- Universidad Cesar Vallejo, Trujillo, Peru
Introduction: The study of general well-being in older adulthood is of vital importance due to the negative repercussions of aging on daily life. Therefore, the objective of this research was to analyze the psychometric properties of the WHO-5 well-being index in a sample of participants from hospitals and older care centers in Peru.
Method: A total of 661 older adults from Metropolitan Lima participated in the study (65% women and 35% men), aged between 60 and 93 years. They concurrently completed the WHO-5 well-being index and the Family APGAR.
Results: The findings demonstrated adequate fit indices for the original five-item model: χ2/df = 3.73, CFI = 0.998, TLI = 0.995, SRMR = 0.03, and RMSEA = 0.06. Factor loadings were above 0.50. Convergent validity, assessed through Pearson’s correlation coefficient, was significant and direct (r = 0.35). Internal consistency indices (α = 0.84; ω = 0.84) were satisfactory. The unidimensional structure of the instrument was confirmed, as well as its measurement invariance across sexes.
Discussion and conclusions: The WHO-5 well-being index, when applied to older adults in Peru, confirms its unidimensional structure, demonstrates evidence of validity and reliability, and is an equivalent measure across sexes. This suggests its utility as a brief, reliable instrument for evaluating well-being in this population.
Introduction
Study context
Research on subjective well-being in older adults has shown that social and emotional factors play a central role in healthy aging. In Europe, loneliness and social isolation are associated with sustained declines in well-being (1, 108, 112, 114), whereas community-based programs and positive psychology interventions exhibit significant protective effects (2). In Latin America, studies in Chile highlight the close relationship between self-perceived health, functional capacity, and social support with higher levels of well-being (3, 113), and in Mexico, non-contributory pensions have been documented to produce significant improvements in the perception of well-being in old age (4). Similarly, comparisons between Costa Rica and Spain have underscored the influence of cultural factors in shaping successful aging (5). In the Peruvian case, the recent adaptation of the WHO-5 into Quechua represents an important intercultural advancement (6); however, psychometric studies supporting its use among Spanish-speaking older adults are still lacking, revealing an empirical gap and providing justification for the present study.
Recent research confirms that the quality of life of older adults depends on institutional and community factors (110), with significant differences observed across European countries such as Poland, Germany, and Austria (7). In Lithuania, the need for specific policies to improve quality of life has been documented (8), while in Spain, differences in residence area (urban vs. rural) generate variations in health, lifestyle, and well-being (9). Internationally, social and community support are determinants of subjective well-being (10, 109). Community dining programs and participation in social activities reinforce belongingness and life satisfaction (11). Psychological resilience, promoted through body–mind exercise programs, has also been identified as a key protective mechanism (12, 116).
Concepts and indicators of well-being
The concept of well-being has evolved from a definition centered on the absence of disease to a holistic approach integrating biological, social, mental, environmental, and economic aspects (13). Traditionally, objective indicators such as income level, life expectancy, and literacy have been used (14). However, subjective measures have also been employed, such as perceived quality of life, levels of anxiety and depression, life satisfaction, and happiness (15–20, 107).
Recent studies emphasize the importance of contextual and material factors for older adults’ well-being. In Greece, physical activity has been associated with better quality of life (21), while in the European Union, living conditions significantly affect well-being (22). Public health research shows that subjective well-being can be understood as a multidimensional construct influenced by health literacy and territorial context (23). At the individual level, anxiety and depression predict negative trajectories of well-being (24), and loneliness exacerbates the effects of ageism in widowed populations (25). Conversely, older adults demonstrate resilience and emotional stability in the face of adversity (26), and positive attitudes toward aging are linked to greater overall well-being (27).
WHO-5 as a measure of well-being
The WHO-5 well-being index, developed by the WHO, consists of five items that assess subjective well-being globally and simply. It is recommended as a depression screening tool in primary care (28–30).
The content of the WHO-5 is directly linked to the hedonic-oriented model of subjective well-being, as it focuses on the frequency of positive affective experiences. The first item, referring to feeling cheerful and in good spirits, reflects the central component of positive affect described by Diener (31) and Watson, Clark, and Tellegen (32). The second item, concerning feeling calm and relaxed, assesses the experience of emotional tranquility and the absence of distress, in line with the concept of positive health proposed by the WHO (33) and the clinical interpretation of Bech et al. (34). The third item, related to energy and vitality, connects with self-determination theory, which considers vitality a central indicator of well-being (35). The fourth item, associated with waking up feeling rested, integrates a somatic component of subjective well-being linked to healthy functioning and physiological recovery (36). Finally, the fifth item, which explores interest in daily life, alludes to motivation and life purpose, dimensions that combine the hedonic perspective with life satisfaction as described in broader models of well-being (37, 117). Taken together, these items enable a stepped assessment that ranges from basic emotional experience to life engagement, providing evidence of coherence with contemporary models of psychological well-being.
Multiple studies have confirmed its psychometric validity across countries and contexts, showing internal consistency and good fit to the unidimensional model (19, 29, 38–48, 111). Likewise, it has proven useful in detecting depression in various medical conditions (28, 49–58) and in different age groups (30, 59–65).
Research gap and study objective
The WHO-5, brief and easy to administer, has demonstrated validity among Spanish-speaking older adults and has been adapted into Quechua in Peru, enabling its use in both urban and rural contexts. Its unidimensional structure and regional invariance support comparisons across socioeconomic levels, and its utility as a screening tool for depression underpins its application in both community and clinical settings (6, 65–68). However, despite this international and regional evidence, no studies have specifically examined the psychometric properties of the WHO-5 among Spanish-speaking older adults in Peru. This gap limits the availability of a brief, reliable, and culturally relevant instrument to assess well-being in a highly vulnerable group. Consequently, the present study aims to analyze the psychometric evidence of the WHO-5 well-being index in a Peruvian sample of Spanish-speaking older adults, with the purpose of contributing to early detection and supporting strategies for mental health care and well-being.
Method
Participants
The sample consisted of 661 older adults, with 64.9% women and 35.1% men, aged between 60 and 93 years (M = 70.09; SD = 7.33). Regarding marital status, 46.4% were married, 10.6% cohabiting, 22.1% widowed, 13.4% separated or divorced, and 7.4% single. Household composition was as follows: 12.1% lived alone, 12.9% with a partner, 26.2% with children, 33% with partner and children, and 15.9% with other relatives. Educational levels were diverse: 7.6% did not complete primary school, 13.2% completed primary school, 3% incomplete secondary, 26.5% completed secondary, 2.3% incomplete technical studies, 11.5% completed technical studies, 12% incomplete university studies, 20.3% completed university studies, and 3.8% had postgraduate education. Additionally, 51.7% attended Older Adults Care Centers (CAM), while 48.3% did not.
Inclusion criteria were: being aged 60 years or older, residing in the community or attending older adults care centers, having the capacity to autonomously respond to questionnaires, and providing written or digital informed consent. Exclusion criteria were severe cognitive impairment or confirmed dementia diagnosis, as well as acute medical conditions that limited participation, ensuring stable health at the time of evaluation.
Recruitment was conducted through direct invitations at hospitals, older adults care centers (CAM), and community spaces, complemented by virtual dissemination through institutional support networks.
A non-probabilistic convenience sampling method was used, ensuring voluntariness and anonymity after informed consent. Only participants who fully completed the evaluation protocol were included in the analysis. The sample size (n = 661) was deemed adequate for robust psychometric analysis, considering that categorical data precision improves with ≥300 cases, particularly with ordinal scales, classified as ‘very good’ according to Bandalos (69). Although there is no consensus on the ideal sample size for psychometric studies, Arafat et al. (70) recommend at least 500 participants for validation, while Newsom (71) suggests >400 when using MLR estimation and >500 for DWLS or WLSMV estimators. Therefore, the sample size in this study was appropriate.
