- 1Department of Pharmacy Practice, College of Clinical Pharmacy, Imam Abdulrahman Bin Faisal University, Dammam, Saudi Arabia
- 2College of Clinical Pharmacy, Imam Abdulrahman Bin Faisal University, Dammam, Saudi Arabia
- 3Department of Pharmacology & Toxicology, College of Pharmacy, Umm Al Qura University, Makkah, Saudi Arabia
- 4Department of Clinical Pharmacy, College of Pharmacy, Prince Sattam Bin Abdul Aziz University, Alkharj, Saudi Arabia
- 5Department of Clinical Pharmacy, College of Pharmacy, Umm Al Qura University, Makkah, Saudi Arabia
Objective: Patient satisfaction is an indicator for quality of healthcare service and is sometimes linked to patients’ willingness to pay. Willingness to pay is an economic method for estimating patient’s inclination for a service in monetary terms. This study assessed satisfaction of patients from pharmacist counseling service and estimated their willing to pay for the same.
Methods: A month-long survey was conducted in community and hospital pharmacies located in Khobar, Dammam, and Qatif cities of Saudi Arabia, using Arabic version of Patient Satisfaction Feedback (PSF) questionnaire that measured satisfaction with counseling as well as willingness-to-pay. Convenient sampling method was used, and sample size was calculated based on power analysis. Data was analyzed through SPSS version 23. Chi-square (χ2) test and logistic regression analyses were conducted to report associations between variables and, determinants of satisfaction as well as willingness to pay respectively. The study was approved by concerned ethical committee (IRB-2019-05-020).
Results: Patients (n = 531) with previous counseling experience were more likely to be satisfied [adjusted odds ratio (AOR) 5.2, p < 0.05]. Patients were more willing to pay if, they had an income above SAR 10,000 i.e., USD 2666.5 (AOR 1.78, p < 0.05), were satisfied with counseling time duration (AOR 4.5) and, were able to get counseling without difficulty (AOR 2.1, p < 0.05). Patients were more likely to be satisfied and were willing to pay if, they received required knowledge/information completely (AOR 2.5, 3.7, and p < 0.05) and found pharmacist helpful (AOR 1, 4.5, and p < 0.05). Most patients (43.9%) were satisfied with pharmacist counseling and average satisfaction rating was 7.87 ± 1.99/10.
Conclusion: Patients considered counseling as an important service and were satisfied from it. Less than a third of patients were willing to pay for the service. Knowledge and helpfulness of pharmacist were identified as two major determinants that could not only satisfy and but also promote willingness to pay for the service. A pharmacist with skills in pharmaceutical care and counseling could be useful in promoting the service and making it profitable for pharmacy business.
Background
Patient satisfaction is one of the most common and indirect indicators for evaluating the quality of health service (Prakash, 2010). Available evidence indicates that patients who are satisfied from a healthcare service are more likely to achieve their target goals of therapy (Tabbish, 2001). From a patient’s perspective satisfaction could translate into empowerment in clinical decision making, promote a positive attitude toward health and medicines taking behavior, as well as better disease state management (Wendy and Scott, 1994; Foot, 2004). Besides, satisfied patients are more likely to have better recovery that motivates healthcare provider to deliver better care (Wendy and Scott, 1994; Naqvi et al., 2019). From an organization’s perspective, it is an important for sustaining business as economic analyses related to patient satisfaction estimate a figure of USD 0.2 million as a lifetime income loss to the healthcare facility due to patient discontent (Voluntary Hospitals of America, 1988; Naqvi et al., 2019). In healthcare system of France and Germany, measuring satisfaction of patients from healthcare delivery is required for quality assurance (Boyer et al., 2006; Schoenfelder et al., 2011). On a positive side, satisfaction fosters patient loyalty that results in better patient retention (Pavel et al., 2015). The healthcare facility may receive more recommendations and subsequently increase its profits. Moreover, studies mention that satisfied patients were willing to pay for the service (Poulas et al., 2008; Pavel et al., 2015).
Willingness to pay (WTP) is a pharmacoeconomic evaluation technique to understand how important patients consider the service and prefer it. It is a type of cost-benefit analysis (CBA) that measures the benefit of a health service and cost of service in monetary terms (Johannesson and Jonsson, 1991). In health utility and welfare economics, the WTP is the amount in monetary value that a patient would be ready to spend to utilize a healthcare service (Mitchell & Carson, 1989; Donaldson, 1990). The WTP method is by far the most suitable method to measure the economic value of un-marketed services such as counseling in this case (Smith, 1983; Johannesson and Jonsson, 1991; O’Brien and Viramontes, 1994; O’Brien et al., 1998; Suh, 2000). This could be examined by utilizing several methods namely conjoint analysis, choice modeling, discrete choice experiment (DSE), or the most commonly used contingent valuation (CV) technique, with either revealed or stated preference approach in which patients are asked to quote an amount that they are willing to pay for a particular service (Suh, 2000; Taylor and Armour, 2002; Drummond et al., 2005; Aizuddin et al., 2014; Gupta and Çakanyıldırım, 2016; Lakić et al., 2017). Few studies have endeavored to measure the economic impact of pharmacy services through WTP as a proxy (Smith, 1983; Johannesson et al., 1993; Gafni, 1997; Suh, 2000).
Studies have reported a range of 13–57% of patients who indicated their willingness to pay for various pharmacy services (Smith, 1983; Larson, 2000; Suh, 2000). It was reported in a study that more than half of patients were willing to pay an average USD 23 for one-time pharmaceutical care consultation by pharmacist. A range of USD 4–40 was reported in literature as the amount patients were willing to pay for pharmacist consultations (Shafie and Hassali, 2010). Available evidence suggests that WTP is affected by patients’ demographic factors such as age, health and well-being, monthly family income, provision of medical insurance, as well as previous experience with the service (Einarson et al., 1988; Reutzel and Furmaga, 1993; Gore and Madhavan, 1994; Suh, 2000). Studies that evaluate WTP for pharmacy counseling service in developing countries are scant. A study by Naqvi and colleagues reported that 56% of Pakistani patients appeared willing to pay an average USD 3 as fee for a one-time counseling session with pharmacist (Naqvi et al., 2019). Another study by Shafie and Hassali reported that 67% of Malaysian patients indicated their willingness to pay an average USD 2.86 for a dispensing service by pharmacist (Shafie and Hassali, 2010). Moreover, a study by Alhaddad in Western region of Saudi Arabia revealed that 70% of patients were willing to pay an average USD 16 for pharmacist led medication therapy management service (Alhaddad, 2019).
Apart from the work of Pavel and colleagues, there is no study that has measured satisfaction of patients together with their willingness to pay for the service (Pavel et al., 2015). Moreover, data from the developing countries are lacking as none of the studies had measured patients WTP for a counseling service. The Malaysian and Saudi studies did not measure the WTP for counseling service (Shafie and Hassali, 2010; Alhaddad, 2019). Though, Naqvi and colleagues measured WTP for pharmacist counseling however, the demographics of Pakistani and Saudi patients were quite different. Hence, they could not be compared since demographic characteristics may act as determinants of WTP. Therefore, there was a need to evaluate patients’ satisfaction and WTP for pharmacist counseling in Saudi healthcare settings.
Methods
Study Design and Settings
This cross-sectional study was carried out during March 2019 to April 2019. It was conducted in hospital and community pharmacies located in three cities namely Khobar, Dammam, and Qatif, that are situated in Eastern Province of Saudi Arabia. The study targeted patients who were counseled by pharmacists.
Objective
The aim was to assess patient satisfaction from counseling provided by pharmacists and their willingness to pay (WTP) for the same.
