Abstract
Augmented and virtual reality (AR/VR) technologies are regularly used in psychology research to complement psychological interventions and to enable an individual to feel as if they are in an environment other than that of their immediate surroundings. A scoping review was performed to identify how AR/VR was being used with older adult populations to impact their physical and mental health. The review also sought to determine whether the terminology used in AR/VR research was consistent. The results show that 65 studies have been published in the last 20 years that meet the inclusion criteria (virtual/augmented reality) technology to impact older adults’ physical/mental health and wellbeing. Participants included healthy, physically, and cognitively impaired, and emotionally vulnerable older adults. We argue that over 70% of the studies included in this review were mislabeled as VR and only six papers included fully immersive VR/AR. The remaining studies use less immersive variants of virtual reality with their populations, and only one study made use of AR, which prompted the suggestion of a new definition for virtual reality. This paper also calls for an updated taxonomy of augmented and virtual reality definitions to address the lack of consistency found in studies that identify themselves as AR/VR when they are using less immersive technical set-ups, including displaying non-interactive videos on 2D screens.
Background
The development and impact of virtual and augmented technologies has been examined since the early 60s (Eckert et al., 2019, p. 2). In their current evolution, they provide digital interaction in space. There are many complementary definitions of both terms though the most comprehensive are from McCoy and Stone (2001) and Botella et al. (2015). Virtual reality is “a collection of technologies that allow people to interact efficiently with 3D computerized databases in real time using their natural senses and skills” (McCoy and Stone, 2001, p. 912), whereas augmented reality “combines the real world with virtual elements, using computer graphics mixed with the real world in real time” (Botella et al., 2015, p. 2). Both definitions emphasize the importance of real-time interaction while also establishing their fundamental differences. Virtual reality immerses the user in a digital environment whereas augmented reality enhances the world around the user. Virtual technologies (hereafter referred to as AR/VR), have been incorporated into many areas of psychological research including exposure therapy (Riva et al., 2019, p. 82), pain management (Wiederhold, 2016, p. 577), and even diagnostic proficiency (Tarnanas et al., 2015, p. 12).
The use of AR/VR in older adult populations is often used as a form of Positive technology. This is the application of creative technologies for the benefit of personal experience (Botella et al., 2012, p. 78) through its structuring, augmentation and/or replacement” (Kitson et al., 2018, p. 3). When used to support user engagement, it enhances the environment and supports a person in new ways that better reflect their needs (Graffigna et al., 2013, p. 1). Functions of positive technologies include, encouraging positive emotions, promoting engagement and self-empowerment, and increasing social integration and connectedness (Wiederhold and Riva, 2012, p. 67). Each area can be promoted, affected, and facilitated by AR/VR and, the more interesting or compelling the virtual environment, the greater the enjoyment which can lead directly to increase motivation (Rizzo and Kim, 2005). Given that the population of adults over 65 in the EU27 (member states of the European Union) is expected to increase by 8.9% (Eurostat, 2020) by 2050, new and innovative ways to use AR/VR has become a tenet of research to support older adults to live independently at home for as long as possible (Wiederhold, 2020, p. 141). AR/VR physical activity programs have been successful in terms of increasing physical activity and strength and by influencing the motivations that drive these positive behaviors (Ng et al., 2019, p. 280). These interventions, underpinned by social cognitive theory, can effectively act as supplementary supports to physical actions. Through the observation of “others” or “oneself” in the digital environment, the user can learn and reinforce behaviors. Further research of the effects of intrinsic and extrinsic motivations in AR/VR interventions, is needed. While there are many studies that use AR/VR to impact physical and social factors in varied populations (Tarnanas et al., 2015, p. 2; Wiederhold, 2016; Riva et al., 2019, p. 82, p. 577), there is very little standardization or consistency in the terminology used to describe the technology. This has led to a call to unify definitions by (Kardong-Edgren et al., 2019, p. 29) and this review aims to address some of the gaps highlighted by the researchers.
“Virtual” Behavior Change Theory
Over the last decade virtual reality research has made the leap from “toy” to serious research tool (Stadler et al., 2019, p. 207). Several theories (Riva et al., 2016, p. 2–3) can be used to justify the inclusion and success of virtual interventions and this is important as many interventions have been found to provide inadequate theoretical support for their behavior change interventions (Michie et al., 2014). Perceptual Control Theory (Parker et al., 2020, p. 616) argues that participants occupied with a goal state interact with a digital environment and receive perceptual updates of their progress. Until their current perceptual state matches their goal state, they will receive “error” feedback, prompting them to continue until congruence is achieved. Self-affirmation theory (Velez and Hanus, 2016, p. 721–722) also supports the effectiveness of virtual interventions. During a virtual intervention, participants are often faced with negative information relevant to themselves. Researchers will prompt participants to change these behaviors in response to the intervention, but this can threaten the positive aspects of self-identity so virtual interventions often include positive encouragement to bolster important aspects of self-identity. This positive reinforcement facilitated by the virtual environment (e.g., gaining points in a virtual game) allows participants to fully engage with, and internalize the purpose of, the intervention. The Transtheoretical Model of Behavior Change (Yu-Leung et al., 2019, p. 287) states that there are six stages of health-related behavior change that hold true in both physical and virtual settings. These shifts in attitude are a useful indicator to researchers developing virtual interventions when compared to participants’ prior experience and interest. Finally, Transformative Learning Theory (Huth et al., 2020, p. 1026), unlike self-affirmation theory, suggests that a pre-existing view evolves in response to a conflicting situation. The participant can reflect and engage with the situation in the virtual environment and experience a fundamental shift in perspective.
Rationale for Scoping Review
To date, approximately 19 meta-analyses and systematic reviews (See Supplementary Table S1) have examined the effects of VR on older populations, yet none have investigated the impact of AR in this population. Smart health technologies can benefit the cognitive, emotional, physical, and social domains of day-to-day living (Guisado-Fernández et al., 2019, p. 7–8). As such, illuminating the relationship between AR/VR, older adults and physical and mental health is essential.
Two research questions were posed in this scoping review.
1. How is AR/VR technology currently used in research with older adults to assess and/or improve physical and mental health and general wellbeing?
2. Is consistent terminology used across these studies and if not, what are the inconsistencies, and can this evaluation identify (or construct) a definition that will advance or improve understanding?
Methods
Protocol
The PRISMA Extension for Scoping Reviews (Tricco et al., 2018, p. 4) was guides this review. We selected this framework given the variety of AR/VR technologies in research use, the numerous ways the technology is described, and the need to establish what and how research is conducted to enable appropriate systematic reviews to take place. Our aim is to create a resource for researchers interested in conducting AR/VR research with older adult populations in physical and mental health settings. As AR/VR terminology is multi-varied and (often) used interchangeably, this paper will summarize how these terms are being used and offer a rationale for why they are/are not being used correctly.
Search Keywords and Databases
A comprehensive list of search terms was created to address the three areas of interest in this review: AR/VR, older adults, physical/mental health, and wellbeing. The literature search was conducted on March 24th, 2020 across the following licenced databases: Academic Search Complete, CINAHL, PsycINFO, PsycArticles and Medline. Primary studies with all types of designs were included along with all types of reviews. Table 1 illustrates the key and related search terms used. Terms were combined using the Boolean Operators.
TABLE 1
| # | Search Term | Results | Year |
|---|---|---|---|
| S1 | Virtual Reality OR VR OR Augmented Reality OR AR, OR Augment* AND Reality OR Interreality OR Heads-Up* AND VIRTUAL REALITY or AUGMENTED REALITY Marker* AND virtual reality OR Augmented Reality OR Projection* AND virtual reality OR Augmented Reality OR Superimposition AND virtual reality OR Augmented Reality OR Holo* AND virtual reality OR Augmented Reality OR Tangible AND virtual reality OR Augmented Reality OR Mixed AND virtual reality OR Augmented AND Reality | 437,212 | 1806 - 2020 |
| S2 | Older adults OR elderly OR geriatric OR geriatrics OR aging OR senior OR seniors OR older people OR aged 65 OR 65+ OR age related OR old age OR elder OR mature adult OR oldest old OR aged adult OR Late Life OR Retirement OR retired OR End of life* OR Older people OR older population OR OAP or OAPs OR Pensioner OR pensioners OR vulnerable elderly | 3,200,549 | 1597 – 2021 |
| S3 | Physical health or physical wellbeing or health OR Physical activity or exercise or fitness or physical exercise OR physical therapy or physiotherapy or rehabilitation OR Balance OR Posture OR Fall prevention OR Mental Health OR Wellbeing or well-being or well being or wellness OR Mindfulness Dementia or alzheimers or Parkinson or cognitive impairment or memory or mild cognitive impairment OR emotional health OR Psychological Health OR depression or anxiety OR Psychiatr* OR Psychol* | 20,291,326 | 1597 – 2021 |
| S4 | S1 AND S2 AND S3 | 3,061 | 1926 – 2020 |
| S5 | S4 limited by year | 2,789 | 2000 – 2020 |
| S6 | S5 limited by age: aged: 65+years. Aged, 80 and over Aged (65yrs & older) Very old (85 yrs. & older) Aged, 80 & over | 1,1014 | 2000 – 2020 |
| S7 | S6 Limited to Scholarly (Peer Reviewed) Journals only | 984 | 2000 – 2020 |
| Duplicates Removed | 74 | ||
| Title/Abstract Screening | YES | 91 | |
| NO | 721 | ||
| C1 (Diagnostic) | 24 | ||
| C3 (AR/VR used tool / not intervention | 42 | ||
| R (Review) | 32 | ||
| Total | 910 |
Academic Search Complete + CINAHL Complete + MEDLINE + PsychArticles + PsychINFO – 24/03/2020
Inclusion and Exclusion Criteria
Articles were included if the target group were aged 60+°years, a common threshold for research in this field. If a study had participants of various ages, data relating to the older adults must have been presented separately to be included. All articles using terms such as “virtual,” “augmented” and/or “mixed” reality where included. Finally, articles were only included if they investigated physical/mental health, wellbeing and AR/VR was used as part of their intervention. Articles were excluded if they did not meet the above criteria, if they did not include an active intervention or if they were published abstracts (where no paper was submitted), book reviews, opinion articles, commentaries, letters, editorials, interviews, lectures, legal cases, newspaper articles, or patient education handouts. Articles published from January 1999 to March 2020 were considered so that the review would not only contain recent studies, but also those from the early 2000s (the emergence of modern 3D virtual and augmented reality technologies) and the 00s (when Virtools VR Pack was released, which supported development of virtual environments in immersive spaces such as CAVE’s and HMD’s such as the Oculus Rift). Finally, only articles published in English were included as accurate translation would not be possible in the review timeframe.
Data Sorting and Analysis
Two reviewers screened for title and abstract, and full text reviews. Each reviewer conducted their screening individually, conflicts were discussed, and a final decision made. If any articles were not agreed upon, they were sent to a third party for arbitration. Data from full-text review was charted using the following headings: Title, citation, hypothesis, research question, aim, study design, participant details, methodology, procedure, country, results, conclusions, hardware used, software used, classification of AR/VR and, definitions used. Following the same procedure, reviewers also classified each article as: 1) Immersive VR; 2) Non-Immersive VR; 3) 2D VR; or 4) AR. Classifications were determined separately and a consensus was achieved through discussion.
Results
The literature revealed 984 studies. From this, 74 duplicates were removed. After screening titles and abstracts of the remaining 910 articles, 91 articles were brought forward for full-text review. After review, 52 studies were included in this study (See Figure 1). A further 13 articles were incorporated into this study based on a review of the references included in three systematic reviews identified in our search. The final number of articles included in this review was 65. The most common reasons for exclusion were participants under the age of 60 and studies that did not include an active intervention. Two reviewers screened results at all stages of screening and disagreements were found in approximately 7.5% of cases on average.
FIGURE 1

Scoping Review-Augmented/Virtual Interventions - Study Flow Chart.
Characteristics of the Participants
For a detailed overview of the virtual and augmented reality characteristics included in the 65 studies, please see Table 2. Across the 65 studies identified, there was an average of 65 participants (Range 7–664) with a mean age of 67.63 (SD 8.45). Each study investigated older populations except three that compared older and younger adults. Four studies provided a participant age range (60–90+) and just one study specified a population over 60. Most studies included male and female participants however 13 investigated only male (N = 1), female (N = 5) populations or, did not specify participant gender (N = 7). The majority of studies included healthy participants however others included participants prone to falling (N = 5), participants in hospital (N = 2) or long-term living facilities (N = 3), participants with osteopenia (N = 2), neurological issues (N = 15), PTSD (N = 1) or diabetes (N = 1), participants who had experienced a stroke (N = 1) or persistent dizziness (N = 2), veterans (N = 2), those who were recently bereaved (N = 1) and those with depression (N = 1). Finally, three studies were systematic reviews containing multiple populations.
