- 1Department of Biological Sciences, Faculty of Science, King Abdulaziz University (KAU), Jeddah, Saudi Arabia
- 2Center of Excellence in Bionanoscience Research, King Abdulaziz University, Jeddah, Saudi Arabia
- 3Department of Comparative and Experimental Medicine, Graduate School of Medical Sciences, Nagoya City University, Nagoya, Japan
- 4National Gene Bank of Egypt (NGB), Agricultural Research Center (ARC), Giza, Egypt
- 5Food Business Promotion Division, ROHTO Pharmaceutical Co., Ltd., Osaka, Japan
- 6Department of Biology and Department of Chemistry, College of Science, University of Hafr Al Batin, Hafr Al Batin, Saudi Arabia
- 7Clinical Nutrition Department, Faculty of Applied Medical Sciences, King Abdulaziz University, Jeddah, Saudi Arabia
- 8Pharmacognosy Group, Department of Medicinal Chemistry, Biomedical Centre, Uppsala University, Uppsala, Sweden
Background: This study was designed to investigate Saudis' attitudes toward mental distress and psychotropic medication, attribution of causes, expected side effects, and to analyze participants' expectations toward alternative or complementary medicine using aromatic and medicinal plants, through a survey.
Method: The study included 674 participants (citizens and residents in Saudi Arabia) who were randomly contacted via email and social media and gave their consent to complete a questionnaire dealing with 39 items that can be clustered in six parts. Descriptive statistics and Chi-square for cross-tabulation were generated using SPSS.
Results: Among the 664 participants, 73.4% believed that there are some positive and negative outcomes of psychotropic medication. Participants (72.0%) think that the most important reason leading to psychological disorders is mainly due to the loss of a relative or beloved person, and 73.9% considered psychic session as one of the possible treatments of psychological disorders. Surprisingly, only 18.8% of the participants agreed that medicinal and aromatic plants could be a possible treatment of the psychological disorder. Participants (82%) consider that physicians are the most trustful and preferred source of information about alternative and complementary medicine.
Introduction
Mental health problems and disorders are becoming increasingly widespread throughout the world. The lifetime risk for any psychiatric disorder is ~50% (1). There appears to be a complex relationship between stressful situations, our mind, and the body's reaction to stress, and the onset of mental issues. The term “mental health literacy” was coined by Jorm et al. (2) It is defined as the “knowledge and beliefs about mental disorders, which help to promote, manage, and maintain good mental health” (1). It includes the ability to recognize specific disorders; knowing how to seek mental health information; knowledge of risk factors and sources of self-treatment and of professional help available; and attitudes that promote recognition and appropriate help-seeking (3). A multitude of factors such as socioeconomic status, isolation, discrimination (4), socio-demographic factors (5), race, and level of education (6), financial concerns, health problems, and communication difficulties (7) may affect mental health. How people come to understand their mental distress and attitude toward seeking professional help has been shown to be strongly rooted in wider cultural health beliefs (8, 9).
Recently, several strategies including education and communication have been designed to improve mental health literacy (3). However, few studies have been conducted to promote complementary and alternative medicine (CAM) based on aromatic and medicinal plants as an alternative for mental health care (10). CAM can be defined as “a group of diverse medical and health care systems, practices, and products that are not currently considered to be part of conventional medicine” (11).
The rising image of green consumerism, reduced faith in conventional treatments, and the growth in the availability of alternative remedies have contributed to the increased popularity of CAM around the world. In the United States of America, it was revealed through a national survey that the majority of CAM users are dissatisfied with conventional medicine and they consider CAM to be more congruent with their own values, beliefs, and philosophical orientation toward health and life (12). In Saudi Arabia, several traditional remedies are used for mental health care; although such practices are not well-documented and need to be sustained. To the best of our knowledge, there has been no study that examines Saudis' attitude toward mental distress and the professional use of aromatic and medicinal plants as CAM. Therefore, we conducted a survey among Saudi people to investigate the public's attitude toward mental distress problems and psychotropic drug treatment.
Locally, the percentage of Saudis who practice CAM lies between 33 and 93% (13). The knowledge of CAM derives mainly from family, friends, and media, while religion and local culture play a crucial role in enhancing the knowledge and the number of practitioners within the community. A limited number of studies have been published with regard to the use of CAM by patients in Saudi Arabian hospitals. However, a study has shown that there are various reasons that have driven cancer patients to use CAM as a treatment, whether it be as a mood enhancer, for pain control, as an immune system enhancer, for fitness purposes, or as an appetite enhancer (13). Not only has CAM been reported to be used among cancer patients, but also pregnant women have turned to it during pregnancy, labor, and post-birthing. In a study by Sameer et al., it was reported that 25.3% of Saudi women who participated in their study acknowledged the use of CAM during pregnancy, while a higher percentage used CAM during labor and almost half of the participants used CAM after delivery (14).
Methods
Study Design
The study was approved by the department of Biological Sciences at King Abdulaziz University as a part of a funded academic research. Participants were randomly contacted via social media and they were asked to give their consent to voluntarily participate to the current academic study without giving any detail about their personal details like names, address, email, phone number, among others. Those who did not agree were withdrawn from the study. Collected data was checked and coded by the principal investigators prior to data analysis.
Socio-Demographic Characteristics
Participants were asked to provide information on their age, gender, level of education, job, marital status, and living status. With regard to their cultural background, participants were asked to select their region of origin and to select whether they were Saudi's citizens or residents. In addition, they were asked to select their monthly income in Saudi Riyal (SR).
Beliefs About Psychological Disorders
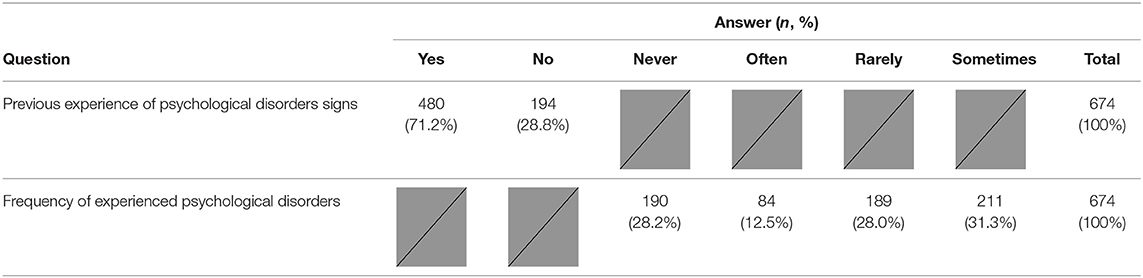
The participants' attitude toward mental distress and the relationship between their background and actual state of chronic disease was surveyed in the beliefs about psychological disorders (BPD) questionnaire. Questions about the recognition of the existence of a psychological disease and the individual's experience with mental distress were included. The first question was “Have you ever experienced signs and symptoms related to psychological disorders such as depression, anxiety, or stress?” Additional questions were about the frequency of these signs and symptoms. The first question was a Yes/No question. The next question dealt with the frequency of the experience psychological issue using the following scale: very often, occasionally, rarely, and never.
The next section mainly concerned the individual's experience regarding medications for physical or mental chronic disease and their side effects on the body and behavior. Answers ranged from positive effects, negative effects, no effects at all, or had neither positive nor negative side effects.
Attribution of Causes of Psychological Disorder and Potential Remedies
The attribution of causes of psychological disorder (ACPD) questionnaire was designed to assess the individual's attributions of cause and some possible remedies for psychological disorders. The APCD questionnaire included nine statements, which examined attributions reflecting (i) biological factors, (ii) psychosocial factors (work, study, or stressful events), (iii) environment factors, and (iv) supernatural factors (The evil eye, magic, astrology), which lead to mental distress, and the participants were also asked to add other possible causes that might lead to mental distress. These causal attribution dimensions were based on constructs in the studies of Al-Krenawi et al. (6). Possible remedies for psychological disorders in the survey included six statements, which investigated the preferred treatment approach such as relying on personal resources for help, pharmacotherapy medication, psychological consulting, meditation, diet, medicinal and aromatic plants, religious activities, and practicing sports. In addition, the participant was given the opportunity to add other remedies for the psychological disorders. The items were rated on a 3-point scale (yes = 1, maybe = 2, no = 3).
Expected Effects of Psychotherapy Medications and Perceived Influence of Ethnocultural Context
This questionnaire included six statements and was adapted from a previous study by Thorens et al. (9). It investigated the expected side effects of psychotropic agents by patients (positive or negative changes in character or attitude), interference of treatment with religious beliefs, and opinions of the individuals surrounding the patient, and the use of alternative medicines (complementary medicine, homeopathy, and traditional medicines). These items were given as Yes/No questions.