Study Venues
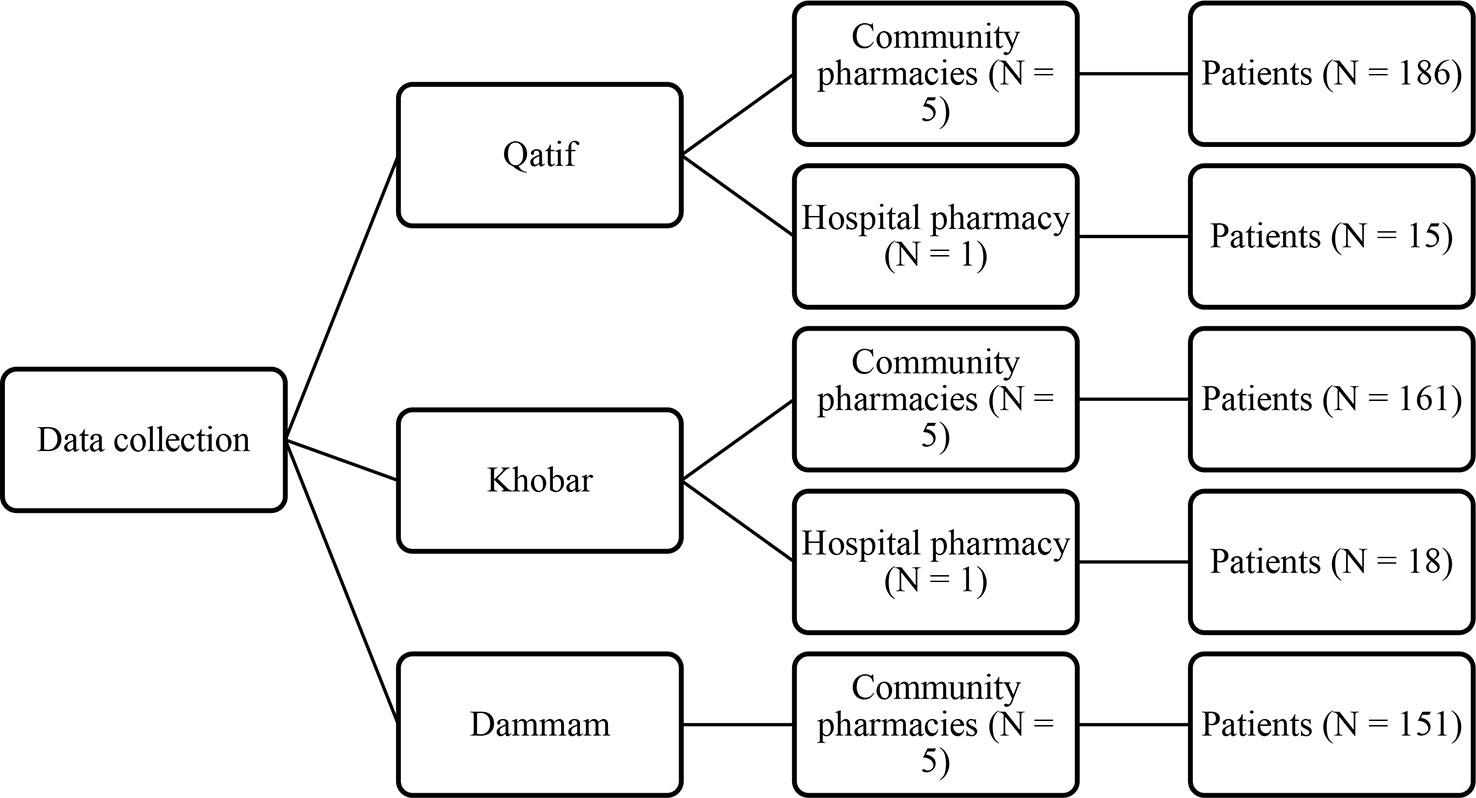
The venues of the study were hospital and community pharmacies. Hospital pharmacies of King Fahd Hospital of the University located in city of Khobar and, Al Zahra Hospital in Qatif city, as well as community pharmacies located in cities of Khobar, Dammam, and Qatif served as venues. All the three cities are located in Dammam Region that forms the third most populated metropolitan region of Saudi Arabia. The major city of this region is Dammam which is also the Governorate of the province. The city of Khobar is the second most populated city in the province. Selection of hospital pharmacies was made to sample a representative population of Saudi patients. Community pharmacies were located in every suburb of the cities in this region. Hence, each city was hypothetically divided into five zones namely north, south east, west, and central. One community pharmacy was selected as a venue from each hypothetical zone of the cities (Figure 1).
Eligibility Criteria
The study included adult male and female patients who spoke either Arabic or English. Patients aged 18 years or older were included. Patients with an acute or chronic illness, who had a counseling session with pharmacist were invited to participate. Patients who did not fill the above-mentioned criteria were not included. Patients who did not consent to participate and those who returned incomplete questionnaires were left out. Pharmacists with a bachelor’s degree, registered with the country’s regulatory body and, with at least 1-year work experience were included in the study.
Data Collection and Counseling Session
The data collection in hospital pharmacies was carried out in evening hours on weekdays. Additionally, data collection in community pharmacies was carried out on weekends (Friday and Saturday) in evening. The selection of these timings was based on peak patient visiting hours. The pharmacist counseling session was a single face-to-face oral communication session with patient. The counseling was based on patient’s prescription related queries, disease and therapy education, or any other query the patient had. The average duration of the session was around 8 min.
Research Tool and Translation
We used the patient satisfaction feedback (PSF) questionnaire to collect data. It was developed by Naqvi and colleagues in Urdu and English languages. The PSF is a 10-item questionnaire that contains questions related to patients’ satisfaction and WTP for counseling session with pharmacist. All items of the scale except item 8 and 10, are multiple choice. Item 8 is related to WTP and is open-ended. A respondent is free to mention any amount he/she is willing to pay considering if the counseling is a charged service. Item 10 is in the form of a rating scale (Naqvi et al., 2019).
The tool was translated in Arabic language before use. The translation process was conducted based on standard guidelines for translating and cross-culture adaptation for questionnaires (Gjersing et al., 2010; Epstein et al., 2015). We used the forward and backward translation by bilinguals (Degroot et al., 1994). Two academicians whose first language was Arabic and English as second language, translated and prepared the first draft in Arabic language. Both academicians were blinded to each other. Subsequently, the two drafts were then compared, and any disagreements were sorted out at this point. An Arabic version of PSF questionnaire (PSF-AR) was finalized. This PSF-AR was then back-translated into English by a team comprising of a pharmacist, a linguist, and a professor. The pharmacist, linguist, and professor were unaware of the purpose of the tool. The Arabic version of PSF was a deemed suitable to use at this point.
Piloting of the Translated Version
The Arabic version of the tool was piloted in a total of 58 patients and this process was conducted in two phases. The methodology of piloting was adopted from Converse and Presser (Converse and Presser, 1986). The first phase was participatory in which the questionnaire was given to 23 patients who were informed that the survey was a pre-test for the newly formulated Arabic version of the PSF. The patients were asked to fill the survey and were invited to give feedback. All patients found the instructions clear and no changes or modifications were proposed. The second phase was an undeclared survey and the questionnaire was handed to another 35 patients in a real-time scenario as a quality control feedback on their experience with pharmacist counseling. Participants filled the questionnaire after attending a counseling session with pharmacists. Attention was paid to identify any query raised by patients in filling their response. No difficulty in reading and understanding of PSF-AR was observed during this process. This two-tiered piloting process ensured robust pre-testing of questionnaire. The results of pilot study were not included in main findings.
Sample Size and Sampling
Due to generalization of results over the population, sample size adequacy demand major concern. To determine sample size from unknown size of population, “power study” is a useful and frequently used tool in medical research. A total of 510 sample can achieve more than 90% power when 3% margin of error is considered. The size of sample was calculated using the following formula after collecting required information from the available literature (Naing et al., 2006).
where, n is required sample size, Z1-β is Z value at power 1-β (considered 95% power and the value is 1.64), p is the value for referred prevalence as retrieved from published article i.e., 44.4% (value is 0.444), d is the margin of error (at 3% the value is 0.03). Convenient sampling method was used to collect the samples and the collection procedure stopped after completing the required number of patients.
Variable Management and Data Cleaning
Counseling satisfaction and willingness to pay were the two outcome variables for the current study. At the initial level, data of counseling satisfaction were collected using response of four categories (very satisfied, satisfied, uncertain, and not satisfied). For multivariate analysis satisfaction level was re-categorized into two groups, i.e., very satisfied and satisfied into, “satisfied” (coded, 1) and, uncertain and not satisfied into, unsatisfied (coded 0). To find the predictors of “willingness to pay” the dependent variable, “yes” was coded as 1 and, “no” as 0. Independent variables including patients’ demographics were coded and recoded as required. Data were checked and cleaned for missing cases, incomplete information, and also for extreme value using informal technique (Dunn and Clark, 1975; Islam et al., 2016).
Data Analyses
IBM SPSS version 23 (IBM Corp. Armonk, NY, USA) was used to analyze the data. Descriptive statistics was used to describe patient demographic and the results were mentioned as frequency and their percentage (%). Continuous data was reported in mean (X) with standard deviation (SD), and median (M) with inter quartile range (IQR). Chi-square (χ2) test was used to select significant independent variables to run a multiple model. Logistic regression was conducted to determine the predictors of counseling satisfaction and WTP. The model fitness was tested using Hosmer and Lemeshow test, classification table, and Negelkerker R2. Magnitude of standard error (SE) can be an indicator of testing multicollinearity among the predictors in multiple model. For current study we considered the value of SE less than 2.0 indicating no evidence of multicollinearity (Chan, 2004). A two-tailed p value of 0.05 was considered significant at the 95% CI (confidence interval) level.
Ethics Approval and Consent
All patients who agreed to participate in the study were briefed about the study objectives and were required to provide their written consent. Data was collected from those patients who provided their consent. The study was approved from the Institutional Review Board of Imam Abdulrahman Bin Faisal University, Dammam, Saudi Arabia (IRB-2019-05-020).
