- 1Adult Health Nursing and Critical Care, Riyadh Elm University, Riyadh, Saudi Arabia
- 2Department of Nursing Management and Education, Princess Nourah Bint Abdulrahman University, Riyadh, Saudi Arabia
- 3Department of Nursing Management, Zarqa University, Zarqa, Jordan
- 4Community Health Nursing, Al-Zaytoonah University of Jordan, Amman, Jordan
Background: Needle stick injuries constitute the greatest threat to nursing students during clinical practice because of accidental exposure to body fluids and infected blood. The purpose of this study was to (1) determine the prevalence of needle stick injuries and (2) measure the level of knowledge, attitude and practice among nursing students about needle stick injuries.
Methods: Three hundred participants undergraduate nursing students at a private college in Saudi Arabia were included, of whom 281 participated, for an effective response rate of 82%.
Results: The participants showed good knowledge scores with a mean score of 6.4 (SD = 1.4), and results showed that students had positive attitudes (Mean = 27.1, SD = 4.12). Students reported a low level of needle stick practice (Mean = 14.1, SD = 2.0). The total prevalence of needle stick injuries in the sample was 14.1%. The majority, 65.1%, reported one incidence in the last year, while (24.4%) 15 students reported two incident of needle stick injuries. Recapping was the most prevalent (74.1%), followed by during injection (22.3%). Most students did not write a report (77.4%), and being worried and afraid were the main reasons for non-reports (91.2%). The results showed that female students and seniors scored higher level in all needle stick injuries domains (knowledge, attitude and practice) than male students and juniors. Students who had needle stick injuries more than three times last year reported a lower level of all needle stick injury domains than other groups (Mean = 1.5, SD =1.1; Mean = 19.5, SD =1.1; Mean = 9.5, SD =1.1, respectively).
Conclusion: Although the student’s showed good knowledge and positive attitudes in NSI, the students reported a low level of needle stick practice. Raising awareness among nursing students and conducting continuing education related to sharp devices and safety and how to write an incident reporting is highly recommended.
Background
Nearly all nursing students experience some adverse effects or challenges in their clinical or training placement that compromise their safety or the patient’s safety (1). One primary challenge nursing students face is needle stick injuries (2). Needle Stick Injury (NSI) is a nonintentional wound or injury that results from needles connected with Intravenous (IV) and blood transfusion sets (3). Exposure to contaminated needles may expose those injured to the potential risk of pathogens such as Hepatitis B (HBV), Hepatitis C (HCV) and Human Immunodeficiency Virus (HIV), with a post-exposure transmission rate of 30%, 5–10, and 0.4%, respectively, (4).
Percutaneous exposure to body fluids and blood during sharp equipment and needle stick infection is considered the main occupational hazard for mortality and morbidity risk of pathogens in the clinical environment (5). The risk of exposure and transmission to blood-borne pathogen infections through needle sticks and sharp injuries is very high among healthcare students, specifically nursing students (6–8). The prevalence of NSI among nursing students varied in numerous studies worldwide, ranging from 11.8 to 85.0% (6, 9). In recent systematic review showed prevalence of NSI in developing countries was significantly higher than in developed countries among nurses (10). Alsabaani et al. found that the prevalence of needle stick injury among healthcare workers in Saudi Arabia was 11.57% (11). In a recent study conducted among healthcare workers in Saudi Arabia, the prevalence of needle stick injury was 22.2% (12).
Most NSI incidents occurred through drug preparation, administration, recapping, holding syringes without a suitable container, opening needle caps, suturing and blood sampling (12–15). Other causes include inadequate staff, lack of training, lack of experience with infection-control standards, and insufficient appropriate resources (16, 17).
Several psychological consequences of NSI have been noted. For example, a systematic review found that depression, fear, and anxiety were the main psychological effects of NSI among nursing students, and the study suggested that students in their clinical fields need more support and counseling services after being exposed to injury (18). Another study in a psychiatric trauma clinic reported that exposure to NSI can create mental problems (19). Thus, policymakers and teachers need to direct their attention to the mental and physical consequences of NSI.
The National Institute for Occupational Safety and Health has issued prevention guidelines for healthcare providers and students to control needle stick injuries (20). Post-exposure prophylaxis plays a significant role in preventing a person from HIV, HBV and HCV and their chronicity (21). Therefore, promptly reporting an incident is crucial for a student or healthcare personnel; failure to do that may result in catastrophic consequences (19). Using safer devices, administering Hepatitis B vaccination, pre-exposure prophylaxis and administering post-exposure prophylaxis contribute to decreasing the incidences drastically and are cost-effective (20).
Most studies conducted in Saudi Arabia included healthcare workers and ignored the nursing students. In fact, the nursing students are more vulnerable to NSIs because of their lack of clinical experience. The current study aimed to address this issue by (1) assessing the prevalence of NSI and (2) measuring the level of knowledge, attitude and practice among nursing students about NSI.
Methodology
Study design
This cross-sectional and descriptive study was conducted among undergraduate nursing students.
Sample size and study setting
The study was performed in a private college in Saudi Arabia. This college has seven branches in Saudi Arabia (Riyadh, Jeddah, Najran, Abha, Tabuk, Al Madinah Al Munawwarah and Dammam) and includes more than 440 undergraduate nursing students. G* power software was used to calculate the sample size. Based on an estimated effect size of (d) = 0.7, ά = 0.05, power = 0.95, the required sample size was estimated at 254 to run a paired sample t-test. Three hundred students were asked to participate, of whom 281 participated, for a response rate of 82%. In literature reviews, as a general rule, a sample size of 200–300 is considered sufficient for this type of study (22, 23). This study specifically focuses on students from the second to the final year, which is their clinical practice time, where they are at high risk of contracting NSI through a particular procedure–for instance, applying intravenous cannula and venipunctures, among others.
