- 1Neglected Zoonotic Diseases, Department of Control of Neglected Tropical Diseases, World Health Organization, Geneva, Switzerland
- 2Global Alliance for Rabies Control, Manhattan, KS, USA
- 3World Organisation for Animal Health, Paris, France
- 4Institute of Epidemiology, Friedrich-Löffler-Institut, Federal Research Institute for Animal Health, Greifswald, Germany
- 5Veterinary Public Health Institute, University of Bern, Bern, Switzerland
- 6Food and Agriculture Organization of the United Nations, Bangkok, Thailand
- 7Department of Microbiology and Plant Pathology, Natural and Agricultural Sciences, University of Pretoria, Pretoria, South Africa
Rabies, a vaccine preventable neglected tropical disease, still claims an estimated 35,000–60,000 human lives annually. The international community, with more than 100 endemic countries, has set a global target of 0 human deaths from dog-transmitted rabies by 2030. While it has been proven in several countries and regions that elimination of rabies as a public health problem is feasible and tools are available, rabies deaths globally have not yet been prevented effectively. While there has been extensive rabies research, specific areas of implementation for control and elimination have not been sufficiently addressed. This article highlights some of the commonest perceived barriers for countries to implementing rabies control and elimination programs and discusses possible solutions for sociopolitical, organizational, technical, and resource-linked requirements, following the pillars of the global framework for the elimination of dog-mediated human rabies adopted at the global rabies meeting in December 2015.
Background
During the past decade, neglected tropical diseases (NTDs) have gained more recognition on the global health and development agendas (1–3). The transition from the Millennium Development Goals to the Sustainable Development Goals has renewed emphasis on ending the inequality that has deprived neglected communities from access to effective and affordable health care (Goal 3.8) and includes a specific goal to end NTDs by 2030 (Goal 3.3) (4).
Rabies, a viral disease categorized by the World Health Organization (WHO) as a NTD, kills tens of thousands of people every year, mostly among underserved populations in Africa and Asia; more than 95% of human rabies deaths result from the bites of infected dogs (5, 6). While the disease is almost 100% fatal, effective human and dog vaccines to prevent rabies are available. Elimination of dog-transmitted rabies as a public health problem is feasible (7, 8) by vaccinating dogs and providing post-exposure prophylaxis (PEP) to humans until dog rabies is eliminated (5).
Elimination of canine rabies is integral to the WHO–OIE1–FAO2 tripartite collaboration, which works at the animal–human–ecosystems interface (9, 10). A joint global meeting (Geneva, December 2015) marked a milestone at which human and animal health sectors agreed a framework to eliminate canine rabies with the vision of ending dog-mediated human rabies by 2030 (8) (Figure 1). All 180 Member countries of the OIE affirmed this commitment in Resolution N.26 adopted by the World Assembly of Delegates of the OIE in May 2016.3
Rabies is widely recognized as a public health threat that warrants prioritization of control efforts in Asia (11–13), Africa (14), and among the least developed nations globally (15). Health leaders are increasingly aware that this fatal disease could be eliminated as a public health problem cost effectively in a relatively short time (7, 16), yet rabies remains neglected and progress remains slow.
While there has been extensive research on the rabies virus, a comparative lack of operational research has led to knowledge gaps in how to design and implement control and elimination programs where they are needed most (11, 17) and calls for a “science of rabies elimination” (18). What barriers remain to coordinated efforts within and among countries? What is needed to transform the increased public and political awareness into real progress on the ground? And ultimately, what is needed to translate existing knowledge into success against rabies in a country? This paper discusses aspects of the “science to policy gap,” (perceived) barriers to progress and possible solutions (Table 1). It is structured according to the pillars of the Global framework for the elimination of dog-mediated human rabies (Figure 1), namely, sociocultural, technical, organization, political, and resources, reflecting a coordinated approach.
