- 1Gerontology Program, Department of Human Development and Family Studies, Iowa State University, Ames, IA, United States
- 2Virtual Reality Applications Center, Human Computer Interaction, Iowa State University, Ames, IA, United States
- 3Gerontology Program, Human Computer Interaction, Virtual Reality Applications Center, Department of Industrial and Manufacturing Systems Engineering, Iowa State University, Ames, IA, United States
- 4Gerontology Program, Department of Psychology, Iowa State University, Ames, IA, United States
- 5Department of Psychology, Institute for Successful Longevity, Florida State University, Tallahassee, FL, United States
Research has pointed to the potential of extended reality (XR), including virtual, mixed, and augmented reality, for broadly impactful benefits, including learning, physical activity and health, and psychosocial aspects such as increased empathy and reduced loneliness. More research is needed to evaluate the outcomes of XR in new populations of users, including older adults. The purpose of this systematic review is to summarize the extant literature that centers on older adult use of XR in order to identify key themes, as well as identified benefits and barriers to XR use. In total, 17 studies from 2015 to 2019 met the inclusion criteria, namely that the study collected data from a sample of adults at least 60 years of age interacting with a 3D virtual environment. Through qualitative analysis of the corpus, six thematic areas were identified: Socialization, Physical Rehabilitation, Driving Simulation, Cognitive Training, Reminiscence, and Assessment. Furthermore, the unique contexts and outcomes of XR use, preferences for XR use, and reported occurrences of cybersickness in older adults are highlighted. Research after 2019 is also noted. This review is intended to guide future research supporting deployment of XR with older adults, emphasizing the psychosocial impacts of the technology.
Systematic Review Registration: (website), identifier (registration number)
Introduction
Virtual reality (VR) may appear to be a new phenomenon, with a surge of interest in the wake of the Kickstarter-funded release of two modern head-mounted displays (HMDs) Oculus DK1 and DK2 (Development Kit 1 and 2; McGill, 2016). However, academic attention to VR in the 1990s led to many of the theories that shape our understanding of the technology, including Milgram and Kishino’s virtuality-reality continuum (Milgram and Kishino, 1994). According to this continuum, VR is a manifestation of virtuality in which system users can view and interact with digital objects within a virtual environment (VE). Augmented virtuality (AV) occurs when real objects are represented in a virtual world. Augmented Reality (AR) falls closer to the reality end of the continuum, and consists of viewing virtual objects overlaid on a view of the real environment using pass-through devices (such as through a camera or specialized lenses; e.g., when someone on a video call turns on a “filter” and appears to have animated bunny ears added to their head). Mixed reality (MR) falls in the middle range of the continuum, allowing people to interact with both real and virtual objects together (e.g., exploring a virtual environment but using your actual smart phone while in it). In recent years, the many possible ways through which one can interact virtual systems has been summed up as extended reality (XR).
Prior to 2016, when Oculus released their first consumer VR device (Oculus Rift CV1), HMDs were expensive, saw attention in limited professional and academic settings, and had several performance and usability concerns (Hutchison, 2007). Because of the focus on developing usable and powerful devices, little research focused on users who do not fall within the innovation adopter categories of enthusiast or early adopters (Rogers, 2003).
Prior work highlights the potential of XR for diverse outcomes including increasing empathy (Bertrand et al., 2018; Barbot and Kaufman, 2020), training new skills (Johnson-Glenberg et al., 2014; Molka-Danielsen et al., 2018; Radianti et al., 2020), reducing loneliness (Gunkel et al., 2018; Smith and Neff, 2018), and improving mental health (Geraets et al., 2020), which are all of benefit to broad swaths of users. While research has begun to turn toward underserved populations, including older adults (Montana et al., 2020), more work is needed. Now that research surrounding XR is opening to include attention to the challenges of the “everyday user” (such as Gugenheimer et al., 2019, 2017), there is a need to uncover the gaps deserving of attention.
Reviews seeking to enumerate and close these gaps have focused on general use of VR in sports (Neumann et al., 2018), XR games for physical functioning among older adults (Miller et al., 2014; Molina et al., 2014). Beyond the physical uses of VR, recent reviews have focused on XR use in the support of persons with dementia (Hayhurst, 2018) and community-dwelling older adults (Dermody et al., 2020). Still other work has focused on the need for user-centered design including a framework of design recommendations for HMD-based VR exergames (Li et al., 2020) and the outcomes of a workshop on designing and using VR in sensitive settings (Waycott et al., 2018). The purpose of this systematic review is to guide future research on the use of XR by older adults, themselves, and in contexts beyond physical functioning.
Background
For older adults, there exist concerns outside of the usability and transferability of previous findings in younger samples of XR users which intersect with the study of the prosocial benefits of the technology. In the United States of America, and indeed worldwide, falling birthrates combined with innovations in medical practices and technology are leading to the expansion of the older adult population (Ageing and health, 2018). While longer life is to be welcomed, it brings with it its own list of challenges, including planning for the costs of healthcare and combating isolation. One possible way to solve such problems is to leverage technology such as XR.
However, the focus of technology-centric research must expand to be able to offer broader offerings and accessibility to diverse users. Much of the development and design of innovative technology is conducted by younger adults, and it is common that developers and designers focus on creating technology that caters to people who are like them. This has been reflected in the lack of focus on accessibility in game consoles (until the Xbox Adaptive controller; Kujawski and Johnson, 2018) and XR HMDs (until the WalkinVR Driver; WalkinVR, 2020) and a reduced initial focus on narrow application areas. This naïveté coupled with the relative newness of XR has meant a focus on getting the technology to work for the “average” consumer of these new technology, as well as on making them more financially accessible (Lawton, 2006). While technical functionality is important to get right, this has meant the user experience and inclusive design needs have largely been neglected in HMDs.
Still, these technologies are being used by older adults who find useful applications for XR (for example, VR HMDs Baker et al., 2019; Roberts et al., 2019). Therefore, it is important that researchers work to enhance adoption of XR technology among older adult populations. This paper describes a systematic literature review that seeks to highlight extant research as well as areas that are lacking to in order to guide the continued advancement of scientific discovery in this area. Specifically, this review explores the current ways XR technologies are used with older adults, as well as how interaction is different as individuals age, summarizing the extant literature that centers on older adult use of XR in order to identify key themes, including benefits and barriers to XR use.
Definitions and Perspectives
This review focuses on the use of XR technology by older adults; specifically of interest are the ways in which interaction is different as we age and how interaction with XR technology can impact psychosocial health and quality of life. However, these concepts deserve better clarity. As such, we delineate below what we mean by older adults, XR Technology – including a brief review of the history of XR and the interaction challenges inherent in the technology, and psychosocial health and quality of life.
Defining Older Age
Aging adults are more diverse in abilities than their younger counterparts, so choosing any specific chronological age cutoff to define “older adult” is difficult. Aging studies often select those aged 65 years and older as a minimum; however, this leaves a large age range encompassing multiple decades and persons with extremely heterogeneous functional abilities and experiences. In the U.S., age eligibility criteria are often used to determine who is legally “old.” For instance, the Age Discrimination in Employment Act defines the protected class, older workers, as persons at or over 40 years of age. For U.S. social security benefits, ages 62, 67, and 70 entitle eligible people to partial, full, and enhanced retirement benefits. As a result of such variability in legal and functional status, aging adults are often categorized into chronological age bands, such as the young-old (65–74 years), middle-old (75–84 years) and old-old (85 + yrs.; see Czaja et al., 2019). However, for this review a cutoff age for study inclusion was needed. Maximal human longevity is approximately 120 years (the record being 122 years for Jeanne Calment; Robine et al., (2019), so choosing the half-way point, age 60, was a reasonable cutoff that was also backed by the World Health Organization (2018).
From the perspective of usability of XR technology, functional capacity for vision, hearing, and balance are probably the most critical factors for aging adults. Loss of ability to focus the lens of the eye, a normative vision change that occurs in the mid-40s, leaves most adults needing corrective lenses for focusing on near objects, such as the screen area in an XR headset. Hence, aging users need to be able to fit their glasses-wearing heads into a VR headset comfortably or be able to fit a glasses-like AR device (e.g., Google Glass) over their own glasses. Hearing acuity declines normatively from early childhood onward, particularly for low-volume, high frequency (high pitch) sounds. By the old-old years, many adults (most males) may be wearing hearing aids in one or both ears, meaning that XR sound sources should be compatible with hearing aids (e.g., built into the headset rather than piped in through earbuds).
