- 1Nursing of Colloge, Jiangxi University of Chinese Medicine, Nanchang, Jiangxi, China
- 2College of Clinical Medicine, Jiangxi University of Chinese Medicine, Nanchang, Jiangxi, China
Objective: This study aims to comprehensively evaluate the efficacy of different non-pharmacological interventions in treating constipation symptoms in lung cancer patients through a network meta-analysis, providing evidence-based support for personalized treatment decisions in clinical practice.
Methods: We retrieved randomized controlled trials (RCTs) from well-known databases and compared the efficacy of non-pharmacological interventions with traditional treatments or placebos in improving constipation symptoms in lung cancer patients. The search was conducted through January 2025. Two researchers independently screened the literature, extracted data, and assessed the quality of the studies using the Cochrane risk of bias tool. Traditional meta-analysis was performed using Stata 16.0 software. Network meta-analysis (NMA) was conducted using RStudio software to integrate the data and create a network diagram to display the comparisons between non-pharmacological interventions. The credibility of the evidence was assessed using the Confidence in Network Meta-Analysis (CINeMA) tool.
Results: A total of 33 studies involving 3,471 participants were included in this study. The traditional meta-analysis revealed that non-pharmacological interventions effectively reduced the incidence of constipation and improved constipation symptom management in lung cancer patients during treatment. Additionally, these interventions positively impacted the time to first bowel movement and reduced negative emotions (such as anxiety) in hospitalized lung cancer patients with constipation. The network meta-analysis (31 studies, 3,287 participants) indicated that acupoint stimulation was the most effective non-pharmacological intervention for reducing constipation incidence in lung cancer patients during treatment. The combined use of two types of acupoint patches showed optimal efficacy in improving constipation symptoms. However, for overall therapeutic effectiveness, the combination of acupoint patch therapy and acupoint massage most effectively reduced constipation incidence and improved overall constipation symptom management in lung cancer patients during treatment.
Conclusion: The combination of acupoint patch therapy and acupoint massage is recommended as the preferred clinical intervention for treating constipation symptoms in lung cancer patients.
Systematic Review Registration: https://www.crd.york.ac.uk/prospero/, identifier CRD42025631567.
1 Introduction
As of 2020, new cases of lung cancer accounted for 11.4% of all global cancer cases, making it the second most prevalent malignancy in terms of incidence (1). Particularly in China, lung cancer is the leading malignancy in terms of both incidence and mortality among male patients (2). Currently, surgery, radiotherapy, and chemotherapy are the primary clinical treatments for lung cancer (3). Constipation is one of the most common symptoms during anticancer treatment, particularly in patients with stage III/IV lung cancer. Chemotherapy drugs such as carboplatin and cisplatin, which are commonly used in these patients, are known to cause side effects like nausea and vomiting. To alleviate or control these symptoms, antiemetic drugs, such as ondansetron, are often required. While these medications can manage nausea and vomiting by suppressing gastrointestinal motility, they can also significantly increase the risk of constipation (4). Research has demonstrated that lung cancer patients exhibit a significant reduction in the abundance of beneficial bacteria such as Bifidobacteria and Lactobacilli in their gut microbiota, while the proportion of opportunistic pathogens like Enterococci increases, which consequently leads to intestinal dysfunction (5). Severe constipation in lung cancer patients increases cardiopulmonary burden and may even precipitate cardiovascular and cerebrovascular accidents. Although constipation management is crucial for patient health, existing research predominantly focuses on pain and cough management (6, 7). In recent years, non-pharmacological interventions (NPIs) have demonstrated distinct advantages in constipation management for lung cancer patients. In this study, NPIs are defined as an integrated intervention system covering diet, exercise, behavior therapy and external treatment of traditional Chinese medicine (such as acupuncture and moxibustion, massage and other standardized traditional therapies), so as to build a more clinical representative intervention network. These interventions are characterized by high safety profiles, absence of drug dependency, and hepatorenal toxicity risks, making them suitable for long-term use. Furthermore, NPIs can simultaneously address symptom relief and constitutional adjustment while offering significant economic cost-effectiveness. However, systematic exploration of NPIs for constipation management remains lacking. Current research on NPIs still presents limitations. Existing studies predominantly involve short-term follow-up periods and lack evidence supporting long-term efficacy and safety, making it difficult to comprehensively evaluate the durability and potential impacts of NPIs on constipation symptoms in lung cancer patients. Therefore, this study employs network meta-analysis, a statistical method that integrates direct and indirect evidence, to compare the efficacy and safety of various NPIs comprehensively. Through this methodology, we can systematically evaluate the relative advantages of different NPIs in constipation management for lung cancer patients, thereby providing more scientific and comprehensive evidence for clinicians to develop individualized treatment protocols.
2 Methods
2.1 Registration
This study was conducted according to the PRISMA-NMA guidelines and registered with PROSPERO (ID: CRD42025631567).
2.2 Literature search and screening
2.2.1 Search strategy
We searched journals published up to January 2025 in PubMed, Embase, The Cochrane Library, Web of Science, CINAHL, China National Knowledge Infrastructure (CNKI), Wanfang Database, and VIP Database. The search keywords primarily focused on “Lung Neoplasms,” “Lung Cancer,” “Constipation,” “Colonic Inertia,” and related terms. The final search formula was determined by searching subject headings, subheadings, and free text terms. (See the Supplementary Materials for the PubMed search formula.)
2.2.2 Literature screening
The retrieved literature was imported into the NoteExpress reference management software for screening. Two researchers (CM and YJ) independently conducted literature screening and data extraction. If there were any disagreements, they were resolved through discussion between the two parties or with the assistance of a third party (XYY). The extracted content included author, publication date, age, sample size, intervention protocol for the experimental group, intervention duration, outcome measures, and effect size.
2.2.3 Inclusion and exclusion criteria
Inclusion criteria: Study type: The included studies encompass double-arm or multi-arm randomized controlled trials.
(P) Participants: The research subjects must be adults over 18 years old who have been diagnosed with lung cancer and have symptoms of constipation. There are no restrictions on the type, staging, or severity of lung cancer and constipation.
(I) Non-pharmacological interventions (NPIs) are the primary treatment methods, including but not limited to:
Traditional Chinese Medicine (TCM) interventions: moxibustion, acupuncture, massage, acupoint application, ear acupressure, etc.
Behavioral interventions: biofeedback training, scheduled toilet routines, relaxation techniques, etc.
Dietary and lifestyle interventions: fiber-rich diets, hydration protocols, structured physical activity, etc.
Studies employing single or multiple complementary and alternative medicine (CAM) interventions will also be considered.
(C) Control group intervention measures: These include routine treatment, placebo, sham intervention, blank control, or other different non-pharmacological intervention measures.
(O) Outcome indicators: Endpoint assessments must include at least one outcome indicator related to constipation or constipation-related measures under NPIs, such as effectiveness rate, incidence rate, etc. Outcome measurement types: This study uses the incidence of constipation symptoms and the effectiveness rate of treatment at the end of treatment as the primary outcome indicators. The time to first bowel movement recorded during treatment is a secondary outcome indicator.
(S) Study type: Randomized controlled trials (RCTs).
Exclusion criteria: Abstracts, unpublished academic papers, editorials, clinical observations, case studies, cohort design studies, non-randomized trials, and case-control studies.
2.2.4 Data extraction and quality assessment
Two researchers (CM and YJ) created a data extraction table based on the information needed for the study, including author, year, research subjects, gender, sample size, intervention measures, follow-up time, outcome indicators, quality assessment information, and other relevant content. When the information extracted by the two individuals was inconsistent, they first discussed it with each other to resolve the issue. If the problem could not be resolved, a final decision was made through discussion with or consultation of a third researcher (XYY). Two researchers (CM and YJ) used the standards from the “Cochrane Handbook for Systematic Reviews of Interventions” to conduct quality assessments of the included RCTs across seven aspects: generation of random sequence, allocation concealment, blinding of researchers and subjects, blinding of study endpoints, completeness of outcome data, selective reporting, and other biases (8). The assessment was independently completed by both researchers and cross-checked. In case of disagreement, a third researcher (XYY) was consulted to determine the final assessment results. Additionally, we used the CINeMA (Confidence in Network Meta-Analysis) web application to assess the credibility of evidence, categorizing the credibility of results into four levels: high, moderate, low, and very low (9).
2.3 Statistical analysis
2.3.1 Traditional meta-analysis
This study used Stata 16.0 software for traditional meta-analyses on extracted dichotomous and continuous variables. For dichotomous variables, odds ratios (OR) and 95% confidence intervals (CI) were used as effect indicators, while for continuous variables, standardized mean differences (SMD) and 95% CI were used as effect indicators. Results from different studies were combined using a random effects model. Heterogeneity between studies was assessed using the I² statistic and its associated p-value. Specifically, I² values of 25%, 50%, and 75% represented low, moderate, and high statistical heterogeneity, respectively. If P > 0.1 and I² ≤ 50%, this indicated low heterogeneity between studies, and a fixed effects model was applied for analysis; if P < 0.1 or I² > 50%, this indicated significant heterogeneity between studies, and a random effects model was applied for analysis, followed by subgroup and sensitivity analyses to infer the source of heterogeneity.
2.3.2 Network meta-analysis
Network meta-analysis involves splitting all included studies into combinable two-arm comparisons and entering them into RStudio software. Markov chain Monte Carlo simulation chains were used to conduct network meta-analysis on primary outcomes including incidence rates and effectiveness, with odds ratio (OR) and its 95% confidence interval (CI) as effect size indicators. The BUGSnet 1.1.1 package was used for Bayesian network meta-analysis and to draw network relationship diagrams, calling JAGS (Just Another Gibbs Sampler). JAGS’ generalized linear model was used to process the included study data. The Bayesian network meta-analysis was set with 50,000 burn-in iterations, 100,000 formal iterations, and 10,000 adaptations for Markov chain Monte Carlo (MCMC) chain simulation. The potential scale reduction factor (PSRF) was used to evaluate the convergence results of the model, with a PSRF of 1.00-1.05 suggesting satisfactory model convergence. Network relationship diagrams of outcome indicators were drawn. When closed loops were formed in the diagram, the node-splitting method was used for inconsistency testing, with P > 0.05 suggesting consistency between direct and indirect comparison results. In the generated network diagram, each node represented different interventions and controls, and lines connecting nodes represented direct comparisons between different interventions. The size of each node and the width of connecting lines were proportional to the number of studies. The efficacy of each indicator was ranked to obtain the surface under the cumulative ranking (SUCRA), and the probability ranking was plotted on the chart. SUCRA was expressed as a percentage; the higher the percentage, the more effective the intervention, with a zero value indicating the intervention was ineffective.