Results
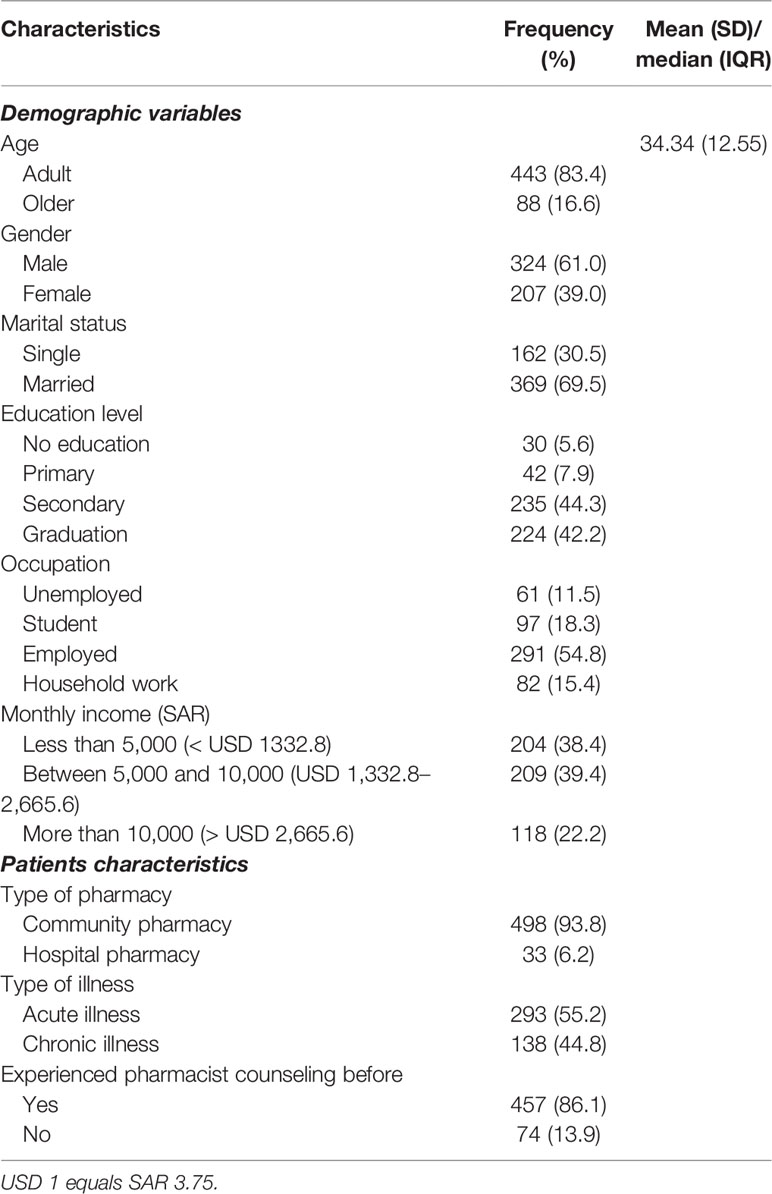
A total of 531 patients responded to the survey. Most responses were from patients who visited community pharmacy (N = 498, 93.8%). The mean age of patients was 34.3 ± 12.5 years ranging from 18 to 80 years. Three quarters of patients were adults (N = 400, 75.3%) and more than half were males (N = 324, 61%). Most patients were married (N = 369, 69.5%) and had secondary education (N = 223, 44.3%). Slightly more than half of patients were employed (N = 291, 54.8%) and had acute illness (N = 293, 55.2%). Majority had a monthly family income between SAR 5,000 and 10,000 (N = 209, 39.4%) (Table 1).
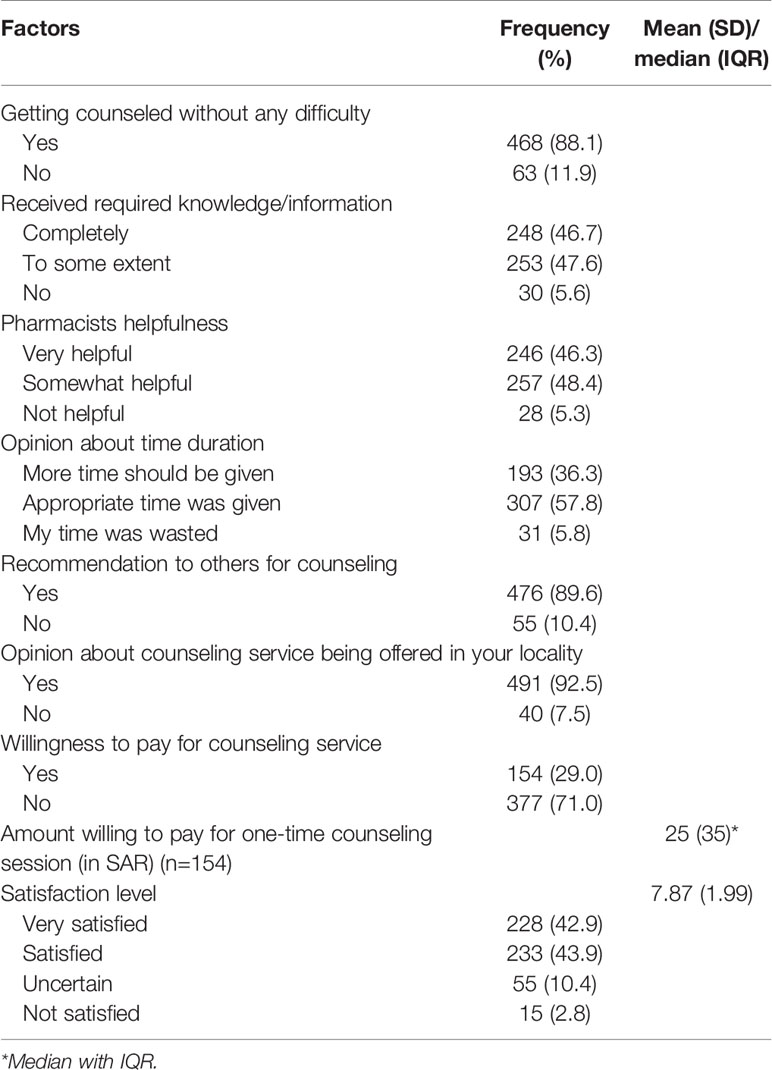
Regarding patient counseling information, most of the patients (N = 468, 88%) received counseling without any difficulty while less than half (N = 252, 47.6%) indicated that they received required information/knowledge to some extent. Almost similar proportion of patients (N = 257, 48.4%) indicated that they found the pharmacist somewhat helpful in resolving their queries. More than half of patients (N = 307, 57.8%) opined that appropriate time was given in counseling. They further mentioned that counseling service should be offered by pharmacies in localities (N = 491, 92.5%), and indicated that they would recommend others to seek counseling from pharmacists (N = 476, 89.6%). However, less than a third of patients (N = 154, 29%) indicated their willingness to pay for counseling service should it be charged, and an average of SAR 25 (USD 6.67) was indicated as possible fee payable by patients for one-time counseling session. Most patients (N = 233, 43.9%) were satisfied with pharmacist counseling and average satisfaction rating was 7.87 ± 1.99 out of 10 (Table 2).
The patient demographics and counseling factors were cross tabulated with their satisfaction and willingness to pay for counseling service using chi-square test for association. The association of “gender” with “willingness to pay,” was significant (p < 0.05). Moreover, association of “monthly family income” was significantly associated with “willingness to pay” (p < 0.05). No other demographic variable was significantly associated with willingness to pay. Furthermore, no significant association was observed in cross tabulation between demographics and satisfaction (p > 0.05).
In addition, the counseling factors were cross tabulated with the same to observe any association. There was a significant association between “satisfaction” and the variable of “getting counseled without difficulty” (p < 0.001). The counseling variable of “received required information/knowledge” was significantly associated with “patient satisfaction” (p < 0.001), and “willingness to pay” (p < 0.01). Similarly, significant association was reported for the variable of, “found pharmacist helpful,” with, “patient satisfaction” (p < 0.001), as well as, “willingness to pay” (p < 0.05). The counseling variables of “patient opinion about time of counseling,” “recommending counseling to others,” and, “should this service be offered in locality,” were significantly associated with “patient satisfaction” and p-values obtained were less than 0.001 (Table 3).
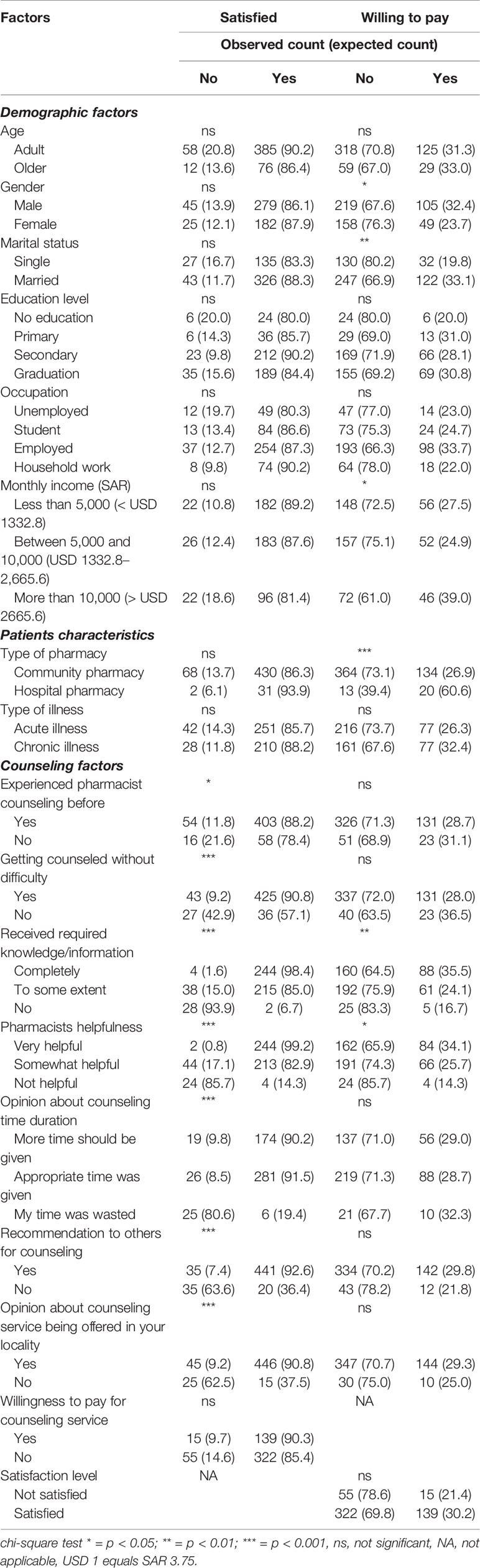
Table 3 Association of various demographic and counseling factors with patients’ satisfaction and willingness to pay for counseling.