Instruments
Sociodemographic questionnaire: collected information on age, sex, marital status, household composition, educational level, and participation in older adults permission to use the instrument was obtained care centers. These indicators contextualized well-being factors, given the influence of sociodemographic variables on quality of life and mental health in older adults (27, 72, 73).
WHO-5 well-being index: a self-report instrument developed by the WHO (33) to assess depressive symptoms through five items related to energy, interest, and mood, using a 4-point ordinal scale (0 = never, 1 = sometimes, 2 = often, 3 = always) (74). This study used the Spanish version validated by Simancas-Pallares et al. (75), which reported internal reliability of ω = 0.877 and α = 0.852, with a factorial structure explaining 56.17% of total variance, demonstrating adequate functioning.
Family APGAR: developed by Smilkstein in 1978, this instrument assesses family functioning through five items related to participation, resource gradient, adaptation, affection, and problem-solving capacity, with a 5-point Likert-type scale (0 = never, 1 = hardly ever, 2 = sometimes, 3 = almost always, 4 = always) (76).
Procedure
The study followed an instrumental design aimed at analyzing the psychometric properties of the WHO-5 in older adults. Permission to use the instrument was obtained from the authors. Data were collected using two modalities: (a) a face-to-face protocol including informed consent, sociodemographic questionnaire, and instruments, and (b) a virtual form. In the online modality, participants were presented with the study’s objective, the voluntary and anonymous nature of participation, and the informed consent form, with only those providing affirmative consent proceeding to the evaluation protocol.
Data collection spanned 6 months. Protocols not meeting inclusion criteria were excluded. Data were systematized in Excel and exported to Jamovi and RStudio for analysis. The study was funded by the Faculty Research Fund of Universidad César Vallejo (Resolution RVI No. P-2024-017 -VI-UCV, July 31, 2024) and approved by the university’s ethics committee (PID No. 003–2024, April 10, 2024).
Data analysis
The study conducts a psychometric analysis, which is essential to ensure that an instrument measures the intended construct with validity and reliability. This process allows for the verification of internal structure, consistency, and comparability by sex, thereby preventing interpretative bias. In specific populations such as older adults, this type of evidence is critical to guarantee clinical relevance and practical utility (77).
Statistical analyses were conducted with RStudio (version 4.1.2) and Jamovi (version 2.3.2.6). A polychoric correlation matrix was calculated, suitable for ordinal items, following recommendations by Gadermann et al. (78), Jöreskog (79), and Viladrich et al. (80). Item analysis criteria included corrected item-total correlations (IHC) > 0.30 (81), and skewness and kurtosis values between ±1.50 (82). Significant correlations with an external criterion were also examined.
Internal structure validity was evaluated through confirmatory factor analysis (CFA) using the robust WLSMV estimator, recommended for ordinal data. Model fit indices were assessed with RMSEA ≤ 0.08, CFI ≥ 0.95, TLI ≥ 0.90, and χ2/df, following Escobedo et al. (83). Convergent validity required significant correlations (p < 0.01) with external variables. Factorial invariance was examined using ΔCFI > 0.010 and ΔRMSEA < 0.015 cutoffs (84). Reliability was assessed with McDonald’s omega (85), with acceptable values between 0.70 and 0.90 (86), though values above 0.65 may be accepted in specific cases (87).
Results
This section presents the psychometric analysis results of the WHO-5 well-being index applied to Peruvian older adults. Findings include polychoric correlations, item analysis, confirmatory factor analysis, factorial invariance by sex, validity with family functioning, reliability indices, and reference percentiles. These outcomes demonstrate the instrument’s internal consistency, validity, and applicability within the studied population.
Polychoric correlation matrix
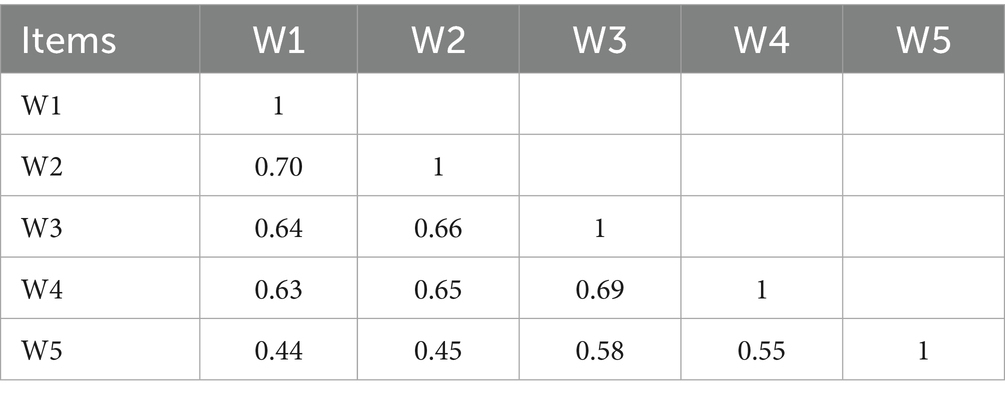
Table 1 presents the polychoric correlations obtained among the five items of the WHO-5 well-being index. Polychoric correlations are appropriate for evaluating the relationship between ordinal categorical variables, as is the case with Likert-scale items. The correlations ranged from 0.44 (W1 and W5) to 0.70 (W1 and W2), indicating moderate to high levels of association among the items. These values show that there is no problem of collinearity, meaning that redundancy between items is not present (88). This pattern suggests that the items are interrelated, reflecting a possible unidimensional structure of the evaluated construct. These findings support the internal consistency of the instrument and suggest that the items measure related aspects of the same construct.
Item analysis of the WHO-5 in Peruvian older adults
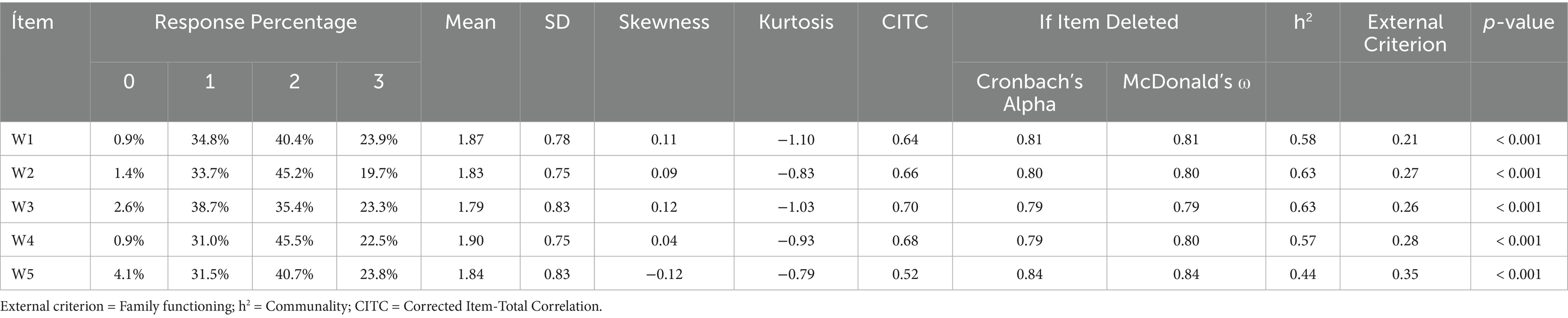
Table 2 presents a detailed analysis of the five items of the WHO-5 well-being index, evaluating their psychometric characteristics. Response percentages for each Likert-scale category are reported, along with descriptive measures such as mean, standard deviation (SD), skewness, and kurtosis. None of the response percentages exceeded 80%, indicating the absence of bias. Regarding response frequencies, all were above 10, which is optimal since frequencies below this threshold would suggest insufficient response effort (89). The means ranged from 1.79 (W3) to 1.90 (W4), with standard deviations between 0.75 and 0.83, reflecting adequate variability in responses. Skewness and kurtosis indices indicated that the item distributions approximated normality, although with a slight negative skew and leptokurtic tendency (90).