3 Result
3.1 Literature search results
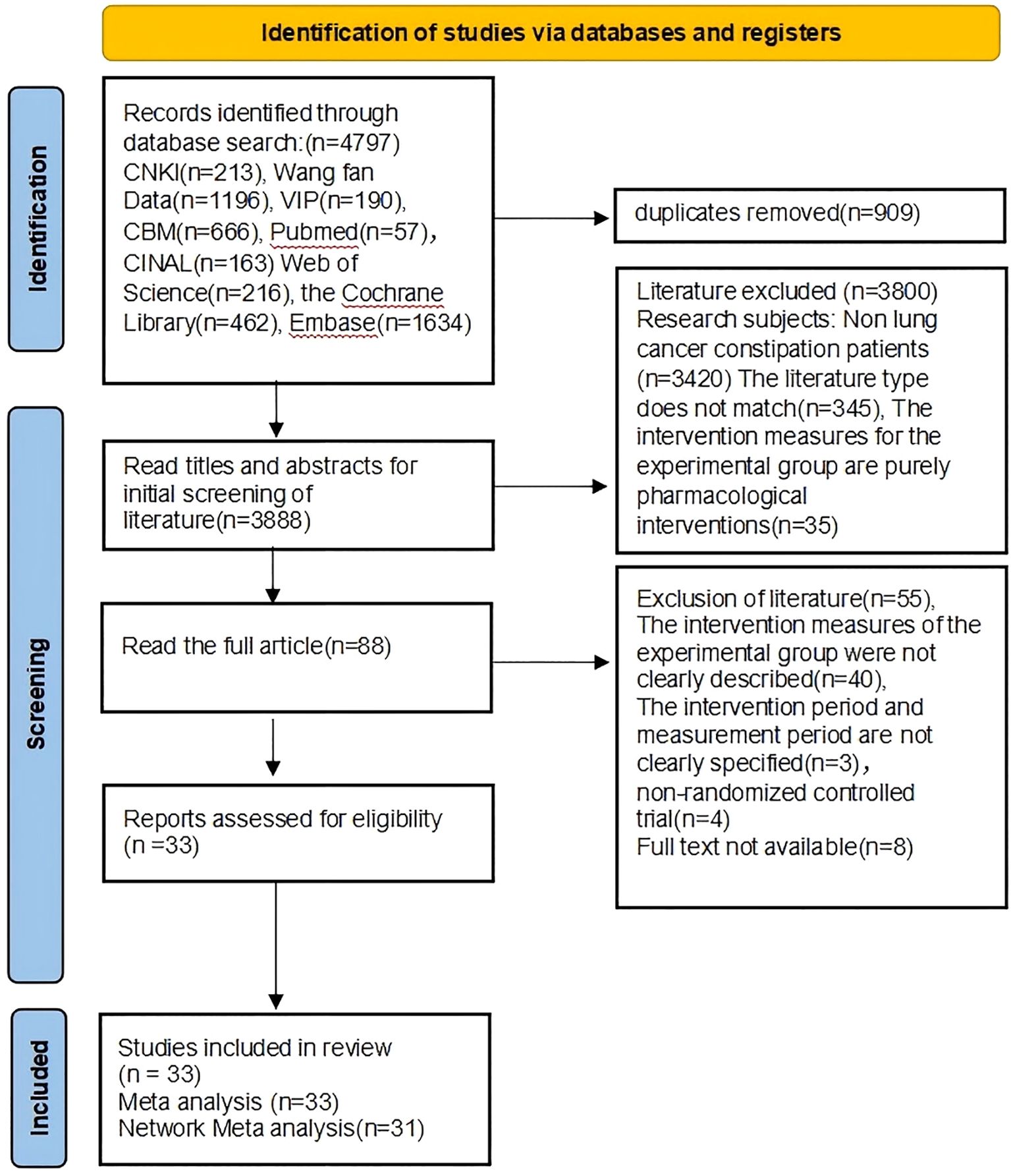
Figure 1 shows the flowchart of PRISMA system overview. In the preliminary review stage, we conducted a comprehensive search of the database using retrieval methods and retrieved a total of 4797 relevant papers. We used NoteExpress software to remove 909 duplicate articles leaving 3888 articles. Subsequently, we conducted a first screening of the titles and abstracts, excluding 3800 studies, including 3420 articles unrelated to the research topic, 345 reviews and animal studies, and 35 studies involving drug interventions. For the remaining 88 relevant research articles, we conducted full-text reading for the second round of screening. Among them, full texts of 8 studies could not be found, and we attempted to contact the corresponding authors but were unable to obtain them. 40 studies did not clearly describe intervention measures, 3 studies did not describe intervention cycles and measurement times, and 4 studies were non-randomized controlled trials. Finally, 33 studies were included in the analysis, with all 33 studies included in the meta-analysis and 31 studies included in the network meta-analysis.
3.2 General characteristics
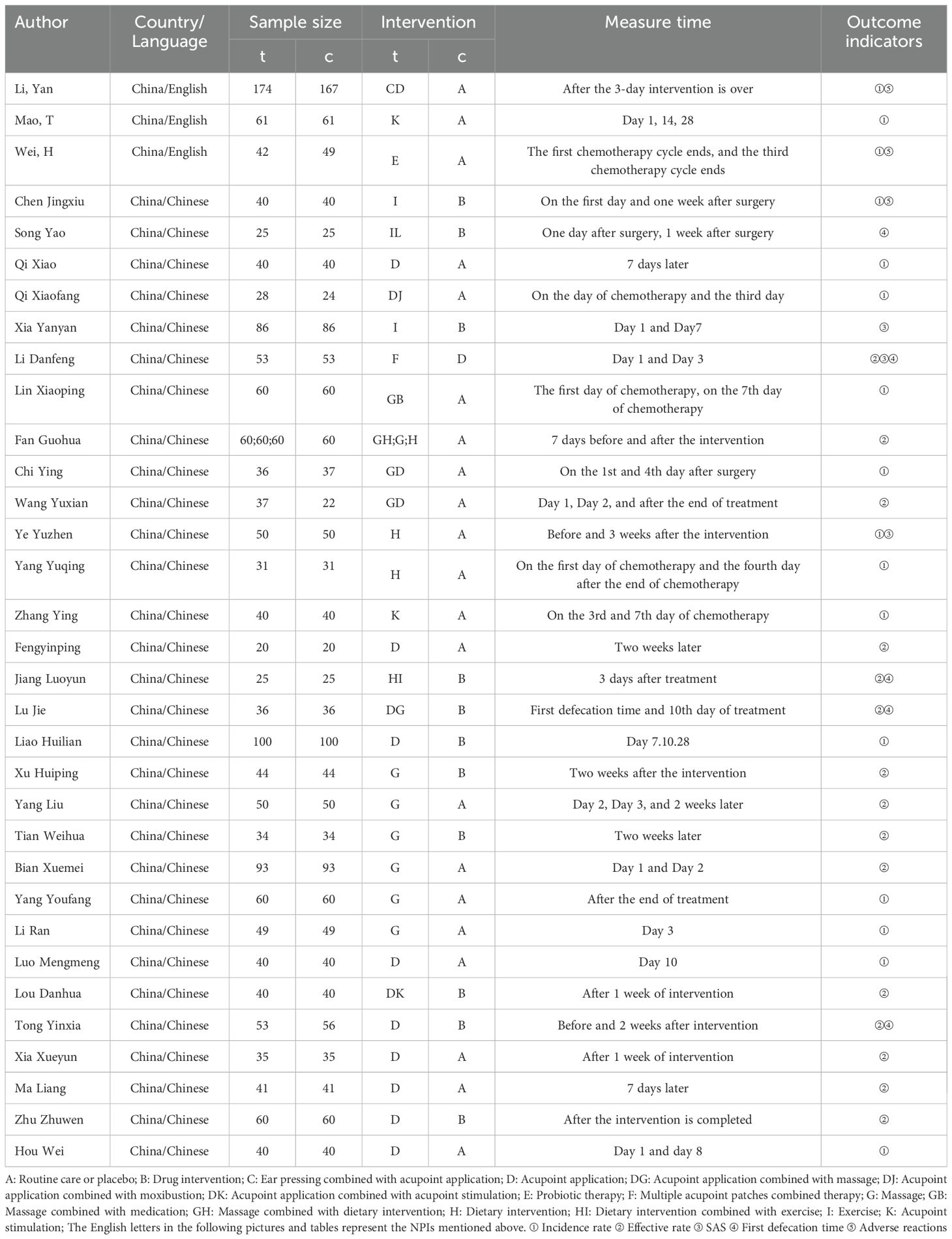
Table 1 lists the characteristics of the included studies. Among the 33 included studies ( (10–42), a total of 3,471 patients met the analysis criteria. The interventions in these studies included exercise (including intestinal function training and therapeutic exercises), ear acupoint pressure, acupoint application, moxibustion, acupoint stimulation (including acupuncture and electroacupuncture), massage, probiotics, dietary interventions, and their combinations. Key characteristics were extracted, including sample size, intervention methods, treatment duration, and outcome measures.
3.3 Quality assessment
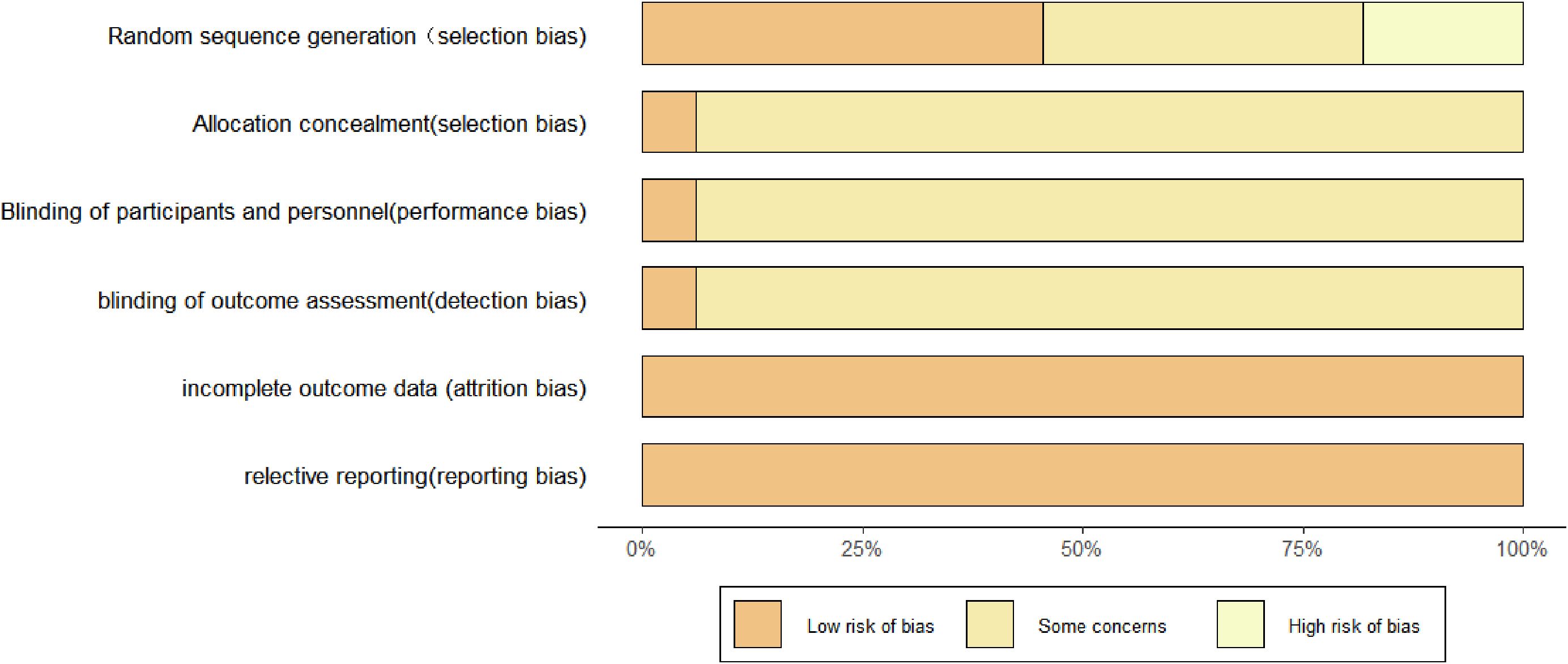
Using the Cochrane Collaboration’s RoB 2 tool, we assessed 33 included studies: 2 (6.1%) were judged to have low risk of bias, 25 (75.8%) had some concerns (primarily due to deviations from intended interventions or missing outcome data), and 6 (18.1%) were rated as high risk (especially the risk of bias in random processes). The overall risk-of-bias distribution is presented in Figure 2. For all outcome indicators, the overall certainty of evidence was relatively low. For the primary outcome indicators, we assessed the credibility of evidence in comparisons with the control group; all evidence was rated as moderate or low quality. In comparisons between different NPIs, most evidence was rated as low quality. Details can be found in the Supplementary Figure 1.