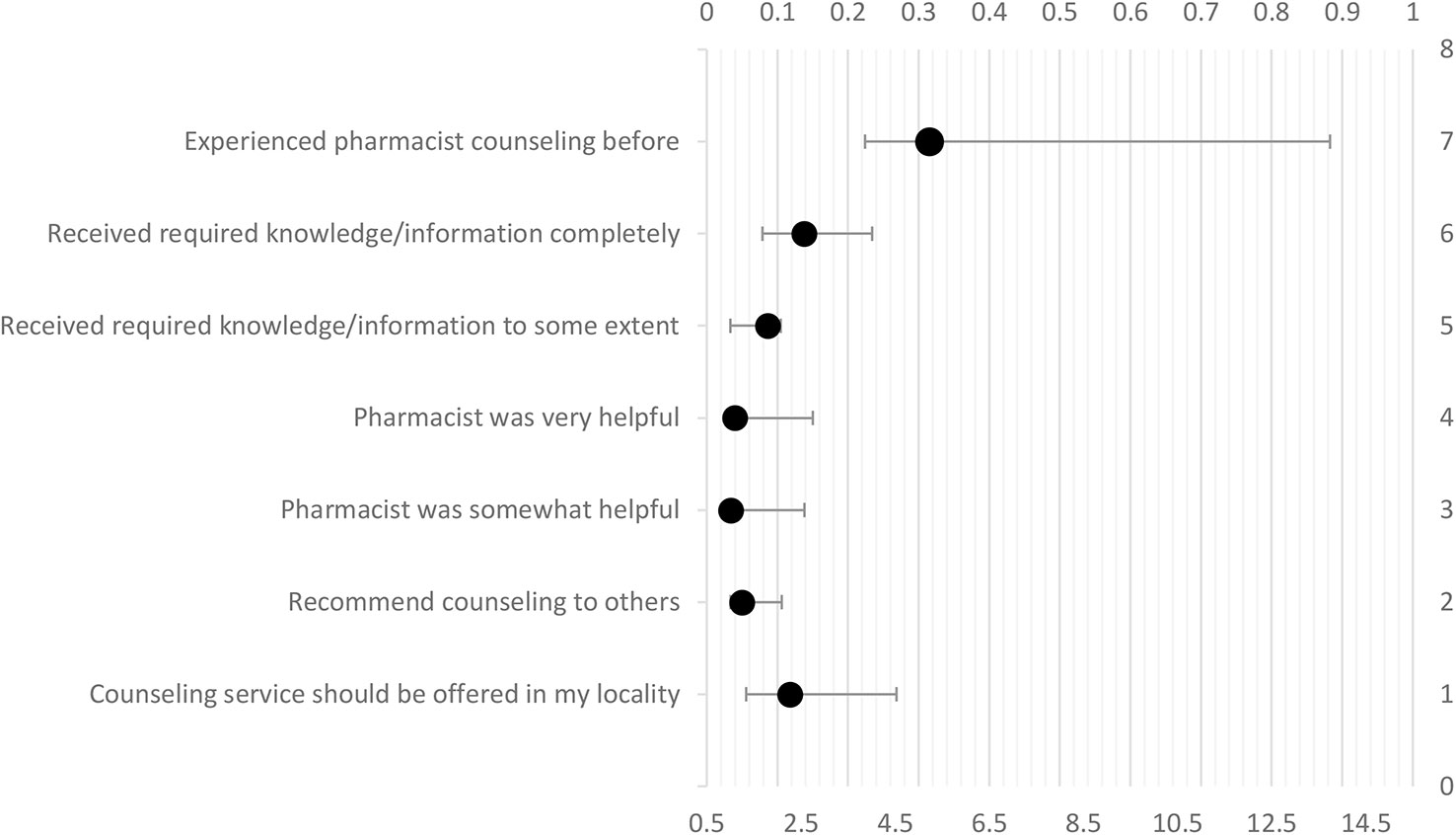
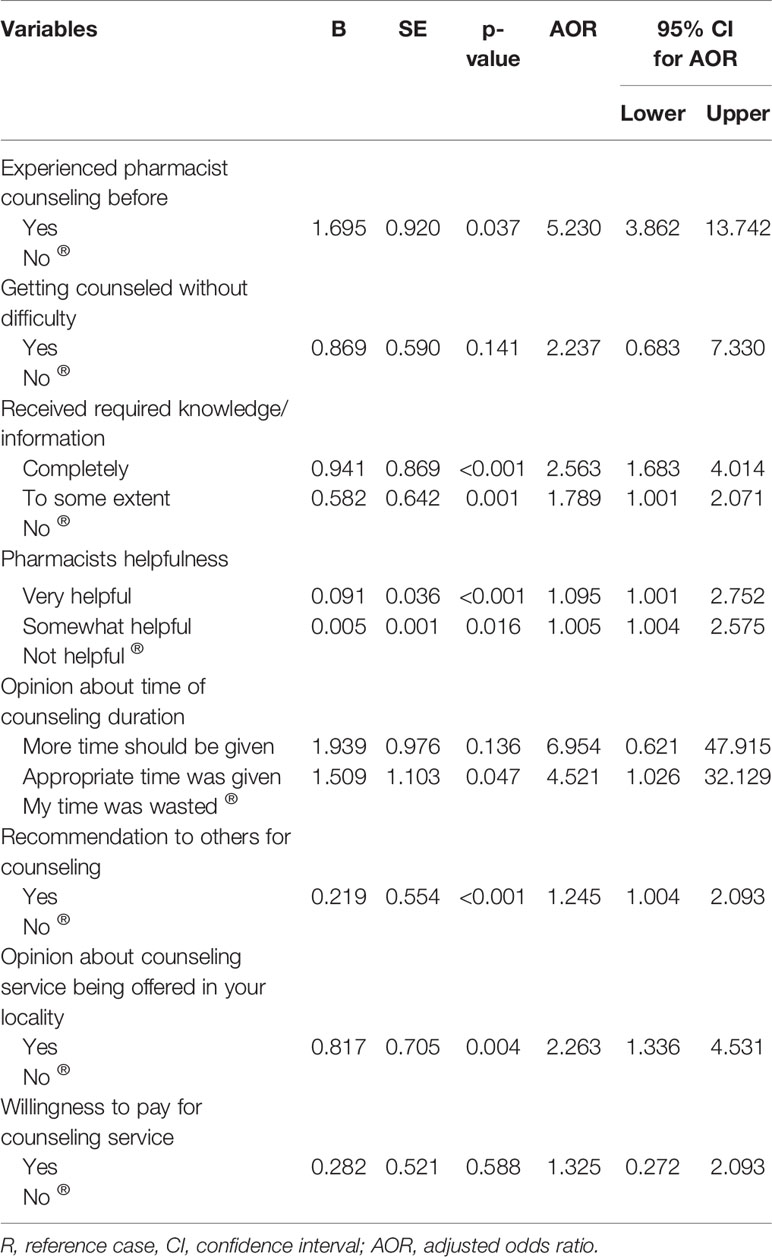
Logistic regression revealed that patients who previously had counseling sessions with pharmacists were five times more likely to be satisfied [adjusted odds ratio (AOR) = 5.2, p < 0.05] compared to patients who never had counseling before. Patients who found pharmacist helpful were more likely to be satisfied (AOR = 1.09, p < 0.001) compared to patients who did not find them helpful, patients who completely received required information/knowledge from pharmacist were 2.5 times more likely to be satisfied (AOR = 2.563, p < 0.001). Besides, patients who indicated that they received required information/knowledge to some extent, were 1.8 times more likely to be satisfied (AOR = 1.789, p < 0.01). Patients who opined that counseling time was appropriate, were 4.5 times more likely to be satisfied (AOR = 4.521, p < 0.05) compared to those who considered counseling as a waste of time. Patient who recommended counseling to others and those who opined that the counseling service should be offered in pharmacies in their locality, were more likely to be satisfied (AOR = 1.245, p < 0.01) as compared to patients who did not. The model for patient satisfaction is tabulated in Table 4 and represented graphically in Figure 2. The model is adjusted for demographic variables namely age, education, occupation, and income. In multiple logistic regression, “Enter” method was applied, multicollinearity was checked and was not found. Hosmer-Lemeshow test value was χ2 = 2.444, p = 0.964, Pearson chi-square, significance for model at p < 0.001, and classification table (overall correctly classified percentage = 86.8), were applied to check the model fitness. Cox & Snell R Square was 0.396 while Nagelkerke R Square was reported at 0.732 (Table 4; Figure 2).