TABLE 2
| Article | Participants | Population | Design | AR/VR Category | AR/VR Equipment | Protocol |
|---|---|---|---|---|---|---|
| Agmon et al. (2011) | N = 7 | Healthy | Quasi-Experiment | Non-Immersive VR | Wii Balance Board | Nintendo Wii Fit exergames with balance board to improve balance in older adults |
| Mean Age = 84.0 | Played for an average of 50, half hour sessions | |||||
| Gender: 3 M:4 F | ||||||
| Anderson-Hanley et al. (2011) | N = 14 | Healthy | RCT | 2D VR | Stationary Bicycle | Cybercycle over 1 month period with virtual competitors to examine the effect of social facilitation and competitiveness on exercise in exergaming |
| Mean Age = 78.1 | ||||||
| Gender: 1 M:13 F | ||||||
| Anderson-Hanley et al. (2012) | N = 63 | Healthy | RCT | 2D VR | Stationary Bicycle | Cybercycle and stationary bicycle groups: 1 month familiarization period. Participants asked to gradually increase their exercise frequency to 45 min per session, five-times/week for an additional 3 months |
| Mean Age = 78.69 | ||||||
| Gender: 17 M: 62 F | ||||||
| Anderson-Hanley et al. (2014) | N = 30 | Healthy | Quasi-Experiment | 2D VR | Stationary Bicycle | Cybercycle and stationary bicycle groups: gradually increase exercise to 45 min, 5 days/week for 3 months |
| Mean Age = 79.5 | ||||||
| Gender: 17 M: 46 F | ||||||
| Bacha et al. (2018) | N = 46 | Healthy | Non Randomized Pilot Trial | Non-Immersive VR | Xbox Console and Kinect Camera | Xbox 360 and Kinect Camera |
| Mean Age = 69.3 | Kinect Adventures Games and Conventional physical therapy groups: 14 1 h training sessions, twice/week | |||||
| Gender: 12 M: 34 F | ||||||
| Barbosa et al. (2019) | N = 12 | Dizziness + Unilateral Vestibular Hypo-function | RCT | Non-Immersive VR | Xbox Console and Kinect Camera | Xbox 360 and Kinect camera |
| Mean Age = 70.1 | VR and Control Group: Three times/week over a 5 week period | |||||
| Gender: 4 M: 8 F | ||||||
| Bell et al. (2011) | N = 21 | Assisted Living Facility | Repeated Measures Design | Non-Immersive VR | Wii Consoles | Nintendo Wii Console over an 8 week period, playing one bowling game on each weekly session to examine effects on quality of life, social relationships and confidence in ability to prevent falls |
| Age: 60–90+ | ||||||
| Gender: 5 M: 16 F | ||||||
| Benoit et al. (2015) | N = 18 | MCI | Quasi-Experiment | 2D VR | BARCO | BARCO iSpace VR system with projectors to display a familiar image-based virtual environment. Participants spent a maximum in 15 min in two VR conditions (7 min each) and after each condition were asked whether they recognized the environment they saw |
| Mean Age = 68.2 | ||||||
| Gender: 11 M: 7 F | ||||||
| Bisson et al. (2007) | N = 24 | Healthy | RCT | Non-Immersive VR | IREX | IREX 3D VR displayed on 3D screen |
| Mean Age = 74.4 | VR and Biofeedback Training Groups: Two 30 min sessions/week for 10 weeks | |||||
| Gender: 10 M: 14 F | ||||||
| Blackman et al. (2007) | N = 38 | Dementia | Quasi-Experiment | 2D VR | Joystick/Controller | Images of a town center on a PC projected onto a large 6 × 2 m screen with ambient street sounds. Participants interacted with the environment using a joystick |
| Age: 71–84 | ||||||
| Gender: 19 M: 19 F | ||||||
| Cacciata et al. (2019) | N = 614 | Not Specified | Systematic Review | RCT’s that evaluated the effect of exergaming on health-related QoL in older adults and published between 2007 and 2017 | ||
| Mean Age = 73.6 | ||||||
| Gender: 204 M: 413 F | ||||||
| Chan et al. (2010) | N = 27 | Long-Term Care | RCT | Non-Immersive VR | IREX | IREX 3D VE displayed on a 2D screen |
| Mean Age = 66.1 | Ten, 15 min long sessions of two VR activities over a period of 5 weeks | |||||
| Gender: 18 M: 9 F | ||||||
| Choi and Lee (2019) | N = 60 | Mild Cognitive Impairment | Quasi-Experiment | 2D VR | Custom Scenario: 2D Display Screen | 1st person video recorded and viewed on a projector screen |
| Mean Age = 76.3 | VKP Group: Two 60 min sessions/week for 6 weeks | |||||
| Gender: 9 M: 51 F | Control Group: Performed home exercises for the same time period | |||||
| Corno et al. (2014) | N = 10 | Healthy | Exploratory Study | VR | Joystick/Controller and HMD | HMD with tracker and wand for interaction. Participants interacted with a VR apartment and were required to achieve eight tasks as part of the virtual memory training program |
| Age: Over 60 years | ||||||
| Gender: 6 M: 5 F | ||||||
| Coyle et al. (2015) | N = 664 | MCI and Dementia | Systematic Review | Search included computerized training and interventions for older adults with memory impairment between 2000 and 2014 | ||
| Mean Age = 76 | ||||||
| Gender: Not Specified | ||||||
| Eggenberger et al. (2015) | N = 71 | Healthy | Quasi-Experiment | 2D VR | Dance Platform | Dance Platform–2D VE displayed on screen |
| Mean Age = 78.9 | Two 1 h training sessions/week with at least 1 day between sessions for recovery over a 6 month period, leading to a total of 52 sessions for all three groups (Dance, Memory, and Phys) | |||||
| Gender: 25 M: 46 F | ||||||
| Fasilis et al. (2018) | N = 10 | Mild Dementia | Study Design | 2D VR | Joystick/Controller | 3D VE displayed on a 2D screen |
| Mean Age 73.6 | Three training sessions for 1 h each | |||||
| Gender: Not Specified | No Control Group | |||||
| Felnhofer et al. (2014) | N = 124 | Healthy younger and older adults | Quasi-Experiment | VR | Joystick/Controller and HMD | HMD with smart phone controller, displaying a virtual café |
| Mean Age = 46.2 | Participants completed a set list of tasks in the VE | |||||
| Gender: 62 M: 62 F | ||||||
| Franco et al. (2012) | N = 23 | Healthy | RCT | Non-Immersive VR | Wii Balance Board | Wii Fit and Balance Board |
| Mean Age = 78.2 | Participants met for individual sessions twice/week for three weeks. Each exercise session lasted 10–15 min and participants played 5 different games | |||||
| Gender: 7 M: 25 F | Matter of Balance program. Participants attended group exercise sessions (30–45 min) twice/week for 3 weeks | |||||
| Gamito et al. (2010) | N = 10 | PTSD War Vets | Quasi-Experiment | VR | HMD | 3D VE in HMD. |
| Mean Age = 63.5 | VRET and EI Group: 12 sessions | |||||
| Gender: Male Only | ||||||
| Gamito et al. (2019) | N = 25 | Healthy | Quasi-Experiment | 2D VR | Keyboard/Mouse | 3D VE displayed on a 2D monitor with mouse and keyboard |
| Mean Age: 65–74 | Intervention performed twice a week for a total of twelve 30 min sessions | |||||
| Gender: 4 M: 21 F | No Control Group | |||||
| Glännfjord et al. (2017) | N = 8 | Healthy | Observation and Qualitative Interview | Non-Immersive VR | Wii Consoles and Wii Remote | Wii Sport Bowling |
| Mean Age: 78.0 | Participants met with the researcher on nine occasions over a 17 week period for an approximate total time of 15.5 h | |||||
| Gender: 6 M: 2 F | ||||||
| Gomes et al. (2018) | N = 30 | Frail and Pre-frail | RCT | Non-Immersive VR | Wii Consoles and Wii Remote | Wii Fit Plus |
| Mean Age: 84.0 | Participants attended 14 training sessions, lasting 50 min each, twice/week. In each session, participants played five of 10 selected games, with two attempts at each game | |||||
| Gender: 2 M: 28 F | ||||||
| Hsieh et al. (2018) | N = 60 | Cognitive Impairment | Non-Randomised Control Trial | Non-Immersive VR | Xbox Console and Kinect Camera | Xbox 360 and Kinect camera |
| Mean Age = 78.2 | VRTC Group: 50 min group sessions, twice/week for 24 weeks | |||||
| Gender: 17 M: 43 F | Control Group: Maintain usual daily physical activities for the 6 month period | |||||
| Kahlbaugh et al. (2011) | N = 35 | Healthy | RCT | Non-Immersive VR | Wii Remote | Wii Console and Wii Remote |
| Mean Age = 82.0 | Wii and TV Group: 1 h/week for 10 weeks | |||||
| Gender: 4 M: 32 F | Control Group: maintained current lifestyle | |||||
| Karahan et al. (2015) | N = 52 | Healthy | Non-RCT | Non-Immersive VR | Xbox Console and Kinect Camera | Xbox 360 and Kinect Motion Sensor, Dance Central |
| Mean Age = 70.2 | Participants attended three dance training sessions per week for 12 weeks | |||||
| Gender: Female Only | ||||||
| Kizony et al. (2006) | N = 16 | Healthy and Neurological Deficits | Quasi-Experiment | Non-Immersive VR | IREX | PC with webcam. Java based visual interaction system |
| Mean Age = 70.6 | Healthy participants interacted with the system for one 20–30 min session. After training, participants played two games for 5 min each | |||||
| Gender: 5 M:7 F:4 Not specified | Participants with neurological symptoms also interacted with the system for one 30 min session with an occupational therapist and they played 3 different games | |||||
| For one participant who suffered a stroke, the system was installed at home and his wife trained to use the system. They recorded what games/how long he played for | ||||||
| Kizony et al. (2010) | N = 22 | Healthy and Post Stroke | Observation | 2D VR | Treadmill | VE of a grocery store aisle with a custom built treadmill using a computer assisted rehabilitation environment system (CAREN) to synchronize treadmill speed and scene progression |
| Mean Age = 69.2 | Participants we provide with instructions (how many items to collect) in various ways (listed together, sequentially etc.) | |||||
| Gender: 11 M: 11 F | ||||||
| Korsgaard et al. (2019) | N = 7 | Mobility Problems | Qualitative | AR | Augmented Reality Environment | Oculus Rift HMD with a GoPro helmet mount connected to a VRREeady PC, a green table cloth used to help the software separate the table elements from the surrounding environment. Virtual elements created in Unity and librealsense API used to align real world color and depth images |
| Mean Age = 80.2 | Participants were provided with three desserts and ate them while interacting with the mixed reality environment | |||||
| Gender: 1 M:6 F | ||||||
| Knowles et al. (2017) | N = 27 | Recently Bereaved | Quasi-Experiment | 2D VR | Keyboard/Mouse and MMORPG | 3D VE displayed on a 2D screen with mouse and keyboard |
| Mean Age = 67.2 | VR Support Group: 1 h, twice/week on non-consecutive days for 8 weeks (16 sessions) | |||||
| Gender: 9 M: 21 F | Control Group: One reading on grief/week approx. 1 page in length. Time online was tracked | |||||
| Laver et al. (2012) | N = 44 | Acute Care Patients Currently Hospitalized | RCT | Non-Immersive VR | Wii Balance Board | Wii Fit and Balance Board |
| Mean Age = 85.0 | Gaming Participants: Played games using the Wii console for 25 min each day, 5 days per week during their hospital stay | |||||
| Gender: 9 M:35 F | Control Participants: took part in conventional physiotherapy throughout their hospital stay | |||||
| Lee and Shin (2013) | N = 55 | Diabetes Mellitus | RCT | Non-Immersive VR | PlayStation and EyeToy Camera | PlayStation 2 and EyeToy |
| Mean Age = 74.3 | Exercise Group: 50 min twice/week for 10 weeks | |||||
| Gender: 16 M: 39 F | Exercise and Control Group: Received health education throughout this time | |||||
| Lee et al. (2015) | N = 47 | Healthy | RCT | Non-Immersive VR | Xbox Console and Kinect Camera | Xbox 360 and Kinect Camera |
| Mean Age = 68.24 | Individualized feedback-based VR and Group-based Exercise Groups: 60 min intervention, 3 times/week for 8 weeks | |||||
| Gender: Female Only | ||||||
| Levy et al. (2016) | N = 16 | Healthy | RCT | Non-Immersive VR | PlayStation and EyeToy Camera | PlayStation 2 and EyeToy |
| Mean Age = 70.53 | Treatment Group: Twelve, 40 min sessions, once/week | |||||
| Gender: 6 M: 10 F | Control Group: Waiting List | |||||
| Lee et al. (2017) | N = 40 | Healthy | Open Label Trial | Non-Immersive VR | Joystick/Controller; Treadmill and Wii Balance Board | Wii Console, Balance Board and Joystick |
| Mean Age = 75.93 | Experimental Group: Two, 60 min training sessions/week for 6 weeks | |||||
| Gender: 17 M: 23 F | Experimental Group and Control Group: Three sessions of fall prevention education during weeks 1, 3, and 5 | |||||
| Liu (2010) | N = 128 | Healthy | Quasi-Experiment | 2D VR | Keyboard/Mouse | Virtual shop displayed on a 19” LCD TV. |
| Mean Age = 69.5 | The shop contained four show-rooms, with 144 goods displayed and each showroom had approx. 36 pieced. Objects were displayed as either 2D or 3D | |||||
| Gender: 64 M: 64 F | ||||||
| Lokka et al. (2018) | N = 81 | Healthy Younger and Older Adults | Controlled Experiment | 2D VR | Videos | Large Projection screen 2.2 m from participants |
| Mean Age = 48.5 | Participants were shown a representative image from each of the three VE (displaying various routes) and asked to rate their preference for hypothetical route learning tasks. Next, participants were given a scenario where someone takes them to a market in an unfamiliar neighborhood and they were told to memorize the route as they would need to navigate the same route themselves unsupervized. This initial session took approx. 1–1 h 40 min. Later participants were brought back for a second session approx. 40 min–1 h | |||||
| Gender: 41 M: 40 F | ||||||
| Man et al. (2012) | N = 44 | Questionable Dementia | RCT | 2D VR | Joystick/Controller | 3D VE displayed on 2D screen with keyboard and joystick |
| Mean Age = 80.29 | VR-based and therapist-led memory training groups: 10 individual sessions for 30 min each, two–three times/week | |||||
| Gender: 5 M: 39 F | ||||||
| Manera et al. (2016) | N = 57 | MCI and Dementia | Quasi-Experiment | 2D VR | BARCO | Barco OverView full HD 3D stereoscopic LED video wall 1.55 × 1.74 m Participants were asked to identify target characters in a series of increasingly complex levels. Participants were only allowed to progress in levels after the initial five targets are found |
| Mean Age = 75.65 | Participants sat at a distance of 1.9 m while wearing 3D LCD shutter glasses and interacted with the VE using a wireless mouse | |||||
| Gender: 32 M: 25 F | ||||||