To evaluate how high-risk studies influenced the network estimates, we examined the distribution and impact of the 6 high-risk studies. These studies involved direct comparisons of exercise, acupoint application, massage combined with acupoint application, massage, and combined acupoint applications against control interventions, all contributing direct evidence to the network.
We conducted one-study-removed sensitivity analyses for the primary outcomes to assess the individual impact of each study, including the high-risk studies, on network estimates. Sensitivity analyses of 31 studies for primary outcomes (incidence rate and effectiveness rate) demonstrated that excluding any single study did not alter the pooled estimates (incidence rate: OR=0.16, 95%CI [0.11–0.24], P<0.01; effectiveness rate: OR=3.41, 95%CI [1.75–6.65], P<0.01). This finding indicates that the network estimates remained stable even when high-risk studies were individually removed, suggesting that the inclusion of studies with methodological concerns did not substantially bias the overall network meta-analysis results. The robustness of these findings supports the reliability of our primary conclusions, despite the presence of studies with high risk of bias in the network.
3.4 Conventional meta-analysis
3.4.1 Incidence rate
16 studies with 1,779 participants evaluated the incidence rate of constipation symptoms after treatment. Meta-analysis showed that the incidence rate in the non-pharmacological intervention group was significantly reduced (OR=0.16; 95% CI [0.11, 0.24], P<0.01), with moderate heterogeneity (I²=56.3%). Subgroup analysis results showed that studies with intervention duration ≤7 days had moderate heterogeneity (I²=33.9%), while those with intervention duration >7 days had moderate-to-high heterogeneity (I²=74.4%). Regarding sample size, the subgroup with a total sample size ≥120 showed moderate-to-high heterogeneity (I²=73.3%), while the group with a sample size <120 showed moderate-to-low heterogeneity (I²=43.2%). I In terms of intervention types, the combined non-pharmacological intervention groups showed moderate-to-low heterogeneity (I²=38.1%). However, the single non-pharmacological intervention group showed moderate-to-high heterogeneity (I²=62.5%) (see Figure 3).
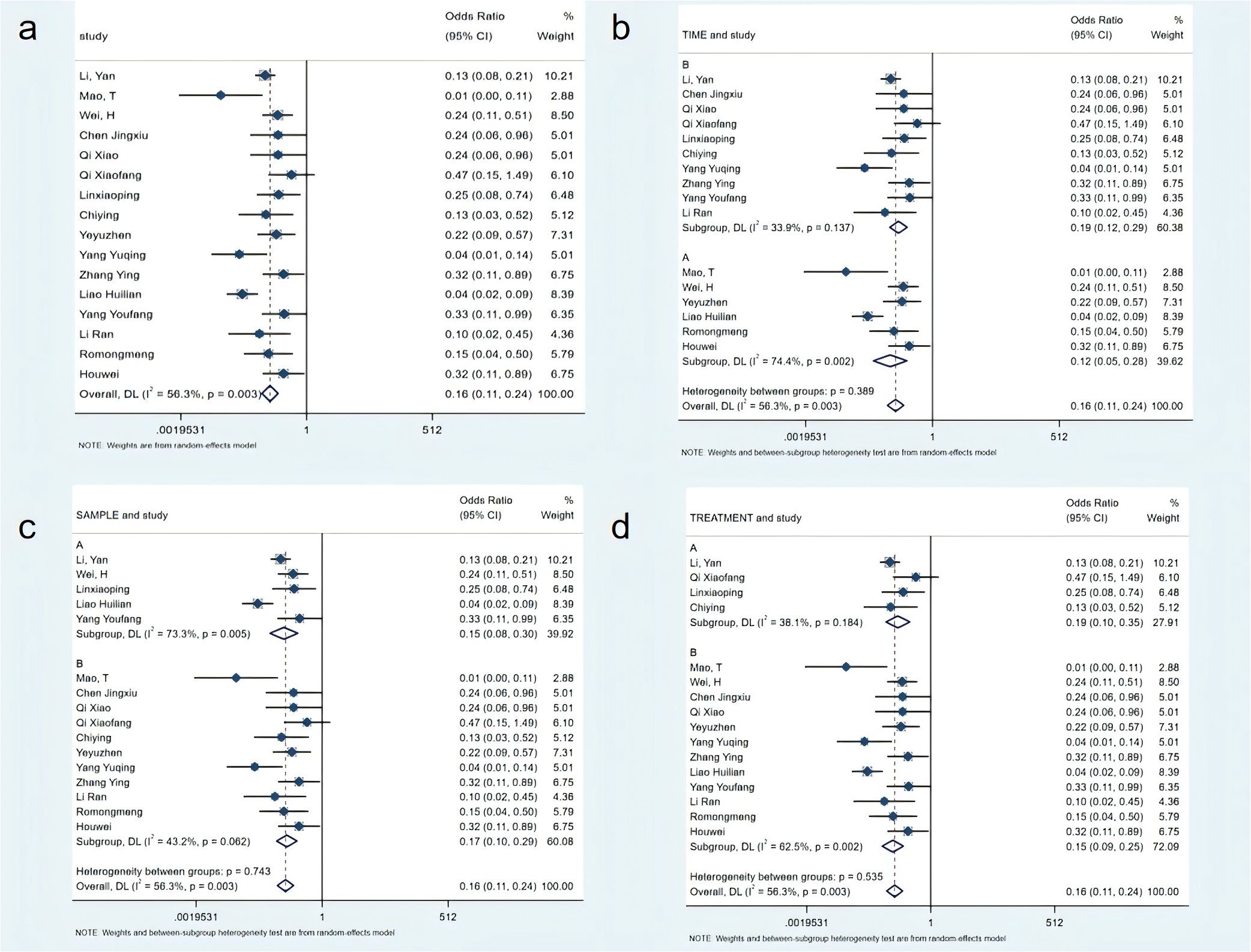
Figure 3. Meta-analysis of incidence rates. (a) Meta-analysis of incidence rate; (b) Subgroup analysis of incidence rate based on intervention time; (c) Subgroup analysis of incidence rate based on sample size; (d) Subgroup analysis of incidence rate by sample size.
3.4.2 Effective rate
A total of 15 studies, comprising 1,508 patients, were included in the evaluation of the effective rate of constipation symptom treatment. Meta-analysis showed that the non-pharmacological intervention group had a significantly higher effective rate (OR=3.41; 95% CI [1.75, 6.65], P<0.01). Subgroup analysis results showed that the group with intervention duration ≥7 days had moderate-to-high heterogeneity (I²=73%), while the group with intervention duration <7 days had extremely high heterogeneity (I²=84.7%). The group with a sample size ≥120 had moderate heterogeneity (I²=51%), while the group with a sample size <120 had moderate-to-high heterogeneity (I²=76.3%). Regarding intervention types, the combined non-pharmacological intervention groups had extremely low heterogeneity (I²=0), while the single intervention group had extremely high heterogeneity (I²=83.5%) (see Figure 4).
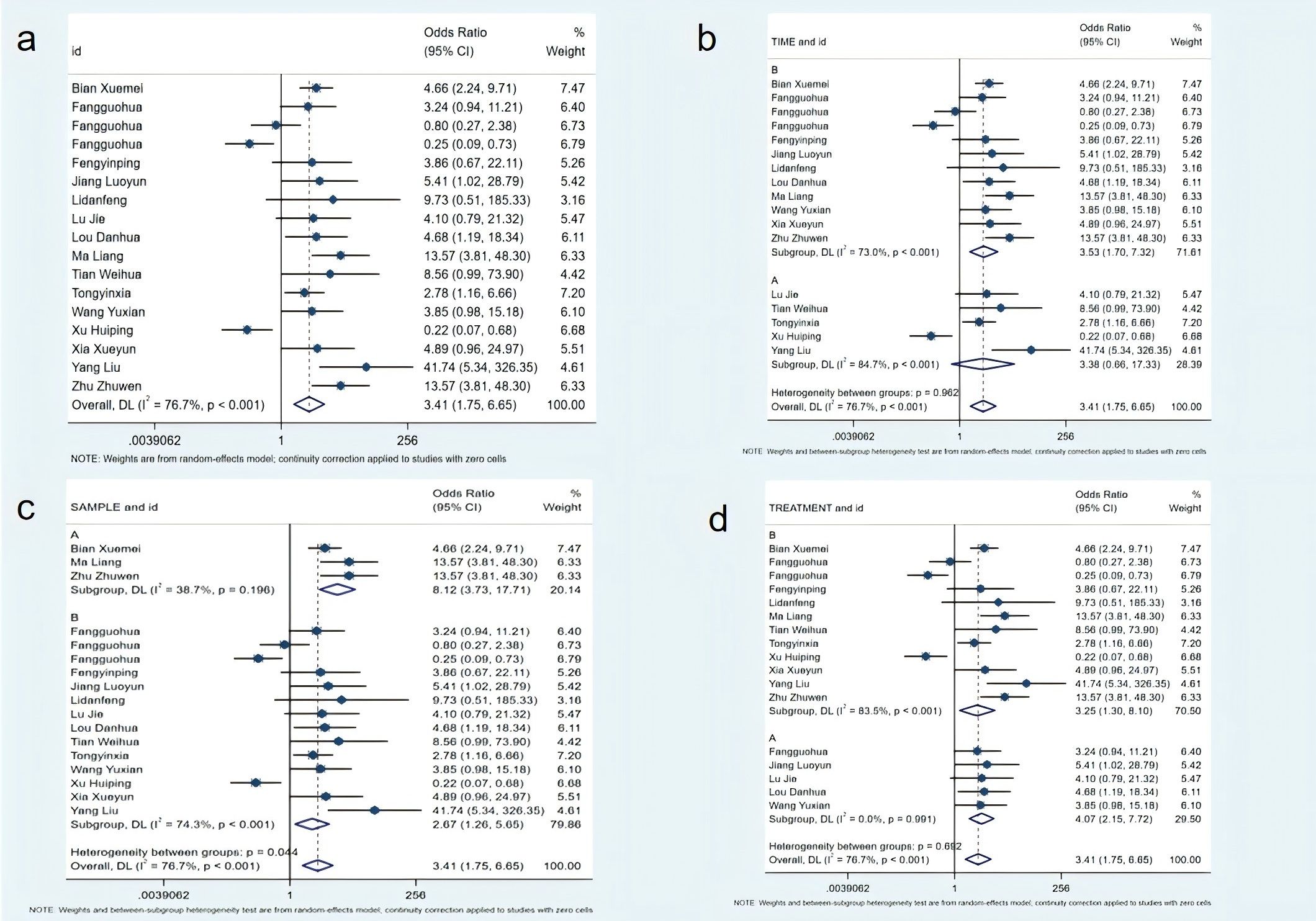
Figure 4. Meta-analysis of effective rate. (a) Meta-analysis of effective rate; (b) Subgroup analysis of adequate intervention time; (c) Subgroup analysis of adequate sample size; (d) Subgroup analysis of effective intervention measures.