Data collection tool
The researchers prepared the questionnaire based on NSI studies (6, 8). The questionnaire had four parts. The first part consisted of two parts, the first part asked for demographic data such as gender, age, year of study, previous education of NSI, the second part were related Prevalence of NSI such as number of NSI incidences last year, how the incidences occurred, writing an incident report and reasons for not reporting. Part two comprised eight knowledge questions related to general information about NSI, such as definitions of NSI, common causes, sharps containers, and knowledge about blood-borne diseases. Each question included two options (True, False). The true answer was scored 1, while the false answer was 0. The total knowledge score could range from 0 to 8, where a higher score represents a higher knowledge level. The third part comprised seven statements related to attitudes toward NSI perceptions. Responses were from 1 to 5, using a 5-point Likert-type scale (“Strongly Agree 5,” to “Strongly Disagree 1”). The positive score ranged from 5 to 35, where a higher score represents a higher knowledge level. The last part contained statements about five practice-related needle stick injuries, including standard precautions and vaccination status for the protections, preventions precautions about NSI and what you should do after an incidence occurs Post-exposure prophylaxis (PEP). These statements used a 5-point Likert-type scale (always 5, often 4, sometimes 3, rarely 4, never 5), with a total score ranging from 5 to 25, where a higher score represents a higher practice level.
Three doctors of nursing and infection control reviewed the content validity and item language to evaluate whether the questionnaire items effectively captured the most information students need to prevent NSI. The review committee recommended that the questionnaires cover most NSI prevention information, the language being easy to understand and straightforward. A pilot was conducted with information from ten respondents. The questionnaires had good reliability and internal consistency with Cronbach’s alpha of 0.80, 0.71, and 0.72 in terms of knowledge, attitude and practice categories, respectively. A good degree of inter-rater inter-observer reliability was found between questionnaire items. The average interclass correlation coefficient was 0·81 with a 95% confidence interval from 0·79 to 0·86 [F = 4·5, p = 0·01].
Data collection
After the ethical approval was secured from the ethical review committee at the university where the study was held, with reference number (2022/77/10), the researchers recruited students through an online survey widely used for surveys worldwide. An online survey in Google forms was sent to students via social media such as Facebook and WhatsApp. Information, including the study’s aim and link attachment, was sent along with instruments to guide the participants in filling out the survey. Agreement to participate in the study was obtained when the participants completed the online survey. Reminders were sent frequently to remind students to fill out the survey. The study was open from January until December 2022. The study was open from January until December 2022. To prevent the duplicate submission of the survey, participants could only fill out the survey once.
Statistical analysis
The data were imported from the online survey into the Statistical Package for the Social Sciences (SPSS) Version 20. Descriptive statistics percentage, frequency, mean, and standard deviation were calculated. Independent t-tests and a One-Way Analysis of Variance (ANOVA) were applied to compare the means of total knowledge with sample characteristics. A value of p of <0.05 was considered significant.
Results
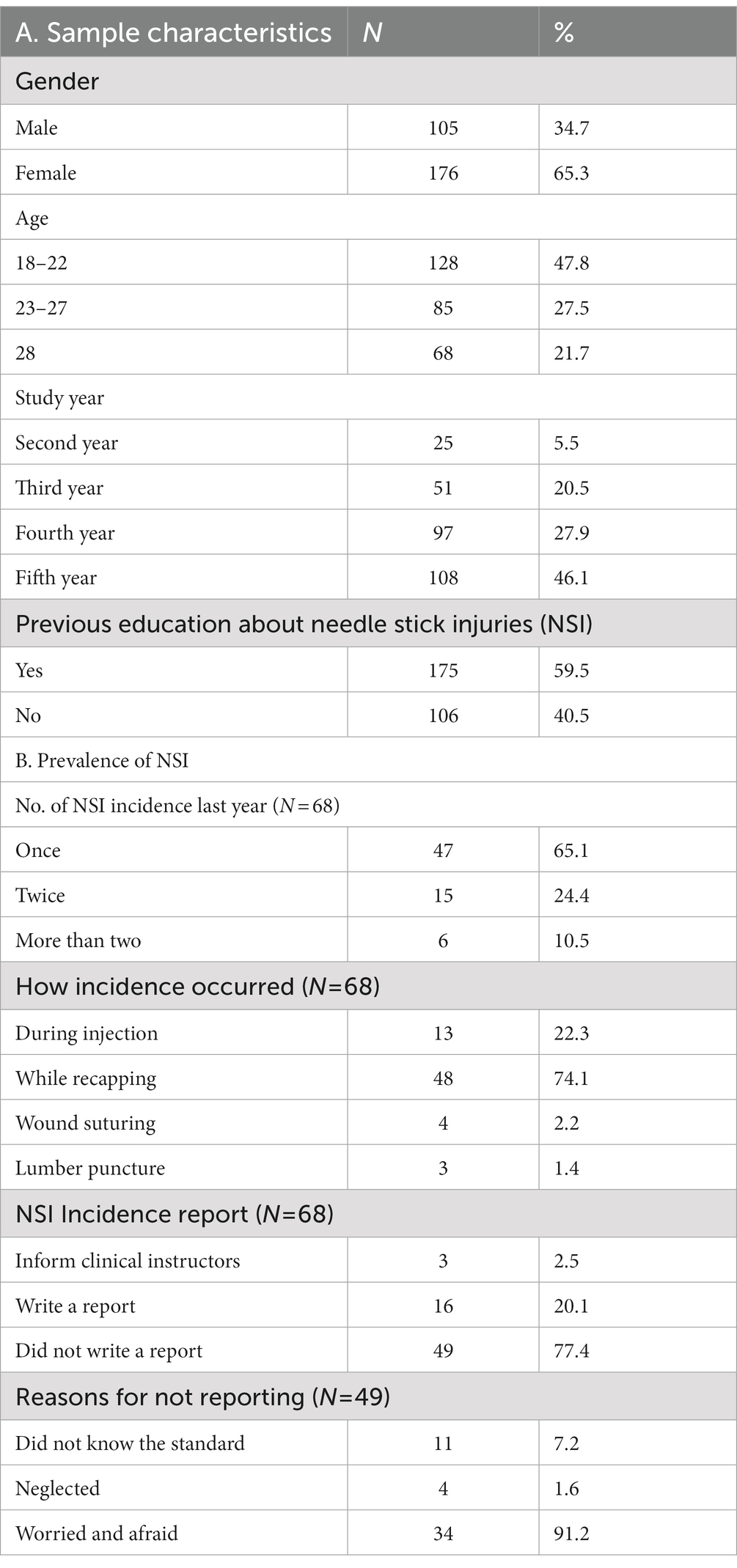
A total of 281 students completed the electronic survey, which gave an overall 81.5% response rate. The mean age was 24.9 (SD = 1.3) years. Most participants were female students 65.3% (n = 176). Of the total sample, 46.1% (n = 108) were in their fifth year of study. Of the 281 students, (n = 68) reported having experienced needle stick injuries. Regarding previous NSI education, 59.5% of them had previous education. The total prevalence of NSI among our sample was 14.1%. The majority of students n = 47 (65.1%) reported one incidence in the last year, while n = 15 (24.4%) students reported two incidences. Recapping incidents occurred the most (74.1%) which is considered as a wrong practice, followed by during injection (22.3%). Most students did not write a report (77.4%) and being worried and afraid were the main reasons for non-reports (91.2%; Table 1).
