypothalamic astrocytes, known to morphologically and physically interact with GnRH cell bodies (Witkin et al., 1995; Cashion et al., 2003; Baroncini et al., 2007; Sandau et al., 2011a) both in rodents and humans (Figures 3 and 4; Ma et al., 1999; Prevot et al., 2003b; Sharif et al., 2009). In addition, hypothalamic astrocytes express the erbB1 ligand, transforming growth factor alpha (TGFα; Figure 4), and several forms of the erbB4 ligand, neuregulin (Ma et al., 1992, 1994a, 1999; Sharif et al., 2009). Importantly, gonadal steroids have been found to induce dramatic increases in the expression levels of the erbB receptors and their ligands within the hypothalamus at puberty; no such changes are seen in the cortex or other brain regions unrelated to reproductive control (Ma et al., 1992, 1994a, 1999).
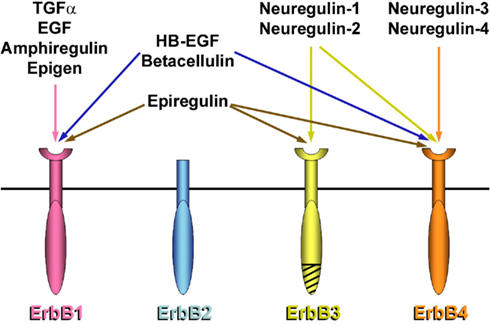
Figure 2. The erbB family of receptors and their ligands. ErbB1 (or EGFR, epidermal growth factor receptor) and erbB4 are fully functional receptors that possess an extracellular ligand-binding domain and a cytoplasmic protein tyrosine kinase domain and can function as homo- or heterodimers. In contrast, erbB2 (or neu), which lacks a ligand-binding domain, and erbB3, which is defective in its intrinsic tyrosine kinase activity (dashed lines), must heterodimerize with another member of the erbB family for signal transduction. The different EGF-like growth factors exhibit different binding specificities for the erbB receptors. While TGFα, EGF, amphiregulin, epigen, neuregulin-3, and neuregulin-4 are specific for a single member of the receptor family, the five other EGF-like ligands can bind two or three receptors each. EGF, epidermal growth factor; HB-EGF, heparin binding-EGF; TGFα, transforming growth factor α.
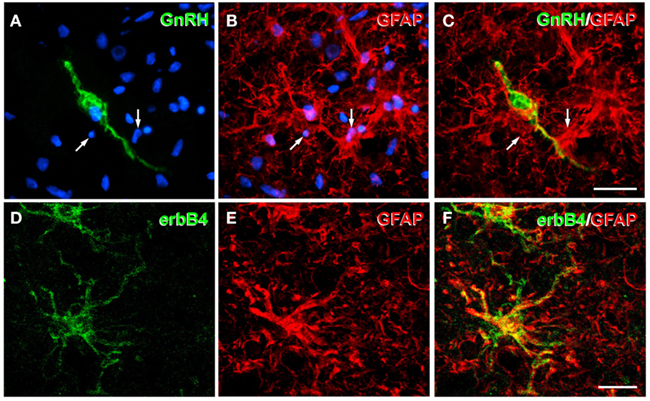
Figure 3. Astrocytes morphologically interact with GnRH neurons and express erbB4 receptors in the tuberal region of the human hypothalamus. (A–C) Photomicrographs showing a GnRH neuronal cell body (green) to which the processes of glial fibrillary acidic protein (GFAP)-immunoreactive astrocytes (red, arrows) are abundantly apposed. Cell nuclei are stained with Hoechst (blue). Adapted from (Baroncini et al., 2007) with permission. (D–F) GFAP-immunoreactive astrocytes (red) of the tuberal region of the human hypothalamus express erbB4 receptors (green; M. Baroncini and V. Prevot, unpublished data). Scale bars = 20 μm (C), 10 μm (F).
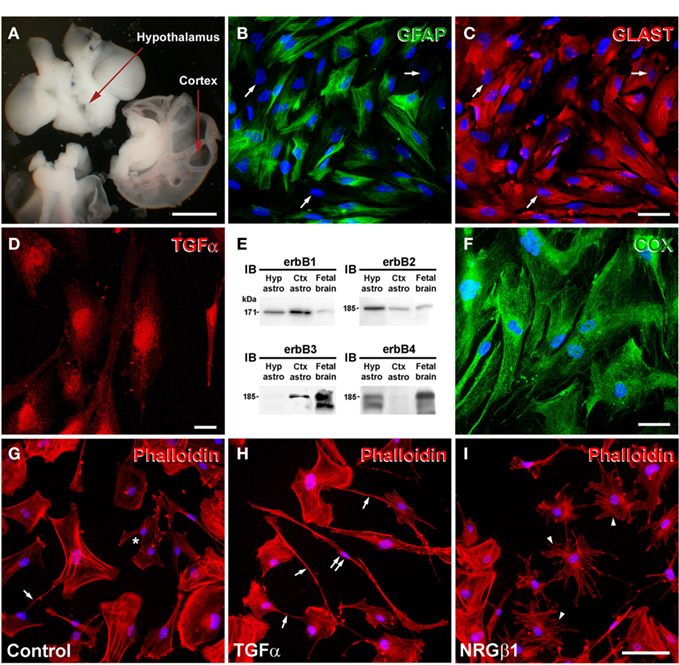
Figure 4. Human hypothalamic astrocytes express the molecular components required for a glia-to-neuron communication through the erbB-prostaglandin signaling system. Primary cultures of human hypothalamic astrocytes have been prepared from 9 to 12-week-old human fetuses (A). The cultures are composed of 98% of cells immunopositive for the astrocytic markers GFAP [(B) green] and the glutamate–aspartate transporter GLAST [(C) red]. Note that cells that express GFAP at low to undetectable levels are nevertheless strongly immunopositive for GLAST (arrows). (D) Human astrocytes in culture express TGFα protein (red). (E) Western blot analysis of erbB receptor expression in primary cultures of human cortical and hypothalamic astrocytes. While all four erbB receptors are expressed in the fetal brain, hypothalamic astrocytes (Hyp astro) express erbB1, erbB2, and erbB4, but not erbB3, and cortical astrocytes (Ctx astro) express erbB1, erbB2, and erbB3 but not erbB4 receptors. IB, immunoblot. (F) Human hypothalamic astrocytes in culture are immunopositive for COX (green). (G–I) EGF ligands induce profound morphological rearrangements of human hypothalamic astrocytes in vitro. Cell morphology was examined by visualization of the actin cytoskeleton using Alexa Fluor 568-conjugated phalloidin (red). Hypothalamic astrocytes exhibit heterogeneous shapes under control conditions, i.e., polygonal cells, cells with short and thick extensions (asterisk) or long and thin processes (arrow) (G). TGFα (50 ng/mL for 3 days) stimulates the extension of long and thin processes (arrows) and the apparition of bipolar cells (double arrows) (H) while treatment with neuregulin-1 NRGβ1 (50 ng/mL for 3 days) increases the number of multipolar cells with thick processes (arrowheads) (I). Nuclei are counter-stained with Hoechst [(B,C,F–I), blue]. Scale bars = 3 mm (A), 50 μm (B,C,F), 20 μm (D), 100 μm (G–I). Adapted from (Sharif et al., 2009) with permission.
The pharmacological or genetic inhibition of erbB1, erbB2, and/or erbB4 receptors delays the onset of puberty (Ma et al., 1992; Apostolakis et al., 2000; Prevot et al., 2003b, 2005) and alters adult reproductive function in rodents (Prevot et al., 2005). In vitro studies using either hypothalamic explants or primary cultures of hypothalamic astrocytes with a GnRH-producing neuronal cell line have shown that erbB receptor ligands can stimulate GnRH release from the explants or neuronal cells, but do so indirectly, by inducing astrocytes to secrete PGE2 (Ojeda et al., 1990; Ma et al., 1997, 1999; Prevot et al., 2003b, 2005). In addition, ligand activation of erbB receptors has been shown to promote morphological rearrangements in hypothalamic astrocytes (Figure 4G–I; Sharif et al., 2009) thus raising the possibility that erbB signaling may also influence the astrocytic coverage of GnRH neurons in vivo (see for review Prevot et al., 2010b).