People's Opinion About Medicinal and Herbal–Based Functional Food Formulations
This questionnaire consists of four statements. Patients were requested to answer using yes or no responses regarding their preferred source of information about these products (doctor, herbalist, nutritionist, family, fellow patient, books and magazines, television, and the internet). We also asked participants to add another source of information. Finally, we added an open question related to the individual's suggestions about plants or herbs used traditionally for psychotherapy.
Study Participants
Participants were recruited through electronic media using several platforms. The study was conducted using a questionnaire written in Arabic from October 1st to October 17th, 2018. The participants included 674 adults from different Saudi regions.
Data Collection, Measures, and Statistical Analysis
Survey
Two preliminary versions were tested, thus permitting to reformulate or eliminate questions that were difficult to understand or ambiguous. The questionnaire dealt with the individual's concept of mental distress, attribution of causes, and remedies for psychological disorders. Several studies were conducted to predict treatment-seeking behavior across different ethnic groups, and across various age groups, including students and other adults, by administering self-reported questionnaires.
Data Analysis
Chi-square was calculated and significance were considered at p < 0.05. Data were analyzed using the IBM SPSS Version 25.0, 2017.
Results
Socio-Demographics of Participants
As shown in Table 1, a total of 674 participants agreed to participate in the survey with good male/female diversity: 304 (45.1%) males and 370 (54.9%) females. The majority of the participants were from the central region, which included the capital of Saudi Arabia (57.4%) followed by the western region (20.6%). Few participants responded to the survey from the other regions: 8.9% from the Eastern region, 6.4% from the Northern Region, 4.3% from the Southern Region, while very few participants (2.4%) originated from regions outside the Kingdom of Saudi Arabia. The majority of the participants were aged 18–30 years old (41.1%), while the fewest were over age 60 years (4.6%). Participants aged 31–40, 41–50, and 51–60 years old were 22.8, 16.0, and 15.4%, respectively. Most participants were Saudis (98.2%), with only (1.8%) from other nationalities. Over half of the participants were married (56.4%), while 39.9% of participants were single. The martial status with the fewest participants were divorced (2.7%) and widowed (1.0%). The participants who lived as a couple were 56.2%, while 37.7% responded that they still lived with their parents. Few of the participants lived alone or with roommates (4.5 and 1.6%, respectively). The majority of participants held a bachelor's degree (69.6%), while 11.6% of the total participants held higher degrees. The remaining 16% of the participants held a secondary school certificate, and the fewest participants indicated a middle school certificate as their educational level (2.8%). The occupations of the participants differed greatly, and included employees (24.7%), housekeepers (15.3%), retirees (14.4%), or students (13.8%). Also included were unemployed participants (8.9%) and merchants (1.3%). Financially, participants whose monthly income ranged between 11,000 and 20,000 SR were 29.1%, while participants having a monthly income ranging between 5,000 and 10,000 SR, and <5,000 SR were 25.4 and 25.5%, respectively. Finally, 18.8% of participants had a monthly income >20,000 SR.
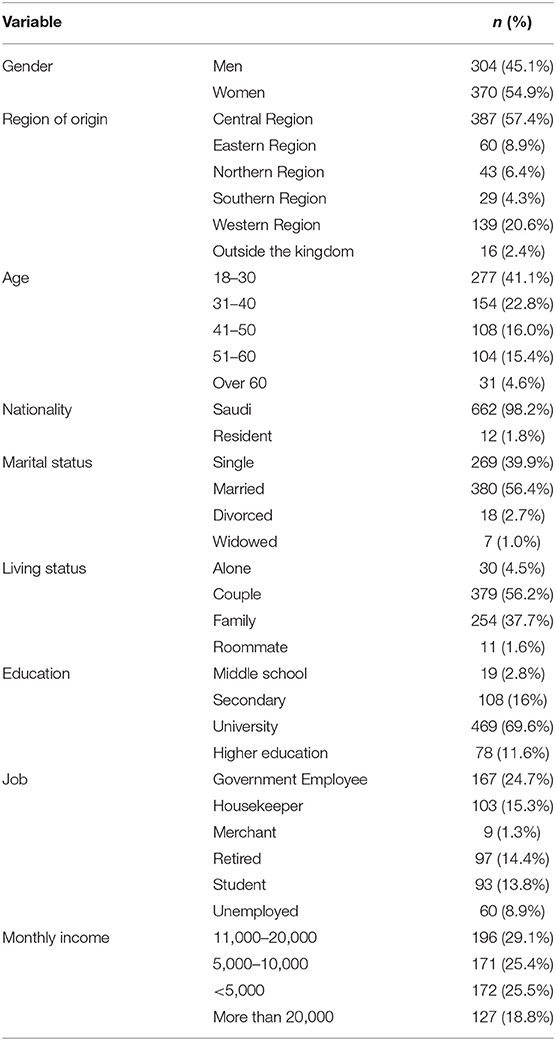
Table 1. The distribution of participants by gender, age, region, marital and living status, education, income, and occupation.
Perception About Experiencing Psychological Disorder Symptoms (BPD)
As shown in Table 2, participants were asked if they had experienced signs or symptoms related to psychological disorders. The majority of the participants acknowledged that they had experienced these signs (71.2%), while 28.8% of the participants said they have not experienced any signs or symptoms related to psychological disorders. For 31.1% of the participants, the intensity and the frequency of these signs were reported as “sometimes,” while 28% described symptom occurrence as “rarely” and 12.5% as “often.”
Expected Effects of Psychotherapy Medication, and Perceived Influence of Ethnocultural Context
As shown in Table 3, among the 664 participants, the majority (73.4%) believed that there were both positive and negative effects of psychotropic drugs on the treatment of psychological disorders, while 16.3% of the participants believed that there were only negative effects due to these drugs. Only 5.0% of participants believed that psychotropic drugs exerted positive effects, while 3.7% of the participants believed that these drugs did not have any therapeutic effects at all. With regard to the effects of psychotropic drugs on behavior and personality of the patients, 68.7% of the participants believed that there were both negative and positive effects on behavior and personality, while 14.2% of the participants believed that these drugs only exerted negative effects. Overall, 12.0% of the participants believed that psychotropic drugs had a positive effect on behavior and personality, and only 2.7% felt that there was no effect of these psychotropic drugs on the behavior and personality of the patients. Participants were also asked about the impact of the psychotropic drugs on the general functions of the human body: 47.9% stated that these agents had either a positive and negative influence on the general functions of the human body, while 36.6% believed that they had only negative effects. Participants believing that psychotropic drugs exerted positive effects on the general functions of the human body represented 4.3% of the total participants, while 9.5% of the participants felt that they had no effect.
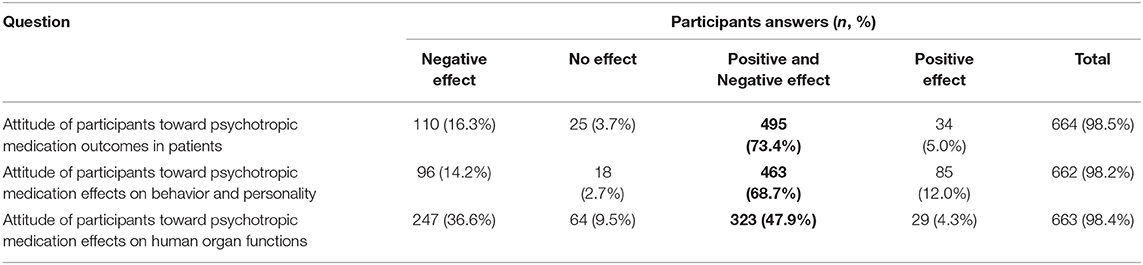
Table 3. Participants attitude toward psychotropic medication outcomes in general and their effect on behavior and body function in human.
Attribution of Causes of Psychological Disorder and Possible Remedies
As shown in Table 4, the most important causes of psychological disorders according to the participant's perspective were losing someone close (72.0%), stress form work and school (71.8%), and social responsibilities (70.2%). Almost half of the participants believed that a biological disorder was one of the most important causes of psychological disorders (50.6%). Environmental factors and genetics constituted the most important causes of psychological disorders according to 45.4% and 45.3% of the participants, respectively. In addition, 36.6% of the participants agreed that Black magic was a potential cause, while (36.5%) of participants agreed that the evil eye could be an attributed cause. Only 6.7% of the participants said that astrology leads to psychological disorders.