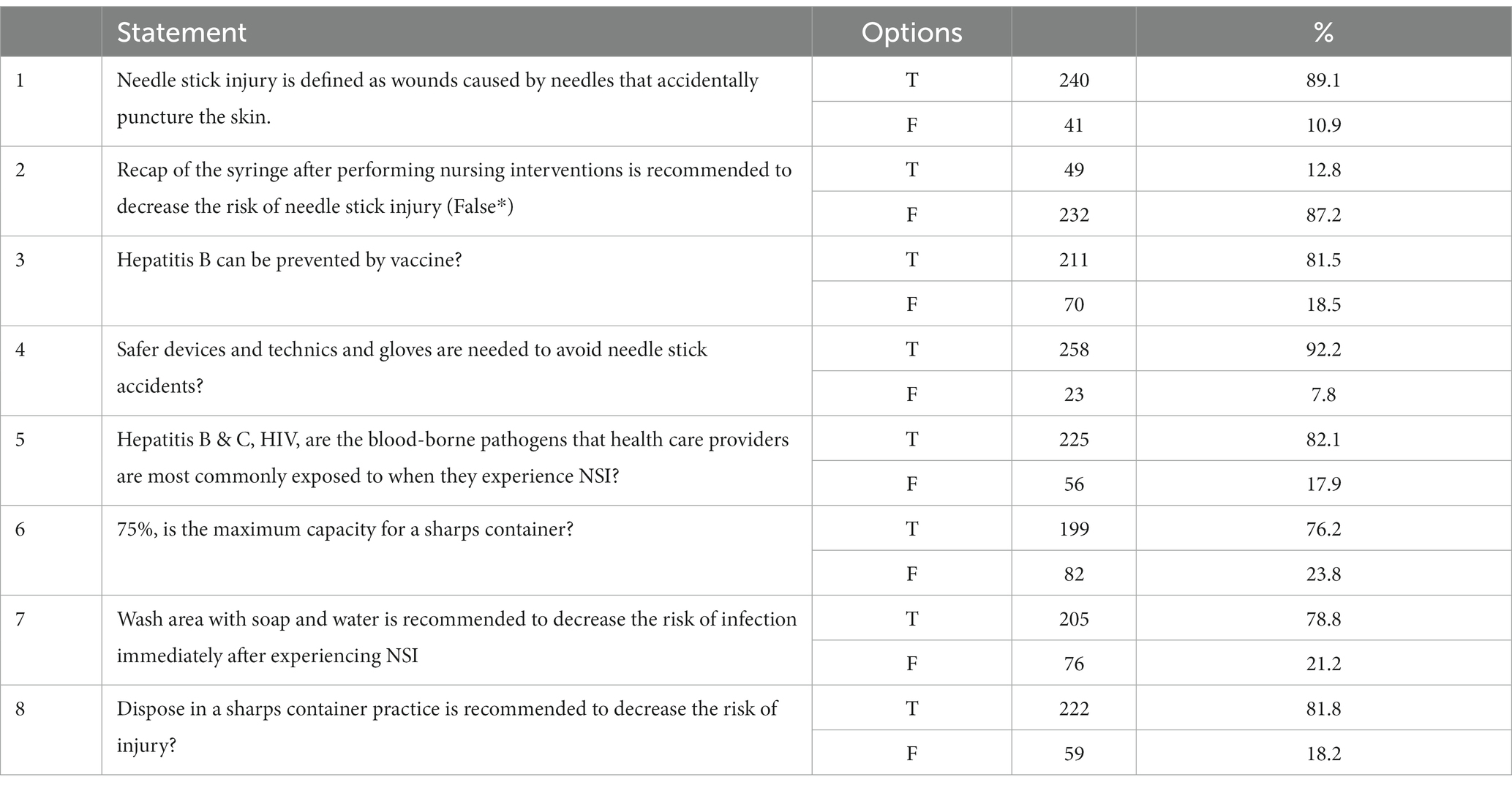
Total NSI knowledge scores for the participating students ranged from 1 to 8, with a mean score of 6.4 (SD = 1.4). The range of correct answers to each question ranged from 76.2 to 92.2%, which was 77.0% of the highest possible score. “Safer devices and technics and gloves are needed to avoid needle stick accidents” received the highest correct answer percentage (92.2%). The lowest correct answers percentage (75%) was for the item “is the maximum capacity for a sharps container” (76.2%; Table 2).
