- 1Department of Social Medicine and Health Management, Xiangya School of Public Health, Central South University, Changsha, China
- 2College of Data Science and Information Engineering, Guizhou Minzu University, Guiyang, China
- 3Department of Mathematics and Statistics, Mzuzu University, Mzuzu, Malawi
- 4Department of Epidemiology and Health Statistics, Xiangya School of Public Health, Central South University, Changsha, China
- 5School of Medicine and Health Management, Tongji Medical College of Huazhong University of Science and Technology, Wuhan, China
Background: Chinese government conducted unprecedented massive public health prevention interventions at the national level, which have effectively contained the spread of Coronavirus Disease 2019 (COVID-19) infections. Specifically, the outbreak in Wuhan has been effectively controlled. Meanwhile, the Chinese efforts to contain the virus have been widely recognized. Even the World Health Organization has praised the efforts of the Chinese government and advised other countries to learn from China's experience in the fight against COVID-19. However, the measures that have been conducted by China to effectively prevent the spread of COVID 19 in the country have not been rigorously analyzed. Therefore, this study aimed to explore the characteristics of China's control and prevention strategies, and identify the elements that changed the epidemiological curve of rapidly rising new confirmed cases of COVID-19.
Methods: Public health intervention measures and their effects on the spread of COVID-19 in terms of daily newly confirmed and cumulative cases were collected between January 20, 2020, and March 5. Notices of the Joint Prevention and Control Mechanism for COVID-19 of the State Council on Implementing Measures in Hubei were collected. Information obtained by relevant important documents and announcements was collected from the official website of the Chinese government. Additionally, from other media platforms, news, articles, and reviews were used to explain the intervention measure. Thus, using these data, we performed a retrospective description of the intervention strategies at three stages.
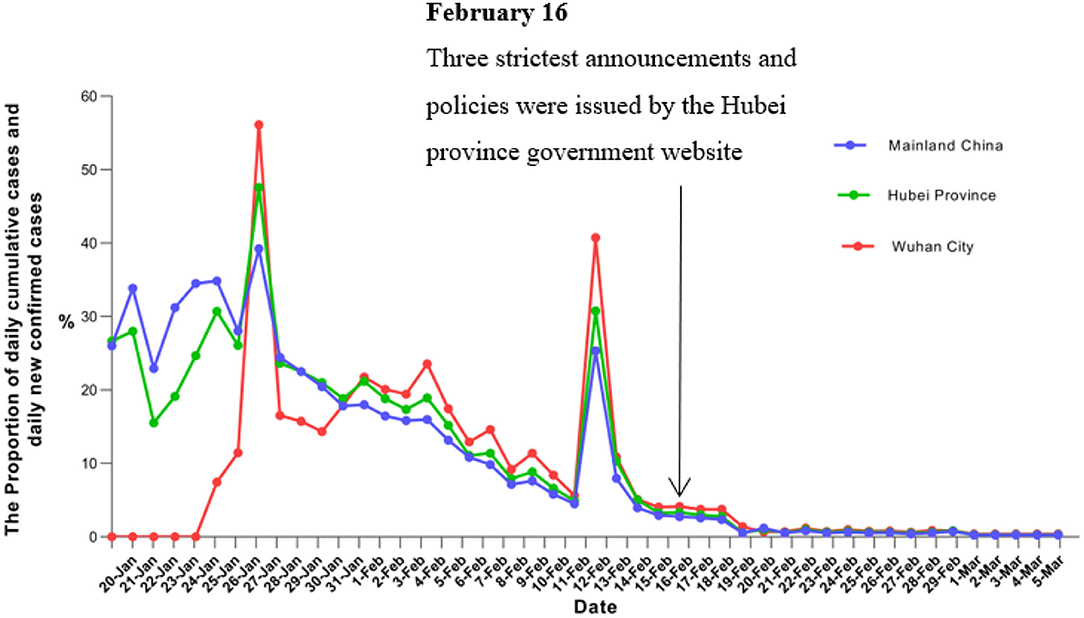
Results: The Chinese government adopted non-pharmacological interventions measures (NPIs) timely and efficiently. On February 20, the declining epidemic trend in China indicated that the three strictest disease prevention and control strategies issued by the Hubei Government had contributed to a smooth decline in the spread of the epidemic.
Conclusions: The NPIs taken by China play a decisive role to control the spread of novel coronavirus outbreaks. Further research and action are needed to ensure a sufficiently sensitive surveillance system and strong response mechanism, including the establishment of a highly accessible laboratory network, maintenance of awareness of both primary healthcare providers and the public, and regular training and exercise of local Centers for Disease Control and Prevention and general practitioners in the community-level.
Introduction
An unprecedented outbreak of pneumonia of unknown etiology in Wuhan, Hubei Province, China, emerged in December 2019 (1, 2). However, this was identified as a symptom of COVID-19 disease, 2019-nCoV, caused by a novel coronavirus (3). The spread of COVID-19 turned into an epidemic when it quickly affected 31 provinces and regions of China. Later the spread of COVID-19 became a pandemic, when it was announced on March 5 at 23:00 CET that a total of 98,067 new cases were confirmed globally, with 3,281 deaths (4). Specifically, a total of about 17,637 cases were confirmed in 78 countries outside China. In this regard, the COVID-19 outbreak surpassed the severity of the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) outbreak in 2003 (5–7).
In China, the COVID-19 outbreak coincided with China's Spring Festival travel peak. Therefore, to curb the spread of the infectious disease, the Chinese government launched unprecedented public health intervention measures such as shutting down Wuhan transportation, extending the legal holiday, mass isolation of individuals from cases, strict enforcement of quarantine of all individuals who had contact with the suspected cases, cancellation of all public gatherings, and educating the public on how to prevent the spread of the disease by practicing hygiene (8). In addition, a nationwide health monitoring of people who had visited the Hubei province or other regions was implemented. Also, mass epidemiological investigations have been carried out for suspected cases, confirmed cases, clusters, and contacts to identify sources of spread to implement targeted control measures. Thus, these measures quickly started producing the desired outcomes. For example, the number of new confirmed cases per day declined from a high peak of 3,900 cases on 13 February 2020 to 323 cases on 27th February 2020 (9). Besides, at a COVID-19 news conference on February 24, 2020, the WHO leader, Bruce Aylward, said “China's made comprehensive non-pharmaceutical interventions, which have effectively prevented the transmission of the virus, providing important experiences for the global response to new virus” (10). Also, at 16:00 h on 28 February 2020, Dr. Wannian Liang, the China team leader and the expert team leader of the New Coronary Pneumonia Epidemic Response said: “the virus outbreak in Wuhan was curbed basic” (10). Moreover, Wilder-Smith et al. noticed that the unprecedented efforts by the Chinese government surpassed the previous efforts to combat sirs (11). Further, as of March 7, 2020, the total number of close contacts tracked was 6,740,388. Therefore, there is no doubt that the prevention and control measures implemented by China have been very effective and could serve as an example for other countries (10). Thus, it is against this background that this paper aims to summarize the foregoing intervention measures, from the perspective of social epidemiology, and try to explain how the COVID-19 outbreak in Wuhan, Hubei Province was effectively controlled. Also, this study aimed to explore the effectiveness of the ambitious non-pharmacology interventions taken by the Chinese government. It is therefore hoped that the findings of this study would provide references and suggestions for other countries in the progress of the epidemic.
Methods
Ethical Approval
In this study, it was not necessary to obtain the institutional review board's approval due to the use of publicly accessible data of published cases, and the project is not involved with patient consent.
