- 1Department of Pediatrics, University of California San Diego, San Diego, CA, United States
- 2Rady Children's Hospital, San Diego, CA, United States
Background and aim of the study: We previously published the increased frequency of new CPP cases during the Covid-19 pandemic in our pediatric endocrinology clinic at Rady Children's Hospital in San Diego, CA, US. We conducted this follow-up study to examine the incidence of new CPP cases requiring treatment with GnRH agonist (GnRHa) in our clinic during 2 years post-pandemic.
Methods: We performed a retrospective comparison of the number of visits of children newly diagnosed with CPP treated with GnRHa during the 2 years following the first year of Covid-19 pandemic (5/2021–7/2023). We evaluated clinical and bone maturation data as well as differences in timing from diagnosis to onset of treatment.
Results: We previously reported in the pre-Covid year, 28 children (1 boy, 27 girls) treated with GnRHa for CPP out of 2,340 new endocrinology visits (1.2% of patients seen). During Covid-19 year, 64 children (7 boys, 57 girls) were treated out of 2,261 new visits (2.8%). The incidence of new CPP cases requiring GnRHa during the pandemic more than doubled compared to pre-pandemic. In the first year post-year 1 of the pandemic (5/2021–4/2022), 46 children (3 boys, 40 girls) started treatment with GnRHa for CPP out of 2,595 new endocrinology visits (1.6% of patients seen). During the second follow-up year (5/2022–4/2023), 22 children (4 boys, 18 girls) started treatment with GnRHa for CPP out of 2,676 new endocrinology visits (0.8% of patients seen). Age at onset of treatment, degree of bone age (BA) advancement, time from diagnosis to onset of treatment, and changes in BMI during the pandemic were not different from pre-pandemic or post-pandemic.
Conclusions: CPP cases requiring GnRHa treatment significantly increased during the first year of the Covid-19 pandemic and then decreased each year post-pandemic. This was not related to BMI, age at diagnosis, degree of bone age advancement, or time from diagnosis to onset of treatment as all these factors have been similar during pre-pandemic, pandemic, and post-pandemic years. It is reasonable that the postulated hypotheses published regarding the increase during the pandemic would resolve post-pandemic.
Introduction
We and others previously reported an increase in cases of CPP during the first year of Covid-19 (1–9). To evaluate if this trend continued further into or post-pandemic, we conducted this follow-up study to assess whether the incidence of CPP cases in years post-pandemic continued at the increased rate or returned to pre-pandemic rates. Despite ample evidence that CPP cases increased during the pandemic, the mechanisms for this change in incidence are not yet well understood and many hypotheses remain unexplained. Most hypotheses link the increased incidence to either a direct effect of SARS-CoV-2 infection, or to factors associated with the change in lifestyle and associated emotional and physical changes induced by social isolation during the pandemic. Understanding trends post-Covid-19, may bring insight into those hypotheses and help target areas for research.
Methods
Study design and setting
We performed a single-center retrospective comparison of the incidence of newly diagnosed children with CPP requiring GnRHa treatment pre-Covid-19 year (5/2018–4/2019), during the Covid-19 pandemic (5/2020–4/2021) and 2 years post-Covid-19 (5/2021–4/2022, and 5/2022–4/2023). The study was conducted at a free-standing, tertiary care academic children's hospital and pediatric endocrinology specialty outpatient clinic in San Diego, California. Patients with suspected CPP are referred to endocrinology clinic by general pediatricians and other subspecialists practicing in the San Diego County and surrounding areas. Subjects were identified by electronic medical record (EMR) query (Epic Systems Corporation, Verona, Wisconsin). A new diagnosis of CPP was defined as having all of the following: (1) at least 1 endocrinology clinic visit associated with one of the following 4 CPP ICD codes: early puberty, premature thelarche, precocious puberty, or central precious puberty; (2) chronological age <8 years for girls and <9 years for boys at onset of symptoms; (3) a random luteinizing hormone (LH) level >0.3 IU/L (10), or a GnRH-stimulated peak LH level >5 IU/L (11), or a GnRH-stimulated estradiol >40 pg/ml in girls (12, 13) or testosterone >30 ng/dl in boys (13). GnRHa stimulation tests were performed by administering aqueous leuprolide acetate subcutaneously, at a standard dose of 20 mcg/kg (maximum dose 500 mcg). Blood samples were obtained at 1 h for measurement of LH level and at 18–24 h for measurement of estradiol in girls or testosterone in boys. In addition, only patients who received GnRHa treatment were included to eliminate the potential for borderline cases meeting diagnostic criteria but not deemed necessary to treat. Date of diagnosis was defined by date of confirmatory blood test. Patient characteristics and outcome variables were obtained by EMR query and manual chart review (KK, MVT). Bone age assessment was done according to the atlas of Greulich and Pyle (14) and determined by the patient's endocrinologist. The University of California San Diego (UCSD) Institutional Review Board approved this study, and a waiver of informed consent was granted for the collection.
