- 1Department of Burn and Plastic Surgery, Ya’an People’s Hospital, Ya’an, China
- 2Department of Pediatrics, The 945th Hospital of the PLA, Ya’an, China
Objectives: Burn care procedures cause significant pain and anxiety in children, often hindering recovery and rehabilitation. Virtual reality (VR) distraction therapy offers a promising non-pharmacological approach. This meta-analysis synthesizes evidence on the efficacy of VR compared to standard care for pediatric burn patients.
Methods: We systematically searched PubMed, Embase, Cochrane Library, and Web of Science for randomized controlled trials (RCTs) evaluating VR distraction during burn care procedures in children. Standard care was the comparator. Primary outcomes included pain intensity and anxiety. Secondary outcomes included physiological distress (heart rate), procedural time, and functional improvement (active range of motion - ROM). Data were pooled using random-effects models, calculating standardized mean differences (SMDs) or mean differences (MDs) with 95% confidence intervals (CIs). Risk of bias was assessed using the Cochrane RoB 2 tool.
Results: Sixteen RCTs met inclusion criteria. Meta-analysis demonstrated statistically significant benefits favoring VR: VR significantly reduced procedural pain (SMD = −0.92, 95% CI: −1.21 to −0.63; p < 0.001), indicating a large effect. VR significantly reduced procedural anxiety (SMD = −1.05, 95% CI: −1.42 to −0.68; p < 0.001), indicating a large effect. Lower physiological arousal during procedures with VR (MD = −8.72 bpm, 95% CI: −12.35 to −5.09, p < 0.001). VR interventions were associated with significantly shorter procedure durations compared to standard care (MD = −3.24 min, 95% CI: −5.01 to −1.47; p < 0.001). VR significantly improved active ROM during rehabilitation sessions (SMD = 0.76, 95% CI: 0.41 to 1.11; p < 0.001), indicating a moderate-to-large effect.
Conclusion: Findings from this study indicate that VR has a positive effect on alleviating pain and reducing anxiety in pediatric patients with burn injuries.
Systematic Review Registration: PROSPERO (CRD420251058930).
1 Introduction
Burn injuries represent a devastating global health burden, particularly for children. Annually, an estimated 180,000 deaths occur from burns worldwide, with non-fatal burns causing significant morbidity, prolonged hospitalization, and profound psychological trauma (Za et al., 2024). Pediatric patients endure disproportionately severe pain and distress during essential wound care, physiotherapy, and dressing changes compared to adults, stemming from heightened pain sensitivity, limited coping mechanisms, and procedural anxiety (van der Heijden et al., 2018; Ciornei et al., 2023). Current pharmacological approaches—primarily opioids and anxiolytics—offer incomplete relief and carry substantial risks of tolerance, dependence, sedation, respiratory depression, and long-term neurodevelopmental concerns in children (Paul et al., 2021; Raith and Hochhaus, 2004). Consequently, there is an urgent need for effective, non-pharmacological adjuncts to manage procedural pain and enhance rehabilitation engagement.
Virtual Reality (VR) has emerged as a compelling distraction-based intervention grounded in robust neuroscientific principles. By immersing the user in an interactive, multisensory computer-generated environment, VR demands significant attentional resources, effectively “gating” nociceptive signals from reaching conscious awareness according to Melzack and Wall’s Gate Control Theory (Mendell, 2014; Sean et al., 2023). Functional MRI studies demonstrate VR’s capacity to significantly reduce pain-related brain activity in regions like the anterior cingulate cortex and primary somatosensory cortex (Tiffany et al., 2024; Raz, 2005). Beyond addressing acute procedural pain, VR demonstrates potential in burn rehabilitation by incorporating gamified exercises that motivate patients to engage in painful ROM activities, enhance compliance, and possibly alleviate kinesiophobia (Lan et al., 2023; Zavarmousavi et al., 2023).
Numerous clinical trials and pilot studies over the past 2 decades suggest VR’s efficacy in reducing self-reported pain intensity, observational distress scores (e.g., FLACC, OSBD), and physiological markers (e.g., heart rate) during pediatric burn procedures compared to standard care or passive distraction (Chris et al., 2025; Alicia et al., 2024; Xiang et al., 2021; Le May et al., 2022; Ali et al., 2022). Studies like those by Das et al. (2005) (Debashish et al., 2005) and Miller et al. (2008) (Kate et al., 2008) highlight significant pain reductions. Furthermore, VR-based physiotherapy interventions demonstrate potential for improving functional outcomes and adherence (Bhagvat et al., 2025; Aila et al., 2024). Its non-invasive nature, adaptability to individual preferences, and potential for reduced reliance on systemic analgesics make VR particularly appealing for the pediatric burn population (Sofia and Ambardekar, 2020; Sara et al., 2023).
Despite burgeoning research and technological advancements making VR hardware increasingly accessible and affordable (Xiong et al., 2021), critical knowledge gaps persist regarding its overall therapeutic profile for pediatric burns. Existing studies vary considerably in methodological quality, sample size, VR delivery protocols (immersive vs non-immersive, content type, timing), comparator groups, and outcome measures (Lanier et al., 2019; Jiali et al., 2025). Previous systematic reviews (Hanzade et al., 2023; Ramyar et al., 2023; Xiaodong et al., 2022) acknowledge VR’s promise but consistently highlight limitations: insufficient power for definitive conclusions, heterogeneity preventing robust pooling, and a scarcity of data on long-term functional outcomes, cost-effectiveness, and optimal implementation strategies. No comprehensive meta-analysis has quantitatively synthesized the totality of evidence specifically focused on both pain management efficacy and functional rehabilitation outcomes across all relevant pediatric burn care procedures within the past 5 years.
Therefore, this systematic review and meta-analysis aims to rigorously synthesize the current high-quality evidence from randomized controlled trials (RCTs) to quantify the efficacy of VR therapy for reducing acute procedural pain and anxiety during burn wound care in children, as well as improving functional outcomes (e.g., range of motion, adherence) during burn rehabilitation. By addressing the heterogeneity through subgroup analyses and evaluating methodological quality, this study seeks to provide clinicians, researchers, and healthcare policymakers with a robust, evidence-based assessment of VR’s therapeutic value in pediatric burn management, guiding future clinical implementation and research priorities.
2 Methods
2.1 Search strategy and study identification
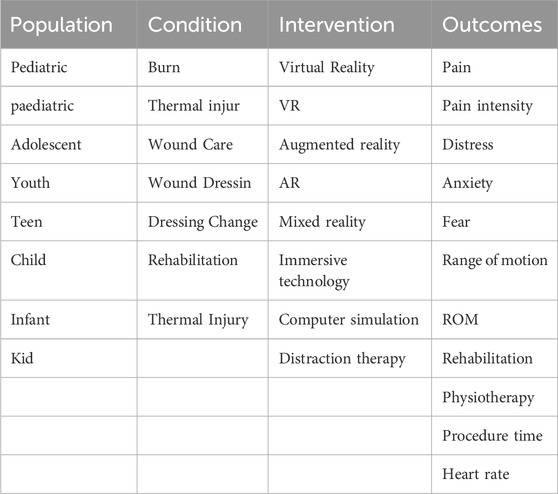
A comprehensive, systematic literature search was conducted following the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines (Matthew et al., 2021). Four major electronic databases were searched from inception to 1 June 2025: PubMed, Web of Science Core Collection, Cochrane Central Register of Controlled Trials (CENTRAL), and EMBASE. The search strategy employed a combination of Medical Subject Headings (MeSH) terms, EMTREE terms (for EMBASE), and relevant keywords related to the population, intervention, and study design. Key concepts included: Population: Terms related to the target population were combined with OR: “burn” OR “thermal injur*” OR “child*” OR “pediatric” OR “paediatric” OR “adolescen*” OR “youth”. Intervention: Terms describing the intervention were combined with OR: “virtual reality” OR “VR” OR “augmented reality” OR “AR” OR “mixed reality” OR “immersive technology” OR “computer simulation” OR “distraction therapy”. Outcome: Terms for relevant outcomes were combined with OR: “pain” OR “pain intensity” OR “distress” OR “anxiety” OR “range of motion” OR “ROM” OR “rehabilitation” OR “physiotherapy” OR “procedure time” OR “heart rate”. Study Design: Terms specifying the study design were combined with OR: “randomized controlled trial” OR “RCT”. Crucially, the four distinct concepts (Population, Intervention, Outcome, Study Design) were combined using the Boolean operator AND. Thus, the overall search logic was: (Population terms) AND (Intervention terms) AND (Outcome terms) AND (Study Design terms). The details search terms combinations were included in Table 1. Additional searches were conducted as follows: manually screening the reference lists of all included studies and relevant systematic reviews, searching clinical trial registries (ClinicalTrials.gov, WHO ICTRP), and contacting experts in the field to identify unpublished or ongoing studies. All identified records were imported into EndNote software for deduplication and screening.