Data Collection
Public health intervention data were collected from January 11, 2020, to March 5, 2020. Thus, detailed intervention measures conducted by China in Hubei Province were described, along with the subsequent changes in trends and analysis of its effects. Data were extracted, tabulated, and analyzed in Microsoft Excel 2010 and drawn a graph by software of Graph Pad Prism (version 9.0). The following steps describe the data collection process for this study.
Step 1: Data were extracted from the information reporting system of the National Health Committee, issued by the health emergency office, between January 11, 2020 and March 5, 2020 (http://www.nhc.gov.cn/xcs/situationreportofCOVID-19). Specifically, extracted data included the cumulative number of confirmed COVID-19 cases (in the Mainland China, Hubei Province) and the number of daily new confirmed COVID-19 cases (in the Mainland China, Hubei Province, Wuhan City). In addition, the ratio of daily new confirmed COVID-19 cases to daily cumulative COVID-19 cases was considered as an indicator of the effectiveness of the interventions.
Step 2: Relevant important information and announcements were also collected from the official website of the Chinese government (https://www.gov.cn); National Health Commission of the People's Republic of China; announcements of the Joint Prevention and Control Mechanism for new coronary pneumonia of 2019 of the State Council on Implementing Measures to rescue Hubei Province; press conference on the progress of prevention, control and treatment of the epidemic situation of new coronary pneumonia of 2019 (http://www.nhc.gov.cn/xcs); the website of the People's Government of Hubei Province (http://www.hubei.gov.cn); the website of the People's Government of Wuhan (http://www.wuhan.gov.cn); Health commission of Hubei Province (http://www.wjw.hubei.gov.cn); Health Commission of Wuhan (http:www.wjw.wuhan.gov.cn); and Chinese Center for or Disease Control and Prevention website (https://www.chinacdc.cn/)and Hubei Provincial Center for Disease Control and Prevention website (http://www.hbcdc.com/). Additionally, relevant information was obtained from other media platforms such as news, articles, and reviews.
Results
Response Measures Summary and Data Analysis
A retrospective description and summary of the observed public health intervention strategies are presented in three stages as follows:
Stage 1: During the early stage of the outbreak, before 20 January 2020, the main strategy focused on preventing the exportation of COVID-19 cases from Wuhan and Hubei Province; and preventing the importation of cases by other provinces. The overall global was to control the source of infection as much as possible, block transmission, and prevent further spread to the other provinces. On Jan 26,30 provinces across the country initiated a first-level response to a nationwide level. Wuhan City organizes experts to analyze the condition, outcome of treatment, epidemiological investigation, preliminary laboratory testing, and efforts were made to identify the zoonotic source diseases (7). Information on the epidemic was sent to WHO on January 3, 2020, and the whole genome sequence of the SARS-CoV-2 virus was shared with World Health Organization and the United States and other countries on January 10, 2020 (12, 13). Subsequently, the first guidelines for COVID-19 diagnosis and treatment were formulated (14).
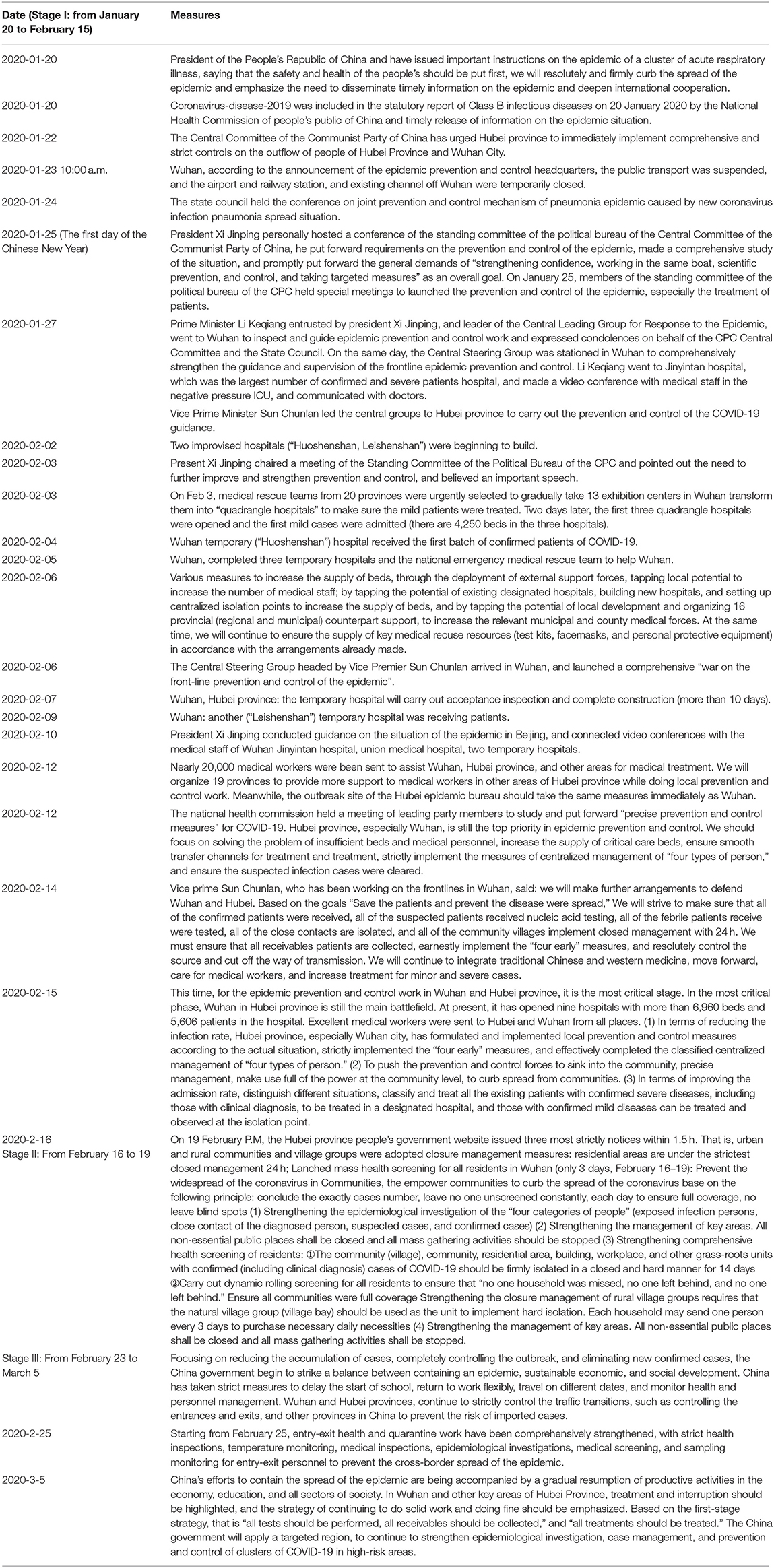
As we all know, since the outbreak of COVID-19, the Chinese government puts the people's life safety and physical health first, with firm courage and confidence, and adopting the most comprehensive, strictest, and thorough prevention and control measures to control the epidemic (15). For example, Wuhan public transport was closed and the National Health Commission of the People's Republic of China and other six departments issued the “Notice on Strictly Preventing Pneumonia Caused by the Transmission of New Coronavirus Through Transportation,” subsequently, all provinces across the country have successively initiated a provincial-level emergency response to major public health emergencies. Sixteen temporary treatment hospitals were opened by February 24, a large-scale health quarantine was implemented, social isolation at a whole society level was enforced, hygiene practices were encouraged, and every citizen was ordered to wear a face mask and keep a distance of 1.5 m from other individuals. These interventions were coordinated by an established Central Leadership Group for Epidemic Response and the Joint Prevention and Control Mechanism of the State Council. Furthermore, President Xi Jinping personally directed and deployed the prevention and work control, and requested that the prevention and control of the COVID-19 outbreak be the top priority of the government at the national level. In this regard, the prevention and control measures have been conducted quickly, from the early stages in Wuhan and other key areas of Hubei province. Table 1 shows the three phases in which these interventions were undertaken. Noteworthy, the novel coronavirus outbreak was included in the statutory report of Class B infectious diseases and management measures for Class A infectious diseases have been adopted on January 20, 2020, which marked the transition from the initial partial control approach to the comprehensive adoption of various control measures by the law (16).