| Marivan et al. (2016) | N = 8 | Healthy | Experiment | Non-Immersive VR | Joystick/Controller | PC, video projector and joystick |
| Mean Age = 87.4 | Participants were asked to get their avatar to walk in a straight line along a corridor over a period of 1 week including 3–5 sessions day | |||||
| Gender: 4 M: 4 F | ||||||
| Matas et al. (2015) | N = 88 | Post-Fall Rehabilitation | Cohort Survey | 2D VR | Joystick/Controller and Driving Simulator | 3D VE displayed on 2D screen with gaming wheel and peddles |
| Mean Age = 72.8 | Participants sat at a desk chair and controlled a virtual car using a small gaming wheel and pedals | |||||
| Gender: 54 M: 34 F | Practice drive of 10 min.Drive 1: 15 min Drive 2: 15 min with additional attention tasks | |||||
| Merriman et al. (2015) | N = 76 | Fall-Prone + Healthy | RCT | Non-Immersive VR | Wii Balance Board | Wii Console and Balance Board |
| Mean Age = 74.18 | Intervention Group: Two, 30 min sessions of balance training/week for 5 weeks | |||||
| Gender: 16 M: 60 F | Control Group: Keep a diary of daily light, moderate and heavy physical activities | |||||
| Merriman et al. (2018) | N = 56 | Healthy and Fall-Prone | RCT | Non-Immersive VR | Wii Balance Board | Nintendo Wii Balance Board with waist high support frame. Software: CityQuest |
| Mean Age = 71.8 | Participants took part in two pre-training sessions followed by 10 training sessions with an average of two sessions/week over 5 weeks. Sessions lasted approx. 60 min | |||||
| Gender: 21 M: 35 F | ||||||
| Miller et al. (2014) | N = 355 | Healthy and Neurologically Impaired | Systematic Review | Search for gaming and virtual reality with older adults between 2000 and 2012 | ||
| Mean Age = 82.28 | ||||||
| Gender: Not Specified | ||||||
| Mirelman et al. (2011) | N = 20 | Parkinson’s Disease | RCT | 2D VR | Treadmill | 3D VE on a 2D screen with treadmill |
| Mean Age = 67.1 | Intervention: Three sessions/week for 6 weeks | |||||
| Gender: 14 M: 6 F | No Control Group | |||||
| Monteiro-Junior et al. (2017) | N = 19 | Long-Term Care | Quasi-Experiment | Non-Immersive VR | Wii Consoles | Wii Console |
| Mean Age = 86.0 | Wii Group: 1 h of exergaming with resting periods included | |||||
| Gender: 3 M: 16 F | Control Group: 30–45 min of exercising | |||||
| Morone et al. (2016) | N = 38 | Bone Loss | Quasi-Experimental | Non-Immersive VR | Wii Balance Board | Wii Fit and Balance Board |
| Mean Age = 68.9 | Participants in both the Wii group and the control group took part in 1 h training exercises, 2 days/week for 8 weeks. Exercises were supervised by two physiotherapists | |||||
| Gender: Female Only | ||||||
| Optale et al. (2010) | N = 36 | Memory Impaired | RCT | VR | Joystick/Controller and HMD | HMD with PC and joystick |
| Mean Age = 80.0 | VRMT: 6 months of virtual reality memory training including auditory stimulation and VR experiences in path finding. 3 months initial training, with 3 auditory and 3 VR sessions every 2 weeks) and 3 months booster training (1 auditory and 1 VR session per week) | |||||
| Gender: 12 M: 24 F | Control Group | |||||
| 6 months face-to-face music therapy | ||||||
| Padala et al. (2012) | N = 22 | Alzheimer’s Dementia | Prospective Randomized Pilot Study | Non-Immersive VR | Wii Consoles | Wii Console |
| Mean Age = 80.4 | Nintendo Wii Fit and Walking group: 30 min’ activity/day, five times/week, for 8 weeks | |||||
| Gender: 6 M: 16 F | ||||||
| Padala et al. (2017a) | N = 30 | Veterans | Prospective Randomized Pilot Study | Non-Immersive VR | Wii Consoles | Wii Console |
| Mean Age = 68.0 | Wii Fit Group: 45 min, 3 days/week for, 8 weeks | |||||
| Gender: 26 M: 4 F | Control Group: A computer-based cognitive program for 45 min, 3 days/week, for 8 weeks | |||||
| Padala et al. (2017b) | N = 30 | Mild Alzheimer’s Disease | Quasi-Experimental | Non-Immersive VR | Wii Consoles | Wii Console |
| Mean Age = 73.0 | Wii and Walking Groups: 30 min, 5 days/week for 8 weeks | |||||
| Gender: 38 M: 22 F | ||||||
| Parijat et al. (2014) | N = 24 | Healthy | Quasi-Experimental | VR | Treadmill and HMD | HMD with treadmill where virtual slips are created by tilts in pitch plane of the VR scene at random intervals |
| Mean Age = 72.35 | Baseline Measure: Walk approx. 10 min to gather slip data | |||||
| Gender: 12 M: 12 F | Training acquisition: Control group, normal walking for 10–15 min. Training group, 5 min walking with harness on treadmill, 15 min with HDM on treadmill where virtual slips may occur | |||||
| Transfer of Training: 1 day later, participants returned to the baseline measure location and matched walking pace to the first meeting. A final slip trial was conducted | ||||||
| Rodrigues et al. (2018) | N = 47 | Fallers vs. non-fallers | RCT | Non-Immersive VR | Xbox Console and Kinect Camera | Xbox 360 and Kinect Camera |
| Mean Age = 70.2 | Intervention Group: 12 weeks of video game dance training. 40 min sessions, three times/week | |||||
| Gender: Female Only | Control Group: Maintained their current lifestyle | |||||
| Rosenberg et al. (2010) | N = 19 | Subsyndromal Depression | Quasi-Experimental | Non-Immersive VR | Wii Consoles | Wii Console |
| Mean Age = 78.7 | Participants completed a 12 weeks intervention, playing Wii Sports for 35 min, three times per week | |||||
| Gender: 6 M: 13 F | ||||||
| dos Santos Mendes et al. (2012) | N = 27 | Parkinson’s and Healthy | Longitudinal Controlled Clinical Study | Non-Immersive VR | Wii Consoles and Wii Remote | Wii Console and Wii Fit |
| Mean Age = 68.65 | Participants took part in 14 twice-weekly individual training sessions overseen by a physiotherapist. Sessions included 30 min warm-up. Afterward, participants played five games, twice. At the end of the 14 week period, participants received two attempts at 10 Wii Fit games | |||||
| Gender: Not Specified | ||||||
| Sápi et al. (2019) | N = 75 | Healthy | RCT | Non-Immersive VR | Xbox Console and Kinect Camera | Xbox 360 and Kinect Camera |
| Mean Age = 68.62 | Kinect and Conventional Balance Groups: 30 min training, three times/week for 6 weeks | |||||
| Gender: 6 M: 70 F | ||||||
| Sauzéon et al. (2016) | N = 60 Mean Age 44.4 Gender: Not Specified | University (Younger) Community Leisure Institutions | RCT | 2D VR | Keyboard/Mouse | 3D VE displayed on 2D screen with mouse and keyboard |
| There were two learning trials were participants were participants watched a target version of the apartment (which is presented twice) | ||||||
| Each participant was asked to complete a free recall task immediately after each presentation | ||||||
| The same instructions were repeated before the presentation of the second version | ||||||
| Smaerup et al. (2016) | N = 57 | Chronic Dizziness | RCT | 2D VR | Webcam. Keyboard/Mouse | PC with webcam |
| Mean Age = 70.21 | Software: “Move It to Improve It” | |||||
| Gender: 21 M: 36 F | Participants played a series of individual games each day for 20–30 min for 12 weeks | |||||
| Studenski et al. (2010) | N = 25 | Healthy | Quasi-Experimental | 2D VR | Xbox Console and Kinect Camera and Dance Platfrom | TV and DanceTown™. |
| Mean Age = 80.2 | Participants took part in supervised dance sessions with the aim of completing 24 sessions in a three-month period. Sessions two place twice per week for 30 min each | |||||
| Gender: 5 M: 20 F | ||||||
| Sun et al. (2019) | N = 29 Mean Age = 77.5 | Osteopenia or Osteoporosis | Quasi-Experimental | 2D VR | Xbox Console and Kinect Camera | Kinect Camera, PC and 2D screen |
| Gender: Female Only | Participants took part in a series of fall risk assessments with FRAAn (a fall risk assessment avatar) guiding each session. Each session lasted approx. 20 min | |||||
| Tsuda et al. (2016) | N = 16 | Hematologic Malignancies receiving Chemotherapy | Quasi-Experimental | Non-Immersive VR | Wii Balance Board | Nintendo Wii Fit and Balance Board |
| Mean Age = 66.81 | Participants took part in two physical activities one-on-one with a physical therapist for approx. 20 min, each day, five times/week from the beginning of chemotherapy until hospital discharge | |||||
| Gender: 10 M: 6 F | ||||||
| Vallejo et al. (2014) | N = 36 | Healthy | Quasi-Experimental | Non-Immersive VR | Joystick/Controller | PC, TV screen, joystick, touchpad and game controllers. Software: 3D Memory Island |
| Mean Age = 70.5 | Participants tried out four different interfaces. Their task was to guide an avatar through a pathway to reach a goal by following the navigation signs along the way | |||||
| Gender: 22 M: 14 F | ||||||
| De Vries et al. (2018) | N = 30 | Healthy | Quasi-Experimental | Non-Immersive VR | Xbox Console and Kinect Came and Wii Consoles | Wii Console (two games), Xbox Kinect (four games), Dynstable (two games) |
| Mean Age = 69.62 | Participants in all three conditions, played each game three times except for two games in the Xbox condition which were longer so were only played once | |||||
| Gender: 10 M: 20 F | ||||||
| Williams et al. (2011) | N = 22 | Healthy | Quasi-Experimental | Non-Immersive VR | Wii Balance Board | Wii Fit and Balance Board |
| Mean Age = 83.86 | Over 4 weeks participants completed 12, 20 min sessions using different games in the Wii Fit package | |||||
| Gender: 4 M: 18 F | ||||||
| Yeh et al. (2019) | N = 294 | Healthy | Quasi-Experimental | Non-Immersive VR | Wii Consoles | Wii Console |
| Age = 61–76+ | Participants played Wii Fit games for 10 weeks with an average 10 opportunities to play with the system and 2–4 people playing each game at the same time. A new group took over if the first became tired | |||||
| Gender: Not Specified |
Study details.
VR, a virtual environment which envelops the user often through HMD’s; Non-Immersive VR, a virtual environment where the user can see themselves or an avatar representing themselves within a virtual world; 2D VR, where the user interacts with a 3D virtual environment using a 2D monitor display but does not see themselves or an avatar representing themselves.
Study Designs
Of the included studies, 24 were randomized controlled trials, four were non-randomized controlled trials one was an exploratory study, two were observational two were qualitative, and one was an open label trail. The remaining studies were quasi-experimental (see Table 2).
Research Focus (Measures)
The measures used across the 65 studies were categorized into seven main themes, with most research examining two or more (See Table 3). Themes included physical activity, general health, balance and falls, cognition, affect, wellbeing and user experience (UX). One measure looked at a person’s motivations within a natural or therapeutic environment and was categorized as other.
TABLE 3
Areas of research interest across 65 studies.
*Studies that include UX questions, but not standardized measures.
**Systematic Reviews.
***Study uses the Volitional Questionnaire, which does not fit into the above categories.
AR/VR Equipment
The 65 studies included a combination of custom-made and commercially available virtual technologies. Custom systems usually consisted of a specially designed virtual environment displayed on a monitor or projector and interacted with using keyboard/mouse (N = 5), joystick/controller (N = 10) or, exercise equipment such as treadmills (N = 4) or stationary bicycles (N = 3). Other customized equipment included the BARCO™ (N = 2) and IREX™ (N = 3) systems. Commercially available systems included use of Xbox Console™ and Kinect Cameras™ (N = 10), PlayStation™ and EyeToy™ Cameras (N = 2) or, Wii Console™ (N = 11) with Wii Remote™ (N = 4) and Wii Balance Board™ (N = 9). Only six studies used HMDs to immerse users in a virtual (N = 5) or augmented (N = 1) environment. Alternate set-ups included: 1) a two custom scenarios where participants “rowed” along with a first person video displayed on screen (N = 1) or where participants memories a route (N = 1), 2) a bereavement study where the participants interacted with each other through “Second Life,” a massively multiplayer online roleplaying game (MMORPG) (N = 1); 3), studies that looked at the impact of using dance platforms (N = 2); and 4) a study that looked at cybersickness and drop-out rates in a driving simulator (N = 1).
Virtual Reality Characteristics
This scoping review aimed to identify AR/VR technology used to support older adults’ physical and/or mental health. However, only one augmented reality study (Korsgaard et al., 2019) was identified. As described earlier this paper categorized the technology used in each study as either: 1) 2D VR, 2) Non-Immersive VR, 3) Immersive VR and 4) AR. Despite self-identifying as Immersive VR, 16 of 21 studies were in fact 2D VR. The remaining five studies correctly identified themselves as either a “virtual environment” (Liu, 2010; Fasilis et al., 2018; Lokka et al., 2018), a video game (Studenski et al., 2010) and a virtual avatar (Sun et al., 2019). This review categorized 35 studies as non-immersive VR but, only seven of these studies did not include the phrasing “Immersive VR” or “virtual reality” in their interventions. Five papers described themselves as “exergames” (Rosenberg et al., 2010; Franco et al., 2012; Karahan et al., 2015; Padala et al., 2017a; Padala et al., 2017b), one as a videogame (Laver et al., 2012), one as a “virtual environment” (Merriman et al., 2015) and one only described the type of console used (Padala et al., 2012). Finally, five studies can be categorized as “Immersive VR” (Gamito et al., 2010; Optale et al., 2010; Corno et al., 2014; Parijat et al., 2014; Lokka et al., 2018) and each study accurately described itself as such. Despite the large number of studies included in this review, only 16 provided a definition for virtual reality (See Table 4), one offered a definition for virtual reality exposure therapy (Barbosa et al., 2019) and one described “mixed reality” (Korsgaard et al., 2019).