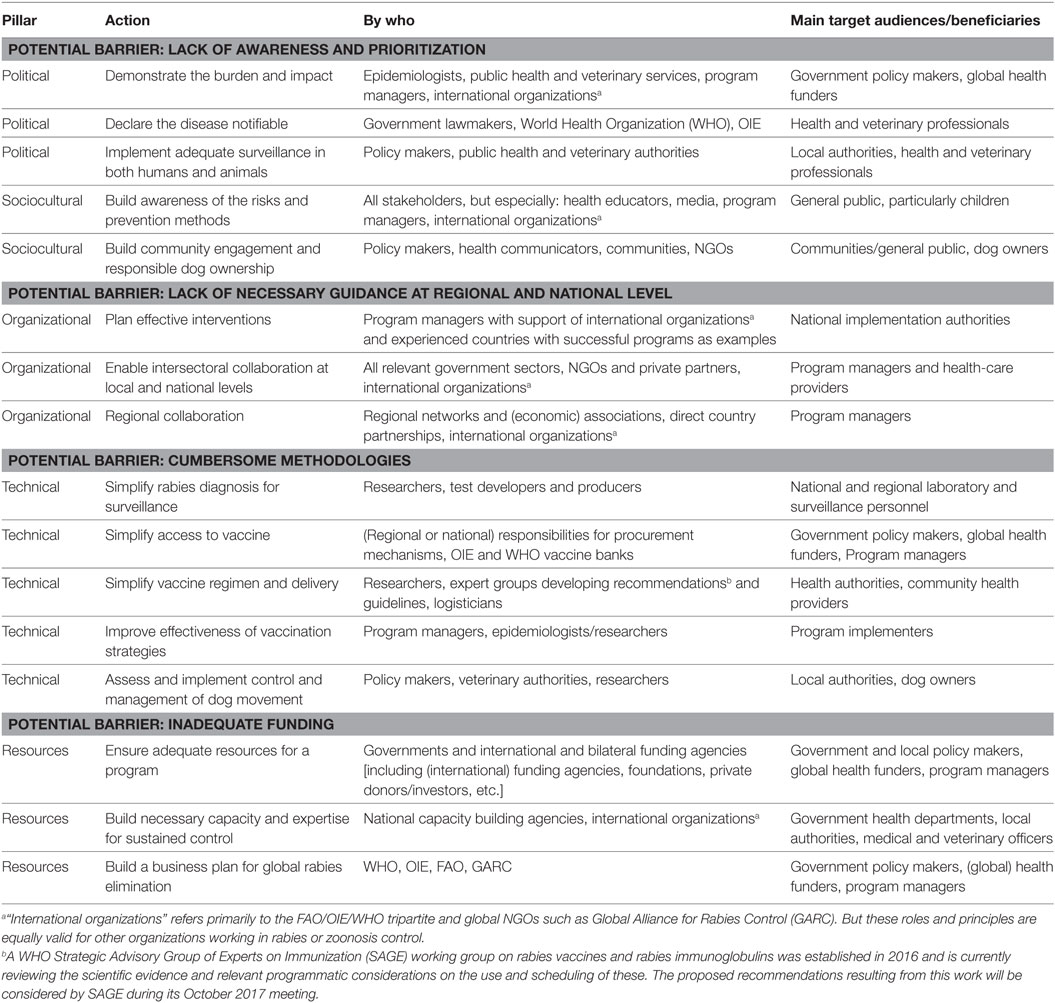
Table 1. Key areas for improvement, necessary actions, and the stakeholders required to take action to support programmatic success for canine rabies elimination.
Overcoming Barriers to Rabies Elimination
Political or Sociocultural—Raising Public Awareness and Political Will
Making the Burden Visible, Demonstrating Impact
Prioritization of a disease is brought about through increasing public awareness and political will (19). One of the most important means of convincing policy makers to prioritize a disease and invest resources is to demonstrate its impact on public health and the economy and the potential benefit of targeting the disease.
High-quality surveillance data are needed, but human rabies deaths are commonly underreported 100-fold (20–22), and the absence of data and solid evidence for estimates induces a cycle of neglect (23). Conversely, the onset of a control program that delivers better surveillance data is a precondition to increased awareness. Where quantitative assessments have been attempted, rabies has been ranked consistently among the top five zoonotic diseases, for example, in India (12), Mongolia (13), Jordan (24), Ethiopia (25), Myanmar (26), and Kenya (27).
Declaring a disease notifiable is crucial to establish functional reporting (28), and monitoring and surveillance of the disease should, therefore, be a central element of every rabies program. Rabies is also included in the OIE list of notifiable diseases.4 Disease surveillance starts at the community level, where awareness about the disease needs to be complemented by clear guidance on reporting to the authorities, ideally integrated into the wider national health information and statistics systems. Pathways must be included for transmission of data from the community level to the national level and to the OIE and WHO, resulting in feedback and action to keep individuals along the reporting chain informed and engaged. To ensure that data are comparable and informative, indicators should be well-defined and measurable. Novel technology such as notification via cell phones could be further explored (29).
Creating Public Awareness
Rabies burdens individuals, families, societies, and economies (6). As communities become aware of this threat, political pressure to act will accumulate. Building awareness and education about how to avoid and treat rabies exposures is, therefore, crucial in mobilizing a country to eliminate rabies. Champions at all levels (community to national) are central to this effort as they directly advocate and educate communities (7). World Rabies Day, recognized by the United Nations and commemorated every year on 28th September, celebrated its 10th anniversary in 2016 with 302 events in 57 countries (as of December 21, 2016). This annual awareness-raising event has shown a remarkable upwards trend since its inception and is an example of the dedication of innumerable people worldwide (30, 31).