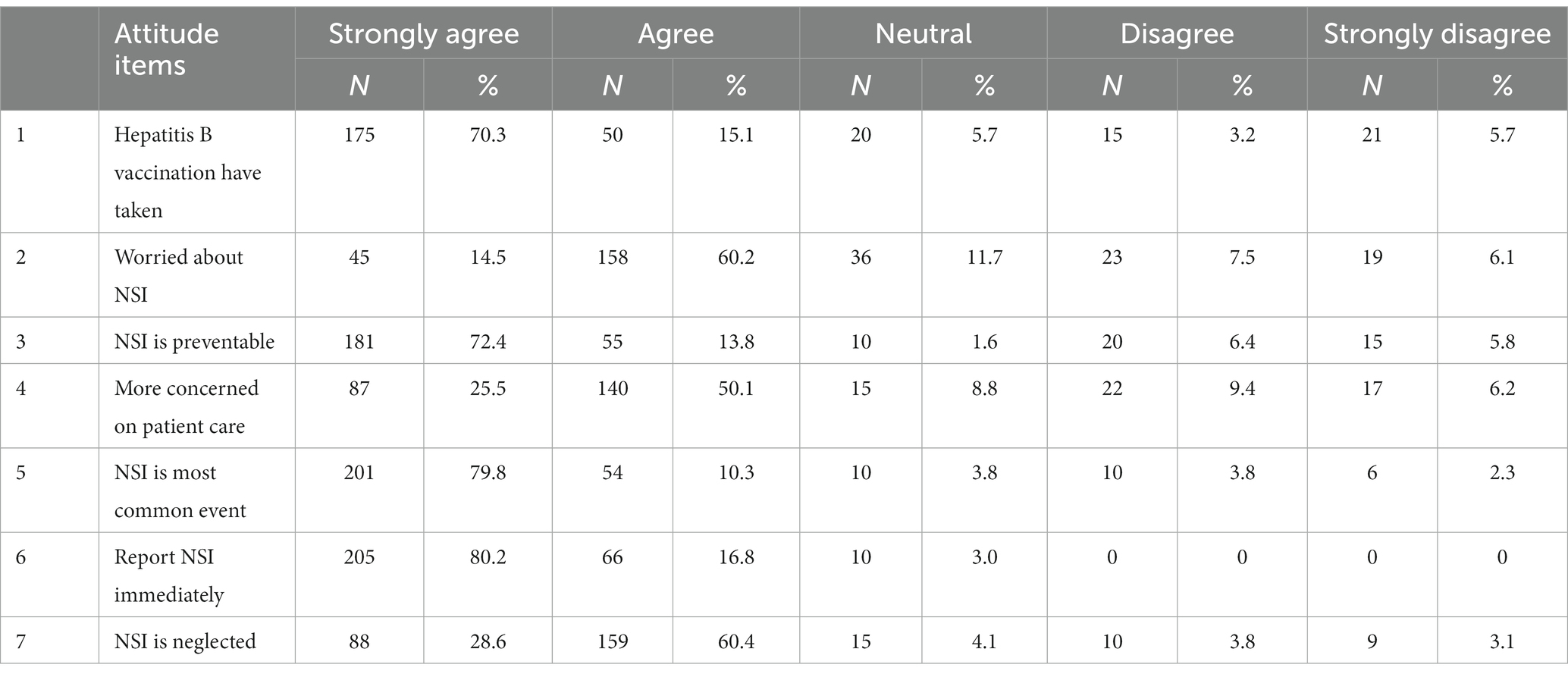
Table 3 shows the mean for the attitude of needle stick injury among nursing students. In general, results showed that students had positive attitudes (Mean 27.1, SD = 4.12). For example, two-thirds of students had taken a hepatitis B vaccination. Likewise, 60.2% reported that they worried about NSIs, and 72.4% believed that an NSI was preventable. Only half of the students were more concerned about patient care. Most students perceived NSI as the most common event (79.8%). Finally, 60.4% of students agreed that NSI was neglected.
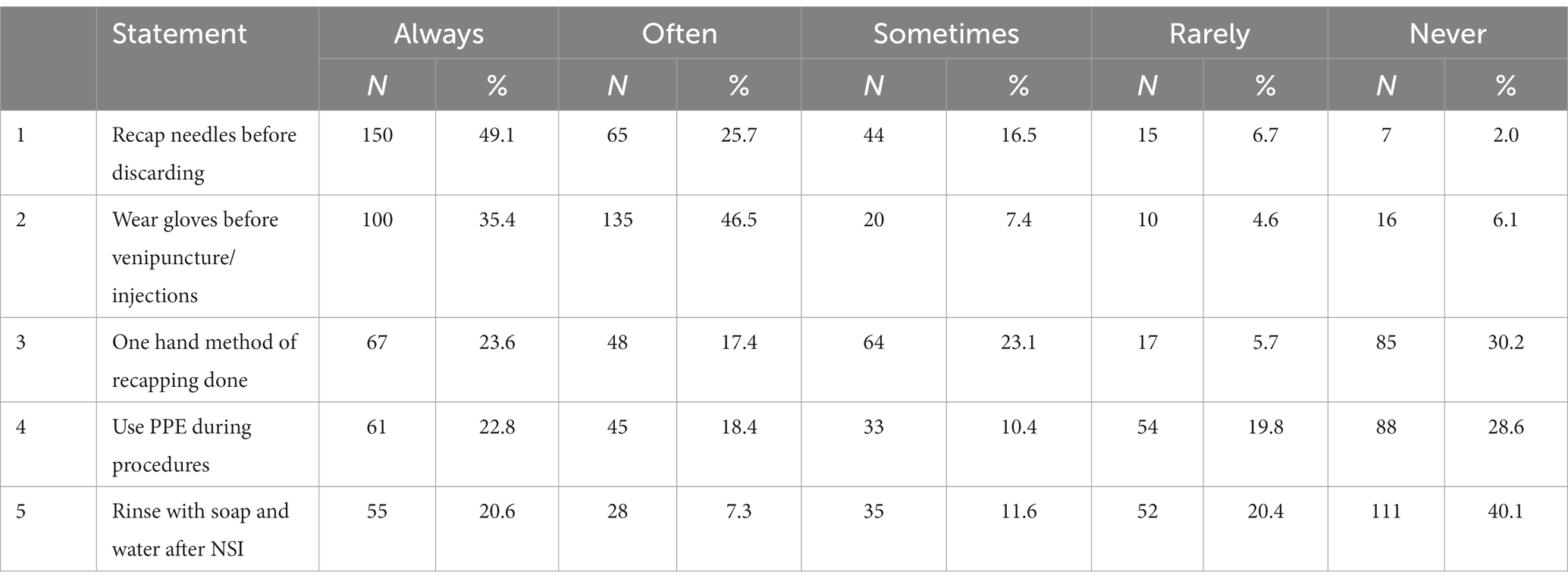
Students reported a low level of needle stick practices (M = 14.1, SD = 2.0). Half of the students always recapped needles before discarding them (50.1%). Approximately one-third of the students reported wearing gloves before venipuncture/injections (35.4%). Only one-quarter of the students reported using one-handed recapping, using PPE during procedures, and rinsing with soap and water after NSI (23.6, 22.8, 20.6%), respectively (Table 4).