In terms of psychometric quality, the corrected item-total correlation (CITC), communality (h2), and the impact of deleting each item on the internal consistency of the instrument were evaluated. CITC values ranged from 0.52 (W5) to 0.70 (W3), indicating that most items adequately contribute to the overall construct (84, 91). Communalities were all above 0.30, indicating shared variance among items (92). The deletion of any item did not significantly affect internal consistency coefficients (Cronbach’s α and McDonald’s ω), which remained high across all cases, evidencing the reliability of the instrument (80, 93). Finally, correlations with the external criterion (Family functioning) were examined, showing significant associations (p < 0.001) for all items, supporting the criterion validity of the WHO-5.
Validity evidence based on the internal structure of the WHO-5 in Peruvian older adults
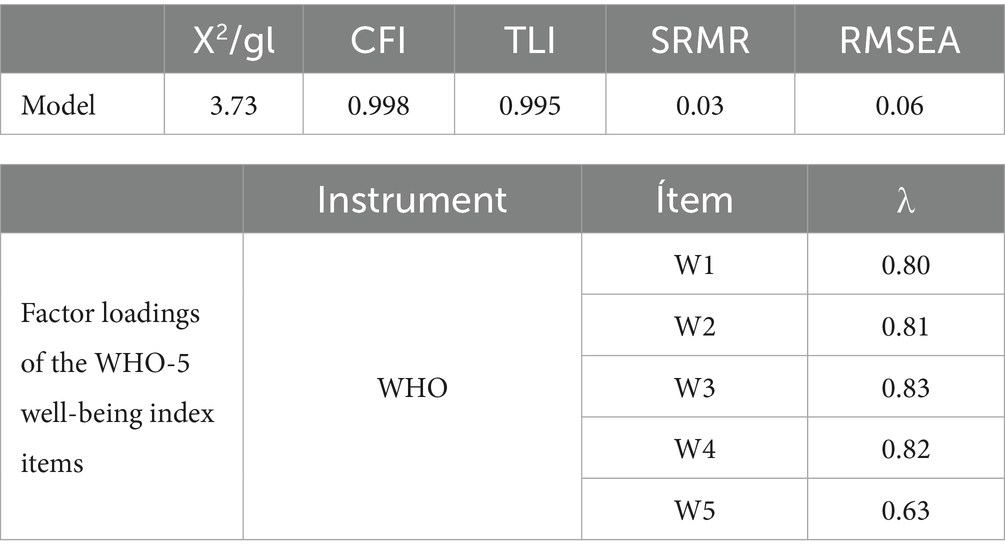
Table 3 shows the results of the confirmatory factor analysis (CFA) of the WHO-5 well-being index, using the WLSMV estimator, which is appropriate for ordinal data. The global fit indices indicate an excellent fit of the proposed unidimensional model. The chi-square statistic divided by degrees of freedom (χ2/df = 3.73) is acceptable and consistent with reasonable fit. The Comparative Fit Index (CFI = 0.998) and Tucker–Lewis Index (TLI = 0.995) are above the 0.95 threshold, providing evidence of very good model fit. The error indices, both SRMR (0.03) and RMSEA (0.06), are also within the recommended values (< 0.08 and < 0.06, respectively), suggesting a low level of discrepancy between the model and the data (83, 94, 95).
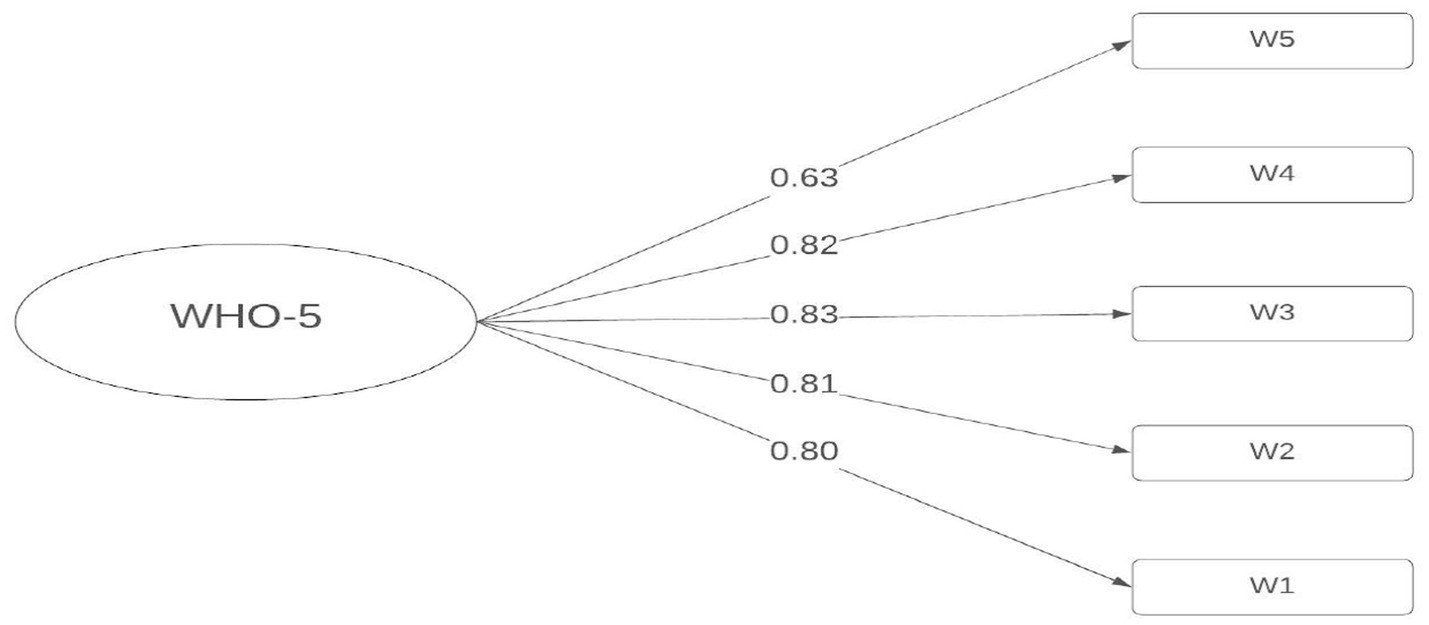
Regarding the factor loadings (λ), these reflect the contribution of each item to the overall construct of general well-being. All factor loadings are statistically significant and above the recommended threshold of 0.40, ranging from 0.63 (W5) to 0.83 (W3). This indicates that all items are adequate indicators of the latent construct, although item W5 shows a relatively lower loading, suggesting lower saturation compared to the other items. These results support the unidimensional structure of the WHO-5 and confirm the factorial validity of the instrument in the analyzed sample. This analysis provides strong evidence for its use in measuring general well-being (Figure 1).
Factorial invariance of the WHO-5 by sex in Peruvian older adults
Table 4 presents the results of the factorial invariance analysis of the WHO-5 well-being index conducted by sex. This analysis evaluates whether the underlying factorial model is equivalent across groups, allowing valid comparisons of scores between them. Five levels of invariance were analyzed: configural, metric, scalar, partial scalar (strict), and structural. The configural model, which assesses equivalence in the factorial structure, showed good fit (CFI = 0.987; RMSEA = 0.123), indicating that the structure of the model is consistent across groups. In the metric model, where equality of factor loadings is assumed, a chi-square change was observed (Δχ2 = 5.747, p < 0.001), with minimal changes in fit indices (ΔCFI = 0.001; ΔRMSEA = 0.018). This suggests that the relationships between items and the latent construct are similar across sexes.