In vitro experiments suggest that erbB signaling in hypothalamic astrocytes is functionally connected to the neuronal glutamatergic system, the primary mode of excitatory transsynaptic communication used by hypothalamic neurons (van den Pol and Trombley, 1993), and one that is known to increase GnRH secretion (Donoso et al., 1990; Claypool et al., 2000) and accelerate the initiation of puberty in both rodents and primates (Urbanski and Ojeda, 1987, 1990; Plant et al., 1989). In hypothalamic and non-hypothalamic astrocytes alike (Bezzi et al., 1998; Zonta et al., 2003a,b), transmitter spillover from nearby synaptic activity results in an elevation of PGE2 release (McCarthy et al., 2008; Glanowska and Moenter, 2011). For example, neuronally released glutamate can engage biochemical signaling in astrocytes through the co-activation of AMPA and metabotropic glutamate receptors to cause a ligand-dependent increase in astrocytic erbB signaling and PGE2 release (Dziedzic et al., 2003). This in turn signals back to GnRH neurons (Figure 5) facilitating neuroendocrine development and adult reproductive function (Prevot et al., 2003b, 2005).
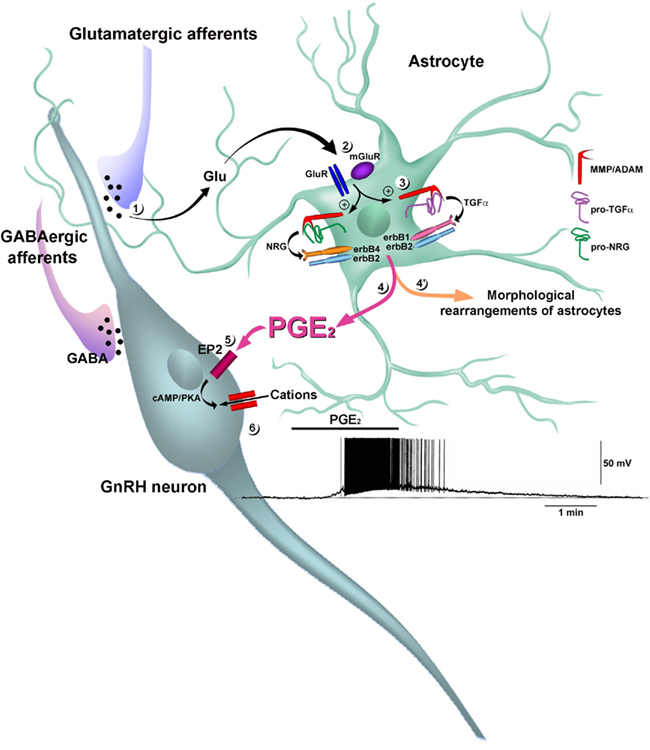
Figure 5. Prostaglandin E2 acts as a gliotransmitter to stimulate GnRH neuron electrical activity. Neuronally released glutamate (Glu) (1) co-activates metabotropic glutamatergic (mGluR) and AMPA glutamatergic receptors (GluR) in astrocytes (2), stimulating the activity of zinc-dependent matrix metalloproteinases (MMPs) of the ADAM (a disintegrin and metalloproteinase) family (3). The MMPs catalyze ectodomain shedding of the pro-EGF ligands pro-TGFα and pro-NRG (pro-neuregulin). In particular, the processing of pro-TGFα has been shown to involve the metalloproteinase ADAM17, also known as tumor necrosis factor α converting enzyme (TACE). The subsequently released mature TGFα and NRG activate erbB1/erbB2 and erbB4/erbB2 heterodimers, respectively (Dziedzic et al., 2003). The co-activation of glutamatergic receptors induces the recruitment of erbB1, erbB4, and their pro-ligands to the cell membrane, where multiprotein complexes form, as demonstrated by the direct physical association of glutamatergic and erbB receptors (not shown). The activation of erbB receptors in hypothalamic astrocytes promotes profound morphological changes, including the retraction of cytoplasm, stellation of cells and the elongation of processes (see Figure 4G–I) (4′). The activation of erbB receptors also promotes the release of PGE2 (Ma et al., 1997, 1999; Dziedzic et al., 2003) (4), which stimulates a cAMP/protein kinase A (PKA) pathway in GnRH neurons through the mobilization of EP2 receptors (EP2; Clasadonte et al., 2011) (5). Activation of this signaling pathway induces a reversible membrane depolarization of GnRH neurons leading to the initiation of spike firing via a postsynaptic effect involving the activation of a non-selective cation current (Clasadonte et al., 2011) (6).
Prostaglandin E2, a Newly Uncovered Gliotransmitter within the GnRH Neurosecretory System
Even though PGE2 has been known to trigger GnRH release from the hypothalamic neurons controlling reproduction for almost 40 years, it is only very recently that it has been identified as a potent excitatory regulator of GnRH neuronal activity, both in male and female mice (Clasadonte et al., 2011). Using patch-clamp recordings in brain slices from transgenic mice expressing green fluorescent protein (GFP) under the control of the GnRH promoter, we showed that PGE2 induced a reversible membrane depolarization of GnRH neurons leading to the initiation of spike firing via the postsynaptic effect involving activation of a non-selective cation current (Figure 5; Clasadonte et al., 2011) reminiscent of the ones recently described in GnRH neurons by other groups (Zhang et al., 2008; Roland and Moenter, 2011). Although GnRH neurons are known to express both the EP1 and EP2 subtypes of prostaglandin receptors in vivo (Rage et al., 1997; Jasoni et al., 2005), the excitatory effect of PGE2 on GnRH neuronal activity was selectively mimicked by the EP2 receptor agonist butaprost (Clasadonte et al., 2011) previously shown to promote GnRH release in the GnRH-producing neuronal cell line, GT1–7 (Rage et al., 1997). The PGE2-mediated membrane depolarization of GnRH neurons was also shown to require the cAMP/protein kinase A (PKA) pathway (Clasadonte et al., 2011), which is known to be coupled to the EP2 receptor (Figure 1; Coleman et al., 1994; Sang et al., 2005) and to underlie the stimulatory effect of PGE2 on GnRH secretion (Figure 5; Ojeda et al., 1985).
As alluded to above, the selective disruption of erbB4 signaling in astrocytes by the overexpression of a dominant-negative erbB4 receptor under the control of the human GFAP promoter leads to diminished PGE2 release in response to ligand-dependent erbB4 activation, leading in turn to reduced GnRH release, delayed puberty, and disrupted adult reproductive function (Prevot et al., 2003b, 2005). Intriguingly, electrophysiological analyses have shown that the spontaneous activity of GnRH neurons in these animals is decreased and that this deficiency is mimicked by the bath application of either fluoroacetate, an inhibitor of astrocyte metabolism (Fonnum et al., 1997; Henneberger et al., 2010), or the COX blocker indomethacin, to slices of the preoptic region from wild-type animals (Clasadonte et al., 2011). The fact that GnRH neuronal activity in all these conditions can be rescued by exogenous PGE2 (Clasadonte et al., 2011) strongly suggests that glial PGE2 is an important component of the homeostatic mechanism controlling GnRH neuronal excitability. The role of glia in the control of GnRH neuronal activity is further supported by a recent study demonstrating that glial prostaglandins may regulate the efficacy of GABAergic inputs to GnRH neurons in ovariectomized mice (Glanowska and Moenter, 2011). Using GnRH–GFP transgenic mice and patch-clamp recordings in brain slices, the authors demonstrated that the repeated action-potential-like depolarization of a GnRH neuron caused a short-term reduction in the frequency of spontaneous GABAergic postsynaptic currents in the same neuron, suggesting the presence of local circuit interactions between GnRH neurons and their GABAergic afferents (Chu and Moenter, 2005; Glanowska and Moenter, 2011). It is important to note that in this local circuit, the activation of GABAA receptors exerts a depolarizing action that can trigger action potential firing due to the elevated chloride levels maintained in adult GnRH neurons (DeFazio et al., 2002; Han et al., 2002; Herbison and Moenter, 2011). Consequently, this represents a negative feedback loop in which depolarized GnRH neurons reduce the activity of their own excitatory GABAergic afferents. In addition to being steroid-dependent and under the influence of both glutamatergic and endocannabinoid signaling mechanisms via the activation of presynaptic metabotropic glutamate receptors and cannabinoid CB1 receptors respectively (Chu and Moenter, 2005; Glanowska and Moenter, 2011) this local negative feedback loop also requires the action of glial-derived prostaglandins (Glanowska and Moenter, 2011). Indeed, the incubation of brain slices with indomethacin, the broad-spectrum prostaglandin receptor antagonist AH 6809, or fluorocitrate, which like fluoroacetate, is a specific blocker of astrocyte metabolism, prevents the depolarization-induced suppression of GABAergic transmission in GnRH neurons (Glanowska and Moenter, 2011). Since GABA exerts a depolarizing action in this local circuit, we could envisage that glial prostaglandins, by suppressing excitatory drive, would reduce GnRH neuronal activity. Estradiol could also differentially influence this local inhibitory feedback to exert its positive or negative feedback effects (Glanowska and Moenter, 2011). Thus, in addition to exerting a direct postsynaptic excitatory action on the cell body of GnRH neurons, prostaglandins released from astrocytes can also participate in mechanisms that regulate the activity of their GABAergic presynaptic inputs (Figure 5). In the GnRH system, thus, PGE2 fulfills all the criteria that qualify a compound as a “gliotransmitter” (Parpura and Zorec, 2010): (i) it is synthesized by astrocytes, (ii) its regulated release is triggered by physiological stimuli, (iii) it acutely activates the firing of GnRH neurons and modulates the activity of their GABAergic afferents, and (iv) it plays a role in an important physiological function, i.e., the neuroendocrine control of reproduction, which is vital to species’ survival.