3.4.3 Self-Rating Anxiety Scale
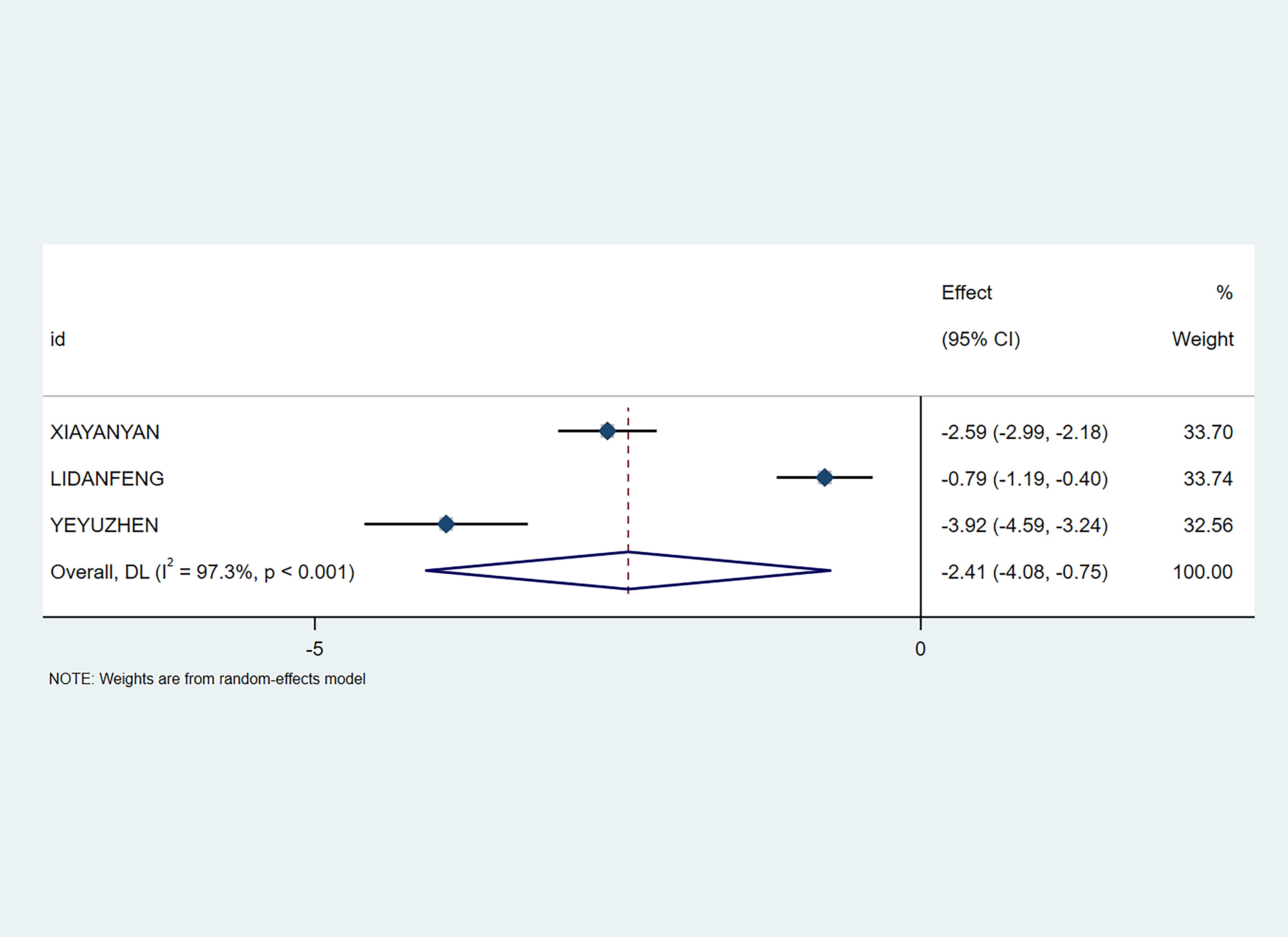
A total of 3 studies involving 378 patients evaluated the Self-Rating Anxiety Scale (SAS) scores. Meta-analysis showed that the non-pharmacological intervention group effectively reduced patients’ post-intervention SAS scores (SMD=-2.41; 95% CI [-4.08, -0.75], P<0.01) (see Figure 5).
3.4.4 Time to first bowel movement
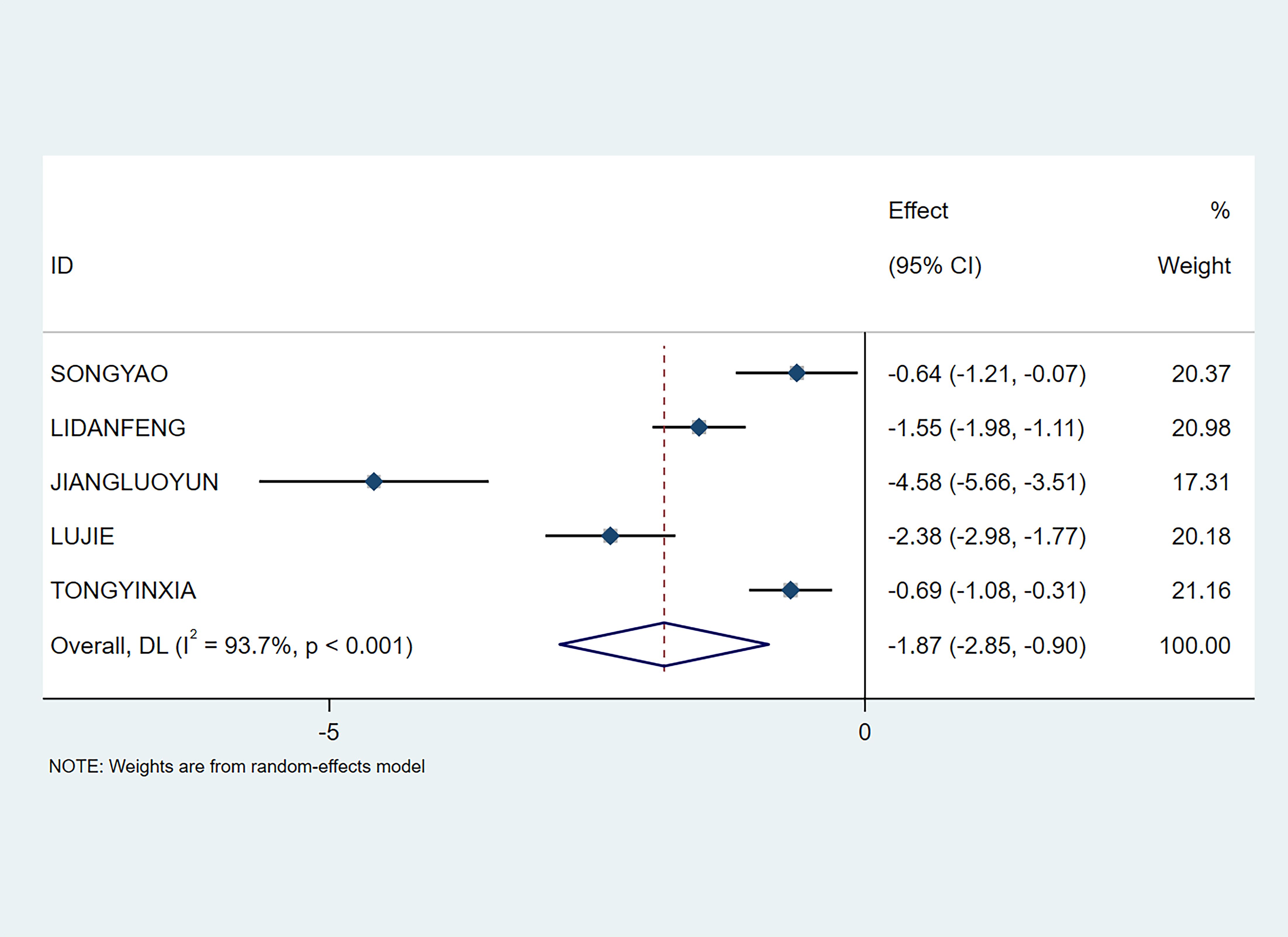
A total of 5 studies involving 387 participants reported the time to first bowel movement. Meta-analysis showed that NPIs could effectively shorten the time patients took for their first bowel movement (SMD=-1.87; 95% CI [-2.85, -0.9], P<0.01) (see Figure 6).
3.5 Network meta-analysis
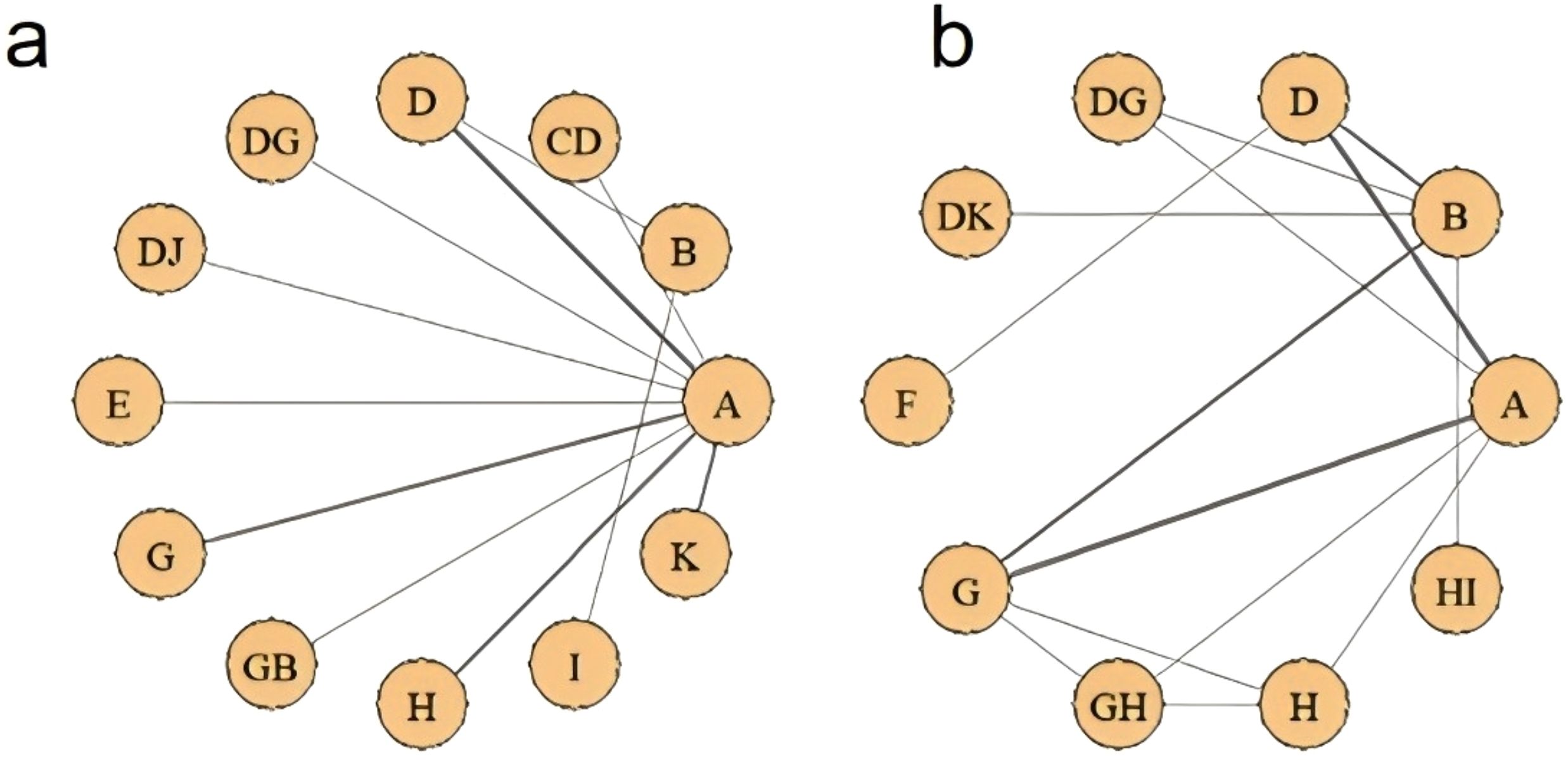
Figure 7 presents the eligible comparison network diagram of different NPIs for constipation symptoms in lung cancer patients. 31 studies involving 3,827 participants evaluated the effects of various NPIs on constipation symptoms in lung cancer patients. All NPIs were directly compared with at least the control group.
