- Sociology, Interface Demography, Vrije Universiteit Brussel, Brussels, Belgium
To fight the COVID-19 epidemic, many countries implemented containment measures that made physical distancing the norm and imposed restrictions on the use of public space. In countries where access to public green spaces (PGSs) was safeguarded, they were expected to partially counterbalance the negative health outcomes of these containment measures, as they offered a unique opportunity to meet others, to avoid isolation, and to move, play and relax at a safe distance. Research on PGS use and its objective association with health during the COVID-19 epidemic is rather limited and is based on quantitative research methodologies. Such methodologies are useful to detect objective associations between PGS use and health or between COVID-19 and PGS use, but fall short in explaining the observed associations. This qualitative research filled this gap by examining how PGS users perceived the health advantages of PGSs and how the use of PGSs changed during the epidemic in the Brussels-Capital Region, Belgium. In total, 23 individual face-to-face in-depth interviews were conducted in various PGSs. We found that while PGSs were initially perceived as a possible threat to health in the first period of the epidemic, they gradually became associated in users' minds with both improved physical and mental health. Although the mechanisms behind this association were also present prior to the epidemic, they became more tangible and more universal. We also found that the use of PGSs changed during the epidemic due to measures and restrictions and due to health risk perceptions. We distinguished five different health risk perception profiles in relation to COVID-19: the denier, the fatalist, the negotiator, the conformer and the worrier. These different health risk perceptions impacted on the use of and behaviour within PGSs. This research confirms the importance of PGSs during an epidemic and may inspire further research, offer pointers to policymakers for developing and implementing strategies related to the use of PGSs during epidemics, and assist them in providing available and accessible PGSs and in designing attractive, more epidemic-proof PGSs.
Introduction
When the World Health Organisation declared COVID-19 an international public health emergency on 30 January 2020 (WHO, 2020), many countries implemented policy measures that reduced personal contact in order to “flatten the curve” of infection. Physical distancing became the norm in public spaces and restrictions on the use of public spaces were imposed in many countries around the globe in order to protect public health. These policy measures resulted in a shrinkage of our physical and social world, thereby causing collateral damage to the physical and mental health of a substantial proportion of the population (Rajkumar, 2020; Tang et al., 2020).
In places where the use of public green spaces (PGSs) was not prohibited, PGSs may indirectly have played an important role in counterbalancing the negative health outcomes of these policy measures, as they offered a unique place to meet others, to avoid isolation and to move, play and relax at a safe distance. Research also suggests that transmission of COVID-19 is lower outdoors than indoors; PGSs may therefore also have directly influenced health outcomes (Leclerc et al., 2020; Qian et al., 2020).
The physical and mental benefits of interaction with nature and the ecosystem services provided by nature are well-established in the literature. Regardless of the current COVID-19 epidemic, a large body of literature highlights the importance of PGSs associated with self-perceived health (Maas et al., 2006; Mitchell and Popham, 2008; Bowler et al., 2010; de Jong et al., 2012; van Dillen et al., 2012), morbidity (Mitchell and Popham, 2008; Pereira et al., 2013; Astell-Burt et al., 2014), and mortality (Gascon et al., 2016). Reviews generally suggest that stronger evidence exists for mental health benefits than for other dimensions of health, such as physical health for example (Lee and Maheswaran, 2011; Gascon et al., 2015).
To explain the association between health and PGSs, several pathways have been put forward. First, PGSs provide opportunities for physical activity, which is associated with reduced physical and mental disorders (Pretty et al., 2005). Second, social interaction is facilitated by the availability of green spaces (Maas et al., 2009). Third, exposure to green spaces promotes psychological restoration (Hartig et al., 1991; Carter and Horwitz, 2014). Last, green areas are associated with a mitigation of environmental hazards such as air pollution, noise pollution and heat (Gómez-Baggethun and Barton, 2013; Lovell and Taylor, 2013).
A large amount of COVID-19-related research covers a wide range of topics originating from different disciplines. Research on PGS use and its association with health during the COVID-19 epidemic is rather limited, however. Derks et al. (2020) showed that the positive association between PGS use and health persisted during the epidemic and that—depending on local restrictions—the use of PGSs increased. Xie et al. (2020) observed in Chengdu (China) that visiting city parks improved physical and mental health and allowed residents to fulfil their social interaction needs. Soga et al. (2020) focused on how proximity to nature contributed to mental health patterns during the COVID-19 pandemic in Tokyo (Japan). They found that people's degree of self-esteem, life satisfaction, and subjective happiness were all positively related to the frequency of green space use around the home but also to green views through windows at home. Pouso et al. (2020) found that in Spain, under severe lockdown, contact with nature from the home (having a green/blue nature view or access to private outdoor spaces such as a garden or a balcony) reduced the likelihood of suffering from symptoms of depression and anxiety. Moreover, the presence of these views and spaces was perceived as positively contributing to mental health.
Venter et al. (2020) found that physical distancing measures brought about a significant increase in the recreational use of urban green space during the partial COVID-19 lockdown (March 2020) in Oslo (Norway), especially on trails within greener and suburban periphery. Geng et al. (2020) analysed the impact of COVID-19 policies on the frequency of park visits at the global, regional and national level. For most countries, they observed a higher number of park visitors from 16 February 2020 than during the pre-epidemic period. Restrictions on social gatherings and free movement and the closure of workplaces and indoor recreational places proved to be correlated with a higher park visit frequency. Measures forcing citizens to stay at home were the most significant correlate of a drop in the number of park visits, followed by restrictions on the use of public transport and personal mobility. Ugolini et al. (2020) explored the ways in which human behaviour, perceptions and attitudes towards urban green spaces had changed due to restrictions imposed by the COVID-19 outbreak in different countries. Countries with stringent restrictions on personal mobility witnessed a huge drop in the use of urban green spaces, especially among women and among people going to urban green spaces for non-essential reasons, such as observing nature, or for reasons which could pose a risk of contagion such as meeting people.
All these studies are based on quantitative research methodologies. These are useful to detect associations between PGS use and health or between COVID-19 and PGS use, but fall short in explaining the observed associations. To our knowledge, qualitative research aiming to reveal insights into the “why” and “how” of the observed associations is still absent. In this paper, we employ a qualitative approach in order to increase our understanding of the perceptions of users about PGSs during the COVID-19 epidemic in the urban setting of the Brussels-Capital Region. The aim of this exploratory research crystallises into two research questions:
1. How do PGS users perceive the relation between PGSs and health during the COVID-19 epidemic?
2. How has the use of PGSs changed during the COVID-19 epidemic and why?
The research results may give decision-makers inspiration and pointers on developing and implementing strategies related to the use of PGSs during epidemics, and assist them in providing available and accessible PGSs and in designing attractive PGSs that are better protected against epidemics (at least of a kind similar to COVID-19). Our study may also inspire future quantitative and qualitative research further developing our findings in other settings and possibly with an even more diverse set of respondents.
The COVID-19 epidemic has evolved into a pandemic. However, since this paper is about local perceptions and does not take an international view, we prefer to consistently use the term “epidemic” instead of “pandemic.”
Methods
Study Setting
The Brussels-Capital Region (BCR), situated in the heart of Belgium, consists of 19 municipalities with an area of 162 km2. The BCR is a rather green region: 54% of its surface is covered with vegetation (2008) and there is 28 m2 of accessible public green and recreational space per capita. These PGSs are unevenly distributed over the 19 municipalities within the BCR, with the densely populated and poorer communities clearly facing a lack of available PGSs. In addition, there are also big differences in the quality of these spaces (Stessens et al., 2017, 2020; Brussels Environment, 2020; Phillips et al., 2021).
Belgium and the Brussels-Capital Region were severely hit by the COVID-19 epidemic. Many continuously changing measures have been taken since the outbreak. Between March 2020 and January 2021, there were two lockdowns. The first lockdown started on 18 March 2020 and was followed by a gradual relaxation of restrictive measures starting in May 2020. The second, less stringent lockdown followed in October 2020 and was still in effect at the time of writing.
During both lockdowns, general measures were implemented consisting of enforced teleworking, closure of non-essential shops, restaurants and pubs and suspension of cultural or sporting events amongst other things. During the first lockdown schools were closed as well, but not during the second lockdown. Outdoor activities were allowed and (most) PGSs were kept open throughout the epidemic. However, many stringent restrictions applying to PGSs were in force during the first lockdown: playgrounds and outdoor fitness equipment were closed, sitting in green spaces was prohibited and visits to PGSs further away were considered to be non-essential movements that were not allowed. Furthermore, there were restrictions regarding the number of people with whom interaction was allowed and a distance of 1.5 m between people needed to be maintained. During the second lockdown, more than one person could not be invited into the house, while up to four people were allowed to meet outside as long as a distance of 1.5 m was maintained. In the BCR, a curfew was introduced between 10 pm and 6 am. Wearing a mask covering both nose and mouth was obligatory in PGSs during the second lockdown only, except for people performing sporting activities (VRT, 2020).