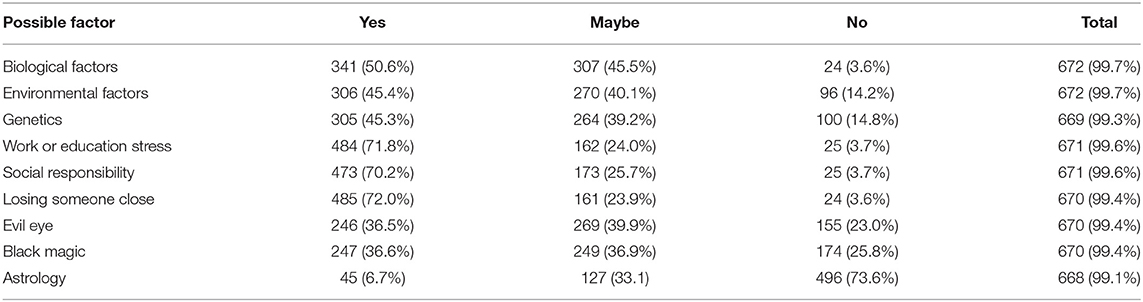
Table 4. Participants perception and beliefs about the most important factor leading to psychological disorders.
Participant's Opinions on Medicinal and Herbal–Based Functional Food Formulations
As shown in Table 5, 73.9% of the participants considered a psychic session could represent a possible treatment for psychological disorders, while 72.3% said that physical activities and sport are a possible treatment. In addition, 63.9% believed that religious activities were a possible treatment for psychological disorder, while prescribed medications (60.4%), diet (33.8%), spiritual exercise (23.1%), and medicinal and herbal plants (18.8%) also represented treatment alternatives.
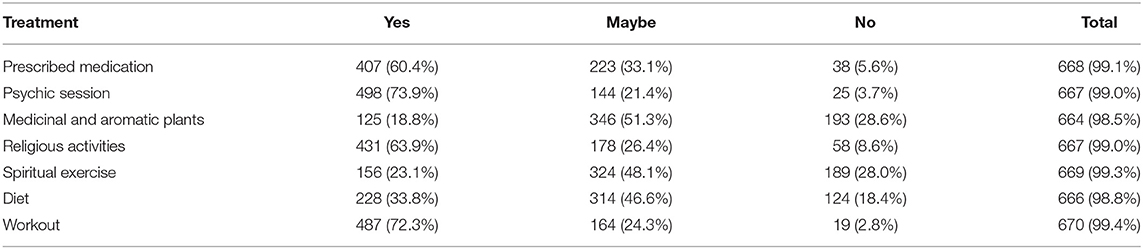
Table 5. Participants perception and beliefs about the possible treatment of psychological disorders.
As shown in Table 6, the majority of participants chose physicians as the preferred source of information for the usage of medicinal plants to treat psychological disorders (81.8%), while (63.9%) of the participants considered nutritionists as the preferred source of information. In addition, other patients (47.3%), the internet (46.9%), family members (36.4%), and herbalists (34.3%) were the preferred sources of information for treating psychological disorders. Books and magazines were the preferred sources for 30.0% of the participants, while TV was the least preferred source of information for 25.2% of participants.
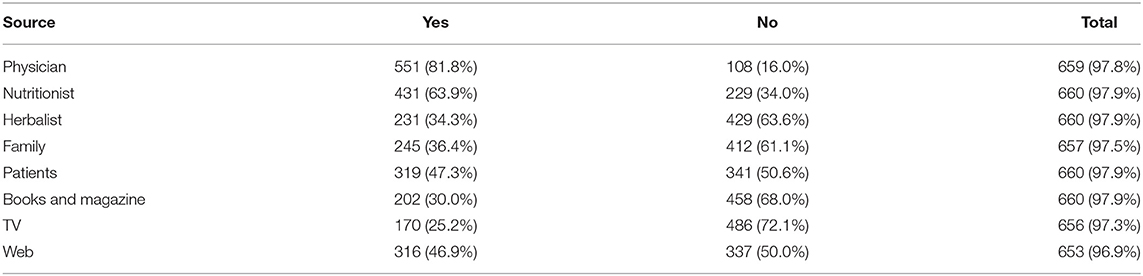
Table 6. Participants perception and beliefs about their preferred source of information to treat psychological disorders by medicinal plants.
As shown in Table 7, our results showed that the gender of the participants was significantly correlated with experiencing symptoms related to psychological disorders, although, there was no significant correlation in terms of the intensity of these symptoms. The age of the participant was significantly correlated with experiencing symptoms and their intensity and on the participant's perspective on the side effects of the drugs and on its effects on the normal function of the human body (Table 7 and Supplementary Material 1).
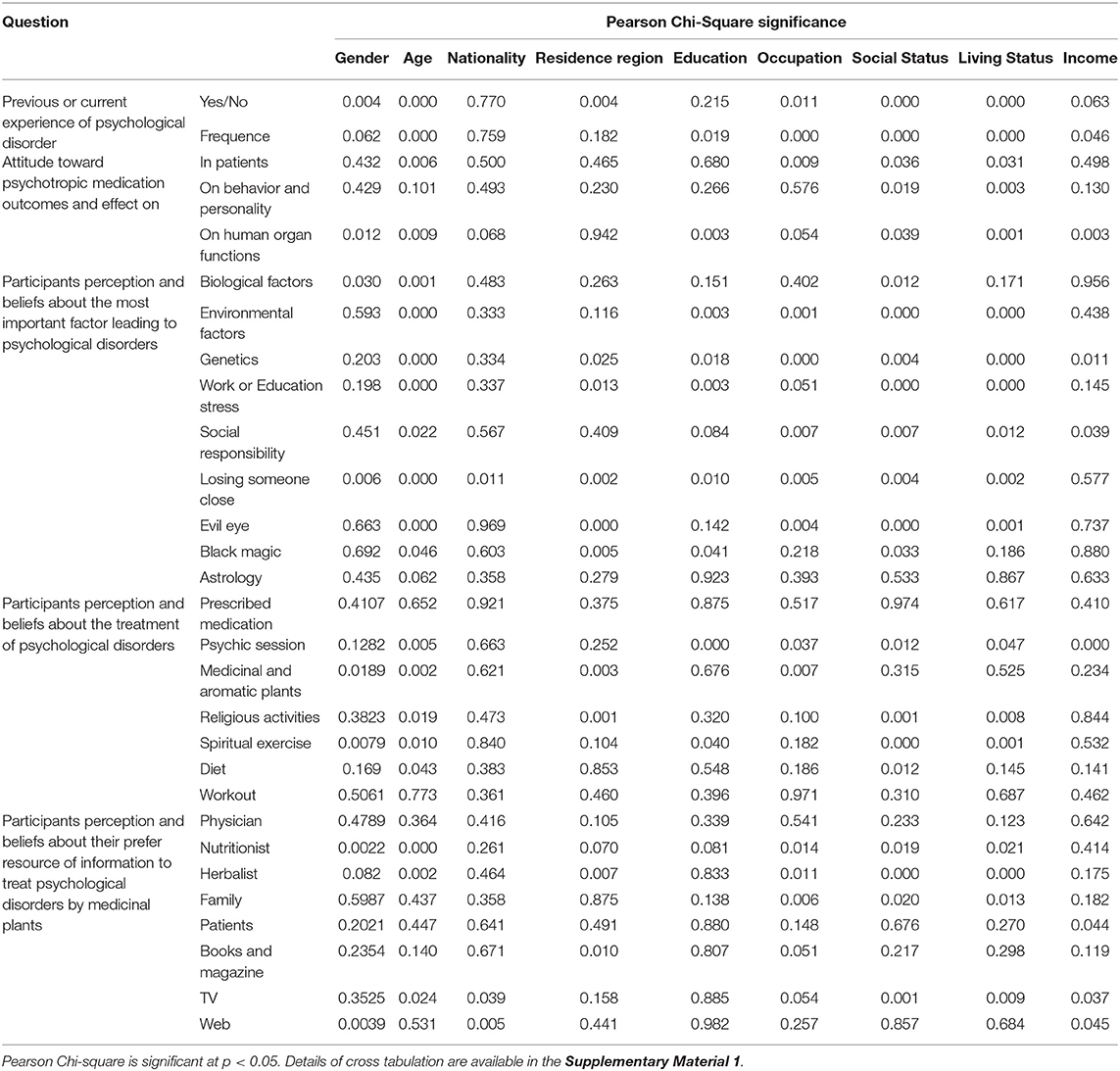
Table 7. Cross tabulation between participants' socio-demographic parameters and different survey question.
The region of residence of the participants was correlated with experiencing symptoms of psychological disorders. Furthermore, the educational level of the participants significantly correlated with the intensity of the psychological episode and with the participant's perspective of the impact of the psychotropic drugs on the normal function of the human body (Table 7 and Supplementary Material 1).