TABLE 4
| Article | Definition |
|---|---|
| Bacha et al. (2018) | “VR is defined as the simulation, in real time, of an environment, scenario, or activity where the individual can interact” |
| Barbosa et al. (2019) | “Virtual reality is defined as the human-machine connection, where situations occur that can be compared to those experienced during daily life, thus, the individual experiences a considerable number of stimuli through interaction with the proposed scenario.” |
| Benoit et al. (2015) | VR “a computer-simulated environment that can provide the sensation of physical presence in places representing real or imagined worlds” |
| Bisson et al. (2007) | Virtual Reality is defined as “a computerized simulation in two or three dimensions that is in real time and interactive.” |
| Chan et al. (2010) | “VR entails the use of advanced technologies, including computers and various multimedia peripherals, to produce a relatively lifelike situation that users perceive as comparable with real-world objects and events.” |
| Choi and Lee (2019) | Virtual reality is “a computer-simulated environment and interaction of computer-generated experience used to enhance physical or psychological function in another place” |
| Glännfjord et al. (2017) | Virtual Reality is a “computer-generated simulation that creates a realistic looking world.” |
| Hsieh et al. (2018) | “A type of user-computer interface that implements real-time simulation of an activity or environment that allows user interaction via multiple sensory modalities” |
| Kizony et al. (2010) | Virtual Reality: “the use of interactive simulations created with computer hardware and software to introduce users to opportunities to interact in environments that seem and feel similar to the real world.” |
| Korsgaard et al. (2019) | Mixed Reality: the concept of experiencing the real and virtual world at the same time as a coherent and perceivable merged reality |
| Levy et al. (2016) | Virtual Reality “involves the creation of an interactive computer-generated, three-dimensional (3D) environment” |
| Marivan et al. (2016) | VR “interactive simulations that create environments that appear and feel similar to real world objects and events.” |
| Optale et al. (2010) | VR is an experiential interface in which the components of perception (visual, tactile, and kinaesthetic) are the bases for interactivity, encouraging a sense of “being there”–that is, the sensation of being actually inside the virtual environment |
| Parijat et al. (2014) | VR “an approach to generate simulated, interactive, and multidimensional environments on a head-mounted display (HMD) or on a computer monitor.” |
| dos Santos Mendes et al. (2012) | Virtual Reality “A computer-based technology providing a multisensorial environment with which the user can interact.” |
| Yeh et al. (2019) | VR “a computer-generated reality that allows users to enter a virtual world through a computer interface” |
Virtual reality definitions.
Usability and Virtual/Augmented Technologies
Over a third of the studies included in this review directly investigated the usability and feasibility of various AR/VR systems for use with older populations to support physical and mental health and wellbeing. However, only ten of these studies used standardized questionnaires (see Table 3) to evaluate participants’ sense of presence and the usability of each system. The remaining studies that included evaluations of usability or design provided their participants with bespoke questionnaires tailored to fit their purpose. Key findings from this group of studies indicated that there were no age differences (between older and younger users) in physical and social presence (Felnhofer et al., 2014), or in experience of cybersickness (Sauzéon et al., 2016). One study demonstrated a reduction in cybersickness with older adults with schizophrenia (Chan et al., 2010), another indicated that most of their PTSD patients reported no negative effects after exposure to a virtual environment displayed in an HMD. Despite this, research still maintains that older adults are a high-risk group for cybersickness (Matas et al., 2015). One study did find a gender difference in level of presence, where men were more likely to experience a greater sense of presence (Felnhofer et al., 2014).
Analysis of the 28 studies that considered UX design of AR/VR environments (See Table 5), and the technologies used has established three main categories, each with further sub-categories, to describe the factors by. These include usability, feasibility, and tailored design.
TABLE 5
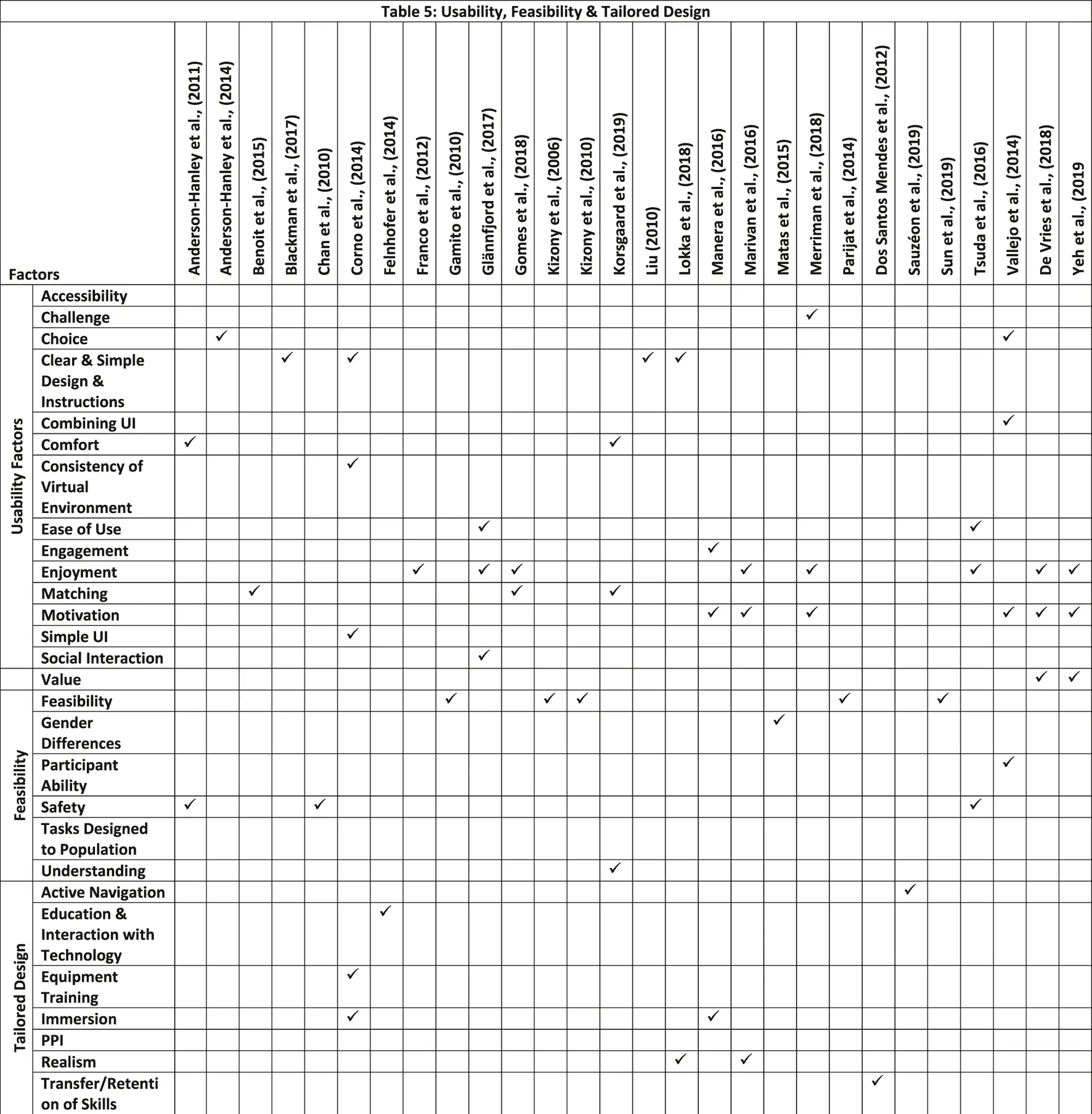 |
Usability, Feasibility & Tailored Design.
Usability
Enjoyment (N = 8) and Motivation (N = 6) are the most common themes with researchers identifying them as vital to user engagement. Additional themes included, clear and simple design/instructions (N = 4), Matching (N = 3), Value (N = 2), Ease of Use (N = 2), Comfort (N = 2) and Choice (N = 2). The remaining themes within the category of Usability each had one mention and they included, Accessibility, Challenge, Combining UI, Consistency of Virtual Environment, Engagement, Simple UI and Social Interaction.
Feasibility
Feasibility (N = 5), Safety (N = 3), Gender Differences (N = 1), Participants Ability (N = 1), Tasks Designed to Population (N = 1) and Understanding (N = 1) were sub-categories identified across the research studies.
Tailored Design
Finally, there were seven suggestion/outcome sub-categories identified. These included, Realism (N = 2), Active Navigation (N = 1), Education and Interaction with Technology (N = 1), Equipment Training (N = 1), Immersion (N = 1), Public and Patient Involvement (PPI) (N = 1), and Transfer/Retention of Skills (N = 1).
Intervention-Based Theories
This paper outlines four popular theories that can be applied to AR/VR research; perceptual control theory, Self-affirmation theory, the transtheoretical model of behavior change and the transformative learning theory. However, none of these theories were considered by the studies included in review. Instead, 13 additional theories were used to support the AR/VR methodologies used in those papers (See Table 6) and only the theory of planned behavior (Anderson-Hanley et al., 2012; Merriman et al., 2018) was cited twice. Overall, the theories that were cited focused on either the impact of the surrounding environment (Anderson-Hanley et al., 2011; Felnhofer et al., 2014; Glännfjord et al., 2017), the intrinsic motivations of the individual (Anderson-Hanley et al., 2011; Kahlbaugh et al., 2011; Anderson-Hanley et al., 2014; Glännfjord et al., 2017; De Vries et al., 2018) or the complex cognitive processes occurring in the unconscious (Fasilis et al., 2018; Lokka et al., 2018; Merriman et al., 2018).
TABLE 6
| Article | Theory | Domain | Summary |
|---|---|---|---|
| Anderson-Hanley et al., (2011) | Social Facilitation Theory (Allport, 1955) | Social | “behavior in simple tasks is improved in the presence of others” (pp. 275–276) |
| Generalized Drive Hypothesis (Zajonc, 1965) | Social | “social facilitation increases one’s innate internal drive and activation levels, which are found to be elevated in competitive environments.” (p. 276) | |
| Anderson-Hanley et al., (2014) | Theory of Planned Behavior (Ajzen, 1991) | Social | “people’s attitudes and beliefs about objects and themselves influence their participation in health-relevant behaviors” (p. 2) |
| Temporal Self-Regulation Theory (Hall and Fong, 2007) | Biopsychosocial | “people decide to engage in immediate behaviors that yield later, but not immediate, effects.” (p. 2) | |
| Fasilis et al., (2018) | Theory of Interactive Cognitive Complexity (Tennyson and Breuer, 1997) | Cognitive | “simulation games are more effective than other instructional methods, because they simultaneously engage trainees’ affective and cognitive processes.” (p. 43) |
| Decomposition Hypothesis (Anderson, 2002) | Cognitive | “the daily presented tasks that we face in our life, complex and non-complex, can be degraded, decomposed, into equally fundamental actions, and by training ourselves in those actions/operations, we can get improved overall.” (p. 47) | |
| Felnhofer et al., (2014) | Social Influence Theory (Kelman, 1958) | Social | “to explain why people, tend to react to virtual characters as if they were real: (i) agency as the user’s belief that the avatar is being controlled by a human in contrast to a computer, (ii) communicative realism as the believability of the avatar’s communicative behavior.” (p. 273) |
| Glännfjord et al., (2017) | Social Interaction Theory (Vygotsky, 1978) | Social | “keeping an active life is important when growing older.” (p. 334) |
| Activity Theory (Havighurst, 1961) | Social | “it is important to keep active while growing older and to socially interact with others.” (p. 334) | |
| Kahlbaugh et al., (2011) | Theory of Active Engagement (Rowe and Kahn, 1997) | Social | The “positive role of activity in supporting a sense of purpose or place via role support.” (p. 332) |
| Lokka et al., (2018) | Dual Channel Theory (Mayer and Moreno, 2003) | Cognitive | “people do not rely only on visuospatial memory systems for key executive functions such as the encoding, storage and recall of information.” (p. 2) |
| Merriman et al., (2018) | Theory of Planned Behavior (Ajzen, 1991) | Social | “beliefs and attitudes can predict intentions and behavior.” |
| Cognitive Load Theory (Sweller, 1980) | Cognitive | “If too much cognitive load is present in a complex learning environment, performance may be hindered due to insufficient working memory resources available to complete the task at hand .” (p. 552) | |
| De Vries et al., (2018) | Means-End Theory | Cognitive | “consumers or players in this case will prefer one game to another because of how certain attributes or game mechanics lead to certain benefits, or desired consequences, or ultimately tailor to the goals or values a player seeks.” (p. 2) |
Theories supporting AR/VR methodologies.
Discussion
This scoping review was undertaken to assess the variety and scale of AR/VR in use with older adults in relation to physical and mental health and wellbeing. As this study was completed in the first half of 2020, it includes the most recent relevant articles from 2019. Findings from this review, indicate that AR is not readily being used with this population in a health setting. More studies are using non-immersive VR (53%) compared to 2D VR (32%), but research of this kind is less likely to define VR before including it in the methodology.
Designing AR/VR Environments
As described in the results above, over a third of papers identified in this review are investigating the usability, feasibility, and design considerations important for AR/VR environments aimed at assisting older adults in their physical/mental health and general wellbeing. Despite the large number of papers investigating this area, very few used standardized measures. This impedes reviews such as this as comparisons and developments are more difficult to evaluate. However, three primary categories were identified including usability, feasibility, and tailored design (See Table 7). Within those categories there were many themes, which will now be discussed.