A Role for Astroglial Prostaglandin E2 in Dendritic Spine Plasticity in GnRH Neurons?
Gonadotropin-releasing hormone neurons exhibit a simple bipolar morphology (Figure 3A) with one or two very long dendritic processes that can extend up to 1 mm (Campbell et al., 2005, 2009). Intriguingly, recent studies have demonstrated that the density of spines along these dendrites is subject to robust increases not only during sexual development in immature animals (Cottrell et al., 2006), but also at the onset of the GnRH/LH surge induced by gonadal steroids in ovariectomized adult mice (Chan et al., 2011). Although sexual maturation and the surge mechanism have been shown to require the neuronal expression of sex-steroid receptors (Wintermantel et al., 2006; Raskin et al., 2009; Mayer et al., 2010), studies suggesting that astrocytic mechanisms might control the stabilization of individual dendritic processes and their subsequent maturation into spines (Nishida and Okabe, 2007), together with the demonstration that specific juxtacrine signaling pathways are involved in sculpting astrocyte–dendritic spine interactions (Murai et al., 2003), raise the possibility that astrocytes play a role in the physiological changes of synaptic structure underlying GnRH neuronal maturation and function. PGE2 release by astrocytes could be central in this process and PGE2 has in fact been shown to mediate the dramatic neuronal spine plasticity induced by estrogens in the developing preoptic region (Amateau and McCarthy, 2002, 2004; Wright and McCarthy, 2009). This effect involves the activation of AMPA and metabotropic glutamate receptors (Amateau and McCarthy, 2002; Wright and McCarthy, 2009), known to promote erbB-dependent PGE2 release in hypothalamic astrocytes (Dziedzic et al., 2003), as well as the EP2/PKA signaling pathway (Amateau and McCarthy, 2002), recently found to be functional in native GnRH neurons (Clasadonte et al., 2011; Figure 5). Importantly, estrogens, which have long been known to regulate neuronal spine plasticity in the adult hippocampus (Woolley and McEwen, 1992, 1994), have also been shown to promote comparable changes in the immature hippocampus (Amateau and McCarthy, 2002). However, in the hippocampus, the underlying mechanisms do not appear to require PGE2 synthesis (Amateau and McCarthy, 2002), suggesting that increases in PGE2 synthesis are selectively used by estrogens to promote dendritic spine plasticity in the developing preoptic region. Further studies are required to determine whether estrogenic effects on the plasticity of hypothalamic neurons such as those seen in newborn rodents can also occur later in postnatal life and/or in adulthood.
Prostaglandin E2 is a Key Mediator of GnRH Release, Neuronal–Glial–Endothelial Interactions, and Cell Plasticity at the GnRH Neurohemal Junction
Neuroendocrine GnRH neurons send axons to the median eminence, where they release their neurohormone into the pituitary portal blood vessels for delivery to the anterior pituitary. The median eminence, which lies ventral to the third ventricle in the tuberal region of the hypothalamus, constitutes one of the key sites for the regulation of GnRH release (see for review Hrabovszky and Liposits, 2008; Ojeda et al., 2008; Prevot et al., 2010a; Yin and Gore, 2010). The modulation of GnRH release by PGE2 within the median eminence was suggested as soon as in vitro systems to statically incubate median eminence nerve terminals were developed, i.e., in the late 70s (Negro-Vilar et al., 1979; Ojeda et al., 1979). Experiments showing that the PGE2-induced GnRH release from median eminence explants requires the mobilization of intracellular calcium stores (Ojeda and Negro-Vilar, 1985; Ojeda et al., 1988) have suggested a role for the EP1 receptor in this process (Figure 1). In line with this assumption are other findings demonstrating that GnRH neurons express EP1 receptors in vivo and that the EP1 agonist 17-phenyl trinor PGE2 promotes GnRH release from GT1–1 cells in vitro (Rage et al., 1997) without affecting GnRH neuronal firing in brain slices (Clasadonte et al., 2011).
Within the median eminence, GnRH axon terminals are intimately associated with cell processes belonging to specialized unciliated ependymal cells named tanycytes. Tanycyte cell bodies are attached together at the apex by tight junctions (Mullier et al., 2010) and line the floor of the third ventricle. They send out long slender processes that eventually contact the pial surface of the brain where the fenestrated pituitary portal vessels reside, via end-feet (Page, 1994; Ciofi et al., 2009; Mullier et al., 2010). These tanycyte end-feet not only enclose the GnRH nerve terminals, possibly providing a diffusion barrier (Kozlowski and Coates, 1985; Meister et al., 1988; Ugrumov et al., 1989; King and Letourneau, 1994), but also display a high degree of structural plasticity across the ovarian cycle in rats (Prevot et al., 1998, 1999). During the estrous cycle, under basal conditions, e.g., in diestrus, GnRH nerve terminals are completely wrapped up in tanycyte end-feet (Prevot et al., 1998, 1999). In proestrus, following the activation of the reproductive axis, the end-feet are retracted, presumably due to increasing levels of gonadal steroids (King and Letourneau, 1994), thus allowing GnRH neurons to directly contact the pericapillary space (Prevot et al., 1998). By analogy with the function-related plasticity documented in the neural lobe of the pituitary (Hatton, 1997), these data argue for the importance of tanycyte structural rearrangement in delivering peak levels of GnRH to the pituitary during the preovulatory surge. The intriguing possibility that PGE2 could be involved in the control of these plastic phenomena arises from recent studies using either median eminence explants (de Seranno et al., 2010) or primary cultures of tanycytes isolated from the median eminence (Prevot et al., 2003a; De Seranno et al., 2004; de Seranno et al., 2010; Figure 6). When PGE2 is applied to median eminence explants at concentrations known to stimulate GnRH release, structural remodeling occurs at the neurohemal junction in a matter of minutes causing GnRH neurosecretory terminals to advance toward the pericapillary space (de Seranno et al., 2010), a phenomenon that probably results from the retraction of tanycyte end-feet (Figure 6B), as suggested by the PGE2-promoted tanycyte retraction seen in vitro (Figure 6A). As extensively reviewed elsewhere (Prevot et al., 2010a,b; Bellefontaine et al., 2011), PGE2 synthesis in tanycytes of the median eminence could be prompted by two independent but complimentary cell-based mechanisms, one involving glial–glial interactions set in motion by the paracrine activation of TGFα/erbB1 signaling pathway in tanycytes, as depicted in Figure 7A (Prevot et al., 2003a), and another involving endothelial–tanycyte interactions and the release of nitric oxide (NO) by vascular endothelial cells, which in turn directly modulates COX activity in tanycytes, as described in Figure 7B (De Seranno et al., 2004; de Seranno et al., 2010). Both pathways could be subject to the modulatory influence of gonadal steroids, as estrogens are known to upregulate both TGFα expression in astroglial cells (Ma et al., 1992, 1994a) and COX expression in tanycytes (de Seranno et al., 2010). Finally, the physiological importance of PGE2 in the cell–cell communication processes regulating GnRH release has been highlighted by experiments in which the COX inhibitor indomethacin is infused directly into the median eminence, resulting in the marked impairment of the rat ovarian cycle, which requires the coordinated delivery of GnRH into the hypothalamo-hypophyseal portal system (de Seranno et al., 2010). Indeed, the local inhibition of prostaglandin synthesis has been shown to arrest the ovarian cycle in either diestrus or estrus when GnRH release is low (Levine and Ramirez, 1982) and GnRH neuroendocrine terminals are enclosed by tanycyte end-feet (Prevot et al., 1998, 1999).