Finally, balance declines with age in terms of less effective vestibular (inner ear) function and slowing in information processing rate that results in slower reflexive responses to maintain a safe posture. Older adults appear to compensate for vestibular changes by weighting visual input more heavily to maintain balance. Hence few can successfully stand on one foot for more than a second with eyes closed compared to eyes open. As a result, they may be at higher risk than younger adults for cybersickness and risk of falling when walking around with an XR headset that does not permit adequate view of the surrounding environment. This issue suggests that they might perform better with AR headsets, with their transparent displays, rather than VR headsets that occlude vision of one’s surroundings if required to stand and move around.
Defining XR Technology for This Systematic Review
In this review, we define XR as the continuum of technologies that allow immersive interaction or exploration of virtual, augmented, or mixed reality environments. In this way, “XR interfaces” for the purposes of this review include: CAVEs (rooms in which the walls are screens, possibly along with the floor and ceiling), HMDs, and three-dimensional (3D) displays (e.g., TVs with 3D glasses). When discussing specific kinds of XR, the more specific terms (AR, VR, or MR) will be used, while the more general “XR” will be used in all other cases.
One usability concern has been the phenomena known as cybersickness, simulator sickness, or visually-induced motion sickness (VIMS). This is a feeling of nausea or dizziness that can occur when experiencing XR. For our purposes, we refer to each of these as cybersickness, but all three terms were used in the review. This is a vast simplification of this area of research (e.g., Davis et al., 2014; Stanney et al., 2020; Stone III, 2017), but when considering the impact of the range of symptoms on immersive XR users, there is little difference. Cybersickness is typically measured by the Simulator Sickness Questionnaire (SSQ; Stone, 2017).
Defining Psychosocial Well-Being
An aim of this study is to articulate the extent to which prior studies demonstrate the ability of XR to enhance the experience of everyday life among aging adults. Of relevance are several important indicators of functioning and well-being. Psychosocial well-being encompasses cognitive, emotional, and social components of everyday life. This construct is closely aligned and supports whole-person wellness which incorporates intellectual, physical, spiritual, emotional, occupational, and social components (Kang and Russ, 2009; Montague et al., 2002). Quality of life refers to individuals’ subjective well-being overall as well as the ability to participate in typical and desired daily activities, including physical, mental, and social roles. For older adults, this may include a preference to live independently for longer in a setting of their choosing (e.g., “aging in place”). Determination of quality of life can vary across individuals, thus it is typically assessed via self-report (e.g., Diener et al., 1985, 2009). Together, whole-person wellness and quality of life underpin individuals’ ability to “successfully” or “optimally” age (e.g., Martin et al., 2018).
Given that quality of life is evaluated with a whole-person lens including physical and psychosocial health aspects, we focused on studies with these emphases.
Methods
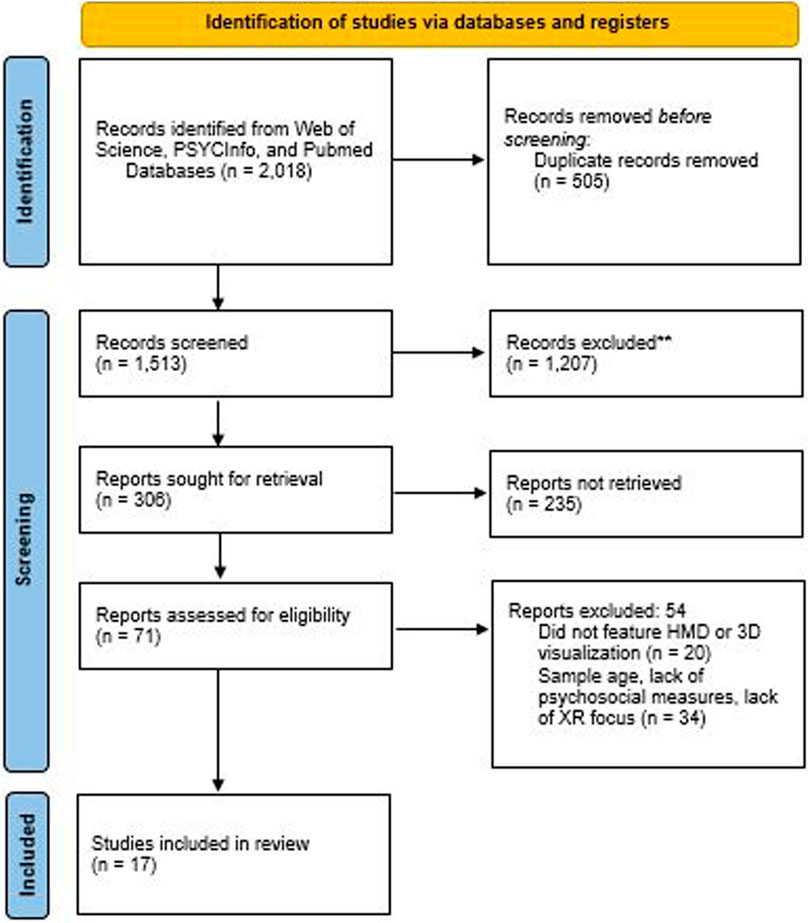
Following the recommendations of PRISMA (Moher et al., 2009) and Cochrane (Higgins et al., 2019), the methods were set out prior to the initiation of the study. Keywords, inclusion criteria, exclusion criteria, and databases were identified and agreed upon by an interdisciplinary team of researchers prior to the start of the review. Web of Science, PSYCInfo, and Pubmed were searched on September 30, 2019. Searches were limited to articles on older adult humans published in the English language. The databases were searched using terms representing: age; psychosocial health; and XR (see Supplementary Appendix SA for a full list). Using these keywords, 2,018 citations were pulled from the databases and filtered to 1,513 citations after duplicate removal (see Figure 1).
Next, titles and abstracts were examined according to inclusion and exclusion criteria. We included published data that fulfilled the following inclusion criteria: 1) data were collected for samples with a minimum age of 60 years or older; 2) the psychosocial data were collected at the level of the individual; 3) data about the use of the XR were collected, rather than simply using the technology as a delivery mechanism; and 4) papers were published after 2013 because, for HMDs, the release of the Oculus Rift Development Kit 2 provided vast improvements of frames-per-second, weight, and resolution over previous HMDs.
Excluded were published data that: 1) took the form of an abstract-only conference proceedings, magazine article, or other non-peer-reviewed source (e.g., commentary, editorial report); or 2) were presented as a review or meta-analysis. Given that this research area is developing, theses and dissertations were included to reduce the publication bias that may have otherwise been present. All qualitative and quantitative studies meeting these criteria were included.
Next, abstracts and titles were reviewed by a team to determine whether papers fit the criteria defined above, resulting in 306 citations. The papers were downloaded and a second manual screening, which used the search feature of Mendeley to identify studies that did not meet inclusion criteria, reduced the corpus to 71 papers which used a virtual environment and included psychosocial or physical health measures. Given the intent to examine the use of 3D virtual environments, papers were not included if they did not feature an HMD or 3D visualizations (e.g., a 3D television was appropriate, but a projected image with no active or passive stereo lenses was not). Thus, the 71 papers were further reduced to 51. Through a thorough reading of each paper, 35 were determined to not meet inclusion criteria and were omitted from further review, while an additional paper 1) was added through citation chaining, bringing the final corpus, which is listed in Supplementary Appendix SB, to 17 papers.
Overview of the Corpus and Focus Areas
The final corpus consisted of 17 papers that were published from 2015 to 2019. These publications included 19 studies which resulted from a dissertation including three studies (i.e., Almajid, 2019). Therefore, studies form the unit of analysis.
As a result of the range of outcomes evaluated and the relatively small number of studies, a meta-analysis was deemed unsuitable at this time. Instead, we describe the themes and commonalities and use these insights to offer suggestions for future research. First, the six identified focus areas of these studies are delineated. In addition, we identified eight technology types: four areas that had been studied in the XR literature at large and four that emerged during the literature review. The counts of occurrences of specific technologies in the corpus are also delineated below.