Similarly, multiple logistic regression for WTP adjusted for demographic variables age, gender, education, and occupation, was applied using “Enter” method. Multicollinearity was checked and was not present. The value for Hosmer-Lemeshow test was reported at χ2 = 7.452, p=0.489. Pearson chi-square, significance for model at p < 0.01, and classification table (overall correctly classified percentage = 72.5) were applied to check the model fitness. Cox & Snell R Square value was 0.172 while Nagelkerke R Square was reported at 0.209.
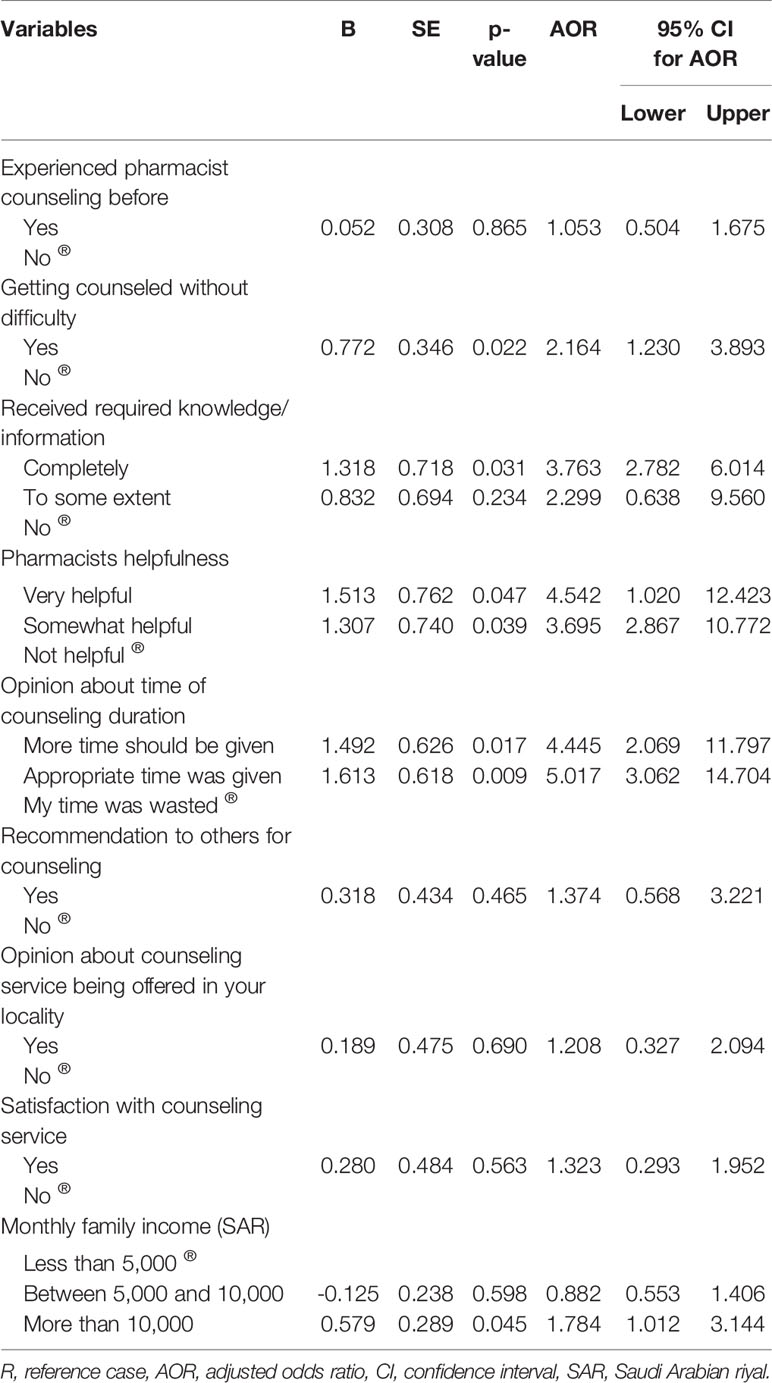
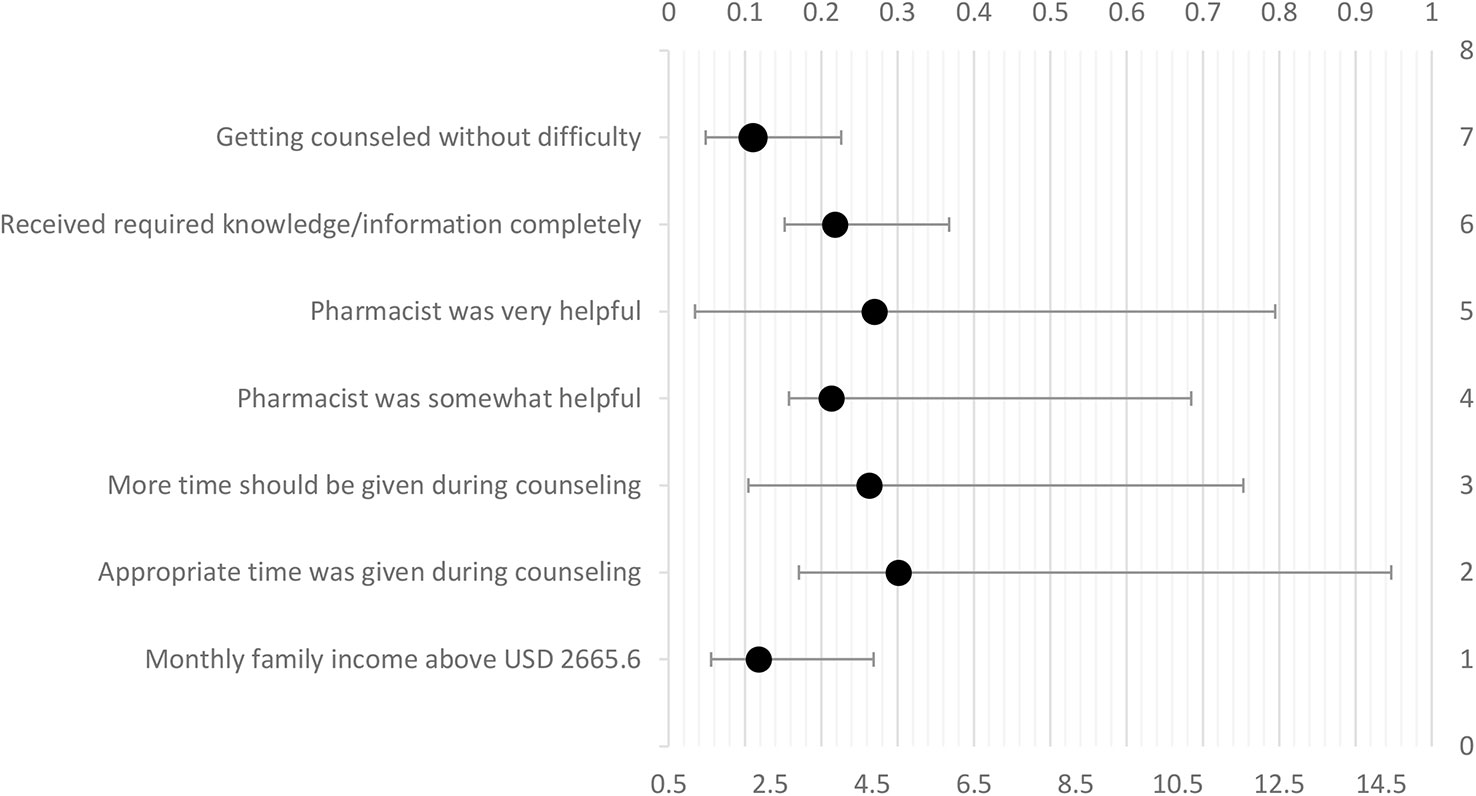
Patients who had counseling without experiencing any difficulty were 2.16 times more likely to pay (AOR = 2.164, p < 0.05) as compared to patients who had difficulties in getting counseled. Patients who completely received required information/knowledge from pharmacist counseling appeared more likely to pay for the service (AOR = 3.76, p < 0.05) as compared to patients who did not. Patients who found pharmacist very helpful and somewhat helpful in resolving their queries appeared more likely to pay (AOR = 4.54, and 3.69 respectively; p < 0.05) as compared to patients who did not. Patients who opined that more time should be given for counseling appeared more likely to pay (AOR = 4.45, p < 0.05) as compared to patients who opined that their time was wasted in counseling. For patients who mentioned that appropriate time was given in counseling session, had higher odds (AOR = 5.017) of paying for counseling. Patients who had higher income were more likely to pay for counseling (AOR 1.78, p < 0.05). The model is presented in Table 5 and Figure 3.
Discussion
Patient satisfaction is regarded as an indirect indicator of quality of healthcare service. It has the potential to translate into better patient care and as well as increase profitability for the service provider. Studies mention that satisfaction increases patients’ willingness to pay for service. This is important considering marketable potential of service. Our study documented patient satisfaction and their willingness to pay for counseling, as a pharmaceutical service provided at hospital and community pharmacies. With the exception of the work of Alhaddad, no study has been conducted in Saudi Arabia that reports this phenomenon (Alhaddad, 2019). This study was conducted in the third largest metropolitan region of Saudi Arabia comprising of three major cities with a population of over 0.3 million (General Authority for Statistics, 2016; AlQarni et al., 2019). The study utilized a previously validated instrument known as patient satisfaction feedback (PSF) that was translated in Arabic language, and gathered responses from a large patient sample in both hospital and community pharmacy settings (Naqvi et al., 2019). These are some notable strengths of this work.