Occupation also showed a significant correlation with experiencing symptoms and their intensity, and also with participant's perspective on the side effects of the psychotropic agent. Furthermore, social status and living conditions of the participants were also significantly correlated with experiencing symptoms and their intensity, as were their perspective on the side effects of the medications and their influence on behavior and the normal function of the human body. The income of the participants also showed a significant correlation with the intensity of the symptoms and the participant perspectives on the impact of the psychotropic medications reflections on the normal function of the human body (Table 7 and Supplementary Material 1).
The participants' gender was also significantly correlated with biological factors and losing someone close as the most important causes leading to psychological disorders, while the age of the participant was significantly correlated with considering biological factors, environmental factors, genetics, stress from work or school, social responsibility, losing someone close, the evil eye, and black magic as the most important causes leading to psychological disorders. The nationality of the participants was significantly correlated only with considering losing someone close as the most important reason leading to a psychological disorder (Table 7 and Supplementary Material 1).
The educational level of the participants significantly correlated with choosing environmental factors, genetics, stress from work or school, losing someone close, and black magic as the most important causes leading to psychological disorders, while the participant's occupation significantly correlated with environmental factors, genetics, social responsibility, losing someone close, and the evil eye as causes of psychological disorders (Table 7 and Supplementary Material 1).
The perspective of surveyed participants with regard to potential treatments for psychological disorders was significantly correlated with the gender of the participant and also with considering medicinal and herbal plants and spiritual exercises as possible treatments, while the age of the participants correlated with choosing psychic sessions, religious activities, spiritual exercises, medicinal and herbal plants, and diet as possible forms of treatment. The educational level of the participants was significantly correlated with believing that psychic sessions and spiritual activities were possible treatments for psychological disorders, while occupation was correlated with considering psychic sessions and medicinal and herbal plants as possible treatments. The social status of the participants was significantly correlated with considering a psychic session, religious activities, spiritual exercise, and diet as possible treatments, while the living conditions of the participants was correlated with choosing psychic sessions, religious activities, and spiritual exercises as potential treatments. Monthly income correlated only with considering psychic sessions as a possible treatment (Table 7 and Supplementary Material 1).
The participants' perspective on their preferred source of information regarding medicinal plants to treat psychological disorders was significantly correlated with gender, age, region of residence, occupation, social status, living conditions, and monthly income of the participants. The gender of the participant was also correlated with considering nutritionists and the internet as preferred sources of information, while the age of the participants correlated with choosing nutritionists, herbalists, and the TV as sources of information. The participants' region of origin correlated with considering herbalists, and books and magazines, while the occupation of the participants showed a significant correlation with nutritionists, herbalists, and family as sources of information about medicinal plants to treat psychological disorders. Social and living status of the participants were correlated with considering nutritionists, herbalists, and family as sources of information (Table 7) and for more details about the cross tabulation between the sociodemographic parameters and the different survey question refer to the Supplementary Material 1.
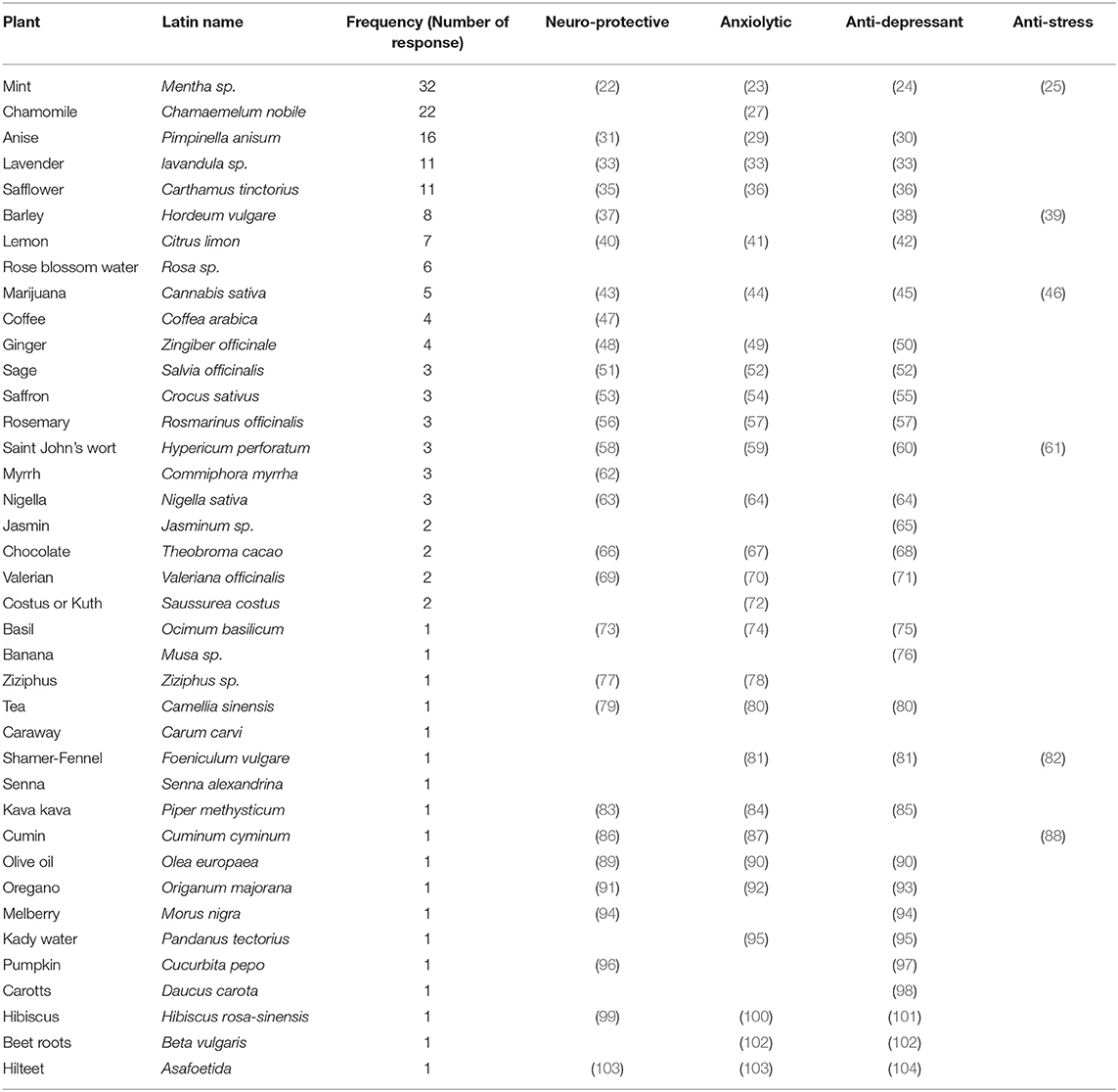
The participants were asked to suggest plants or herbs that they knew were traditionally used in psychotherapy. As shown in Table 8, the participants reported a total of 39 plants (Table 8, and references therein).
Discussion
The younger population is exposed to significant stress from social interactions, school, and work. Moreover, rapid changes are occurring in the global society due to technological expansion, which influences the quality of mental health (15). Thus, it is expected that a significant proportion of the respondents (71.2%) in our study are individuals who have experienced signs of psychological disorders such as depression or anxiety.
Male and females were equally distributed among the responders to our survey. However, the results showed a significantly higher correlation between the gender of the participant and experiencing of symptoms relating to psychological disorders. In this study, female participants (58.5%) more frequently experienced these symptoms than male participants (41.5%). Hormonal fluctuation is a possible factor that contributes to the increased prevalence of psychological disorders like depression among women, the global prevalence of depression in 2010 was 5.5% in women, while the prevalence among men was 3.2% (16).
The level of household income has been associated with the presence of mental disorders in some studies, while other studies have shown no association. A reduction of household income is associated with an increased risk for incident mental disorders (17). In our study, the monthly income of the participants was correlated with the intensity of the signs of psychological disorders: 38.1% of the participants who described the intensity of their signs of psychological disorder as “often” were from the lowest monthly income group while this percentage had an inverse relationship with the increase in monthly income.
In a study on postpartum depression in the western region of Saudi Arabia, among the causes and risk factors of postpartum depression, the least picked reasons by the participants were paranormal and supernatural causes such as the evil eye, ghosts, magic, and committing sins (18). In our study, the three least picked reasons chosen were black magic, the evil eye, and astrology. Some of these causes are based on a religious background, while others have a cultural background. The majority of the participants did not choose any of these reasons as the most important cause leading to psychological disorders. This reflects the perspective of the Saudis toward paranormal and supernatural events vs. reasons backed by logic and scientific reasoning in relation to human psychology.
Medicinal and herbal plants were the least picked agents for treatment of psychological disorders by the Saudis which reflects the low confidence in medicinal plants as a possible treatment option. In contrast, Saudis seem to have some belief in the application of alternative medicine and medicinal plants during pregnancy, post-delivery, and for some types of cancer symptoms (13, 14). In psychology-related disorders, our data showed doubts about the efficacy and safety of using alternative medicine and medicinal plants.