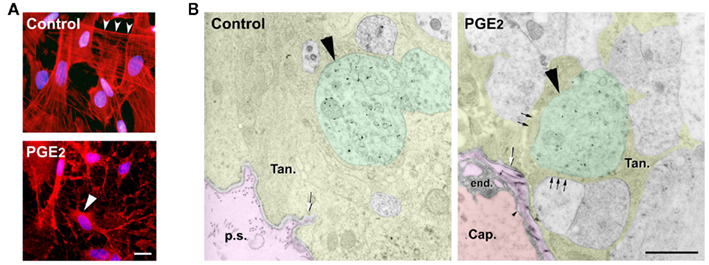
Figure 6. Prostaglandin E2 promotes the retraction of tanycytic processes in vitro and induces neuroglial plasticity causing GnRH neurosecretory terminals to advance toward the pericapillary space in isolated median eminence explants. (A) Tanycytes in culture were stained with Alexa Fluor 568-conjugated phalloidin to visualize filamentous actin (red) and with Hoechst to stain nuclei (blue). In control unstimulated tanycyte cultures, actin was localized adjacent to the cell membrane (top panel, cortical actin, arrowheads) and was also diffused throughout the cytoplasm. PGE2 treatment (280 nM, 30 min) promoted tanycyte retraction (bottom panel, long arrowhead). (B) Electron micrographs of GnRH immunoreactive axon terminals (big arrowhead, green) from female rat median eminence explants incubated for 30 min in the presence or absence of PGE2 (1 μM). Under basal unstimulated conditions (Control), GnRH nerve endings (big arrowhead, green) were maintained at a distance from the brain basal lamina (white arrow) delineating the pericapillary space (p.s., pink) by thick enclosing tanycyte end-feet (Tan., yellow). PGE2 treatment caused the advancement of GnRH axon terminals (big arrowhead, green) toward the brain basal lamina (white arrow) and the apparent retraction of most of the astroglial sheath (black arrows, yellow) from those neurosecretory terminals that were separated from the fenestrated (small arrowhead) portal capillaries (Cap., red) by only a few nanometers. end., endothelium. Scale bars = 10 μm (A), 1 μm (B). Reproduced from (de Seranno et al., 2010) with permission.
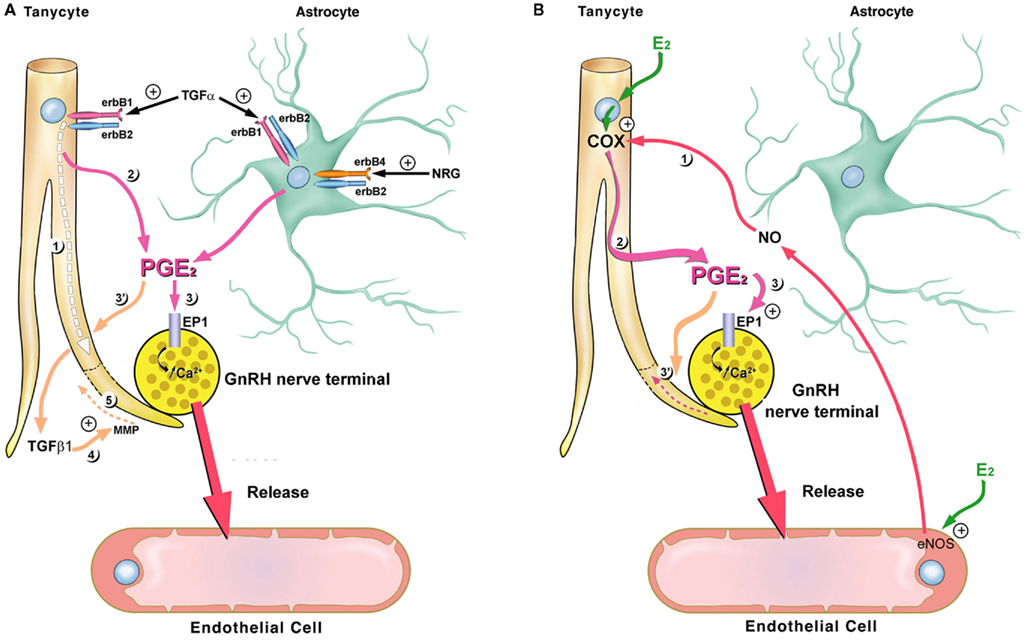
Figure 7. Schematic representation of neural–glial–endothelial interactions involved in the control of GnRH neurosecretion in the median eminence. (A) Glial–neuronal interactions in the median eminence involve the production of epidermal growth factor (EGF)-related peptides by glial cells. Activation of erbB1/erbB2 and erbB4/erbB2 heterodimers by TGFα and NRG, respectively, promotes the release of PGE2 from astrocytes. The binding of TGFα to tanycytic erbB1 receptors results in the recruitment of erbB2 co-receptors and signal transduction. The ligand-dependent activation of erbB1 receptors in tanycytes results in biphasic plastic changes characterized by an initial phase of tanycyte outgrowth (1) and a secondary phase of retraction (5). Although the initial outgrowth (1) is independent of the TGFβ1 system, the subsequent retraction requires PGE2 synthesis (2), a PGE2-dependent increase in the production of TGFβ1 (3′) and matrix metalloproteinase (MMP) activity (4). In addition to promoting TGFβ1 synthesis by tanycytes (3′), PGE2 released by tanycytes (2) and astrocytes is able to directly stimulate GnRH release at nerve endings through the EP1 receptor (EP1)-mediated mobilization of intracellular calcium stores (3). (B) Endothelial–neuronal interactions at the level of the median eminence involve the production of nitric oxide (NO) by the endothelial cells of fenestrated capillaries of the portal blood vessels. Upon its secretion, NO diffuses from its source and stimulates the production of PGE2 from tanycytes. PGE2 promotes the release of GnRH into the blood stream by the direct stimulation of nerve endings (3) and by promoting their access to the pericapillary space by inducing cytoarchitectural changes in tanycyte end-feet (1–3′). Estrogens are likely to be the key humoral factors involved in the orchestration of the endothelia-to-glia communication that allows GnRH neurons to directly contact the pituitary portal blood vessels on the day of proestrus. Estrogen treatment upregulates COX expression in tanycytes and stimulates endothelial nitric oxide synthase (eNOS) expression in median eminence endothelial cells. Adapted from (Prevot, 2002) with permission.
Conclusion
Several observations made over the last two decades have demonstrated that PGE2 known for almost 40 years to play an important role in the regulation of the hypothalamic–pituitary–gonadal axis, is a transmitter released by astrocytes and tanycytes, and intimately linked with GnRH neuronal function in both the preoptic region and the median eminence of the hypothalamus, where the cell bodies and the neuroendocrine terminals of GnRH neurons in rodents are respectively located. However, many mysteries regarding the underlying mechanisms remain unsolved. For example, even though recent studies suggest that GnRH neurons can directly communicate with neighboring astrocytes via juxtacrine signaling pathways (Sandau et al., 2011a,b), a true understanding of how these GnRH neurons interact with hypothalamic astrocytes to modulate PGE2 gliotransmission is missing. Are these communication processes involved in sculpting astrocyte–dendritic spine interactions and in promoting the physiological changes in synaptic structure that underlie GnRH neuronal maturation and function? How is PGE2 released from hypothalamic astrocytes?
Now that a general strategy for the application of molecular genetics to the study of neuron–glia interactions and gliotransmission has been elucidated, the next several years should provide an opportunity to begin to address these questions.
Conflict of Interest Statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Acknowledgments
This research was supported by the Agence Nationale pour la Recherche (ANR, France) grants ANR-07-NEURO-026-03 and ANR-09-BLAN-0267, the Fondation pour la Recherche Médicale (Equipe FRM 2005, France). Jerome Clasadonte was supported by a doctoral fellowship from the INSERM and the Région Nord Pas de Calais.
References
Amateau, S. K., and McCarthy, M. M. (2002). A novel mechanism of dendritic spine plasticity involving estradiol induction of prostaglandin-E2. J. Neurosci. 22, 8586–8596.
Amateau, S. K., and McCarthy, M. M. (2004). Induction of PGE2 by estradiol mediates developmental masculinization of sex behavior. Nat. Neurosci. 7, 643–650.