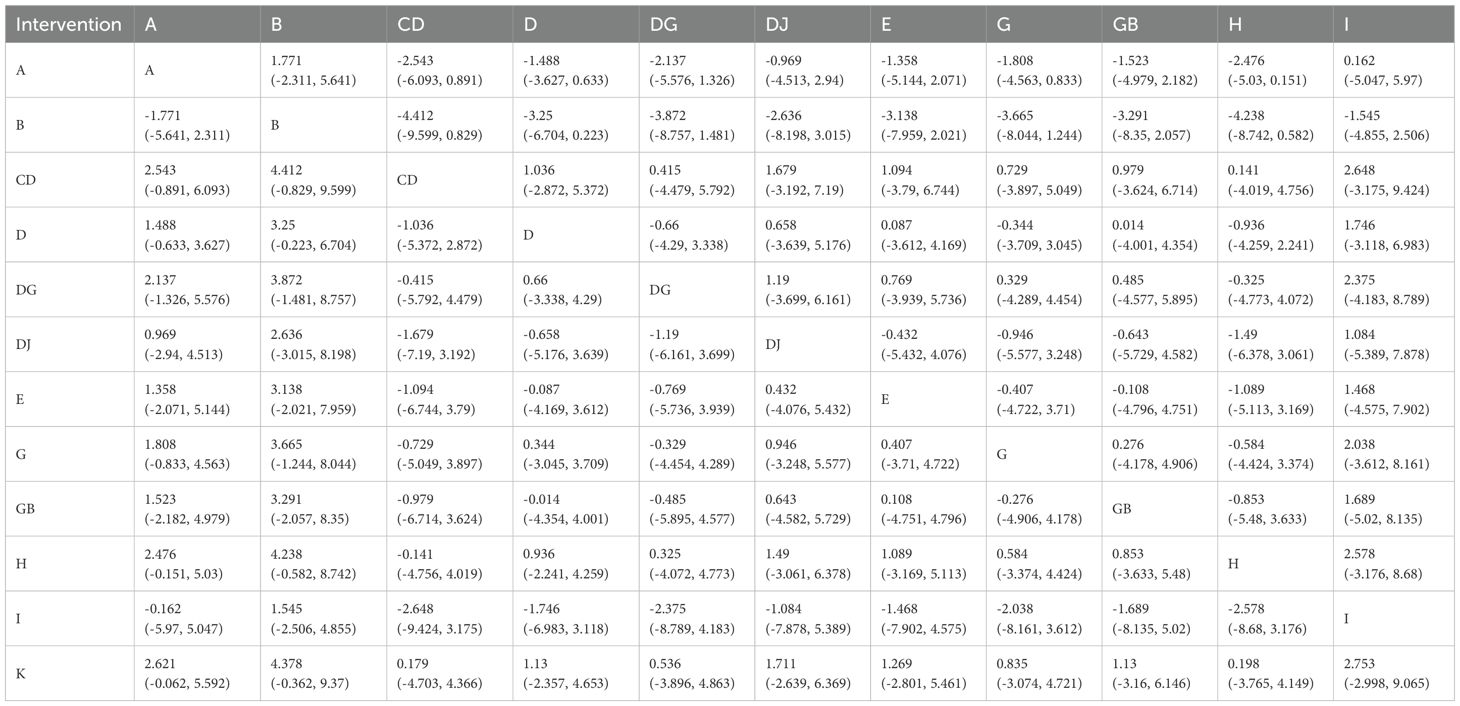
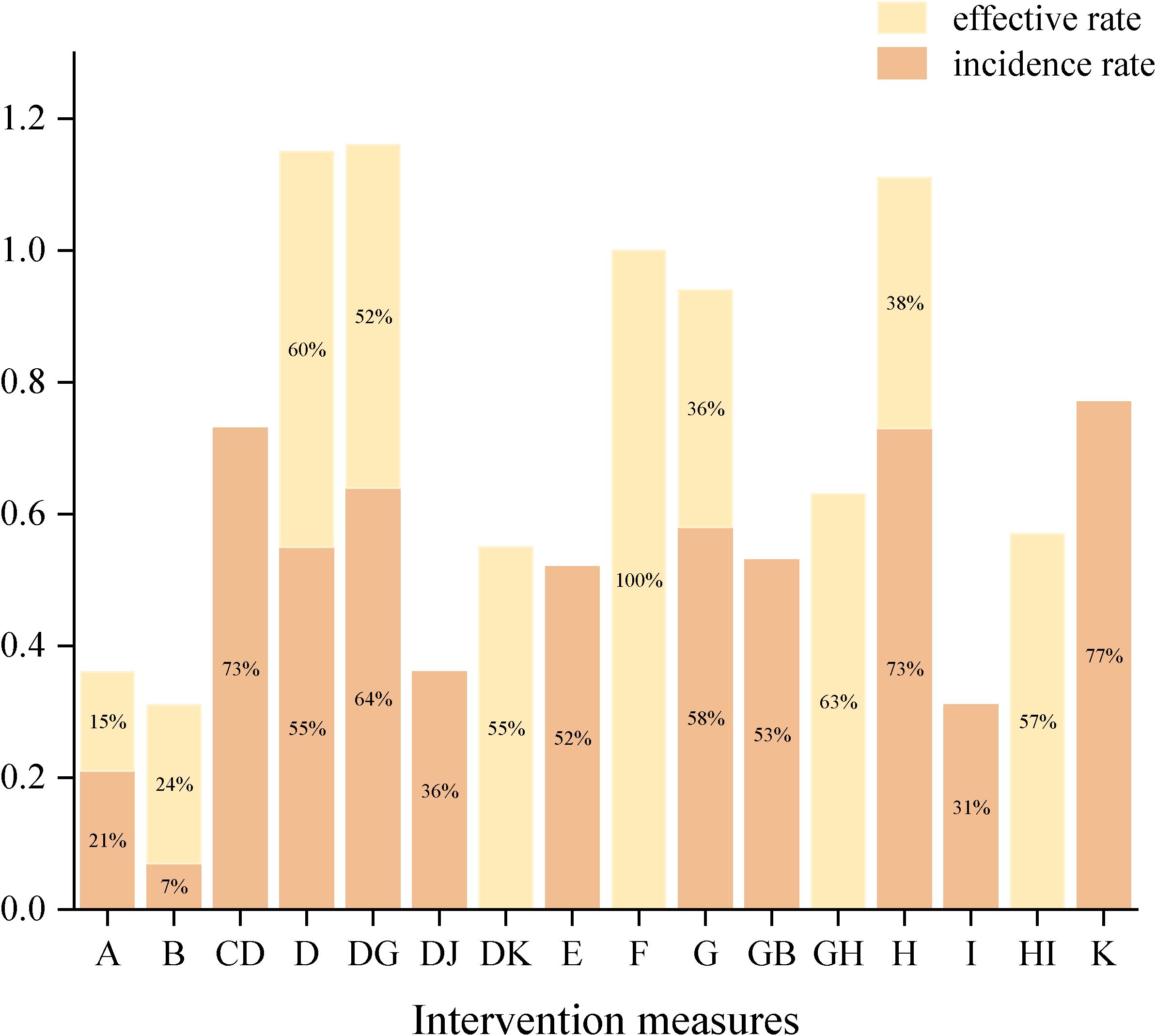
Among NPIs for reducing the incidence of constipation symptoms after treatment in lung cancer patients, only one intervention showed a statistically significant reduction in the incidence of constipation symptoms after treatment compared to the routine control group: acupoint stimulation. Compared with the laxative control group, although various NPIs showed lower incidence rates of constipation symptoms after treatment in lung cancer patients, none of these differences were statistically significant (details shown in Table 2). According to the SUCRA results, for reducing the incidence of constipation symptoms after treatment in lung cancer patients, acupoint stimulation ranked highest with a SUCRA probability of 77%, followed by ear acupuncture combined with acupoint application ranking second with a SUCRA probability of 74%, and dietary intervention ranking third with a SUCRA probability of 73%. The remaining interventions ranked as follows: acupoint application combined with massage (SUCRA=70%), massage (SUCRA=60%), acupoint application (SUCRA=54%), probiotics (SUCRA=51%), massage combined with laxatives (SUCRA=50.0%), acupoint application combined with moxibustion (SUCRA=40%), exercise (SUCRA=28%), routine care group (SUCRA=19%), and laxative group (SUCRA=6%) (see Figure 8a).
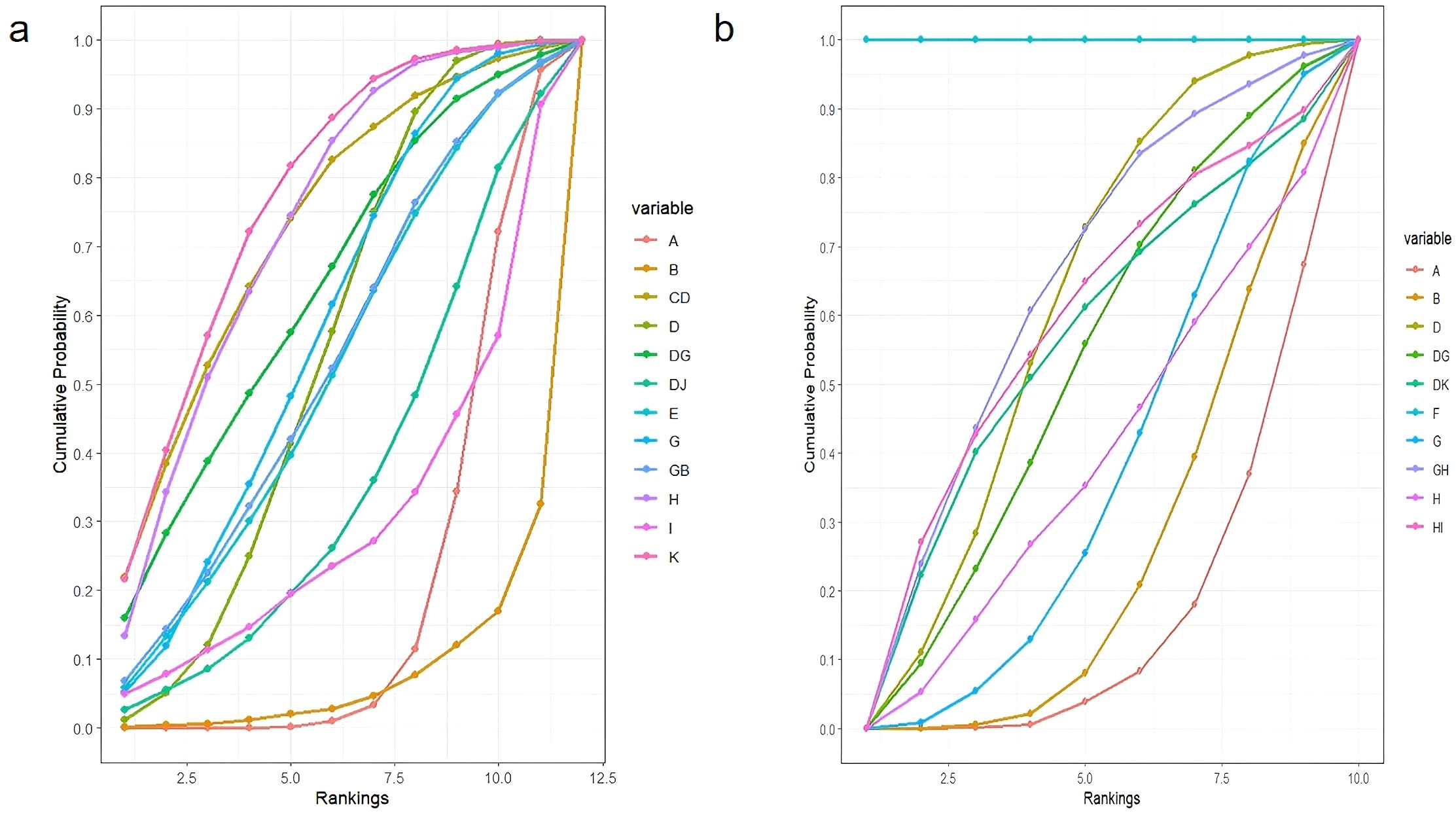
Figure 8. Ranking of SUCRA. (a) Ranking of SUCRA incidence rates; (b) Ranking of SUCRA effective rates.