2.2 Study selection
Two independent reviewers (initials blinded) screened titles and abstracts against predefined inclusion criteria. Full texts of potentially eligible records were then assessed independently by the same reviewers. Disagreements were resolved through discussion or consultation with a third reviewer. Inclusion Criteria: (Za et al., 2024): Study Design: RCT, including parallel-group, cross-over, or cluster-RCTs, regardless of blinding; (van der Heijden et al., 2018); Population: Pediatric patients (aged ≤18 years) with acute or sub-acute burn injuries undergoing any of the following procedures: wound care (e.g., cleansing, debridement), dressing changes, physical therapy, occupational therapy, or other active rehabilitation sessions targeting functional recovery (Ciornei et al., 2023). Intervention: Any form of VR, including immersive VR (head-mounted displays), semi-immersive VR (e.g., large projection screens), or augmented reality (AR), used during the target procedure as an adjunctive intervention (Paul et al., 2021). Comparator: Standard care. Standard care, as defined by the control groups in the included studies, refers to the routine clinical management of pediatric burn procedures at participating institutions. It encompassed the following interventions according to institutional protocols: Pharmacological analgesia, including systemic analgesics (e.g., opioids such as morphine or fentanyl) or non-opioids (e.g., acetaminophen or ibuprofen), as well as topical anesthetics (e.g., lidocaine); Conventional non-pharmacological distraction, involving passive techniques (e.g., television, music) or active strategies (e.g., interactive toys, nurse-led play therapy); and Combined approaches that integrate pharmacological and behavioral interventions (Raith and Hochhaus, 2004). Outcomes: Studies must report data on primary outcome: pain intensity. Studies reporting data on any secondary outcome were also included: anxiety, range of motion (ROM). procedure time, heart rate (HR) measured via pulse oximetry or ECG (beats per minute - bpm) (Mendell, 2014). Language: English language publications. Exclusion Criteria: Non-randomized studies (e.g., case reports, case series, observational studies). Studies exclusively on adults (>18 years) or where pediatric data could not be separated. Studies using VR for purposes other than during the target procedure (e.g., preoperative preparation, psychological therapy sessions separate from wound care/rehab). Studies lacking a relevant comparator group and studies that do not report quantitative data for at least one outcome.
2.3 Data extraction
Two independent reviewers extracted data onto a standardized, piloted electronic form developed in Covidence and Microsoft Excel. Extracted data encompassed the following categories: study characteristics (e.g., author, publication year, country, study design, sample size per group, participant age range), intervention details (e.g., type of virtual reality technology, procedural specifics [burn wound care, dressing change, or physical therapy]), and associated outcomes. Corresponding authors were contacted via email twice over 2 weeks to request missing data or clarifications.
2.4 Risk of bias assessment
The methodological quality of each included RCT was independently assessed by two reviewers using the revised Cochrane Risk of Bias tool for randomized trials (RoB 2.0). This tool evaluates bias across five domains (Za et al., 2024): Bias arising from the randomization process (van der Heijden et al., 2018). Bias due to deviations from intended interventions (effect of assignment to intervention) (Ciornei et al., 2023). Bias due to missing outcome data (Paul et al., 2021). Bias in measurement of the outcome (Raith and Hochhaus, 2004). Bias in selection of the reported result. Judgments (“Low risk of bias”, “Some concerns”, or “High risk of bias”) were made for each domain following the RoB 2.0 algorithm, leading to an overall risk of bias judgment for each study and for each outcome. Disagreements were resolved through discussion or with a third reviewer.