Descriptive analysis used means ± standard deviation (SD). Chi-square was used for comparing proportions of newly diagnosed patients with CPP during different years. Two-tailed Student T-tests were used to compare variables of retrospective data.
The primary outcome measure was the proportion of endocrinology visits associated with new CPP diagnosis and GnRHa treatment during the 2 years post an initial year of Covid-19 pandemic compared to the pre-pandemic and pandemic period. We evaluated bone age (BA), BMI, time from diagnosis to GnRHa order, and time from GnRHa order to first day of treatment. GnRHa included leuprolide, triptorelin, and histrelin. First day of GnRHa treatment was captured by the date of the first endocrinology nurse visit for GnRHa administration or day of insertion for the patient receiving histrelin implant.
Analysis
Between groups. We obtained the data regarding Covid-19 cases per month in California and in San Diego County from Government data (15, 16) for children under 18 years of age. San Diego infection rates paralleled those of California, so California data was used for more robust statistics and divided by 3,000 for visual scaling.
Results
Incidence of patients diagnosed with CPP and treated with GnRHa
There were 2,340 new patients seen in our endocrinology clinic during pre-Covid-19 year (5/2019–4/2019), including all chief complaints. Of these, 28 children (1 boy, 27 girls) were diagnosed with CPP and treated with GnRHa (1.2% of patients seen). During Covid-19 year (5/2020–4/2021), 64 children (7 boys, 57 girls) were diagnosed with CPP and treated with GnRHa, out of 2,261 new visits (2.8% of patients seen). In the first year post-year 1 of the pandemic (5/2021–4/2022), 43 children (3 boys, 40 girls) started treatment with GnRHa for CPP out of 2,595 new endocrinology visits (1.6% of patients seen). During the following year (5/2022–4/2023), 22 children (4 boys, 18 girls) started treatment with GnRHa for CPP out of 2,676 new endocrinology visits (0.8% of patients seen).
The incidence of new CPP cases requiring GnRHa more than doubled during Covid compared to the pre-Covid years (p < 0.01, Chi Square) and decreased to pre-covid rates over 2 subsequent years.
Patient demographics
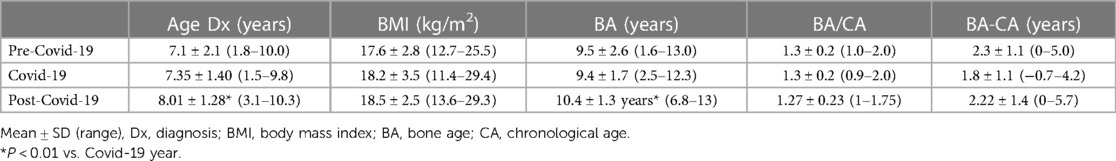
Onset of puberty was less than 8 years for all girls and less than 9 years for all boys. The mean age at diagnosis was 7.1 ± 2.1 (1.8–10.0) years in pre-Covid-19 years, 7.6 ± 1.43 (1.5–10.5) (7.3 ± 1.4 for girls, 6.5 ± 2.4 for boys) years during Covid-19 year, and significantly higher at 8.12 ± 1.4 (2.6–10.6) (8.0 ± 1.3 for girls, 9.5 ± 0.8 for boys) years over 2 years post covid (p = 0.0004 and p = 0.01 for girls, p < 0.05 for boys). BMI in pre-Covid-19 years was 17.6 ± 2.8 kg/m2 (12.7–25.5), 18.2 ± 3.5 kg/m2 (11.4–29.4) during Covid-19, and 18.5 ± 2.5 kg/m2 (13.6–29.3) over 2 years post covid (similar for girls and boys. Bone age at diagnosis was 9.5 ± 2.6 y (1.6–13.0) in the pre-Covid-19 year, 9.5 ± 1.7 y (2.5–12.6) in the Covid-19 year, and 10.6 ± 1.4 y (6.8–13) (10.4 ± 1.3 for girls, 11.9 ± 1.2 for boys) over the 2 years post-Covid-19, consistent with increasing CA over the years. When corrected for CA (chronological age), BA/CA and BA-CA did not show a statistical significance between the different study periods. Increasing age and bone age was not influenced by the number of boys included each year. Table 1 presents only girls for consistency (Table 1).