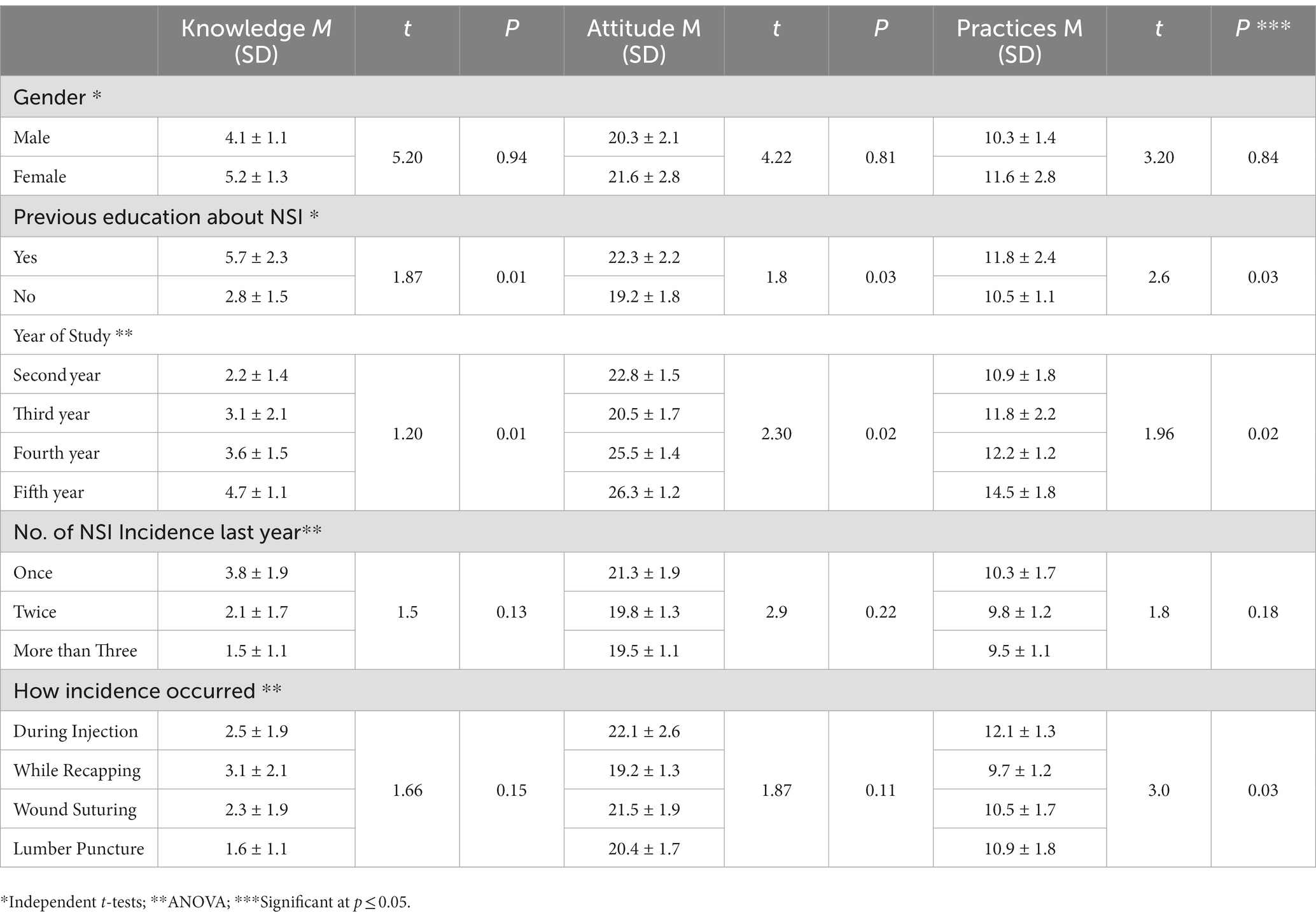
The total knowledge, attitude and practice scores were compared among nursing students. The results showed that female students and seniors scored higher in all NSI domains than male students and juniors. Students who reported NSI incidences more than three times in the last year had a lower level of all NSI domains than other groups (M = 1.5, SD =1.1; M = 19.5, SD =1.1; M = 9.5, SD =1.1, respectively; Table 5).
Discussion
Needle stick injuries constitute the greatest threat to nursing students during clinical practice because of accidental exposure to body fluids and infected blood affect the patient safety (24–26). The current study demonstrated significant results related to nursing students in terms of knowledge, attitudes, and practices related to needlestick injuries. Notably, the students had adequate knowledge of NSI. This result aligns with a study conducted in Northern Cyprus, where participants showed inadequate knowledge (27) and contrasted with international studies that showed the students had inadequate knowledge of NSI (8, 28, 29). Such a high score indicates that nursing students in the current study had sufficient knowledge regarding NSI, confirming that the nursing school offered special courses such as infection control to students before starting clinical practice (30). More than half of the nursing students were senior students and had previous education about NSI, meaning they have high exposure to the causes and risk factors of needle stick injuries.