Focus Areas
One of the questions we sought to answer was centered on the currently documented uses for VR by older adults in the literature. Of the sampled studies, six focus areas were identified: physical rehabilitation; cognitive training; reminiscence; assessment; driving simulation; and socialization (see Figure 2). The distribution of these focus areas over the years of this review (note: no relevant articles were identified for 2014) includes physical rehabilitation consistently over the years, with attention to driving simulation and socialization occurring more recently, and a revived focus on reminiscence in the most recent year of the review.
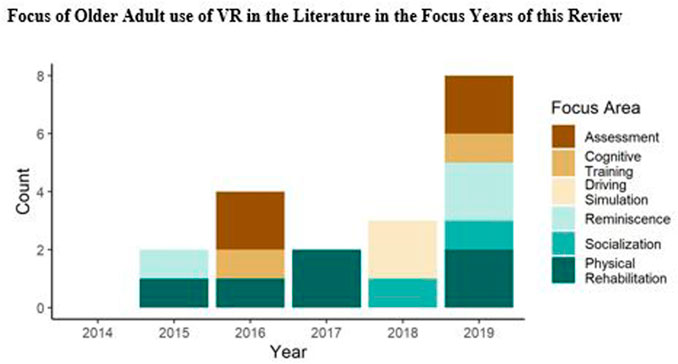
FIGURE 2. Distribution of the identified focus areas over the years included in the systematic review.
Physical Rehabilitation
Physical rehabilitation is the focus area of the most studies in the corpus. In total, six of the studies (Lee et al., 2015; Bruun-Pedersen et al., 2016; Kim et al., 2017; Lee et al., 2017; Almajid, 2019; Howes et al., 2019) focused on the use of VR for training balance and guided exercise or on evaluating the safety of VR for use in older adult populations.
Cognitive Training
Cognitive health is a chief concern associated with aging, and as such, researchers are interested in studying the use of technologies such as VR for the maintenance of cognitive abilities or remediation of any decline through targeted training (Manera et al., 2016; Micarelli et al., 2019). One of the studies in the corpus focused on using VR to conduct attentional training (Manera et al., 2016), while the other was interested in the use of low-cost phone-based HMDs in training spatial memory and orientation (Micarelli et al., 2019).
Reminiscence
The ability for VR to transport embodied individuals into the environments has been identified in research (Kraus and Kibsgaard, 2015), and for older adults, this presents an opportunity to revisit places physically and mentally in addition to the chance to experience novel locations. Three studies in the corpus examined the use of VR for travel, either to physical locations or location-specific memories. One study (Benoit et al., 2015) explored whether VR is safe and desired by older adults, as well as whether it is effective at evoking autobiographical memories, by comparing participant performance in producing memories for familiar places presented in VR and as photographs compared to non-familiar places and familiar non-places (a single-color screen). A second study conducted by Brown and others (2019) explored the usability of a VR HMD and the video preferences and perceived use-cases for the technologies. The third study in this focus area (Niki et al., 2019) explored the impacts of location-based VR experiences in palliative care.
Assessment
VR, due to its use of simulated environments, offers a potentially invaluable alternative to paper-based assessments of memory and physical ability, as well as a new way to test specific aspects of the aging experience while controlling for variables that are not easily managed in other replications of real-world experience. While many of the papers in this corpus used VR to evaluate the abilities of their participants (for example, Ramkhalawansingh et al., 2018, evaluated the integration of stimuli important to distinguishing heading), four studies directly evaluated the use of VR in conducting assessments related to memory (Craig et al., 2016), balance (Chang et al., 2016), and the effect of visual perturbations on a popular measure of range of motion (Almajid, 2019, studies 2 and 3).
Driving Simulation
Another focus area was the use of VR driving simulations. One study examined the ability of older adults, compared to young adults, to distinguish heading from visual, vestibular, or integrated cues (Ramkhalawansingh et al., 2018). The other study in this focus area was conducted by Bier et al. (2018) that sought to train attention using VR was interested in the transferability of skills to driving tasks.
Socialization
A recent direction for research regarding the use of VR by older adults has focused on socialization and social health. Specifically, this review identified two studies which investigated the effect of VR on isolation (Lin et al., 2018) and the needs of older adults from social VR applications (Baker et al., 2019). Specifically, Lin et al. found that older adults who used VR HMDs perceived themselves as possessing better physical and social health and experienced lower negative affect. Baker et al. (2019) revealed through participatory action research that older adults believe social VR has potential to improve social wellbeing, while also cautioning against using it as a one-size-fits-all intervention.
Technology Types
Of interest to this review were the types of XR technology used in each of the reported studies. The researchers identified four potential technologies that were expected within the corpus: VR HMDs with three degrees-of-freedom (3DoF), which allow tracking where a user is looking; VR HMDs with six degrees-of-freedom (6DoF), which allow tracking where a user is moving around a room); projector-based VR; and AR systems. Within the corpus, 11 studies utilized 6DoF VR HMDs, three used 3DoF VR HMDs, four used projector-based VR, and none used AR systems. It should be noted that three studies did use a pass-through camera with their VR HMD intervention, which technically qualifies as a use of AR; however, the focus of the study was on the use of VR, rather than AR. Still, these three studies are represented as examples of AR in tables and figures in the present article.
In addition to these expected forms of XR technology, two studies used 3DTVs, and one-each used Wii and Xbox Kinect systems to deliver their interventions through said 3DTVs. Three studies also used TV screens as comparison technologies. The studies and their respective technology distributions are highlighted in Table 1. In the table, Almajid (2019) uses the same technology throughout studies 1–3 (shortened to S1-3), while each of two phases in Baker et al. (2019) use different technology (6DoF HMDs and projector-based VR).
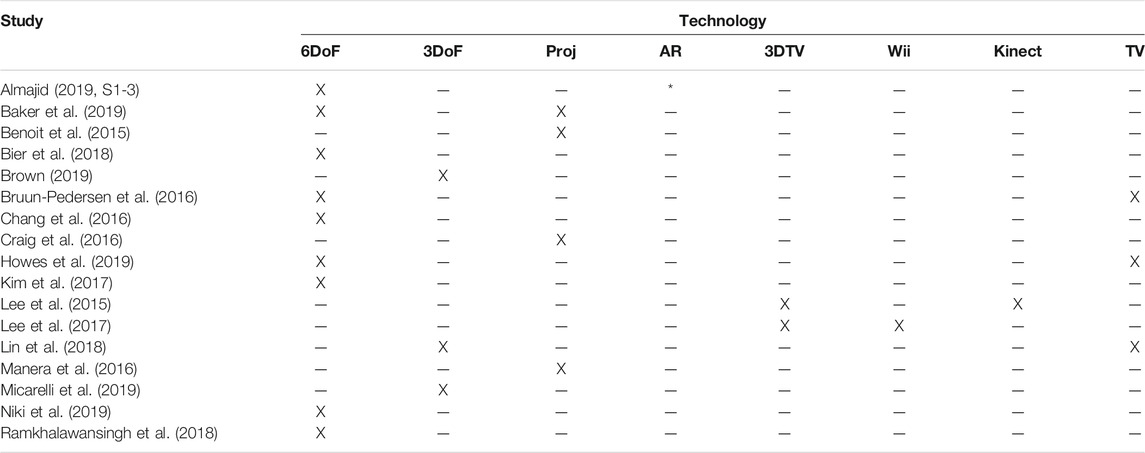
TABLE 1. The technologies used in the corpus. * is used to indicate the coupling of AR technology with a VR HMD.
Results
XR and Older Adults: Contexts, Outcomes, Preferences, and Cybersickness
Contexts and Outcomes of Use
Most of the current research on the use of XR by older adults has been lab-based. All 2) of the studies which centered on Driving Simulation, all 4) of the studies of use in Assessment, one of the Socialization studies, two of the Reminiscence studies, and two of the Physical Rehabilitation studies took place in a lab. In other words, each focus area saw attention in laboratory-based research studies. Less common were field-based studies. Six studies were conducted in care facilities or older adult communities. Two studies (one each from physical rehabilitation and socialization focus areas) were conducted in home environments.