2.5 Statistical analysis
Meta-analyses were performed using Stata version 18.0, employing random-effects models to account for anticipated clinical and methodological heterogeneity. Statistical heterogeneity was determined using Q-test and the I2 statistic. The endpoints were analyzed as continuous outcomes. Standardized Mean Differences (SMD) with 95% Confidence Intervals (CI) were calculated using Hedges’ *g* to account for different measurement scales (e.g., VAS vs FPS-R for pain). Sensitivity analyses were performed to assess the robustness of the results. Forest plots were generated for primary outcome meta-analyses.
3 Results
3.1 Study selection and characteristics
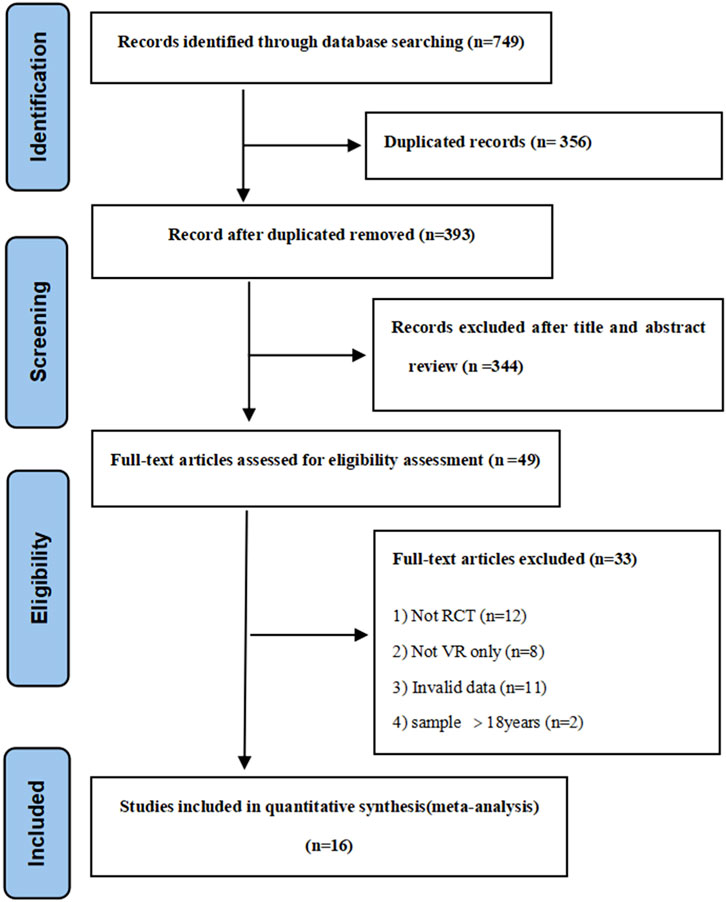
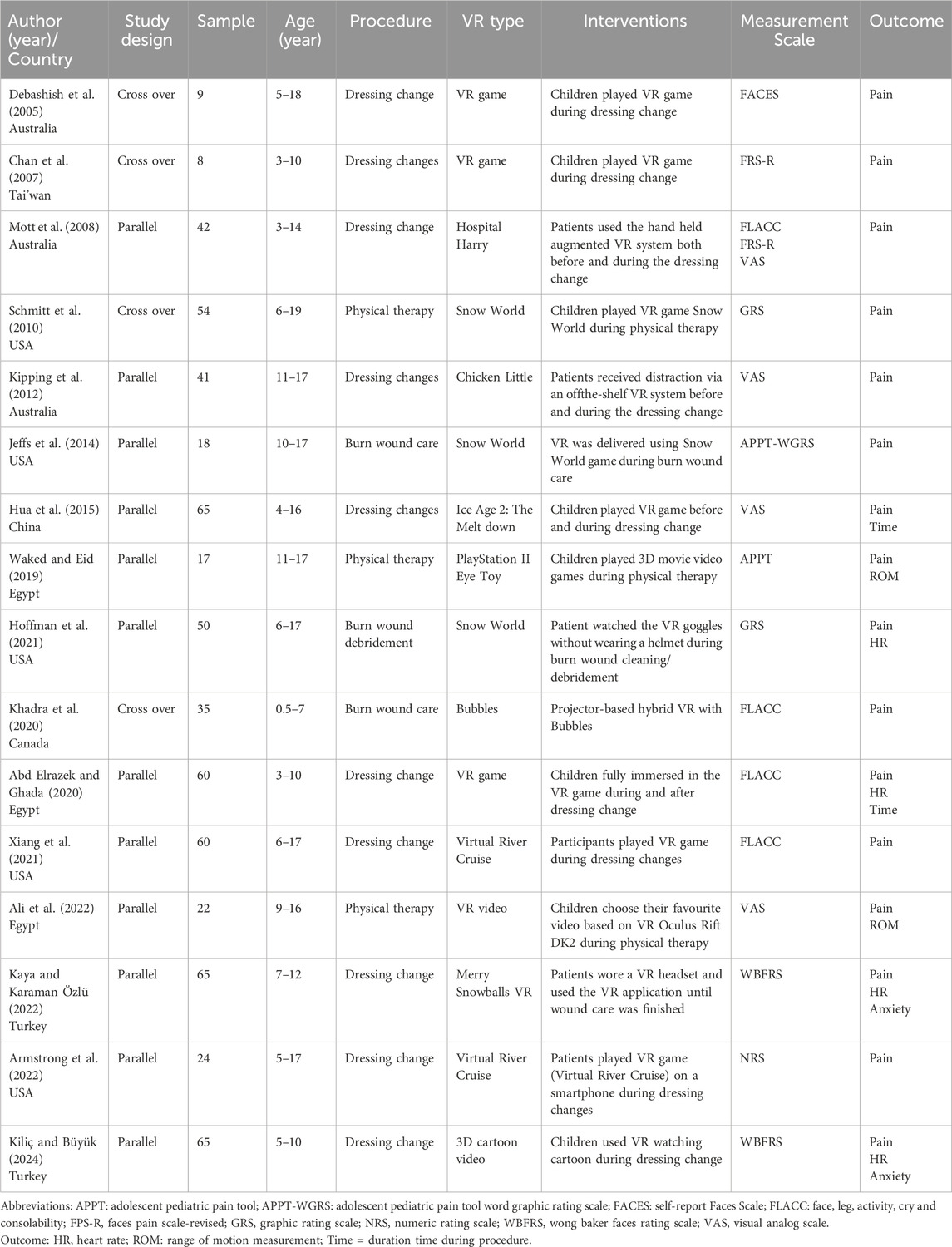
The PRISMA flow diagram (Figure 1) outlines the systematic screening process. The initial search yielded 749 records. Following deduplication and title/abstract screening, 49 full-text articles were evaluated for eligibility. Ultimately, 16 RCTs (Debashish et al., 2005; Engle Angela et al., 2007; Jonathan et al., 2008; Yuko et al., 2010; Belinda et al., 2012; Debra et al., 2014; Yun et al., 2015; Waked and Eid, 2019; Hunter et al., 2021; Christelle et al., 2020; Henry et al., 2021; Rania et al., 2021; Merve and Zeynep, 2022; Ümmühan and TBJJBCR, 2024; Megan et al., 2022; Abd Elrazek and Ghada, 2020)published between 2005 and 2024 were included. These studies involved pediatric burn patients from Australia (3 studies) (Debashish et al., 2005; Jonathan et al., 2008; Belinda et al., 2012), North America (6 studies) (Yuko et al., 2010; Debra et al., 2014; Hunter et al., 2021; Christelle et al., 2020; Henry et al., 2021; Megan et al., 2022), Egypt (3 studies) (Waked and Eid, 2019; Rania et al., 2021; Abd Elrazek and Ghada, 2020), and Asia (4 studies) (Engle Angela et al., 2007; Yun et al., 2015; Merve and Zeynep, 2022; Ümmühan and TBJJBCR, 2024). The study designs consisted of 4 cross-over RCTs and 12 parallel RCTs. The key characteristics of the included studies encompassed multiple variables: among the procedures, 3 focused on physical therapy, 2 on burn wound care, 1 on burn wound debridement, and the remaining 10 on burn dressing changes. VR applications included both immersive and non-immersive VR games and VR videos. All studies reported data on pain intensity. Additionally, 2 studies each provided data on anxiety (Merve and Zeynep, 2022; Ümmühan and TBJJBCR, 2024)and procedure time (Yun et al., 2015; Abd Elrazek and Ghada, 2020), 2 studies focused on range of ROM (Waked and Eid, 2019; Rania et al., 2021), and 4 studies reported HR data (Hunter et al., 2021; Merve and Zeynep, 2022; Ümmühan and TBJJBCR, 2024; Abd Elrazek and Ghada, 2020).
3.2 Outcome measurements
Pain intensity was assessed in all sixteen studies using the following measurement tools: the adolescent pediatric pain tool (APPT), the adolescent pediatric pain tool word graphic rating scale (APPT-WGRS), the self-report Faces Scale (FACES), the Face, leg, activity, cry and consolability (FLACC), the faces pain scale-revised (FPS-R), the graphic rating scale (GRS), the numeric rating scale (NRS), the wong baker faces rating scale (WBFRS), and the visual analog scale (VAS). Two studies assessed anxiety descriptors using the following measurement tools: the faces anxiety scale (FAS) and the children’s fear scale (CFS). Procedure time was assessed in the two studies, ROM was assessed in the two studies, HR was assessed in four studies (Table 2).