Building an Engaged Society
An integral part of a regional or national plan is to build a proactive society that is fully engaged in the dog rabies elimination efforts of the country. Awareness of rabies at the community level alone is not enough to increase pressure on governments to improve their control efforts. Besides well-informed general public and responsible pet owners, committed, supportive policy makers are needed who will cohesively support national efforts to achieve and maintain freedom from rabies. Currently, most efforts to raise public awareness focus on promoting rabies information, which may not translate into the desired behavior, practices, and actions. Thus, it is important to invest in a national communication strategy and in impact monitoring that use the science of behavioral change and consider the diverse behavioral drivers, incentives, motivations, and larger sociocultural context of the target audience.
An example of behavioral change necessary for rabies control is that owners accept responsibility for their dogs and any offspring they may produce. This includes protecting dogs from rabies through vaccination and from unwanted reproduction. The promotion of such responsible dog ownership can be achieved only through a combination of adequate legislation, public awareness, and education, recognizing cultural and economic conditions. Public health and veterinary authorities, animal welfare organizations, and private veterinarians should work together to establish and maintain responsible dog ownership programs especially in communities at risk.
Organizational—Establishing Necessary Policies and Guidance
Effective Planning of Elimination Programs
National authorities are responsible for developing national strategies and implementing programs but they are frequently overwhelmed by multiple human and animal disease priorities and the challenges associated with programs stretched across sectors and administrative levels. It may be difficult to know where to start and what is needed—a potential barrier. Guidance for developing and monitoring control and elimination programs is, however, freely available. For example, the Stepwise Approach toward Rabies Elimination, which is embedded in the rabies blueprint,5 follows the principles of enhancing intersectoral collaboration. This guidance has been used by countries across three continents, mostly at national or regional stakeholder consultations, to kick-start coordinated rabies control (32). Likewise, the rabies surveillance blueprint6 provides guidance for planning of surveillance in particular. Knowledge about these tools needs to be disseminated and promoted more widely.
Intersectoral Collaboration
While the incremental benefits of a One Health approach for rabies control are established at the highest international level, its operationalization at national or local levels remains a challenge. Administrative and management structures may need to be harmonized across sectors according to different ministries and budget lines and coordinated with stakeholders from the private sector (33). National stakeholder consultations that convene all actors across ministries, local and national levels as well as the private and public sectors, however, have proven excellent platforms from which to build connections and trust and from where operational barriers and constraints to effective collaboration in rabies prevention as well as possible solutions can be explored. The outcome of these consultations is the drafting of integrated, multidisciplinary rabies action plans (34). For example, coordination at the national level can pave the way for integrated management of bite cases at the local level, jointly involving human and animal professionals to ensure reporting of bite and rabies incidents, proper risk assessments, and a coordinated response while at the same time sharing logistic resources (35, 36). Close involvement of social sciences, the education sector, and municipalities is now equally recognized, for example, as a powerful method for preventing dog bites in children, increasing knowledge and awareness about rabies, and in sustainably managing dog populations in affected communities (36).
Sharing and Comparing: Transparency and Regional Collaboration
International cooperation and coordination in planning, implementing, and evaluating rabies control programs at all levels is crucial for success and cost effectiveness (5). As canine rabies is a transboundary disease, collaboration, cooperation, and transparency between countries can provide new insights for tackling the disease. Authorities often perceive admitting public health problems as failure and prefer not to address endemic rabies at international level, thereby missing an opportunity to share information. Establishing contacts between public health and veterinary authorities of neighboring regions and countries and frequently exchanging information and data can be a first step toward building trust and more regular bilateral or multilateral interaction. WHO collaborating centers, OIE, and FAO reference laboratories and other organizations can help countries to share, compare, and learn from each other’s experience (5, 37). Participation at international disease conferences can also attract more international attention at a political level.
A regional approach has been fundamentally important for the effective control of rabies in Western Europe (5) and, more recently, Latin America (38). Rabies control program managers from across Latin America and the Caribbean meet at meetings facilitated by the Pan American Health Organization (REDIPRA) and the large scale, parallel declines in dog and human rabies achieved are striking (39). In Asia, the Association of Southeast Asian Nations launched a joint Rabies Elimination Strategy that encapsulates a regional approach in 2015.7 The Middle Eastern, Eastern Europe, Central Asia, and North Africa Rabies Experts Bureau has held meetings since 2010 (40) and has called for a strong regional initiative with high level political support (41). In sub-Saharan Africa, the Pan-African Rabies Control Network was created in 2015 and shows promise as a suitable platform to drive a regional approach to rabies control (37). Such regional approaches will be vital to implementing the global strategic framework to eliminate dog-mediated rabies and will, therefore, require further extension with strong participation and political support from all countries for success.