Fieldwork
The study adhered to a symbolic interactionist perspective, viewing social interaction in terms of the meaning that social actors attach to action and things (Bryman, 2004, p. 544). In line with this perspective, we used a qualitative research methodology.
Data collection was accomplished through individual, face-to-face, in-depth interviews with a diverse group of PGS users within the BCR.
Questions were open-ended and the interview guide semi-structured. In total, 23 interviews, including four double interviews, were conducted with 27 persons lasting on average 17 min (ranging from 7 to 30 min). Five respondents did not give permission to record the interview.
The interviews were conducted during the second lockdown, between 23 November and 6 December, in six PGSs that differed in terms of size, naturalness, popularity, infrastructure, and neighbourhood location (see Annexes 1, 2).
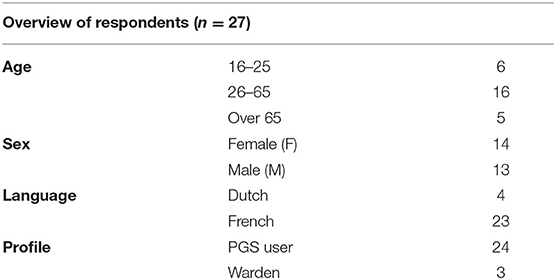
In each of the PGSs, people were randomly selected and asked to participate in a short interview in situ. Interviews were started with an associative question, and then focused concretely on (1) how PGS users perceived the impact of COVID on their PGS use and their experiences, (2) how PGS users perceived the relation between PGS use and health during the COVID-19 epidemic, and (3) recommendations for future epidemics (see Annex 3). Besides PGS users, three wardens who worked in the PGSs were also interviewed. The respondents were diverse in terms of age and gender (see Table 1 for an overview of the respondents that were interviewed). Migration background was not asked for explicitly, but the sample contained a wide diversity of people in terms of nationality or origin.
Analyses
Data were generated through 23 individual, face-to-face, in-depth interviews that were audio-recorded if the respondent approved and then transcribed, analysed and manually coded according to the pre-determined research questions. No specific qualitative data analysis software was used.
The analysis is supplemented with quotations of respondents referring to some main characteristics through an identification code. For example, “22_45_F_Dauw Park” where “22” is the number of the interview, “45” is the age of the respondent, “M/F” the gender of the respondent and “Dauw Park” the place where the interview took place. When “wardens” is mentioned in the code, it refers to a quotation from a warden. In order to increase the readability of the quotations, they were slightly “tidied up” without changing the content or meaning.
Results
Respondents mainly described PGSs during the epidemic as places where they could feel at ease and find relief and tranquillity; as places where they could forget the epidemic and personal problems; as a refuge where they could escape the lockdown and feel free; as restorative places where they could breathe; as recreational places; and as an environment that enabled them to meet others safely.
An important question, however, is whether the epidemic had altered these perceptions, and if so, how and why? First, we will elaborate on the way in which respondents perceived the relation between PGSs and health during the epidemic; secondly we will investigate whether the use of PGSs changed during the epidemic. If PGSs are perceived as beneficial for health, it is important to understand their use and how this changed due to COVID-19.
How Do PGS Users Perceive the Relation Between PGSs and Health During the COVID-19 Epidemic?
In relation to the COVID-19 epidemic in Belgium, it is important to distinguish different periods characterised by different containment measures. In the beginning of the outbreak, during the first wave, in March 2020, a stringent lockdown was in force and knowledge about the virus, its behaviour, transmissions modes and health impacts was still limited. Due to increasing infection rates, many respondents were afraid to go out. Even though it was allowed to leave home and use PGSs and public spaces in general, their use was rather limited. The use of PGSs was not unanimously perceived as beneficial for health at that time; on the contrary it was regarded by many respondents as a possible health risk. Once most respondents started going out again (some time into the first lockdown), PGSs were perceived as having a positive effect on physical health, and even more on mental health.
Physical Health
PGSs were considered by all respondents to have a health-enhancing impact, because they made it possible to exercise, walk and play.
“Yes, since coronavirus I have been in parks more often. Especially with young children. They love to go to the park. I do exercises or sport. The children can then play while I exercise. I don't sit down. I am not on my mobile phone all the time. Sport is good for your health.” (22_45_F_ Dauw Park)
PGSs were deemed very important during the epidemic since many of the COVID-19 measures induced a more sedentary, less active lifestyle. For instance, exercising in PGSs was perceived by many as counterbalancing extra “corona-kilos” or, as one 26-year-old woman stated, as a way to avoid becoming infected and falling ill through a strengthened immune system resulting from increased physical activity. Another respondent aged 26 who increased her use of PGSs through daily training sessions during the epidemic spoke of a direct and observable positive health impact in terms of better physical condition and decreased allergic reactions.
“I am allergic to cats, dogs, everything. And it has decreased, so since coronavirus I no longer take my asthma medication. I also have asthma. Allergy and asthma. I no longer take it. And I do more sports and I feel it (asthma) much less. Before, when I ran for 20 min, I could run but I used the puffer. Now I run for an hour without the puffer. I am so happy.” (9_26_F_ Florist's Gardens)
PGSs were comprehended by many respondents as beneficial because fresh(er) air could be breathed there than at home. The obligation to wear face masks in PGSs was not always complied with as it was perceived as preventing enjoyment of the fresh air or even worsening the quality of the air that was breathed. Some respondents considered PGSs as places for escaping from the heat in their dwellings during heatwaves, thereby indirectly fostering physical health. Compared to other public spaces, large PGSs were, moreover, seen as places where the infection risk was limited since they were in the open air and people could more easily comply with physical distance measures.
“I don't really have words, but I think that it's more a place we can go to without being afraid of getting infected. It is more a free space.” (4_18_F_ Youth park)
PGSs were thus both directly (through exercise, walk, play, losing extra weight put on during the lockdown) and indirectly (through strengthening the immune system, mitigation of environmental hazards and limited infection risk) perceived by respondents as contributing to physical health.
Mental Health
The benefits of PGSs for mental health were emphasised even more strongly. During the epidemic, there were many restrictions on meeting people and inviting them into the home. In this context, PGSs offered unique opportunities to meet and interact with people as long as a face mask was worn and physical distancing measures were complied with. PGSs were actively used by most respondents as places to meet family, friends and acquaintances, to meet new people or to simply be surrounded by people or stay connected to society. A 33-year-old woman who had recently become a mother said in this respect:
“It is also a meeting point. It is not allowed to invite anyone to your home but you sometimes want to. For example, my mom came and I have a niece who lives nearby and ok, we met in the park because we know, we are outside, we are wearing our masks, so it is a safe meeting point.“ (14_33_F_Florist's Gardens)
A man aged 70 who was taking a morning walk in the park explained that even without making contact with other park visitors, the very fact that he was surrounded by others enhanced his mental wellbeing.
“People came with their little ones. So, we remained without making contact with anyone. But we were still surrounded by people. So good. Mentally it definitely did me good.” (7_70_M_ Jean Sobieski Park)
A woman aged 26 years who had recently finished higher education and was now looking for a job came to the park to exercise but also to meet other people with whom she interacted regularly in this way.
“I'm not very into social media. I don't have it so I don't know how I could meet people elsewhere apart from school or work. I've finished school. And work, well, I'm looking for a job, so I don't have one right now.” (9_26_F_Florist's Gardens)
The other side of the coin was that social interactions were perceived as different, less spontaneous and sometimes also less satisfactory. A 33-year-old woman considered the epidemic to have a negative impact on the spontaneity of interactions with others:
“When I used to run into people, we could be together but now, I always have to pay attention. You have to cheque with others, do they want to talk, do they not want to talk? So it's less spontaneous too. You have to think so much more about what is allowed and what is not allowed.” (1_33_F_Youth Park)
Another young woman felt that the epidemic limited her interactions with others and that the choice between desired behaviour and safe behaviour was constantly being weighed up.
“For example, there was a woman I met in the park. I see her three times a week. Not by chance, well, she takes her dog out so we meet. And the poor thing, she is alone and in fact, 1 day she was crying and I wanted to take her in my arms and I saw that she was afraid yet wanted to be hugged at the same time. Finally, we decided not to hug. She was divorcing and that was frustrating. I wanted to hug her so much. And I felt she wanted it too. There was a sudden love and we couldn't hug, that was very sad.” (9_26_F_Florist's Gardens)
While most respondents perceived the opportunities that PGSs offered for social contact as beneficial for their mental wellbeing, conversely some respondents appreciated the tranquillity and the opportunity to be alone in PGSs. The tranquillity of PGSs was contrasted with other public places that could not provide this much-needed quality.