Thus, on January 22, 2020, the State Council, and the Communist Party of China (CPC) central committee “made an official announcement” that Wuhan City, a metropolis of 11 million people, of Hubei Province, must shut down traffic transportation to control the flow of people. Further, on January 23, 2020, the authorities in Wuhan announced the lockdown of the City, which implied shutting down all public transportation, canceling flights and trains, and closing schools and factories (17, 18).
In addition, on January 27, 2020, Premier Li Keqiang, member of the Standing Committee of the Political Bureau of the CPC Central Committee, Premier of the State Council, and leader of the Central Leading Group for Response to the Epidemic, went to Wuhan to inspect and guide epidemic prevention and control work and expressed condolences on behalf of the CPC Central Committee and the State Council. Moreover, Li Keqiang went to Jingyintan Hospital, which had the largest number of confirmed and severe cases, and made a video conference with medical staff in the negative pressure ICU, and communicated with frontline health workers. Similarly, the vice prime minister, Sun Chunlan, led the central groups to Hubei to carry out the prevention and control measures of the COVID-19. Thus, by January 29, 2020, 31 provinces and autonomous regions and municipalities across China had launched the first- level of emergency response against the COVID-19 epidemic.
On 3 February 2020, medical rescue teams from 20 provinces were urgently selected to gradually transform 13 exhibition centers in Wuhan into “temporary treatment centers” to ensure that all patients with mild symptoms were treated. Two days later, the first Fangcang shelter hospital was opened, and the first cases with mild symptoms were admitted (there were 4,250 beds in the three hospitals). In addition, on 4 February 2020, “Huoshengshan” improvised hospitals in Wuhan began to accept the patients. On 7 February 2020, another temporary hospital underwent an acceptance inspection and was completed (10 days) in Wuhan. Later, on 10 February 2020, President Xi Jinping conducted a video conference in Beijing with the medical staff of Wuhan Jinyintan Hospital and Wuhan Union Hospital, and “Huoshenshan Hospital” in Wuhan to give guidance on the prevention and control of the epidemic (19). On 12 February 2020, nearly 20,000 medical staff were sent to assist in providing medical services in Wuhan, Hubei Province, and other areas (20). Therefore, the Chinese government organized medical staff from 19 provinces to take the form of “one province support to one region” to provide support to other areas of Hubei Province (It is a national strategy in China for a province or major city to assist in a designated region that needs help). These medical staff carried with them ventilators, electrocardiograph monitors, and ECMO (Extracorporeal Membrane Oxygenation) other medical and protective equipment.
Stage 2: On 16 February 2020, epidemic prevention and control measures in Wuhan and Hubei came to the most critical stage. The main strategy was to reduce the intensity of the outbreak and slow down the occurrence of new cases. Thus, in Wuhan and other key areas of Hubei Province, the focus was on treating patients aggressively, reducing the infection rate and deaths, and preventing cases from exporting the infection to other places. Nevertheless, in other provinces, the focus was on the prevention of importation, containment of disease transmission, and implementation of joint prevention and control measures. On 15 February, at present, the epidemic prevention and control work in Hubei and Wuhan has reached the most urgent time, Wuhan was still the main battle area. As of on 24 February 2020, nine new hospitals with more than 6,960 beds were opened in Wuhan, and 5,606 patients were accomodated. Accordingly, more medical workers from all places in China were sent to these hospitals to offer medical rescue services.
The state council information office of the Public of China press conference was held in Wuhan, Hubei to introduce the epidemic prevention and control and medical treatment work organized and carried out in Hubei.
As regards reducing the infection rate, Hubei Province, especially Wuhan, formulated and implemented local prevention and control measures according to the actual situation. Therefore, “four early stages” measures were strictly implemented (early detection, reporting, quarantine, and treatment). Also, and effectively completed the classified centralized management of “four categories of vulnerable people” (confirmed cases, suspected cases, febrile patients who might be carriers, and close contacts) was effectively completed classified centralized management. The prevention and control measures were conducted in the community, with precise management, and it was imperative to make full use of the power at the community level to curb the spread from communities.
Also, medical conditions and resources have been greatly improved, so the admission rate was improved greatly, and COVID-19 cases were classified as mild or severe; hence, management of patients was performed according to these categories of patients in designated hospitals (21). In addition, a nucleic acid test was conducted on suspected cases and the results were released the same day. Thus, when the test results were positive, patients were transported to designated hospitals depending on the severity of the symptoms. Noteworthy, all patients, those with mild or severe symptoms, and the asymptomatic patients were admitted. At least one designated hospital was strategically placed in each district/country.
Most importantly, the strategy in Wuhan and other critical areas of the epidemic was to “leave no one unscreened.” Therefore, closed community management every 24 h was launched in Wuhan while conducting a massive medical screening of COVID-19 infections (22). On the afternoon of 16 February 2020, the people's government of Hubei Province issued the three strictest announcements within 1.5 h. Therefore, the following actions were carried out according to the preceding strictest orders.
(1) Urban and rural communities and village groups adopted closure management measures. Thus, residential areas were under the strictest 24 h of closed management. Also, dragnet dynamic rolling screening was performed for all residents (only 3 days, 16–19 February 2020). To find the exact number of cases based on the foregoing strategies, everyone was screened; and also the epidemiological investigation of the following “four categories of vulnerable people” was strengthened; (2) Strengthening the management of key areas. This demanded closing all non-essential public places and banning all mass gathering activities; (3) Strengthening comprehensive health screening of residents: (a) the communities (villages), residential areas, buildings, workplaces, and other grass-root units with confirmed (including clinical diagnosis) cases of COVID-19 were firmly isolated in a closed and hard manner for 14 days. (b) The dynamic rolling screening was carried out for all residents to ensure that no one was left unscreened. Therefore, it was important to ensure that all communities and residents accepted medical screening. (4) Closure management of rural village groups was strengthened and this required that the natural village groups (villages) be used as the units for implementing hard isolation. Each household could send one person every 3 days to provide daily necessities to the family members who were in isolation.
Stage 3: In this third stage, the rapid rise of the epidemic situation in Hubei Province and Wuhan City has been contained. The situation of the epidemic situation in the country except Hubei Province is generally stable. In mid of March, the daily new cases were controlled within single digits, and the epidemic prevention and control achieved an important process. In accordance with the development of the epidemic prevention and control situation, the Central Committee of the Communist Party of China has made a major decision to coordinate epidemic prevention and control, economic and social development, and orderly resume work and production. Wuhan and Hubei Province continued to strictly control traffic transitions, such as controlling entrances and exits. Similarly, other provinces in China are also trying to prevent the risk of imported cases from other provinces and countries. These detailed measures are summarized in Table 1.