Apostolakis, E. M., Garai, J., Lohmann, J. E., Clark, J. H., and O’Malley, B. W. (2000). Epidermal growth factor activates reproductive behavior independent of ovarian steroids in female rodents. Mol. Endocrinol. 14, 1086–1098.
Baroncini, M., Allet, C., Leroy, D., Beauvillain, J. C., Francke, J. P., and Prevot, V. (2007). Morphological evidence for direct interaction between gonadotrophin-releasing hormone neurones and astroglial cells in the human hypothalamus. J. Neuroendocrinol. 19, 691–702.
Bellefontaine, N., Hanchate, N. K., Parkash, J., Campagne, C., de Seranno, S., Clasadonte, J., d’Anglemont de Tassigny, X., and Prevot, V. (2011). Nitric oxide as key mediator of neuron-to-neuron and endothelia-to-glia communication involved in the neuroendocrine control of reproduction. Neuroendocrinology 93, 74–89.
Bezzi, P., Carmignoto, G., Pasti, L., Vesce, S., Rossi, D., Rizzini, B. L., Pozzan, T., and Volterra, A. (1998). Prostaglandins stimulate calcium-dependent glutamate release in astrocytes. Nature 391, 281–285.
Bosetti, F. (2007). Arachidonic acid metabolism in brain physiology and pathology: lessons from genetically altered mouse models. J. Neurochem. 102, 577–586.
Botting, J. H., Linton, E. A., and Whitehead, S. A. (1977). Blockade of ovulation in the rat by a prostaglandin antogonist (N-0164). J. Endocrinol. 75, 335–336.
Brock, T. G., McNish, R. W., and Peters-Golden, M. (1999). Arachidonic acid is preferentially metabolized by cyclooxygenase-2 to prostacyclin and prostaglandin E2. J. Biol. Chem. 274, 11660–11666.
Campbell, R. E., Gaidamaka, G., Han, S. K., and Herbison, A. E. (2009). Dendro-dendritic bundling and shared synapses between gonadotropin-releasing hormone neurons. Proc. Natl. Acad. Sci. U.S.A. 106, 10835–10840.
Campbell, R. E., Han, S. K., and Herbison, A. E. (2005). Biocytin filling of adult gonadotropin-releasing hormone neurons in situ reveals extensive, spiny, dendritic processes. Endocrinology 146, 1163–1169.
Carlson, J. C., Barcikowski, B., Cargill, V., and McCracken, J. A. (1974). The blockade of LH release by indomethacin. J. Clin. Endocrinol. Metab. 39, 399–402.
Carlson, J. C., Wong, A. P., and Perrin, D. G. (1977). Luteinizing hormone secretion in the rhesus monkey and a possible role for prostaglandins. Biol. Reprod. 16, 622–626.
Cashion, A. B., Smith, M. J., and Wise, P. M. (2003). The morphometry of astrocytes in the rostral preoptic area exhibits a diurnal rhythm on proestrus: relationship to the luteinizing hormone surge and effects of age. Endocrinology 144, 274–280.
Chan, H., Prescott, M., Ong, Z., Herde, M. K., Herbison, A. E., and Campbell, R. E. (2011). Dendritic spine plasticity in gonadotropin-releasing hormone (GnRH) neurons activated at the time of the preovulatory surge. Endocrinology 152, 4906–4914.
Christian, C. A., and Moenter, S. M. (2010). The neurobiology of preovulatory and estradiol-induced gonadotropin-releasing hormone surges. Endocr. Rev. 31, 544–577.
Chu, Z., and Moenter, S. M. (2005). Endogenous activation of metabotropic glutamate receptors modulates GABAergic transmission to gonadotropin-releasing hormone neurons and alters their firing rate: a possible local feedback circuit. J. Neurosci. 25, 5740–5749.
Ciofi, P., Garret, M., Lapirot, O., Lafon, P., Loyens, A., Prevot, V., and Levine, J. E. (2009). Brain-endocrine interactions: a microvascular route in the mediobasal hypothalamus. Endocrinology 150, 5509–5519.
Clasadonte, J., Poulain, P., Hanchate, N. K., Corfas, G., Ojeda, S. R., and Prevot, V. (2011). Prostaglandin E2 release from astrocytes triggers gonadotropin-releasing hormone (GnRH) neuron firing via EP2 receptor activation. Proc. Natl. Acad. Sci. U.S.A. 108, 16104–16109.
Claypool, L. E., Kasuya, E., Saitoh, Y., Marzban, F., and Terasawa, E. (2000). N-methyl D, L-aspartate induces the release of luteinizing hormone-releasing hormone in the prepubertal and pubertal female rhesus monkey as measured by in vivo push-pull perfusion in the stalk-median eminence. Endocrinology 141, 219–228.
Coleman, R. A., Smith, W. L., and Narumiya, S. (1994). International Union of Pharmacology classification of prostanoid receptors: properties, distribution, and structure of the receptors and their subtypes. Pharmacol. Rev. 46, 205–229.
Cottrell, E. C., Campbell, R. E., Han, S. K., and Herbison, A. E. (2006). Postnatal remodeling of dendritic structure and spine density in gonadotropin-releasing hormone neurons. Endocrinology 147, 3652–3661.
Dale, N. (2011). Purinergic signaling in hypothalamic tanycytes: potential roles in chemosensing. Semin. Cell Dev. Biol. 22, 237–244.
de Seranno, S., d’Anglemont de Tassigny, X., Estrella, C., Loyens, A., Kasparov, S., Leroy, D., Ojeda, S. R., Beauvillain, J. C., and Prevot, V. (2010). Role of estradiol in the dynamic control of tanycyte plasticity mediated by vascular endothelial cells in the median eminence. Endocrinology 151, 1760–1772.
De Seranno, S., Estrella, C., Loyens, A., Cornea, A., Ojeda, S. R., Beauvillain, J. C., and Prevot, V. (2004). Vascular endothelial cells promote acute plasticity in ependymoglial cells of the neuroendocrine brain. J. Neurosci. 24, 10353–10363.
de Souza, A. S., Fernandes, F. S., and do Carmo, M. G. (2011). Effects of maternal malnutrition and postnatal nutritional rehabilitation on brain fatty acids, learning, and memory. Nutr. Rev. 69, 132–144.
DeFazio, R. A., Heger, S., Ojeda, S. R., and Moenter, S. M. (2002). Activation of A-type gamma-aminobutyric acid receptors excites gonadotropin-releasing hormone neurons. Mol. Endocrinol. 16, 2872–2891.
Di Castro, M. A., Chuquet, J., Liaudet, N., Bhaukaurally, K., Santello, M., Bouvier, D., Tiret, P., and Volterra, A. (2011). Local Ca(2+) detection and modulation of synaptic release by astrocytes. Nat. Neurosci. 14, 1276–1284.
Donato, J. Jr., Cravo, R. M., Frazao, R., and Elias, C. F. (2011). Hypothalamic sites of leptin action linking metabolism and reproduction. Neuroendocrinology 93, 9–18.
Donoso, A. O., Lopez, F. J., and Negro-Vilar, A. (1990). Glutamate receptors of the non-N-methyl-D-aspartic acid type mediate the increase in luteinizing hormone-releasing hormone release by excitatory amino acids in vitro. Endocrinology 126, 414–420.
Dziedzic, B., Prevot, V., Lomniczi, A., Jung, H., Cornea, A., and Ojeda, S. R. (2003). Neuron-to-glia signaling mediated by excitatory amino acid receptors regulates ErbB receptor function in astroglial cells of the neuroendocrine brain. J. Neurosci. 23, 915–926.
Eroglu, C., and Barres, B. A. (2010). Regulation of synaptic connectivity by glia. Nature 468, 223–231.
Eskay, R. L., Warberg, J., Mical, R. S., and Porter, J. C. (1975). Prostaglandin E2-induced release of LHRH into hypophysial portal blood(1). Endocrinology 97, 816–824.
Fonnum, F., Johnsen, A., and Hassel, B. (1997). Use of fluorocitrate and fluoroacetate in the study of brain metabolism. Glia 21, 106–113.
Gallardo, E., and Ramirez, V. D. (1977). A method for the superfusion of rat hypothalami: secretion of luteinizing hormone-releasing hormone. Proc. Soc. Exp. Biol. Med. 155, 79–84.
Garcia-Segura, L. M., and McCarthy, M. M. (2004). Minireview: role of glia in neuroendocrine function. Endocrinology 145, 1082–1086.