The results indicated a correlation between considering possible treatments for psychological disorders and gender, age, region of origin, educational level, occupation, social status, living conditions, and monthly income of the participants. However, the gender of the participant correlated significantly with considering spiritual activity as a possible treatment for psychological disorders, where 27.8% of the female participants believed in spiritual exercises compared to 17.7% of the male participants. While meditation could represent one of the spiritual exercises, the study shows that meditation might be more beneficial to females than to males due to differences in the mechanism of emotion regulation (19). This factor might explain why female participants showed a stronger belief in spiritual exercises than males in our study.
The 39 plants and herbs that were reported by the participants were a good start to building a local library of medicinal plants traditionally used for psychotherapy. Mint (Mentha sp.) was the most frequently cited plant among the answers, mentioned 32 times. Followed by chamomile (Chamaemelum nobile) suggested 22 times, anise (Pimpinella anisum) 16, lavender (lavendula sp.), and safflower (Carthamus tinctorius), 11 each. Most of the reported plants and herbs have been documented for their psychological properties such as neuroprotective, anxiolytic, anti-depressant, and anti-stress properties by its phytochemicals and secondary metabolites.
Mint (Mentha sp.) and its essential oils are popularly used in food, cosmetics, and pharmaceutical industries (20). Despite the different species of the plant, several studies have named carvone as its main active component (21). Mentha sp. has multiple biological activities that enhance its presence in CAM, and is used as a carminative, antispasmodic, diuretic, antibacterial, antifungal, and antioxidant agent. It has also been used to treat colds and flu, respiratory tract problems, gastralgia, hemorrhoids, and stomachache (20). As psychological treatment, several studies have reported that Menthe (Mentha sp.) has a neuroprotective, anxiolytic, anti-depressant, and anti-stress properties (22–25).
Chamomile (Chamaemelum nobile) dried flowers and its essential oil have been used in food and cosmetics. It has also been used as treatment for fever, inflammation, muscle spasms, gastrointestinal disorders, rheumatic pain, hemorrhoids, and other pathologies (26). Among the psychological properties, it has been reported that Chamomile (Chamaemelum nobile) has anxiolytic properties due to the presence of apigenin, which binds to central benzodiazepine receptors (27).
Anise (Pimpinella anisum) and its essential oil are used as flavoring and as an aromatic agent in food and has been used also as a digestive, carminative, and for gastrointestinal problems. Trans-anethole, estragole, γ-hymachalen, panisaldehyde, and methyl chavicol are considered the main constituents of the plant's oil (28). It has been reported that the extract of Anise seeds has an anxiolytic effect (29). In addition, the aqueous extract shows antidepressant-like effects (30). Its oil shows neuroprotective advantages as well (31).
Lavender (lavandula sp.) oil exerts antimicrobial activity in vitro and spasmolytic activity in vivo (32). It also exerts anxiolytic, anti-depressant-like effects, and neuroprotective properties (33).
Safflower (Carthamus tinctorius) has been used in food and traditional medicine due to its active compounds such as flavonoids, phenylethanoid glycosides, coumarins, fatty acids, and steroids to treat conditions such as dysmenorrhea, amenorrhea and other health issues (34). It has been shown that Safflower (Carthamus tinctorius) petal extract exerts neuroprotective, antidepressant, and antianxiety activities (35, 36). The list of suggested plants and their respective psychological properties are listed in Table 8.
Conclusion
This study revealed the surveyed participants' perceptions and beliefs about psychological disorder in general and their experience about using medicinal plants to treat mental distress. Surveyed Saudis in the study have shown good knowledge about complementary and alternative medicine. However, they have some concerns about its efficacy and safety. Moreover, they consider that physicians are the most trustful to prescribe aromatic and medicinal plants as a part of psychotherapy.
Data Availability Statement
The raw data supporting the conclusions of this article will be made available by the authors, without undue reservation.
Ethics Statement
Ethical review and approval was not required for the study on human participants in accordance with the local legislation and institutional requirements. The patients/participants provided their written informed consent to participate in this study.
Author Contributions
MA: conceptualization, data curation, formal analysis, methodology, writing—original draft, and review and editing. NH: conceptualization, data curation, funding acquisition, methodology, project administration, and review and editing. NA: data curation, formal analysis, methodology, and writing—original draft. HS: conceptualization, validation, methodology, and writing—original draft. MK and IA: formal analysis, methodology, validation, and review and editing. HZ: conceptualization, formal analysis, methodology, validation, and writing—original draft. AA and LA: formal analysis, methodology, validation, and writing—review and editing. YK: conceptualization, data curation, methodology, validation, and review and editing. HA and AH: formal analysis, funding acquisition, methodology, supervision, validation, and writing—review and editing. HE-S: conceptualization, validation, and review and editing. LJ: conceptualization, methodology, validation, and review and editing. JS: conceptualization, funding acquisition, methodology, project administration, supervision, validation, and review and editing. AE: conceptualization, data curation, formal analysis, funding acquisition, methodology, project administration, supervision, validation, writing—original draft, and review and editing. All authors contributed to the article and approved the submitted version.
Funding
This project was funded by Knowledge Economy & Technology Transfer Center, King Abdulaziz University (KAU), Jeddah, Saudi Arabia (Grant Number 004/2020).
Conflict of Interest
YK and LJ were employed by the company Rohto Pharmaceuticals.
The remaining authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Supplementary Material
The Supplementary Material for this article can be found online at: https://www.frontiersin.org/articles/10.3389/fpsyt.2021.577103/full#supplementary-material
References
1. Lauber C, Nordt C, Falcato L, Rössler W. Do people recognise mental illness? Eur Arch Psychiatry Clin Neurosci. (2003) 253:248–51. doi: 10.1007/s00406-003-0439-0
2. Jorm AF, Korten AE, Jacomb PA, Christensen H, Rodgers B, Pollitt P. ‘Mental health literacy': a survey of the public's ability to recognise mental disorders and their beliefs about the effectiveness of treatment. Med J Aust. (1997) 166:182–6. doi: 10.5694/j.1326-5377.1997.tb140071.x
3. Francis DD, Diorio J, Plotsky PM, Meaney MJ. Environmental enrichment reverses the effects of maternal separation on stress reactivity. J Neurosci. (2002) 22:7840–3. doi: 10.1523/JNEUROSCI.22-18-07840.2002
4. Murphy-Shigematsu S. Psychological barriers for international students in Japan. Int J Adv Counsel. (2002) 24:19–30. doi: 10.1023/A:1015076202649
5. Choi MR, Eun HJ, Yoo TP, Yun Y, Wood C, Kase M, et al. The effects of sociodemographic factors on psychiatric diagnosis. Psychiatry Investig. (2012) 9:199–208. doi: 10.4306/pi.2012.9.3.199
6. Al-Krenawi A, Graham JR, Al-Bedah EA, Kadri HM, Sehwail MA. Cross-national comparison of Middle Eastern university students: help-seeking behaviors, attitudes toward helping professionals, and cultural beliefs about mental health problems. Commun Ment Health J. (2009) 45:26–36. doi: 10.1007/s10597-008-9175-2
7. Hirai M, Clum GA, Ollendick H, Stephens RS. A cross-cultural comparisons of factors related to help-seeking attitudes for psychological disorder. [Thesis] Virginia Polytechnic Institute and State University, Blacksburg, VA, United States (1999).