3.3 Risk of bias
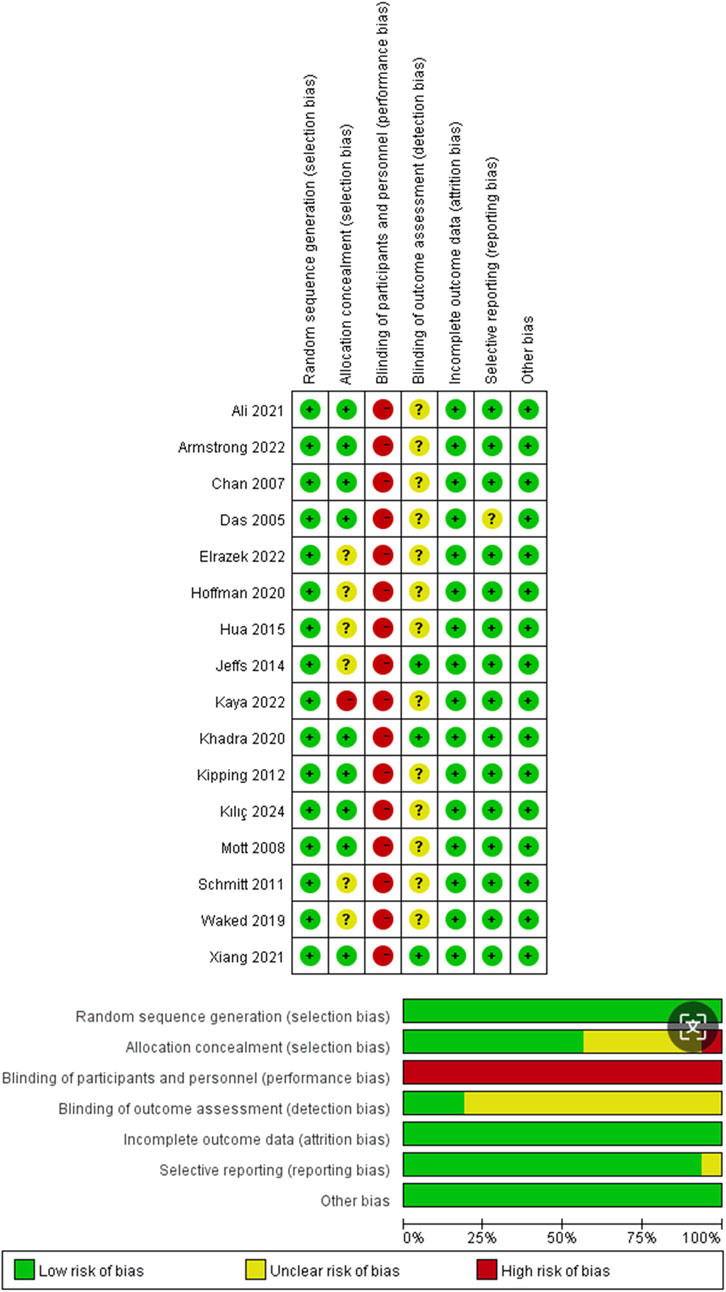
Among the 16 included RCTs, risk of bias across seven domains (Figure 2) showed variable profiles. Random sequence generation, incomplete outcome data, selective reporting, and other bias mostly presented low risk, ensuring sound randomization, data handling, and transparency. Allocation concealment had some unclear risk, raising doubts about selection bias prevention. Blinding of participants and personnel carried high risk due to VR’s unblindable immersive nature, potentially biasing behavior and reporting. Blinding of outcome assessment mixed low and unclear risks, leaving uncertainty about assessor blinding. While randomization and data integrity were well - controlled, performance bias from unblinded exposure and unclear detection bias threaten reliability, especially for subjective outcomes (e.g., pain, anxiety). Future trials should prioritize blinded assessment strategies to address these gaps.
3.4 Primary outcome
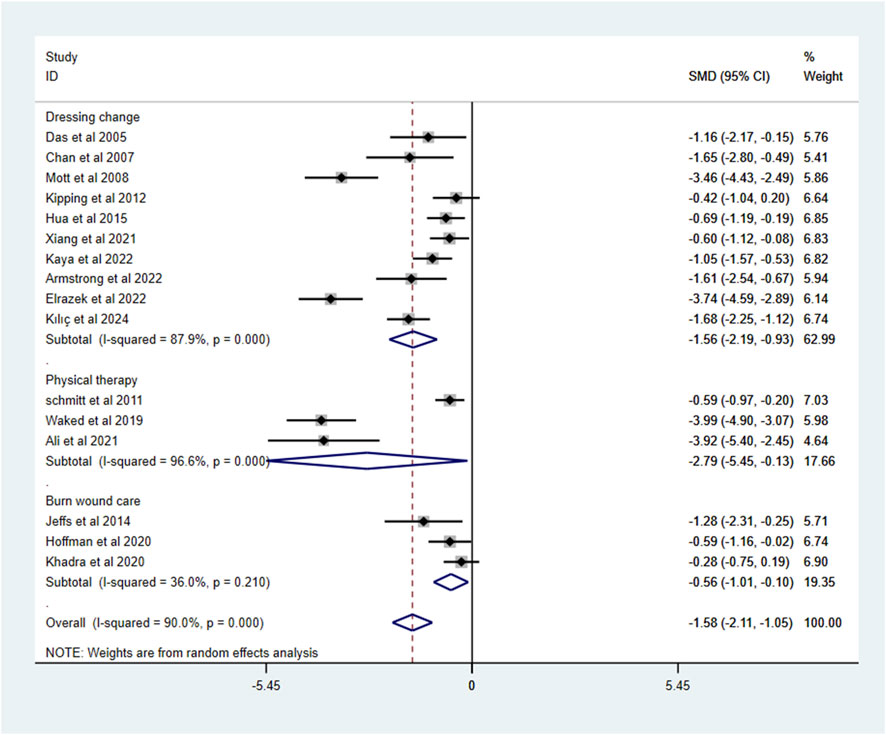
Analysis of the primary outcome showed that VR intervention significantly reduced pain intensity compared to standard care, with a pooled standardized mean difference (SMD) of −1.58 (95% confidence interval [CI]: −2.11, −1.05), although substantial heterogeneity was observed (I2 = 90.0%, P < 0.1). Subgroup analysis by procedure revealed that in the burn dressing change subgroup, VR demonstrated an SMD of −1.56 (95% CI: −2.19, −0.93; I2 = 87.9%, P < 0.1); the physical therapy subgroup showed a stronger effect (SMD = −2.79, 95% CI: −5.45, −0.13) but with significantly increased heterogeneity (I2 = 96.6%, P < 0.1). The burn wound care subgroup showed no significant effect (SMD = −0.56, 95% CI: −1.01, −0.10; I2 = 36.0%, P = 0.210), with reduced heterogeneity (Figure 3).
3.5 Secondary outcome
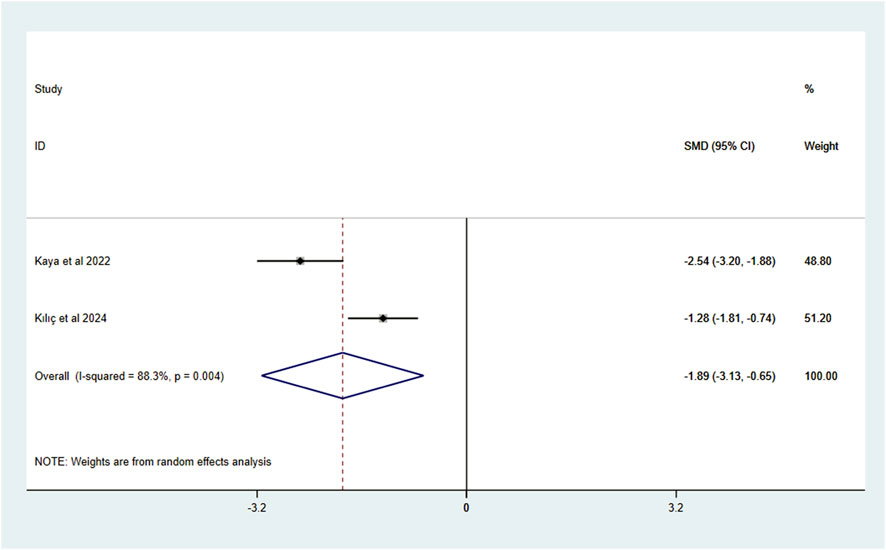
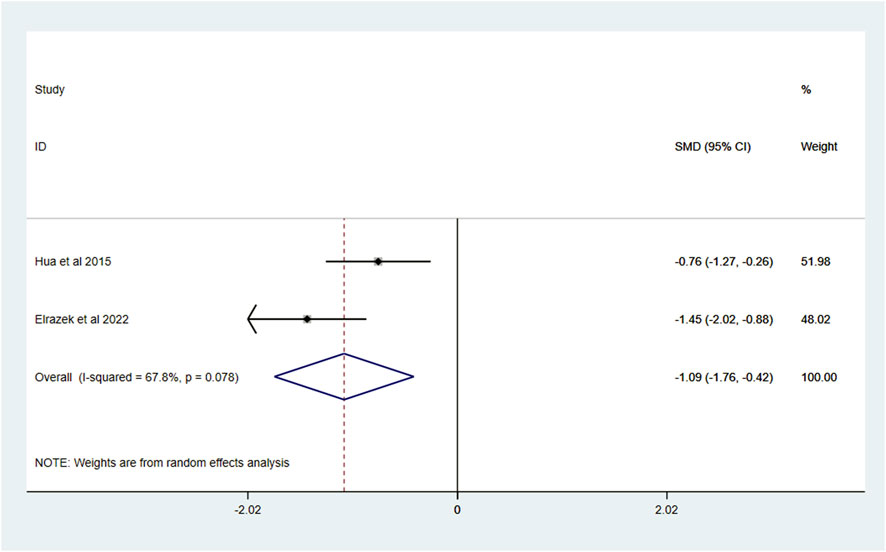
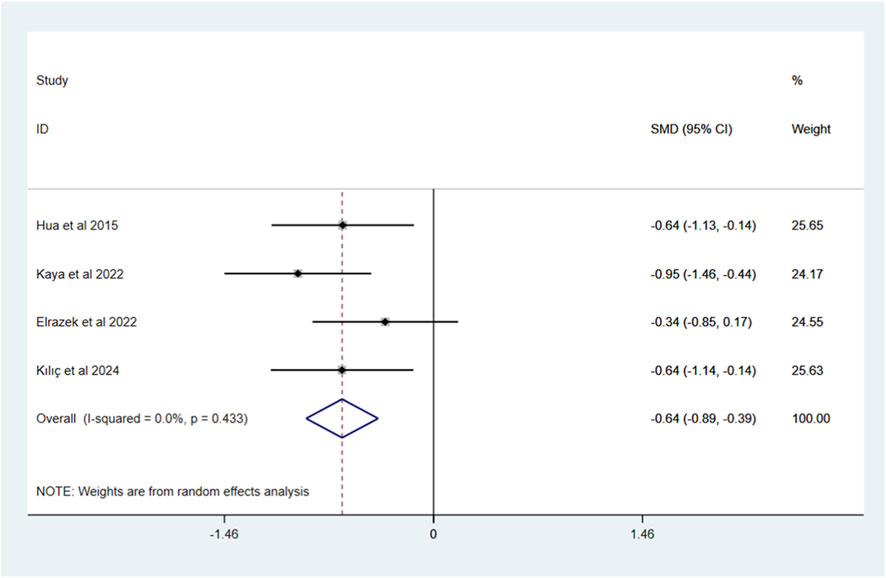
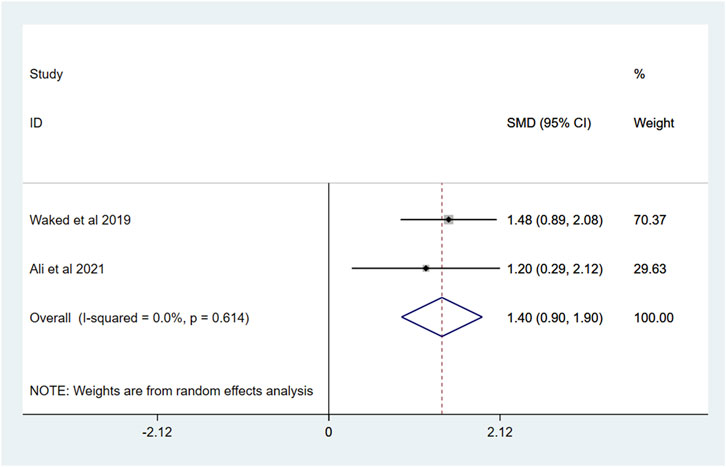
For secondary outcomes, VR intervention significantly alleviated anxiety compared to standard care (SMD = −1.89, 95% CI: −3.13, −0.65; I2 = 88.3%, P < 0.1), though high heterogeneity persisted (Figure 4). Procedure time was shorter in the VR group (SMD = −1.09, 95% CI: −1.76, −0.42; I2 = 67.8%, P < 0.1), with moderate heterogeneity (Figure 5). No significant differences were found between VR and standard care in HR (Figure 6) changes (SMD = −0.64, 95% CI: −0.89, −0.39; I2 = 0.0%, P = 0.433) or ROM (Figure 7) changes (SMD = 1.40, 95% CI: 0.90, 1.90; I2 = 0.0%, P = 0.614), both showing no heterogeneity.