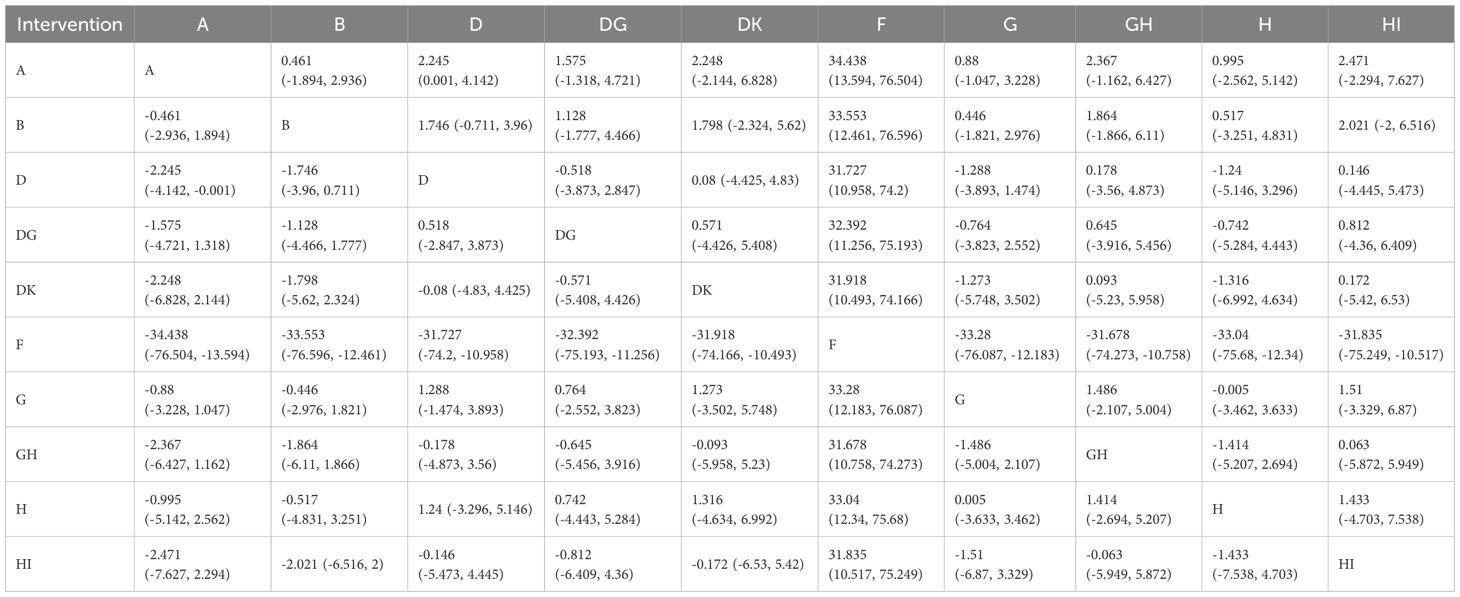
Regarding improving the effectiveness rate of constipation symptom treatment in lung cancer patients, NPIs showed significantly higher effectiveness rates than the routine control group. However, only two interventions demonstrated statistically significant differences: single acupoint application and combined use of two types of acupoint applications (detailed information shown in Table 3). For improving the effectiveness rate in treating constipation symptoms in lung cancer patients, combined use of two types of acupoint patches ranked highest (SUCRA=100%), followed by massage combined with dietary intervention, ranking second (SUCRA=61.35%), and acupoint application, ranking third (SUCRA=61.33%). The remaining interventions ranked as follows: dietary intervention combined with exercise (SUCRA=60%), acupoint application combined with acupoint stimulation (SUCRA=57%), acupoint application combined with massage (SUCRA=50%), dietary intervention (SUCRA=36%), massage (SUCRA=35%), laxatives (SUCRA=24%), and routine care (SUCRA=14.0%) (see Figure 8b).
Finally, based on SUCRA rankings across different outcome indicators, acupoint application combined with massage ranked highest overall in treating constipation symptoms in lung cancer patients (see Figure 9). It is important to note that these rankings represent treatment hierarchy based on probability estimates rather than definitive clinical superiority, and should be interpreted alongside the statistical significance of pairwise comparisons and clinical considerations.
3.6 Heterogeneity, inconsistency, and sensitivity analysis
3.6.1 Heterogeneity assessment
Potential sources of heterogeneity were systematically assessed through multiple approaches. Clinical heterogeneity was evaluated by examining study characteristics including intervention duration, sample size, intervention type. Statistical heterogeneity was assessed using I² statistics and tau² values for direct comparisons. Although these factors contributed to observed heterogeneity, subgroup analyses revealed that none significantly altered the overall network meta-analysis results or conclusions.
3.6.2 Network inconsistency assessment
Network inconsistency was rigorously evaluated using node-splitting analysis where applicable. For the incidence rate outcome, no closed loops existed in the network structure, thus inconsistency assessment was not applicable. For the effectiveness rate outcome, node-splitting analysis was performed to compare direct and indirect estimates for treatment comparisons with both types of evidence. The results showed no significant inconsistency for any comparison: D-A (P=0.8419), DG-A (P=0.816), G-A (P=0.7317), D-B (P=0.8294), DG-B (P=0.826), and G-B (P=0.7222). All P-values were well above 0.05, indicating good agreement between direct and indirect evidence and supporting the validity of our network meta-analysis assumptions (Supplementary Figure 2).
3.6.3 Sensitivity analysis
Sensitivity analyses of 31 studies for primary outcomes demonstrated robust results. Excluding any single study did not materially alter the pooled estimates (incidence rate: OR=0.16, 95%CI [0.11–0.24], P<0.01; effectiveness rate: OR=3.41, 95%CI [1.75–6.65], P<0.01; see Supplementary Tables 2, 3). The results remained robust to single-study exclusion, confirming that while high-risk studies may marginally influence effect magnitude, their impact on clinical interpretation is limited (Supplementary Figures 3, 4).
3.7 Safety and adverse events
Four randomized controlled trials (RCTs) (15, 37, 40, 42) included in this systematic review reported safety outcomes. Three studies documented specific cases of 20 adverse events, while one study reported only statistical data on adverse reaction incidence rates. The safety results for each study are detailed as follows:
Study 1 (40) (Auricular acupoint combined with acupoint application vs. routine care, total sample size n=341).
Intervention group: 6 serious adverse events (SAEs), including chylothorax (n=1), arrhythmia (n=2), deep vein thrombosis (n=1), and hypoxemia (n=1).
Control group: 3 SAEs, including arrhythmia (n=1) and hypoxemia (n=2).
Study 2 (42) (Probiotics vs. placebo, total sample size n=91)
No grade 3 or higher serious adverse events were observed.
The intervention group showed significantly lower incidence of gastrointestinal adverse reactions (nausea, vomiting, diarrhea, anorexia) compared to the control group (p<0.05). No statistically significant differences were found between groups for other adverse events.
Study 3 (15) (combined use of two types of acupoint patches vs. single acupoint application, total sample size n=106)
Intervention group: 5 adverse events, including rash (n=1), diarrhea (n=3), and abdominal pain (n=1).
Control group: 2 adverse events, including diarrhea (n=1) and nausea/vomiting (n=1).
Study 4 (37) (acupoint application vs. placebo, total sample size n=82)
Intervention group: 3 adverse events, including vomiting (n=1) and skin allergy (n=2).
Control group: 2 adverse events, including diarrhea (n=1) and vomiting (n=1).
4 Discussion
4.1 Methodological quality of included studies
This study included 30 Chinese literature papers and 3 English literature papers, of which 2 were level A evidence, and the remaining 31 were level B evidence. However, there were significant differences in heterogeneity. The English literature had a more rigorous design and relatively higher quality.
4.2 Efficacy of NPIs for constipation management in lung cancer patients
Constipation represents one of the prevalent adverse effects encountered during lung cancer treatment protocols, with an exceptionally high incidence among patients undergoing chemotherapy regimens. The clinical presentation of constipation in lung cancer patients typically encompasses a spectrum of manifestations, including defecatory difficulty, reduced stool frequency, and fecal hardening or impaction (43). From a Traditional Chinese Medicine (TCM) perspective, the pathophysiological mechanisms underlying constipation in lung cancer patients are twofold. Primarily, there exists a disruption in the exterior-interior relationship between the lungs and large intestine (known as the “biao-li” connection), resulting in compromised peristaltic function and impaired intestinal transit. Secondarily, deficiencies in vital substances—namely, qi, blood, yin, and yang—coupled with pathological accumulations of phlegm and blood stasis, contribute to dysregulated intestinal motility and aberrant bowel function (44).
4.2.1 Optimal intervention for reducing constipation incidence in lung cancer patients: acupoint stimulation
Our study demonstrates that acupoint stimulation confers significant advantages in reducing constipation incidence amongst lung cancer patients, achieving a noteworthy SUCRA ranking of 77%. These findings Optimal Intervention for Reducing Constipation Incidence in Lung Cancer Patients: Acupoint Stimulation
Our study demonstrates that acupoint stimulation confers significant advantages in reducing constipation incidence amongst lung cancer patients, achieving a noteworthy SUCRA ranking of 77%. These findings correspond with the theoretical framework of “meridian theory” in Traditional Chinese Medicine, which postulates that acupoint stimulation modulates gastrointestinal function via specific energetic pathways. Contemporary biomedical research has elucidated the physiological mechanisms underpinning this therapeutic approach: stimulation of acupoints such as “Zusanli” facilitates activation of the vagal-enteric neural axis, promoting secretion of gastrointestinal peptide hormones and enhancing colonic peristalsis. Research indicates that stimulation of the “Neiguan” and “Zusanli” acupoints significantly reduces the incidence of constipation in lung cancer patients receiving chemotherapy. The underlying mechanism may be associated with inhibiting 5-HT3 receptor hyperactivation and attenuating intestinal water reabsorption (41, 45). Furthermore, acupoint stimulation demonstrates pronounced safety advantages, circumventing adverse effects of pharmacological interventions such as lactulose, including electrolyte disturbances and melanosis coli (46). This therapeutic approach is particularly advantageous for lung cancer patients with concomitant comorbidities or compromised pharmacological tolerance. the theoretical framework of “meridian theory” in Traditional Chinese Medicine, which postulates that acupoint stimulation modulates gastrointestinal function via specific energetic pathways. Contemporary biomedical research has elucidated the physiological mechanisms underpinning this therapeutic approach: stimulation of acupoints such as “Zusanli” facilitates activation of the vagal-enteric neural axis, promoting secretion of gastrointestinal peptide hormones and enhancing colonic peristalsis. Research indicates that stimulation of the “Neiguan” and “Zusanli” acupoints significantly reduces the incidence of constipation in lung cancer patients receiving chemotherapy. The underlying mechanism may be associated with inhibiting 5-HT3 receptor hyperactivation and attenuating intestinal water reabsorption (41, 45). Furthermore, acupoint stimulation demonstrates pronounced safety advantages, circumventing adverse effects of pharmacological interventions such as lactulose, including electrolyte disturbances and melanosis coli (46).This therapeutic approach is particularly advantageous for lung cancer patients with concomitant comorbidities or compromised pharmacological tolerance.