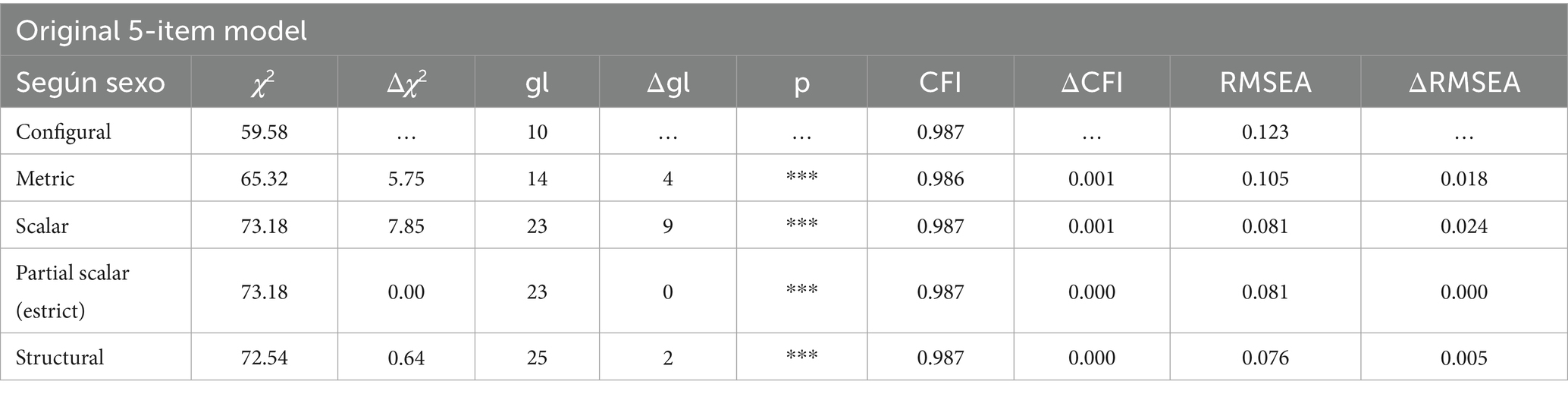
Table 4. Fit indices of the factorial invariance analysis of the WHO-5 well-being index (original 5-item model) by sex.
In the scalar model, which assumes equality of both factor loadings and intercepts, the changes in indices were also minimal (ΔCFI = 0.001; ΔRMSEA = 0.024), supporting the comparability of scores between sexes. The partial scalar (strict) model added equality in residual variances, without changes in fit (ΔCFI = 0.000; ΔRMSEA = 0.000). Finally, the structural model, which evaluates equality in the variance of the latent construct, maintained adequate fit (CFI = 0.987; RMSEA = 0.076; ΔCFI = 0.000). Taken together, these results support the factorial invariance of the WHO-5 by sex, allowing valid comparisons of general well-being scores across groups (84, 91, 96).
Validity evidence of the WHO-5 in relation to other variables among Peruvian older adults
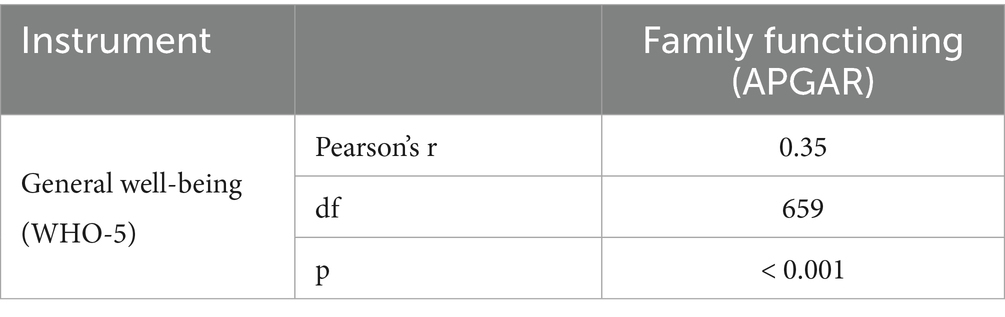
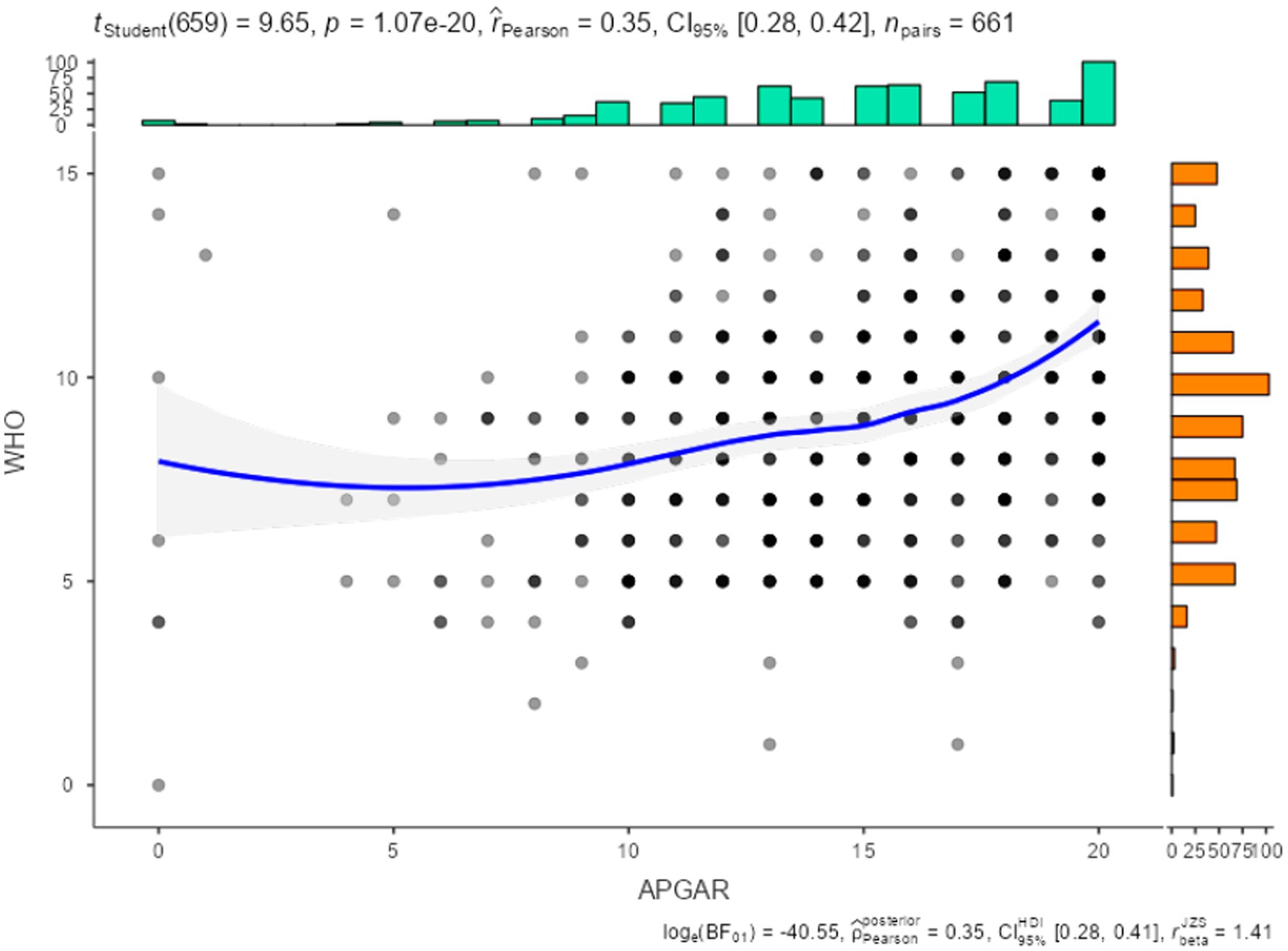
Table 5 and Figure 2 show the correlation between the Family Functioning scale (APGAR) and the WHO-5 well-being index, revealing a statistically significant and positive correlation (r = 0.35). This provides evidence of convergence between the constructs measured by the two instruments.