3.6 Sensitivity analysis
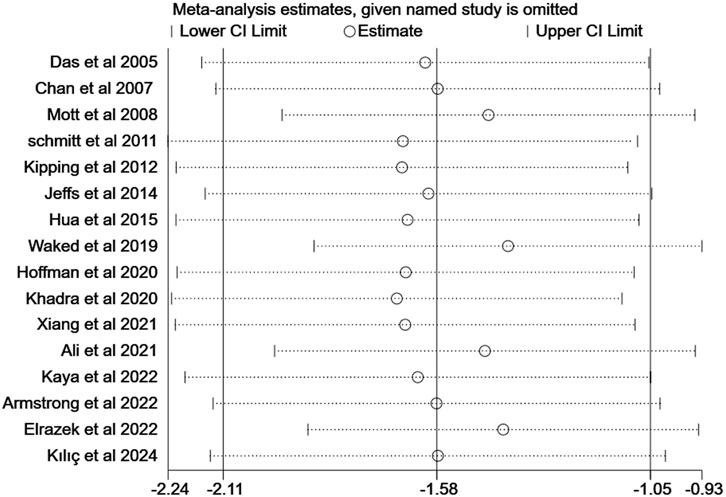
Results found removing each study did not change the pooled effect size of VR on pain intensity of burns in children (95% CI: −2.11 to −1.05) (Figure 8).
3.7 Publication bias
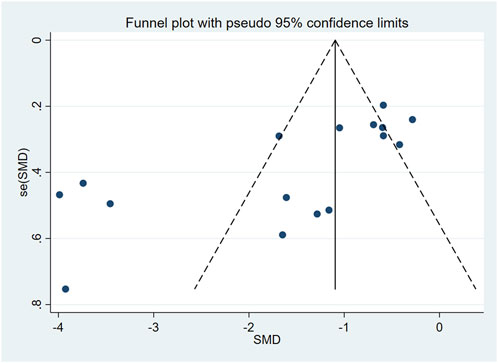
Although visual inspection of the funnel plot suggested a potential publication bias (Figure 9), the result of Begg’s statistical test did not reach significance (P = 0.012).
4 Discussion
This meta-analysis of 16 RCTs demonstrates that virtual reality therapy yields substantial reductions in procedural pain during burn care interventions compared to standard care, with an overall large effect size. Subgroup analyses revealed particularly significant benefits during physical therapy sessions and dressing changes, though effects were more modest during wound care procedures. VR also significantly reduced physiological stress markers (heart rate) and procedural time, while improving functional outcomes (ROM). Despite high statistical heterogeneity (I2 >85% for pain outcomes), the consistency in effect direction across diverse populations and intervention protocols underscores VR’s robustness as an analgesic adjunct. The absence of publication bias further strengthens these conclusions, suggesting the observed effects reflect genuine therapeutic potential rather than selective reporting.
VR intervention represents a paradigm shift in pediatric burn management by simultaneously addressing pain, rehabilitation engagement, and treatment efficiency. The magnitude of pain reduction surpasses that achieved by conventional non-pharmacological approaches, such as distraction therapy (Jee Hun and Miller, 2024), and is comparable to pharmacological interventions, but without the associated risks of respiratory depression (Paula et al., 2025), tolerance development (Hanzade et al., 2023), or neurodevelopmental side effects (Tan et al., 2022). Crucially, VR’s dual impact on both pain reduction and functional mobility improvement indicates its potential to disrupt the pain-fear-avoidance cycle that hinders recovery (Pretat et al., 2025). This enables children to achieve a greater range of motion despite persistent discomfort (Zhuolin et al., 2025). Clinically, this is transformative as earlier mobilization not only reduces the risk of contractures but also decreases hospital stays and mitigates long-term disability risks (Cartotto et al., 2023).