TABLE 7
| Study | Measures | Key Elements | Detailed Description of Usability, Feasibility and Design Considerations |
|---|---|---|---|
| Anderson-Hanley et al. (2011) | No standardized UX measures | • Safety | This study uses an exercise bike. Design considerations included ensure the safety and comfort of older adult participants to help reverse negative thinking about exercise |
| • Comfort | |||
| Anderson-Hanley et al. (2014) | Cybercycling Attitudes Test (CAT)–1 Item Likert | • Choice | Giving participants choice to continue in whatever group they choose after the RCT is completed is a good way to continue to engage participants in research |
| Benoit et al. (2015) | Cybersickness Questionnaire–22 Items) | • Virtual/Real World Matching | Using physical apparatus (e.g., chair) as part of the immersive experience may help to ground older users in the virtual environment and reduce cybersickness (i.e., the user is sitting in the VE, the user is also seated in real life) |
| Spatial Presence Questionnaire | |||
| Blackman et al. (2007) | No standardized UX measures | • Clear and Simple Design/Instructions | No discussion regarding usability, feasibility or design considerations for technology used, however the study does discuss the importance clear and simple of building design so those with cognitive impairment can navigate the space with ease |
| Chan et al. (2010) | Simulator Sickness Questionnaire–16 items | • Safety | The researchers discuss the safety of virtual environment to older adult participants with schizophrenia based on a lack of simulator sickness. Factors which contribute to this low score include immersion in a 2D space and the use of projector screens instead on HMD’s |
| Corno et al. (2014) | System Usability Scale–10 items | • Clear and Simple Design/Instructions | Three factors |
| • Simple User Interface | • Task related issues–where instructions are too long or complex | ||
| • Consistency of Virtual Environment | • Hardware related issues–where participants had difficult using the input devices (e.g., wand) | ||
| • Equipment Training | • Difficulties with the HMD directly (i.e., perception of the environment is inconsistent with expectations–colors are too bright etc. | ||
| • Tasks designed to population | General suggestions | ||
| • PPI | • Dedicate more time to training participants how to use the environment/technology so they do not become distracted with learning how to do a task during the intervention | ||
| • Re-design tasks and instructions for the sample population | |||
| • Test the environment with the users to identify and resolve any technical problems as a direct result of the technology. This may include modifying the sensitivity and response interactions of the input devices | |||
| Felnhofer et al. (2014) | Social Presence Survey (SPS)–five items iGroup Presence Questionnaire (IPQ–14 items | • Education and Interaction with Technology | In terms of usability, the older adults in this study were highly educated. In conjunction with research that suggests a link between education and increase technology-related computer self-efficacy, the authors suggest that higher education level in older adults can explain a lack of age-related differences in experience of presence |
| It is vital that older adults are willing to interact with the technology as this is a key factor in the experience of presence | |||
| Franco et al. (2012) | Wii Fit Enjoyment Questionnaire | • Enjoyment | Wii Fit exercise program is both feasible and enjoyable for older adults. This is important as enjoyment may result in continued engagement in research and exercise interventions |
| Gamito et al. (2010) | ITC SOPI | • Feasibility | No discussion regarding usability, feasibility or design considerations for technology used, however the study did consider the feasibility of using VR to treat PTSD in retired veterans |
| Glännfjord et al. (2017) | No standardized UX measures | • Enjoyment | Enjoyment was discussed as an important factor for continued engagement in the study. Also, many participants noted it was easier to play bowling using the Wii Console as there was no extra equipment required. The social component also factored into their continued attendance |
| • Ease of Use | |||
| • Social Interaction | |||
| Gomes et al. (2018) | No standardized UX measures | • Enjoyment• | Enjoyment was mentioned as a factor in acceptable of the technology. Noted that games which included a stationary gait while taking quick steps, could result in adverse events, but they do not make recommendations to prevent or circumvent these risks |
| • Motion Matching | |||
| Kizony et al. (2006) | No standardized UX measures | • Feasibility | The equipment tested in this study can be used with older adults’ post-stroke, however it is likely they will need assistance when the system is installed in their own home |
| Kizony et al. (2010) | No standardized UX measures | • Feasibility | As feasibility of the set-up was assessed in this study, no surface manipulations were made which facilitated participants attention on the specific tasks |
| Korsgaard et al. (2019) | No standardized UX measures | • User Interface–Comfort | Suggestions |
| • Environment Matching | • Participants who wore glasses could use the HMD, but only if the glasses did not exceed dimensions | ||
| • Understanding | • Potential for environmental factors to influence participant opinion (i.e., easting out-side in a VR may be more enjoyable if the real-life weather is cold outside) | ||
| • Participants had difficulties understanding the ability to eat “anywhere” in mixed reality even after immersion in the MR environment | |||
| Liu (2010) | No standardized UX measures | • Clear and Simple Design/Instructions | Suggestions |
| • “Landmarks” are an important feature for older adults immersed in environments depicting a virtual shop | |||
| Lokka et al. (2018) | No standardized UX measures | • Clear and Simple Design/Instructions • Realism | Suggestions |
| • Route recall accuracy improves in mixed VR (image is a combination of abstract and photorealistic structures)–too much or too little information can negatively affect recall performance | |||
| • A smaller number of older participants (compared with younger participants) initially preferred the realistic VE before the experiment, but still switched to the mixed VR afterward (38%), however unlike the younger participants, 54% continued to prefer the realistic environment | |||
| Manera et al. (2016) | No standardized UX measures | • Immersion | Noted that participants with Alzheimer’s and Dementia preferred the VR condition due to immersion, engagement, and motivation to continue |
| • Engagement | |||
| • Motivation | |||
| Marivan et al. (2016) | No standardized UX measures | • Enjoyment | Researchers noted the impact and importance of enjoyment, realism, and motivation to continue using the system |
| • Realism | |||
| • Motivation | |||
| Matas et al. (2015) | Useful Field of View (UFOV) Divided Attention Subtest | • Gender Differences | SSQ can be used to predict dropout in older adults and females were more likely to drop-out than men; supporting research which suggests that women are more susceptible to both motion and simulator sickness.–Suggests drivers with a history of motion sickness not take part in immersive driving simulation studies |
| Simulator Sickness Questionnaire–16 items | |||
| Merriman et al. (2018) | Game Experience Questionnaire (GEQ) | • Challenge | Evaluation of acceptability and game experience in health and fall-prone older adults. Both groups reported high acceptability scores though on average, fall-prone adults reported higher acceptability rates. Participants noted that the challenge of the games were their primary motivation to continue playing. Game enjoyment was also discussed, thought there was little difference between the population groups |
| • Motivation | |||
| • Enjoyment | |||
| Parijat et al. (2014) | No standardized UX measures | • Feasibility | No discussion regarding usability, feasibility or design considerations for technology used, however the study did consider the suitability of VR perturbation as a means of improving motor skills in older adults |
| dos Santos Mendes et al. (2012) | No standardized UX measures | • Transfer/Retention of Skills | People with Parkinson’s disease may experience grater motor difficulties (compared with cognitively impaired and healthy older adult populations) while playing most Wii Fit games but, this does not impact their ability to learn and improve with practice nor, their ability to retain any benefits of training |
| In contrast, those with cognitive impairments (particularly, difficulties with decision-making and working memory) were at greater risk of impeded learning in certain Wii games. This study adds credibility to the concept that effects of VR training is transferable and retained in Parkinson’s patients | |||
| Sauzéon et al. (2016) | No standardized UX measures | • Active Navigation | No discussion regarding usability, feasibility or design considerations for technology used, however the study did note some interesting results based on active or passive navigation. Regardless of age, active navigation can benefit recognition hits in a navigation task, compared to passive navigation. However, active navigation also increases the number of false recognition hits made by older adults (compared with younger adults) |
| Sun et al. (2019) | System Usability Scale–10 item scale | • Feasibility | The FRAAn system can be used effectively to assess fall risk in older adults. Over 80% of participants reported high usability |
| Tsuda et al. (2016) | No standardized UX measures | • Safety | The authors did not include any standardized UX measures but claim that the Wii Fit is feasible, safe with high efficacy. The reasons they provide for this increased usability include the enjoyment and ease of use for fragile patients, the accessibility it provides for patients who are isolated in clean rooms and the reduced cost compared with full VR systems (approx. $200 at time of publication) |
| • Enjoyment | |||
| • Ease of Use | |||
| • Accessibility (Financial) | |||
| • Accessibility (Environmental) | |||
| Vallejo et al. (2014) | System Usability Scale–10 item scale | • Choice | Preference of user interface is dependent of the task to be completed and the abilities of the users. Combining several user interfaces provides increased interaction opportunities in line with the tasks and users abilities. When creating a serious game intervention, it is paramount to consider the types of devices in use, the patients’ abilities, and their motivation to play |
| • Combining UI | |||
| • Participant Ability | |||
| • Motivation | |||
| De Vries et al. (2018) | No standardized UX measures | • Motivation | Older adults were motivated to play VR balance games, and this was also linked with high enjoyment and value scores indicating that motivation was correlated with enjoyment of the game and the perceived value of the exercise |
| • Enjoyment | |||
| • Value | |||
| Yeh et al. (2019) | No standardized UX measures | • Value | No discussion regarding usability, feasibility or design considerations for technology used however, the researchers did discuss factors which impact willingness to participant/use VR interventions. These factors included perceiving the value of the intervention, and the use of enjoyment/fun to increase motivation |
| • Enjoyment | |||
| • Motivation |
Usability, feasibility and design considerations.
Usability
The most common factors identified as vital to usability were enjoyment and motivation. Many of the articles noted that participants reported either feeling enjoyment or a need to enjoy the activity to continue with the interventions. Similarly, motivation was identified as essential to continued engagement with the interventions over time. The remaining themes were not identified as often but were nonetheless important. Usability was dependent on participants receiving clear and simple instructions (Corno et al., 2014) and/or taking part in environments that were designed with clear and simple layouts (Blackman et al., 2007; Liu, 2010; Lokka et al., 2018). The concept of “matching” came up in three separate studies, though each with a different emphasis. Benoit et al. (2015) identified the importance of creating an environment where both the virtual and the real-world mirror each other (e.g., sitting at a table in a virtual environment, and sitting a table of similar height in the real-world) to help reduce the symptoms of cybersickness. Gomes et al. (2018) discusses the impact of games where the user/avatar appears stationary, but the user is required to take quick steps in the real-world and how this could result in adverse effects for the user. However, despite identifying this concern, they made no attempt to prevent or propose solutions. Finally, Korsgaard et al. (2019) considered the potential to increase use and willingness to use VR technology and applications through weather matching, or rather “miss-matching.” The ability of VR environments to provide a warm comfortable outside environment for exercise and other activities may entice older adult users into engaging with the technology on cold, wet days when they are unable to leave their homes. Perceived value of an intervention also had an impact on the usability of a piece of technology or virtual environment. Participants who could see how the exercise would help them were more likely to continue an intervention to the end and they were more likely to link it with their motivation to continue. How easy the technology was to use (Tsuda et al., 2016; Glännfjord et al., 2017) also played a part in the usability of the system; however, it was surprising that this factor was not mentioned more across the identified studies. Participant comfort considered both the equipment being used (Anderson-Hanley et al., 2011) and the features of users (e.g., eyeglasses) (Korsgaard et al., 2019), though again, not many findings or observations were identified. Other factors which played a part in the overall usability of a system included providing participants with a challenge (Merriman et al., 2018), choice of different user interfaces (Vallejo et al., 2014) so their motions/interactions are identified/picked-up, providing an environment that is consistent (Corno et al., 2014) with expectations (e.g., colors are not too bright etc.), easy to engage with (Manera et al., 2016), using simple user interfaces (Corno et al., 2014) and social interaction (Glännfjord et al., 2017) where the ability to compete and take part with others influenced participants decisions to continue engaging with the interventions.
Feasibility
Three studies considered the importance of safety in regards to the feasibility of their intervention. One study considered how the intervention itself provided additional safety to its participants when compared to completing a similar intervention in a real-world setting (Anderson-Hanley et al., 2011), another considered the impact simulator sickness may have on individuals with schizophrenia and determined there set-up was a safe alternative to HMD’s (Chan et al., 2010) and another considered the increased safety VR systems could provide to chemotherapy patients required to remain in clean-rooms (Tsuda et al., 2016). One study noted gender differences as a feasibility consideration (Matas et al., 2015); women were more prone to both motion and simulator sickness and the authors went on to suggest that drivers with a history of motion sickness should not take part in any immersive driving simulations. Participants inherent abilities should also be taken into consideration of the feasibility of a AR/VR set-up (Vallejo et al., 2014) as overly mismatching their ability to the task could pre-dispose participants to reduced motivation and incompletion of the intervention. This is in-line with research that argues that tasks themselves be tailored to the population (Corno et al., 2014). The final theme identified in this category related to older adults ability to understand the combining of virtual and real aspects of a mixed reality setting; for example, understanding that they could eat “anywhere” within the virtual environment even though no tables were visible despite having spent time in that environment while seated at their own table (Korsgaard et al., 2019). This is of particular importance as older adults and those with cognitive impairment must understand the environments they are immersed in so as to avoid any upset or negative effects on the participant.
Tailored Design
The final category could be broken into seven themes. Realism was identified as an important factor in continued use of a system (Marivan et al., 2016) but it was also worth noting that the level of realism was important for older adult populations (Lokka et al., 2018). Older adults initially preferred the realistic environment and a small percentage switched to using a mixed reality environment. However, despite the switch, over 50% of the older adults’ participants continued to prefer the realistic environment compared with a younger population. This is interesting as this research suggests that the mixed environment produced better recall (both long and short-term) in younger and older adult populations. This poses an interesting ethical dilemma that merits further examination; if personal choice and preference is important in establishing and retaining participant trust, comfort, and engagement until the end of an intervention, but researcher selected equipment and environments are expected to demonstrate greater efficacies, is it justifiable to remove those choices? Are the potential results, the expected savings in study finance, resources, and time acceptable reasons for limiting interventions with these vulnerable populations?
Many studies using AR/VR use navigation tasks to assess memory and attention in cognitively impaired populations. Active navigation is an interesting factor to consider as it requires the participant to navigate a virtual environment themselves using some form of UI, whereas passive navigation typically demonstrates a route or direction through pre-recorded video. Active navigation increases recognition hits in older adults, however it also increases false positives in older adult populations (Sauzéon et al., 2016). Often it is both necessary and preferred that participants actively engage in a virtual intervention, but if there is a possibility that the subsequent results are Type 1 errors, then checks and controls should be built into the intervention procedures. An interesting interaction between education level and computer self-efficacy was also reported (Felnhofer et al., 2014). Older adults with higher education were better able and more confident in using the virtual environments. Many current older adults may have missed educational opportunities due to historic circumstance, however as education levels in the global aging population increase, progressively more and more older adults will be proficient technology users. Researchers should no longer assume older populations are technologically illiterate. Older adults are more capable than ever at interacting with complex technology, but there is still a learning curve. It has been suggested that when instructing participants on the procedure of an intervention or task, they should first be introduced to the technology and allowed to interact with it (Corno et al., 2014). Adjustment periods ensure that participants do not become distracted by the technology during the data collection period. The level of immersion is also an important factor to consider for Alzheimer’s and Dementia populations. There may be an assumption that these populations can become confused with high levels of immersion or through the use of 3D glasses but Manera et al. (2016) found that participants preferred the 3D environment when compared with a 2D paper task. Similarly, research with Parkinson’s patients (dos Santos Mendes et al., 2012) has noted that also they can have difficulty with virtual games due to increased motor difficulties, this does not prevent them from learning, improving and retaining the positive effects of exergaming. In contrast, those with cognitive impairment are more likely to experience inhibited learning.