Gearing, M., and Terasawa, E. (1991). Prostaglandin E2 mediates the stimulatory effect of methoxamine on in vivo luteinizing hormone-releasing hormone (LH-RH) release in the ovariectomized female rhesus monkey. Brain Res. 560, 276–281.
Glanowska, K. M., and Moenter, S. M. (2011). Endocannabinoids and prostaglandins both contribute to gonadotropin-releasing hormone (GnRH) neuron-GABAergic afferent local feedback circuits. J. Neurophysiol. doi: 10.1152/jn.00046.2011. [Epub ahead of print].
Gordon, G. R., Iremonger, K. J., Kantevari, S., Ellis-Davies, G. C., MacVicar, B. A., and Bains, J. S. (2009). Astrocyte-mediated distributed plasticity at hypothalamic glutamate synapses. Neuron 64, 391–403.
Halassa, M. M., and Haydon, P. G. (2010). Integrated brain circuits: astrocytic networks modulate neuronal activity and behavior. Annu. Rev. Physiol. 72, 335–355.
Han, S. K., Abraham, I. M., and Herbison, A. E. (2002). Effect of GABA on GnRH neurons switches from depolarization to hyperpolarization at puberty in the female mouse. Endocrinology 143, 1459–1466.
Harms, P. G., Ojeda, S. R., and McCann, S. M. (1973). Prostaglandin involvement in hypothalamic control of gonadotropin and prolactin release. Science 181, 760–761.
Hatton, G. I. (1997). Function-related plasticity in hypothalamus. Annu. Rev. Neurosci. 20, 375–397.
Hatton, G. I., and Wang, Y. F. (2008). Neural mechanisms underlying the milk ejection burst and reflex. Prog. Brain Res. 170, 155–166.
Haydon, P. G., and Carmignoto, G. (2006). Astrocyte control of synaptic transmission and neurovascular coupling. Physiol. Rev. 86, 1009–1031.
Henneberger, C., Papouin, T., Oliet, S. H., and Rusakov, D. A. (2010). Long-term potentiation depends on release of D-serine from astrocytes. Nature 463, 232–236.
Herbison, A. E., and Moenter, S. M. (2011). Depolarising and hyperpolarising actions of GABA(A) receptor activation on gonadotrophin-releasing hormone neurones: towards an emerging consensus. J. Neuroendocrinol. 23, 557–569.
Herbison, A. E., and Neill, J. D. (2006). “Physiology of the gonadotropin-releasing hormone neuronal network,” in Knobil and Neill’s Physiology of Reproduction, 3rd Edn, eds E. Knobil, and J. D. Neill (New York: Elsevier), 1415–1482.
Hirst, W. D., Young, K. A., Newton, R., Allport, V. C., Marriott, D. R., and Wilkin, G. P. (1999). Expression of COX-2 by normal and reactive astrocytes in the adult rat central nervous system. Mol. Cell. Neurosci. 13, 57–68.
Hrabovszky, E., and Liposits, Z. (2008). Novel aspects of glutamatergic signalling in the neuroendocrine system. J. Neuroendocrinol. 20, 743–751.
Hynes, N. E., and Lane, H. A. (2005). ERBB receptors and cancer: the complexity of targeted inhibitors. Nat. Rev. Cancer 5, 341–354.
Iadecola, C., and Nedergaard, M. (2007). Glial regulation of the cerebral microvasculature. Nat. Neurosci. 10, 1369–1376.
Jasoni, C. L., Todman, M. G., Han, S. K., and Herbison, A. E. (2005). Expression of mRNAs encoding receptors that mediate stress signals in gonadotropin-releasing hormone neurons of the mouse. Neuroendocrinology 82, 320–328.
Junier, M. P., Ma, Y. J., Costa, M. E., Hoffman, G., Hill, D. F., and Ojeda, S. R. (1991). Transforming growth factor alpha contributes to the mechanism by which hypothalamic injury induces precocious puberty. Proc. Natl. Acad. Sci. U.S.A. 88, 9743–9747.
King, J. C., and Letourneau, R. J. (1994). Luteinizing hormone-releasing hormone terminals in the median eminence of rats undergo dramatic changes after gonadectomy, as revealed by electron microscopic image analysis. Endocrinology 134, 1340–1351.
Kozlowski, G. P., and Coates, P. W. (1985). Ependymoneuronal specializations between LHRH fibers and cells of the cerebroventricular system. Cell Tissue Res. 242, 301–311.
Labhsetwar, A. P., and Zolovick, A. (1973). Hypothalamic interaction between prostaglandins and catecholamines in promoting gonadotropin secretion for ovulation. Nature New Biol. 246, 55–56.
Lauritzen, L., and Carlson, S. E. (2011). Maternal fatty acid status during pregnancy and lactation and relation to newborn and infant status. Matern. Child Nutr. 7(Suppl. 2), 41–58.
Levine, J. E., and Ramirez, V. D. (1982). Luteinizing hormone-releasing hormone release during the rat estrous cycle and after ovariectomy, as estimated with push-pull cannulae. Endocrinology 111, 1439–1448.
Ma, Y. J., Berg-von der Emde, K., Moholt-Siebert, M., Hill, D. F., and Ojeda, S. R. (1994a). Region-specific regulation of transforming growth factor alpha (TGF alpha) gene expression in astrocytes of the neuroendocrine brain. J. Neurosci. 14, 5644–5651.
Ma, Y. J., Hill, D. F., Junier, M. P., Costa, M. E., Felder, S. E., and Ojeda, S. R. (1994b). Expression of epidermal growth factor receptor changes in the hypothalamus during the onset of female puberty. Mol. Cell. Neurosci. 5, 246–262.
Ma, Y. J., Berg-von der Emde, K., Rage, F., Wetsel, W. C., and Ojeda, S. R. (1997). Hypothalamic astrocytes respond to transforming growth factor-alpha with the secretion of neuroactive substances that stimulate the release of luteinizing hormone-releasing hormone. Endocrinology 138, 19–25.
Ma, Y. J., Hill, D. F., Creswick, K. E., Costa, M. E., Cornea, A., Lioubin, M. N., Plowman, G. D., and Ojeda, S. R. (1999). Neuregulins signaling via a glial erbB-2-erbB-4 receptor complex contribute to the neuroendocrine control of mammalian sexual development. J. Neurosci. 19, 9913–9927.
Ma, Y. J., Junier, M. P., Costa, M. E., and Ojeda, S. R. (1992). Transforming growth factor-alpha gene expression in the hypothalamus is developmentally regulated and linked to sexual maturation. Neuron 9, 657–670.
Mahesh, V. B., Dhandapani, K. M., and Brann, D. W. (2006). Role of astrocytes in reproduction and neuroprotection. Mol. Cell. Endocrinol. 246, 1–9.
Malpaux, B. (2006). “Seasonal regulation in mammals,” in Knobil and Neill’s Physiology of Reproduction, eds E. Knobil, and J. D. Neill (New York: Raven Press).
Martineau, M., Baux, G., and Mothet, J. P. (2006). D-serine signalling in the brain: friend and foe. Trends Neurosci. 29, 481–491.
Mayer, C., Acosta-Martinez, M., Dubois, S. L., Wolfe, A., Radovick, S., Boehm, U., and Levine, J. E. (2010). Timing and completion of puberty in female mice depend on estrogen receptor alpha-signaling in kisspeptin neurons. Proc. Natl. Acad. Sci. U.S.A. 107, 22693–22698.
McCarthy, M. M., Schwarz, J. M., Wright, C. L., and Dean, S. L. (2008). Mechanisms mediating oestradiol modulation of the developing brain. J. Neuroendocrinol. 20, 777–783.
Meister, B., Hokfelt, T., Tsuruo, Y., Hemmings, H., Ouimet, C., Greengard, P., and Goldstein, M. (1988). DARPP-32, a dopamine- and cyclic AMP-regulated phosphoprotein in tanycytes of the mediobasal hypothalamus: distribution and relation to dopamine and luteinizing hormone-releasing hormone neurons and other glial elements. Neuroscience 27, 607–622.
Melcangi, R. C., Martini, L., and Galbiati, M. (2002). Growth factors and steroid hormones: a complex interplay in the hypothalamic control of reproductive functions. Prog. Neurobiol. 67, 421–449.
Milatovic, D., Montine, T. J., and Aschner, M. (2011). Prostanoid signaling: dual role for prostaglandin E2 in neurotoxicity. Neurotoxicology 32, 312–319.
Mong, J. A., and Blutstein, T. (2006). Estradiol modulation of astrocytic form and function: implications for hormonal control of synaptic communication. Neuroscience 138, 967–975.