Figure 3 shows a path analysis conducted to evaluate the predictive capacity between two variables: family functioning (measured with the APGAR scale) and general well-being (measured with the WHO-5). In both directions (from APGAR to WHO-5 and from WHO-5 to APGAR), a path coefficient of 0.35 was observed, p < 0.001, R2 = 0.124 (12%). This indicates a moderate, positive, and bidirectional association between the two variables. These results suggest that family functioning influences general well-being and vice versa, to a similar extent. At the same time, this may indicate that the two variables are highly interrelated reciprocally, although it does not necessarily imply bidirectional causality.

Figure 3. Path analysis evaluating the predictive capacity of both variables on each other. Funcionalidad familiar (APGAR); Bienestar general (WHO-5).
Reliability of the WHO-5 in Peruvian older adults
Table 6 presents the reliability indices of the WHO-5 well-being index. Cronbach’s alpha, with a value of 0.84, indicates a high level of internal consistency, reflecting strong interrelations among the items and a consistent measurement of the general well-being construct. Similarly, McDonald’s omega, also with a value of 0.84, demonstrates a high level of reliability, confirming the robustness of the instrument in measuring this construct. In all cases, the values exceed 0.70, which is considered acceptable (97–99).
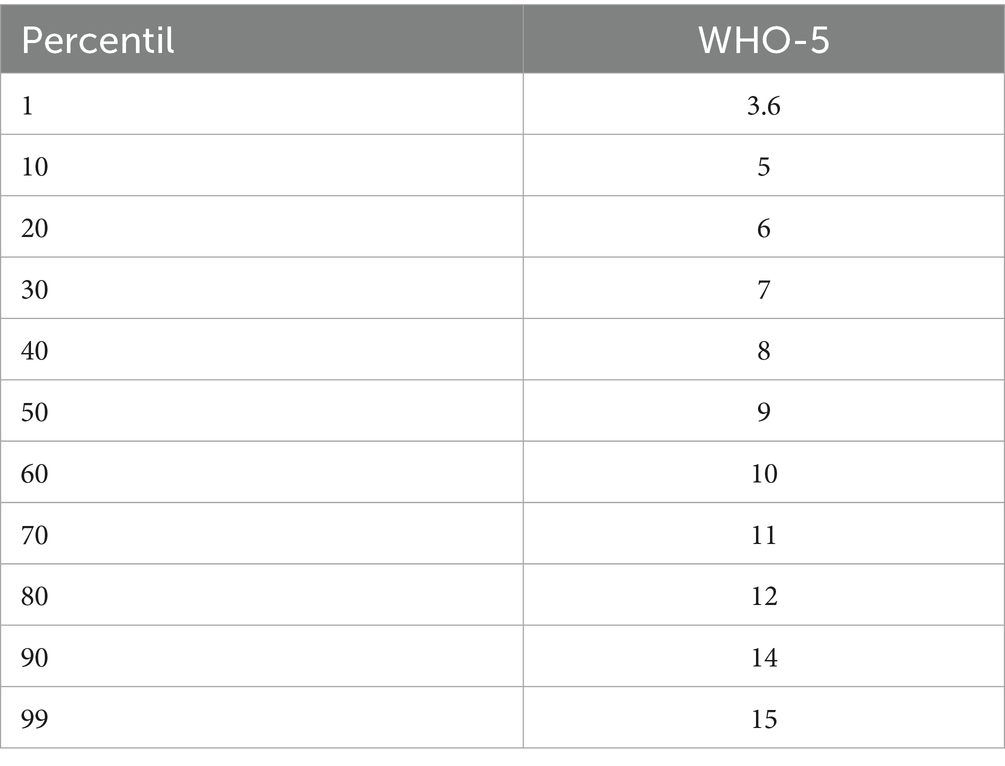
The table presents the general percentiles corresponding to the scores of the WHO-5 well-being index. Percentiles allow for the interpretation of the score distribution in the sample, facilitating the relative comparison of individual values with the rest of the evaluated population. These data help situate individuals within the overall distribution of well-being in the population and are useful for classifying levels of well-being according to percentile ranges (Table 7).
Taken together, the results provide evidence that the WHO-5 demonstrates adequate levels of reliability and validity in the sample of Peruvian older adults. The factor analysis confirmed its unidimensional structure, factorial invariance ensured valid comparisons between sexes, and associations with family functioning supported its convergent validity. In addition, percentiles provide useful benchmarks for interpreting individual scores. These findings support the use of the WHO-5 as a brief and reliable instrument for assessing general well-being in this population.
Discussion
The results of this study demonstrate that the WHO-5 exhibits solid psychometric properties among Peruvian older adults, confirming its suitability as a brief measure of subjective well-being. Item analysis showed adequate dispersion, absence of extreme biases, and high homogeneity indices, supporting the quality of the items and their internal coherence (46, 80, 84, 90, 93). These findings are consistent with research underscoring the usefulness of the WHO-5 for reliably capturing states of well-being in diverse populations (63, 64).
Confirmatory factor analysis revealed an excellent fit for the unidimensional model, in line with the theoretical framework of the instrument and with international validations that highlight its cross-cultural validity (38, 40, 43, 47, 48). Furthermore, its consistency with studies that have demonstrated clinical utility across various conditions (28, 49, 50) reinforces its value for monitoring mental health and well-being in older adults.
Convergent validity, reflected in the significant correlations between the WHO-5 and family functioning, confirms the influence of the immediate social environment on older adults’ well-being (100, 101). These results align with research emphasizing the role of social support, community, and family networks as key determinants of quality of life in old age (7, 9, 102, 115).
Factorial invariance across sex supports the equivalence of the instrument and indicates that well-being differences are not explained by gender, but rather by contextual factors such as social, economic, and community resources, in accordance with international literature (17, 21, 22, 62, 103, 104). This reinforces the relevance of using the WHO-5 in comparative studies and in the development of public health policies on mental health targeting older adults in the Peruvian context.
In sum, this study not only provides evidence of the validity and reliability of the WHO-5 in a sample of Peruvian older adults, but also contributes to filling a gap in the regional literature, given that most prior studies have focused on general populations or linguistic adaptations without a specific emphasis on aging.
Theoretical and practical implications
The findings reinforce the conceptualization of subjective well-being as a unidimensional construct, shaped by family, social, and community factors. They also support the WHO framework on healthy aging (73), emphasizing that well-being is not solely the absence of disease but also involves social resources, resilience, and community participation (11, 12).
Practically, the WHO-5 proves to be a brief and effective tool for depression screening and well-being promotion in clinical, hospital, and community settings. It can guide preventive interventions, support early risk identification, and inform public health policies aimed at improving the quality of life in older adults.