The key take home message across these studies is the importance of positive user experience influencing the usability and feasibility of AR/VR environments and technologies (Vallejo et al., 2014, p. 24; Yeh et al., 2019, p. 10).
Increasingly, research is being conducted with the assistance of experts by experience (public, patient involvement; PPI). The is an important paradigm shift for researchers. By asking living experts to help design (make suggestions), and evaluate virtual environments as they are created you increase the likelihood that your intervention will meet the needs and requirements necessary for that population group (Corno et al., 2014). By including PPI researchers will address two vital factors for feasibility of AR/VR research interventions, designing tasks with a population in mind and matching the abilities of the participants to the task.
The Lack of Augmented Reality
This review indicates that AR is rarely being used as a form of digital intervention. There are many reasons for this. When the original articles were screened for title and abstract two main clusters of articles were identified that closely matched the current search but were different enough to warrant exclusion. These included articles where AR/VR were used as either a means of diagnosis or studies that used virtual technology as a convenient alternative to a potentially dangerous real-world setting; the effects of the virtual environment or equipment was not itself examined. A greater number of AR papers may have fallen into these alternate categories. Another reason AR technology may have been absent from these results is the current focus of AR studies. Much of the research employs smart-phone applications (such as Pokémon Go), which older adults are less likely to engage with. AR also features in research in the areas of education, tourism, and advertising; areas where digital interventions are not always targeted toward older adults. In comparison to VR, many AR studies may still be in their infancy and while they would suit an older population, research tends not to be directed to those 60°years and above. Finally, several studies in this review include samples where younger participants were present, but where older adults’ results were reported separately. AR research may not yet categorize their samples to the degree required by this review.
VR-Based Interventions
This review has identified several sub-populations and areas of interest where virtual reality technology is being used to affect the physical/mental health and wellbeing of older adults. Populations include healthy, physically, and cognitively impaired, and emotionally vulnerable older adults (Tarnanas et al., 2015, p. 3; Wiederhold, 2016, p. 577–578; Riva et al., 2019, p. 82–88). VR technology has demonstrated its positive impacts using immersive environments that can display games, exercises and true-to-life digitally created surroundings. The environments in the 65 studies in this review were used to increase physical activity, improve balance, memory, attention, and quality of life, and to reduce falls, anxiety, and depression. The most common limitations described included small sample sizes not representative of the larger populations (including limited gender balances), a lack of control groups, limited access to technical (gameplay) data and short intervention periods often due to a lack of time/resources. Future research in this area should look at large scale studies with interventions capable of being personalized and meeting the recommended length of time for behavior change (12 weeks). Participants should be more representative of the general population with gender, education level, ethnicity and socioeconomic status all taken into consideration. Technical interventions should include neurobiological assessments as control measures to further support physical and cognitive change assessments. Areas needing further exploration include, active identify of older adults and its role in influencing VR related exercise behavior (Anderson-Hanley et al., 2011), acceptance of VR supported interventions in hospital-bound populations (Korsgaard et al., 2019), the experience of immersion and flow in 3D VR training (Lee et al., 2017), and investigating natural user interfaces to allow for simultaneous dual motion input (Vallejo et al., 2014).
Theories in Practice
This review drew attention to four well known theories (Riva et al., 2016) that can be applied to AR/VR research. The authors expected to find these theories being used to support the methodologies used by the identified articles but only nine papers used psychological theory to support their intervention. Unexpectedly, none of the theories put forth by Riva and colleagues (2016) were used. However, the 13 theories adopted by researchers to support AR/VR research (see Table 6 above) were also based on social, cognitive, and biopsychosocial frameworks. Most of the theories were social, and a common theme included the influence of others of behavior (38%). Other areas of effect included impact of the surrounding environment (23%), intrinsic motivation of the individual (7%) and interaction with cognitive processes (38%). These studies clearly demonstrate the psychological underpinnings related to and influencing the effects of AR/VR methodological design. However, most studies evaluated in this review offered no theoretical support for their experimental design. Behavior change research is complex and often interventions designed to effect change are activating many interconnected components that work together to produce a response. Even when an intervention is successful, the lack of appropriate theoretical supports means there is no way to accurately determine what underpinned this success (Michie et al., 2014). Future researchers must reconsider incorporating psychological theory to provide strong foundations from which to develop effective, lasting and, impactful AR/VR interventions.
Specific Domains
Within the social domain, the theories addressed the impact of others on the behaviors of the individual during interventions. The transformative Learning Theory model was also based in a social framework and while it was not referenced specifically, common aspects of this theory included, recognition of the self and revision of beliefs leading to behavior change. The cognitive domain was more prominent in the theories presented by Riva et al. (2016) but these theories were less frequent in the identified literature. However, these theories are similar in that the place the self at the forefront and behavior change is influenced by our perceptions. Socio-cognitive and biopsychosocial models were presented as explanations for behavior change and while these models were the least incorporated, they are the most complex supporting explanations for behavior changes because of complex interconnections between the environment, cognition, social influences, biological predispositions, and psychological health.
Defining Virtual and Augmented Reality
When searching the literature for virtual and augmented reality research it became clear that there was no single definition in use. Many studies used terms like virtual, augmented, and mixed reality to describe 3D virtual environments displayed onto 2D desktop environments. The “reality-virtuality continuum” (Eckert et al., 2019, p. 2) suggests that terms like “virtual environment” and “virtual reality” can be used to describe these two-dimensional displays. However, AR/VR technologies have advanced beyond the systems available in the 1990s and the continuum does not accurately differentiate digitally created environments. A desktop environment like Sims™ or Second Life™ can be called a “virtual environment” but so too can an immersive display in a HMD like the Oculus Rift™. Only 16 of 65 papers in this review provided a definition of VR. All 16 definitions considered the digitally created environment and real-time interaction, but only seven also mentioned the user (See Table 4) and only one defined “mixed reality;” a term often used to describe the combination of virtual and augmented reality technology elements. The remaining definitions described only the technical elements (e.g., computer simulated environment, interaction of computer-generated experience) required to create VR. This illustrates an interesting distinction between papers that focus solely on the technical components (50%) and those that consider the human interaction as a vital step in the virtuality process. There is no clear way to determine which approach is more successful in terms of reaching the objectives of the planned intervention however, future research could set out to identify the definitions/descriptions used in quantitative AR/VR research and complete a meta-analysis comparing the outcomes of the studies. In general, these findings support those of Kardong-Edgren et al. (2019), (p. 33) who identified 14 different VR definitions and six different AR definitions in their review. These combinations of ambiguity and opposing perspectives contributes to the complexity of true AR/VR and clearly demonstrates the need for a more robust taxonomy. This review also aimed to determine if consistent terminology was being used in AR/VR research. Only five studies using the term VR involved a fully immersive virtual environment. The remaining 57 studies used variations of “virtual reality” and “virtual environments” to describe their technology. Over 70% of studies in this analysis mislabeled themselves as “virtual reality” and this may be attributed to two main factors. First, very few studies provided an operational definition of virtual reality and this leads to ambiguities and misunderstandings as readers attempt to ascribe a label to the technology used. Second, while virtual (Milgram and Kishino, 1994, p. 8–12) and augmented reality (Grubert et al., 2017, p. 1711–1715; Hugues et al., 2011, p. 5–15) taxonomies exist, they do not accurately describe the modern technologies available (e.g., describing analogue or digital monitors), which adds further confusion to an already complex and quickly evolving area.
These inconsistent terms and definitions emphasize the need for more sophisticated terminology to describe virtual designs. In addition, one study described their set-up as a virtual reality, referring to a video they had taken as a virtual environment (Choi and Lee, 2019, p. 862). Under the “reality-virtuality continuum” (Eckert et al., 2019, p. 2) this identification is legitimate, but it is inaccurate. Asking participants to watch a video and follow along with the motions is not the same as a participant interacting in real-time within a 3D virtual environment that can track movement and provide an immersive user experience. While the definitions of McCloy and Stone (2001), (p. 912) Botella et al. (2015), (p. 2) used in planning this review are the most acceptable definitions that are currently available, greater nuance is required to convey fully the degree and level of immersion required in a virtual reality system. Based on the definitions identified in this review and those identified in the call for unification of virtual reality theories (Kardong-Edgren et al., 2019, p. 30–31), we have identified the following elements which are required to formulate a more complete definition. There must be reference to 3D graphics displayed in either 2-or-3 dimensions. This should include everything from projector screens, television sets, computer monitors and HMD’s. The second element of a new definition should address the level of interaction available to the users including multimodal systems combining the senses to create full-body experiences and increasing levels of user interfaces ranging from controllers and joysticks to motion control, position tracking and multi-modal interface in-puts. Finally, a new definition should include the ability to view the environment and any avatars in either first or third person perspective. This is a complicated task as even with these factors there are many levels of technology included. To fully address the insufficient language and terminology in this complex area, an updated taxonomy classifying virtual and augmented technologies is urgently required.
Strengths and Limitations
This review evaluated many studies to determine how AR/VR is used when aiming to improve physical/mental health and general wellbeing of older adults. The analysis clearly demonstrates the assortment of technologies available, but also the insufficient terminology available to categorize and identify them. Two researchers conducted the screening for this review ensuring consensus was reached on all points. Finally, three systematic reviews (Hugues et al., 2011; Miller et al., 2014; Coyle et al., 2015) identified in the screening process were used to supplement the initial search and an additional 13 studies were included in this review.
Two branches of AR/VR research were not included in this review (use as a diagnostic tool and use as a methodology rather than the factor under investigation) due to time constraints. Both areas are large enough to warrant their own review. Another limitation to this study is the lack of AR research found. This may be due to the focus on older adults in this review, or that AR research may not report the older participants as an individual group. Another factor may be the availability of AR technology. Newer models of smart phones and tablets may be AR compatible, but these may not be used to the same extent in an older population.
Conclusion
This scoping review aimed to identify how AR/VR technology was used within an older adult population to influence their physical, mental health and wellbeing. Only five studies were objectively classified as VR and only one study used AR. However, these studies encompassed a wide range of domains including improving physical activity, balance, memory, attention, and quality of life, and reducing falls, anxiety, and depression. A secondary aim of this study was to identify whether the terminology used across the studies was consistent. Findings have demonstrated that terms such as virtual reality and virtual environments are used to describe many levels of technology. Many of the papers discussed in this review provide no definition of virtual reality and those that do, lack consensus. Further, half of these definitions fail to include the user despite the user being central to the intervention being conducted. This review has proposed the elements necessary to construct an alternative definition. It also urgently calls for an updated taxonomy to address the varying levels of technology and immersion used in today’s virtual reality research. Similarly, there are many useful theories that can bring focus to the factors influencing behavior change. When designing these interventions, the authors urge researchers to do so with a strong theoretical foundation.
Statements
Author contributions
The main body of research was conducted by JC supported by LH and AF. Contributors to the paper include, RL-V, PB, and EK.
Funding
This review was undertaken as part of the CAPTAIN Project–Horizon 2020: European Union Funding for Research and Innovation Call: S1-PM-15-2017.
Conflict of interest
Author EK was employed by the company WITA.
The remaining authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Supplementary material
The Supplementary Material for this article can be found online at: https://www.frontiersin.org/articles/10.3389/frvir.2021.655338/full#supplementary-material
References
1
AgmonM.PerryC. K.PhelanE.DemirisG.NguyenH. Q. (2011). A Pilot Study of Wii Fit Exergames to Improve Balance in Older Adults. J. Geriatr. Phys. Ther.34 (4), 161–167. 10.1519/JPT.0b013e3182191d98
2
AjzenI. (1991). The Theory of Planned Behavior. Organiz. Behav. Human Dec. Proc.50, 179–211. 10.1016/0749-5978(91)90020-T
3
AllportF. (1995). The Influence of the Group upon Association and Thought (1920). In Small Groups: Studies in Social Interaction. Editors P. Hare, E. F. Borgatta, and R. F. Bales, 31–34.