8. Sheikh S, Furnham A. A cross-cultural study of mental health beliefs and attitudes towards seeking professional help. Soc Psychiatry Psychiatr Epidemiol. (2000) 35:326–34. doi: 10.1007/s001270050246
9. Thorens G, Gex-Fabry M, Zullino DF, Eytan A. Attitudes toward psychopharmacology among hospitalized patients from diverse ethno-cultural backgrounds. BMC Psychiatry. (2008) 8:55. doi: 10.1186/1471-244X-8-55
10. Holmes C, Ballard C. Aromatherapy in dementia. Adv Psychiatr Treat. (2004) 10:296–300. doi: 10.1192/apt.10.4.296
11. Holroyd E, Zhang A, Suen L, Xue C. Beliefs and attitudes towards complementary medicine among registered nurses in Hong Kong. Int J Nurs Stud. (2008) 45:1660–6. doi: 10.1016/j.ijnurstu.2008.04.003
12. Astin JA, Marie A, Pelletier KR, Hansen E, Haskell WL. A review of the incorporation of complementary and alternative medicine by mainstream physicians. Arch Intern Med. (1998) 158:2303–10. doi: 10.1001/archinte.158.21.2303
13. Abuelgasim K, Alsharhan Y, Alenzi T, Alhazzani A, Ali Y, Jazieh A. The use of complementary and alternative medicine by patients with cancer: a cross-sectional survey in Saudi Arabia. BMC Complement Altern Med. (2018) 18:88. doi: 10.1186/s12906-018-2150-8
14. Al-Ghamdi S, Aldossari K, Al-Zahrani J, Al-Shaalan F, Al-Sharif S, Al-Khurayji H, et al. Prevalence, knowledge and attitudes toward herbal medication use by Saudi women in the central region during pregnancy, during labor and after delivery. BMC Complement Altern Med. (2017) 17:196. doi: 10.1186/s12906-017-1714-3
15. Scott D, Valley B, Simecka B. Mental health concerns in the digital age. Int J Ment Health Addict. (2016) 15:604–13. doi: 10.1007/s11469-016-9684-0
16. Albert P. Why is depression more prevalent in women? J Psychiatry Neurosci. (2015) 40:219–21. doi: 10.1503/jpn.150205
17. Sareen J, Afifi T, McMillan K, Asmundson G. Relationship between household income and mental disorders. Arch Gen Psychiatry. (2011) 68:419. doi: 10.1001/archgenpsychiatry.2011.15
18. Ridha A, Abdullah A, Raghad K, Tagwa O. Public's knowledge, attitudes, and barriers to seek healthcare regarding postpartum depression in the Western Region of Saudi Arabia. Int J Women's Health Wellness. (2019) 5:102. doi: 10.23937/2474-1353/1510102
19. Rojiani R, Santoyo J, Rahrig H, Roth H, Britton W. Women benefit more than men in response to college-based meditation training. Front Psychol. (2017) 8:551. doi: 10.3389/fpsyg.2017.00551
20. Snoussi M, Noumi E, Trabelsi N, Flamini G, Papetti A, De Feo V. Mentha spicata essential oil: chemical composition, antioxidant and antibacterial activities against planktonic and biofilm cultures of Vibrio spp. Strains. Mol. (2015) 20:14402–24. doi: 10.3390/molecules200814402
21. Mahboubi M. Mentha spicata L. essential oil, phytochemistry and its effectiveness in flatulence. J Trad Complement Med. (2018) 1–7. doi: 10.1016/j.jtcme.2017.08.011
22. López V, Martín S, Gómez-Serranillos MP, Carretero ME, Jäger AK, Calvo MI. Neuroprotective and neurochemical properties of mint extracts. Phytother Res. (2010) 24:869–74. doi: 10.1002/ptr.3037
23. Caro D, Rivera D, Ocampo Y, Franco L, Salas R. Pharmacological evaluation of Mentha spicata L. and Plantago major L, medicinal plants used to treat anxiety and insomnia in Colombian Caribbean Coast. Evid Based Complement Altern Med. (2018) 2018:5921514. doi: 10.1155/2018/5921514
24. Jedi-Behnia B, AbbasiMaleki S, Mousavi E. The antidepressant-like effect of Mentha spicata essential oil in animal models of depression in male mice. J Fasa Univ Med Sci. (2017) 7:141–9.
25. Tian W, Akanda M, Islam A, Yang H, Lee S, Lee J, et al. The anti-stress effect of Mentha arvensis in immobilized rats. Int J Mol Sci. (2018) 19:355. doi: 10.3390/ijms19020355
26. Srivastava J, Shankar E, Gupta S. Chamomile: a herbal medicine of the past with a bright future (Review). Mol Med Rep. (2010) 3:895–901. doi: 10.3892/mmr.2010.377
27. Al-Snafi A. Medical importance of Anthemis Nobilis (Chamaemelum nobile) - a review. Asian J Pharmaceut Sci Technol. (2016) 6:89–95.
28. Shojaii A, Abdollahi Fard M. Review of pharmacological properties and chemical constituents of Pimpinella anisum. ISRN Pharm. (2012) 2012:510795. doi: 10.5402/2012/510795
29. Niksokhan M, Hedarieh N, Maryam N, Masoomeh N. Effect of hydro-alcholic extract of Pimpinella anisum seed on anxiety in male rat. J Gorgan Univ Med Sci. (2015) 16:28–33.
30. Shahamat Z, Abbasi-Maleki S, Mohammadi MS. Evaluation of antidepressant-like effects of aqueous and ethanolic extracts of Pimpinella anisum fruit in mice. Avicenna J Phytomed. (2016) 6:322–8.
31. Karimzadeh F, Hosseini M, Mangeng D, Alavi H, Hassanzadeh G, Bayat M, et al. Anticonvulsant and neuroprotective effects of Pimpinella anisum in rat brain. BMC Complement Altern Med. (2012) 12:12–76. doi: 10.1186/1472-6882-12-76
32. Chu CJ, Kemper KJ. Lavender (Lavandula ssp.). Longwood Herbal Task Force (2001). Available online at: https://naturalingredient.org/wp/wp-content/uploads/lavender-sedative.pdf (accessed March 5, 2020).
33. Koulivand P, Khaleghi Ghadiri M, Gorji A. Lavender and the nervous system. Evid Based Complement Altern Med. (2013) 2013:681304. doi: 10.1155/2013/681304
34. Delshad E, Yousefi M, Sasannezhad P, Ayati Z. Medical uses of Carthamus tinctorius L (Safflower): a comprehensive review from traditional medicine to modern medicine. Electr Phys. (2018) 10:6672–81. doi: 10.19082/6672
35. Hiramatsu M, Takahashi T, Komatsu M, Kido T, Kasahara Y. Antioxidant and neuroprotective activities of Mogami-benibana (Safflower, Carthamus tinctorius Linne). Neurochem Res. (2008) 34:795–805. doi: 10.1007/s11064-008-9884-5
36. Qazi N, Khan RA, Rizwani GH. Short communication-evaluation of antianxiety and antidepressant properties of Carthamus tinctorius L (Safflower) petal extract. Pak J Pharm Sci. (2015) 28:991–5.
37. Byun E, Kim K, Kim Y, Cho E, Min H, Lee J, et al. Comparison study of antioxidant activity and neuroprotective effects of barley sprout leaf, root, and stem ethanol extracts. J Kor Soc Food Sci Nutri. (2018) 47:973–80. doi: 10.3746/jkfn.2018.47.10.973
38. Yamaura K, Shimada M, Fukata H, Nakayama N, Bi Y, Ueno K. Antidepressant-like effects of young green barley leaf (Hordeum vulgare L.) in the mouse forced swimming test. Pharmacogn Res. (2012) 4:22. doi: 10.4103/0974-8490.91030
39. Yamaura K, Tanaka R, Bi Y, Fukata H, Oishi N, Sato H, et al. Protective effect of young green barley leaf (Hordeum vulgare L.) on restraint stress-induced decrease in hippocampal brain-derived neurotrophic factor in mice. Pharmacogn Mag. (2015) 11:86. doi: 10.4103/0973-1296.157702
40. Campêlo LM, Gonçalves FC, Feitosa CM, de Freitas RM. Antioxidant activity of Citrus limon essential oil in mouse hippocampus. Pharmaceut Biol. (2011) 49:709–15. doi: 10.3109/13880209.2010.541924
41. Khan R, Riaz A. Behavioral effects of Citrus limon in rats. Metab Brain Dis. (2015) 30:589–96. doi: 10.1007/s11011-014-9616-2
42. Lopes CML, Gonçalves SC, de Almeida AA, da Costa JP, Marques TH, Feitosa CM, et al. Sedative, anxiolytic and antidepressant activities of Citrus limon (Burn) essential oil in mice. Pharmazie. (2011) 66:623–27.