Days from diagnosis to treatment order and to start of treatment
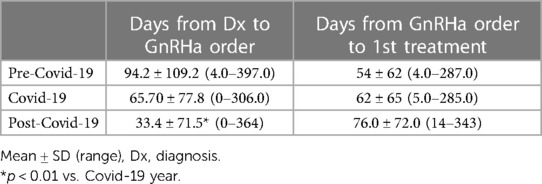
Average time from diagnosis to GnRHa order was 94.2 ± 109.2 (4.0–397.0) days and average time from GnRHa order to first injection was 54 ± 62 days pre-covid 19. During Covid-19, the average time was 65.70 ± 77.8 (0–306) days between diagnosis and GnRHa order, and 62 ± 65 days between GnRHa order and treatment onset. In the 2 years post-covid the average time from diagnosis to GnRHa order was much shorter (p = 0.002) with a range of 33.3 ± 71.5 (0–364) and from order to treatment was similar at 76 ± 72 (14–343) days. The time range is broad for all years (Table 2).
CPP incidence and COVID-19 peaks in the community
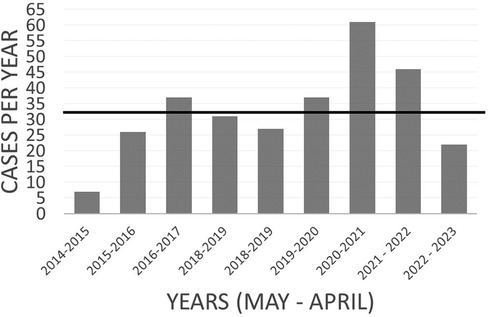
We previously reported the number of cases per month appeared to increase approximately 5–6 months after the highest peak of Covid-19 cases at the time in January 2021, however after an even greater peak in Covid-19 cases in January 2022, there was an apparent rise in CPP cases 6 months later, but to a lesser degree (5 cases in 2022 vs. 11 cases in 2021) although the percent of cases for the year was similar (Figure 1). Thirty two out of 64 cases (50%) were started on treatment in the 3 months between May and July 2021 and 20 of 46 cases (43%) between May and July 2022.
Discussion
The number of cases of CPP requiring treatment with GnRHa more than doubled during the first year of Covid-19 compared to prior years, and rates dropped again to previous numbers post Covid-19 pandemic.
Time from diagnosis to onset of treatment was similar in the 1st year of Covid-19 compared to pre-Covid-19, but decreased post-covid-19 pandemic. This may be related to increased support from pharmacy technicians at our institution, and potentially, a faster response for authorization from insurance companies. Additionally, time to onset of treatment might have been longer during the pandemic due to higher volume of patients. In our study, BMI was similar for both groups, so the higher incidence of CPP during the pandemic is unlikely to be related to nutrition or weight gain.
Bone age advancement was not different between the Covid-19 pandemic and post-pandemic timeframes, suggesting there was no delay in presentation for medical care during Covid-19 at our institution. In contrast, however, age at diagnosis was significantly higher post-covid, which is an unexpected finding as one would infer access to healthcare was easier during the post-pandemic period, although access at our center didn't seem to be affected based on our data. However, some patients and families might have delayed medical attention during and immediately after the pandemic, thus presenting at an older age after the pandemic resolved. Another consideration for the older age at diagnosis post Covid-19 is the possible trend towards considering treatment of slightly older 7 to 8 year old girls.
We previously reported a trend of increased CPP cases approximately 5–6 months following Covid-19 peaks (1). As we continued to analyze the data overtime, we again observed that CPP cases increased after the largest Covid-19 peak in December, 2021 (data not shown). Our findings are concordant with those reported by Chioma et al. (17), who showed a decline in CPP cases to pre-pandemic numbers after 2021, compared to an increase observed during the Covid-19 pandemic.