The study reported that slightly less than half of the patients (43.9%) were satisfied while 42.9% of patients indicated that they were “very” satisfied with counseling. This indicated that about 87% of patients were content with the service. This figure for satisfaction was quite high compared to previous studies reported from other parts of the world. Yang and colleagues conducted a study in South Korean patients to report satisfaction with medication counseling provided in community pharmacies. They reported that a third of patients (34%) were satisfied (Yang et al., 2016). In a study in the Netherlands, Geffen and colleagues reported that less than half of patients (42%) were satisfied with medication counseling. The authors of that study concluded that patients’ expectations may not have been met (van Geffen et al., 2011). Another study in Pakistan reported that 60% of patients appeared satisfied with counseling (Naqvi et al., 2019). All studies except the one in Pakistan, were conducted in community pharmacies where the majority of patients appeared unsatisfied. The Pakistani study was based in hospital pharmacy settings where most patients appeared satisfied.
The present study included patients from both hospital and community pharmacy settings and based on the cross-tabulation results, there was no significant (p > 0.05) association between healthcare settings and satisfaction. A possible explanation to this occurrence in our study could be based on patient population. Patients who have had an experience with counseling before would be more acquainted with the service compared to those who have not had counseling before. In this study, most patients (86%) had previously attended some sort of counseling by pharmacists. Logistic regression analysis highlighted that such patients were more likely to be satisfied as compared to those who had no previous exposure. This finding is in line with results of Naqvi and colleagues (Naqvi et al., 2019). The hypothesis is further strengthened by findings of the study in Netherlands where most patients who were dissatisfied had never attended counseling sessions before (van Geffen et al., 2011). In addition, there was no significant (p > 0.05) association of demographic characteristics such as education, type of illness, and income, with satisfaction. This meant that educated and uneducated patients have an equal chance of being satisfied and vice versa. This highlights that patients may have expectations regarding counseling that are not dependent on patients’ level of education. Such expectations could be related to knowledge of disease and treatment.
A benchmark could be the work of Naqvi and colleagues where significant (p < 0.05) association of satisfaction was reported with type of illness and health insurance. This may be due to expectation of patients with chronic and acute illnesses. Pakistani patients with chronic illnesses seemed more likely to be satisfied with counseling compared to those with acute illnesses. Whereas satisfaction of Saudi patients was not associated with type of illness. This could be due to number of patients and time duration of counseling. Pakistan has a population of over 200 million while Saudi population is just over 30 million (General Authority for Statistics, 2016). Secondly, there are about 32,500 registered pharmacists in Pakistan while registered pharmacists in Saudi Arabia are about 24,395 (Naqvi et al., 2017; AlRuthia et al., 2018). Therefore, pharmacy workforce density in Saudi healthcare system is higher as compared to Pakistan. Hence, pharmacists in Saudi healthcare system can afford to give more time to patients during counseling (Alfadl et al., 2018). This hypothesis is further strengthened by our study findings regarding time duration of counseling, in which more than half of patients (58%) indicated that counseling time duration was “appropriate” whereas less than half of patients (42%) mentioned the same in Pakistani study (Naqvi et al., 2019). Therefore, patients with severe illnesses may have been prioritized for counseling in Pakistan.
Further, there was no significant association of satisfaction with income in Saudi patients. This occurrence could be explained based on out-of-pocket expenditure. Unlike patients in Pakistan, Saudi patients do not have to pay direct costs for treatment. Therefore, income is not a determinant of satisfaction. Patients of developing countries may have to bear out-of-pocket cost to purchase medicines. Though, Pakistani study reported no significant association of income with satisfaction, there was a significant association for availability of “health insurance” (Naqvi et al., 2019). This meant that Pakistani patients who had health insurance were more likely to be satisfied with counseling as they did not have to pay out-of-pocket costs.
The second parameter to observe while documenting the satisfaction was the quality of service. Patients satisfaction was significantly (p < 0.05) associated with, having counseling without facing difficulties, received required information and finding the pharmacist helpful. In our study patients who indicated that they found the pharmacist helpful in resolving their queries and had received required information/knowledge completely, were more likely to be satisfied. Yang and colleagues mentioned the attitude of pharmacist, use of patient-intelligible language and simpler information contents, as determinants of patient satisfaction (Yang et al., 2016). Considering the advancements in pharmacy profession, pharmacists have to assume the role of patient care provider and a member of allied healthcare team alongside traditional job responsibilities of medication dispensing and drug information services (Alamri et al., 2017). This could increase workload and subsequently add to the job stress that has the potential to decrease work efficiency of pharmacist. As a result, patients may be dissatisfied (Lea et al., 2012; Yang et al., 2016). Higher job stress levels related to patient care have been reported from pharmacists working in Saudi healthcare settings (Suleiman, 2015). Appropriate number of staff and effective time management could help pharmacists manage their traditional and clinical roles. This aspect is of paramount importance to pharmacy human resource as proper staffing would ensure better performance that could result in increased satisfaction from service and translate into business profitability (León et al., 2001; McIntosh et al., 2011).
There was a significant association between counseling time and satisfaction. Patients who mentioned that counseling time was appropriate were four times more likely to be satisfied and five times more likely to pay. Insufficient counseling time has been observed to be a determinant of patient dissatisfaction as studies indicate that counseling time >1 min has more potential to satisfy patients as compared to counseling session lasting less than a minute. Additionally, there may be a direct relationship between counseling duration and patient satisfaction (Yang et al., 2016; Naqvi et al., 2019). Moreover, less time duration of counseling session was observed to be the single most common predictor of dissatisfaction among South Korean patients (León et al., 2001; Lee et al., 2009; Yang et al., 2016).
The patients were asked about their willingness to pay for the counseling service should it be charged. Regression analysis indicated that satisfied patients were 1.3 times more likely to pay for the service. However, less than a third of patients (29%) indicated that they were willing to pay and declared an average SAR 25, i.e., USD 6.67, as fee for a one-time pharmacist counseling session. This amount was higher than that reported from Pakistani patients, i.e., USD 3, and, an American study in which patients were willing to pay USD 5.6 for pharmacist’s consultation (Suh, 2000; Naqvi et al., 2019). This is an indication of patients’ satisfaction and their inclination toward pharmacist counseling service. Evidence indicates that despite being satisfied, most patients are not willing to pay for pharmacy services and are likely to avail such extended pharmacy services only if it is available free of cost (Lee et al., 2009). The proportion of patients willing to pay for pharmacist counseling service in this study were lower than the figures reported in the literature, i.e., 31–45% (Smith, 1983; Laverty, 1984; Metge et al., 1998). WTP was significantly associated (p < 0.05) with patients’ monthly family income that implied that most patients with an income greater than SAR 10,000, i.e., USD 2,666.5, were 1.7 times more likely to pay for the service. This is in line with previous studies as WTP may depend on consumer’s purchasing power (Donaldson, 1999; Suh, 2000).
Consumer buying power is the capacity of the individual to buy a certain quantity of goods/services. A high value would indicate that the consumer has a higher income and power to purchase goods/service relative to the supply and economic value of goods/service available (Offodile and Ho, 2018). Therefore, patients with a high purchasing power, i.e., higher income relative to economic value of pharmacist counseling service, would be in a better position to utilize and pay for the service. Furthermore, willingness to pay was significantly associated (p < 0.05) with pharmacy settings. Patients who attended counseling session in hospital settings were more likely to pay as compared to those who attended the same in community pharmacy settings. Studies have mentioned that achievement of positive health outcomes are linked to WTP. Evidence indicates that patients would be willing to pay if their satisfaction with the following three healthcare features is increased. These are namely, relationship with healthcare professionals, fulfillment of patient’s medicines needs and, increased likelihood of recovery (Pavel et al., 2015). Since these three attributes are more likely to be achieved in a hospital setting, the patients are more likely to be willing to pay in those settings.
The variable of previous counseling experience was not significantly associated (p > 0.05) with WTP. Previous counseling experience may have increased their knowledge and have empowered them in managing their conditions. Hence, they are satisfied and may not require a paid session with pharmacist anymore. The association of satisfaction with previous counseling experience can also be explained by this occurrence. The patients who received counseling without facing any difficulty such as understanding of language, voice and speech, were 2.16 times more likely to pay for the session. Besides, patients who received required knowledge/information were 2.29–3.76 times more likely to pay for the service. Moreover, patients who indicated that they found the pharmacist useful were 3.69–4.54 times more willing to pay. These factors highlight the importance of acquiring skills for pharmaceutical care and patient counseling. A skilled pharmacist has more potential to not only promote patient satisfaction and WTP for the service but also to increase the likelihood of achieving positive health outcomes. Based on the Common-Sense Model of Illness Representation (CSM), a patient’s perception of health risk and the emotional response associated with the risk would define patient’s overall response to illness (French and Weinman, 2008). The response would affect the outcome of illness. The perception of illness is based on disease identity, timeline, consequences, cause, controllability, and emotionality (McAndrew et al., 2008; Huston and Houk, 2011; Cameron and Leventhal, 2012). A pharmacist with pharmaceutical care and counseling skills could provide disease education and conditioning that may empower patients in all six domains. As a result, patients with a positive perception of disease and controlled emotional response to the risks associated with negative outcomes of the disease, would be in a better position to achieve positive health outcomes.