Participants’ attitudes toward NSI were positive and dissimilar to a previous study (31) but similar to a national study that showed positive attitudes toward NSI among healthcare providers (21). Students’ positive attitudes confirm that nursing schools are the proper place to raise students’ awareness and behavior in terms of NSI attitudes before transmission in clinical practice and enhance their decision-making skills (32).
Regarding post-exposure treatment for NSI and methods of prevention practice, the mean was low. For example, less than half of the participants reported consistently engaging in post-exposure treatment for NSI, and this finding is consistent with previous studies (8, 28). Inadequate post-exposure treatment for NSI practice has been considered the most significant risk of NSI, leading to unsafe practice during clinical practice (33, 34). However, preventive and post-exposure measures topics should be taught and mandatory in all nursing schools’ curriculums before starting clinical practice (35).
The total prevalence of NSI among our sample was 14.1%. These percentages are lower than different studies, such as Germany (21.4%) (36) and Taiwan (18.2%) (37). A recent systematic review and meta-analysis showed that the prevalence of NSI among nursing students in Asia countries was higher than in Europe (39.7%) (38). Failure to recap the needles was reported as a common cause of NSIs, similar to several studies (6, 8). Finally, many students did not fill out an incident report because they were worried and feared being blamed. Under-reporting NSI is a major clinical challenge that may have undermined the validity of existing data regarding this issue (38, 39).
In the current study, the results showed no significant differences in NSI domain scores between the participants regarding genders, although females demonstrated higher scores on all domains than male students. These results were similar to study nursing students in Turkey, where students showed a different level of NSI knowledge (40). Conversely, Jordanian nursing students did not show significant differences in knowledge of NSI (8). The varied level of knowledge among the students may be related to infection control courses and contents in the different nursing schools.
Our study shows that senior nursing students had better scores than junior students, similar to (8). These results can be because senior nursing students had more experience in infection control practices and had taken more courses. This result emphasized that infection control courses would be better given a preparatory year to ensure that students had adequate knowledge before shifting to clinical practice.
In this study, nursing students with more than three incidences in the last year of NSI showed lower overall NSI knowledge domains than other groups. This result may be explained because students were inexperienced or stressed while carrying out invasive procedures. Underdeveloped skills and lack of clinical experience may be associated with an increased risk of NSIs among health professional students (41–43). However, the risk of NSIs is linked with clinical skill and may also be associated with the frequency of procedures and inherent hazards and influences individual health management (44, 45).
This study had limitations. Using online surveys in data collection could lead to inaccurate results and recall bias. Because the study was conducted in one private university and one nursing faculty with different branch, this may reduce the generalizability of our findings. Nonetheless, this study helps fill a knowledge gap because there are few studies in nursing education in Saudi Arabia about injuries and safety issues. Future studies, including students in healthcare professions, are highly recommended.
Conclusion
Although the student’s showed good knowledge and positive attitudes in NSI, the students reported a low level of needle stick practice. The exposure of nursing students to needle stick injury and its non-reporting remains a persistent challenge. Raising awareness among nursing students and conducting continuing education related to sharps devices and safety is highly recommended. Policymakers should implement several initiatives to reduce NSI incidences, such as safe injection practices, safety precautions, reporting systems, and the use of post-exposure prophylaxis.
Data availability statement
The raw data supporting the conclusions of this article will be made available by the authors, without undue reservation.
Ethics statement
The studies involving human participants were reviewed and approved by After the ethical approval was secured from the ethical review committee, with reference number (2022/77/10). The patients/participants provided their written informed consent to participate in this study.
Author contributions
All authors listed have made a substantial, direct, and intellectual contribution to the work and approved it for publication.
Funding
This research was funded by Princess Nourah bint Abdulrahman University Researchers Supporting Project number (PNURSP2023R293), Princess Nourah bint Abdulrahman University, Riyadh, Saudi Arabia.
Acknowledgments
The authors extend their appreciation to Princess Nourah bint Abdulrahman University Researchers Supporting Project, Princess Nourah bint Abdulrahman University, Riyadh, Saudi Arabia for funding this research work through the project number (PNURSP2023R293).
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Publisher’s note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
References
1. García-gámez, M, Morales-Asencio, JM, García-Mayor, S, Kaknani-Uttumchandani, S, Martí-García, C, and Lopez-Leiva, I. Adverse events encountered during clinical placements by undergraduate nursing students in Spain. Nurse Educ Today. (2020) 91:104480. doi: 10.1016/j.nedt.2020.104480
2. Yao, WX, Wu, YL, Yang, B, Zhang, LY, Yao, C, Huang, CH, et al. Occupational safety training and education for needlestick injuries among nursing students in China: intervention study. Nurse Educ Today. (2013) 33:834–7. doi: 10.1016/j.nedt.2012.02.004
3. Akeem, BO, Abimbola, A, and Idowu, AC. Needle stick injury pattern among health workers in primary health care facilities in Ilorin, Nigeria. Acad Res Int. (2011) 1:419.