“I look a little bit for the tranquillity and also for the peace I don't have in the city centre. Here, we are a little bit disconnected from the real world of the city.” (10_61_F_ Florist's Gardens)
As the schools were closed during the first lockdown, respondents with children at home especially experienced the need to be alone from time to time. A mother of two young children said:
“It is because, well, we weren't going outside anymore. We were confined to the house and I also needed to exercise and to have this relaxation. We had the children at home all day, every day. We were stressed out, so I needed that little bubble of fresh air for myself, to walk around and so on.” (5_30_F_ Youth park)
Many respondents ended up being locked down with large numbers of people in quite small apartments, limited privacy and no private outdoor space. However, those with more spacious housing, who were not used to constantly sharing their living or working space with others, could also find relief in the tranquillity that PGSs offered. Intensive sharing of limited space was experienced as causing bad mental health and interpersonal conflicts. The possibility of going to a PGS was perceived as creating mental and physical space, as the following respondent expresses.
“At home we are stuck. We are trapped. We cannot move, we cannot do activities. We are heavy, we have heaviness. And, as my wife says, that is going to have an impact on your mind. Going to the park clears everything up. The negative vibes, the negative thoughts. Parks are very important for this… I think that it is important that there are parks that allow you to go outside. Even if there cannot be physical and human contact, you can externalise what is within you. So that's very important. That's an exit. Parks have an impact on the morale. Also for the children. It's like an exit. Too many people at the same time (in the house) causes tensions and arguments that you don't have room for. Parks really give the opportunity to externalise and to survive. It is very important that the parks remain open, even when the playgrounds are closed. It gives us the opportunity to walk, to talk, to discuss things, even if you have to keep your distance. It's a vital thing.” (23_48_M_ Dauw Park)
PGSs were also often associated with freedom, which was deemed important at a time when people were feeling imprisoned in their own homes.
“We come here to take a little breath. How can I explain that? It's like you're locked up, and when I come to the park, I am free.” (11_56_M_ Florist's Gardens)
Importantly, as many places and events were no longer in reach, visiting PGSs was more valued as it was one of the few activities/excursions that was allowed.
The naturalness of PGSs too was perceived as positively impacting mental wellbeing. Seeing, feeling, breathing and hearing nature evoked in many respondents a feeling of happiness, belonging to and connexion with nature. The fact that nature constantly changes turned natural PGSs into places where there was always something new and different and that were therefore continuously interesting.
Two respondents said that they actively searched for natural PGSs.
“Yes, it (PGS) also has a positive impact on your mental health because it is natural. The trees, even more when the flowers are there… During the summer we used to go to a park in Ukkel (a municipality in southern Brussels), it is more like a forest… If there were more small parks in the city centre with more greenery, more trees, more nature, it wouldn't have been necessary to go there (to the bigger, more natural park in Ukkel). But we went there since here there was almost nothing.” (22_45_F_Dauw Park)
“Since coronavirus I prefer going to a forest instead of to a park because it is more natural. Before, the park was sufficient but now, the forest has really helped me. I have always wanted to go there more often but now was the moment to actually do it.” (1_33_F_Youth Park)
Another respondent underlined the stress-reducing quality of PGSs, describing them as inherently relaxing since they absorbed all kinds of stress and tensions.
“I think the park absorbs all of that (tensions). The park will absorb people's negative energy so much that it enables them to feel good. The parks are like islands, they will absorb. But this is invisible to us.” (23_48_M_Dauw Park)
Some respondents even stated that COVID-19 seemed less “present” in PGSs and that going to PGSs helped them to forget about the epidemic and the problems it generated, as they could disconnect from the harsh reality. Two women aged 26 and 45 put it like this:
“Here I can disconnect from the city. We forget. Ah, you can write, the park makes us forget coronavirus.” (9_26_F_ Florist's Gardens)
“The park is a good place to spend some time. You can breathe, calm down, be in nature. Here I can forget all my problems. It's a break from my problems. It's like alcohol. When I come here, I forget all of my problems.” (22_45_F_Dauw Park)
However, some respondents were less positive, stating that the constant focus on wearing face masks and physical distancing prevented them from being relaxed.
Nonetheless, most respondents perceived PGSs as beneficial for their health during the epidemic. It is therefore important to study and understand their use and to investigate how and why it changed.
How Has the Use of PGSs Changed During the COVID-19 Epidemic and Why?
In the second part of this paper, we will focus on how the use of PGSs changed in the context of the COVID-19 epidemic. We found that changes in PGS use during the epidemic were a result of both the imposed measures and restrictions and perceptions of the health risk associated with COVID-19.
Measures and Restrictions
Almost all respondents indicated that lockdown measures had impacted hugely on their PGS use. This impact was far from static: it fluctuated depending on the changing severity of restrictions during the epidemic. Different kinds of measures and restrictions should be distinguished.
General measures such as closure schools, teleworking, closure of non-essential shops, closure of restaurants and pubs, and suspension of cultural or sporting events increased the need for PGSs and resulted in more intensive use for almost all respondents. An 18-year-old woman stated it as follows:
“Especially during the lockdown it (park use) has intensified more. Outside the lockdown or before coronavirus, I was less likely to go there on purpose. Now that we don't have too much opportunity to go out and everything is closed, I go to the park more often.” (4_18_F_ Youth park)
A 56-year-old man who was on vacation explained that there were few options other than visiting a park, apart from staying at home.
“Yes, I come more often than before. That is good. With coronavirus it is good that we can come here to get some fresh air and clear our heads a bit. If I'm not going to work, and have to stay at home, I'd rather go to the park. I'm on holiday right now, for 2 weeks. I work in fruit and vegetables. I am obliged to work. Even with coronavirus I am obliged to work. So during these 2 weeks I have nowhere else to go, so I prefer to come here.” (11_56_M_ Florist's Gardens)
A young mother, whose main activities predominantly took place in the city in the pre-epidemic period, also expressed a higher need for PGSs.
“Yes, it has become more important to me. Because, before you always had something to do. You could go to someone's house or go into town, or go shopping or have brunch. Now everything is closed and you are stuck inside, so what can you do? You have to be able to walk a bit. There is clearly more need.” (14_33_F_ Florist's Gardens)
While in the past, some respondents took PGSs for granted and/or did not actively use them, they had now become places that were increasingly appreciated and used. A young mother who had started to look actively for new PGSs to go to with her children during the summer holidays stated:
“Listen, to tell the truth, yes it has become more important. Because now we enjoy it. Before, they were right in front of us, but we didn't particularly feel like going there. We passed through them, but without looking. But coronavirus has changed my perception of green spaces. Now I think that they are really important in big cities like here in Brussels. Having a lot of green spaces is important I think. I believe in the need for green spaces in the city.” (16_33_F_ Ninoofsepoort Park)
General measures not only resulted in an increased need for, appreciation and use of PGSs, it also changed the way in which they were used. For instance, working from home or attending school classes at home made it possible to use PGSs at different times than before.
Besides the time of use, behaviour within PGSs changed as well. For instance, the closure of indoor sport facilities stimulated outdoor sport, while the prohibition on inviting people into the home stimulated people to meet friends in PGSs. However, as these general measures resulted in increased PGS use, small PGSs became overcrowded, reducing their appeal for some respondents who were looking for tranquillity.
Other restrictions had a more direct negative impact on the availability and accessibility of PGSs. During the first lockdown, people were not allowed to make non-essential journeys and were forced to use the PGSs available in their neighbourhoods. In addition, some PGSs were closed, which was another factor in decreased use. Accessibility was also hindered for early and late PGS users due to the introduction of a curfew in the second lockdown. In neighbourhoods where PGSs were scarce, they became inaccessible after overcrowding compromised compliance with physical distance measures and led to closures by the police. One of the wardens in a small PGS situated in a neighbourhood with few PGSs explained:
“There have been days when there were so many people in the park that the police came and everyone had to leave. They were sent back home. Suddenly the park was completely empty.” (17_32_M_Bonneviepark_warden)
PGS-specific restrictions such as the closure of playgrounds and fitness equipment impacted negatively on the attractiveness of PGSs especially for specific groups of potential users (parents with children and people wanting to exercise).
During the first lockdown, there was also a prohibition on sitting in PGSs; benches were sealed off and people sitting on the grass were asked to leave. Such restrictions impacted negatively on the attractiveness of PGSs, their use and, possibly, the health of their potential users as it prevented them from going to PGSs or shortened their walks or time spent there considerably. This was especially the case for parents with young children and people who were unfit.
A mother explained that the experience of the park was different since playgrounds were closed and sitting was not allowed:
“They allowed us to go to the parks, that is a positive thing. But, what was a little complicated was that the children couldn't play in the playgrounds. It was also a bit sad, the park was a synonym for sadness due to the fact that they had closed down the playgrounds and due to the fact that we had to keep moving. We were not allowed to sit although the weather was nice.” (16_33_F_ Ninoofsepoort Park)
Another mother also criticised the ban on sitting in PGSs. Since she had access to a private garden, she preferred to stay in the garden and used the PGSs less frequently than before.
“We have stayed a lot in our garden and we have been very little in the park. Also because you were not allowed to sit. We went to the park a few times and then, we just wanted to sit on the grass and that was not allowed. I found that very annoying. I did use the park much more in the evening. I did that when my daughter was not with me. Then, I met with others and we always went to the park.” (1_33_F_Youth Park)
A woman aged 45 also explained that not being allowed to sit in the PGS prevented her from using it.