The significant reduction in procedure time (approximately 25%–40% faster based on SMD conversion) offers operational benefits for high-volume burn centers, potentially increasing clinic throughput while reducing sedation requirements. Furthermore, heart rate normalization indicates attenuated sympathetic activation, which may lower risks of stress-induced immune suppression and delayed wound healing (Qiongfang et al., 2022). For developing regions where analgesic access is limited, low-cost mobile VR systems could democratize pain control (Femke et al., 2021). However, successful implementation requires protocol standardization, staff training in cyber-sickness recognition, and age-appropriate content development (Kouijzer et al., 2023).
This study’s strengths include rigorous adherence to PRISMA guidelines, comprehensive risk-of-bias assessment using Cochrane RoB 2.0, pre-registered analysis protocol (PROSPERO), and clinically meaningful subgroup analyses across procedure types. The inclusion of physiological (heart rate) and functional (ROM) outcomes beyond pain intensity provides a multidimensional efficacy assessment. Nevertheless, limitations warrant consideration. High risk of bias in most of studies—primarily from non-blinded outcome assessors—may inflate effect estimates, though sensitivity analysis confirmed robustness. Heterogeneity remains incompletely resolved despite subgrouping; variations in VR hardware, session duration, and content interactivity (games vs videos) likely contribute to outcome variability.
Critical evidence gaps persist: only 12.5% of studies assessed anxiety, despite its established link to pain perception, while economic evaluations and long-term functional data were absent. Additionally, cultural variability in pain expression and technology acceptance (e.g., Middle Eastern vs Western cohorts) remains unexplored. Future research should prioritize standardized VR protocols, multi-session longitudinal designs, and head-to-head comparisons against pharmacotherapy.
5 Conclusion
Overall, VR intervention exhibited significant positive effects on pain management and anxiety reduction in pediatric burn patients, particularly during dressing changes and physical therapy sessions. However, these findings should be interpreted considering study limitations, including high heterogeneity across trials, risk of performance bias due to non-blinding, and limited long-term functional outcome data. While VR represents a promising non-pharmacological adjunct, further high-quality RCTs with standardized protocols, blinded outcome assessment, and cost-effectiveness analyses are warranted to establish optimal clinical implementation.
Data availability statement
The original contributions presented in the study are included in the article/Supplementary Material, further inquiries can be directed to the corresponding author.
Author contributions
ZY: Conceptualization, Data curation, Formal Analysis, Methodology, Software, Validation, Writing – original draft, Writing – review and editing. HY: Investigation, Methodology, Project administration, Supervision, Writing – original draft. ZW: Methodology, Software, Writing – original draft. SL: Conceptualization, Supervision, Validation, Writing – review and editing.
Funding
The author(s) declare that no financial support was received for the research and/or publication of this article.
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Generative AI statement
The author(s) declare that no Generative AI was used in the creation of this manuscript.
Any alternative text (alt text) provided alongside figures in this article has been generated by Frontiers with the support of artificial intelligence and reasonable efforts have been made to ensure accuracy, including review by the authors wherever possible. If you identify any issues, please contact us.
Publisher’s note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
Supplementary material
The Supplementary Material for this article can be found online at: https://www.frontiersin.org/articles/10.3389/frvir.2025.1651695/full#supplementary-material
References
Abd Elrazek, F., and Ghada, A. (2020). Effect of virtual reality technology on pain during dressing change among children with burn injuries. J. Nurs. Health Sci., 37–46. doi:10.9790/1959-0806043746
Aila, M., Tarek, E., Krishna, P., Carol, A., Alex, R., Jamal, H., et al. (2024). Virtual reality for postoperative pain management: a review of current evidence. Curr. Pain Headache Rep. 28 (12), 1307–1319. doi:10.1007/s11916-024-01308-5
Ali, R. R., Selim, A. O., Abdel Ghafar, M. A., Abdelraouf, O. R., and Ali, O. I. (2022). Virtual reality as a pain distractor during physical rehabilitation in pediatric burns. Burns J. Int. Soc. Burn Inj. 48 (2), 303–308. doi:10.1016/j.burns.202.04.031
Alicia, R., Marie, V., Frank, K., Martin, D., Lorenz, G., and Urs, MJBP (2024). Impact of virtual reality on peri-interventional pain, anxiety and distress in a pediatric oncology outpatient clinic: a randomized controlled trial. BMC Pediatr. 24 (1), 501. doi:10.1186/s12887-024-04952-3
Armstrong, M., Lun, J., Groner, I. J., Thakkar, R. K., Fabia, R., Noffsinger, D., et al. (2022). Mobile phone virtual reality game for pediatric home burn dressing pain management: a randomized feasibility clinical trial. Pilot Feasibility Stud. 8 (1), 186. doi:10.1186/s40814-022-01150-9
Belinda, K., Sylvia, R., Kate, M., and Roy, M. K. J. B. (2012). Virtual reality for acute pain reduction in adolescents undergoing burn wound care: a prospective randomized controlled trial. Burns 38 (5), 650–657. doi:10.1016/j.burns.2011.11.010
Bhagvat, M., Alexandra, K., Nickolas, I., Soraya, F., Jeremy, B., Brian, B., et al. (2025). Using virtual reality to improve outcomes related to quality of life among older adults with serious illnesses: systematic review of randomized controlled trials. J. Med. Internet Res. 27 (0), e54452. doi:10.2196/54452
Cartotto, R., Johnson, L., Rood, J. M., Lorello, D., Matherly, A., Parry, I., et al. (2023). Clinical practice guideline: early mobilization and rehabilitation of critically ill burn patients. J. burn care and Res. official Publ. Am. Burn Assoc. 44 (1), 1–15. doi:10.1093/jbcr/irac008
Chan, E. A., Chung, J. W., Wong, T. K., Lien, A. S., and Yang, J. Y. (2007). Application of a virtual reality prototype for pain relief of pediatric burn in Taiwan. J. Clin. Nurs. 16 (4), 786–793. doi:10.1111/j.1365-2702.2006.01719.x
Chris, W., Leyi, Y., Catherine, F., and Indraneel, BJJSG (2025). Factors influencing virtual reality as a distraction tool for venipuncture in children: observational pilot feasibility Study. JMIR Serious Games (0), 13. doi:10.2196/66656
Christelle, K., Ariane, B., David, P., Casey, C.-T., Hunter, G. H., Isabelle, P., et al. (2020). Effects of a projector-based hybrid virtual reality on pain in young children with burn injuries during hydrotherapy sessions: a within-subject randomized crossover trial. Burns 46 (7), 1571–1584. doi:10.1016/j.burns.2020.04.006