New Confirmed Cases Situation
As shown in Figure 1, on 12 February, the number of confirmed cases was taken from the highest day, and the new confirmed cases number rose sharply before 20 January 2020, and this trend almost continued to the third week, but the epidemiological curve shows that the extraordinary intervention measures implemented by China government directly led to flat declines or lower levels of transmission from 17 to 20 February 2020 in Hubei province. Additionally, the epidemiological curve declined sharply on 19 February, and this positive outcome is attributed to the lockdown of Wuhan City, and the opening of new hospitals in Wuhan, with more than 6,960 beds, which accommodated 5,606 patients. Accordingly, more medical workers from all places in China were sent to these hospitals to offer medical services. Therefore, the hospital admission capacity was raised greatly (23). Besides, during the stage II period, the medical conditions and rescue resources were substantially improved; the centralized isolation and treatment of “four categories of vulnerable people” was implemented, and the control measures of the community using 24-h close management were constantly upgraded. Thus, the risk of infection was greatly reduced. Noteworthy, to promote the implementation of the five “100%” work goals, resolutely curb the spread of the epidemic, the Wuhan City government launched a mass screening in four thousand communities with 4.21 million residents between 16 February and 19 February 2020. A door-to-door and individual-to-individual universal symptom survey to single out suspected cases in the community, which was strongly associated with further reductions in the spread of COVID-19 in Wuhan. Besides, to further reduce the risk of infection in the community, Wuhan city adopted the methods of a closed community, closed residential areas, all residents were asked home isolation, the government is responsible for centralized distribution of living materials and other means. Therefore, the epidemiological curve shown in Figure 1 proves that the preceding prevention and control measures are successful and directly lead to desired outcomes.
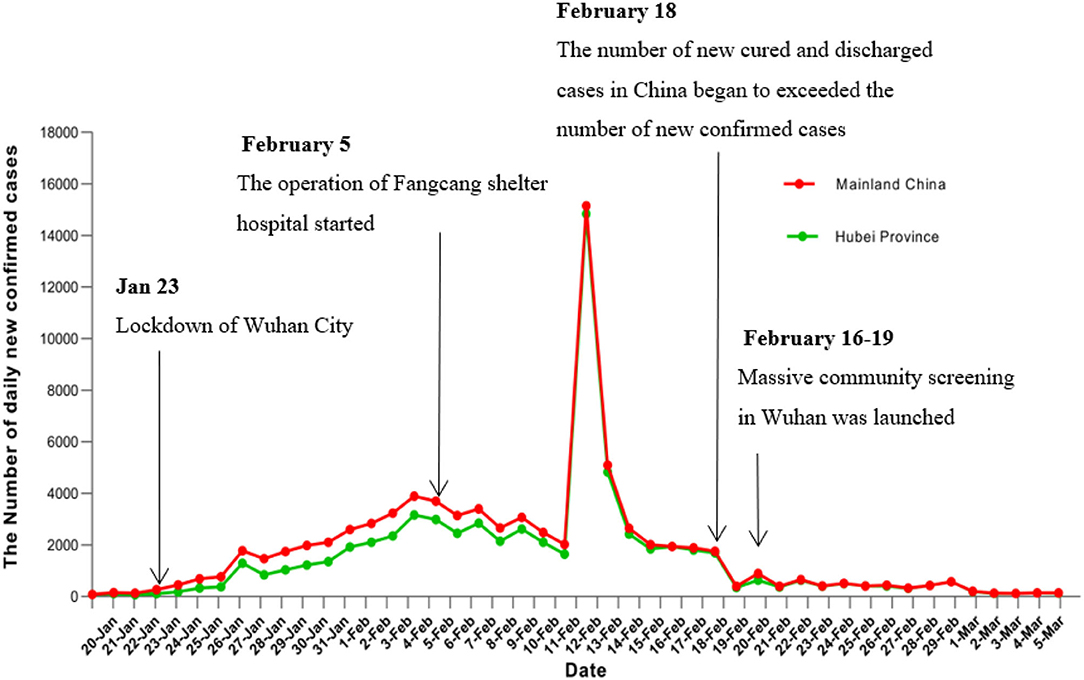
Figure 1. Situation daily confirmed cases number of COVID-19 in China mainland and Hubei province (from January 20 to March 5).
Change Trends of New Confirmed Cases
Figure 2 also presents a trend that peaks near a plateau and then declines on 20 February 2020. This changing trend also indicates that the three strictest announcements and policies achieved a smooth decline in the epidemic. Additional measures included restrictions on inter-city travel during the stage I period, early identification, and isolation of cases as well as restrictions on personal contact and measures of social alienation. In addition, the expansion of services for PCR testing improve day by day, continue to improve nucleic acid detection capabilities, and enhance the capacity of test kit supply, many commercial organizations have also joined nucleic acid testing and the capacity of nucleic acid testing to 2, 5 000 tests per day on 26 February 2020, in Wuhan (24). It added that there was inventory enough to fulfill testing for about two million people.
So greatly shorten the diagnosis time of patients and reduce the risk of transmission. Moreover, community villages implemented 24-h closed management, each resident who was isolated in the home, the government centralized distribution of living necessities supply to them, etc. Twenty-four closed community management and control measures continue to keep in Wuhan. These comprehensive intervention measures contributed to the decline in the epidemiological curve shown in Figure 2.
Discussion
COVID-19 outbreak is the world's most serious infectious disease epidemic since the 1918 pandemic and the most challenging global public health emergency since the end of the Second World War. Since the founding of the People's Republic of China in 1949, the COVID-19 epidemic is a major public health emergency with the fastest spread, the widest range of infections, and the most difficult prevention and control has occurred (25). Thus, it has been the biggest battle to prevent and control its rapid spread across the country, which required the involvement of all the people in China. This study, therefore, systematically collected and analyzed data to evaluate the prevention and control measures implemented by China. The purpose was to inform the reader how China government has thus far performed in the prevention and control of COVID-19 and to highlight non-pharmacology measures that could effectively, timely reduce the spread of the COVID-19 pandemic globally. Thus, this is consistent with the WHO declaration in the early stages of the outbreak that COVID-19 is the Public Health Emergency of International Concern, based on the International Health Regulation (2005), as he said that China has taken extraordinary and powerful measures, and China has provided an example for responding to the epidemic for many aspects, as it is an extraordinary event to constitute a public health risk to the states through the international spread of the disease, and this potentially required coordinated international cooperation and response to jointly control the virus (26, 27).
Therefore, the international community needs to work together in the prevention and against the COVID-19 pandemic (28). Nevertheless, some countries, such as Sweden and The United Kingdom, still take a vague attitude about this outbreak, such as “herd immunity” (29). Also, some people may refuse to wear face masks in other countries. Mankind will eventually defeat the epidemic, but a major public health emergency will not be the last time for mankind (30, 31).
Experience has shown that non-pharmacology interventions can successfully reduce or even stop transmission in some cases. Even in the face of widespread transmission, China's experiences have shown that if we keep calm, take action immediately, and implement a systematic identification of cases as well as contact tracing, then we could change the course of the pandemic, prevent people from getting sick, and prevent the most vulnerable from dying.
To the best of our knowledge, the main four early strategies: “early identification, early report, early isolation, and early treatment” were critical to the containment of the COVID-19 epidemic in China. These efforts were accomplished via a process of “lockdown Wuhan” to conduct two rounds of community-based mass screening of its 4.21 million households, finally, the infection rate was minimized greatly in Wuhan and achieved success based on the principle of “leave no one unscreened household unchecked” and to ensure that there are no new potential sources of infection occurred (32).