Technical—Ensuring Necessary Technology and Knowledge
Diagnostics
Diagnostic tests confirm animal rabies cases, allowing better PEP decision-making and monitoring the progress of control efforts. The reference, fluorescent antibody test, is not practicable in many endemic settings due to costs and enhanced laboratory requirements. Thus, alternative tools using less specialized equipment, such as Direct Rapid Immunohistochemical Test (42) and lateral flow devices (43), could play an important role provided further validation and quality approval.
Predicting the Need for Vaccine: Forecasting
Manufacturing cycles of both human and animal rabies vaccines require several years of appropriate forecasting by countries in order to supply the actual need. An absence of accurate data impairs forecasting and thereby resource allocation. The veterinary services of endemic countries often have insufficient knowledge of dog population size or ecology and human health services lack accurate data on bite case exposures. Both sectors thus suffer from procurement delays or stock shortages, which can result in less effective control of the disease and may force countries to turn to manufacturers selling vaccines that are overly expensive or may not meet international quality standards (44). Vaccine banks or stockpiles at regional levels as managed by OIE or WHO have become a solid mechanism for countries to maintain the supply of quality-assured vaccines and allow manufacturers to forecast and stabilize their production over years with lowered pricing through bulk purchase (45). Moreover, vaccine banks have contributed demonstrably to the scaling up and maintenance of local, national, or sub-regional programs in Asia and Africa (46) and incentivized recipient countries to increase data collection, as reporting on vaccine use and results is required. The opportunity of a potential investment from GAVI (the Vaccine Alliance) into human rabies vaccine from 2018 onward (47) could substantially facilitate low-income countries’ access to affordable rabies vaccine and stimulate the necessary political will to tackle human rabies at a large scale.
Getting the Vaccines to the Community
Despite the encouraging improvements observed in the field of universal health coverage, poor accessibility to and affordability of PEP [particularly of rabies immunoglobulin (RIG)] remain in most rabies-endemic countries (48). Certainly, progress has been made, for example, on shortening PEP regimens (fewer health facility visits) and countries changing their policy to cost-saving intradermal administration of rabies vaccines as recommended by WHO (49). There is hope that new technologies currently under evaluation by WHO (thermostable rabies vaccine, monoclonal antibodies as an alternative to human and equine RIG) will facilitate cost-effective delivery of PEP as well as dog vaccine to where it is needed. The long needed scale up and adaption of mechanisms for supply and distribution of PEP has received a global push through discussions around a potential GAVI investment.
More Tailored Dog Vaccination Strategies
Rabies is integrally linked to the ways people live with their dogs. Its control requires an adequate understanding of the dog ecology and dog-keeping practices in a country in locally differing sociocultural contexts (e.g., urban vs rural, among different economic, religious, or ethnic groups). Factors that can profoundly affect rabies transmission and control are usually not sufficiently understood to design the most appropriate control strategy, and as a result, efforts and resources can be wasted. In most circumstances, almost all dogs can be handled and vaccinated by the parenteral route (50). In rare cases, however, dogs may not be accessible to parenteral vaccination, thus jeopardizing the coverage of vaccination campaigns. Improved dog capture and vaccination techniques, as shown through the establishment of rabies A-teams by FAO in Bali, can assist with reaching dogs that are difficult to capture and handle.8 Oral dog vaccination using a hand-out model may be used effectively to immunize those inaccessible dogs while ensuring the safety of the vaccinators, the community, and non-target species. The best feasible solution for long-lasting marking of vaccinated dogs should be decided on during planning of campaigns (51).
The lack in dog movement control has been attributed as responsible for rabies spread in endemic areas and incursion in previously free countries or regions. Vaccinating at least 70% of animals in order to eliminate rabies from a free-roaming dog population is a widely acknowledged recommendation (8). However, empirical work [e.g., on area-specific basic reproductive ratio (R0) (52)] suggests that different settings probably require different vaccination strategies and coverages to control rabies successfully. High vaccination coverage in high-risk areas may be more crucial than medium coverage across the whole country, but clear guidance on this is lacking. Better knowledge of area/country specific factors related to dog-keeping practices, dog population turnover, and contact rates between dogs and wildlife can help in determining a more flexible, realistic required dog vaccination coverage. This can help to optimize resource allocation (53, 54) and define the most appropriate vaccination strategies and financing (55), the best vaccination campaign frequency (52), and how to target vaccination to the highest risk areas and segments of the dog population.