Mullier, A., Bouret, S. G., Prevot, V., and Dehouck, B. (2010). Differential distribution of tight junction proteins suggests a role for tanycytes in blood-hypothalamus barrier regulation in the adult mouse brain. J. Comp. Neurol. 518, 943–962.
Murai, K. K., Nguyen, L. N., Irie, F., Yamaguchi, Y., and Pasquale, E. B. (2003). Control of hippocampal dendritic spine morphology through ephrin-A3/EphA4 signaling. Nat. Neurosci. 6, 153–160.
Negro-Vilar, A., Ojeda, S. R., and McCann, S. M. (1979). Catecholaminergic modulation of luteinizing hormone-releasing hormone release by median eminence terminals in vitro. Endocrinology 104, 1749–1757.
Nishida, H., and Okabe, S. (2007). Direct astrocytic contacts regulate local maturation of dendritic spines. J. Neurosci. 27, 331–340.
Ojeda, S. R., and Campbell, W. B. (1982). An increase in hypothalamic capacity to synthesize prostaglandin E2 precedes the first preovulatory surge of gonadotropins. Endocrinology 111, 1031–1037.
Ojeda, S. R., Harms, P. G., and McCann, S. M. (1975a). Effect of inhibitors of prostaglandin synthesis on gonadotropin release in the rat. Endocrinology 97, 843–854.
Ojeda, S. R., Wheaton, J. E., and McCann, S. M. (1975b). Prostaglandin E2-induced release of luteinizing hormone-releasing factor (LRF). Neuroendocrinology 17, 283–287.
Ojeda, S. R., Jameson, H. E., and McCann, S. M. (1977). Hypothalamic areas involved in prostaglandin (PG)-induced gonadotropin release. I: effects of PGE2 and PGF2alpha implants on luteinizing hormone release. Endocrinology 100, 1585–1594.
Ojeda, S. R., Lomniczi, A., and Sandau, U. S. (2008). Glial-gonadotrophin hormone (GnRH) neurone interactions in the median eminence and the control of GnRH secretion. J. Neuroendocrinol. 20, 732–742.
Ojeda, S. R., and Negro-Vilar, A. (1985). Prostaglandin E2-induced luteinizing hormone-releasing hormone release involves mobilization of intracellular Ca+2. Endocrinology 116, 1763–1770.
Ojeda, S. R., Negro-Vilar, A., and McCann, S. M. (1979). Release of prostaglandin Es by hypothalamic tissue: evidence for their involvement in catecholamine-induced luteinizing hormone-releasing hormone release. Endocrinology 104, 617–624.
Ojeda, S. R., Negro-Vilar, A., and McCann, S. M. (1982). Evidence for involvement of alpha-adrenergic receptors in norepinephrine-induced prostaglandin E2 and luteinizing hormone-releasing hormone release from the median eminence. Endocrinology 110, 409–412.
Ojeda, S. R., and Skinner, M. K. (2006). “Puberty in the rat,” in Knobil and Neill’s Physiology of Reproduction, ed. J. D. Neill (San Diego: Academic Press), 2026–2126.
Ojeda, S. R., Urbanski, H. F., Costa, M. E., Hill, D. F., and Moholt-Siebert, M. (1990). Involvement of transforming growth factor alpha in the release of luteinizing hormone-releasing hormone from the developing female hypothalamus. Proc. Natl. Acad. Sci. U.S.A. 87, 9698–9702.
Ojeda, S. R., Urbanski, H. F., Katz, K. H., and Costa, M. E. (1985). Stimulation of cyclic adenosine 3′,5′-monophosphate production enhances hypothalamic luteinizing hormone-releasing hormone release without increasing prostaglandin E2 synthesis: studies in prepubertal female rats. Endocrinology 117, 1175–1178.
Ojeda, S. R., Urbanski, H. F., Katz, K. H., and Costa, M. E. (1986a). Activation of estradiol-positive feedback at puberty: estradiol sensitizes the LHRH-releasing system at two different biochemical steps. Neuroendocrinology 43, 259–265.
Ojeda, S. R., Urbanski, H. F., Katz, K. H., Costa, M. E., and Conn, P. M. (1986b). Activation of two different but complementary biochemical pathways stimulates release of hypothalamic luteinizing hormone-releasing hormone. Proc. Natl. Acad. Sci. U.S.A. 83, 4932–4936.
Ojeda, S. R., Urbanski, H. F., Katz, K. H., and Costa, M. E. (1988). Prostaglandin E2 releases luteinizing hormone-releasing hormone from the female juvenile hypothalamus through a Ca2+-dependent, calmodulin-independent mechanism. Brain Res. 441, 339–351.
Oliet, S. H., and Bonfardin, V. D. (2010). Morphological plasticity of the rat supraoptic nucleus – cellular consequences. Eur. J. Neurosci. 32, 1989–1994.
Page, R. B. (1994). “The anatomy of the hypothalamo-hypophysial complex,” in The Physiology of Reproduction, eds E. Knobil, and J. D. Neill (New York: Raven Press), 1527–1619.
Panatier, A. (2009). Glial cells: indispensable partners of hypothalamic magnocellular neurones. J. Neuroendocrinol. 21, 665–672.
Panatier, A., Vallee, J., Haber, M., Murai, K. K., Lacaille, J. C., and Robitaille, R. (2011). Astrocytes are endogenous regulators of basal transmission at central synapses. Cell 146, 785–798.
Parpura, V., and Zorec, R. (2010). Gliotransmission: exocytotic release from astrocytes. Brain Res. Rev. 63, 83–92.
Pfrieger, F. W. (2010). Role of glial cells in the formation and maintenance of synapses. Brain Res. Rev. 63, 39–46.
Plant, T. M. (2006). “Puberty in non-human primates and humans,” in Knobil and Neill’s Physiology of Reproduction, ed. J. D. Neill (San Diego: Academic Press), 2177–2230.
Plant, T. M., Gay, V. L., Marshall, G. R., and Arslan, M. (1989). Puberty in monkeys is triggered by chemical stimulation of the hypothalamus. Proc. Natl. Acad. Sci. U.S.A. 86, 2506–2510.
Prevot, V. (2002). Glial-neuronal-endothelial interactions are involved in the control of GnRH secretion. J. Neuroendocrinol. 14, 247–255.
Prevot, V., Bellefontaine, N., Baroncini, M., Sharif, A., Hanchate, N. K., Parkash, J., Campagne, C., and de Seranno, S. (2010a). GnRH nerve terminals, tanycytes and neurohaemal junction remodeling in the adult median eminence: functional consequences for reproduction and dynamic role of vascular endothelial cells. J. Neuroendocrinol. 22, 639–649.
Prevot, V., Hanchate, N. K., Bellefontaine, N., Sharif, A., Parkash, J., Estrella, C., Allet, C., de Seranno, S., Campagne, C., de Tassigny, X., and Baroncini, M. (2010b). Function-related structural plasticity of the GnRH system: a role for neuronal-glial-endothelial interactions. Front. Neuroendocrinol. 31, 241–258.
Prevot, V., Cornea, A., Mungenast, A., Smiley, G., and Ojeda, S. R. (2003a). Activation of erbB-1 signaling in tanycytes of the median eminence stimulates transforming growth factor beta1 release via prostaglandin E2 production and induces cell plasticity. J. Neurosci. 23, 10622–10632.
Prevot, V., Rio, C., Cho, G. J., Lomniczi, A., Heger, S., Neville, C. M., Rosenthal, N. A., Ojeda, S. R., and Corfas, G. (2003b). Normal female sexual development requires neuregulin-erbB receptor signaling in hypothalamic astrocytes. J. Neurosci. 23, 230–239.
Prevot, V., Croix, D., Bouret, S., Dutoit, S., Tramu, G., Stefano, G. B., and Beauvillain, J. C. (1999). Definitive evidence for the existence of morphological plasticity in the external zone of the median eminence during the rat estrous cycle: implication of neuro-glio-endothelial interactions in gonadotropin-releasing hormone release. Neuroscience 94, 809–819.
Prevot, V., Dutoit, S., Croix, D., Tramu, G., and Beauvillain, J. C. (1998). Semi-quantitative ultrastructural analysis of the localization and neuropeptide content of gonadotropin releasing hormone nerve terminals in the median eminence throughout the estrous cycle of the rat. Neuroscience 84, 177–191.
Prevot, V., Lomniczi, A., Corfas, G., and Ojeda, S. R. (2005). erbB-1 and erbB-4 receptors act in concert to facilitate female sexual development and mature reproductive function. Endocrinology 146, 1465–1472.