43. Iuvone T, Esposito G, Esposito R, Santamaria R, Di Rosa M, Izzo AA. Neuroprotective effect of cannabidiol, a non-psychoactive component from Cannabis sativa, on beta-amyloid-induced toxicity in PC12 cells. J Neurochem. (2004) 89:134–41. doi: 10.1111/j.1471-4159.2003.02327.x
44. Zuardi A, Crippa J, Hallak J, Moreira F, Guimarães F. Cannabidiol, a Cannabis sativa constituent, as an antipsychotic drug. Brazilian J Med Biol Res. (2006) 39:421–9. doi: 10.1590/S0100-879X2006000400001
45. El-Alfy A, Ivey K, Robinson K, Ahmed S, Radwan M, Slade D, et al. Antidepressant-like effect of Δ9-tetrahydrocannabinol and other cannabinoids isolated from Cannabis sativa L. Pharmacol Biochem Behav. (2010) 95:434–42. doi: 10.1016/j.pbb.2010.03.004
46. Gulluni N, Re T, Loiacono I, Lanzo G, Gori L, Macchi C, et al. Cannabis essential oil: a preliminary study for the evaluation of the brain effects. Evid Based Complement Altern Med. (2018) 2018:1709182. doi: 10.1155/2018/1709182
47. Jeong J, Jeong H, Jo Y, Kim H, Lee U, Heo H. Antioxidant and neuronal cell protective effects of columbia arabica coffee with different roasting conditions. Prev Nutr Food Sci. (2013) 18:30–37. doi: 10.3746/pnf.2013.18.1.030
48. M. Waggas, A. Neuroprotective evaluation of extract of Ginger (Zingiber officinale) root in monosodium glutamate-induced toxicity in different brain areas male albino rats. Pakistan J Biol Sci. (2009) 12:201–12. doi: 10.3923/pjbs.2009.201.212
49. Vishwakarma S, Pal S, Kasture V, Kasture S. Anxiolytic and antiemetic activity of Zingiber officinale. Phytother Res. (2002) 16:621–6. doi: 10.1002/ptr.948
50. Martinez DM, Barcellos A, Casaril AM, Savegnago L, Lernardão EJ. Antidepressant-like activity of dehydrozingerone: involvement of the serotonergic and noradrenergic systems. Pharmacol Biochem Behav. (2014) 127:111–7. doi: 10.1016/j.pbb.2014.10.010
51. Hamidpour M, Hamidpour R, Hamidpour S, Shahlari M. Chemistry, pharmacology, and medicinal property of sage (Salvia) to prevent and cure illnesses such as obesity, diabetes, depression, dementia, lupus, autism, heart disease, and cancer. J Trad Complement Med. (2014) 4:82–8. doi: 10.4103/2225-4110.130373
52. El Gabbas Z, Bezza K, Laadraoui J, Makbal R, Aboufatima R, Chait A. Salvia officinalis induces antidepressant-like effect, anxiolytic activity and learning improvement in hippocampal lesioned and intact adult rats. Bangladesh J Pharmacol. (2018) 13:367–78. doi: 10.3329/bjp.v13i4.38375
53. Mehri S, Abnous K, Mousavi S, Shariaty V, Hosseinzadeh H. Neuroprotective effect of Crocin on acrylamide-induced cytotoxicity in PC12 cells. Cell Mol Neurobiol. (2011) 32:227–35. doi: 10.1007/s10571-011-9752-8
54. Hosseinzadeh H, Noraei N. Anxiolytic and hypnotic effect of Crocus sativus aqueous extract and its constituents, crocin and safranal, in mice. Phytother Res. (2009) 23:768–74. doi: 10.1002/ptr.2597
55. Akhondzadeh Basti A, Moshiri E, Noorbala A, Jamshidi A, Abbasi S, Akhondzadeh S. Comparison of petal of Crocus sativus L. and fluoxetine in the treatment of depressed outpatients: a pilot double-blind randomized trial. Prog Neuropsychopharmacol Biol Psychiatry. (2007) 31:439–42. doi: 10.1016/j.pnpbp.2006.11.010
56. Park S, Kim S, Kim S. Neuroprotective effect of Rosmarinus officinalis extract on human dopaminergic cell line, SH-SY5Y. Cell Mol Neurobiol. (2010) 30:759–67. doi: 10.1007/s10571-010-9502-3
57. Ferlemi A, Katsikoudi A, Kontogianni V, Kellici T, Iatrou G, Lamari F, et al. Rosemary tea consumption results to anxiolytic- and anti-depressant-like behavior of adult male mice and inhibits all cerebral area and liver cholinesterase activity; phytochemical investigation and in silico studies. Chem Biol Interact. (2015) 237:47–57. doi: 10.1016/j.cbi.2015.04.013
58. Silva B, Dias A, Ferreres F, Malva J, Oliveira C. Neuroprotective effect of H. perforatum extracts on β-amyloid-induced neurotoxicity. Neurotoxic Res. (2004) 6:119–30. doi: 10.1007/BF03033214
59. Vandenbogaerde A, Zanoli P, Puia G, Truzzi C, Kamuhabwa A, De Witte P, et al. Evidence that total extract of Hypericum perforatum affects exploratory behavior and exerts anxiolytic effects in rats. Pharmacol Biochem Behav. (2000) 65:627–33. doi: 10.1016/S0091-3057(99)00233-6
60. Mennini T, Gobbi M. The antidepressant mechanism of Hypericum perforatum. Life Sci. (2004) 75:1021–7. doi: 10.1016/j.lfs.2004.04.005
61. Kumar V, Singh P, Bhattacharya S. Anti-stress activity of Indian Hypericum perforatum L. Indian J Exp Biol. (2001) 39:344–9.
62. Xu J, Guo Y, Zhao P, Xie C, Jin D, Hou W, et al. Neuroprotective cadinane sesquiterpenes from the resinous exudates of Commiphora myrrha. Fitoterapia. (2011) 82:1198–201. doi: 10.1016/j.fitote.2011.08.001
63. Hobbenaghi R, Javanbakht J, Sadeghzadeh S, Kheradmand D, Abdi F, Jaberi M, et al. Neuroprotective effects of Nigella sativa extract on cell death in hippocampal neurons following experimental global cerebral ischemia-reperfusion injury in rats. J Neurol Sci. (2014) 337:74–9. doi: 10.1016/j.jns.2013.11.019
64. Beheshti F, Norouzi F, Abareshi A, Anaeigoudari A, Hosseini M. Acute administration of Nigella sativa showed anxiolytic and anti-depression effects in rats. Curr Nutr Food Sci. (2019) 14:422–31. doi: 10.2174/1573401313666170607155858
65. Thaakur KA, Lavanya Y, Pradeepthi CH, Bindu P, Santh RT. Antidepressant like effects of Jasminum sambac-investigation of involvement of monoaminergic system. World J Pharmaceut Res. (2014) 3:755–70.
66. Ramiro-Puig E, Casadesús G, Lee H, Zhu X, McShea A, Perry G, et al. Neuroprotective effect of cocoa flavonids on in vitro oxidative stress. Eur J Nutr. (2008) 48:54–61. doi: 10.1007/s00394-008-0761-4
67. Yamada T, Yamada Y, Okano Y, Terashima T, Yokogoshi H. Anxiolytic effects of short- and long-term administration of cacao mass on rat elevated T-maze test. J Nutr Biochem. (2009) 20:948–55. doi: 10.1016/j.jnutbio.2008.08.007
68. Messaoudi M, Bisson J, Nejdi A, Rozan P, Javelot H. Antidepressant-like effects of a cocoa polyphenolic extract in Wistar-Unilever rats. Nutr Neurosci. (2008) 11:269–76. doi: 10.1179/147683008X344165
69. Malva J, Santos S, Macedo T. Neuroprotective properties of Valeriana officinalis extracts. Neurotoxic Res. (2004) 6:131–40. doi: 10.1007/BF03033215
70. Murphy K, Kubin Z, Shepherd J, Ettinger R. Valeriana officinalis root extracts have potent anxiolytic effects in laboratory rats. Phytomedicine. (2010) 17:674–8. doi: 10.1016/j.phymed.2009.10.020
71. Hattesohl M, Feistel B, Sievers H, Lehnfeld R, Hegger M, Winterhoff H. Extracts of Valeriana officinalis L. s.l. show anxiolytic and antidepressant effects but neither sedative nor myorelaxant properties. Phytomedicine. (2008) 15:2–15. doi: 10.1016/j.phymed.2007.11.027
72. Ambavade S, Mhetre N, Patil K, Desai T, Bodhankar S. Anxiolytic activity of root extracts of Saussurea lappa in mice. J Nat Remed. (2006) 6:103–8. doi: 10.18311/JNR/2006/450
73. Bora K, Arora S, Shri R. Role of Ocimum basilicum L. in prevention of ischemia and reperfusion-induced cerebral damage, and motor dysfunctions in mice brain. J Ethnopharmacol. (2011) 137:1360–5. doi: 10.1016/j.jep.2011.07.066
74. Zahra K, Khan M, Iqbal F. Oral supplementation of Ocimum basilicum has the potential to improves the locomotory, exploratory, anxiolytic behavior and learning in adult male albino mice. Neurol Sci. (2014) 36:73–8. doi: 10.1007/s10072-014-1913-3