Making Resources Available
As for any public health program, sustainable funding sources are a precondition to starting a rabies control program, and the absence of those sources is one of the main barriers. There are ways, however, to reduce the investments necessary for rabies control and to integrate rabies into existing streams of work and financing.
Recognizing rabies control as a public good and thus as the responsibility of national governments is key to a sustainable rabies elimination effort. Donor contributions should be structured so as to be catalytic to the establishment of the program, and long-term dependence on donor support should be avoided through a well-planned strategy for donor exit.
In most rabies-endemic countries, human PEP and vaccinating animals against rabies remain an “out-of-pocket” market. As they build on their commitments to universal health coverage and the sustainable development goals (56), governments need to step up their funding and integrate rabies control into sustainable health plans, ensuring dog vaccination, and PEP are available at the primary health-care level. Costs can be substantially decreased by using the intradermal route for human vaccines and tailoring dog vaccination to local circumstances (see above). Rabies surveillance and control in dogs should be integrated into existing infectious diseases reporting mechanisms and vaccination programs, requiring also more integration of funding streams. For example, in the Philippines, the ministry of health invests in dog vaccination as a public health measure, creating a leverage effect (57). Innovative mechanisms for financing and cost sharing can help to make vaccine purchase more affordable. To support funding bodies in planning and costing, WHO is currently developing in collaboration with FAO, OIE, and the Global Alliance for Rabies Control, a comprehensive business plan that encompasses both human and animal perspectives for achieving the 2030 target. In the longer term, investing in rabies prevention and control is cost-efficient, saving both lives and money (16, 58). It is possible to start small and then unlock more investment by demonstrating value.
Capacity building is an investment in human resources with crucial importance for the sustainability of a project. Parallel to the technical efforts made by the country, plans to build related capacity through training, professional development, and/or continuing education will ensure quality at implementation and ensure future sustainability. This contribution to health systems’ strengthening can be a legacy that rabies control efforts leave to a nation.
Conclusion
This paper describes some of the main technical, organizational, and political challenges that countries encounter when implementing measures to control and eliminate rabies. However, there are solutions to many of these perceived barriers and opportunities to fill existing gaps. As summarized in Table 1, health officials, program managers, donors/investors, and all those involved in development of strategies should be aware of those applicable to their local, national, and regional contexts as early as possible, to make coordinated, informed decisions and successfully fight this devastating disease.
Author Contributions
BA-R, LT, and AF prepared the initial concept for this paper. All the authors contributed equally to the further development of the content, delivered specific paragraphs for the paper from their area of expertise, and reviewed and complemented the manuscript. AF coordinated and collated the coauthor’s input.
Conflict of Interest Statement
The authors declare an absence of any commercial or financial relationships to the content of the paper that could constitute a potential conflict of interest.
The reviewer ENJ and handling editor declared their shared affiliation, and the handling editor states that the process nevertheless met the standards of a fair and objective review.
Acknowledgments
The authors thank hundreds of tireless rabies fighters around the globe who do not cease to work hard for awareness, education, and vaccination and save lives by doing so. Dongwook Kim contributed significantly to the literature search for this article and the authors thank him for this contribution.
Funding
All authors contributed to this article as a part of their professional mandate.
Footnotes
- ^World Organization for Animal Health.
- ^Food and Agriculture Organization of the United Nations.
- ^http://www.oie.int/fileadmin/Home/eng/About_us/docs/pdf/Session/2016/A_RESO_2016_public.pdf.
- ^http://www.oie.int/en/international-standard-setting/terrestrial-code/access-online/.
- ^http://caninerabiesblueprint.org/.
- ^http://rabiessurveillanceblueprint.org/.
- ^http://vncdc.gov.vn/files/article_attachment/2015/3/endorsed-ares-final.pdf.
- ^http://www.fao.org/indonesia/news/detail-events/en/c/411271/.
References
1. WHO. Working to Overcome the Global Impact of Neglected Tropical Diseases. First WHO Report on Neglected Tropical Diseases. Geneva: WHO (2010).
2. Uniting to Combat Neglected Tropical Diseases. London Declaration on Neglected Tropical Diseases (2012). Available from: http://unitingtocombatntds.org/london-declaration
3. WHO. WHA66.12 Sixty-Sixth World Health Assembly Resolution on Neglected Tropical Diseases 2013 (2013). Available from: http://www.who.int/neglected_diseases/mediacentre/WHA_66.12_Eng.pdf
4. United Nations. Sustainable Development Knowledge Platform: Goal 3 2015 (2015). Available from: https://sustainabledevelopment.un.org/sdg3
6. Hampson K, Coudeville L, Lembo T, Sambo M, Kieffer A, Attlan M, et al. Estimating the global burden of endemic canine rabies. PLoS Negl Trop Dis (2015) 9(4):e0003709. doi: 10.1371/journal.pntd.0003709
7. WHO. Rabies: Rationale for Investing in the Global Elimination of Dog-Mediated Human Rabies. Geneva: World Health Organization (2015).