4
Anderson-HanleyC.ArcieroP. J.BarcelosN.NimonJ.RochaT.ThurinM.et al (2014). Executive Function and Self-Regulated Exergaming Adherence Among Older Adults. Front. Hum. Neurosci., 8(989) 1–8. 10.3389/fnhum.2014.00989
5
Anderson-HanleyC.ArcieroP. J.BrickmanA. M.NimonJ. P.OkumaN.WestenS. C.et al (2012). Exergaming and Older Adult Cognition: A Cluster Randomized Clinical Trial. Am. J. Prev. Med., 42(2), 109–119. 10.1016/j.amepre.2011.10.016
6
Anderson-HanleyC.SnyderA. L.NimonJ. P.ArcieroP. J. (2011). Social Facilitation in Virtual Reality-Enhanced Exercise: Competitiveness Moderates Exercise Effort of Older Adults. Clin. interventions Aging6, 275. 10.2147/CIA.S25337
7
AndersonJ. R. (2002). Spanning seven orders of magnitude: A challenge for cognitive modeling. Cognitive Sci.26, 85–112. 10.1207/s15516709cog2601_3
8
BachaJ. M. R.GomesG. C. V.de FreitasT. B.ViveiroL. A. P.da SilvaK. G.BuenoG. C.et al (2018). Effects of Kinect Adventures Games versus Conventional Physical Therapy on Postural Control in Elderly People: A Randomized Controlled Trial. Games Health J.7 (1), 24–36. 10.1089/g4h.2017.0065
9
BarbosaC. F. M.PavanelliI. L.SilvaT. D. O. S.JúniorP. R. R.do NascimentoG. B. (2019). Effectof Virtual Reality on the Intensity of Dizziness and Quality of Life in the Elderly Withunilateral Vestibular Hypo-Function. Fisoterapia Brasil, 20 (2), 278 – 287. 10.33233/fb.v20i2.2846
10
BellC. S.FainE.DaubJ.WarrenS. H.HowellS. H.SouthardK. S.et al (2011). Effects of Nintendo Wii on Quality of Life, Social Relationships, and Confidence to Prevent Falls. Phys. Occup. Ther. Geriatr., 29(3), 213–221. 10.3109/02703181.2011.559307
11
BenoitM.PetitP. D.ManeraV. (2015). Is it Possible to Use Highly Realistic Virtual Reality in the Elderly? a Feasibility Study with Image-Based Rendering. Neuropsychiatr. Dis. Treat., 11, 557–563. 10.2147/NDT.S73179
12
BissonE.ContantB.SveistrupH.LajoieY. (2007). Functional Balance and Dual-Task Reaction Times in Older Adults Are Improved by Virtual Reality and Biofeedback Training. Cyberpsychology Behav.10 (1), 16–23. 10.1089/cpb.2006.9997
13
BlackmanT.Van SchaikP. A. U. L.MartyrA. (2007). Outdoor Environments for People with Dementia: an Exploratory Study Using Virtual Reality. Ageing Soc.27 (6), 811. 10.1017/S0144686X07006253
14
BotellaC.Pérez-AraM. A.Bretón-LópezJ.QueroS.García-PalaciosA.BañosR. M. (2015). In Vivo versus Augmented Reality Exposure in the Treatment of Small Animal Phobia: A Randomized Controlled Trial. PLOS ONE11 (2). 10.1371/journal.pone.0148237
15
BotellaC.RivaG.GaggioliA.WiederholdB. K.AlcanizM.BañosR. M. (2012). The Present and Future of Positive Technologies. Cyberpsychology, Behav. Soc. Networking15 (2), 78–84. 10.1089/cyber.2011.0140
16
CacciataM.StrombergA.LeeJ. A.SorkinD.LombardoD.ClancyS.et al (2019). Effect of Exergaming on Health-Related Quality of Life in Older Adults: A Systematic Review. Int. J. Nurs. Stud., 93, 20 – 40. 10.1016/j.ijnurstu.2019.01.010
17
ChanC. L.NgaiE. K.LeungP. K.WongS. (2010). Effect of the Adapted Virtual Realitycognitive Training Program Among Chinese Older Adults with Chronic Schizophrenia: A Pilot Study. Int. J. Geriatr. Psychiatry A J. Psychiatry Late Life Allied Sci.25 (6), 643–649. 10.1002/gps.2403
18
ChoiW.LeeS. (2019). The Effects of Virtual Kayak Paddling Exercise on Postural Balance, Musical Performance, and Cognitive Function in Older Adults with Mild Cognitive Impairment; a Randomized Controlled Trial. J. Aging Phys. Activity, 27(6), 861–870. 10.1123/japa.2018-0020
19
CornoG.BouchardS.ForgetH. (2014). Usability Assessment of the Virtual Multitasking Test (V-mt) for Elderly People. Annu. Rev. Cyberther. Telemed199, 168–172. 10.3233/978-1-61499-401-5-168
20
CoyleH.TraynorV.SolowijN. (2015). Computerized and Virtual Reality Cognitive Training for Individuals at High Risk of Cognitive Decline: Systematic Review of the Literature. Am. J. Geriatr. Psychiatry, 23(4), 335–359. 10.1016/j.jagp.2014.04.009
21
De VriesA. W.Van DieënJ. H.Van Den AbeeleV.VerschuerenS. M. (2018). Understanding Motivations and Player Experiences of Older Adults in Virtual Reality Training. Games Health J.7 (6), 369–376. 10.1089/g4h.2018.0008
22
dos Santos MendesF. A.PompeuJ. E.LoboA. M.da SilvaK. G.de Paula OliveiraT.ZomignaniA. P.et al (2012). Motor Learning, Retention, and Transfer after Virtual-Reality-Based Training in Parkinson's Disease–Effect of Motor and Cognitive Demands of Games: a Longitudinal, Controlled Clinical Study. Physiotherapy, 98(3), 217–223. 10.1016/j.physio.2012.06.001
23
EckertM.VolmergJ. S.FriedrichC. M. (2019). Augmented Reality in Medicine: Systematic and Bibliographic Review. JMIR Mhealth Uhealth7 (4), e10967. 10.2196/10967
24
EggenbergerP.SchumacherV.AngstM.TheillN.de BruinE. D. (2015). Does Multicomponent Physical Exercise with Simultaneous Cognitive Training Boost Cognitive Performance in Older Adults? A 6-month Randomized Controlled Trial with a 1-year Follow-Up. Clin. Interventions Aging10, 1335–1349. 10.2147/CIA.S87732
25
Eurostat(2020). Demographic Balances and Indicators by Type of Projection: Proportion of population aged 65 years or more [Data set]. Avaliable at: https://appsso.eurostat.ec.europa.eu/nui/submitViewTableAction.do dataset
26
FasilisT.PatrikelisP.SiatouniA.AlexoudiA.VeretziotiA.ZachouL.et al (2018). A Pilot Study and Brief Overview of Rehabilitation via Virtual Environment in Patients Suffering from Dementia. Psychiatriki = Psychiatriki29 (1), 42–51. 10.22365/jpsych.2018.291.42
27
FelnhoferA.KothgassnerO. D.HaukN.BeutlL.HlavacsH.Kryspin-ExnerI. (2014). Physical and Social Presence in Collaborative Virtual Environments: Exploring Age and Gender Differences with Respect to Empathy. Comput. Hum. Behav., 31, 272–279. 10.1016/j.chb.2013.10.045
28
FrancoJ. R.JacobsK.InzerilloC.KluzikJ. (2012). The Effect of the Nintendo Wii Fit and Exercise in Improving Balance and Quality of Life in Community Dwelling Elders. Tech. Health Care20 (2), 95–115. 10.3233/THC-2011-0661
29
GamitoP.OliveiraJ.MoraisD.CoelhoC.SantosN.AlvesC.et al (2019). Cognitive Simulation of Elderly Individuals with Instrumental Virtual Reality-Based Activities of Daily Life: Pre-post Treatment Study. Cyberpsychology, Behav. Soc. Networking22 (1), 69–75. 10.1089/cyber.2017.0679
30
GamitoP.OliveiraJ.RosaP.MoraisD.DuarteN.OliveiraS.et al (2010). PTSD Elderly War Veterans: A Clinical Controlled Pilot Study. Cyberpsychology, Behav. Soc. Networking13 (1), 43–48. 10.1089/cyber.2009.0237
31
GlännfjordF.HemmingssonH.Larsson RanadaÅ. (2017). Elderly People’s Perceptions of Using Wii Sports Bowling - A Qualitative Study. Scand. J. Occup. Ther.24 (5), 329–338. 10.1080/11038128.2016.1267259
32
GomesG. C. V.do Socorro SimõesM.LinS. M.BachaJ. M. R.ViveiroL. A. P.VariseE. M.et al (2018). Feasibility, Safety, Acceptability, and Functional Outcomes of Playing Nintendo Wii Fit PlusTM for Frail Older Adults: A Randomized Feasibility Clinical Trial. Maturitas, 118, 20–28. 10.1016/j.maturitas.2018.10.002
33
GraffignaG.BarelloS.RivaG. (2013). Technologies for Patient Engagement. Health Aff.32 (6), 1172. 10.1377/hlthaff.2013.0279
34
GrubertJ.LanglotzT.ZollmannS.RegenbrechtH. (2017). Towards Pervasive Augmented Reality: Context-Awareness in Augmented Reality. IEEE Trans. Visualization Comp. Graphics23 (6), 1706–1723. 10.1109/TVCG.2016.2543720
35
Guisado-FernándezE.GiuntiG.MackeyL. M.BlakeC.CaulfieldB. M. (2019). Factors Influencing the Adoption of Smart Health Technologies for People with Dementia and Their Informal Caregivers: Scoping Review and Design Framework. JMIR Aging2 (1), e12192. 10.2196/12192
36
HallP. A.FongG. T. (2007). Temporal self-regulation theory: A model for individual health behavior. Psychol. Rev.1, 6–52. 10.1080/17437190701492437
37
HavighurstR. J. (1961). Successful Aging1. The Gerontologist1, 8–13. 10.1093/geront/1.1.8
38
HsiehC. C.KinP. S.HsuW. C.WangJ. S.HuangY. C.LimA. Y.et al (2018). The Effectiveness of a Virtual Reality-Based Tai Chi Exercise on Cognitive and Physical Function in Older Adults with Cognitive Impairment. Demen. Geriatr. Cogn. Disord.46 (5–6), 358–370. 10.1016/j.physio.2015.03.3418
39
HuguesO.FuchsP.NannipieriO. (2011). “New Augmented Reality Taxonomy: Technologies and Features of Augmented Environment,” in Handbook of Augmented Reality. Editor FurhtB. (New York: Springer-Verlag), 47–63. 10.1007/978-1-4614-0064-6_2
40
HuthK.Amar-DolanL.PerezJ. M.LuffD.CohenA. P.GladerL.et al (2020). Visiting Jack: Mixed Methods Evaluation of a Virtual home Visit Curriculum with a Child with Medical Complexity. Acad. Pediatr., 20(7), 10.1016/j.acap.2020.05.001
41
KahlbaughP. E.SperandioA. J.CarlsonA. L.HauseltJ. (2011). Effects of Playing Wii on Well-Being in the Elderly: Physical Activity, Loneliness, and Mood. Activities. Adaptation & Aging35 (4), 331–344. 10.1080/01924788.2011.625218
42
KarahanA. Y.TokF.TaşkınH.KüçüksaraçS.BaşaranA.YıldırımP. (2015). Effects of Exergames on Balance, Functional Mobility, and Quality of Life of Geriatrics versus home Exercise Programme: Randomized Controlled Study. Cent. Eur. J. Public Health, 23(Suppl. ment), S14–S18. 10.21101/cejph.a4081
43
Kardong-EdgrenS.FarraS. L.AlinierG.YoungH. M. (2019). A Call to Unify Definitions of Virtual Reality. Clin. Simulation Nurs.31. 28–34. 10.1016/j.ecns.2019.02.006
44
KelmanH. C. (1958). Compliance, identification, and internalization three processes of attitude change. J. Conflict Resolut.2, 51–60. 10.1177/002200275800200106
45
KitsonA.PrpaM.RieckeB. E. (2018). Immersive Interactive Technologies for Positive Change: A Scoping Review and Design Considerations. Front. Psychol.91354. 10.3389/fpsyg.2018.01354
46
KizonyR.LevinM. F.HugheyL.PérezC.FungJ. (2010). Cognitive Load and Dual-Task Performance during Locomotion Poststroke: A Feasibility Study Using a Functional Virtual Environment. Phys. Ther., 90, 252 – 260. 10.2522/ptj.20090061
47
KizonyR.WeissP.ShaharM.RandD. (2006). TheraGame–a home Based Virtual Reality Rehabilitation System. Denmark: Esbjerg. 10.1515/IJDHD.2006.5.3.265
48
KnowlesL. M.StelzerE-M.JovelK. S.O’ConnorM-F. (2017). A Pilot Study of Virtual Support for Grief: Feasibility, Acceptability, and Preliminary Outcomes. Comput. Hum. Behav., 73, 650 – 658. 10.1016/j.chb.2017.04.005
49
KorsgaardD.BjønerT.NilssonN. C. (2019). Where Would You like to Eat? A Formative Evaluation of Mixed-Reality Solitary Meals in Virtual Environments for Older Adults with Mobility Impairments Who Live Alone. Food Res. Int., 117, 30–39. 10.1016/j.foodres.2018.02.051
50
LaverK.GeorgeS.RatcliffeJ.QuinnS.WhiteheadC.DaviesO.et al (2012). Use of an Interactive Video Gaming Program Compared with Conventional Physiotherapy for Hospitalised Older Adults: a Feasibility Trial. Disabil. Rehabil.34 (21), 1802–1808. 10.3109/09638288.2012.662570
51
LeeM.SonJ.KimJ.YoonB. (2015). Individualized Feedback-Based Virtual Reality Exercise Improves Older Women’s Self-Perceived Health: A Randomized Controlled Trail. Arch. Gerontol. Geriatr.61(2), 154–160. 10.1016/j.archger.2015.06.010
52
LeeS.ShinS. (2013). Effectiveness of Virtual Reality Using Video Gaming Technology in Elderly Adults with Diabetes Mellitus. Diabetes Technol. Ther.15 (6), 489–496. 10.1089/dia.2013.0050
53
LeeY.ChoiW.LeeK.SongC.LeeS. (2017). Virtual Reality Training with Three-Dimensional Video Games Improves Postural Balance and Lower Extremity Strength in Community-Dwelling Older Adults. J. Aging Phys. Activity, 25(4), 621–627. 10.1123/japa.2015.2015-0271
54
LevyF.LeboucherP.RautureauG.KomanoO.MilletB.JouventR. (2016). Fear of Falling: Efficacy of Virtual Reality Associated with Serious Games in Elderly People. Neuropsychiatr. Dis. Treat.12, 877–881. 10.2147/NDT.S97809
55
LiuC. L. (2010). The Impact of Goods-Classification and Landmarks for Spatial Knowledge and Goods-Finding in the Elderly within a 3D Virtual Store. Comput. Hum. Behav., 26(6), 1777–1786. 10.1016/j.chb.2010.07.005
56
LokkaI. E.ÇöltekinA.WienerJ.FabrikantS. I.RöckeC. (2018). Virtual Environments as Memory Training Devices in Navigational Tasks for Older Adults. Scientific Rep.8 (1), 1–15. 10.1038/s41598-018-29029-x
57
ManD. W.ChungJ. C.LeeG. Y. (2012). Evaluation of a Virtual Reality-Based Memory Training Programme for Hong Kong Chinese Older Adults with Questionable Dementia: a Pilot Study. Int. J. Geriatr. Psychiatry27 (5), 513–520. 10.1002/gps.2746
58
ManeraV.ChapoulieE.BourgeoisJ.GuerchoucheR.DavidR.OndrejJ. (2016). A Feasibility Study with Image-Based Rendered Virtual Reality in Patients with Mild Cognitive Impairment and Dementia. PLoS ONE11 (3), e0151487. 10.1371/journal.pone.0151487
59
MarivanK.BoullyC.BenvenisteS.ReingewirtzS.RigaudA.-S.KemounG.et al (2016). Rehabilitation of the Psychomotor Consequences of Falling in an Elderly Population: A Pilot Study to Evaluate Feasibility and Tolerability of Virtual Reality Training. Tech. Health Care24 (2), 169–175. 10.3233/THC-151114
60
MatasN. A.NettelbeckT.BurnsN. R. (2015). Dropout during a Driving Simulator Study: a Survival Analysis. J. Saf. Res., 55, 159–169. 10.1016/j.jsr.2015.08.004
61
MayerR. E.MorenoR. (2003). Nine Ways to Reduce Cognitive Load in Multimedia Learning. Educ. Psychol.38, 43–52. 10.1207/S15326985EP3801_6
62
McCloyR.StoneR. (2001). Virtual Reality in Surgery. Bmj323 (7318), 912–915. 10.1136/bmj.323.7318.912
63
MerrimanN. A.RoudaiaE.RomagnoloiM.OrvietoI.NewellF. N. (2018). Acceptability of a custom-designed game, CityQuest, aimed at improving balance confidence and spatial cognition in fall-prone and healthy older adults, Behav. Inf. Tech., 37(6), 538 – 557. 10.1080/0144929X.2018.1462402
64
MerrimanN. A.WhyattC.SettiA.CraigC.NewellF. N. (2015). Successful Balance Training Is Associated with Improved Multisensory Function in Fall-Prone Older Adults. Comput. Hum. Behav., 45, 192–203. 10.1016/j.chb.2014.12.017
65
MichieP. S.WestP. R.CampbellP. R.BrownD. J.GainforthD. H. (2014). ABC of Behaviour Change Theories. Silverback Publishing.