For the most part, lab-based studies were more focused on using VR to present stimuli for other purposes, rather than testing the use of VR, itself. For example, VR is used to test the spatial memory of older and younger adults after either wakeful rest or a distractor task by Craig et al. (2016), to test balance in response to unexpected starts and stops by Chang et al. (2016), and as a means to provide visual cues that either matched or were dissonant with physical movement in a study by Ramkhalawansingh et al. (2018). Other studies used VR in laboratory research to evaluate the safety of immersive VR (Almajid, 2019, S1; Benoit et al., 2015; Kim et al., 2017). Only two lab studies (Baker et al., 2019; Brown, 2019) examined older adults’ opinions of VR, while all but one of the studies which took place in communities or involved at-home use of VR frequently evaluated opinions of VR and its use. The remaining study did not directly evaluate opinions, but Howes et al. (2019) did report the percentage of participants who completed the exercise regimen in each condition, which is indicative of their motivation to continue the program using that particular technology.
Additionally, Bruun-Pedersen et al. (2016) found higher exercise motivation associated with the use of an HMD. Other impacts of use included effective outcomes of exercise. Two studies evaluated the safety of VR use in older adult populations in anticipation of using HMD systems with patients with Parkinson’s disease (Kim et al., 2017) and in physical rehabilitation settings (Almajid, 2019). Exercise training using VR technology was shown to be effective (Lee et al., 2016; Lee et al., 2017) and to be associated with improvements in gait speed and stress (Kim et al., 2017).
Preferences for Use
If older adults are to use XR, the technology should be designed to reflect their unique spectrum of needs (Baker et al., 2019). The literature was mixed with regards to older adult preferences for HMD VR compared to other intervention delivery methods (e.g., televisions and group exercise), which suggests that the commonly applied stereotype – that older adults are unwilling or hesitant to use new technology – is inappropriate. In total, eight studies reported results that provide insight into the range of opinions on XR technology.
One study reported results that suggested participants preferred the other intervention technology over XR, while four studies reported positive preference for the XR technology, and two reported a mix of qualitative opinions from participants. Four of these studies fell in the focus area of Physical Rehabilitation. One found that older adults preferred using a TV screen compared to a VR HMD for guided exercise (Howes et al., 2019), while the remaining three found that older adults preferred using VR to Group exercise (Lee et al., 2016), falls-prevention training (Lee et al., 2017), and TV-based guided exercise (Bruun-Pedersen et al., 2016).
One study each from the focus areas of Cognitive Training and Socialization supported a preference for XR interventions. The Cognitive Training study (Manera et al., 2016) reported that more participants continued playing on the projector-based VR set up rather than with the paper-based condition. The Socialization study (Lin et al., 2018) found that their participants were more likely to recommend VR to others and use it themselves after experiencing the HMD-based intervention, and that these differences were bigger than for the TV control group.
It should be noted that the only study suggesting participants did not enjoy the XR intervention (Howes et al., 2019) admits that their system scored lower than acceptable on the usability scale, which may have impacted the preferences of their participants. While they did not have any adverse events, participants reported concerns such as disorientation and discomfort due to the (or their) lack of awareness of the external physical environment while wearing an HMD. One other study (Bruun-Pedersen et al., 2016) reported that just over half of their participants preferred the HMD to the TV, but the researchers suggested that the HMD was not yet ideal because of usability and accessibility concerns.
Two studies reported a mix of opinions in their sample (Baker et al., 2019; Brown, 2019). Among these are positive opinions and interest in the use of social VR for simultaneously combating isolation and overcoming self-consciousness with one’s own appearance. On the critical side of the spectrum, participants in both studies raised concerns with the ways in which people who are emotionally or mentally vulnerable (such as those with Alzheimer’s disease or dementia) may be affected by the VEs. In one study (Baker et al., 2019), some participants negatively responded to tracking inaccuracies, feeling as though they were the cause of erratic avatar movements or shakiness.
Cybersickness and Study Attrition
While irregularities of the virtual environment were reported by Baker et al. (2019) to intensify negative and/or stigmatizing thoughts, visual perturbations have the additional potential to cause cybersickness. In this review, we were interested in the proportion of studies that have reported cybersickness in their participants. The full distribution of reports by focus area is shown in Figure 3, and specific details are sampled in the text.
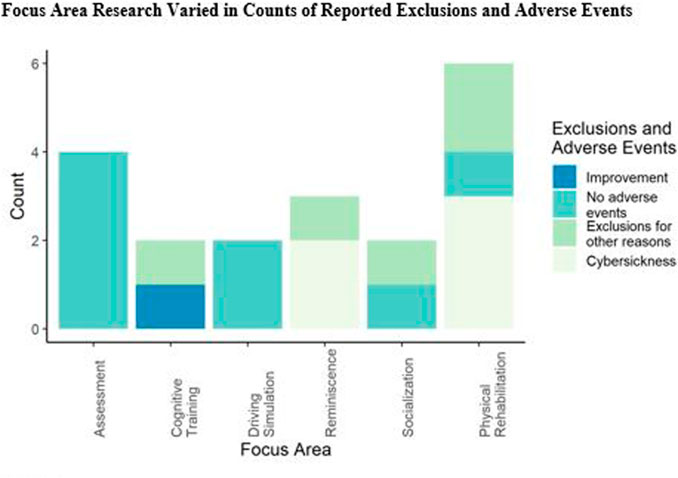
FIGURE 3. Studies in the corpus reported a mix of results on cybersickness and adverse events. Counts by focus area are given here. Improvement category indicates a reduction of Simulator Sickness Questionnaire scores.
Of note, just under half of the studies did not report any cybersickness in their sample, and one study reported a reduction in scores on the SSQ (Stone, 2017). Cybersickness, specifically, was only reported in three studies which either reported scores on the SSQ that were indicative of cybersickness or participant complaints of symptoms.
The remaining five studies reported attrition or exclusions for other reasons or for reasons that were not reported. Specifically, Baker et al. (2019) reported one withdrawal from the study prior to the HMD study, which may have been a sign of apprehension for using the immersive technology; however, a reason for the participant’s dropping out is not formally given. None of their participants who used the HMD reported symptoms of cybersickness, but they did have usability and weight complaints. Benoit et al. (2015) excluded five participants from the data analysis because they did not meet inclusion criteria, but no participants withdrew from the study or reported cybersickness symptoms. Bruun-Pedersen et al. (2016) reported one withdrawal after an accidental issue with the study materials, wherein a misplaced sensor produced rapid and incongruent acceleration of the environment while the participant was wearing the HMD but was not yet interacting with the scene. In the remaining two studies (Lee et al., 2015; Manera et al., 2016), participants either refused to continue in the study or no longer met the inclusion criteria (e.g., scores on a cognitive evaluation outside of the required range or taking actions that interfered with the control of the study).
Interestingly, cybersickness (or similar terminology for it) was only reported in the Physical Rehabilitation and Reminiscence studies, as shown in Figure 3, and none of the Assessment or Driving Simulation studies reported adverse events of any kind. One study which is classified in the Driving Simulation focus area noted that their lack of cybersickness findings may have been due to the brief duration of the VE exposure. Lastly, Micarelli et al. (2019) found that over the course of 1 month of 3DoF VR HMD use, SSQ (Stone, 2017) scores were reduced.
Another potential explanation, at macro scale, is the technology being used in each study. A further examination of the five studies which reported cybersickness reveals this may be the case, as 80% of the studies used immersive VR headsets (three 6DoF and one 3DoF). However, as is shown in Figure 4, not every study which used 3DoF 6DoF HMDs reported cybersickness. In fact, more studies reported no adverse events whatsoever. Because technology use categories are not exclusive, there is a double report of single studies within the 6DoF, Projector, and AR categories. The 6DoF total count includes three duplicates overlapping with AR (these all have no reported adverse events) and one duplicate overlapping with Projector (reporting exclusions for other reasons).