In addition, very strict containment measures for the COVID-19 outbreak included the “four categories of vulnerable people” being accepted screen nationwide, and the community-based epidemic prevention and control were used as the basic unit to carry out a carpet-style investigation by combining on-site investigation with self-report. Fully implement body temperature screening and health quarantine in various places, including travel venues (airports, train stations), strengthening the monitoring of fever cases in medical institutions and direct online reporting of infectious diseases, implemented 2 h direct online reporting, 12 h feedback of PCR test results, complete on-site epidemiological investigations within 24 h, and timely discover and report confirmed cases and universal symptom survey (33).
These active actions were implemented successfully due to strong coordinated efforts by the Chinese government in cooperation with residents. To date, the epidemiological data in this study has shown that China effectively reversed the situation of the epidemic, and China took more than a month to initially contain the spread of the epidemic, and thousands of people were protected from the virus and also save valuable time to the world (32, 34).
Yang et al. (35) used the population migration data on 23 January 2020, and the latest COVID-19 epidemiological data to integrate the classical infectious disease prediction model to predict the epidemic trend, which showed that the response measures are taken by the Chinese government effectively avoid the spread of the epidemic. If these public intervention measures had been delayed for another 5 days, the epidemic trend would have tripled, and the spread of the disease to many places could have grown exponentially in one region, hence devastating for humans (36). Recently, some studies have examined the effects of the shutdown of Wuhan public transportation (37, 38), strong travel restrictions, and prohibits mass gatherings (38), massive health quarantine conducted in the airport (39), isolation of cases for 14 days, and contact tracing on the containment of the disease by 5G network big data technology platform tracking individual health codes (40). Thus, Lai et al. developed a modeling framework that estimated that without non-pharmaceutical interventions, the number of cases would have been 67-fold higher by 29.02.2020 (41). In April, Pan et al. use the real case data of Wuhan to systematically and completely analyze the impact of the continuous improvement of public health intervention measures on the epidemic trend in Wuhan. These studies revealed that public health interventions play an important role in the prevention and control of new emerging infectious diseases. Accordingly, in China, a combination of the preceding non-pharmaceutical interventions and traditional pharmaceutical interventions China achieved the strongest and most rapid effect (32).
There are two positions in the fight against the epidemic, one in the hospital to rescue patients, and the other in the community prevention and control position. The community played an important role in the prevention and control of the epidemic In, In this fight, medical resources from all over China have been mobilized to support the medical treatment of patients in Wuhan and Hubei Province. From New Year's Eve on 24 January to 8 March, a total of 346 national medical teams, 42,600 medical staff, and 965 public health workers from 29 provinces, and Xinjiang production and construction corps were used to assist Wuhan and Hubei Province (42). Besides, it took <10 days to construct two temporary hospitals (43, 44).
As of 28 February 2020, 16 new shelter hospitals were opened to centralize the treatment of patients based on the principle that all patients could be treated. Therefore, the outbreak in China, including the hardest-hit Hubei Province, has been well under control with high-level measures for prevention and control, and temporary hospitals playing the role of isolating non-severe patients. Specifically, the shelter hospitals in this epidemic have created a new model for China to respond to public health emergencies and crises, and to rapidly expand medical resources. That is, as Wang Chen, who is an academician with the Chinese Academy of Engineering said “The shelter hospitals” admitted only patients with mild symptoms, which apart from quarantining the patients, also created room for regular hospitals to treat several types of patients, provided high-quality medical treatment and care, and fulfilled an important triage function (45–48).
In response to the prominent contradiction between the rapid increase in the number of patients in the early stage of the epidemic and insufficient bed resources, the Chinese government did everything possible to reserve beds, and concentrate resources and efforts to build and expand designated critically patients hospitals in Wuhan, and to ensure that all cases could be treated on time. Wuhan and Hubei Provinces were treated as a priority for medical materials needs, and many provinces (a total of 19 provinces) were organized to help one region (49). In addition, make full use of new technologies such as big data and artificial intelligence to enhance contact tracing, focus group management, resource allocation, identification of the source of suspected cases, and conducting epidemiological investigations in the community across the country. The data and information system for epidemic prevention and control, based on the people's public security big data system, were an important “weapon” for Wuhan to win over the battle of epidemic prevention and control.
Additionally, the Wuhan government proposed a large step to ensure that 100% of confirmed patients were received and treated at the hospitals, 100% of suspected cases were undergoing nucleic acid-based testing, 100% of patients with fever were detected, 100% of close contacts persons were isolated, and community villages implemented 100% 24 h closed management (50).
This study, therefore, suggests that non-pharmacological public health interventions are crucial to stopping the global spread and progression of COVID-19 in the absence of targeted vaccines and specific drugs. Also, a series of improved public health intervention measures in Wuhan has been identified by some studies (33, 51–54). These findings may help inform the public health policies in other countries and regions as regards response to the global COVID-19 pandemic. However, the disadvantages of containing COVID-19 in China must be discussed in this study. For example, social isolation between people, and maintenance of strict intervention measures lasting more than 2 months in Wuhan, particularly physical distancing, and thus brings huge socioeconomic costs (55).
First, since the COVID-19 outbreak, the government of China implemented the right to good health a priority. China always adheres to the concept of a community of human destiny, and urges the international community and country leaders to join in the fight against stigma and the politicization of public health issues, but minimize the impact of the epidemic on the economic burden and society, hence protecting the rights of vulnerable populations (56). Second, any possible violation of human rights while carrying out social isolating measures to prevent and control the spread of the pandemic should be discussed. Thus, as a matter of fact, China's mode of response is the most comprehensive, stringent, and thorough regardless of exposing herself to a period of economic decline or even a short-term “shutdown.” This is consistent with an editorial comment in the Lancet, “China's success has come at a huge social and economic cost, and China must make tough decisions to strike the best balance between health and economic protection of its citizens (56).” Besides, isolation and travel bans are often the first response against new infectious diseases; hence, the Chinese authorities also ordered a 14-days quarantine mandatory for any person who has recently visited the Hubei province. However, in the United States of America (USA), quarantines and ban massive gatherings, like these traditional tools are usually of limited utility for highly transmissible diseases, and if it imposed with too heavy a hand, or in a hazardous manner, they can be counterproductive (57). Therefore, the implementation of these strategies in other countries or regions during the current pandemic needs to carefully consider other contextualization principles such as ethics, cultural, and socioeconomic factors.
Lessons and Future Gaps
Heavy lessons have been learned from the COVID-19 outbreak. In addition, this outbreak has sounded an alarm, revealing that China has an obvious knowledge gap in the public health government system and the mechanism of public health emergency management. We summarize the following lessons based on a very limited understanding.
First, very important questions exist: Who should report an epidemic outbreak? Where to report? And who should make these important decisions? To our knowledge, the Centers for Disease Control (CDC) in China has been established as the most effective reporting system since the SARS outbreak in 2003. This has been the case because the China government gives enough importance to the disease control and public health system, which was the best reporting system in the world at that time. For instance, the beginning of a number of high-level biosafety laboratories began, and high-end equipment continued to be deployed (58). Also, laboratory testing capacity, epidemiological investigation capacity, and on-site disposal capacity have been rapidly improved. Unfortunately, it seems that these did not develop fully during this SARS-CoV-2 pandemic (58).
We believe that, when people are facing a sudden outbreak of an unknown infectious disease, it is better to quickly take note and inform the public in a manner that the public health and emergency response could be implemented at an opportune time. According to the situation in early January 2020, the data integration of multiple levels may not have been realized in Wuhan. For example, the data of the infectious disease report system of the local CDC, the diagnosis and treatment data of the medical and administrative system, and the data of various research teams were not integrated on time in the early outbreak of Wuhan (59).