“No, I didn't go to the parks during the first lockdown. It was not closed but it was forbidden to sit. I went there a few times but I was there all alone. It was difficult to go when you cannot sit down.” (22_45_F_ Dauw Park)
The basic restrictions applying to public space—physical distancing, the face mask obligation (only during the second lockdown) and the prohibition on gathering together—led to behavioural changes within PGSs as well. For instance, the face mask obligation pushed some respondents to use PGSs for different activities from previously. Whereas, before the epidemic they went to the PGS to walk, they now went there to jog or cycle since the face mask obligation did not apply to people doing sports.
Health Risk Perception Relating to COVID-19
Changes in PGS use not only resulted from the COVID-19 measures that were imposed, but also from health risk perceptions relating to COVID-19.
Although there were no direct questions about the risk perception of respondents, this was addressed in almost every interview as many questions in the interview guide gave rise to reflections about risk perceptions. More specifically, the following questions resulted in such information: “Since coronavirus, have there been factors that have a negative impact on your experiences in the park, or things that you experience differently compared to the pre-coronavirus period? (e.g., high concentration of people, face mask behaviour, people who cough, intimacy between people, etc.)” and “Do you feel any tension or irritation, or do you experience or observe conflicts in the park due to Covid?”
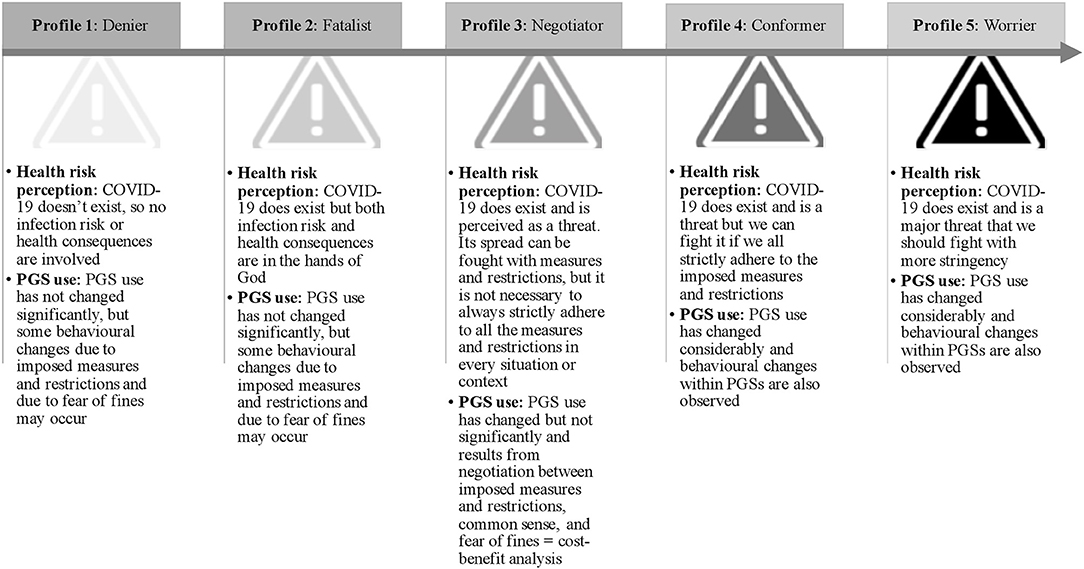
Behaviour in risky situations is heavily influenced by risk perceptions. If a threat is not perceived or recognised as such, people will not adapt their behaviour in a potentially dangerous situation such as the current epidemic. Our data about risk perceptions of park use during COVID-19 led to the identification of five potential profiles of PGS users holding different health risk perceptions in relation to COVID-19 that resulted in different PGS use patterns and behaviours within PGSs. The five profiles can be ordered on a continuum of health risk perception ranging from a very low (profile 1) to a very high health risk perception (profile 5). For an overview of these five profiles, see Figure 1.
Deniers (profile 1) denied the existence of COVID-19. According to this profile, COVID-19 was a fiction created by governments in order to frighten the population and to impose rules on them, thereby decreasing liberties and increasing their power and control. A warden acknowledged the existence of deniers in the PGS he supervised:
“There is a minority that does not believe coronavirus exists. There is also a minority that believes it exists but that there is no need to be careful. I've already had people saying that coronavirus doesn't exist. They say it was invented to scare us and to enforce laws. There are a lot of people who said that and others who said it exists and that you have to be careful and take action.” (21_23_M_ Dauw Park_warden)
For this profile COVID-19 was not considered as a real threat and there was believed to be no infection risk or health risk involved. PGS use or behaviour within PGSs was altered in a limited way and mainly because of the restrictions and the fines handed out when rules were broken, not because of the epidemic as such.
Fatalists (profile 2) acknowledged that COVID-19 existed but did not believe that people had the power to affect its spread or the health consequences resulting from infection. It was believed that both infection and health consequences were in the hands of God. This conviction resulted in limited confidence in the measures implemented to fight the virus and slightly changed behaviour in order to avoid fines. A 45-year-old man with this profile explained that when the warden was watching, he wore his face mask, but that he stopped wearing his mask once the warden left. He justified this behaviour by stating that he did not believe that the mask was going to protect him against a possible infection, nor prevent others from getting infected.
Negotiators (profile 3), making up the majority of the respondents, were convinced that COVID-19 existed, that it was a threat and that it could be fought with the introduced measures. However, these measures were not always perceived as the “right” measures. Based on a cost-benefit analysis, negotiators decided whether and to what extent they would comply with the measures and adapt their behaviour in PGSs accordingly. Their behaviour thus resulted from a trade-off between the perceived immediate threat that COVID-19 posed for health—both personal health and public health—and the perceived negative health impact of specific measures put in place to fight the virus. A couple with a young child who did not wear a face mask explained:
“We are not afraid either. I am a doctor and I am very sure they (masks) are a mistake. Wearing a mask is wrong. It is even more dangerous since you re-inhale your own exhalation. That can cause infections. You also move your mask throughout the day, so there are particles that will get into the mask and that you will inhale. There are people who have pneumonia or fungus that develops because of the mask. It is not good for the immune system. It is very dangerous to wear it. I only wear a veil when I go to the store and in busy places, but here it is fairly quiet. In my neighbourhood there are many people that do not wear them. When people come and ask us to put on a mask, we will. We don't want to create tension. We don't wear masks. We breathe the fresh air. It's not what is going to kill us. On the contrary, the air will allow us to feel good. That is a very important thing.” (23_39_F_Dauw Park)
During an interview, a passer-by interrupted and started talking to the respondent, stating that there was indeed no reason to wear a face mask.
“You do well, madam, well done (passer-by starts to applaud). You take off the mask to breathe, that's good. Did you know that you have 25% less oxygen in your brain if you keep it on all the time? And be careful, all the damage, all the cells in the brain that haven't received oxygen, they die, and it's irreversible. We no longer know how to cure them or regenerate them. It is here in nature, there are a million microbes and viruses in the air. For millions of years we have lived with them, they exaggerate, the government does not care, they want to achieve vaccination with vaccines that are bad for the health, but they don't say it. Because viruses, we're never going to eliminate them. Every year they create vaccines, for the flu. Is the flu gone every year? No, because viruses transmute every year. They change, all the time, all the time. They never know how to do a vaccine, those are all lies. Besides, it's all big pharma money, because they get richer and richer because the more people take vaccines, the richer they get.” (passer-by at Youth Park)
One of the respondents, a sports teacher present in the PGS with her adolescent pupils who were playing in the playground and thus breaching the social distancing measures and the restriction on gatherings to a maximum of four people outdoors, observed:
“I saw you coming from that direction and because you came straight towards me, I thought, that is a police officer in plain-clothes. I said to myself, ayayay, I thought, she is going to tell me off. Recently, I was at the big market and a police officer there also told me off and said that my students could be in groups of up to four, at a distance of 1.5 m. I said, ok, no problem, but they sit together in class every day, next to each other. So when I saw you coming, I thought you were going to question me about the fact that my students are all playing together. I thought that's a police officer in plain clothes who's going to question me. I stayed calm (laughs). And when you told me, it's for an interview for the VUB, I said, phew.” (16_33_F_ Ninoofsepoort Park)
Negotiators would thus only wear a face mask in PGSs when it is crowded or when they go past other people; they would actively look for PGSs where they can easily neglect the restrictions and avoid police checks and fines.
Conformers (profile 4) were convinced that COVID-19 existed, that it was a threat, and that it could be fought if we strictly adhered to the imposed measures and restrictions together. They had faith in the measures and restrictions and saw them as appropriate in order to protect everyone in society. Their risk perception resulted in modified PGS use and behavioural changes within PGSs, since they strictly followed the imposed measures and restrictions and avoided people who did not do so.
The worriers (profile 5) were convinced that COVID-19 existed, that it was a major threat, and that it could be fought if we all complied with more stringent measures. This health risk perception also resulted in changed PGS use and behavioural changes within PGSs.