4. Wilburn, SQ, and Eijkemans, G. Preventing needlestick injuries among healthcare workers: a WHO-ICN collaboration. Int J Occup Environ Health. (2004) 10:451–6. doi: 10.1179/oeh.2004.10.4.451
5. Hashmi, A, Al Reesh, SA, and Indah, L. Prevalence of needle-stick and sharps injuries among healthcare workers, Najran, Saudi Arabia. Epidemiology. (2012) 2:117. doi: 10.4172/2161-1165.1000117
6. Al Qadire, M, Ballad, CC, Al Omari, O, Aldiabat, K, Abu Shindi, Y, and Khala, A. Prevalence, student nurses’ knowledge and practices of needle stick injuries during clinical training: a cross-sectional survey. BMC Nurs. (2021) 20:187. doi: 10.1186/s12912-021-00711-2
7. Motaarefi, H, Mahmoudi, H, Mohammadi, E, and Hasanpour-Dehkordi, A. Factors associated with needlestick injuries in health care occupations: a systematic review. J Clin Diagn Res. (2016) 10:IE01–4. doi: 10.7860/JCDR/2016/17973.8221
8. Sulimana, M, Al Qadireb, M, Alazzama, M, Alousha, S, Alsarairehc, A, and Alsaraireh, FA. Students nurses' knowledge and prevalence of needle stick injury in Jordan. Nurse Educ Today. (2018) 60:23–7. doi: 10.1016/j.nedt.2017.09.015
9. Assen, S, Wubshet, M, Kifle, M, Wubayehu, T, and Aregawi, BG. Magnitude and associated factors of needle stick and sharps injuries among health care workers in Dessie City hospitals, north East Ethiopia. Nursing. (2020) 19:31. doi: 10.1186/s12912-020-00422-0
10. Abdelmalik, MA, Alhowaymel, FM, Fadlalmola, H, Mohammaed, MO, Abbakr, I, Alenezi, A, et al. Global prevalence of needle stick injuries among nurses: a comprehensive systematic review and meta-analysis. J Clin Nurs. (2023) 2023:1–13. doi: 10.1111/jocn.16661
11. Alsabaani, A, Alqahtani, NSS, Alqahtani, SSS, Al-Lugbi, JHJ, Asiri, MAS, Salem, SEE, et al. Incidence, knowledge, attitude and practice toward needle stick injury among health Care Workers in Abha City, Saudi Arabia. Front Public Health. (2022) 10:771190. doi: 10.3389/fpubh.2022.771190
12. Abalkhail, A, Kabir, R, Elmosaad, YM, Alwashmi, AS, Alhumaydhi, FA, Alslamah, T, et al. Needle-stick and sharp injuries among hospital healthcare Workers in Saudi Arabia: a cross-sectional survey. Int J Environ Res Public Health. (2022) 19:6342. doi: 10.3390/ijerph19106342
13. Bagnasco, A, Zanini, M, Catania, G, Watson, R, Hayter, M, Dasso, N, et al. Predicting needlestick and sharps injuries in nursing students: development of the SNNIP scale. Nurs Open. (2020) 7:1578–87. doi: 10.1002/nop2.540
14. Yeshitila, M, Mengistie, B, Demessie, A, and Godana, W. Prevalence and associated factors of needle stick injury among nursing and midwifery students an Haramaya and Jigjiga university, eastern Ethiopia. Prim Health Care. (2015) 5:1–6. doi: 10.4172/2167-1079.1000186
15. Handiyani, H, Kurniawidjaja, LM, Irawaty, D, and Damayanti, R. The effective needle stick injury prevention strategies for nursing students in the clinical settings: a literature review. Enferm Clin. (2018) 28:167–71. doi: 10.1016/S1130-8621(18)30060-3
16. Von, P. Prevalence of needle stick injuries among dental, nursing and midwifery students in shiraz, Iran. GMS Hyg. Infect. Control. (2012) 7:7–12. doi: 10.3205/dgkh000189
17. Cheung, K, Ho, SC, Ching, SS, and Chang, KK. Analysis of needlestick injuries among nursing students in Hong Kong. Accid Anal Prev. (2010) 42:1744–50. doi: 10.1016/j.aap.2010.04.015
18. Hambridge, K, Nichols, A, and Endacott, R. The impact of sharps injuries on student nurses: a systematic review. Br J Nurs. (2016) 25:1064–71. doi: 10.12968/bjon.2016.25.19.1064
19. Green, B, and Griffiths, EC. Psychiatric consequences of needlestick injury. Occup Med. (2013) 63:183–8. doi: 10.1093/occmed/kqt006
20. National Institute for Occupational Safety and Health. Needlestick Injuries are Preventable. Available at: https://www.cdc.gov/niosh/newsroom/feature/needlestick_disposal.html#:~:text=Avoiding%20recapping%20needles,receive%20appropriate%20follow%2Dup%20care. (Accessed February 1, 2021).
21. Benn, P, Fisher, M, and Kulasegaram, R. UK guideline for the use of post-exposure prophylaxis for HIV following sexual exposure. Int J STD AIDS. (2011) 22:695–708. doi: 10.1258/ijsa.2011.171011
22. al-Rawajfah, OM, al-Mugeed, KA, Alaloul, F, al-Rajaibi, HM, and al Omari, O. COVID-19 knowledge, attitude, and precautionary practices among health professional students in Oman. Nurse Educ Pract. (2021) 52:103041. doi: 10.1016/j.nepr.2021.103041
23. Al-Mugheed, K, Al Rawajfah, O, Bani-Issa, W, and Rababa, M. Acceptance, attitudes, and barriers of vaccine booster dose among nursing students: a multicounty survey. J Nurs Manag. (2022) 30:3360–7. doi: 10.1111/jonm.13791
24. Zhang, X, Chen, Y, Li, Y, Hu, J, Zhang, C, Li, Z, et al. Needlestick and sharps injuries among nursing students in Nanjing, China. AAOHN J. (2018) 66:276–84. doi: 10.1177/2165079917732799
25. Al-Mugheed, K, and Bayraktar, N. Patient safety attitudes among critical care nurses: a case study in North Cyprus. Int J Health Plann Manag. (2020) 35:910–21. doi: 10.1002/hpm.2976
26. al-Mugheed, K, Bayraktar, N, al-Bsheish, M, AlSyouf, A, Jarrar, M, AlBaker, W, et al. Patient safety attitudes among doctors and nurses: associations with workload, adverse events, experience. Healthcare. (2022) 10:631. doi: 10.3390/healthcare10040631
27. Akgur, M, and Dal, U. The prevalence of needle stick and sharps injuries in nurses in North Cyprus. Pak J Med Sci. (2012) 28:437–40.