Second, in the early stages of the outbreak, the CDC did not develop good quality production of detection reagent in a very short time and did not ensure good production quality. In this sense, the case sample collection became very difficult. Thus, each communication and consultation channel between the local CDC and medical institutions did not have good collaboration in the early stages, which badly affected the early screening and diagnosis of the infected people (60).
Finally, in the very early stages, due to panic and anxiety among people, and lack of proper screening methods, residents with fever, influenza, and COVID-19 infection cases were admitted into fever clinics, resulting in a large number of patients with COVID-19 becoming the transmission source within the clinic setting, and cross-infection at the community level, hence putting the communities at a huge risk situation of was transmission. Obviously, the roles of general practitioners (GPs) and the community-level health service system may not have been fully developed in this crisis outbreak.
Strengths
• In the context of the global public health crisis, this is the first study to describe China's practices and lessons in fighting the epidemic of COVID-19. It could provide valuable insights for pandemic control and public health emergency management in other countries and regions.
• This analysis shows that NPIs (nong-pharmaceutical intervention) measures initiated the Spring Festival holiday including the unprecedented Wuhan city Lockdown decisions and launched the level −1 emergency response at a national level were strongly associated with a reduction in case numbers during the COVID-19 epidemic in China.
• This study provides a new research perspective on public health emergency management in China and contributes to the relevant research in this field.
Limitations
In this study, several limitations must be acknowledged. First, information on cured cases and death cases or unascertained cases (asymptomatic cases or patients with mild symptoms who could recover without seeking medical care) was not collected, so this was not discussed in the measures regarding medical treatment situations. In particular, the clinical features of the cases so that this shortcoming may not conducive to guide the control of the current Italian epidemic.
Second, we could not examine the impact of other factors of the national emergency response because other provinces were introduced simultaneously initiated across China. Because suspending intra-city public transport, and banning social public gatherings, home quarantine which was introduced at different times in different places, were also associated with overall containment virus transmission.
Finally, mental health sciences including psychiatry reach can play a key role in comforting individuals and front-line medical workers during the COVID-19 epidemic, and their family members. However, although Wuhan City had been shutting down transportation for more than 2 months, we did not discuss mental health services for patients, front-line medical workers, and their families. Therefore, future research should assess these impacts of COVID-19 prevention and control on the mental health issue.
Main Findings of the Study
(1) Prevention and control strategy
• First stage: (27 December 2019 to 19 January 2020) China Government respond promptly to emergencies 27 December 2019 to 19 January 2020, China reported the epidemic as soon as possible and took prompt action to carry out etiological and epidemiological investigations to stop the spread of the epidemic. Proactively notify the World Health Organization, the United States, and other countries of the epidemic situation in a timely manner, and publish the genome sequence of the new coronavirus to the world.
• Second stage: (January 20 to February 20) General Secretary of the CPC Central Committee, President of the People's Republic of China, and Chairman of the Central Military Commission Xi Jinping made important instructions on the pneumonia epidemic caused by the new coronavirus infection, pointing out that people's safety and health should be put first, and the spread of the epidemic should be resolutely curbed. Wuhan has deployed four categories of vulnerable people for centralized management, carried out door-to-door screening of all residents, and conducted centralized isolation and virus testing for those with suspected symptoms. Wuhan City completed and opened the first batch of 3 Fang hospitals. During this period, the daily diagnostic testing capacity has further increased to about 20,000 cases. Big data; Artificial intelligence technologies were applied to identify confirmed cases and their close contacts and to monitor the body temperature of people flow. On 18 February, the number of newly cured and discharged cases nationwide exceeded the number of newly confirmed cases, and the number of confirmed cases began to decline.
• Three stage: (21 February to 5 March) The rapid rise of the epidemic situation in Hubei Province and Wuhan City has been contained. The epidemic situation in the whole country except Hubei Province is generally stable. In March, the daily new cases were controlled within single digits, and the epidemic prevention and control achieved important results in stages. According to the development of the epidemic prevention and control situation, the Central Committee of the Communist Party of China has made a major decision to coordinate epidemic prevention and control, economic and social development, and orderly resumption of work and production.
(2) Lessons
• At the very early in the virus epidemic, the reporting of major national public health epidemics to the public was not timely and appropriate, and the initial scientific prevention and control plan was lacking. After the outbreak of the epidemic, the emergency response mechanism is difficult to deal with major public health emergencies that threaten people's health. The problem of insufficient nucleic acid detection capacity in the early stage of the epidemic.
• Communication and consultation channels between the local CDC and medical institutions did not have good collaboration in the early stages, which badly affected the early screening and diagnosis of virus-infected patients and thus the cases were been delayed diagnosis.
• After the epidemic outbreak, there is no implemented hierarchical diagnosis and treatment in Wuhan, and the functions of the community health service system have not been effectively developed, thus, forming a crowded hospital and greatly increasing the risk your cross-infection.
Conclusions
The NPIs taken by China play a decisive role to control the spread of novel coronavirus outbreaks. Further research and action are needed to ensure a sufficiently sensitive surveillance system and strong response mechanism, including the establishment of a highly accessible laboratory network, maintenance of awareness of both primary healthcare providers and the public, and regular training and exercise of local Centers for Disease Control and Prevention and general practitioners in the community-level.
Data Availability Statement
Publicly available datasets were analyzed in this study. These can be found at: http://www.nhc.gov.cn/xcs/yqtb/list_gzbd_3.shtml.
Author Contributions
SC and HX: conceived, designed the analysis, and conceputalizaion. SC and YZ: performed the analysis, wrote the paper, methodology, and writing—original draft. YZ and XZ: data curation. SC: formal analysis. HX and XZ: supervision. SC, AK, and HX: writing—review and editing. All authors contributed to the article and approved the submitted version.
Funding
This study was supported by the School Scientific Foundation of Guizhou Minzu University [Grant No. GZMU ([2019]YB05)].
Conflict of Interest
The authors have declared that no competing interests exist.
Publisher's Note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
Acknowledgments
We would like to take the opportunity to sincerely thank Xiongjie Guo for his contributions that collect the COVID-19 cases in the very early outbreak of COVID-19 crisis.
References
1. Li Q, Guan X, Wu P, Wang X, Zhou L, Tong Y, et al. Early transmission dynamics inWuhan, China, of novel coronavirus-infected pneumonia. N Engl J Med. (2020) 13:1199–207. doi: 10.1056/NEJMoa2001316
2. Huang C, Wang Y, Li X, Ren L, Zhao J, Hu Y, et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet. (2020) 395:497–506 doi: 10.1016/S0140-6736(20)30183-5
3. Chen L, Liu W, Zhang Q, Xu K, Ye G, Wu W, et al. RNA based mNGS approach identifies a novel human coronavirus from two individual pneumonia cases in 2019 Wuhan outbreak. Emerg Microbes Infect. (2020) 1:313–9. doi: 10.1080/22221751.2020.1725399
4. WHO. Coronavirus Disease 2019 (COVID-19) Situation Reports−03052020. WHO. Available online at: https://www.who.int/docs/default-source/coronaviruse/situation-reports/20200305-sitrep-25-covid-19.pdf?sfvrsn=61dda7d_2
5. Zhou P, Yang XL, Wang XG, Hu B, Zhang L, Zhang W, et al. A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature. (2020) 579:270–3. doi: 10.1038/s41586-020-2012-7
6. Tan WJ, Zhao X, Ma XJ, Wang WL, Niu PH, Xu WB, et al. A novel coronavirus genome identified in a cluster of pneumonia cases — Wuhan, China 2019–2020. China CDC Wkly. (2020) 2:61–2. doi: 10.46234/ccdcw2020.017
7. Zhu N, Zhang D, Wang W, Li X, Yang B, Song J, et al. A novel coronavirus from patients with pneumonia in China, 2019. N Engl J Med. (2020) 382:727–33. doi: 10.1056/NEJMoa2001017
8. WHO. Report of the WHO-China Joint Mission on Coronavirus Disease 2019 (COVID-19). Beijing: WHO (2020). Available online at: https://www.who.int/docs/coronaviruse/who-china-joint-mission-on-covid-19-final-report.pdf (accessed March 20, 2020).