8. WHO, OIE. Global elimination of dog-mediated human rabies: the time is now! Report of the Rabies Global Conference 10-11 December 2015, Geneva, Switzerland. Paris: World Health Organization and World Organisation for Animal Health (2016). p. 27. Available from: http://apps.who.int/iris/bitstream/10665/204621/1/WHO_HTM_NTD_NZD_2016.02_eng.pdf?ua=1
9. OIE. Forum: rabies is a tripartite (WHO-OIE-FAO) priority – collaboration between animal and human health sectors. Bulletin de lOIE (2014) 3:3–4.
10. FAO/OIE/WHO. The FAO-OIE-WHO Collaboration. Sharing Responsibilities and Coordinating Global Activities to Address Health Risks at the Animal-Human-Ecosystems Interfaces. A Tripartite Concept Note. Hanoi: FAO/OIE/WHO (2010).
11. Abbas SS, Kakkar M. Rabies control in India: a need to close the gap between research and policy. Bull World Health Organ (2015) 93(2):131–2. doi:10.2471/BLT.14.140723
12. Sekar N, Shah NK, Abbas SS, Kakkar M; Roadmap to Combat Zoonoses in India Initiative. Research options for controlling zoonotic disease in India, 2010-2015. PLoS One (2011) 6:e17120. doi:10.1371/journal.pone.0017120
13. McFadden AM, Muellner P, Baljinnyam Z, Vink D, Wilson N. Use of multicriteria risk ranking of zoonotic diseases in a developing country: case study of Mongolia. Zoonoses Public Health (2016) 63:138–51. doi:10.1111/zph.12214
14. Grace D, Songe M, Knight-Jones T. Impact of neglected diseases on animal productivity and public health in Africa. 21st Conference of the OIE Regional Commission for Africa 16th-20th February. Rabat, Morocco (2015).
16. Shwiff S, Hampson K, Anderson A. Potential economic benefits of eliminating canine rabies. Antiviral Res (2013) 98(2):352–6. doi:10.1016/j.antiviral.2013.03.004
17. Yin W, Dong J, Tu C, Edwards J, Guo F, Zhou H, et al. Challenges and needs for China to eliminate rabies. Infect Dis Poverty (2013) 2(1):23. doi:10.1186/2049-9957-2-23
18. Zinsstag J. Towards a science of rabies elimination. Infect Dis Poverty (2013) 2(1):22. doi:10.1186/2049-9957-2-22
19. Mangen MJ, Batz MB, Käsbohrer A, Hald T, Morris JG, Taylor M, et al. Integrated approaches for the public health prioritization of foodborne and zoonotic pathogens. Risk Anal (2010) 30(5):782–97. doi:10.1111/j.1539-6924.2009.01291.x
20. Taylor LH, Hampson K, Fahrion A, Abela-Ridder B, Nel LH. Difficulties in estimating the human burden of canine rabies. Acta Trop (2017) 165:133–40. doi:10.1016/j.actatropica.2015.12.007
21. Cleaveland S, Fevre EM, Kaare M, Coleman PG. Estimating human rabies mortality in the United Republic of Tanzania from dog bite injuries. Bull World Health Organ (2002) 80:304–10.
22. Fahrion AS, Mikhailov A, Abela-Ridder B, Giacinti J, Harriesa J. Human rabies transmitted by dogs: current status of global data, 2015. Wkly Epidemiol Rec (2016) 91:13–20.