4.2.2 Optimal intervention for enhancing constipation treatment efficacy: two types of acupoint patches combined
This study indicates that combined use of two types of acupoint patches can significantly improve the treatment effect of constipation (SUCRA=100%). Research has confirmed that the combination of compound clove appetizing patch and traditional Chinese medicine acupoint patch can significantly improve the treatment effect of constipation in lung cancer patients. The underlying mechanism involves multi-pathway regulation: acupoint patches facilitate transdermal absorption of pharmacologically active constituents (such as rhubarb and borneol), directly stimulating the enteric neural plexus, while clove constituents ameliorate nausea and enhance gastrointestinal motility (15). However, the anomalously elevated SUCRA value may stem from zero-event bias attributable to the limited sample size (intervention cohort comprising merely 53 subjects, all demonstrating symptomatic improvement). Validation necessitates expanded cohort dimensions, incorporating objective parameters such as fecal short-chain fatty acid concentrations and implementing standardized protocols to establish treatment stability. This modality may be clinically recommended as second-line therapy; however, acupoint selection should be predicated upon syndrome differentiation principles with periodic efficacy assessments.
4.2.3 Most effective overall intervention: acupoint application combined with acupoint massage
The findings of this study demonstrate that the combination of acupoint application and acupoint massage exhibits comprehensive advantages in reducing constipation incidence (SUCRA=67%) and improving treatment efficacy (SUCRA=50%) among lung cancer patients. This combined approach harnesses the synergistic effects of transdermal drug absorption and physical stimulation, offering dual benefits in managing constipation in lung cancer patients. On the one hand, the applied medications (such as rhubarb and borneol) are absorbed through the skin and directly stimulate the intestinal plexus, activating cholinergic neurons in the myenteric plexus of the intestinal wall. This promotes colonic motility while simultaneously regulating gastrointestinal hormone secretion, creating a “local-systemic” dual regulatory effect that effectively prevents constipation (47). On the other hand, acupoint massage (targeting points such as “Tianshu” and “Zhongwan”) activates the “vagus” nerve-gut brain axis through mechanical stimulation, enhancing parasympathetic excitability and improving local microcirculation. This provides energy support for intestinal peristalsis, effectively treating constipation (48). This synergistic “chemical stimulation + physical stimulation” model aligns with the Traditional Chinese Medicine theory of “acupoint synergistic enhancement.” For instance, the combined use of “Tianshu” acupoint (the alarm point of the large intestine) and “Shenque” acupoint (a crucial point on the Conception Vessel) provides direct access to intestinal pathologies, while the pairing of “Zusanli”: (the uniting point of the Stomach meridian) with “Shangjuxu” (the lower uniting point of the Large Intestine) exemplifies the classical principle of “treating internal organs through uniting points.” Modern research further corroborates that combining acupuncture and abdominal massage can significantly reduce colonic transit time, with efficacy superior to acupuncture alone. This suggests that physical stimulation can amplify the regulatory effects of acupuncture therapy.
Furthermore, this combined therapy demonstrates high safety, making it particularly suitable for lung cancer patients with comorbid cardiovascular diseases or poor drug tolerance. Its operational simplicity also enhances patients’ willingness for self-management. In clinical practice, this combined approach is recommended as a core intervention, especially for chemotherapy prevention, patients with poor response or intolerance to laxatives, and long-term intestinal management in elderly or frail patients. Implementation requires a TCM practitioner to select acupoints based on syndrome differentiation, adjust stimulation intensity dynamically according to patient feedback, and assess efficacy and safety regularly.
Although NPIs demonstrate numerical advantages over laxatives in reducing constipation incidence and improving efficacy, some differences did not reach statistical significance. This may be directly related to the mechanism of laxatives (such as polyethylene glycol and lactulose), which rapidly increase intestinal volume through osmotic effects.
However, NPIs offer significant advantages in terms of safety and patient tolerance in the short term. Methods such as acupoint stimulation and massage carry no risk of drug accumulation, demonstrate better patient acceptance, and can simultaneously address comorbidities such as anxiety, aligning with the “bio-psycho-social” medical model. The “Chinese Expert Consensus on Prevention and Treatment of Cancer Drug-Related Nausea and Vomiting (2019 Edition)” also explicitly recommends incorporating NPIs into supportive care for cancer patients to reduce drug-related adverse effects (49).
4.3 Advantages, limitations, and outlook
4.3.1 Advantages
1. Safety and Adherence: NPIs (such as acupoint stimulation and massage) carry no risk of drug accumulation and offer superior patient tolerance, making them particularly suitable for individuals with underlying conditions or drug intolerances.
2. Comprehensive Benefits: These interventions can simultaneously improve comorbidities such as anxiety and fatigue (e.g., reduction in SAS scores, SMD=-2.41), aligning with the “bio-psycho-social” medical model. They have been recommended in the “Chinese Expert Consensus on Prevention and Treatment of Cancer Drug-Related Nausea and Vomiting (2019 Edition)”.
3. Robustness of Efficacy: Sensitivity analysis indicates that excluding any single study does not alter the pooled results, suggesting high credibility of the findings.
4.3.2 Limitations
1. Sample Size and Intervention Diversity: The included studies had relatively small sample sizes and diverse intervention types, limiting the generalizability and interpretability of results.
2. Significant Heterogeneity: Intervention duration, sample size, and intervention type (e.g., single vs. combined interventions) represented the primary sources of heterogeneity, potentially affecting result interpretation. Furthermore, the scope of interventions examined in this study was limited and did not encompass all potential non-pharmacological methods. Critically, due to the absence of detailed reporting on lung cancer histological subtypes, TNM staging, and constipation severity in the included studies, we were unable to conduct subgroup analyses to explore their impact—this represented a significant additional contributor to the observed heterogeneity.
3. Quality of Evidence: Most included studies were graded as level B. The CINeMA tool assessment indicated relatively low evidence grades for most comparisons between NPIs, suggesting limited reliability (Details can be found in Supplementary Tables 2, 3).
4. Short-term Focus: Existing research predominantly focuses on short-term efficacy observations, lacking long-term effect assessments, while the long-term efficacy of specific interventions remains unclear.
5. Cultural Context and Generalizability: A significant proportion of included studies were conducted in East Asian countries where traditional Chinese medicine (TCM) interventions are commonly integrated with conventional care. The cultural acceptance, implementation mechanisms, and effectiveness of these TCM-based approaches may differ substantially in Western healthcare settings, where such practices face different regulatory frameworks, professional acceptance, and patient expectations. This cultural specificity may limit the direct applicability of findings to diverse global healthcare contexts.
4.3.3 Future directions
Future research should expand sample sizes and increase the number of studies to enhance the persuasiveness of evidence. Additionally, intervention design and implementation should be further optimized, with standardized operational protocols established to reduce the impact of heterogeneity on research outcomes. Moreover, broadening the scope of NPIs to explore more comprehensive treatment options while strengthening long-term efficacy and cost-effectiveness assessments will help provide more thorough and meaningful treatment recommendations for clinicians and patients.
5 Conclusion
This systematic review confirms that combined acupoint application and massage significantly reduce constipation incidence and improve symptoms in lung cancer patients, with superior efficacy compared to single interventions, demonstrating short-term clinical value.
However, critical limitations exist: included studies had extremely short follow-up periods (median ≤1 month), small sample sizes, and complete absence of long-term efficacy and safety data, severely restricting clinical generalizability. Therefore, current results support these interventions only as short-term adjuncts to pharmacological therapy. Clinical practice should involve: carefully developing individualized protocols that prioritize measures with established long-term safety, and avoiding extrapolation of short-term benefits to long-term management while monitoring for delayed adverse effects.
Future research requires large-scale randomized controlled trials (with ≥5 years follow-up), enhanced methodology (blinding, standardized outcomes), and health economic evaluations to validate long-term effectiveness and cost-effectiveness, ultimately providing high-quality evidence for personalized constipation management in lung cancer patients.
Data availability statement
The original contributions presented in the study are included in the article/Supplementary Material. Further inquiries can be directed to the corresponding author.
Author contributions
MC: Writing – original draft, Writing – review & editing, Data curation, Formal Analysis, Methodology, Software. JY: Data curation, Methodology, Software, Writing – review & editing. XF: Project administration, Writing – review & editing. YL: Validation, Writing – review & editing. LH: Visualization, Writing – review & editing. YX: Supervision, Writing – review & editing.
Funding
The author(s) declare financial support was received for the research and/or publication of this article. This study was supported by Project of Jiangxi Provincial Administration of traditional Chinese Medicine (2024A0023) and Jiangxi High-level Undergraduate Teaching Team (TCM Nursing Undergraduate Teaching Team).
Acknowledgments
We would like to thank all the authors of this study for their contributions and dedication to this research.
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Generative AI statement
The author(s) declare that no Generative AI was used in the creation of this manuscript.
Publisher’s note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
Supplementary material
The Supplementary Material for this article can be found online at: https://www.frontiersin.org/articles/10.3389/fonc.2025.1633167/full#supplementary-material
References
1. Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, et al. Global cancer statistics 2020: globocan estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. (2021) 71:209–49. doi: 10.3322/caac.21660
2. Wei W, Zeng H, Zheng R, Zhang S, An L, Chen R, et al. Cancer registration in China and its role in cancer prevention and control. Lancet Oncol. (2020) 21:e342–49. doi: 10.1016/S1470-2045(20)30073-5
3. Dong D, Yiheng H, Yajie Z, and Hecheng L. Chinese medical association guideline for clinical diagnosis and treatment of lung cancer(2023 edition):an interpretation. Chin J Clin Thorac Cardiovasc Surg. (2023) 30:1533–38. doi: 10.16781/j.CN31-2187/R.20240697
4. Wenjing L, Yaping G, and Rong W. Investigation of postoperative constipation in patients with lung cancer and analysis of its influencing factors. Int J Nurs. (2024) 43:2310–14. doi: 10.3760/cma.j.cn221370-20230908-00541
5. Pope JL, Tomkovich S, Yang Y, and Jobin C. Microbiota as a mediator of cancer progression and therapy. Transl Res. (2017) 179:139–54. doi: 10.1016/j.trsl.2016.07.021
6. Yubing H and De Pangher V. Construction and application of lung cancer of breakthrough cancer pain management schem based on symptom theory (master's thesis)., Henan University. (2023). doi: 10.27114/d.cnki.ghnau.2023.001653
7. Ying Z. Research progress on cough symptom management in patients with lung cancer. Cardiovasc Dis Electronic J Integrated Traditional Chin Western Med. (2019) 7:26–7. doi: 10.16282/j.cnki.cn11-9336/r.2019.30.015
8. Higgins JPT, Altman DG, Gotzsche PC, Juni P, Moher D, Oxman AD, et al. The cochrane collaboration’s tool for assessing risk of bias in randomised trials. Bmj. (2011) 343:d5928. doi: 10.1136/bmj.d5928
9. Nikolakopoulou A, Higgins JPT, Papakonstantinou T, Chaimani A, Del Giovane C, Egger M, et al. Cinema: an approach for assessing confidence in the results of a network meta-analysis. PloS Med. (2020) 17:e1003082. doi: 10.1371/journal.pmed.1003082
10. Jingxiu C, Yuanling F, and Jushan H. Nursing effect of intestinal function training combined with simulated defecation training to prevent constipation after radical operation of lung cancer. J Baotou Med Coll. (2021) 37:19–23. doi: 10.16833/j.cnki.jbmc.2021.11.005
11. Yao S. Observation on the nursing effect of intestinal function training combined with simulated defecation training in preventing constipation after radical resection for lung cancer. Tangniaobing Zhiyou. (2023) 5):236–37.