Rage, F., Lee, B. J., Ma, Y. J., and Ojeda, S. R. (1997). Estradiol enhances prostaglandin E2 receptor gene expression in luteinizing hormone-releasing hormone (LHRH) neurons and facilitates the LHRH response to PGE2 by activating a glia-to-neuron signaling pathway. J. Neurosci. 17, 9145–9156.
Raskin, K., de Gendt, K., Duittoz, A., Liere, P., Verhoeven, G., Tronche, F., and Mhaouty-Kodja, S. (2009). Conditional inactivation of androgen receptor gene in the nervous system: effects on male behavioral and neuroendocrine responses. J. Neurosci. 29, 4461–4470.
Rettori, V., Gimeno, M., Lyson, K., and McCann, S. M. (1992). Nitric oxide mediates norepinephrine-induced prostaglandin E2 release from the hypothalamus. Proc. Natl. Acad. Sci. U.S.A. 89, 11543–11546.
Roland, A. V., and Moenter, S. M. (2011). Glucosensing by GnRH neurons: inhibition by androgens and involvement of AMP-activated protein kinase. Mol. Endocrinol. 25, 847–858.
Ronnekleiv, O. K., and Kelly, M. J. (2005). Diversity of ovarian steroid signaling in the hypothalamus. Front. Neuroendocrinol. 26, 65–84.
Sandau, U. S., Mungenast, A. E., McCarthy, J., Biederer, T., Corfas, G., and Ojeda, S. R. (2011a). The synaptic cell adhesion molecule, SynCAM1, mediates astrocyte-to-astrocyte and astrocyte-to-GnRH neuron adhesiveness in the mouse hypothalamus. Endocrinology 152, 2353–2363.
Sandau, U. S., Mungenast, A. E., Alderman, Z., Sardi, S. P., Fogel, A. I., Taylor, B., Parent, A. S., Biederer, T., Corfas, G., and Ojeda, S. R. (2011b). SynCAM1, a synaptic adhesion molecule, is expressed in astrocytes and contributes to erbB4 receptor-mediated control of female sexual development. Endocrinology 152, 2364–2376.
Sang, N., Zhang, J., Marcheselli, V., Bazan, N. G., and Chen, C. (2005). Postsynaptically synthesized prostaglandin E2 (PGE2) modulates hippocampal synaptic transmission via a presynaptic PGE2 EP2 receptor. J. Neurosci. 25, 9858–9870.
Sharif, A., Duhem-Tonnelle, V., Allet, C., Baroncini, M., Loyens, A., Kerr-Conte, J., Collier, F., Blond, S., Ojeda, S. R., Junier, M. P., and Prevot, V. (2009). Differential erbB signaling in astrocytes from the cerebral cortex and the hypothalamus of the human brain. Glia 57, 362–379.
Sharif, A., and Prevot, V. (2010). ErbB receptor signaling in astrocytes: a mediator of neuron-glia communication in the mature central nervous system. Neurochem. Int. 57, 344–358.
Sild, M., and Ruthazer, E. S. (2011). Radial glia: progenitor, pathway, and partner. Neuroscientist 17, 288–302.
Smith, S. S., Neuringer, M., and Ojeda, S. R. (1989). Essential fatty acid deficiency delays the onset of puberty in the female rat. Endocrinology 125, 1650–1659.
Terasawa, E., and Fernandez, D. L. (2001). Neurobiological mechanisms of the onset of puberty in primates. Endocr. Rev. 22, 111–151.
Theodosis, D. T., Poulain, D. A., and Oliet, S. H. (2008). Activity-dependent structural and functional plasticity of astrocyte-neuron interactions. Physiol. Rev. 88, 983–1008.
Ugrumov, M., Hisano, S., and Daikoku, S. (1989). Topographic relations between tyrosine hydroxylase- and luteinizing hormone-releasing hormone-immunoreactive fibers in the median eminence of adult rats. Neurosci. Lett. 102, 159–164.
Urbanski, H. F., and Ojeda, S. R. (1987). Activation of luteinizing hormone-releasing hormone release advances the onset of female puberty. Neuroendocrinology 46, 273–276.
Urbanski, H. F., and Ojeda, S. R. (1990). A role for N-methyl-D-aspartate (NMDA) receptors in the control of LH secretion and initiation of female puberty. Endocrinology 126, 1774–1776.
van den Pol, A. N., and Trombley, P. Q. (1993). Glutamate neurons in hypothalamus regulate excitatory transmission. J. Neurosci. 13, 2829–2836.
Vidensky, S., Zhang, Y., hand, T., Goellner, J., Shaffer, A., Isakson, P., and Andreasson, K. (2003). Neuronal overexpression of COX-2 results in dominant production of PGE2 and altered fever response. Neuromolecular Med. 3, 15–28.
Voigt, P., Ma, Y. J., Gonzalez, D., Fahrenbach, W. H., Wetsel, W. C., Berg-von der, E. K., Hill, D. F., Taylor, K. G., Costa, M. E., Seidah, N. G., and Ojeda, S. R. (1996). Neural and glial-mediated effects of growth factors acting via tyrosine kinase receptors on luteinizing hormone-releasing hormone neurons. Endocrinology 137, 2593–2605.
Wintermantel, T. M., Campbell, R. E., Porteous, R., Bock, D., Grone, H. J., Todman, M. G., Korach, K. S., Greiner, E., Perez, C. A., Schutz, G., and Herbison, A. E. (2006). Definition of estrogen receptor pathway critical for estrogen positive feedback to gonadotropin-releasing hormone neurons and fertility. Neuron 52, 271–280.
Witkin, J. W., O’Sullivan, H., and Ferin, M. (1995). Glial ensheathment of GnRH neurons in pubertal female rhesus macaques. J. Neuroendocrinol. 7, 665–671.
Woolley, C. S., and McEwen, B. S. (1992). Estradiol mediates fluctuation in hippocampal synapse density during the estrous cycle in the adult rat. J. Neurosci. 12, 2549–2554.
Woolley, C. S., and McEwen, B. S. (1994). Estradiol regulates hippocampal dendritic spine density via an N-methyl-D-aspartate receptor-dependent mechanism. J. Neurosci. 14, 7680–7687.
Wright, C. L., and McCarthy, M. M. (2009). Prostaglandin E2-induced masculinization of brain and behavior requires protein kinase A, AMPA/kainate, and metabotropic glutamate receptor signaling. J. Neurosci. 29, 13274–13282.
Yin, W., and Gore, A. C. (2010). The hypothalamic median eminence and its role in reproductive aging. Ann. N. Y. Acad. Sci. 1204, 113–122.
Zhang, C., Roepke, T. A., Kelly, M. J., and Rønnekleiv, O. K. (2008). Kisspeptin depolarizes gonadotropin-releasing hormone neurons through activation of TRPC-like cationic channels. J. Neurosci. 28, 4423–4434.
Zonta, M., Sebelin, A., Gobbo, S., Fellin, T., Pozzan, T., and Carmignoto, G. (2003a). Glutamate-mediated cytosolic calcium oscillations regulate a pulsatile prostaglandin release from cultured rat astrocytes. J. Physiol. (Lond.) 553, 407–414.
Keywords: gliotransmitter, cyclooxygenase, nitric oxide, hypothalamus, reproduction
Citation: Clasadonte J, Sharif A, Baroncini M and Prevot V (2011) Gliotransmission by prostaglandin E2: a prerequisite for GnRH neuronal function? Front. Endocrin. 2:91. doi: 10.3389/fendo.2011.00091
Received: 24 October 2011; Paper pending published: 16 November 2011;
Accepted: 17 November 2011; Published online: 08 December 2011.
Edited by:
Carol F. Elias, University of Texas Southwestern Medical Center, USAReviewed by:
Sue Moenter, University of Michigan, USARebecca E. Campbell, University of Otago, New Zealand
Copyright: © 2011 Clasadonte, Sharif, Baroncini and Prevot. This is an open-access article distributed under the terms of the Creative Commons Attribution Non Commercial License, which permits non-commercial use, distribution, and reproduction in other forums, provided the original authors and source are credited.
*Correspondence: Vincent Prevot, INSERM U837, Bâtiment Biserte, Place de Verdun, 59045 Lille Cedex, France. e-mail:dmluY2VudC5wcmV2b3RAaW5zZXJtLmZy

 Ariane Sharif1,2,3
Ariane Sharif1,2,3