66
MilgramP.KishinoF. (1994). A Taxonomy of Mixed Reality Visual Displays. IEICE Trans. Inf. Syst.E77 (12), 1321–1329. 10.1.1.102.4646
67
MillerK. J.AdairB. S.PearceA. J.SaidC. M.OzanneE.MorrisM. M. (2014). Effectiveness and Feasibility of Virtual Reality and Gaming System Use at home by Older Adults for Enabling Physical Activity to Improve Health-Related Domains: a Systematic Review. Age and ageing, 43(2), 188–195. 10.1093/ageing/aft194
68
MirelmanA.MaidanI.HermanT.DeutschJ. E.GiladiN.HausdorffJ. M. (2011). Virtual Reality for Gait Training: Can it Induce Motor Learning to Enhance Complex Walking and Reduce Fall Risk in Patients with Parkinson’s Disease?. The Journals Gerontol. Ser. A66 (2), 234–240. 10.1093/Gerona/glq201
69
Monteiro-JuniorR. S.da Silva FigueiredoL. F.de Tarso Maciel-PinheiroP.AbudE. L. R.BragaA. E. M. M.BarcaEngedalM. L. K.et al (2017). Acute Effects of Exergames on Cognitive Function of Institutionalized Older Persons: A Single-Blinded, Randomized and Controlled Pilot Study. Aging Clin. Exp. Res.29 (3), 387–394. 10.1007/s40520-016-0595-5
70
MoroneG.PaolucciT.LuziatelliS.IosaM.PiermatteiC.ZangrandoF.et al (2016). Wii Fit Is Effective in Women with Bone Loss Condition Associated with Balance Disorders: a Randomized Controlled Trial. Aging Clin. Exp. Res.28 (6), 1187–1193. 10.1007/s40520-016-0578-6
71
NgY. L.MaF.HoF. K.IpP.FuK. W. (2019). Effectiveness of Virtual and Augmented Reality-Enhanced Exercise on Physical Activity, Psychological Outcomes, and Physical Performance: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Comput. Hum. Behav., 99, 278–291. 10.1016/j.chb.2019.05.026
72
OptaleG.UrgesiC.BusatoV.MarinS.PironL.PriftisK.et al (2010). Controlling Memory Impairment in Elderly Adults Using Virtual Reality Memory Training: a Randomized Controlled Pilot Study. Neurorehabil. Neural Repair24 (4), 348–357. 10.1177/1545968309353328
73
PadalaK. P.PadalaP. R.LensingS. Y.DennisR. A.BoppM. M.ParkesC. M.et al (2017a). Efficacy of Wii-Fit on Static and Dynamic Balance in Community Dwelling Older Veterans: a Randomized Controlled Pilot Trial. J. Aging Res., 2017:4653635. 10.1155/2017/4653635
74
PadalaK. P.PadalaP. R.LensingS. Y.DennisR. A.BoppM. M.RobersonP. K.et al (2017b). Home-based Exercise Program Improves Balance and Fear Offalling in Community-Dwelling Older Adults with Mild Alzheimer’s Disease: a Pilot Study. J. Alzheimer's Dis.59 (2), 565–574. 10.3233/JAD-170120
75
PadalaK. P.PadalaP. R.MalloyT. R.GeskeJ. A.DubbertP. M.DennisR. A.et al (2012). Wii-fit for Improving Gait and Balance in an Assisted Living Facility: a Pilot Study. J. Aging Res., 2012:597573, 10.1155/2012/597573
76
ParijatP.LockhartT. E.LiuJ. (2014). EMG and Kinematic Responses to Unexpected Slips after Slip Training in Virtual Reality. IEEE Trans. Biomed. Eng.62 (2), 593–599. 10.1109/TBME.2014.2361324
77
ParkerM. G.WillettA. B.TysonS. F.WeightmanA. P.MansellW. (2020). A Systematic Evaluation of the Evidence for Perceptual Control Theory in Tracking Studies. Neurosci. Biobehavioral Rev., 112, 616–633. 10.1016/j.neubiorev.2020.02.030
78
RivaG.BañosR. M.BotellaC.MantovaniF.GaggioliA. (2016). Transforming Experience: The Potential of Augmented Reality and Virtual Reality for Enhancing Personal and Clinical Change. Front. Psychiatry7, 164. 10.3389/fpsyt.2016.00164
79
RivaG.WiederholdB. K.MantovaniF. (2019). Neuroscience of Virtual Reality: From Virtual Exposure to Embodied Medicine. Cyberpsychology, Behav. Soc. networking22 (1), 82–96. 10.1089/cyber.2017.29099.gri
80
RizzoA.KimG. J. (2005). Virtual Reality Rehabilitation and Therapy. PRESENCE: Teleoperators Virtual Environ.14, 119–146. 10.1162/1054746053967094
81
RodriguesE. V.GalloL. H.GuimaraesA. T. B.Melo FilhoJ.LunaB. C.GomesA. R. S. (2018). Effects of Dance Exergaming on Depressive Symptoms, Fear of Falling,and Musculoskeletal Function in Fallers and Nonfallers Community-Dwelling Older Women. Rejuvenation Res.21 (6), 518–526. 10.1089/rej.2017.2041
82
RosenbergD.DeppC. A.VahiaI. V.ReichstadtJ.PalmerB. W.KerrJ.et al (2010). Exergames for Subsyndromal Depression in Older Adults: a Pilot Study of a Novel Intervention. Am. J. Geriatr. Psychiatry18 (3), 221–226. 10.1097/JGP.0b013e3181c534b5
83
RoweJ. W.KahnR. L. (1997). Successful Aging1. The Gerontologist37, 433–440. 10.1093/geront/37.4.433
84
SápiM.DomjánA.Fehérné KissA.PintérS. (2019). Is Kinect Training Superior to Conventional Balance Training for Healthy Older Adults to Improve Postural Control?Games Health J., 8(1), 41–48. 10.1089/g4h.2018.0027
85
SauzéonH.N’KaouaB.Arvind PalaP.TailladeM.GuittonP. (2016). Age and Active Navigation Effects on Episodic Memory: A Virtual Reality Study. Br. J. Psychol.107 (1), 72–94. 10.1111/bjop.12123
86
SmaerupM.LaessoeU.GrönvallE.HenriksenJ. J.DamsgaardE. M. (2016). The Use of Computer-Assisted home Exercises to Preserve Physical Function after a Vestibular Rehabilitation Program: a Randomized Controlled Study. Rehabil. Res. Pract., 2016:7026317, 10.1155/2016/7026317
87
StadlerS.CornetH.TheotoT. N.FrenklerF. (2019). “A Tool, Not a Toy: Using Virtual Reality to Evaluate the Communication between Autonomous Vehicles and Pedestrians,” in Augmented Reality and Virtual Reality (Cham: Springer), 203–216. 10.1007/978-3-030-06246-0_15,
88
StudenskiS.PereraS.HileE.KellerV.Spadola-BogardJ.GarciaJ. (2010). Interactive Video Dance Games for Healthy Older Adults. J. Nutr. Health Aging14 (10), 850–852. 10.1007/s12603-010-0119-5
89
SunR.AldunateR. G.ParamathayalanV. R.RatnamR.JainS.MorrowD. G.et al (2019). Preliminary Evaluation of a Self-Guided Fall Risk Assessment Tool for Older Adults. Arch. Gerontol. Geriatr., 82, 94–99. 10.1016/j.archger.2019.01.022
90
SwellerJ. (1980). Transfer Effects in a Problem Solving Context. Quart. J. Exp. Pyschol.32, 233–239. 10.1080/14640748008401159
91
TarnanasI.PapagiannopoulosS.KazisD.WiederholdM.WiderholdB.TsolakiM. (2015). Reliability of a Novel Serious Game Using Dual-Task Gait Profiles to Early Characterize aMCI. Front. Aging Neurosci.7 (50), 1–15. 10.3389/fnagi.2015.00050
92
TennysonR. D.BreuerK. (1997). Psychological Foundations for Instructional Design Theory. In Instructional Design: International Perspectives I: Volume I: Theory, Research, and Models:volume Ii: Solving Instructional Design Problems.Editors R. D. Tennyson, F. Schott, N. M. Seel, & S. Dijkstra (Routledge). Available at:https://books.google.ie/books?hl=en&lr=&id=9dg6q9FO5H0C&oi=fnd&pg=PA113&ots=--htjWy83E&sig=MLn-G-31dDwcbFwuPxjsUdHSPlA&redir_esc=y#v=onepage&q&f=false
93
TriccoA. C.LillieE.ZarinW.O’BrienK. K.ColquhounH.LevacD.et al (2018). PRISMA Extension for Scoping Reviews (PRISMA-ScR): Checklist and Explanation. Ann. Intern. Med.169 (7), 467–473. 10.7326/M18-0850
94
TsudaK.SudoK.GotoG.TakaiM.ItokawaT.IsshikiT.et al (2016). A Feasibility Study of Virtual Reality Exercise in Elderly Patients with Hematologic Malignancies Receiving Chemotherapy. Intern. Med., 55(4), 347–352. 10.2169/internalmedicine.55.5275
95
VallejoV.TarnanasI.YamaguchiT.TsukagoshiT.YasudaR.MüriR.et al (2014). Usability assessment of natural user interfaces during serious games: Adjustments for dementia intervention. Virtual Reality, 8.http://www.icdvrat.reading.ac.uk/2014/papers/ICDVRAT2014_S01N3_Vallejo_etal.pdf.
96
VelezJ. A.HanusM. D. (2016). Self-affirmation Theory and Performance Feedback: When Scoring High Makes You Feel Low. Cyberpsychology, Behav. Soc. Networking19 (12), 721–726. 10.1089/cyber.2016.0144
97
VygotskyL. S. (1978). Mind in Society: Development of Higher Psychological Processes. Harvard University Press. 10.2307/j.ctvjf9vz4
98
WiederholdB. K. (2020). How Virtual Reality Is Changing the Reality of Aging. Cyberpsychology, Behav. Soc. Networking23 (3). 10.1089/cyber.2020.29176.bkw
99
WiederholdB. K. (2016). Lessons Learned as We Begin the Third Decade of Virtual Reality. Cyberpsychology, Behav. Soc. Networking19 (10), 577–578. 10.1089/cyber.2016.29052.bkw
100
WiederholdB. K.RivaF. (2012). Positive Technology Supports Shift to Preventive, Integrative Health. Cyberpsychology, Behav. Soc. Networking15 (2), 67–68. 10.1089/cyber.2011.1533
101
WilliamsB.DohertyN. L.BenderA.MattoxH.TibbsJ. R. (2011). The Effect of Nintendo Wii on Balance: A Pilot Study Supporting the Use of the Wii in Occupational Therapy for the Well Elderly. Occup. Ther. Health Care, 25 (2-3), 131–139. 10.3109/07380577.2011.560627
102
YehT. M.PaiF. Y.JengM. Y. (2019). The Factors Affecting Older Adults’ Intention toward Ongoing Participation in Virtual Reality Leisure Activities. Int. J. Environ. Res. Public Health16 (3), 333. 10.3390/ijerph16030333
103
Yu-LeungN.FloraM.FrederickH.PatrickI.King-WaF. (2019). Effectiveness of Virtual and Augmented Reality-Enhanced Exercise on Physical Activity, Psychological Outcomes, and Physical Performance: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Comput. Hum. Behav., 99, 278–291. 10.1016/j.chb.2019.05.026
104
ZajoncR. B. (1965). Social Facilitation. Science149, 269–274. https://www.jstor.org/stable/1715944
Summary
Keywords
virtual reality, augmented reality, older adults, physical/mental health, scoping review, psychology
Citation
Carroll J, Hopper L, Farrelly AM, Lombard-Vance R, Bamidis PD and Konstantinidis EI (2021) A Scoping Review of Augmented/Virtual Reality Health and Wellbeing Interventions for Older Adults: Redefining Immersive Virtual Reality. Front. Virtual Real. 2:655338. doi: 10.3389/frvir.2021.655338
Received
18 January 2021
Accepted
07 May 2021
Published
02 June 2021
Volume
2 - 2021
Edited by
John Naslund, Harvard Medical School, United States
Reviewed by
Vangelis Lympouridis, University of Southern California, United States
Savita G Bhakta, University of California, San Diego, United States
Updates
Copyright
© 2021 Carroll, Hopper, Farrelly, Lombard-Vance, Bamidis and Konstantinidis.
This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Joanne Carroll, joanne.carroll@dcu.ie
This article was submitted to Virtual Reality in Medicine, a section of the journal Frontiers in Virtual Reality
Disclaimer
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.