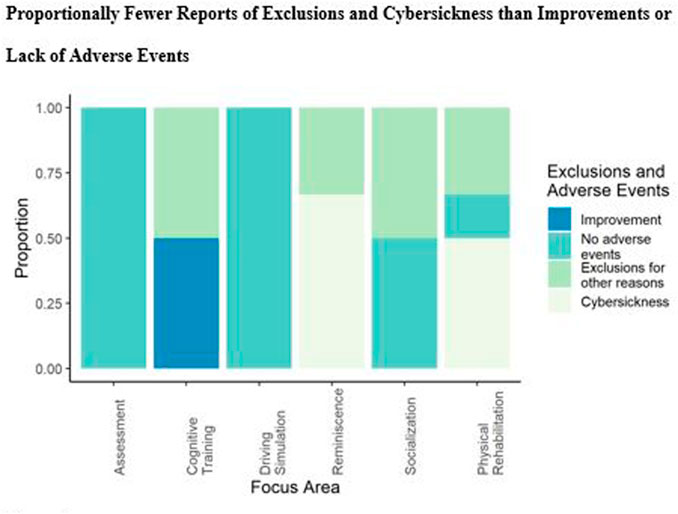
FIGURE 4. Proportion of reported exclusions and adverse events (such as cybersickness) within the studies in the corpus by identified focus area.
Methodological Reflections
Not every study in the corpus used the SSQ, a standard measure for cybersickness (Stone, 2017), to evaluate their participant’s experience with the VE. Additionally, not every study reported why they excluded participants or followed up to understand what prompted attrition, and a range of qualitative and quantitative data were collected. To better guide future research, it is worthwhile to reflect on the methods of the studies in this corpus. The full list of quantitative metrics used, as well as a rough categorization of these metrics, is provided in Supplementary Appendices SC, SD.
As mentioned above, the researchers were particularly interested in the number of reported adverse events, including cybersickness. Surprisingly, only two of the studies in the corpus used the SSQ (in full or shortened) to assess the level of cybersickness in their participants. One study used an 11-point Numerical Rating Scale (NRS) to assess dizziness and headache after VR exposure, and another used a 22-item cybersickness questionnaire which had been used in previous research but had not been validated. Four additional studies that did not measure it, objectively, reported participant subjective complaints of discomfort related to the weight of the HMD or dizziness during the activity, itself.
Another interest of the present review aligned with participants’ opinions of XR and the impact of XR on psychosocial health. In terms of the psychosocial health impacts, the majority 11) of the studies in the corpus included some measure that related to this dimension of experience. In terms of participant opinions of the XR technology, researchers used Likert-response questions asking about likelihood for use in the future and to recommend to another person as well as participant satisfaction with the system. Others asked participants which of the two interventions they more enjoyed or they would prefer to use for future exercise activity. Relatively few (three) used validated measures – specifically the System Usability Scale (SUS), and the Slater-Usoh-Steed Presence scale.
In terms of methodological paradigms, most studies 14) collected quantitative data. These included physical measures (such as task performance, physiological measures, and Kinesthetic performance), psychometric measures (such as the Apathy Inventory, GDS, and cognitive recall/recognition performance), and psychosocial measures (including both validated batteries, e.g., the PANAS and the Immersive Tendencies Questionnaire, and researcher-generated response scales). Five studies collected qualitative responses, including three that also collected quantitative data. Qualitative data included unstructured designs, such as opportunities to offer feedback or recorded off-hand comments, as well as more-rigorous qualitative studies – one using participatory action through guided workshops, one using semi-structured interviews and focus groups centered on an intervention, and one using semi-structured exit interviews to capture participant opinions of the interventions.
Studies in the corpus were largely interested in answering questions about safety and efficacy of XR experiences either for the older adult population in general, or as a tool for delivering an intervention (such as cognitive or physical training) to the older adult user of the technology. Other research questions related to the validity of driving simulator-based tests and to the perceptual and cognitive differences associated with aging. Only three (Lee et al., 2015; Baker et al., 2019; Brown, 2019; Howes et al., 2019) studies directly addressed the question of what older adults need from XR experiences, and only three addressed the impact of quality of life (Lin et al., 2018; Micarelli et al., 2019; Niki et al., 2019) in response to XR interventions.
Research Since 2019
While this systematic analysis was conducted in 2019 and yielded useful insights regarding older adults and XR in the form of the six focus areas, XR research using older adults has continued (e.g., Syed-Abdul et al., 2019; Appel et al., 2020; Mostajeran et al., 2020). A survey of these articles suggests that the six focus areas described in this article still encompass this newer research, though more systematic investigation is warranted.
More notable are several newer systematic review articles that focus on this topic. Systematic reviews as a form of academic publication are increasing in frequency (Hoffmann et al., 2021), and thus these publications are to be expected. At least seven systematic reviews of XR’s role in improving mental health and physical rehabilitation for older adults were published: Campo-Prieto et al., 2021 with 11 studies; Corregidor-Sánchez et al., 2021 with 16 studies; Dermody et al., 2020 with 7 studies; Montana et al., 2020 with 11 studies; Nishchyk et al., 2021 with 12 studies; Skurla et al., 2021 with 55 studies; Zhu et al., 2021 with 11 studies. These reviews reinforce the two focus areas of physical rehabilitation and cognitive training. An additional systematic review with 15 studies focused on older adult and VR used for life enrichment (Thach et al., 2020). This review reinforces the two focus areas of reminiscence and socialization.
Discussion
This paper presents research from the beginning of an important area of inquiry, with the hope that the insights will be useful to researchers and developers advancing XR technology. We have identified six focus areas of XR research in the extant literature: Assessment, Cognitive Training, Reminiscence, Driving Simulation, Physical Rehabilitation, and Socialization. Since we were interested in the use of XR by older adults specifically, information about use of XR by their caregivers was excluded from this analysis, although research does include this area – especially for training and informal caregiver support (Hayhurst, 2018).
One limitation of this study is the age-range defined in the inclusionary criteria. Many otherwise-relevant studies were excluded from our analysis because the youngest participants were in their 50s (Roberts et al., 2019), while we required at least one sample (to allow for age-comparison studies) to be aged 60 or older. A multi-disciplinary approach including researchers from gerontology is needed to define a clear range of age and abilities for studies with samples of “older adults” to allow better generalization within this population.
However, it is worth repeating that the group, “older adults,” should not be reduced to a single voice. As noted by participants in one study, older adults cannot speak to others’ experiences. This is a common mistake to be made, as members of minority groups and sensitive populations are often asked to play the role of “spokesperson” for the entire community as “token individuals.” To better avoid excluding voices or reducing their variability, we suggest a few converging paths: First, better measurement tools are needed to understand what components of individuals in the older adult population group are interesting to research; similar to the Big Five for understanding general trends in personality, a tool is needed to allow more fine-grained assessment of the aging process from a psychosocial and biological perspective. This is seemingly echoed in the finding that proficiency with navigating the VR platform in Brown (2019)’s study was reflective of individual experience with digital technology, rather than age. Second, more qualitative studies of adequate rigor are needed on the subject. Using these two approaches could lead to increased diversity in XR study sample populations both in 1) age and ability and 2) technology experience and proficiency.
Some of the studies presented methodological limitations, such as small quantitative or psychometric samples. One in particular noted that one of the two centers at which they conducted the study was not staffed by technologically-savvy individuals, stating that one center being evaluated had a Nintendo WiiTM that had never been used because the staff “didn’t understand it” (Howes et al., 2019). The same study split their sample in two, with five participants using only a TV screen to complete guided exercise and the other four using both a TV screen and a 3DoF HMD. It is not clear if use of the HMD and TV was counterbalanced to account for order effects, nor is the split of participants in each condition between the two centers addressed in the paper.
Since the studies in the corpus do not center on specific outcomes, we have taken care to understand what has been studied and identify avenues for further research. Specifically, more work is needed to understand the specific usability and accessibility needs of the technology. A handful of studies commented on the need for better external awareness and reduced HMD weight, but relatively few user evaluative studies have been performed with this population of users. In need of evaluation are both the hardware considerations, such as the form factor of controllers and robust tracking, and software considerations like movement-smoothing and selection-interaction parameters.
Another concern raised by older adult participants was that of safety, both physical and emotional. Participants of these studies were hesitant to recommend the use of HMDs and immersive XR to those who may be emotionally or cognitively vulnerable, such as persons with dementia. Additionally, the usability concern for external awareness highlights the need for better support of safe use of XR HMDs. As noted by Yang et al. (2018), the physical play space may be used by other people or include movable objects that will pose safety challenges to the unaware HMD user.