75. Abdoly M, Farnam A, Fathiazad F, Khaki A, Khaki A, Ibrahimi A, et al. Antidepressant-like activities of Ocimum basilicum (sweet Basil) in the forced swimming test of rats exposed to electromagnetic field (EMF). Afr J Pharmacy Pharmacol. (2012) 6:211–15. doi: 10.5897/AJPP11.761
76. Dubey A, Reddy A, Handu S, Mediratta P, Shukla R, Ahmed Q. Effect of Musa sapientum stem extract on animal models of depression. Pharmacogn Res. (2016) 8:249. doi: 10.4103/0974-8490.188876
77. Waggas A, Al-Hasani R. Neurophysiological study on possible protective and therapeutic effects of Sidr (Zizyphus spina-christi L.) leaf extract in male albino rats treated with pentylenetetrazol. Saudi J Biol Sci. (2010) 17:269–74. doi: 10.1016/j.sjbs.2010.05.003
78. Setorki M. Effect of hydro-alcoholic extract of Ziziphus spina-christi against scopolamine-induced anxiety in rats. Bangladesh J Pharmacol. (2016) 11:421. doi: 10.3329/bjp.v11i2.26505
79. López V, Calvo MI. White Tea (Camellia sinensis Kuntze) exerts neuroprotection against hydrogen peroxide-induced toxicity in PC12 cells. Plant Foods Hum Nutr. (2011) 66:22–6. doi: 10.1007/s11130-010-0203-3
80. Siddiqui Z, Rizvi S, Tabassum I. Effects of Ocimum sanctum and Camellia sinensis on stress-induced anxiety and depression in male albino Rattus norvegicus. Indian J Pharmacol. (2010) 42:283. doi: 10.4103/0253-7613.70108
81. Ghazanfarpour M, Mohammadzadeh F, Shokrollahi P, Khadivzadeh T, Najafi MN, Hajirezaee H, et al. Effect of Foeniculum vulgare (fennel) on symptoms of depression and anxiety in postmenopausal women: a double-blind randomised controlled trial. J Obstetr Gynaecol. (2017) 38:121–6. doi: 10.1080/01443615.2017.1342229
82. Koppula S, Kumar H. Foeniculum vulgare Mill (Umbelliferae) attenuates stress and improves memory in Wister rats. Trop J Pharmaceut Res. (2013) 1:553–8. doi: 10.4314/tjpr.v12i4.17
83. Backhauβ C, Krieglstein J. Extract of kava (Piper methysticum) and its methysticin constituents protect brain tissue against ischemic damage in rodents. Eur J Pharmacol. (1992) 215:265–9. doi: 10.1016/0014-2999(92)90037-5
84. Garrett KM, Basmadjian G, Khan IA, Schaneberg BT, Seale TW. Extracts of kava (Piper methysticum) induce acute anxiolytic-like behavioral changes in mice. Psychopharmacology. (2003) 170:33–41. doi: 10.1007/s00213-003-1520-0
85. Sarris J, Kavanagh DJ, Byrne G, Bone KM, Adams J, Deed G. The Kava Anxiety Depression Spectrum Study (KADSS): a randomized, placebo-controlled crossover trial using an aqueous extract of Piper methysticum. Psychopharmacology. (2009) 205:399–407. doi: 10.1007/s00213-009-1549-9
86. Al-Snafi A. The pharmacological activities of Cuminum cyminum- a review. IOSR J Pharm. (2016) 6:46–65.
87. Jabeen A, Ramya B, Soujanya J, Bhattacharya B. Evaluation of anxiolytic, muscle relaxant & locomotor activity of Cuminum cyminum. J Med Plants Stud. (2017) 5:259–62.
88. Koppula S, Choi D. Cuminum cyminum extract attenuates scopolamine-induced memory loss and stress-induced urinary biochemical changes in rats: a noninvasive biochemical approach. Pharm Biol. (2011) 49:702–8. doi: 10.3109/13880209.2010.541923
89. Omar S. Cardioprotective and neuroprotective roles of oleuropein in olive. Saudi Pharm J. (2010) 18:111–21. doi: 10.1016/j.jsps.2010.05.005
90. Perveen T, Hashmi B, Haider S, Tabassum S, Saleem S, Siddiqui M. Role of monoaminergic system in the etiology of olive oil induced antidepressant and anxiolytic effects in rats. ISRN Pharmacol. (2013) 2013:615685. doi: 10.1155/2013/615685
91. Raafat K, Jassar H, Aboul-Ela M, El-Lakany A. Protective effects of Origanum majorana L. against neurodegeneration: fingerprinting, isolation and in vivo glycine receptors behavioral model. Int J Phytomed. (2013) 5:46–57.
92. Rezaie A, Mousavi G, Nazeri M, Jafari B, Ebadi A, Ahmadeh C, et al. Comparative study of sedative, pre-anesthetic and anti-anxiety effect of Origanum majorana extract with diazepam on Rats. Res J Biol Sci. (2011) 6:611–4. doi: 10.3923/rjbsci.2011.611.614
93. Abbasi-Maleki S, Kadkhoda Z, Taghizad-Farid R. The antidepressant-like effects of Origanum majorana essential oil on mice through monoaminergic modulation using the forced swimming test. J Trad Complement Med. (2019) 10:327–35. doi: 10.1016/j.jtcme.2019.01.003
94. Dalmagro A, Camargo A, Zeni A. Morus nigra and its major phenolic, syringic acid, have antidepressant-like and neuroprotective effects in mice. Metab Brain Dis. (2017) 32:1963–73. doi: 10.1007/s11011-017-0089-y
95. Bhatt PR, Bhatt KP. Neurobehavioral activity of Pandanus tectorius Parkinson (Pandanaceae) leaf extract in various experimental models. J PharmaSciTech. (2015) 5:16–8.
96. Zaib S, Khan M. Protective effect of Cucurbita pepo fruit peel against CCl4 induced neurotoxicity in rat. Pakistan J Pharm Sci. (2014) 27:1967–73.
97. Kim NR, Kim HY, Kim MH, Kim HM, Jeong HJ. Improvement of depressive behavior by Sweetme Sweet Pumpkin™ and its active compound, β-carotene. Life Sci. (2016) 147:39–45. doi: 10.1016/j.lfs.2016.01.036
98. Patibandla N, Bandaru N, Yamini K, Dhananjaneyulu M, Venkateswarlu V, Mubina M. Evaluation of antidepressant activity of ethanolic extract of Dacus carota in mice. J Pharm Sci Res. (2014) 6:73–77.
99. Nade V, Kawale L, Dwivedi S, Yadav A. Neuroprotective effect of Hibiscus rosa sinensis in an oxidative stress model of cerebral post-ischemic reperfusion injury in rats. Pharm Biol. (2010) 48:822–7. doi: 10.3109/13880200903283699
100. Mohammed J, Amber V, Manju S, Deependra S. Acute and chronic effect of Hibiscus rosa sinensis flower extract on anxiety induced exploratory and locomotor activity in mice. J Plant Sci. (2011) 6:102–7. doi: 10.3923/jps.2011.102.107
101. Shewale P, Hiray Y, Patil R. Antidepressant-like activity of anthocyanidins from Hibiscus rosa-sinensis flowers in tail suspension test and forced swim test. Indian J Pharmacol. (2012) 44:454–57. doi: 10.4103/0253-7613.99303
102. Sulakhiya K, Patel V, Saxena R, Dashore J, Srivastava A, Rathore M. Effect of Beta vulgaris Linn. Leaves extract on anxiety- and depressive-like behavior and oxidative stress in mice after acute restraint stress. Pharmacogn Res. (2016) 8:1–7. doi: 10.4103/0974-8490.171100
103. Amalraj A, Gopi S. Biological activities and medicinal properties of Asafoetida: a review. J Trad Complement Med. (2017) 7:347–59. doi: 10.1016/j.jtcme.2016.11.004
Keywords: alternative medicine, psychological disorder, psychopharmacology, survey, Saudi participants
Citation: Alegiry MH, Hajrah NH, Alzahrani NAY, Shawki HH, Khan M, Zrelli H, Atef A, Kim Y, Alsafari IA, Arfaoui L, Alharby HF, Hajar AS, El-Seedi H, Juneja LR, Sabir JSM and El Omri A (2021) Attitudes Toward Psychological Disorders and Alternative Medicine in Saudi Participants. Front. Psychiatry 12:577103. doi: 10.3389/fpsyt.2021.577103
Received: 07 July 2020; Accepted: 04 January 2021;
Published: 12 February 2021.
Edited by:
Wulf Rössler, Charité – Universitätsmedizin Berlin, GermanyReviewed by:
Mansour Adam Mahmoud, Taibah University, Saudi ArabiaEmad Masuadi, King Saud bin Abdulaziz University for Health Sciences, Saudi Arabia
Copyright © 2021 Alegiry, Hajrah, Alzahrani, Shawki, Khan, Zrelli, Atef, Kim, Alsafari, Arfaoui, Alharby, Hajar, El-Seedi, Juneja, Sabir and El Omri. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Abdelfatteh El Omri, b21yaWFiZGVsQGdtYWlsLmNvbQ==
†These authors have contributed equally to this work
 Mohamed H. Alegiry1†
Mohamed H. Alegiry1† Hossam H. Shawki
Hossam H. Shawki Abdelfatteh El Omri
Abdelfatteh El Omri