In our initial report showing an increase in the incidence of CPP during Covid-19 pandemic (1) we hypothesized reasons for increased cases of CPP during the Covid-19 pandemic, which have also been presented by others, including other hypotheses (2–9, 18, 19). Many of those hypotheses would predict a decrease in CPP cases post-pandemic; these include the impact of emotional changes and increased screen use, sedentarism, nutrition and sleep disturbances seen during the pandemic, which theoretically could have caused an impact on biochemical changes in the brain (implicating gamma aminobutyric acid, N-methyl-D-aspartate, catecholamines, dopamine, and melatonin). The negative psychological impact, more sedentary lifestyle, more time spent indoors, and more prolonged use of electronic devices during the pandemic theoretically changed post-Covid-19 with a return to in-person school and extracurricular activities. Likewise, the direct relationship to the viral infection and the immune response, should all have decreased post-Covid-19. None of the children in the first year of Covid-19 were vaccinated, so the increase in CPP was not related to the vaccine. By the first year post-Covid-19, many children were vaccinated. Since the incidence of CPP decreased during that time, the vaccine is not related to causing CPP. However, the converse cannot be proven. That is, a decrease in cases could be related to the vaccine protecting children or could be unrelated.
Strengths of our study include continued analyses post-Covid-19, which is important as data are scant. The same search criteria were used as in the previous study, so even if the absolute numbers may miss some children evaluated, the relative numbers should be consistent. We used the same months for 4 years to control for any potential seasonal variation. We only report cases of CPP who initiated treatment with GnRHa. We list this primarily as a strength, since this ensures inclusion of only those truly requiring treatment based on all parameters. Another strength of our study is the description of CPP cases in relationship to Covid-19 peaks noted in children in California.
A continued limitation of our study is that we were unable to determine how many children had a confirmed Covid-19 infection. The study was retrospective, but EMR query and potential extraction errors cannot all be assessed.
In conclusion, CPP cases requiring GnRHa treatment significantly increased during the first year of Covid-19 compared to pre-Covid-19 years. Cases started to decrease after the first Covid-19 year, and even more so the following year. The factors that led to a higher incidence of CPP during the pandemic appear to be reversible, but further study with larger cohorts is needed to understand the pathogenic factors contributing to a higher incidence of CPP in association with Covid-19 and whether this trend continues.
Data availability statement
The original contributions presented in the study are included in the article/Supplementary Material, further inquiries can be directed to the corresponding author.
Ethics statement
The studies involving humans were approved by University of California San Diego IRB. The studies were conducted in accordance with the local legislation and institutional requirements. Written informed consent for participation was not required from the participants or the participants’ legal guardians/next of kin in accordance with the national legislation and institutional requirements.
Author contributions
MVT: Conceptualization, Methodology, Writing – original draft, Writing – review & editing. TR: Data curation, Methodology, Writing – review & editing. KOK: Conceptualization, Methodology, Formal analysis, Writing – original draft, Writing – review & editing.
Funding
The author(s) declare that no financial support was received for the research, authorship, and/or publication of this article.
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
References
1. Trujillo MV, Rungvivatjarus T, Klein KO. Incidence of central precocious puberty more than doubled during COVID-19 pandemic: single-center retrospective review in the United States. Front Pediatr. (2022) 10:1007730. doi: 10.3389/fped.2022.1007730
2. Stagi S, De Masi S, Bencini E, Losi S, Paci S, Parpagnoli M, et al. Increased incidence of precocious and accelerated puberty in females during and after the Italian lockdown for the coronavirus 2019 (COVID-19) pandemic. Ital J Pediatr. (2020) 46 (1):1–10. doi: 10.1186/s13052-019-0764-1