9. China-WHO COVID-19 Joint Expert Group: Press Conference of WHO-China Joint Mission on COVID-19. Available online at: http://www.nhc.gov.cn/xcs/fkdt/202002/35991766592b4f9a83b5f2448ee6bbab.shtml (accessed February 16, 2020).
10. WHO. Report of the WHO-China Joint Mission on Coronavirus Disease 2019 (COVID-19). Beijing: WHO (2020). Available online at: https://www.who.int/docs/default-source/coronaviruse/WHO-China-joint-mission-on-covid-19-final-report.pdf (accessed March 2, 2020).
11. Wilder-Smith A, Chiew CJ, Lee VJ. Can we contain the COVID-19 outbreak with the same measures as for SARS? Lancet Infect Dis. (2020) 205:e102–7. doi: 10.1016/S1473-3099(20)30129-8
12. Special expert group for control of the epidemic of novel coronavirus pneumonia of the Chinese preventive medicine association. Chinese center for disease control and prevention. Zhonghua Liu Xing Bing Xue Za Zhi Zhi (in Chinese). (2020) 41:139–44. doi: 10.3760/cma.j.issn.0254-6450.2020.02.002
13. Chinese Center for Disease Control and Prevention. Guidelines for investigation and management of close contacts of COVID-19 cases. China CDC Wkly, (2020) 2:329–31. doi: 10.46234/ccdcw2020.084
14. National Health Commission of the People's Republic of China. Protocol on Prevention and Control of COVID-19. COVID-19 Prevention and Control.Protocol.V6.pdf. Beijing: National Health Commission of the People's Republic of China (2020).
15. President Xi Jinping's Speech at the Meeting on The Coordinated Implementation of COVID-19 Prevention and Control and Economic Social Development.pdf. Beijing: Xinhua news (2020). Available online at: http://www.gov.cn/xinwen/2020-02/23/content_5482453.htm (accessed February 29, 2020).
16. Novel Coronavirus-Infected Pneumonia is Managed as Class A Infectious Disease [EB/OL]. (2020). Available online at: http://www.nhc.gov.cn/jkj/s3578/202001/3a13637e1a9249a2b6047f34b772b5e6.shtml (accessed February 20, 2020).
17. Hubei Province People's Government. Notice of Novel Coronavirus in Wuhan Infected With Pneumonia Coronavirus Prevention and Control No. 1 [EB/OL]. (2020). Available online at: http://www.hubei.gov.cn/zhuanti/2020/gzxxgzbd/zxtb/202001/t20200123_2014402.shtml (accessed January 27, 2020).
18. Hubei Province People's Government. Notice of Novel Coronavirus in Wuhan infected with pneumonia Coronavirus Prevention and Control No. 7 [EB/OL]. (2020). Available online at: http://www.hubei.gov.cn/zhuanti/2020/gzxxgzbd/zxtb/202001/t20200124_2014779.shtml (accessed January 24, 2020).
19. During the Critical Period the the President Xi Jinping Further Pointed Out the Direction of the War “Epidemic Disease” in Bejing. Xinhua News. Available online at: http://www.xinhuanet.com/2020-02/11/c_1125556458.htm (accessed February 11, 2020).
20. Renming net News Reviews. As of the 10 February, the Number of Medical Workers Who Were Assist in Wuhan has Been Reached 18,000 Persons. Available online at: http:www.people.com (accessed February 11, 2020).
21. XinhuWuhan News review. Wuhan has opened seven shelter hospitals, more than 40 designated medical institutions. Available online at: http://www.xinhuanet.com/678politics/2020-02/12/c_1125566309.htm (accessed February 11, 2020).
22. Changjiang Daily news. Wuhan Will Launch a Three-Days Massive Roll Screenging. Available online at: http://news.hbtv.com.cn/p/1785297.html (accessed February 16, 2020).
23. Hubei Province COVID-19 prevention and control headquarters: Introducing treatment situation and progress in the containment of COVID-19. The 29th Press Conference of Hubei Province COVID-19 Prevention and Control on February 22. Wuhan. Available online at: http://www.hubei.gov.cn/xinwen/2020-02/022/content_5473551.htm (accessed February 29, 2020).
24. The The State Council's Joint Prevention Control Mechanism was Introduced at a Press Conference held on March 6: “China's State Council Stated on a March 6 Conference That as of February 26 Nearly, 15,.4 Million Test Kits had Been Served, With an Average Daily Supply of 2 5, 000” in Hubei province. Available online at: http://www.hubei.gov.cn/xinwen/2020-03/02/content_5473551.htm (accessed March 30, 2020).
25. New views. World Health Organization Declares the New Coronavirus Outbreak Listed as Public Health Emergency of International Concern(PHEIC), Regarding the Outbreak of Novel Coronavirus 2019 in the People's Republic of China, With Exportations to Other Countries, Took Place on Thursday,2020. January 30 13:30 to 18:35 Geneva time (CEST). Geneva: New views. Available online at: http://www.people.cn/xinwen/2020-01/30/content_5473551.htm (accessed March 2, 2020).
26. Calisher C, Carroll D, Colwell R, Corley RB, Daszak P, Drosten C, et al. Statement in support of the scientists, public health professionals, and medical professionals of China combatting COVID-19. Lancet. (2020) 395:e42–3. doi: 10.1016/S0140-6736(20)30418-9
27. Wang FS, Zhang C. What to do next to control the 2019-nCoV epidemic? Lancet. (2020) 395:391–3. doi: 10.1016/S0140-6736(20)30300-7
28. Heymann DL, Shindo N. COVID-19: what is next for public health? Lancet. (2020) 395:542–5. doi: 10.1016/S0140-6736(20)30374-3
30. Saglietto A, D'Ascenzo F, Zoccai GB, De Ferrari GM. COVID-19 in Europe: the Italian lesson. Lancet. (2020) 395:1110–1. doi: 10.1016/S0140-6736(20)30690-5
31. International Financial News. The British Call for “Herd Immunity” Will be Implemented in This Country? Available online at: https://tech.sina.com.cn/roll/2020-04-21/doc-iircuyvh9079282.shtml (accessed April 11, 2020).