12. Xiao Q. Clinical observation on the treatment of constipation caused by lung cancer chemotherapy at shangqu point with rhubarb. Electronic J Clin Med Literature. (2019) 6:152–59. doi: 10.16281/j.cnki.jocml.2019.76.118
13. Xiaofang Q, Shuping X, and Xi Y. Observation on the efficacy of rhubarb acupoint plaster combined with salt-isolated moxibustion in treating constipation in patients with lung cancer undergoing chemotherapy. Med Inf. (2017) 30:180–81. doi: 10.3969/j.issn.1006-1959.2017.01.119
14. Yanyan X, Jia Z, Keli Y, Shudi J, Yue Y, and Jie J. Effect of intestinal rehabilitation training on chemotherapy-related constipation in patients with lung cancer. J Nurs Sci. (2019) 34:55–7. doi: 10.3870/j.issn.1001-4152.2019.03.054
15. Danfeng L, Lan Z, and Hongmin Z. The effect of fufang dingxiang kaiwei tie combined with acupoint application of chinese medicine in the treatment of constipation of lung cancer patients. Shaanxi J Traditional Chin Med. (2018) 39:1375–77. doi: 10.3969/j.issn.1000-7369.2018.10.018
16. Xiaoping L, Yongyi C, Yongchang Z, Jie L, and Xuying L. Preventive effect of compound polyethylene glycol electrolyte powder combined with abdominal massage on cisplatin-induced constipation of lung cancer patients. Anti-Tumor Pharm. (2017) 7:441–45. doi: 10.3969/j.issn.2095-1264.2017.04.12
17. Guohua F, Xingxiang X, Lingfeng M, Jingyun S, and De Pangher V. Clinical effects of abdomen massage combined with dialectic meal on the treatment of constipation in lung carcinoma patients after chemotherapy. Chin J Lung Disease(Electronic Edition). (2017) 10:445–49. doi: 10.3877/cma.j.issn.1674-6902.2017.04.017
18. Ying C and Limin H. Abdominal massage combined with acupoint application in prevention of constipation. J Clin Nurs Pract. (2018) 4:49–51. doi: 10.27114/d.cnki.ghnau.2023.001653
19. Yuxian W, Hongwu K, Jingjing Du, Baisheng X, Jun W, and Yong Y. The observation of the effect of abdominal massage combined with acupoint-application. China Modern Doctor. (2020) 58:166–69.
20. Yuzhen Y. Experience on the impact of personalized diet care on constipation in elderly lung cancer patients after chemotherapy. Diet Health. (2019) 6:140.
21. Ying Z and Jing L. Observation on the effect of percutaneous acupoint electrical stimulation in preventing constipation in lung cancer patients after chemotherapy. Int J Nurs. (2019) 38:2786–88. doi: 10.3760/cma.j.issn.1673-4351.2019.17.031
22. Yinping F, Lingyong C, and Zhouhua H. Observation on the therapeutic effect of mirabilite acupoint application in treating constipation caused by analgesic drugs in patients with lung cancer. Yi Yao Wei Sheng. (2021) 8):61–2.
23. Yun JL, Hongtao L, Qiaoling Z, Rong L, and Guijuan Z. Research on the application of camellia oil combined with medical exercises in chemotherapy-induced constipation in lung cancer patients. Nei Meng Gu Yi Xue Za Zhi. (2024) 56:1015–17. doi: 10.16096/J.cnki.nmgyxzz.2024.56.08.027
24. Jie L. The effect of specific acupuncture point application with acupoint application and acupoint massage on improving constipation in patients with advanced lung cancer. China Health Care Nutr. (2021) 31:13.
25. Huilian L. Application of acupoint application with xiao yuzi oil meridian flowing combined with traditional chinese medical nursing in prevention of constipation caused by aoshikangding. Chin Nurs Res. (2016) 30:1333–36. doi: 10.3969/j.issn.1009-6493.2016.11.015
26. Huiping X. The prevention effect of acupuncture point massage on constipation caused by opioid drugs. Military Nurs. (2015) 32:71–3. doi: 10.3969/j.issn.1671-5217.2018.08.153
27. Liu Y. The preventive and therapeutic effects of acupoint massage on constipation caused by opioid drugs in patients with lung cancer. Bao Jian Wen Hui. (2018) 8):152. doi: 10.3969/j.issn.1671-5217.2018.08.153
28. Weihua T. Analysis of prevention and treatment effect of acupoint massage on constipation caused by opioids in patients with lung cancer. Biped Health. (2019) 28:40–1. doi: 10.19589/j.cnki.issn1004-6569.2019.15.040
29. Xuemei B. Acupoint massage for preventing constipation after lung cancer chemotherapy: 93 cases. Zhejiang J Traditional Chin Med. (2009) 44:38. doi: 10.27114/d.cnki.ghnau.2023.001653
30. Youfang Y. The application effect of acupoint massage in preventing constipation after lung cancer chemotherapy. Modern Nurse. (2012) 07):133–34. doi: 10.3969/j.issn.1006-6411.2012.07.082
31. Ran L, Yang L, and Wenjing L. Observation on the efficacy of acupoint pressing method in treating constipation in lung cancer patients undergoing chemotherapy. Chin Gen Pract Nurs. (2014) 12:2853–54. doi: 10.3969/j.issn.1674-4748.2014.30.43
32. Mengmeng L, Bo Z, and Yaqin Y. Clinical observation on the prevention of constipation after lung cancer chemotherapy by applying a small amount of gold paste to shenque acupoint. World Latest Med Inf. (2016) 16:183–279. doi: 10.3969/j.issn.1671-3141.2016.94.158
33. Yuqing Y and De Pangher V. Research about dietary intervention for constipation of patients with lung cancer when cured by chemotherapy. Chin J Pract Nurs. (2010) 26:6–07. doi: 10.3760/cma.j.issn.1672-7088.2010.02.040
34. Danhua L and Hong Z. Observation on the effect of traditional chinese medicine applied to the abdominal center combined with pinching needling in the treatment of patients with lung cancer undergoing postoperative chemotherapy and constipation. Chin J Traditional Med Sci Technol. (2023) 30:541–43.
35. Yinxia T, Yan W, Ping W, Chunlan Z, Guijun L, Lihua L, et al. Effect of acupoint sticking therapy with chinese herbals on chemotherapy-induced gastrointestinal symptoms in patients with advanced lung cancer. J Nurs Sci. (2019) 34:49–51. doi: 10.3870/j.issn.1001-4152.2019.03.048
36. Xueyun X, Qi A, Yujuan Z, and Xiao Y. Clinical observation on constipation in lung cancer patients taking opioids by chinese medicine acupoint application. Capital Food Med. (2024) 31:129–31. doi: 10.3969/j.issn.1005-8257.2024.14.043
37. Liang M, Ying Z, Baoxia Z, Lanhui Z, and Wenqing L. Application of acupoint patch therapy at shenque point for treating advanced lung cancer with opioid-induced constipation: 41 cases. J Shaanxi Univ Chin Med. (2022) 45:93–6. doi: 10.13424/j.cnki.jsctcm.2022.02.021
38. Zhuwen Z, Xiaojuan Z, and Yaping T. Applicated effect of self -made dahuang paste on preventing bloating and constipation after lung cancer endoscopic surgery. Chin J Primary Med Pharm. (2018) 25:1943–46. doi: 10.3760/cma.j.issn.1008-6706.2018.15.011
39. Wei H, Lijin R, and Chunyan L. Effect of self-made ronghuang catharsis umbilical paste on constipation in patients with Malignant tumor. J Nurs Sci. (2017) 32:41–2. doi: 10.3870/j.issn.1001-4152.2017.15.041
40. Li Y, Qi D, Gong L, Qu H, Xu B, Wen X, et al. Effect of auricular points treatment combined with acupoints application in patients with constipation after lung cancer surgery. J Cancer Res Ther. (2017) 13:844–48. doi: 10.4103/jcrt.JCRT_709_17
41. Mao T, Cheng Q, Liu X, and Chen Y. Effect of electrical stimulation on gastrointestinal symptoms in lung cancer patients during chemotherapy: a randomized controlled trial. Asia Pac J Oncol Nurs. (2021) 8:246–54. doi: 10.4103/apjon.apjon_61_20
42. Wei H, Yue Z, Han J, Chen P, Xie K, Sun Y, et al. Oral compound probiotic supplements can improve the quality of life for patients with lung cancer during chemotherapy: a randomized placebo-controlled study. Thorac Cancer. (2024) 15:182–91. doi: 10.1111/1759-7714.15177
43. Chen H, Gu X, Zhang Y, Feng J, and Gu Y. Associated factors with constipation and health-related quality of life in lung cancer patients with platinum-based chemotherapy: a cross-sectional study. Med (Baltimore). (2021) 100:e26547. doi: 10.1097/MD.0000000000026547
44. Li Y, Zhai H, and Yang C. Research on the theory of “ lung and large intestine connecting externally and internally. J Basic Chin Med. (2024) 30:336–41. doi: 10.19945/j.cnki.issn.1006-3250.2024.02.032
45. Zhang R, Huang C, Wu F, Fang K, Jiang S, Zhao Y, et al. Review on melanosis coli and anthraquinone-containing traditional chinese herbs that cause melanosis coli. Front Pharmacol. (2023) 14:1160480. doi: 10.3389/fphar.2023.1160480
46. Neyrinck AM, Rodriguez J, Taminiau B, Herpin F, Cani PD, Daube G, et al. Constipation mitigation by rhubarb extract in middle-aged adults is linked to gut microbiome modulation: a double-blind randomized placebo-controlled trial. Int J Mol Sci. (2022) 23:14685. doi: 10.3390/ijms232314685
47. Ong SS, Tang T, Xu L, Xu C, Li Q, Deng X, et al. Research on the mechanism of core acupoints in electroacupuncture for functional constipation based on data mining and network acupuncture. Front Med (Lausanne). (2024) 11:1482066. doi: 10.3389/fmed.2024.1482066
48. Ziwei L. Observation on the clinical curative effect of acupuncturecombined with acupuncture at shu and mu points andabdominal massage in the treatment of (qi stagnationtype)slow transit const[Master]. China: Fujian University of Chinese Medicine (2022).
Keywords: lung cancer, constipation, non-pharmacological intervention, NMA (network meta-analysis), systematic review
Citation: Cai M, Yin J, Fang X, Li Y, Hu L and Xu Y (2025) The efficacy of non-pharmacological interventions for treating constipation symptoms in lung cancer patients: a systematic review and network meta-analysis. Front. Oncol. 15:1633167. doi: 10.3389/fonc.2025.1633167
Received: 22 May 2025; Accepted: 25 July 2025;
Published: 18 August 2025.
Edited by:
Run-Qi Guo, Chinese Academy of Medical Sciences, ChinaReviewed by:
Adnan Lakdawala, George Washington University, United StatesSabyasachi Mohanty, University of Nebraska-Lincoln, United States
Copyright © 2025 Cai, Yin, Fang, Li, Hu and Xu. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Yiyong Xu, eHV5aXlvbmcyMDA3QDEyNi5jb20=
†These authors have contributed equally to this work
 Mian Cai
Mian Cai Jie Yin
Jie Yin Xiwei Fang
Xiwei Fang Yanjing Li2
Yanjing Li2 Yiyong Xu
Yiyong Xu