Clearly, as respondents mentioned, there was an interplay between the measures and restrictions and risk perception. Stringent measures increased the perception of the severity of the virus threat. For instance, closing the schools during the first lockdown increased the perception of the virus as a serious threat and resulted in people avoiding going outside, especially with children.
Profiles 1 and 2 tended to be rather static, while the other profiles were likely to change more frequently due to shifts in risk perception induced by new knowledge, experiences and beliefs.
As profiles 4 and 5, and to a limited extent profile 3, adapted their PGS use during the epidemic, we focused in more depth on the how and why of these changes. Again, it is necessary to distinguish different periods during the epidemic. We observed changes in the frequency of use, in preferences for specific PGSs, in the time of use, in the companions with whom PGSs were visited and in behaviour within the PGSs.
During the first lockdown, especially at the beginning, many respondents stated that they did not visit PGSs since they were afraid to leave their home. Health risk perceptions were very high at this time (profile 5), in relation not only to people's own health, but also to the health of their children and other people perceived as vulnerable. Over time, health risk perceptions generally decreased, and people started to use PGSs again. A young woman said:
“In the beginning people didn't take any risks, but from June to July the parks were full. Also because travel wasn't allowed and because there were no other activities to do. That's why people started going to the park.” (13_17_F_ Jean Sobieski Park)
A mother of three living in a small home acknowledged:
“During the first lockdown, I didn't go out. Because they asked us not to go out unless it was necessary. So we kind of complied with the rules of the government. But from July onwards, I started to come out because it simply wasn't possible to be locked up for such a long time. Especially because I live in a duplex. I don't have a garden, I don't have a balcony, I only have a small courtyard where the children could get a little air. I have three children. So, it was not easy. So in July and August, I went to the parks.” (16_33_F_ Ninoofsepoort Park)
Negotiators (profile 3) on the other hand were—based on a cost-benefit analysis of the restrictions during the first lockdown—pushed to start using PGSs at an early stage of the lockdown since they preferred to go outside rather than staying permanently at home and since there was nothing else to do and nowhere else to go to.
Preferences for specific PGSs changed as well. For people without a car who avoided public transport, PGS usage became more local. A 55-year-old woman who had been ill for a long time (not COVID-19-related) said:
“I am now less inclined to take the metro or other public transport to go somewhere else. I used to do that, but now I prefer to stay in my own neighbourhood and I am starting to really get to know it after so long.” (8_55_F_ Jean Sobieski Park)
Quite a few respondents also deliberately avoided PGSs where people did not wear face masks and PGSs that were congested. A woman aged 61 who was still recovering from a serious disease (not COVID-19 related) said that she actively avoided other people.
“Yes, I actively avoid people.” (10_61_F_ Florist's Gardens)
A 30-year-old mother admitted that she avoided congested places within PGSs such as playgrounds.
Well, yes, I avoid crowded spaces, let's say. When I see that the playground is crowded, I tend to go away, to go for a walk rather than to go with the little one into small crowded spaces.” (5_30_F_ Youth Park)
Congested PGSs were avoided for two reasons. Profiles 4 and 5 avoided congested PGSs for safety reasons, as respondents experienced difficulties complying with physical distancing measures in such places.
“I avoid small parks to ensure that there is enough space between users.” (6_65_M_ Jean Sobieski Park)
Profile 3, on the other hand avoided congested PGSs because respondents in this category were looking for less crowded spaces with little social control so that they could take their face mask off.
“I am not sure whether I should tell you but since this park is a bit hidden, you don't get many police coming here. Haha (laughs). So I can feel more comfortable about taking off my mask and so on. I think in the park, I came every day and the police have only come once in the last month and a half. Before that I was on a trip. But, at Laken Park (another park) near the Atomium, I have to be careful because there is the police station and they patrol more often. You even have to keep more of a distance when talking with people, and so on. Here, the advantage is that there is less surveillance. We have the impression of being hidden. And I feel that people taking off their masks here. There are few people who are stressed about it.” (9_26_F_ Florist's Gardens)
Health risk perceptions also affected the times when PGSs were used. Respondents with profiles 4 and 5, and to a lesser extend profile 3, seemed to avoid peak hours, both in PGSs and on public transport to reach PGSs. A 30-year-old mother claimed in this respect:
“I admit that I avoid rush hours. Let's say, after meals and just before meals too.” (5_30_F_ Youth Park)
PGSs were—especially during the first lockdown in spring—often frequented in the evening. A mother explained that she was too afraid at the time to leave her apartment with her children or to go alone to a PGS when there were many people.
“Yes, I went out but not with my children. During the first lockdown I did not go out during the day, but in the evening I went out for two, 3 h to walk and jog. So, I came out in the evening to avoid going near people. Because, yes, back then, there was fear. The climate of fear was well-established, anchored in our heads.” (16_33_F_ Ninoofsepoort Park)
Our data also indicated behavioural changes within PGSs in terms of the activities performed and the people with whom they were performed. Some respondents belonging to profile 3 mentioned, for instance, that they had started to jog in the PGSs as doing sport was the only way to escape from the face mask obligation. Concerning social contact in PGSs, profiles 3 and 4 stated that they used PGSs in order to meet family and friends, which for some of them had not been the case before the epidemic. A 33-year-old woman explained that since the imposition of general measures to restrict social contact, she preferred to go to PGSs with friends during the weekend as she was lacking social contacts during the week.
“Because you have so few social contacts nowadays. At the weekend, I often ask whether my friends want to join me to go to the forest, in a small group of four people. So I do this more often with friends than before. Before I would have said that I have been seeing people all week, but now I prefer to do that with others.” (1_33_F_Youth Park)
A 56-year-old man acknowledged that due to the general measures, he now came to the PGS to meet his family, whereas in the past he would have met them elsewhere.
“When coronavirus started, when we were really completely confined to our house (first lockdown), I called my son. He has a young child who is now 1 year old. I met him here with his son. I was sitting here and he was there. I could look at his son. We met here with his wife. We had no choice. We were not allowed to go to a pub, they were not allowed to come to my house. That was because of the fear. I also fear the disease. But without coronavirus it is different, then your friends can come to you, you can go with your family. I've often invited him here. We usually meet there, at the chairs. They are mobile and so we can keep our distance (chairs on rails, which can be moved). That way we can keep our distance and talk a bit. And his wife is a bit further away and then we can have a chat. That gives me the opportunity to see my grandchild and my son too.” (11_56_M_ Florist's Gardens)
The extent to which measures were complied with by different profiles not only affected their own PGS use and behaviour, but also that of other potential PGS users. For instance, non-compliance with the measures, such as not wearing face masks, created fear amongst other users resulting in altered PGS use or even in avoidance of (specific) PGSs. Two mothers waiting for their child to come out of school perceived the PGSs as a dangerous place since others did not comply with the measures, which prevented them from using them.
“We are just waiting here for our children to come out of school, but we never come to this park because nobody follows the rules here. It's a dangerous park.” (18_35_F_ Bonneviepark)
A warden observed the same tendency in this PGS; people stopped using the PGS due to non-compliance with the measures by other users.
“There are those who don't come anymore and who prefer to stay at home or hang out of their windows. Because here in the park, the people wear their masks, but when the police or when we are not there for a while, they revert to their old habits and then there are people who take off their masks.” (17_32_M_ Bonneviepark_warden)
The interplay between the restrictions and health risk perceptions and the differences in this respect clearly led to conflicts and tensions within PGSs resulting in altered PGS use (whether a PGS was used or not or how it was used). Conflicts mainly arose between PGS users and the police or wardens of PGSs due to breaches of measures such as the curfew, the face mask obligation or sealed playgrounds or outdoor fitness equipment. Tensions between users arose when physical distancing, the face mask obligation or the prohibition on gathering together were not observed, which affected people's behaviour in PGSs. In these circumstances, some respondents changed their behaviour by keeping more distance, by trying to avoid going past people, by changing their route or by simply leaving the PGS. A 55-year-old woman said that the presence of people not wearing a face mask led to her keeping her distance from them.
“With coronavirus it is strongly recommended that people wear a mask and some don't follow this recommendation. Sometimes I tell them to wear a mask. It's so infuriating and I find it so irresponsible because you wear that mask in the first place to protect others and in the second place to protect yourself. When people are not wearing their masks, then I keep much more distance when I have to go past them or I try to avoid going past them. I really keep my distance in order to make it clear to them.” (8_55_F_ Jean Sobieski Park)
Another woman explained that she avoided a congested PGS in which social distancing was impossible.
“I avoided this park because during the summer, it was overcrowded and there was no social distancing at all. That was scary because you did not necessarily know these people and I was not in my neighbourhood, so, they are people that I don't know and that makes you afraid when you don't know people. No social distancing, that is frightening.” (6_33_F_ Ninoofsepoort Park)
A young woman of 17 years acknowledged that she and her friend actively avoided people who did not comply with the restrictions on gatherings to a maximum of four people.