23. Taylor LH, Nel LH. Global epidemiology of canine rabies: past, present, and future prospects. Vet Med (2015) 6:361–71. doi:10.2147/VMRR.S51147
24. Sorrell EM, El Azhari M, Maswdeh N, Kornblet S, Standley CJ, Katz RL, et al. Mapping of Networks to Detect Priority Zoonoses in Jordan. Front Public Health (2015) 3:219. doi:10.3389/fpubh.2015.00219
25. Pieracci EG, Hall AJ, Gharpure R, Haile A, Walelign E, Deressa A, et al. Prioritizing zoonotic diseases in Ethiopia using a one health approach. One Health. (2016) 2:131–5. doi:10.1016/j.onehlt.2016.09.001
26. FAO. New Myanmar One Health (OH) Strategy. (2016). Available from: http://www.fao.org/ag/againfo/programmes/en/empres/news_170316b.html
27. Munyua P, Bitek A, Osoro E, Pieracci EG, Muema J, Mwatondo A, et al. Prioritization of zoonotic diseases in Kenya, 2015. PLoS One (2016) 11:e0161576. doi:10.1371/journal.pone.0161576
28. Taylor LH, Knopf L; Partners for Rabies Prevention. Surveillance of human rabies by national authorities – a global survey. Zoonoses Public Health (2015) 62(7):543–52. doi:10.1111/zph.12183
29. Zaidi SM, Labrique AB, Khowaja S, Lotia-Farrukh I, Irani J, Salahuddin N, et al. Geographic variation in access to dog-bite care in Pakistan and risk of dog-bite exposure in Karachi: prospective surveillance using a low-cost mobile phone system. PLoS Negl Trop Dis (2013) 7(12):e2574. doi:10.1371/journal.pntd.0002574
30. World rabies day 2016: educate, vaccinate, eliminate. Vet Rec (2016) 179(12):297. doi:10.1136/vr.i5066
31. Balaram D, Taylor LH, Doyle KAS, Davidson E, Nel LH. World rabies day – a decade of raising awareness. Trop Dis Travel Med Vaccines (2016) 2(19). doi:10.1186/s40794-016-0035-8
32. Coetzer A, Kidane AH, Bekele M, Hundera AD, Pieracci EG, Shiferaw ML, et al. The SARE tool for rabies control: current experience in Ethiopia. Antiviral Res (2016) 135:74–80. doi:10.1016/j.antiviral.2016.09.011
33. Jerolmack C. Who’s worried about Turkeys? How ‘organisational silos’ impede zoonotic disease surveillance. Sociol Health Illn (2013) 35(2):200–12. doi:10.1111/j.1467-9566.2012.01501.x
35. Pudjiatmoko P, Kandun IN. Integrated Bite Case Management (IBCM) in Bali: One Health in Action. Republic of Indonesia. p. 1–24. Available from: http://www.pmaconference.mahidol.ac.th/dmdocuments/PMAC_2013_PPT_%20PS3.4%20Pudjiatmoko.pdf
36. Lapiz SMD, Miranda MEG, Garcia RG, Daguro LI, Paman MD, Madrinan F, et al. Implementation of an intersectoral program to eliminate human and canine rabies: the Bohol rabies prevention and elimination project. PLoS Negl Tro0070 Dis (2012) 6:e1891. doi:10.1371/journal.pntd.0001891
37. Scott TP, Coetzer A, de Balogh K, Wright N, Nel LH. The Pan-African rabies control network (PARACON): a unified approach to eliminating canine rabies in Africa. Antiviral Res (2015) 124:93–100. doi:10.1016/j.antiviral.2015.10.002
38. Vigilato MA, Clavijo A, Knobl T, Silva HM, Cosivi O, Schneider MC, et al. Progress towards eliminating canine rabies: policies and perspectives from Latin America and the Caribbean. Philos Trans R Soc Lond B Biol Sci (2013) 368(1623):20120143. doi:10.1098/rstb.2012.0143
39. Vigilato MA, Cosivi O, Knobl T, Clavijo A, Silva HM. Rabies update for Latin America and the Caribbean. Emerg Infect Dis (2013) 19:678–9. doi:10.3201/eid1904.121482
40. Aylan O, El-Sayed AF, Farahtaj F, Janani AR, Lugach O, Tarkhan-Mouravi O, et al. Report of the first meeting of the Middle East and Eastern Europe rabies expert bureau, Istanbul, Turkey (June 8-9, 2010). Adv Prev Med (2011) 2011:812515. doi:10.4061/2011/812515
41. Aikimbayev A, Briggs D, Coltan G, Dodet B, Farahtaj F, Imnadze P, et al. Fighting rabies in Eastern Europe, the Middle East and Central Asia – experts call for a regional initiative for rabies elimination. Zoonoses Public Health (2013) 61:219–26. doi:10.1111/zph.12060
42. Durr S, Naissengar S, Mindekem R, Diguimbye C, Niezgoda M, Kuzmin I, et al. Rabies diagnosis for developing countries. PLoS Negl Trop Dis (2008) 2:e206. doi:10.1371/journal.pntd.0000206
43. Léchenne M, Naïssengar K, Lepelletier A, Alfaroukh IO, Bourhy H, Zinsstag J, et al. Validation of a rapid rabies diagnostic tool for field surveillance in developing countries. PLoS Negl Trop Dis (2016) 10(10):e0005010. doi:10.1371/journal.pntd.0005010
44. Abela-Ridder B, Martin S, Gongal G, Engels D. Rabies vaccine stockpile: fixing the supply chain. Bull World Health Organ (2016) 94(9):635–635A. doi:10.2471/BLT.16.183012
45. WHO, OIE. Human and Dog Rabies Vaccines and immunoglobulins. Report of a Meeting. Geneva, 12-13 October 2015. Geneva: WHO (2015).