28. Al-Dabbas, M, and Abu-Rmeileh, E. Needle stick injury among interns and medical students in the occupied Palestinian territory. East Mediterr Health J. (2012) 18:700–6. doi: 10.26719/2012.18.7.700
29. Prasuna, J, Sharma, R, Bhatt, A, Arazoo, PD, Butola, H, and Yadav, A. Occurrence and knowledge about needle stick injury in nursing students. J Ayub Med Coll Abbottabad. (2015) 27:430–3.
30. al-Mugheed, K, Bayraktar, N, al-Bsheish, M, AlSyouf, A, Aldhmadi, BK, Jarrar, M’t, et al. Effectiveness of game-based virtual reality phone application and online education on knowledge, attitude and compliance of standard precautions among nursing students. PLoS One. (2022) 17:e0275130. doi: 10.1371/journal.pone.0275130
31. Wang, D, Anuwatnonthakate, A, and Nilvarangkul, K. Knowledge attitude and practice regarding prevention of needle stick injuries among nursing students in Henan province, China. J Pak Med Assoc (1951). (2021) 71:2420–2. doi: 10.47391/JPMA.03-4294
32. Rababa, M, Bani-Hamad, D, Hayajneh, AA, and Al, MK. Nurses’ knowledge, attitudes, practice, and decision-making skills related to sepsis assessment and management. Electron J Gen Med. (2022) 19:em420. doi: 10.29333/ejgm/12556
33. Siddique, K, Mirza, S, Tauqir, SF, Anwar, I, and Malik, AZ. Knowledge attitude and practices regarding needle stick injuries amongst healthcare providers. Pak J Surg. (2008) 24:243–8.
34. Kwanzaa, CS, Clarke, K, Ramlal, C, Singh, R, and Ocho, ON. Factors contributing to needle stick injuries among new registered nurses at a hospital in Trinidad. Infect Dis Health. (2020) 25:294–301. doi: 10.1016/j.idh.2020.06.003
35. Alkhazali, MN, Bayraktar, N, and Al-Mugheed, KA. Knowledge and barriers of critical care nurses regarding evidencebased practices in ventilator-associated pneumonia prevention. Cyprus J Med Sci. (2021) 6:185–91. doi: 10.5152/cjms.2021.1292
36. Lauer, AC, Reddemann, A, Meier-Wronski, CP, Bias, H, Gödecke, K, Arendt, M, et al. Needlestick and sharps injuries among medical undergraduate students. Am J Infect Control. (2014) 42:235–9. doi: 10.1016/j.ajic.2013.08.013
37. Yang, YH, Wu, T, Ho, K, Chuang, Y, Chen, L, Yang, CY, et al. Needlestick/sharps injuries among vocational school nursing students in southern Taiwan. Am J Infect Control. (2004) 32:431–5. doi: 10.1016/j.ajic.2004.02.007
38. Xu, X, Yin, Y, Wang, H, and Wang, F. Prevalence of needle-stick injury among nursing students: a systematic review and meta-analysis. Front Public Health. (2022) 10:937887. doi: 10.3389/fpubh.2022.937887
39. Rn, C, Siu, S, Ching, Y, Ka, K, and Chang, P. American journal of infection control prevalence of and risk factors for needle stick and sharps injuries among nursing students in Hong Kong. Am J Infect Control. (2012) 40:997–1001. doi: 10.1016/j.ajic.2012.01.023
40. Yamazhan, T, Durusoy, R, Tasbakan, M, Tokem, Y, Pullukcu, H, Sipahi, O, et al. Nursing students' immunisation status and knowledge about viral hepatitis in Turkey: a multi-Centre cross-sectional study. Int Nurs Rev. (2011) 58:181–5. doi: 10.1111/j.1466-7657.2010.00869.x
41. Hambridge, K. Needlestick and sharps injuries in the nursing student population. Nurs Standard. (2011) 25:38–45. doi: 10.7748/ns2011.03.25.27.38.c8389
42. Talas, MS. Occupational exposure to blood and body fluids among Turkish nursing students during clinical practice training: frequency of needlestick/sharp injuries and hepatitis B immunization. J Clin Nurs. (2009) 18:1394–403. doi: 10.1111/j.13652702.2008.02523.x
43. Yao, X, Yang, B, Yao, C, Bai, S, Qian, R, Huang, H, et al. Needlestick injuries among nursing students in China. Nurse Educ Today. (2010) 30:435–7. doi: 10.1016/j.nedt.2009.09.018
44. Alsyouf, A, Abdalwali, L, Alsubahi, N, and Alhazmi, FN. The use of a technology acceptance model (TAM) to predict patients’ usage of a personal health record system: the role of security, privacy, and usability. Environ Res Public Health. (2023) 20:1347. doi: 10.3390/ijerph20021347
Keywords: needle stick injury, nursing students, incidence, knowledge, attitude, practice
Citation: Al-Mugheed K, Farghaly SM, Baghdadi NA, Oweidat I and Alzoubi MM (2023) Incidence, knowledge, attitude and practice toward needle stick injury among nursing students in Saudi Arabia. Front. Public Health. 11:1160680. doi: 10.3389/fpubh.2023.1160680
Edited by:
Louise A. Ellis, Macquarie University, AustraliaReviewed by:
Ayat Tawfik, Port Said University, EgyptMatteo Riccò, IRCCS Local Health Authority of Reggio Emilia, Italy
Copyright © 2023 Al-Mugheed, Farghaly, Baghdadi, Oweidat and Alzoubi. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Khalid Al-Mugheed, a2hhbGlkLmVkdUB5YWhvby5jb20=
 Khalid Al-Mugheed
Khalid Al-Mugheed Sally Mohammed Farghaly
Sally Mohammed Farghaly Nadiah A. Baghdadi2
Nadiah A. Baghdadi2 Islam Oweidat
Islam Oweidat