“When we see a group, we avoid it, but in general we know that where we are going it is not NECESSARILY VERY BUSY.” (13_17_F_ SOBIESKIPARK)
Discussion
Discussion of Results
The aim of this research was two-fold. First, we studied how PGS users perceived the relation between PGSs and health during the COVID-19 epidemic. While PGSs were initially perceived as a potential threat to health in the first period of the epidemic, they gradually became associated with improved physical and mental health. This gradual shift from negative to positive perceived associations between PGSs and health is an important finding, since it shows that the perception of PGSs as having a positive impact on health is context-dependent and not automatic. In addition, when PGSs are perceived as a potential threat for health they may not be used regardless of the health advantages that their use may offer.
In line with the existing body of research (Hartig et al., 1991; Pretty et al., 2005; Maas et al., 2009; Gómez-Baggethun and Barton, 2013; Lovell and Taylor, 2013; Carter and Horwitz, 2014; Nieuwenhuijsen et al., 2017), our study identified several mechanisms as pathways linking PGS use and health: opportunities for physical activity, facilitated social interaction, psychological restoration and mitigation of environmental hazards. However, specific COVID-19-related elements seem to have altered some of these pathways. For instance, respondents mentioned that social interactions had changed as they had become less spontaneous and less satisfactory due to the measures. Moreover, the constant focus on wearing face masks and on physical distancing was experienced as a barrier to feeling relaxed. Specific behaviours within PGSs were also considered to induce negative health impacts during the epidemic. Especially when people did not adhere to or only partially adhered to the measures in force, an increased infection risk, with associated implications for physical health and mental well-being.
On the other hand, the mechanisms behind the association between PGS use and health seemed more tangible and more universal within the context of the epidemic. Measures limiting social contact with and visits to family and friends at home amplified the positive perception of PGSs, which offered a safe place to meet others and to enhance social cohesion. The opportunity to meet others in PGSs had always been important for specific groups of people—e.g., for people with cramped living conditions, for people with limited financial means, for seniors living alone—but now seemed to have extended to other groups of people as well. Using PGSs may thus have partially counterbalanced the negative health outcomes resulting from abrupt changes in lifestyle and living conditions due to measures and restrictions imposed to fight the virus.
From a health perspective it is therefore important for people to continue or start using PGSs, especially during epidemics such as the COVID-19 epidemic (as long as the measures and restrictions are complied with).
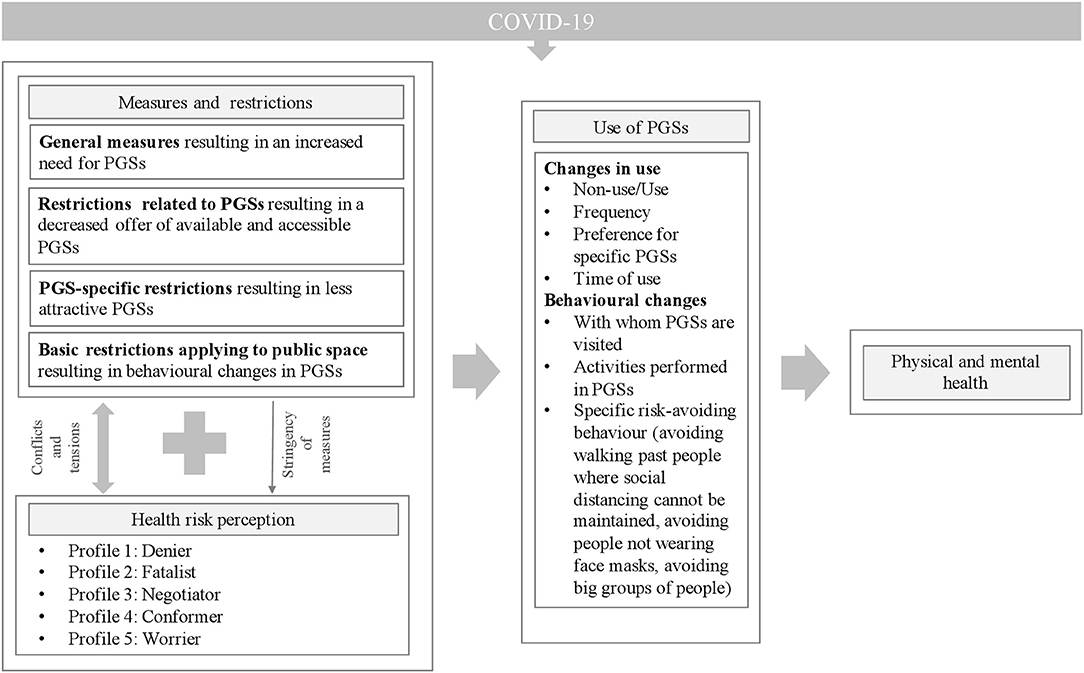
This brings us to the second aim of this research, namely, to investigate how and why PGS use changed during the epidemic. The observed changes in the use of PGSs during the epidemic were influenced both by the government measures and restrictions and by the health risk perceptions of COVID-19, as schematically presented in Figure 2.
In line with earlier research (Geng et al., 2020; Ugolini et al., 2020; Venter et al., 2020), we observed that different kinds of measures and restrictions affected the need for and the availability/accessibility of PGSs, leading to changes in the way PGSs were used. Our focus on the impact of measures and restrictions on the attractiveness of PGSs brought new insights. We found that the way in which PGS use changed during the epidemic depended on the health risk perception relating to COVID-19. Five different profiles with different health risk perceptions were identified. These profiles were not static but evolved as health risk perceptions changed due to shifts in knowledge, experiences and beliefs with regard to the virus. “The denier” and “the fatalist” seemed more static profiles; their PGS use did not change, and they only adapted their PGS behaviour partially, mainly to avoid potential fines. “The negotiator,” “the conformer,” and “the worrier” profiles changed their PGS use: their frequency of use, their preferences for specific PGSs and the time of their PGS use. These profiles clearly demonstrated behavioural changes within PGSs relating to the people with whom they visited PGSs, the activities they performed in PGSs and their specific risk-avoiding behaviour (avoiding walking past people where social distancing could not be maintained, avoiding people not wearing face masks, avoiding big groups of people). The extent to which measures were complied with by different profiles had an impact on their own PGS use and behaviour within PGSs, but also on that of other potential PGS users. In addition, the interplay between the restrictions and health risk perceptions and differences in this respect resulted in conflicts and tensions within PGSs. This triggered changes in PGS use and negatively affected the perceived health improving characteristics of PGSs.
Limitations and Further Research
Our research had several shortcomings. We conducted interviews with PGS users only. First, it would have been interesting to generate insights into both the perception of the relation between PGSs and health and the barriers to PGS use during the epidemic encountered by those who did not use PGSs (anymore). Second, the five profiles with different health risk perceptions relating to COVID-19 were developed in an inductive way and should therefore be seen as exploratory. They cannot be generalised, since they resulted from a limited number of interviews. Third, as the number of interviews was rather limited and the interviews were relatively short, we lacked more in-depth information about both profile 1 and profile 2 discussed in this paper. We did interview respondents with both profiles, but these were the respondents who did not agree to the interview being recorded, so that data and quotations generated from these interviews were rather limited. Further research might thus be interesting to validate and fine-tune these profiles, since a sharp image of the different health risk perception profiles is key to developing effective communication strategies in order to inform and sensitise different groups within society. Further research could also quantify the profiles to generate insights about their prevalence in order to make decisions about the importance of profile-specific communication strategies.
Furthermore, future research might also shed light on how and to what degree different sociodemographic groups align with the proposed typology. One might expect that people who perceive themselves as vulnerable will have higher health risk perceptions and will therefore reduce their PGS use or use them differently. Although we considered this as very relevant, the design of this research was too limited to be able to reach firm conclusions about this. For this aim quantitative research methods might be more suitable.
Our research illustrated that the need for PGSs during the COVID-19 epidemic increased. This need was, however, not exclusively attributable to the true nature of PGSs but could also be explained by the unusual situation in which visiting PGSs was one of the few activities that were allowed. This could raise questions about the durability of changes in the use of PGSs. It might in this sense be interesting to study the long-term effects of the epidemic on PGS use both qualitatively and quantitatively.
Policy Implications
The likelihood of new epidemic/pandemic outbreaks is on the rise and as Chin et al. (2020) state, they may be an emerging element of the “Anthropocene.” Therefore, it is important not only to increase our understanding of the relation and interactions between health and the public living environment during epidemics, but also to stimulate in an active, structural, proactive and inclusive way the potential environmental health benefits they may offer.
More concretely, in order for PGSs to maximise their health-improving qualities during COVID-19-like epidemics in an urban living environment, their (safe) use should be stimulated and facilitated. First and foremost, PGSs need to be both available and accessible to all, and especially to vulnerable population groups.