One concern that was not directly raised in the samples of the reviewed studies is that of privacy. Whenever a person interacts with the Internet, they are exchanging data such as browsing and location history. In VR, and especially Social VR (Blackwell et al., 2019), privacy should be a concern – both understanding the transparency requirements of users and designing these systems and experiences with privacy in mind.
Overall, XR seems to have strong potential value as a technology for older adults. It has demonstrated efficacy in many areas including those explicitly tested with older adult users (Lee et al., 2017; Niki et al., 2019). In addition, older adults, themselves have largely preferred using VR over other methods, as discussed above. Lastly, there is no current indication that age alone affects cybersickness propensity, as only seven of the 17 studies in this corpus reported any indications of cybersickness.
Still, work is needed to verify these claims. In addition to creating more usable and accessible XR, attention to the prevalence of cybersickness is needed, and validated measures should be used to assess this. Relatively little work has focused on the psychosocial impacts of XR. While longitudinal studies have commented on the impacts on social health and quality of life, there have not been, to the authors’ knowledge, any that have addressed the topic of prolonged use of XR on psychosocial outcomes.
This review has presented information on the extant literature that centers on the use of XR by older adults. In total, 19 studies in a 5-years period met inclusion criteria and focused on six areas: Socialization; Physical Rehabilitation; Driving Simulation; Cognitive Training; Reminiscence; and Assessment. The contexts and outcomes of use, preferences for use, and reported occurrences of cybersickness, dropouts, and data exclusions are delineated, and conclusions are drawn from the data. We hope that this review will guide future research to address areas that are important to deployment of XR among older adult populations, while also examining the psychosocial impacts of the technology.
Recommendations for Older Adults and XR
Based on the reviewed research, there are multiple beneficial opportunities for older adults to use XR for physical health such as rehabilitation, mental health and cognitive therapy, and overall life improvement. While reviews on specific technologies were mixed, it was clear that older adults were willing to engage with XR technologies if they found them both helpful and usable. Potential XR experiences can be optimized by choosing software based on third-party reviews and by using more recent XR hardware that will minimize cybersickness.
Data Availability Statement
The original contributions presented in the study are included in the article/Supplementary Material, further inquiries can be directed to the corresponding author.
Author Contributions
JM, KO, and LG contributed to conceptualization and implementation of the review, analysis, writing, and interpretation; they share first authorship. LP and NC contributed to the review conceptualization, interpretation, and writing.
Funding
Funding for this project was provided by Iowa State University Nanovaccine Institute (award # 2901738) and support for JM was provided by the National Institute of Food and Agriculture (project # IOW04116).
Conflict of Interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Publisher’s Note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors, and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
Supplementary Material
The Supplementary Material for this article can be found online at: https://www.frontiersin.org/articles/10.3389/frvir.2021.760064/full#supplementary-material
References
Almajid, R. (2019). “Aging-related Decrements during the Activities of the Timed up and Go Test when Combined with Motor Task and Visual Stimulation [Temple University],” in Dissertation Abstracts International: Section B: The Sciences and Engineering. Available From: https://search.proquest.com/docview/2140744279?accountid=10906.
Appel, L., Appel, E., Bogler, O., Wiseman, M., Cohen, L., Ein, N., et al. (2020). Older Adults with Cognitive And/or Physical Impairments Can Benefit from Immersive Virtual Reality Experiences: a Feasibility Study. Front. Med. 6, 329. doi:10.3389/fmed.2019.00329
Baker, S., Kelly, R. M., Waycott, J., Carrasco, R., Hoang, T., Batchelor, F., et al. (2019). Interrogating Social Virtual Reality as a Communication Medium for Older Adults. Proc. ACM Hum.-Comput. Interact. 3, 1–24. (CSCW). doi:10.1145/3359251
Barbot, B., and Kaufman, J. C. (2020). What Makes Immersive Virtual Reality the Ultimate Empathy Machine? Discerning the Underlying Mechanisms of Change. Comput. Hum. Behav. 111 (February), 106431. doi:10.1016/j.chb.2020.106431
Benoit, M., Guerchouche, R., Petit, P. D., Chapoulie, E., Manera, V., Chaurasia, G., et al. (2015). Is it Possible to Use Highly Realistic Virtual Reality in the Elderly? A Feasibility Study with Image-Based Rendering. Neuropsychiatr. Dis. Treat. 11, 557–563. doi:10.2147/NDT.S73179
Bertrand, P., Guegan, J., Robieux, L., McCall, C. A., and Zenasni, F. (2018). Learning Empathy through Virtual Reality: Multiple Strategies for Training Empathy-Related Abilities Using Body Ownership Illusions in Embodied Virtual Reality. Front. Robot. AI 5 (MAR), 1–18. doi:10.3389/frobt.2018.00026
Bier, B., Ouellet, É., and Belleville, S. (2018). Computerized Attentional Training and Transfer with Virtual Reality: Effect of Age and Training Type. Neuropsychology 32, 597–614. doi:10.1037/neu0000417
Blackwell, L., Ellison, N., Elliott-Deflo, N., and Schwartz, R. (2019). Harassment in Social Virtual Reality. Proc. ACM Hum.-Comput. Interact. 3 (CSCW), 1–25. doi:10.1145/3359202
Brown, J. A. (2019). An Exploration of Virtual Reality Use and Application Among Older Adult Populations. Gerontol. Geriatr. Med. 5, 233372141988528. doi:10.1177/2333721419885287
Bruun-Pedersen, J. R., Serafin, S., and Kofoed, L. B. (2016). “Going outside while Staying inside - Exercise Motivation with Immersive vs. Non-immersive Recreational Virtual Environment Augmentation for Older Adult Nursing Home Residents,” in Proceeding of the 2016 IEEE International Conference on Healthcare Informatics (ICHI), Chicago, IL, USA, Oct. 2016 (IEEE), 216–226. doi:10.1109/ICHI.2016.31
Campo-Prieto, P., Cancela, J. M., and Rodríguez-Fuentes, G. (2021). Immersive Virtual Reality as Physical Therapy in Older Adults: Present or Future (Systematic Review). Virtual Reality 25, 801–817. doi:10.1007/s10055-020-00495-x
Chang, C.-J., Chern, J.-S., Yang, T.-F., and Yang, S.-W. (2016). Age-related Changes in Postural Re-balanced Ability during a Continuous and Unexpected Perturbation Integrated with Virtual Reality Scenes. Biomed. Eng. Appl. Basis Commun. 28 (03), 1650020. doi:10.4015/S1016237216500204
Corregidor-Sánchez, A. I., Segura-Fragoso, A., Rodríguez-Hernández, M., Jiménez-Rojas, C., Polonio-López, B., and Criado-Álvarez, J. J. (2021). Effectiveness of Virtual Reality Technology on Functional Mobility of Older Adults: Systematic Review and Meta-Analysis. Age and Ageing 50 (2), 370–379. doi:10.1093/ageing/afaa197
Craig, M., Wolbers, T., Harris, M. A., Hauff, P., Della Sala, S., and Dewar, M. (2016). Comparable Rest-Related Promotion of Spatial Memory Consolidation in Younger and Older Adults. Comparable rest-related Promot. Spat. Mem. consolidation younger Old. adultsNeurobiology Aging 48, 143–152. doi:10.1016/j.neurobiolaging.2016.08.007
Czaja, S. J., Boot, W. R., Charness, N., and Rogers, W. A. (2019). Designing for Older Adults: Principles and Creative Human Factors Approaches. 3rd Edition. Boca Raton: CRC Press.