Limitations and future directions
This study presents limitations. First, a non-probabilistic sample from Metropolitan Lima restricts the generalizability of the results. Second, older adults with specific clinical diagnoses such as depression, Alzheimer’s, Parkinson’s, or other neurodegenerative conditions were not included, limiting evidence on discriminant validity. Third, no clinical external criterion was applied, constraining conclusions about diagnostic accuracy.
Future studies should validate the WHO-5 in clinical and multi-regional populations, assess sensitivity with ROC curves, and explore longitudinal stability. Cross-cultural comparative research could further clarify contextual and cultural differences in the perception of well-being (7–9).
Finally, a content-focused approach and coherence of the construct under evaluation are recommended through qualitative strategies such as cognitive interviews, in-depth interviews, and focus groups. These techniques allow for the identification of ambiguities, the interpretation of how participants understand the items, and the provision of validity evidence based on content (105, 106). Furthermore, in accordance with the Standards for Educational and Psychological Testing (77), the incorporation of qualitative data supports the collection of validity evidence based on response processes by clarifying the correspondence between the theoretical intent of the item and the respondent’s interpretation. This approach not only strengthens the quality of the instrument but also ensures its cultural and contextual relevance across diverse populations, thereby optimizing the validity of inferences derived from its use.
Conclusion
In summary, the WHO-5 well-being index demonstrated strong validity, reliability, and measurement invariance in a sample of Peruvian older adults. The instrument confirmed its unidimensional structure, with adequate internal consistency and convergent validity with family functioning. These findings support its use as a culturally appropriate, brief, and reliable tool for assessing general well-being in older adults.
Data availability statement
The raw data supporting the conclusions of this article will be made available by the authors, without undue reservation.
Ethics statement
The studies involving humans were approved by Comité de ética de la Escuela de Psicología, Universidad César Vallejo. The studies were conducted in accordance with the local legislation and institutional requirements. The participants provided their written informed consent to participate in this study.
Author contributions
PPDG: Conceptualization, Data curation, Formal analysis, Funding acquisition, Investigation, Methodology, Project administration, Resources, Software, Supervision, Validation, Visualization, Writing – original draft, Writing – review & editing. FRQ: Conceptualization, Data curation, Formal analysis, Funding acquisition, Investigation, Methodology, Project administration, Resources, Software, Supervision, Validation, Visualization, Writing – original draft, Writing – review & editing. EA: Conceptualization, Data curation, Formal analysis, Funding acquisition, Investigation, Methodology, Project administration, Resources, Software, Supervision, Validation, Visualization, Writing – original draft, Writing – review & editing. NIY: Conceptualization, Data curation, Formal analysis, Funding acquisition, Investigation, Methodology, Project administration, Resources, Software, Supervision, Validation, Visualization, Writing – original draft, Writing – review & editing. MMC: Conceptualization, Data curation, Formal analysis, Funding acquisition, Investigation, Methodology, Project administration, Resources, Software, Supervision, Validation, Visualization, Writing – original draft, Writing – review & editing.
Funding
The author(s) declare that no financial support was received for the research and/or publication of this article.
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Generative AI statement
The authors declare that no Gen AI was used in the creation of this manuscript.
Any alternative text (alt text) provided alongside figures in this article has been generated by Frontiers with the support of artificial intelligence and reasonable efforts have been made to ensure accuracy, including review by the authors wherever possible. If you identify any issues, please contact us.
Publisher’s note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
References
1. Steptoe, A, Shankar, A, Demakakos, P, and Wardle, J. Social isolation, loneliness, and all-cause mortality in older men and women. Proc Natl Acad Sci U S A. (2015) 110:5797–801. doi: 10.1073/pnas.1219686110
2. Orsega-Smith, E, Goodwin, S, Ziegler, M, and Greenawalt, K. Aging and tha art of happiness: time effects os a positive psychology program with older adults. OMB Geriatr. (2019) 3:1029. doi: 10.21926/obm.geriatr.1901029
3. Sarmiento-Loayza, LS. Bienestar subjetivo, estado de salud, funcionalidad y participación social en personas mayores chilenas. Rev Med Chile. (2022) 150:1010–7. doi: 10.4067/S0034-98872022000801010
4. Aguila, E, Díaz, C, Manqing, F, Kapteyn, A, and Pierson, A. Living longer in Mexico: income security and health. J Aging Soc Policy. (2011) 31:57–74. Available online at: https://pmc.ncbi.nlm.nih.gov/articles/PMC4945250
5. Blanco-Molina, M, Pinazo-Hernandis, S, Montoro-Rodríguez, J, and Tomás, JM. Testing a proactive model of successful aging among older adults in Costa Rica and Spain. Int J Aging Hum Dev. (2021) 93:619–35. doi: 10.1177/0091415020974621
6. Carranza Esteban, RF, Mamani-Benito, O, Cjuno, J, Tito-Betancur, M, Lingán-Huamán, SK, and Arias-Chávez, D. Translation and validation of the WHO-5 general well-being index into native language Quechua of the Peruvian south. Heliyon. (2023) 9:e16843. doi: 10.1016/j.heliyon.2023.e16843
7. Swakowska, K, Olejniczak, D, and Staniszewska, A. Quality of life of residents in seniors’ homes in Poland and Germany. Healthcare. (2024) 12:829. doi: 10.3390/healthcare12080829
8. Iždonaitė-Medžiūnienė, I, and Preikšaitienė, L. Disposition of improving quality of life in older adults: the case of Lithuania. Aging Clin Exp Res. (2024) 36:26. doi: 10.1007/s40520-023-02687-2
9. Jiménez-Ten Hoevel, C, Queral, J, Besora-Moreno, M, Tarro, L, Besora-Moreno, M, Valls, RM, et al. Health status, lifestyle and quality of life in older adults of rural and urban areas of Tarragona province (Catalonia, Spain): a cross-sectional descriptive study. BMC Public Health. (2025) 25:895. doi: 10.1186/s12889-025-22045-3
10. Zhang, Y, and Sun, L. The health status, social support, and subjective well-being of older individuals: evidence from the Chinese general social survey. Front Public Health. (2024) 12:1312841. doi: 10.3389/fpubh.2024.1312841
11. Gao, D, Li, R, and Yang, Y. The impact of social activities on mental health among older adults in China. Front Public Health. (2024) 12:1422246. doi: 10.3389/fpubh.2024.1422246
12. Yang, Q, Zhang, Y, and Li, S. The impact of mind–body exercise on the quality of life in older adults: the chain mediation effect of perceived social support and psychological resilience. Front Public Health. (2024) 12:1446295. doi: 10.3389/fpubh.2024.1446295