Many imposed restrictions and especially the restriction regarding non-essential movements during the first lockdown, forced people to reconnect with their immediate living environment, their neighbourhoods. However, in the BCR there are still many neighbourhoods where the availability and accessibility of PGSs is limited (Van de Voorde, 2017). These are generally the neighbourhoods in which the most vulnerable population groups live, often in precarious living conditions (limited space per person, poor insulation, no separate rooms for teleworking or telelearning, no private outdoor spaces, etc.) (Observatorium Voor Gezondheid en Welzijn, 2006; Brussels Environment, 2020).
The uneven access to PGSs and the resulting uneven access to their health-improving qualities could therefore result in increasing health inequalities during and after the epidemic (Cortinez-O'Ryan et al., 2020; Honey-Rosés et al., 2020).
Governments should thus be careful not to limit the availability of the already scarce PGSs in specific neighbourhoods by further closing PGSs during an epidemic. Furthermore, compromising the accessibility of PGSs by implementing a curfew has a negative impact on the promotion of their use and leads to higher concentrations of visitors and is in this sense inadvisable. Consideration could also be given to extending the opening hours of PGSs that have closing times.
Furthermore, apart from availability and accessibility, the attractiveness of PGSs is also key to facilitating their use and making them more restorative.
In this respect, size and connectedness are important points to consider; large or smaller connected PGSs decrease the visitor density and allow people to stay at a distance from one another which increases their attractiveness. On the other hand, as Honey-Rosés et al. (2020) state, cities with a decentralised network of small PGSs may be better prepared to provide easily accessible opportunities to enjoy nature. In the urban core of the Brussels-Capital Region, PGSs tend to be small, more crowded and less natural (Phillips et al., 2021). This naturalness in particular seemed to be an important dimension of attractiveness, as it contributed to the experience of PGSs as healthy places. It is therefore important to design PGSs that are green, which, contrary to what the term “green spaces” suggests, is not always the case. Furthermore, is it important to keep play and sports infrastructure available during an epidemic as this positively contributes to physical health and mental wellbeing. Especially in neighbourhoods with a high population density and a limited offer of PGSs, they tend to be small and less natural and are often mainly designed for play and sport. As a result, when sports and play infrastructure is closed, there is not much left to enjoy in these PGSs. Mitra et al. (2020) state in this respect that since it is unclear whether closing outdoor spaces played an important role in reducing transmission, it may be more important to provide children and youth opportunities for outdoor physical activity and play to boost their health and immune systems. Keeping sports and play infrastructure open could perhaps be facilitated by putting restrictions on the maximum number of users (schedules, time slots, sign-up sheets or monitoring by wardens) and/or by improving hygiene by providing disinfecting gel, for instance. Prohibiting visitors to sit down is another measure that tends to negatively affect PGS use, since it prevents visitors from walking further distances and shortens their stay in the PGS. The severity of measures and restrictions should therefore be weighted to ensure that their benefits exceed the health risks they present, especially for vulnerable population groups. The starting-point should be the perspective of the most vulnerable population groups within society, not that of those with spacious dwellings, private outdoor space and available, accessible and attractive PGSs in their neighbourhoods.
Apart from infrastructural measures and restrictions, individual behaviour also affects the attractiveness of PGSs, resulting in less frequent use, less qualitative use and even avoidance. It is therefore important that responsible behaviours are encouraged through effective and well-targeted communication strategies that inform and raise the awareness of different groups within society, as it is probable that from a health perspective the most vulnerable people are the ones that would benefit the most from PGS use, but are at the same time the ones that are too anxious to make use of them (profile 5).
To conclude with a more general long-term recommendation, future infrastructure plans should be designed in order to create healthy environments and should therefore include PGSs in an active way. In addition, other greening strategies such as greenscapes, green streets, green roofs, and green facades should be included, since research has shown that not only being in PGSs but also being able to see greenery is beneficial for mental wellbeing (Pouso et al., 2020; Soga et al., 2020). This may be especially important for vulnerable population groups that have no access to PGSs and are afraid to use PGSs, but it applies to all citizens when a more severe lockdown is in force during this or possible future epidemics.
Conclusion
This qualitative research examined how PGS users perceived the health advantages of PGSs and how the use of PGSs changed during the epidemic in the Brussels-Capital Region and produced important and novel insights that confirm the importance of PGSs during an epidemic.
We found that while PGSs were initially perceived as a possible threat to health in the first period of the epidemic, they gradually became associated with improved physical and mental health. Although the mechanisms behind this association were also present prior to the epidemic, they became more tangible and more universal. We further found that the use of PGSs changed during the epidemic due to measures and restrictions and due to health risk perceptions. We distinguished five different health risk perception profiles in relation to COVID-19: the denier, the fatalist, the negotiator, the conformer and the worrier.
Since it is probable that more waves of COVID-19 or other viral epidemics will occur in the future, these insights may give decision-makers inspiration and pointers on developing and implementing strategies related to the use of PGSs during epidemics and assist them in providing available and accessible PGSs and in designing attractive more epidemic-proof PGSs. In addition, the proposed health risk perception typology that emerged may serve as a starting point for further research and result in the development of effective and well-targeted communication strategies in order to inform and raise the awareness of different groups within society.
Data Availability Statement
The raw data supporting the conclusions of this article will be made available by the authors, without undue reservation.
Ethics Statement
Ethical review and approval was not required for the study on human participants in accordance with the local legislation and institutional requirements. Written informed consent from the participants' legal guardian/next of kin was not required to participate in this study in accordance with the national legislation and the institutional requirements.
Author Contributions
CN, CV, and SG contributed to the conception and design of the study. CN did the fieldwork, analyzed the data, and wrote the first draft of the manuscript. LR-L wrote a section of the manuscript. All authors contributed to manuscript revision, read, and approved the submitted version.
Funding
We performed this research within the framework of the Green&Quiet Brussels project, funded by Innoviris, the regional institute for research and innovation. Innoviris was not involved in the study design, the collection, analysis or interpretation of data, or the decision to submit this paper for publication.
Conflict of Interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest. The reviewer FB declared a shared affiliation with several of the authors CN, LR-L, CV, and SG at the time of review.
Acknowledgments
The authors would like to thank all the respondents that were willing to take the time to participate in an interview and to share their thoughts, ideas and experiences.
Supplementary Material
The Supplementary Material for this article can be found online at: https://www.frontiersin.org/articles/10.3389/frsc.2021.668443/full#supplementary-material
References
Astell-Burt, T., Feng, X., and Kolt, G. S. (2014). Is neighborhood green space associated with a lower risk of type 2 diabetes evidence from 267,072 australians. Diabetes Care 37, 197–201. doi: 10.2337/dc13-1325
Bowler, D. E., Buyung-Ali, L. M., Knight, T. M., and Pullin, A. S. (2010). A systematic review of evidence for the added benefits to health of exposure to natural environments. BMC Public Health 10, 456–466. doi: 10.1186/1471-2458-10-456
Brussels Environment (2020). HET MILIEU: STAND VAN ZAKEN. Brussels: Brussels Environment. Available online at: https://standvanzaken.leefmilieu.brussels/nl/ (accessed January 22, 2021).