Davis, S., Nesbitt, K., and Nalivaiko, E. (2014). “A Systematic Review of Cybersickness,” in Proceedings of the 2014 Conference on Interactive Entertainment - IE2014, December 2014, 1–9. doi:10.1145/2677758.2677780
Dermody, G., Whitehead, L., Wilson, G., and Glass, C. (2020). The Role of Virtual Reality in Improving Health Outcomes for Community-Dwelling Older Adults: Systematic Review. J. Med. Internet Res. 22, e17331. doi:10.2196/17331
Diener, E., Emmons, R. A., Larsen, R. J., and Griffin, S. (1985). The Satisfaction with Life Scale. J. Personal. Assess. 49, 71–75. doi:10.1207/s15327752jpa4901_13
Diener, E., Wirtz, D., Biswas-Diener, R., Tov, W., Kim-Prieto, C., Choi, D.-w., et al. (2009). New Measures of Well-Being. Soc. Indicators Res. 39, 247–266. doi:10.1007/978-90-481-2354-4_12
Geraets, C. N. W., Snippe, E., van Beilen, M., Pot-Kolder, R. M. C. A., Wichers, M., van der Gaag, M., et al. (2020). Virtual Reality Based Cognitive Behavioral Therapy for Paranoia: Effects on Mental States and the Dynamics Among Them. Schizophrenia Res. 222, 227–234. doi:10.1016/j.schres.2020.05.047
Gugenheimer, J., Mai, C., McGill, M., Williamson, J., Steinicke, F., and Perlin, K. (2019). “Challenges Using Head-Mounted Displays in Shared and Social Spaces,” in Conference on Human Factors in Computing Systems - Proceedings, May 2019, 1–8. doi:10.1145/3290607.3299028
Gugenheimer, J., Stemasov, E., Frommel, J., and Rukzio, E. (2017). “ShareVR,” in Conference on Human Factors in Computing Systems - Proceedings, 2017-May, 4021–4033. doi:10.1145/3025453.3025683
Gunkel, S., Stokking, H., Prins, M., Niamut, O., Siahaan, E., and Cesar, P. (2018). “Experiencing Virtual Reality Together,” in TVX 2018 - Proceedings of the 2018 ACM International Conference on Interactive Experiences for TV and Online Video, June 2018, 233–238. doi:10.1145/3210825.3213566
Hayhurst, J. (2018). “How Augmented Reality and Virtual Reality Is Being Used to Support People Living with Dementia-Design Challenges and Future Directions,” in Augmented Reality and Virtual Reality. Editors T. Jung, and M. C. tom Dieck, 295–305. doi:10.1007/978-3-319-64027-3_20
Hoffmann, F., Allers, K., Rombey, T., Helbach, J., Hoffmann, A., Mathes, T., et al. (2021). Nearly 80 Systematic Reviews Were Published Each Day: Observational Study on Trends in Epidemiology and Reporting over the Years 2000-2019. J. Clin. Epidemiol. 138, 1–11. doi:10.1016/j.jclinepi.2021.05.022
Howes, S. C., Charles, D., Pedlow, K., Wilson, I., Holmes, D., and McDonough, S. (2019). User-centred Design of an Active Computer Gaming System for Strength and Balance Exercises for Older Adults. J. Enabling Tech. 13 (2), 101–111. doi:10.1108/JET-12-2018-0057
Hutchison, A. (2007). “Back to the Holodeck,” in Proceedings of the 2nd International Conference on Digital Interactive Media in Entertainment and Arts - DIMEA ’07, September 2007, 98. doi:10.1145/1306813.1306838
Johnson-Glenberg, M. C., Birchfield, D. A., Tolentino, L., and Koziupa, T. (2014). Collaborative Embodied Learning in Mixed Reality Motion-Capture Environments: Two Science Studies. J. Educ. Psychol. 106 (1), 86–104. doi:10.1037/a0034008
J. P. Higgins, J. Thomas, J. Chandler, M. Cumpston, T. Li, M. J. Pageet al. (Editors) (2019). Cochrane Handbook for Systematic Reviews of Interventions (John Wiley & Sons).
Kang, M., and Russ, R. (2019). Activities that promote wellness for older adults in rural communities. J. Extension 47(5), 1-5. doi:10.3389/fnagi.2021.586999
Kim, A., Darakjian, N., and Finley, J. M. (2017). Walking in Fully Immersive Virtual Environments: an Evaluation of Potential Adverse Effects in Older Adults and Individuals with Parkinson's Disease. J. Neuroengineering Rehabil. 14, 16. doi:10.1186/s12984-017-0225-2
Kraus, M., and Kibsgaard, M. (2015). “A Classification of Human-To-Human Communication during the Use of Immersive Teleoperation Interfaces,” in Proceedings of the 2015 Virtual Reality International Conference on ZZZ - VRIC ’15, 08-10-Apri, 1–8. doi:10.1145/2806173.2806198
Kujawski, C., and Johnson, R. B. (2018). Controller Device (Patent No. USD848424S1). United States. Available From: https://patents.google.com/patent/USD848424S1/en.
Lawton, G. (2006). Making Virtual Reality More Accessible. Computer 39 (6), 12–15. doi:10.1109/MC.2006.204
Lee, M., Son, J., Kim, J., Pyun, S.-B., Eun, S.-D., and Yoon, B. (2016). Comparison of Individualized Virtual Reality- and Group-Based Rehabilitation in Older Adults with Chronic Stroke in Community Settings: a Pilot Randomized Controlled Trial. Eur. J. Integr. Med. 8 (5), 738–746. doi:10.1016/j.eujim.2016.08.166
Lee, M., Son, J., Kim, J., and Yoon, B. (2015). Individualized Feedback-Based Virtual Reality Exercise Improves Older Women's Self-Perceived Health: A Randomized Controlled Trial. Individualized feedback-based virtual reality Exerc. improves Old. women’s self-perceived Health A randomized controlled trialArchives Gerontol. Geriatr. 61, 154–160. doi:10.1016/j.archger.2015.06.010
Lee, Y., Choi, W., Lee, K., Song, C., and Lee, S. (2017). Virtual Reality Training with Three-Dimensional Video Games Improves Postural Balance and Lower Extremity Strength in Community-Dwelling Older Adults. J. Aging Physcial Activity 25 (4), 621–627. doi:10.1123/japa.2015-0271
Li, Y., Muñoz, J., Mehrabi, S., Middleton, L., Cao, S., and Boger, J. (2020). “Multidisciplinary Iterative Design of Exergames (MIDE): A Framework for Supporting the Design, Development, and Evaluation of Exergames for Health,” in HCI International 2020. Editor X. Fang (Springer), 128–147. doi:10.1007/978-3-030-50164-8_9
Lin, C. X., Lee, C., Lally, D., and Coughlin, J. F. (2018). “Impact of Virtual Reality (VR) Experience on Older Adults' Well-Being,” in Human Aspects of IT for the Aged Population. Applications in Health, Assistance, and Entertainment. ITAP 2018, 10927 LNCS, June 2018, 89–100. doi:10.1007/978-3-319-92037-5_8
Manera, V., Chapoulie, E., Bourgeois, J., Guerchouche, R., David, R., Ondrej, J., et al. (2016). A Feasibility Study with Image-Based Rendered Virtual Reality in Patients with Mild Cognitive Impairment and Dementia. PLOS ONE 11 (3), e0151487. doi:10.1371/journal.pone.0151487
Martin, P., Poon, L. W., Lee, K., Baek, Y., and Margrett, J. A. (2018). “Successful Aging: The Role of Cognition, Personality, and Whole-Person Wellness,” in Aging: Exploring a Complex Phenomenon. Editor S. Ahmad (CRC Press-Taylor & Francis), 525–541.
McGill, M. (2016). Supporting Collocated and At-A-Distance Experiences with TV and VR Displays. Glasgow: University of Glasgow.
Micarelli, A., Viziano, A., Micarelli, B., Augimeri, I., and Alessandrini, M. (2019). Vestibular Rehabilitation in Older Adults with and without Mild Cognitive Impairment: Effects of Virtual Reality Using a Head-Mounted Display. Arch. Gerontol. Geriatr. 83 (April), 246–256. doi:10.1016/j.archger.2019.05.008
Milgram, P., and Kishino, F. (1994). Taxonomy of Mixed Reality Visual Displays. IEICE Trans. Inf. Syst. 12, 1321–1329.