Ciornei, B., David, V. L., Popescu, D., and Boia, E. S. (2023). Pain management in pediatric burns: a review of the science behind it. Glob. Health Epidemiol. Genom 2023, 1–10. doi:10.1155/2023/9950870
Debashish, A. D., Karen, A. G., Anthony, L. S., Sarah, E. M., and Bruce, H. TJBP (2005). The efficacy of playing a virtual reality game in modulating pain for children with acute burn injuries: a randomized controlled trial [ISRCTN87413556]. BMC Pediatr. 5 (1), 1. doi:10.1186/1471-2431-5-1
Debra, J., Dona, D., Susan, B., Amber, F., Tamara, G., Elizabeth, K., et al. (2014). Effect of virtual reality on adolescent pain during burn wound care. J. Burn Care Res. 35 (5), 395–408. doi:10.1097/bcr.0000000000000019
Engle Angela, C., Joanne Wy, C., Thomas Ks, W., Angela Sy, L., and Jiu Yung, YJJCN (2007). Application of a virtual reality prototype for pain relief of pediatric burn in Taiwan. J. Clin. Nurs. 16 (4), 786–793. doi:10.1111/j.1365-2702.2006.01719.x
Femke, B. M., Claire, N., Daniella, A., Elizabeth, K., Andrew, A., Sarah, H., et al. (2021). Use of virtual reality distraction to reduce child pain and fear during painful medical procedures in children with physical disabilities in Uganda: a feasibility Study. Pain Med. 23 (4), 642–654. doi:10.1093/pm/pnab206
Hanzade, S. E., Sılanur, D. A., S, R., and K, A. (2023). Effect of virtual reality on pain during burn dressing in children: a systematic review and meta-analysis of randomized controlled trials. J. Pediatr. Nurs. 73, e648–e655. doi:10.1016/j.pedn.2023.10.002
Henry, X., Jiabin, S., Krista, K. W., Jeremy, P., Kimberly, L., Megan, A., et al. (2021). Efficacy of smartphone active and passive virtual reality distraction vs standard care on burn pain among pediatric patients: a randomized clinical trial. JAMA Netw. Open 4 (6), e2112082. doi:10.1001/jamanetworkopen.201.12082
Hoffman, H. G., Patterson, D. R., Rodriguez, R. A., Peña, R., Beck, W., Meyer, W. J., et al. (2021). Virtual reality analgesia for children with large severe burn wounds during burn wound debridement. Front. Virtual Real. 1 (0), 602299. doi:10.3389/frvir.2020.602299
Hua, Y., Qiu, R., Yao, W. Y., Zhang, Q., and Chen, X. L. (2015). The effect of virtual reality distraction on pain relief during dressing changes in children with chronic wounds on lower limbs. Pain Manag. Nurs. 16 (5), 685–691. doi:10.1016/j.pmn.2015.03.001
Hunter, G. H., David, R. P., Robert, A. R., Raquel, P., Wanda, B., and Walter, J. MJFVR (2021). Virtual reality analgesia for children with large severe burn wounds during burn wound debridement. Front. Virtual Real 1 (0). doi:10.3389/frvir.2020.602299
Jee Hun, J., and Miller, J. (2024). Clinical question: can virtual reality be an effective adjunctive to conventional treatment in patients with chronic lower back pain? J. Okla State Med. Assoc. 117 (3), 88–91. doi:10.1097/ACO.0000000000000859
Jeffs, D., Dorman, D., Brown, S., Files, A., Graves, T., Kirk, E., et al. (2014). Effect of virtual reality on adolescent pain during burn wound care. J. Burn Care Res. 35 (5), 395–408. doi:10.1097/bcr.0000000000000019
Jiali, Z., Mingxiu, L., Junlin, Y., Jinmei, Y., Yan, X., Jie, Y., et al. (2025). Effects of virtual reality with different modalities on upper limb recovery: a systematic review and network meta-analysis on optimizing stroke rehabilitation. Front. Neurol. 16 (0), 1544135. doi:10.3389/fneur.2025.1544135
Jonathan, M., Sam, B., Leila, C., Julie, M., Melanie, H., Kate, M., et al. (2008). The efficacy of an augmented virtual reality system to alleviate pain in children undergoing burns dressing changes: a randomised controlled trial. Burns 34 (6), 803–808. doi:10.1016/j.burns.2007.10.010
Kate, M., Sam, B., Emma, P., and Roy, M. KJSHTI (2008). The emergence of multi-modal distraction as a paediatric pain management tool. Stud. Health Technol. Inf. 132 (0), 287–292.
Kaya, M., and Karaman Özlü, Z. (2022). The effect of virtual reality on pain, anxiety, and fear during burn dressing in children: A randomized controlled study. Burns. 49 (4), 788–796. doi:10.1016/j.burns.2022.06.001
Khadra, C., Ballard, A., Paquin, A., Ballard, D., Cotes - Turpin, C., Hoffman, H. G., Perreault, I., et al. (2020). Effects of a projector-based hybrid virtual reality on pain in young children with burn injuries during hydrotherapy sessions: A within-subject randomized crossover trial. Burns. 46 (7), 1571–1584. doi:10.1016/j.burns.2020.04.006
Kiliç, Ü, and Büyük, E T. (2024). The effect of using virtual reality during burn dressing on pain, anxiety and fear felt in children: a randomized controlled trial. J Burn Care Res. 45 (4), 949–957. doi:10.1093/jbcr/irae005
Kipping, B., Rodger, S., Miller, K., and Kimble, R. M. (2012). Virtual reality for acute pain reduction in adolescents undergoing burn wound care: a prospective randomized controlled trial. Burns. 38 (5), 650–657. doi:10.1016/j.burns.2011.11.010
Kouijzer, M., Kip, H., Bouman, Y. H. A., and Kelders, S. M. (2023). Implementation of virtual reality in healthcare: a scoping review on the implementation process of virtual reality in various healthcare settings. Implement. Sci. Commun. 4 (1), 67. doi:10.1186/s43058-023-00442-2
Lan, X., Tan, Z., Zhou, T., Huang, Z., Huang, Z., Wang, C., et al. (2023). Use of virtual reality in burn rehabilitation: a systematic review and meta-analysis. Arch. Phys. Med. Rehabil. 104 (3), 502–513. doi:10.1016/j.apmr.2022.0.005
Lanier, M., Waddell, T. F., Elson, M., Tamul, D. J., Ivory, J. D., and Przybylski, A. (2019). Virtual reality check: statistical power, reported results, and the validity of research on the psychology of virtual reality and immersive environments. Comput. Hum. Behav. 100, 10070–10078. doi:10.1016/j.chb.2019.06.015
Le May, S., Genest, C., Francoeur, M., Hung, N., Guingo, E., Khadra, C., et al. (2022). Virtual reality mobility for burn patients (VR-MOBILE): a within-subject-controlled trial protocol. Paediatr. and neonatal pain. 4 (4), 192–198. doi:10.1002/pne2.12086
Matthew, J. P., Joanne, E. M., Patrick, M. B., Isabelle, B., Tammy, C. H., Cynthia, D. M., et al. (2021). The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. Int. J. Surg. 88 (0), 105906. doi:10.1016/j.ijsu.2021.105906
Megan, A., Jonathan, L., Jonathan, I. G., Rajan, K. T., Renata, F., Dana, N., et al. (2022). Mobile phone virtual reality game for pediatric home burn dressing pain management: a randomized feasibility clinical trial. Pilot Feasibility Stud. 8 (1), 186. doi:10.1186/s40814-022-01150-9
Mendell, L. M. (2014). Constructing and deconstructing the gate theory of pain. Pain 155 (2), 210–216. doi:10.1016/j.pain.2013.12.010
Merve, K., and Zeynep, KÖJB (2022). The effect of virtual reality on pain, anxiety, and fear during burn dressing in children: a randomized controlled study. 49(4) doi:10.1016/j.burns.2022.06.001