Carter, M., and Horwitz, P. (2014). Beyond proximity: the importance of green space useability to self-reported health. EcoHealth 11, 322–332. doi: 10.1007/s10393-014-0952-9
Chin, A., Simon, G. L., Anthamatten, P., Kelsey, K. C., Crawford, B. R., and Weaver, A. J. (2020). Pandemics and the future of human-landscape interactions. Anthropocene 31:100256. doi: 10.1016/j.ancene.2020.100256
Cortinez-O'Ryan, A., Moran, M. R., Rios, A. P., Anza-Ramirez, C., and Slovic, A. D. (2020). Could severe mobility and park use restrictions during the COVID-19 pandemic aggravate health inequalities? insights and challenges from Latin America. Cadernos Saude Publica 36:e00185820. doi: 10.1590/0102-311x00185820
de Jong, K., Albin, M., Skärbäck, E., Grahn, P., and Björk, J. (2012). Perceived green qualities were associated with neighborhood satisfaction, physical activity, and general health: results from a cross-sectional study in suburban and rural Scania, southern Sweden. Health Place 18, 1374–1380. doi: 10.1016/j.healthplace.2012.07.001
Derks, J., Giessen, L., and Winkel, G. (2020). COVID-19-induced visitor boom reveals the importance of forests as critical infrastructure. For. Policy Econ. 118:102253. doi: 10.1016/j.forpol.2020.102253
Gascon, M., Mas, M. T., Martínez, D., Dadvand, P., Forns, J., Plasència, A., et al. (2015). Mental health benefits of long-term exposure to residential green and blue spaces: a systematic review. Int. J. Environ. Res. Public Health 12, 4354–4379. doi: 10.3390/ijerph120404354
Gascon, M., Triguero-Mas, D., Mart inez, P., Dadvand, J., Forns, A., and Plasencia, M. J. N. (2016). Residential green spaces and mortality: a systematic review. Environ. Int. 86, 60–67. doi: 10.1016/j.envint.2015.10.013
Geng, D., (Christina), Innes, J., Wu, W., and Wang, G. (2020). Impacts of COVID-19 pandemic on urban park visitation: a global analysis. J. For. Res. 12, 1–15. doi: 10.1007/s11676-020-01249-w
Gómez-Baggethun, E., and Barton, D. N. (2013). Classifying and valuing ecosystem services for urban planning. Ecol. Econ. 86, 235–245. doi: 10.1016/j.ecolecon.2012.08.019
Hartig, T., Mang, M., and Evans, G. W. (1991). Restorative effects of natural-environment experiences. Environ. Behav. 23, 3–26. doi: 10.1177/0013916591231001
Honey-Rosés, J., Anguelovski, I., Chireh, V. K., Daher, C., Konijnendijk van den Bosch, C., Litt, J. S., et al. (2020). The impact of COVID-19 on public space: an early review of the emerging questions—design, perceptions, and inequities. Cities Health 1–17. doi: 10.1080/23748834.2020.1780074
Leclerc, Q. J., Fuller, N. M., Knight, L. E., Funk, S., and Knight, G. M. (2020). What settings have been linked to SARS-CoV-2 transmission clusters? [version 2; peer review: 2 approved]. Wellcome Open Res. 5:83. doi: 10.12688/wellcomeopenres.15889.2
Lee, A. C. K., and Maheswaran, R. (2011). The health benefits of urban green spaces: a review of the evidence. J. Public Health 33, 212–222. doi: 10.1093/pubmed/fdq068
Lovell, S. T., and Taylor, J. R. (2013). Supplying urban ecosystem services through multifunctional green infrastructure in the United States. Landsc. Ecol. 28, 1447–1463. doi: 10.1007/s10980-013-9912-y
Maas, J., van Dillen, S. M. E., Verheij, R. A., and Groenewegen, P. P. (2009). Social contacts as a possible mechanism behind the relation between green space and health. Health Place 15, 586–595. doi: 10.1016/j.healthplace.2008.09.006
Maas, J., Verheij, R. A., Groenewegen, P. P., De Vries, S., and Spreeuwenberg, P. (2006). Green space, urbanity, and health: how strong is the relation? J. Epidemiol. Community Health 60, 587–592. doi: 10.1136/jech.2005.043125
Mitchell, R., and Popham, F. (2008). Effect of exposure to natural environment on health inequalities: an observational population study. Lancet 372, 1655–1660. doi: 10.1016/S0140-6736(08)61689-X
Mitra, R., Moore, S. A., Gillespie, M., Faulkner, G., Vanderloo, L. M., Chulak-Bozzer, T., et al. (2020). Healthy movement behaviours in children and youth during the COVID-19 pandemic: exploring the role of the neighbourhood environment. Health Place 65:102418. doi: 10.1016/j.healthplace.2020.102418
Nieuwenhuijsen, M. J., Khreis, H., Triguero-Mas, M., Gascon, M., and Dadvand, P. (2017). Fifty shades of green: pathway to healthy urban living. Epidemiology 28, 63–71. doi: 10.1097/EDE.0000000000000549
Observatorium Voor Gezondheid en Welzijn (2006). Welzijns- en gezondheidsatlas van Brussel-Hoofdstad 2006. Gemeenschappelijke Gemeenschapscommissie. Available online at: https://www.ccc-ggc.brussels/sites/default/files/documents/graphics/dossiers/dossier-2006-welzijns-en-gezondheidsatlas-van-brussel-hoofdstad.pdf (accessed January 22, 2021).‘
Pereira, G., Christian, H., Foster, S., Boruff, B. J., Bull, F., Knuiman, M., et al. (2013). The association between neighborhood greenness and weight status: an observational study in Perth Western Australia. Environ. Health Glob. Access Sci. Source 12, 49–58. doi: 10.1186/1476-069X-12-49
Phillips, A., Khan, A. Z., and Canters, F. (2021). Use-related and socio-demographic variations in urban green space preferences. Sustainability 13:3461. doi: 10.3390/su13063461
Pouso, S., Borja, Á., Fleming, L. E., Gómez-Baggethun, E., White, M. P., and Uyarra, M. C. (2020). Contact with blue-green spaces during the COVID-19 pandemic lockdown beneficial for mental health. Sci. Tot. Environ. 756:143984. doi: 10.31235/osf.io/gpt3r
Pretty, J., Peacock, J., Sellens, M., and Griffin, M. (2005). The mental and physical health outcomes of green exercise. Int. J. Environ. Health Res. 15, 319–337. doi: 10.1080/09603120500155963
Qian, H., Miao, T., Liu, L., Zheng, X., Luo, D., and Li, Y. (2020). Indoor transmission of SARS-CoV-2. Indoor Air 31, 1–22. doi: 10.1111/ina.12766
Rajkumar, R. P. (2020). COVID-19 and mental health: a review of the existing literature. Asian J. Psychiatry 52:102066. doi: 10.1016/j.ajp.2020.102066
Soga, M., Evans, M. J., Tsuchiya, K., and Fukano, Y. (2020). A room with a green view: the importance of nearby nature for mental health during the COVID-19 pandemic. Ecol. Appl. 31:e2248. doi: 10.1002/eap.2248
Stessens, P., Canters, F., Huysmans, M., and Khan, A. Z. (2020). Urban green space qualities: an integrated approach towards GIS-based assessment reflecting user perception. Land Use Policy 91:104319. doi: 10.1016/j.landusepol.2019.104319
Stessens, P., Khan, A. Z., Huysmans, M., and Canters, F. (2017). Analysing urban green space accessibility and quality: a GIS-based model as spatial decision support for urban ecosystem services in Brussels. Ecosyst. Serv. 28, 328–340. doi: 10.1016/j.ecoser.2017.10.016
Tang, F., Liang, J., Zhang, H., Kelifa, M. M., He, Q., and Wang, P. (2020). COVID-19 related depression and anxiety among quarantined respondents. Psychol. Health 36, 164–178. doi: 10.1080/08870446.2020.1782410
Ugolini, F., Massetti, L., Calaza-Martínez, P., Cariñanos, P., Dobbs, C., Ostoic, S. K., et al. (2020). Effects of the COVID-19 pandemic on the use and perceptions of urban green space: an international exploratory study. Urban For. Urban Green. 56:126888. doi: 10.1016/j.ufug.2020.126888
Van de Voorde, T. (2017). Spatially explicit urban green indicators for characterizing vegetation cover and public green space proximity: a case study on Brussels, Belgium. Int. J. Digit. Earth 10, 798–813. doi: 10.1080/17538947.2016.1252434
van Dillen, S. M. E., de Vries, S., Groenewegen, P. P., and Spreeuwenberg, P. (2012). Greenspace in urban neighbourhoods and residents' health: adding quality to quantity. J. Epidemiol. Community Health 66:e8. doi: 10.1136/jech.2009.104695
Venter, Z. S., Barton, D. N., Gundersen, V., Figari, H., and Nowell, M. (2020). Urban nature in a time of crisis: Recreational use of green space increases during the COVID-19 outbreak in Oslo, Norway. Environ. Res. Lett. 15:104075. doi: 10.1088/1748-9326/abb396
VRT (2020). Brussel voert nog strengere maatregelen in: avondklok van 22 tot 6 uur, mondmaskerplicht en alleen winkelen. Available onlilne at: https://www.vrt.be/vrtnws/nl/2020/10/24/brussel-voert-nog-strengere-maatregelen-in-avondklok-van-22-tot/ (accessed December 1, 2020).
WHO (2020). Statement on the Second Meeting of the International Health Regulations (2005) Emergency Committee Regarding the Outbreak of Novel Coronavirus (2019-nCoV). Available onlilne at: https://www.who.int/news/item/30-01-2020-statement-on-the-second-meeting-of-the-international-health-regulations-(2005)-emergency-committee-regarding-the-outbreak-of-novel-coronavirus-(2019-ncov) (accessed November 30, 2020).
Keywords: COVID-19, public green space, physical health, mental health, health risk perceptions, qualitative research
Citation: Noël C, Rodriguez-Loureiro L, Vanroelen C and Gadeyne S (2021) Perceived Health Impact and Usage of Public Green Spaces in Brussels' Metropolitan Area During the COVID-19 Epidemic. Front. Sustain. Cities 3:668443. doi: 10.3389/frsc.2021.668443
Received: 16 February 2021; Accepted: 28 April 2021;
Published: 03 June 2021.
Edited by:
Rieke Hansen, Hochschule Geisenheim University, GermanyReviewed by:
Chi Xu, Nanjing University, ChinaSimon Bell, University of Edinburgh, United Kingdom
Francesc Baró, Vrije University Brussel, Belgium
Copyright © 2021 Noël, Rodriguez-Loureiro, Vanroelen and Gadeyne. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Charlotte Noël, Y2hhcmxvdHRlLm5vZWxAdnViLmJl
†These authors have contributed equally to this work and share last authorship
 Charlotte Noël
Charlotte Noël Lucia Rodriguez-Loureiro
Lucia Rodriguez-Loureiro Christophe Vanroelen
Christophe Vanroelen Sylvie Gadeyne
Sylvie Gadeyne