13. World Health Organization. Mental health of older adults. (2023). Available online at: https://www.who.int/es/news-room/fact-sheets/detail/mental-health-of-older-adults
14. Manfredi, M, and Actis, E. Measurement of objective and subjective well-being: a proposal for a comprehensive human development index. Rev Econ Mundial. (2021) 57:161–86. doi: 10.33776/rem.v0i57.4648
16. Diener, E, Heintzelman, S, Kushlev, K, Tay, L, Wirtz, D, Lutes, L, et al. Findings all psychologists should know from the new science on subjective well-being. Can Psychol. (2017) 58:87–104. doi: 10.1037/cap0000063
17. Diener, E, Oishi, S, and Tay, L. Advances in subjective well-being research. Nat Hum Behav. (2018) 2:253–60. doi: 10.1038/s41562-018-0307-6
18. Kusier, AO, and Folker, AP. The well-being index WHO-5: hedonistic foundation and practical limitations. Med Humanit. (2020) 46:333–9. doi: 10.1136/medhum-2018-011636
19. Sischka, P, Costa, A, Steffgen, G, and Schmidt, A. WHO-5 well-being index: validation based on item response theory and measurement invariance analysis in 35 countries. J Affect Disord Rep. (2020) 1:100020. doi: 10.1016/j.jadr.2020.100020
20. Solanes, A, Albajes-Eizagirre, A, Fullana, MA, Fortea, L, Fusar-Poli, P, Torrent, C, et al. Can we increase the subjective well-being of the general population? An umbrella review of the evidence. Rev Psiquiatr Salud Ment. (2021) 14:50–64. doi: 10.1016/j.rpsm.2020.08.002
21. Psarrou, A, Adamakidou, T, Apostolara, P, Koreli, A, Drakopoulou, M, Plakas, S, et al. Associations between physical activity and health-related quality of life among community-dwelling older adults: a cross-sectional study in urban Greece. Geriatrics. (2023) 8:61. doi: 10.3390/geriatrics8030061
22. Bieszk-Stolorz, B, and Dmytrów, K. The well-being-related living conditions of elderly people in the European union—selected aspects. Sustainability. (2023) 15:16823. doi: 10.3390/su152416823
23. Chen, Y, Cai, T, and Tian, R. Investigation into the subjective well-being of older adults via confirmatory factor analysis and analytic hierarchy process—an empirical analysis based on CGSS2021 data. Front Public Health. (2025) 13:1585408. doi: 10.3389/fpubh.2025.1585408
24. Wang, X, Ke, Q, Leng, P, Liu, D, and Zeng, W. Association between subjective well-being trajectories and anxiety/depression: findings from a nationally representative cohort study. Front Psychol. (2025) 16:1573260. doi: 10.3389/fpsyg.2025.1573260
25. Shen, H, Pan, G, Zhang, M, He, X, Yao, M, and Yang, Y. The relationship between ageism, loneliness, and anxiety in widowed older adults: cognitive function as a moderator in the mediated model. Front Psychol. (2025) 16:1624197. doi: 10.3389/fpsyg.2025.1624197
26. Hsieh, S, Chang, Y, Yao, Z, Yang, M, and Yang, C. The effect of age and resilience on the dose–response function between the number of adversity factors and subjective well-being. Front Psychol. (2024) 15:1332124. doi: 10.3389/fpsyg.2024.1332124
27. Instituto Nacional de Estadística e Informática [INEI]. Situation of the Peruvian population 2024: a view of ethnic diversity. (2024). Available online at: https://cdn.www.gob.pe/uploads/document/file/6616587/5751291-situacion-de-la-poblacion-peruana-2024-una-mirada-de-la-diversidad-etnica.pdf?v=1720728622
28. Cichón, E, Kiejna, A, Kokoszka, A, Rajba, B, Lloyd, C, and Sartorius, N. Validation of the polish version of WHO-5 as a screening instrument for depression in adults with diabetes. Diabetes Res Clin Pract. (2019) 159:107970. doi: 10.1016/j.diabres.2019.107970
29. Guðmundsdottir, H, Olason, D, Guðmundsdottir, D, and Sigurðsson, J. A psychometric evaluation of the Icelandic version of the WHO-5. Scand J Psychol. (2014) 55:567–72. doi: 10.1111/sjop.12156
30. Low, K, Pheh, K, and Tan, C. Validation of the WHO-5 as a screening tool for depression among young adults in Malaysia. Curr Psychol. (2023) 42:7841–4. doi: 10.1007/s12144-021-02152-1
31. Diener, E. Subjective well-being. Psychol Bull. (1984) 95:542–75. doi: 10.1037/0033-2909.95.3.542
32. Watson, D, Clark, LA, and Tellegen, A. Development and validation of brief measures of positive and negative affect: the PANAS scales. J Pers Soc Psychol. (1988) 54:1063–70. doi: 10.1037/0022-3514.54.6.1063
33. World Health Organization. Wellbeing measures in primary health care/the DepCare project: Report on a WHO meeting: Stockholm, Sweden, 12–13 February 1998. Geneva: World Health Organization, Regional Office for Europe (1998).
34. Bech, P, Gudex, C, and Johansen, K. The WHO (ten) well-being index: validation in diabetes. Psychother Psychosom. (1996) 65:183–90. doi: 10.1159/000289073
35. Ryan, RM, and Deci, EL. On happiness and human potentials: a review of research on hedonic and eudaimonic well-being. Annu Rev Psychol. (2001) 52:141–66. doi: 10.1146/annurev.psych.52.1.141
36. Steptoe, A, O’Donnell, K, Marmot, M, and Wardle, J. Positive affect, psychological well-being, and good sleep. J Psychosom Res. (2008) 64:409–15. doi: 10.1016/j.jpsychores.2007.11.008
37. Diener, E, Wirtz, D, Tov, W, Kim-Prieto, C, Choi, DW, Oishi, S, et al. New well-being measures: short scales to assess flourishing and positive and negative feelings. Soc Indic Res. (2010) 97:143–56. doi: 10.1007/s11205-009-9493-y
38. Bech, P, Fitzgerald, S, and Engelbrecht, M. Patient reported outcome measures (PROMs): examination of the psychometric properties of two measures for burden of symptoms and quality of life in patients with depression or anxiety. Nord J Psychiatry. (2018) 72:251–8. doi: 10.1080/08039488.2018.1451918
39. Cosma, A, Költő, A, Chzhen, Y, Kleszczewska, D, Kalman, M, and Martin, G. Measurement invariance of the WHO-5 well-being index: evidence from 15 European countries. Int J Environ Res Public Health. (2022) 19:9798. doi: 10.3390/ijerph19169798
40. Dadfar, M, Momeni, N, Asgharnejad, A, Shirzy, N, and Abarghouie, G. Reliability, validity, and factorial structure of the World Health Organization-5 well-being index (WHO-5) in Iranian psychiatric outpatients. Trends Psychiatry Psychother. (2018) 40:79–84. doi: 10.1590/2237-6089-2017-0044
41. Fung, S, Kong, C, Liu, Y, Huang, Q, Xiong, Z, Jiang, Z, et al. Validity and psychometric evaluation of the Chinese version of the 5-item WHO well-being index. Front Public Health. (2022) 10:436. doi: 10.3389/fpubh.2022.872436
42. Kassab, A. Development and validation of an Arabic version of the World Health Organization well-being index (WHO-5). Rev Psicopatol Eval Comport. (2023) 45:247–55. Available online at: https://mijn.bsl.nl/development-and-validation-of-an-arabic-version-of-the-world-hea/23981754
43. Lara-Cabrera, M, Bjørkly, S, De Las Cuevas, C, Pedersen, S, and Mundal, I. Psychometric properties of the five-item World Health Organization well-being index used in mental health services: protocol for a systematic review. J Adv Nurs. (2020) 76:2426–33. doi: 10.1111/jan.14445
44. Löve, J, Andersson, L, Moore, C, and Hensing, G. Psychometric analysis of the Swedish translation of the WHO well-being index. Qual Life Res. (2014) 23:293–7. doi: 10.1007/s11136-013-0447-0