The study had a limitation of strategic bias. Some patients may not have liked the questions related to WTP and subsequently chose to not answer them. This was not because they did not perceive the value of the service but felt that counseling service should be free of charge. Besides, there was no question that could identify the reasons behind their answer regarding WTP and their declared amount. Moreover, the selected sampling technique was convenient sampling. Therefore, readers are instructed to generalize the results with caution.
Conclusion
This study highlighted that patients considered pharmacist counseling as an important service that could help in effective disease state management. The quality of counseling offered to patients in hospital and community pharmacies of this region was according to the expectations as most patients were satisfied from it. Contingent valuation method was useful to measure the value of pharmacist counseling service in monetary terms. Though, less than a third of patients were willing to pay for the service, we were able to identify the determinants that prompted patients to pay. The results of the study are useful in practical context if the determinants of WTP are considered while counseling patients. Knowledge and helpfulness of pharmacist were identified as two major determinants that could not only satisfy but make patients willing to pay for the service. A pharmacist with skills in pharmaceutical care and counseling could be useful in promoting the service thereby making it profitable for pharmacy business.
Author’s Note
This research paper is based on student research project undertaken as thesis for partial fulfillment of Doctor of Pharmacy (Pharm.D) degree by MoA (#2150008886), AlA (#2150000700) and MuA (#2150003205), at College of Clinical Pharmacy, Imam Abdulrahman Bin Faisal University, Dammam 31441, Saudi Arabia. A research abstract based on initial preliminary findings related to patient satisfaction was presented as a poster in 1st Knowledge, Skills, Ability in Pharmacy & Toxicology (KSAPT) Conference held on 4th April 2019 in Al Khobar. Another research abstract detailing complete analysis related to satisfaction and WTP was presented as a poster in SIPHA 2020 that took place from January 21 to 23, 2020 at Riyadh, Saudi Arabia.
Data Availability Statement
The raw data supporting the conclusions of this manuscript will be made available by the authors, without undue reservation, to any qualified researcher.
Ethics Statement
The studies involving human participants were reviewed and approved by the Institutional Review Board of Imam Abdulrahman Bin Faisal University (IRB-2019-05-020). The patients/participants provided their written informed consent to participate in this study.
Author Contributions
DA, AN, MAI, MoA, AlA and MuA conceived the idea and designed the study. AN wrote the proposal with DA, AH, MI, MR, MAI, MoA, AlA, AbA and MuA collected the data. DA, AbA, MR, MI and AH helped in translating the questionnaire and entered data in SPSS. DA, AN, and MoA wrote the abstract and introduction section. DA, AN, AlA, MuA and AbA wrote the methodology. MR, MAI, and AH wrote the discussion section. All authors provided their input in revision of the manuscript. All authors read and approved the final manuscript.
Conflict of Interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Acknowledgments
We extend our gratitude to all participating pharmacists and patients for giving their time to our study and for providing their honest response.
Abbreviations
USD, United States dollar; WTP, willingness to pay; CBA, cost benefit analysis; PSF, patient satisfaction feedback; Pharm.D, doctor of pharmacy; PSF-AR, patient satisfaction feedback Arabic version; SPSS, Statistical Package for Social Sciences; SD, standard deviation; USA, United States of America; IQR, interquartile range; SE, standard error; CI, confidence interval; IRB, Institutional Review Board; SAR, Saudi Arabian riyal; AOR, adjusted odds ratio; CSM, common-sense model of illness representation.
References
Aizuddin, A. N., Sulong, S., Aljunid, S. M. (2014). Methods and tools for measuring willingness to pay for healthcare: what is suitable for developing countries? BMC. Public Health 14 (Suppl 1), O20. doi: 10.1186/1471-2458-14-S1-O20
Alamri, S. A., Ali Al Jaizani, R., Naqvi, A. A., Ghamdi, M. (2017). Assessment of drug information service in public and private sector tertiary care hospitals in the eastern province of Saudi Arabia. Pharmacy (Basel Switzerland). 5 (3), E37. doi: 10.3390/pharmacy5030037
Alfadl, A. A., Alrasheedy, A. A., Alhassun, M. S. (2018). Evaluation of medication counseling practice at community pharmacies in Qassim region, Saudi Arabia. Saudi Pharm. J. 26, 258–262. doi: 10.1016/j.jsps.2017.12.002
Alhaddad, M. S. (2019). Youth experience with community pharmacy services and their perceptions toward implementation of medication therapy management services by Community Pharmacists in the Western Region of Saudi Arabia. Ther. Innov. Regul. Sci. 53, 95–99. doi: 10.1177/2168479018769299
AlQarni, K., AlQarni, E. A., Naqvi, A. A., AlShayban, D. M., Ghori, S. A., Haseeb, A., et al. (2019). Assessment of Medication Adherence in Saudi Patients With Type II Diabetes Mellitus in Khobar City, Saudi Arabia. Front. Pharmacol. 10, 1306. doi: 10.3389/fphar.2019.01306
AlRuthia, Y., Alsenaidy, M. A., Alrabiah, H. K., AlMuhaisen, A., Alshehri, M. (2018). The status of licensed pharmacy workforce in Saudi Arabia: a 2030 economic vision perspective. Hum. Resour. Health 16 (1), 28. doi: 10.1186/s12960-018-0294-8
Boyer, L., Francois, P., Doutre, E., Weil, G., Labarere, J. (2006). Perception and use of the results of patient satisfaction surveys by care providers in a French teaching hospital. Int. J. Qual. Health Care 18, 359–364. doi: 10.1093/intqhc/mzl029
Cameron, L., Leventhal, H. (2012). The self-regulation of health and illness behaviour (London: Routledge).
Chan, Y. H. (2004). Biostatistics 202: Logistic regression analysis. Singapore Med. J. 45 (4), 149–153.
Converse, J. M., Presser, S. (1986). Survey questions: Handcrafting the standardized questionnaire (Newbury Park, CA: Sage Publications).
Degroot, A. M. B., Dannenburg, L., Vanhell, J. G. (1994). Forward and Backward Word Translation by Bilinguals. J. Mem. Lang. 33, 600–629. doi: 10.1006/jmla.1994.1029
Donaldson, C. (1990). Willingness to pay for publicly provided goods: a possible measure of benefit? J. Health Econ. 9, 103–118. doi: 10.1016/0167-6296(90)90043-3
Donaldson, C. (1999). Valuing the benefits of publicly-provided health care: does ‘ability to pay’ preclude the use of ‘willingness to pay’? Soc Sci. Med. 49, 551–563. doi: 10.1016/S0277-9536(99)00173-2
Drummond, M. F., Sculper, M. J., Torrance, G. W., O’Brien, B. J., Stoddart, G. L. (2005). Methods for economic evaluation of health care programmes. 3rd ed. (New York: Oxford University Press).
Dunn, O. J., Clark, V. A. (1975). Applied statistics: analysis of variance and regression. 2nd ed. (New York, NY, USA: John Wiley & Sons, Inc.), ISBN: 0-471-81269-2.
Einarson, T. R., Bootman, J. L., Larson, L. N., McGhan, W. F. (1988). Blood level testing in a community pharmacy: consumer demand and financial feasibility. Am. Pharm. 28, 76–79. doi: 10.1016/S0160-3450(15)32004-3
Epstein, J., Santo, R. M., Guillemin, F. (2015). A review of guidelines for cross-cultural adaptation of questionnaires could not bring out a consensus. J. Clin. Epidemiol. 68, 435–441. doi: 10.1016/j.jclinepi.2014.11.021
Foot, F. (2004). How to be a happy dermatologist. Dermatol. Psychosom. 5, 112–113. doi: 10.1159/000081153
French, D. P., Weinman, J. (2008). Current issues and new directions in Psychology and Health: “Assessing illness perceptions: beyond the IPQ”. Psychol. Health 23, 5–9. doi: 10.1080/08870440701616714
Gafni, A. (1997). Willingness to pay in the context of an economic evaluation of healthcare programs: theory and practice. Am. J. Manag. Care 3, S21–S32.
General Authority for Statistics. Kingdom of Saudi Arabia. (2016). Demographic survey. https://www.stats.gov.sa/sites/default/files/en-demographic-research-2016_2.pdf (accessed 10 November 2019).