Miller, K. J., Adair, B. S., Pearce, A. J., Said, C. M., Ozanne, E., and Morris, M. M. (2014). Effectiveness and Feasibility of Virtual Reality and Gaming System Use at home by Older Adults for Enabling Physical Activity to Improve Health-Related Domains: a Systematic Review. Age Ageing 43 (1), 188–195. doi:10.1093/ageing/aft194
Moher, D., Liberati, A., Tetzlaff, J., and Altman, D. G.Prisma Group. (2009). Reprint-Preferred Reporting Items for Systematic Reviews and Meta-Analyses: The PRISMA Statement. Phys. Ther. 89 (9), 873–880. doi:10.1093/ptj/89.9.873
Molina, K. I., Ricci, N. A., de Moraes, S. A., and Perracini, M. R. (2014). Virtual Reality Using Games for Improving Physical Functioning in Older Adults: A Systematic Review. J. Neuroeng Rehabil. 11 (1), 156–220. doi:10.1186/1743-0003-11-156
Montague, D. P., and Walker‐Andrews, A. S. (2002). Mothers, fathers, and infants: The role of person familiarity and parental involvement in infants’ perception of emotion expressions. Child Dev. 73(5), 1339-1352
Molka-Danielsen, J., Prasolova-Forland, E., Fominykh, M., and Lamb, K. (2018). “Use of a Collaborative Virtual Reality Simulation for Multi-Professional Training in Emergency Management Communications,” in Proceedings of 2018 IEEE International Conference on Teaching, Assessment, and Learning for Engineering (TALE), Wollongong, NSW, Australia, Dec. 2018 (IEEE), 408–415. doi:10.1109/TALE.2018.8615147
Montana, J. I., Matamala-Gomez, M., Maisto, M., Mavrodiev, P. A., Cavalera, C. M., Diana, B., et al. (2020). The Benefits of Emotion Regulation Interventions in Virtual Reality for the Improvement of Wellbeing in Adults and Older Adults: A Systematic Review. J. Clin. Med. 9 (2), 500. doi:10.3390/jcm9020500
Mostajeran, F., Steinicke, F., Ariza Nunez, O. J., Gatsios, D., and Fotiadis, D. (2020). “Augmented Reality for Older Adults: Exploring Acceptability of Virtual Coaches for home-based Balance Training in an Aging Population,” in Proceedings of the 2020 CHI Conference on Human Factors in Computing Systems, 2020 April, 1–12. doi:10.1145/3313831.3376565
Neumann, D. L., Moffitt, R., Thomas, P. R., Loveday, K., Watling, D. P., Lombard, C. L., et al. (2018). A Systematic Review of the Application of Interactive Virtual Reality to Sport. Virtual Reality 22 (1), 183–198. doi:10.1007/s10055-017-0320-5
Niki, K., Okamoto, Y., Maeda, I., Mori, I., Ishii, R., Matsuda, Y., et al. (2019). A Novel Palliative Care Approach Using Virtual Reality for Improving Various Symptoms of Terminal Cancer Patients: A Preliminary Prospective, Multicenter Study. J. Palliat. Med. 22, 702–707. doi:10.1089/jpm.2018.0527
Nishchyk, A., Chen, W., Pripp, A. H., and Bergland, A. (2021). Effect of Mixed Reality Technologies for Fall Prevention Among Older Adults: A Systematic Review and Meta-Analysis (Preprint). JMIR aging 4 (2), e27972. doi:10.2196/27972
Radianti, J., Majchrzak, T. A., Fromm, J., and Wohlgenannt, I. (2020). A Systematic Review of Immersive Virtual Reality Applications for Higher Education: Design Elements, Lessons Learned, and Research Agenda. Comput. Edu. 147, 103778. doi:10.1016/j.compedu.2019.103778
Ramkhalawansingh, R., Butler, J. S., and Campos, J. L. (2018). Visual-vestibular Integration during Self-Motion Perception in Younger and Older Adults. Psychol. Aging 33, 798–813. doi:10.1037/pag0000271
Roberts, A. R., De Schutter, B., Franks, K., and Radina, M. E. (2019). Older Adults' Experiences with Audiovisual Virtual Reality: Perceived Usefulness and Other Factors Influencing Technology Acceptance. Clin. Gerontologist 42 (1), 27–33. doi:10.1080/07317115.2018.1442380
Robine, J.-M., Allard, M., Herrmann, F. R., and Jeune, B. (2019). The Real Facts Supporting Jeanne Calment as the Oldest Ever Human. The Journals Gerontol. Ser. A 74 (Suppl. ment_1), S13–S20. doi:10.1093/gerona/glz198
Skurla, M. D., Rahman, A. T., Salcone, S., Mathias, L., Shah, B., Forester, B. P., et al. (2021). Virtual Reality and Mental Health in Older Adults: A Systematic Review. Int. Psychogeriatr., 1–13. doi:10.1017/S104161022100017X
Smith, H. J., and Neff, M. (2018). “Communication Behavior in Embodied Virtual Reality,” in Proceedings of the International Conference on Human Factors in Computing Systems, April 2018, 1. doi:10.1145/3173574.3173863
Stanney, K., Lawson, B. D., Rokers, B., Dennison, M., Fidopiastis, C., Stoffregen, T., Weech, S., and Fulvio, J. M. (2020). Identifying Causes of and Solutions for Cybersickness in Immersive Technology: Reformulation of a Research and Development Agenda. Int. J. Human-Computer Interaction 36 (19), 1783–1803. doi:10.1080/10447318.2020.1828535
Stone, W. B. (2017). Psychometric Evaluation of the Simulator Sickness Questionnaire as a Measure of Cybersickness. Ames, IA: Iowa State University. Available From: https://lib.dr.iastate.edu/etd/15429.
Syed-Abdul, S., Malwade, S., Nursetyo, A. A., Sood, M., Bhatia, M., Barsasella, D., et al. (2019). Virtual Reality Among the Elderly: A Usefulness and Acceptance Study from Taiwan. BMC Geriatr. 19 (1), 223. doi:10.1186/s12877-019-1218-8
Thach, K. S., Lederman, R., and Waycott, J. (2020). “How Older Adults Respond to the Use of Virtual Reality for Enrichment: A Systematic Review,” in Proceeding of the 32nd Australian Conference on Human-Computer Interaction, 2020 December, 303–313. doi:10.1145/3441000.3441003
WalkinVR (2020). WalkinVR Driver. 2MW Elżbieta Bednarska. Available From: https://walkinvrdriver.com.
Waycott, J., Wadley, G., Baker, S., Ferdous, H. S., Hoang, T., Gerling, K., et al. (2018). “Manipulating Reality? Designing and Deploying Virtual Reality in Sensitive Settings,” in DIS 2018 - Companion Publication of the 2018 Designing Interactive Systems Conference, May 2018, 411–414. doi:10.1145/3197391.3197401
World Health Organization (2018). Ageing and Health. Retrieved Nov 1, 2021. Available From: https://www.who.int/news-room/fact-sheets/detail/ageing-and-health.
Yang, K.-T., Wang, C.-H., and Chan, L. (2018). “ShareSpace,” in UIST 2018 - Proceedings of the 31st Annual ACM Symposium on User Interface Software and Technology, October 2018, 499–509. doi:10.1145/3242587.3242630
Zhu, S., Sui, Y., Shen, Y., Zhu, Y., Ali, N., Guo, C., et al. (2021). Effects of Virtual Reality Intervention on Cognition and Motor Function in Older Adults with Mild Cognitive Impairment or Dementia: A Systematic Review and Meta-Analysis. Front. Aging Neurosci. 13, 217. doi:10.3389/fnagi.2021.586999
Keywords: extended reality, older adults, technology use, quality of life, systematic review
Citation: Margrett JA, Ouverson KM, Gilbert SB, Phillips LA and Charness N (2022) Older Adults’ Use of Extended Reality: A Systematic Review. Front. Virtual Real. 2:760064. doi: 10.3389/frvir.2021.760064
Received: 17 August 2021; Accepted: 28 December 2021;
Published: 26 January 2022.
Edited by:
Doug A. Bowman, Virginia Tech, United StatesReviewed by:
Denis Gracanin, Virginia Tech, United StatesSue Cobb, University of Nottingham, United Kingdom
Copyright © 2022 Margrett, Ouverson, Gilbert, Phillips and Charness. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Jennifer A. Margrett, bWFyZ3JldHRAaWFzdGF0ZS5lZHU=
†These authors share first authorship
 Jennifer A. Margrett
Jennifer A. Margrett Kaitlyn M. Ouverson
Kaitlyn M. Ouverson Stephen B. Gilbert
Stephen B. Gilbert L. Alison Phillips
L. Alison Phillips Neil Charness
Neil Charness