Mott, J., Bucolo, S., Cuttle, L., Mill, J., Hilder, M., Miller, K., et al. (2008). The efficacy of an augmented virtual reality system to alleviate pain in children undergoing burns dressing changes: a randomised controlled trial. Burns. 34(6), 803–808. doi:10.1016/j.burns.2007.10.010
Paul, A. K., Smith, C. M., Rahmatullah, M., Nissapatorn, V., Wilairatana, P., Spetea, M., et al. (2021). Opioid analgesia and opioid-induced adverse effects: a review. Pharm. Basel, Switz. 14 (11), 1091. doi:10.3390/ph14111091
Paula, L., Cleiton Pons, F., and N-Ejbs, F. (2025). A crossover Study of virtual reality exposure for emotional and physiological regulation in mild dementia. Brain Sci. 15 (5), 470. doi:10.3390/brainsci15050470
Pretat, T., Koller, C., and Hügle, T. (2025). Virtual reality as a treatment for chronic musculoskeletal pain syndromes. Jt. Bone Spine 92 (1), 105769. doi:10.1016/j.jbspin.2024.10569
Qiongfang, W., Shun, X., Bing, G., Yan, X., and Ljjbcr, W. (2022). Virtual reality as an adjunctive non-pharmacological therapy to reduce pain in school-aged children with burn wounds. J. Burn Care Res. 44 (4), 832–836. doi:10.1093/jbcr/irac149
Raith, K., and Hochhaus, G. (2004). Drugs used in the treatment of opioid tolerance and physical dependence: a review. Int. J. Clin. Pharmacol. Ther. 42 (4), 191–203. doi:10.5414/cpp42191
Ramyar, F., Arman, P., Soudabeh, H., Mansooreh, S. T., Amirreza, J., Pirouz, S., et al. (2023). Effects of non-pharmacological interventions on pain intensity of children with burns: a systematic review and meta-analysis. Int. Wound J. 20 (7), 2898–2913. doi:10.1111/iwj.14134
Rania, R. A., Ali Osman, S., Mohamed, A. A. G., Osama Ragaa, A., and Olfat Ibrahim, A. J. B. (2021). Virtual reality as a pain distractor during physical rehabilitation in pediatric burns. Burns 48 (2). doi:10.1016/j.burns.2021.04.031
Raz, A. (2005). Attention and hypnosis: neural substrates and genetic associations of two converging processes. Int. J. Clin. Exp. Hypn. 53 (3), 237–258. doi:10.1080/00207140590961295
Sara, M. B., Osama, M. F., Abdulaziz, A. A., Moayad, M. T., Ghalia, Y. B., and Bjjcpd, A. M. (2023). The effect of virtual reality distraction on anxiety level during dental treatment among anxious pediatric patients: a randomized clinical trial. J. Clin. Pediatr. Dent. 47 (4), 63–71. doi:10.22514/jocpd.2023.036
Schmitt, Y. S., Hoffman, H. G., Blough, D. K., Patterson, D. R., Jensen, M. P., Soltani, M., et al. (2010). A randomized, controlled trial of immersive virtual reality analgesia, during physical therapy for pediatric burns. Burns. 37 (1), 61–68. doi:10.1016/j.burns.2010.07.007
Sean, K. P., Tannur, C. O., Judith, C. L., Ruby, C., and James, H. W. CJPRSGO (2023). A comparison between the use of patient-worn virtual reality in wound care and hand surgery: how does virtual reality work? Plast. Reconstr. Surg. Glob. Open 11 (8), e5185. doi:10.1097/gox.0000000000005185
Sofia, J., and Ambardekar, A. (2020). Pediatric burn resuscitation, management, and recovery for the pediatric anesthesiologist. Curr. Opin. Anaesthesiol. 33 (3), 360–367. doi:10.1097/aco.0000000000000859
Tan, B. L., Shi, J., Yang, S., Loh, H., Ng, D., Choo, C., et al. (2022). The use of virtual reality and augmented reality in psychosocial rehabilitation for adults with neurodevelopmental disorders: a systematic review. Front. psychiatry 13, 131055204. doi:10.3389/fpsyt.2022.1055204
Tiffany, P., Cinja, K., and Thomas, H. J. (2024). Virtual reality as a treatment for chronic musculoskeletal pain syndromes. Jt. Bone Spine 92 (1), 105769. doi:10.1016/j.jbspin.2024.105769
Ümmühan, K., and Tbjjbcr, E. (2024). The effect of using virtual reality during burn dressing on pain, anxiety and fear felt in children: a randomized controlled trial. J. Burn Care Res. 45 (4), 949–957. doi:10.1093/jbcr/irae005
van der Heijden, M. J. E., de Jong, A., Rode, H., Martinez, R., and van Dijk, M. (2018). Assessing and addressing the problem of pain and distress during wound care procedures in paediatric patients with burns. Burns 44 (1), 175–182. doi:10.1016/j.burns.2017.07.004
Waked, I., and Eid, M. (2019). Virtual reality: a non-pharmacological complementary strategy facilitating Physical Therapy procedures for adolescent burned patients. Phys. Ther. Rehabilitation 6, 61. doi:10.7243/2055-2386-6-1
Xiang, H., Shen, J., Wheeler, K. K., Patterson, J., Lever, K., Armstrong, M., et al. (2021). Efficacy of smartphone active and passive virtual reality distraction vs standard care on burn pain among pediatric patients: a randomized clinical trial. JAMA Netw. open 4 (6), e2112082. doi:10.1001/jamanetworkopen.2021.12082
Xiaodong, L., Ziming, T., Tao, Z., Zhenjia, H., Zhiyong, H., and Chao, W. (2022). Use of virtual reality in burn rehabilitation: a systematic review and meta-analysis. Arch. Phys. Med. Rehabil. (3), 104. doi:10.1016/j.apmr.2022.08.005
Xiong, J., Hsiang, E.-L., He, Z., Zhan, T., and Wu, S.-T. (2021). Augmented reality and virtual reality displays: emerging technologies and future perspectives. Light Sci. and Appl. 10 (1), 216. doi:10.1038/s41377-021-00658-8
Yuko, S. S., Hunter, G. H., David, K. B., David, R. P., Mark, P. J., and Maryam, S. (2010). A randomized, controlled trial of immersive virtual reality analgesia, during physical therapy for pediatric burns. Burns 37 (1). doi:10.1016/j.burns.2010.07.007
Yun, H., Rong, Q., Wen-Yan, Y., Qin, Z., and Xiao-Li, CJPMN (2015). The effect of virtual reality distraction on pain relief during dressing changes in children with chronic wounds on lower limbs. Pain Manag. Nurs. 16 (5), 685–691. doi:10.1016/j.pmn.2015.03.001
Zatriqi, V., Zatriqi, S., Rrusta, D., Nela, A., Zatriqi, Y., and Bektashi, E. (2024). Epidemiologic and therapeutic approaches to severe burn injury in Kosovo: a comprehensive review. Ann. Burns Fire Disasters 37 (3), 175–179.
Zavarmousavi, M., Eslamdoust-Siahestalkhi, F., Feizkhah, A., Mohammadreza, M., Fazeli Masouleh, S. A., Badrikoohi, M., et al. (2023). Gamification-based virtual reality and post-burn rehabilitation: how promising is that? Bull. Emerg. trauma 11 (2), 106–107. doi:10.30476/beat.2023.97911.1416
Keywords: burn, pediatric, virtual reality, pain, anxiety, meta-analysis
Citation: Yang Z, Yang H, Wang Z and Liu S (2025) Efficacy of virtual reality in pediatric burn patients: a systematic review and meta-analysis. Front. Virtual Real. 6:1651695. doi: 10.3389/frvir.2025.1651695
Received: 04 July 2025; Accepted: 08 August 2025;
Published: 29 August 2025.
Edited by:
Clint Bowers, University of Central Florida, United StatesReviewed by:
Devi Prasad Mohapatra, Jawaharlal Institute of Postgraduate Medical Education and Research (JIPMER), IndiaPengju Chen, The Central Theatre Air Force Hospital of the Chinese People’s Liberation Army, Datong, Shanxi, China
Ummuhan Kilic, Istanbul Sabahattin Zaim University, Türkiye
Copyright © 2025 Yang, Yang, Wang and Liu. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Song Liu, MTgyMDI4NzcxODZAMTYzLmNvbQ==
 Zhengbing Yang1
Zhengbing Yang1 Song Liu
Song Liu