Gjersing, L., Caplehorn, J. R. M., Clausen, T. (2010). Cross-cultural adaptation of research instruments: language, setting, time and statistical considerations. BMC. Med. Res. Methodol. 10, 13. doi: 10.1186/1471-2288-10-13
Gore, P. R., Madhavan, S. (1994). Consumers’ preference and willingness to pay for pharmacist counseling of non prescription medicines. J. Clin. Pharm. Ther. 19, 17–25. doi: 10.1111/j.1365-2710.1994.tb00803.x
Gupta, V., Çakanyıldırım, M. (2016). A WTP-Choice Model: Empirical Validation, Competitive and Centralized Pricing. Prod. Oper. Manage. 25, 1866–1884. doi: 10.1111/poms.12582
Huston, S. A., Houk, C. P. (2011). Common sense model of illness in youth with type 1 diabetes or sickle cell disease. J. Pediatr. Pharmacol. Ther. 16, 270–280. doi: 10.5863/1551-6776-16.4.270
Islam, A., Islam, N., Bharati, P., Aik, S., Hossain, G. (2016). Socio-economic and demographic factors influencing nutritional status among early childbearing young mothers in Bangladesh. BMC. Womens Health 16, 58. doi: 10.1186/s12905-016-0338-y
Johannesson, M., Jonsson, B. (1991). Economic evaluation in health care: is there a role for cost-benefit analysis? Health Policy 17, 1–23. doi: 10.1016/0168-8510(91)90114-D
Johannesson, M., Johansson, P. O., Kristrom, B., Gerdtham, U. G. (1993). Willing ness to pay for antihypertensive therapy-further results. J. Health Econ. 12, 95–108. doi: 10.1016/0167-6296(93)90042-D
Lakić, D., Stević, I., Odalović, M., Vezmar-Kovačević, S., Tadić, I. (2017). Patients’ willingness to pay for cognitive pharmacist services in community pharmacies. Croat. Med. J. 58, 364–371. doi: 10.3325/cmj.2017.58.364
Larson, R. A. (2000). Patients’ willingness to pay for pharmaceutical care. J. Am. Pharm. Assoc. 40, 618–624. doi: 10.1016/s1086-5802(16)31101-9
León, F. R., Monge, R., Zumarán, A., García, I., Ríos, A. (2001). Length of counseling sessions and the amount of relevant information exchanged: a study in Peruvian clinics. Int. Family Plann. Perspec. 27, 28–46. doi: 10.2307/2673802
Lea, V. M., Corlett, S. A., Rodgers, R. M. (2012). Workload and its impact on community pharmacists’ job satisfaction and stress: a review of the literature. Int. J. Pharm. Pract. 20, 259–271. doi: 10.1111/j.2042-7174.2012.00192.x
Lee, J. H., Sohn, H. S., Shin, H. T. (2009). Quality Evaluation of Medication Counseling in Korean Community Pharmacies. Korean J. Clin. Pharm. 19, 131–145.
McAndrew, L. M., Musumeci-Szabó, T. J., Mora, P. A., Vileikyte, L., Burns, E., Halm, E. A., et al. (2008). Using the common sense model to design interventions for the prevention and management of chronic illness threats: from description to proces. Br. J. Health Psychol. 13, 195–204. doi: 10.1348/135910708X295604
McIntosh, J., Rafie, S., Wasik, M., McBane, S., Lodise, N. M., El-Ibiary, S. Y., et al. (2011). Changing oral contraceptives from prescription to over-the-counter status: an opinion statement of the Women’s Health Practice and Research Network of the American College of Clinical Pharmacy. Pharmacotherapy 31, 424–437. doi: 10.1592/phco.31.4.424
Metge, C. J., Hendricksen, C., Maine, L. (1998). Consumer attitudes, behaviors, and perceptions about pharmacies, pharmacists, and pharmaceutical care. J. Am. Pharm. Assoc. 38, 37–47. doi: 10.1016/S1086-5802(16)30288-1
Mitchell, R. C., Carson, R. T. (1989). Using Surveys to Value Public Goods (Washington, DC: Resources for the Future).
Naing, L., Winn, T., Rusli, B. N. (2006). Practical Issues in Calculating the Sample Size for Prevalence Studies. Arch. Of. Orofac. Sci. 1, 9–14.
Naqvi, A. A., Zehra, F., Naqvi, S. B. S., Ahmad, R., Ahmad, N., Usmani, S., et al. (2017). Migration Trends of Pharmacy Students of Pakistan: A Study Investigating the Factors Behind Brain Drain of Pharmacy Professionals from Pakistan. Ind. J. Pharm. Educ. Res. 51, 192–206. doi: 10.5530/ijper.51.2.25
Naqvi, A. A., Hassali, M. A., Naqvi, S. B. S., Aftab, M. T., Zehra, F., Nadir, M. N., et al. (2019). Assessment of patient satisfaction following pharmacist counselling session by a novel patient satisfaction feedback on counselling questionnaire. JPHSR 10, 243–254. doi: 10.1111/jphs.12294
O’Brien, B., Viramontes, J. L. (1994). Willingness to pay: a valid and reliable measure of health state preference? Med. Decis. Making 14, 289–297. doi: 10.1177/0272989X9401400311
O’Brien, B. J., Goeree, R., Gafni, A., Torrance, G. W., Pauly, M. V., Erder, H., et al. (1998). Assessing the value of a new pharmaceutical: a feasibility study of contingent valuation in managed care. Med. Care 36, 370–384. doi: 10.1097/00005650-199803000-00013
Offodile, A. C., Ho, V. (2018). Making “Cents” for the Patient: Improving Health Care through Consumerism. Rice University’s Baker Institute for Public Policy. Issue Brief. Available from: https://www.bakerinstitute.org/media/files/files/0675c15a/bi-brief-032018-chb-consumerism-1.pdf (Accessed 21 November 2019).
Pavel, M. S., Chakrabarty, S., Gow, J. (2015). Assessing willingness to pay for health care quality improvements. BMC. Health Serv. Res. 15, 43. doi: 10.1186/s12913-015-0678-6
Poulas, G. A., Brodell, R. T., Mostow, E. N. (2008). Improving quality and patient satisfaction in dermatology office practice. Arch. Dermatol. 144, 263–265. doi: 10.1001/archdermatol.2007.58
Prakash, B. (2010). Patient satisfaction. J. Cutan. Aesthet. Surg. 3, 151–155. doi: 10.4103/0974-2077.74491
Reutzel, T. J., Furmaga, E. (1993). Willingness to pay for pharmacist services in a veterans administration hospital. J. Res. Pharm. Econ. 5, 89–114.
Schoenfelder, T., Klewer, J., Kugler, J. (2011). Determinants of patient satisfaction: a study among 39 hospitals in an in-patient setting in Germany. Int. J. Qual. Health Care 23, 503–509. doi: 10.1093/intqhc/mzr038
Shafie, A. A., Hassali, M. A. (2010). Willingness to pay for a pharmacist’s dispensing service: a cross-sectional pilot study in the state of Penang, Malaysia. Pharm. Pract. (Internet). 8, 116–121. doi: 10.4321/s1886-36552010000200006
Smith, D. L. (1983). APhA national survey: willingness of consumers to pay for pharmacists’ clinical services. Am. Pharm. 23, 58–64. doi: 10.1016/S0160-3450(16)32161-4
Suh, D. C. (2000). Consumers’ willingness to pay for pharmacy services that reduce risk of medication-related problems. J. Am. Pharm. Assoc. (Wash). 40, 818–827. doi: 10.1016/S1086-5802(16)31129-9
Suleiman, A. K. (2015). Stress and job satisfaction among pharmacists in Riyadh, Saudi Arabia. Saudi J. Med. Med. Sci. 3, 213–219. doi: 10.4103/1658-631X.162025
Tabbish, S. (2001). Hospital and Health Services Administration Principles and Practice (Oxford, UK: Oxford University Press), 699.
Taylor, S. J., Armour, C. L. (2002). Acceptability of willingness to pay techniques to consumers. Health Expect. 5, 341–356. doi: 10.1046/j.1369-6513.2002.00201.x
van Geffen, E. C., Philbert, D., van Boheemen, C., van Dijk, L., Bos, M. B., Bouvy, M. L. (2011). Patients’ satisfaction with information and experiences with counseling on cardiovascular medication received at the pharmacy. Patient Educ. Couns. 83, 303–309. doi: 10.1016/j.pec.2011.04.004
Wendy, L., Scott, G. (1994). Service Quality Improvement. The Customer Satisfaction Strategy for Health Care (Chicago, USA: AHA Company).
Keywords: patient satisfaction, counseling, willingness to pay, health services, community pharmacy service, hospital pharmacy service, pharmacoeconomics, cost benefit analyses
Citation: AlShayban DM, Naqvi AA, Islam MA, Almaskeen M, Almulla A, Alali M, AlQaroos A, Raafat M, Iqbal MS and Haseeb A (2020) Patient Satisfaction and Their Willingness to Pay for a Pharmacist Counseling Session in Hospital and Community Pharmacies in Saudi Healthcare Settings. Front. Pharmacol. 11:138. doi: 10.3389/fphar.2020.00138
Received: 12 November 2019; Accepted: 31 January 2020;
Published: 02 March 2020.
Edited by:
Maria Dimitrova, Medical University-Sofia, BulgariaReviewed by:
Maryam Farooqui, Qassim University, Saudi ArabiaJochen Fleischmann, Johnson & Johnson, Germany
Copyright © 2020 AlShayban, Naqvi, Islam, Almaskeen, Almulla, Alali, AlQaroos, Raafat, Iqbal and Haseeb. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Atta Abbas Naqvi, bmFxdmlhdHRhYWJiYXNAZ21haWwuY29t
 Dhfer Mahdi AlShayban
Dhfer Mahdi AlShayban Atta Abbas Naqvi
Atta Abbas Naqvi Md. Ashraful Islam
Md. Ashraful Islam Mohammed Almaskeen
Mohammed Almaskeen Ali Almulla
Ali Almulla Muhab Alali
Muhab Alali Abdullah AlQaroos
Abdullah AlQaroos Mohamed Raafat
Mohamed Raafat Muhammad Shahid Iqbal
Muhammad Shahid Iqbal Abdul Haseeb
Abdul Haseeb