46. From Concept to Completion: The Rabies Control Pilot Project Supported by the Bill & Melinda Gates Foundation. World Health Organization (2015). Available from: http://www.who.int/rabies/bmgf_who_project_outcomes/en/
47. Mohammadi D. Moves to consign rabies to history. Lancet Infect Dis (2016) 16(10):1115–6. doi:10.1016/S1473-3099(16)30342-5
48. Hampson K, Cleaveland S, Briggs D. Evaluation of cost-effective strategies for rabies post-exposure vaccination in low-income countries. PLoS Negl Trop Dis (2011) 5(3):e982. doi:10.1371/journal.pntd.0000982
49. Gongal G, Wright AE. Human rabies in the WHO southeast Asia region: forward steps for elimination. Adv Prev Med (2011) 2011:383870. doi:10.4061/2011/383870
50. Morters MK, McKinley TJ, Horton DL, Cleaveland S, Schoeman JP, Restif O, et al. Achieving population-level immunity to rabies in free-roaming dogs in Africa and Asia. PLoS Negl Trop Dis (2014) 8:e3160. doi:10.1371/journal.pntd.0003160
51. Tenzin T, McKenzie JS, Vanderstichel R, Rai BD, Rinzin K, Tshering Y, et al. Comparison of mark-resight methods to estimate abundance and rabies vaccination coverage of free-roaming dogs in two URBAN areas of south Bhutan. Prev Vet Med (2015) 118:436–48. doi:10.1016/j.prevetmed.2015.01.008
52. IR D, G M. Concepts of infectious disease epidemiology. In: Dohoo IR, Martin W, Stryhn H, editors. Veterinary Epidemiologic Research. Charlottetown, Canada: VER Inc (2009).
53. Durr S, Meltzer MI, Mindekem R, Zinsstag J. Owner valuation of rabies vaccination of dogs, Chad. Emerg Infect Dis (2008) 14:1650–2. doi:10.3201/eid1410.071490
54. Sparkes J, Körtner G, Ballard G, Fleming PJ, Brown WY. Effects of sex and reproductive state on interactions between free-roaming domestic dogs. PLoS One (2014) 9(12):e116053. doi:10.1371/journal.pone.0116053
55. Durr S, Mindekem R, Kaninga Y, Doumagoum Moto D, Meltzer MI, Vounatsou P, et al. Effectiveness of dog rabies vaccination programmes: comparison of owner-charged and free vaccination campaigns. Epidemiol Infect (2009) 137:1558–67. doi:10.1017/S0950268809002386
56. Fitzpatrick C, Engels D. Leaving no one behind: a neglected tropical disease indicator and tracers for the Sustainable Development Goals. Int Health (2016) 8(Suppl 1):i15–8. doi:10.1093/inthealth/ihw002
57. Anonymous. Report of the Sixth Meeting of the International Coordinating Group of the World Health Organization and the Bill & Melinda Gates Foundation Project on Eliminating Human and Dog Rabies. Geneva: World Health Organization (2015). Contract No.: WHO/HTM/NTD/NZD/2015.3.
Keywords: rabies, dog rabies, neglected tropical diseases, zero human deaths, global framework, implementation
Citation: Fahrion AS, Taylor LH, Torres G, Müller T, Dürr S, Knopf L, de Balogh K, Nel LH, Gordoncillo MJ and Abela-Ridder B (2017) The Road to Dog Rabies Control and Elimination—What Keeps Us from Moving Faster? Front. Public Health 5:103. doi: 10.3389/fpubh.2017.00103
Received: 07 November 2016; Accepted: 18 April 2017;
Published: 15 May 2017
Edited by:
Leland Shapiro, University of Colorado at Denver, USAReviewed by:
Edward N. Janoff, University of Colorado at Denver, USAAshley C. Banyard, Animal and Plant Health Agency, United Kingdom
Copyright: © 2017 Fahrion, Taylor, Torres, Müller, Dürr, Knopf, de Balogh, Nel, Gordoncillo and Abela-Ridder. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) or licensor are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Anna S. Fahrion, ZmFocmlvbi5hc0BnbWFpbC5jb20=
 Anna S. Fahrion
Anna S. Fahrion Louise H. Taylor
Louise H. Taylor Gregorio Torres
Gregorio Torres Thomas Müller4
Thomas Müller4 Salome Dürr
Salome Dürr Lea Knopf
Lea Knopf Katinka de Balogh
Katinka de Balogh Louis H. Nel
Louis H. Nel