3. Turriziani Colonna A, Curatola A, Sodero G, Lazzareschi I, Cammisa I, Cipolla C. Central precocious puberty in children after COVID-19 outbreak: a single-center retrospective study. Minerva Pediatr (Torino). (2022). doi: 10.23736/S2724-5276.22.06827-6. [Epub ahead of print]
4. Chioma L, Bizzarri C, Verzani M, Fava D, Salerno M, Capalbo D, et al. Sedentary lifestyle and precocious puberty in girls during the COVID-19 pandemic: an Italian experience. Endocr Connect. (2022) 11(2):e210650. doi: 10.1530/EC-21-0650
5. Acar S, Özkan B. Increased frequency of idiopathic central precocious puberty in girls during the COVID-19 pandemic: preliminary results of a tertiary center study. J Pediatr Endocrinol Metab. (2021) 35(2):249–51. doi: 10.1515/jpem-2021-0565
6. Ariza Jimenez AB, Aguilar Gomez-Cardenas FJ, de la Camara Moraño C. Probable impacto del COVID-19 sobre las derivaciones A endocrinología infantil: aumento de incidencia de pubertad precoz en un hospital de tercer nivel [Likely impact of COVID-19 on referrals to pediatric endocrinology: increased incidence of precocious puberty in A third-level hospital]. Endocrinol Diabetes Nutr. (2021) 69(7):542–4. doi: 10.1016/j.endinu.2021.09.004
7. Umano GR, Maddaluno I, Riccio S, Lanzaro F, Antignani R, Giuliano M, et al. Central precocious puberty during COVID-19 pandemic and sleep disturbance: an exploratory study. Ital J Pediatr. (2022) 48:60. doi: 10.1186/s13052-022-01256-z
8. Chen Y, Chen J, Tang Y, Zhang Q, Wang Y, Li Q, et al. Difference of precocious puberty between before and during the COVID-19 pandemic: a cross-sectional study among Shanghai school-aged girls. Front Endocrinol. (2022) 13:839895. doi: 10.3389/fendo.2022.839895
9. Barberi C, Di Natale V, Assirelli V, Bernardini L, Candela E, Cassio A. Implicating factors in the increase in cases of central precocious puberty (CPP) during the COVID-19 pandemic: experience of a tertiary centre of pediatric endocrinology and review of the literature. Front Endocrinol (Lausanne). (2022) 13:1032914. doi: 10.3389/fendo.2022.1032914
10. Neely EK, Wilson DM, Lee PA, Stene M, Hintz RL. Spontaneous serum gonadotropin concentrations in the evaluation of precocious puberty. J Pediatr. (1995) 127(1):47–52. doi: 10.1016/S0022-3476(95)70255-5
11. Neely EK, Hintz RL, Wilson DM, Lee PA, Gautier T, Argente J, et al. Normal ranges for immunochemiluminometric gonadotropin assays. J Pediatr. (1995) 127(1):40–6. doi: 10.1016/S0022-3476(95)70254-7
12. Garibaldi LR, Aceto T Jr, Weber C, Pang S. The relationship between luteinizing hormone and estradiol secretion in female precocious puberty: evaluation by sensitive gonadotropin assays and the leuprolide stimulation test. J Clin Endocrinol Metab. (1993) 76(4):851–6. doi: 10.1210/jcem.78.1.7507123
13. Ibáñez L, Potau N, Zampolli M, Virdis R, Gussinyé M, Carrascosa A, et al. Use of leuprolide acetate response patterns in the early diagnosis of pubertal disorders: comparison with the gonadotropin-releasing hormone test. J Clin Endocrinol Metab. (1994) 78(1):30–5.
14. Greulich WW, Pyle SI. Radiographic Atlas of Skeletal Development of the Hand and Wrist. Redwood City, CA: Stanford University Press (1959).
15. Available online at: https://covid19.ca.gov (accessed July 25, 2022).
16. Available online at: https://covid.cdc.gov/covid-data-tracker/#demographicsovertime (accessed October 18, 2023).
17. Chioma L, Chiarito M, Bottaro G, Paone L, Todisco T, Bizzarri C, et al. COVID-19 pandemic phases and female precocious puberty: the experience of the past 4 years (2019 through 2022) in an Italian tertiary center. Front Endocrinol (Lausanne). (2023) 14:1132769. doi: 10.3389/fendo.2023.1132769
18. Street ME, Sartori C, Catellani C, Righi B. Precocious puberty and COVID-19 into perspective: potential increased frequency, possible causes, and a potential emergency to be addressed. Front Pediatr. (2021) 9:734899. doi: 10.3389/fped.2021.734899
Keywords: CPP, COVID-19, pandemic, incidence, puberty
Citation: Vargas Trujillo M, Rungvivatjarus T and Klein KO (2024) Incidence of central precocious puberty declines to pre-pandemic levels post COVID-19 pandemic increase: single-center retrospective review in the United States. Front. Pediatr. 12:1352295. doi: 10.3389/fped.2024.1352295
Received: 7 December 2023; Accepted: 27 February 2024;
Published: 13 March 2024.
Edited by:
Mariella Valenzise, University of Messina, ItalyReviewed by:
Gerdi Tuli, Regina Margherita Hospital, ItalyGiorgia Pepe, University of Messina, Italy
© 2024 Vargas Trujillo, Rungvivatjarus and Klein. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Marcela Vargas Trujillo bXZhcmdhczFAcmNoc2Qub3Jn
 Marcela Vargas Trujillo
Marcela Vargas Trujillo Tiranun Rungvivatjarus1,2
Tiranun Rungvivatjarus1,2