32. Pan A, Liu L, Wang C, Guo H, Hao X, Wang Q, et al. Association of public health interventions with the epidemiology of the COVID-19 outbreak in Wuhan, China. JAMA. (2020) 323:1915–23. doi: 10.1001/jama.2020.6130
33. Hao X, Cheng S, Wu D, Wu T, Lin X, Wang C, et al. Reconstruction of the full transmission dynamics of COVID-19 in Wuhan. Nature. (2020) 584:420–4. doi: 10.1038/s41586-020-2554-8
34. Fong MW, Gao H, Wong JY, Xiao J, Shiu EY, Ryu S, et al. Nonpharmaceutical measures for pandemic influenza in nonhealthcare settings-social distancing measures. Emerg Infect Dis. (2020) 26:976–84. doi: 10.3201/eid2605.190995
35. Yang Z, Zeng Z, Wang K, Wong S-S, Liang W, Zanin M, et al. Modified SEIR and AI prediction of the epidemics trend of COVID-19 in China under public health interventions. J Thorac Dis. (2020) 12:165–74. doi: 10.21037/jtd.2020.02.64
36. Kraemer MUG, Yang CH, Gutierrez B, Wu CH, Klein B, Pigott DM, et al. The effect of human mobility and control measures on the COVID-19 epidemic in China. Science. (2020) 368:493–7. doi: 10.1126/science.abb4218
37. Chinazzi M, Davis JT, Ajelli M, Gioannini C, Litvinova M, Merler S, et al. The effect of travel restrictions on the spread of the 2019 novel coronavirus (COVID-19) outbreak. Science. (2020) 368:395–400. doi: 10.1126/science.aba9757
38. Hellewell J, Abbott S, Gimma A, Bosse NI, Jarvis CI, Russell TW, et al. Feasibility of controlling COVID-19 outbreaks by isolation of cases and contacts. Lancet Glob Health. (2020) 8:e488–96. doi: 10.1016/S2214-109X(20)30074-7
39. Quilty BJ, Clifford S, Flasche S, Ego RM. Effectiveness of airport screening at detecting travellers infected with novel coronavirus (2019-nCoV). Euro Surveill. (2020) 25:2000080. doi: 10.2807/1560-7917.ES.2020.25.5.2000080
40. China-WHO Expert Team. Report of the WHO-China Joint Mission on Coronavirus Disease 2019 (COVID-19). Beijing: China-WHO Expert Team (2020).
41. Lai S, Ruktanonchai NW, Zhou L, Prosper O, Luo W, Floyd JR, et al. Effect of non-pharmaceutical interventions to contain COVID-19 in China. Nature. (2020) 585:410–3. doi: 10.1038/s41586-020-2293-x
42. The State Council of the People's Republic of China. Press Conference of the Joint Prevention and Control Mechanism of the State Council on COVID-19: Rescue Works Guided by the Central Leadership Group. (2020). Available online at: http://www.gov.cn/xinwen/2020-02/28/content_5484713.htm (accessed March 27, 2020).
43. Fangcang Shelter Hospitals. Xinhua News. Noah's Ark: The story of Fangcang Shelter Hospitals. (2020). Available online at: http://www.xinhuanetcom/2020-02/19/c_1125598560.htm (accessed February 24, 2020).
44. Changjiang Daily. Wuhan's Qiaokou Wuti Fangcang Shelter Hospital Becomes The First Closed Fangcang Shelter Hospital. (2020). Available online at: https://mp.weixin.qq.com/s/5yEF1YADZ9v1CIa0Dj703w (accessed March 1, 2020).
45. Chen S, Zhang Z, Yang J, Wang J, Zhai X, Bärnighausen T, et al. Fangcang shelter hospitals: a novel concept for responding to public health emergencies. Lancet. (2020) 395:1305–14. doi: 10.1016/S0140-6736(20)30744-3
46. Shang L, Xu J, Cao B. Fangcang shelter hospitals in COVID-19 pandemic: the practice and its significance. Clin Microbiol Infect. (2020) 26:976–8. doi: 10.1016/j.cmi.2020.04.038
47. Fang D, Pan S, Li Z, Yuan T, Jiang B, Gan D, et al. Large-scale public venues as medical emergency sites in disasters: lessons from COVID-19 and the use of Fangcang shelter hospitals in Wuhan, China. BMJ Glob Health. (2020) 5:e002815. doi: 10.1136/bmjgh-2020-002815
48. The National Health Commission of the People's Republic of China. Press Conference of the Joint Prevention and Control Mechanism of the State Council on April 14, 2020. Available online at: http://www.nhc.gov.cn/xcs/fkdt/202005/e78dfc196504497586f324f0d9a5bc36.shtml (accessed May 29, 2020).
49. The National Health Commission of the People's Republic of China. Press Conference of the Joint Prevention and Control Mechanism of the State Council on COVID-19: Hospital Authority Commissioner-Guo Yanhong speeching. National Health Commission of the People's Republic of China. Beijing (2020). Available online at: http://www.nhc.gov.cn/xcs/yqtb/202004/28668f987f3a4e58b1a2a75db60d8cf2.shtml (accessed March 19, 2020).
50. Hubei News. 98.6% Statement Tell us There are Still Missing Some Suspected Cases in Wuhan-Wuhan Government Has Launched A Massive Screening Action. Available online at: http://www.hubei.gov.cn/hbfb/szsm/202002/t20200223_2145590.shtml (accessed March 18, 2020).
51. Tian H, Liu Y, Li Y, Wu CH, Chen B, Kraemer MUG, et al. An investigation of transmission control measures during the first 50 days of the COVID-19 epidemic in China. Science. (2020) 368:638–42. doi: 10.1126/science.abb6105
52. Zhang J, Litvinova M, Wang W, Wang Y, Deng X, Chen X, et al. Evolving epidemiology and transmission dynamics of coronavirus disease 2019 outside Hubei province, China: a descriptive and modeling study. Lancet Infect Dis. (2020) 20:793–802. doi: 10.1016/S1473-3099(20)30230-9
53. Zhang Y, Jiang B, Yuan J, Tao Y. The impact of social distancing and epicenter lockdown on the COVID-19 epidemic in mainland China: a data-driven SEIQR model study. medRxiv. Preprint. (2020) 1:1–12. doi: 10.1101/2020.03.04.20031187. [Epub ahead of print].
54. Li Z, Chen Q, Feng L, Rodewald L, Xia Y, Yu H, et al. Active case finding with case management: the key to tackling the COVID-19 pandemic. Lancet. (2020) 396:63–70. doi: 10.1016/S0140-6736(20)31278-2
55. People. At the 45th Conferences of the UN Human Rights Council, The Representative of China Called on 6l Countries to Put People's Life and Health First. Brussels: Geneva News (2020). Available online at: https://www.People'sDaily.cn (accessed September 20, 2020).
56. Lancet T. Sustaining containment of COVID-19 in China. Lancet. (2020) 395:1230. doi: 10.1016/S0140-6736(20)30864-3
57. Gostin LO, Hodge JG Jr. US emergency legal responses to novel coronavirus: balancing public health and civil liberties. JAMA. (2020) 323:1131–2. doi: 10.1001/jama.2020.2025
58. Why China's. CDC System Faces a Confidence Crisis? Newsweek News Reviewes. Available online at: https://www.newsweek.cn (accessed February 27, 2020).
59. Huang J, Nie SF, Wei S. Reflections on present response to the pneumonia associated with a novel coronavirus (2019 - nCov). J New Med. (2020) 3:1–4.
Keywords: China, COVID-19, intervention measures, change features, lessons
Citation: Cheng S, Zhao Y, Kaminga AC, Zhang X and Xu H (2022) China's Fight Against COVID-19: What We Have Done and What We Should Do Next? Front. Public Health 10:548056. doi: 10.3389/fpubh.2022.548056
Received: 01 April 2020; Accepted: 17 March 2022;
Published: 21 June 2022.
Edited by:
Delia Boccia, University of London, United KingdomReviewed by:
Zachary Desson, Erasmus University Rotterdam, NetherlandsGang Sun, Johns Hopkins University, United States
Copyright © 2022 Cheng, Zhao, Kaminga, Zhang and Xu. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Huilan Xu, aHVpbGFueHVfY3N1QDE2My5jb20=
 Sixiang Cheng1,2
Sixiang Cheng1,2 Yuxin Zhao
Yuxin Zhao Atipatsa Chiwanda Kaminga
Atipatsa Chiwanda Kaminga Huilan Xu
Huilan Xu