45. De Morelatto Souza, C, and Loayza, M. World health organization 5-item well-being index: validation of the Brazilian Portuguese version. Eur Arch Psychiatry Clin Neurosci. (2012) 262:239–44. doi: 10.1007/s00406-011-0255-x
46. Perera, B, Jayasuriya, R, Caldera, A, and Wickremasinghe, A. Assessing mental well-being in a Sinhala speaking Sri Lankan population: validation of the WHO-5 well-being index. Health Qual Life Outcomes. (2020) 18:305. doi: 10.1186/s12955-020-01532-8
47. Quansah, F, Hagan, J, Ankomah, F, Agormedah, E, Nugba, R, Srem-Sai, M, et al. Validation of the WHO-5 well-being scale among adolescents in Ghana: evidence-based assessment of the internal and external structure of the measure. Children. (2022) 9:991. doi: 10.3390/children9070991
48. Gallemit, I, Joy, M, Mordeno, I, Simon, P, and Ferolino, M. Assessing the psychometric properties of the World Health Organization five well-being index (WHO-5) in Filipino samples amid the COVID-19 pandemic. BMC Psychol. (2024) 12:580. doi: 10.1186/s40359-024-01941-0
49. Awata, S, Bech, P, Yoshida, S, Hirai, M, Suzuki, S, Yamashita, M, et al. Reliability and validity of the Japanese version of the World Health Organization-five well-being index in the context of depression screening in diabetic patients. Psychiatry Clin Neurosci. (2007) 61:112–9. doi: 10.1111/j.1440-1819.2007.01619.x
50. Bonnín, CM, Yatham, LN, Michalak, EE, Martínez-Arán, A, Dhanoa, T, Torres, I, et al. Psychometric properties of the Spanish version of the well-being index (WHO-5) in a sample of euthymic patients with bipolar disorder. J Affect Disord. (2018) 228:153–9. doi: 10.1016/j.jad.2017.12.006
51. Chongwo, E, Ssewanyana, D, Nasambu, C, Mwangala, PN, Mwangi, PM, Nyongesa, MK, et al. Validation of a Swahili version of the World Health Organization 5-item well-being index among adults living with HIV and epilepsy in rural coastal Kenya. Glob Health Res Policy. (2018) 3:26. doi: 10.1186/s41256-018-0081-z
52. Du, J, Jiang, Y, Lloyd, C, Wei, J, and Hong, X. Validation of the Chinese version of the World Health Organization five-item well-being index in patients with type 2 diabetes mellitus. BMC Psychiatry. (2023) 23:890. doi: 10.1186/s12888-023-05381-9
53. Fekih-Romdhane, F, Al Mouzakzak, F, and Abilmona, G. Validation and optimal cut-off score of the World Health Organization well-being index (WHO-5) as a screening tool for depression among patients with schizophrenia. BMC Psychiatry. (2024) 24:391. doi: 10.1186/s12888-024-05814-z
54. Halliday, J, Hendrieckx, C, Busija, L, Browne, J, Nefs, N, Pouwer, F, et al. Validation of the WHO-5 as a first-step screening instrument for depression in adults with diabetes: results from diabetes MILES – Australia. Diabetes Res Clin Pract. (2017) 132:27–35. doi: 10.1016/j.diabres.2017.07.005
55. Kong, CL, Lee, CC, Ip, YC, Chow, LP, Leung, CH, and Lam, YC. Validation of the Hong Kong Cantonese version of the World Health Organization five well-being index for people with severe mental illness. East Asian Arch Psychiatr. (2016) 26:18–21. doi: 10.3316/informit.957366193196386
56. Nielsen, CM, Lauridsen, HH, Østergaard, SD, and Kølbæk, P. Structural validity of the 5-item World Health Organization well-being index (WHO-5) in patients with schizophrenia spectrum disorders. J Psychiatr Res. (2024) 170:387–93. doi: 10.1016/j.jpsychires.2023.12.028
57. Omani-Samani, R, Maroufizadeh, S, Almasi-Hashiani, A, Sepidarkish, M, and Amini, P. The WHO-5 well-being index: a validation study in people with infertility. Iran J Public Health. (2019) 48:2058–64.
58. Schougaard, LMV, de Thurah, A, Bech, P, Hjollund, NH, and Christiansen, DH. Test-retest reliability and measurement error of the Danish WHO-5 well-being index in outpatients with epilepsy. Health Qual Life Outcomes. (2018) 16:175. doi: 10.1186/s12955-018-1001-0
59. Allgaier, AK, Pietsch, K, Frühe, B, Prast, E, Sigl-Glöckner, J, and Schulte-Körne, G. Depression in pediatric care: is the WHO-five well-being index a valid screening instrument for children and adolescents? Gen Hosp Psychiatry. (2012) 34:234–41. doi: 10.1016/j.genhosppsych.2012.01.007
60. Bonsignore, M, Barkow, K, Jessen, F, and Heun, R. Validity of the five-item WHO well-being index (WHO-5) in an elderly population. Eur Arch Psychiatry Clin Neurosci. (2001) 251:II27–31. doi: 10.1007/BF03035123
61. Campo, A, Miranda, G, Cogollo, Z, and Herazo, E. Reproducibility of the general well-being index (WHO-5 WBI) in adolescent students. Salud Uninorte. (2015) 31:18–24. doi: 10.14482/sun.31.1.5493
62. Caycho, T, Ventura, J, Azabache, K, Reyes, M, and Cabrera, I. Validity and factorial invariance of the general well-being index (WHO-5 WBI) in Peruvian university students. Rev Cienc Salud. (2020) 18:9797. doi: 10.12804/revistas.urosario.edu.co/revsalud/a.9797
63. Eser, E, Çevik, C, Baydur, H, Güneş, S, Esgin, TA, Öztekin, Ç, et al. Reliability and validity of the Turkish version of the WHO-5, in adults and older adults for its use in primary care settings. Prim Health Care Res Dev. (2019) 20:1–7. doi: 10.1017/S1463423619000343
64. Espitia, D, Caballero, C, and Campo, A. Psychometric performance of the general well-being index WHO-5 in school adolescents. Tesis Psicol. (2020) 15:1–17. doi: 10.37511/tesis.v15n2a10
65. Lucas-Carrasco, R. Reliability and validity of the Spanish version of the World Health Organization-five well-being index in the elderly. Psychiatry Clin Neurosci. (2012) 66:508–13. doi: 10.1111/j.1440-1819.2012.02387.x
66. Caycho-Rodríguez, T, Vilca, LW, Valencia, PD, Carbajal-León, C, Reyes-Bossio, M, White, M, et al. Is the meaning of subjective well-being similar in Latin American countries? A cross-cultural measurement invariance study of the WHO-5 well-being index during the COVID-19 pandemic. BMC Psychol. (2023) 11:102. doi: 10.1186/s40359-023-01149-8
67. Topp, C, Østergaard, S, Søndergaard, S, and Bech, P. The WHO-5: systematic review. Psychother Psychosom. (2015) 84:167–76. doi: 10.1159/000376585
68. World Health Organization. WHO-5 well-being index: scoring and use (fact sheet). (2024). Available online at: https://cdn.who.int/media/docs/default-source/mental-health/who-5_english-original4da539d6ed4b49389e3afe47cda2326a.pdf?sfvrsn=ed43f352_11&download.
69. Bandalos, D. Relative performance of categorical diagonally weighted least squares and robust maximum likelihood estimation. Struct Equ Modeling. (2014) 21:102–16. doi: 10.1080/10705511.2014.859510
70. Arafat, Y, Rahman, H, Shalahuddin, A, and Hafez, M. Cross-cultural adaptation and psychometric validation of research instruments: a methodological review. J Behav Health. (2016) 5:129–36. doi: 10.5455/jbh.20160615121755
71. Newsom, J. Summary of minimum sample size recommendations (Psy 523/623 structural equation modeling, spring 2023). Man. (2023). Available online at: https://web.pdx.edu/~newsomj/semclass/ho_sample%20size.pdf.
72. Instituto Nacional de Estadística e Informática [INEI]. Situation of the elderly population: January–February–march 2024. (2024). Available online at: https://www.gob.pe/institucion/inei/informes-publicaciones/5706764-situacion-de-la-poblacion-adulta-mayor-enero-febrero-marzo-2024.
73. World Health Organization. Depression. Report (2021). Available online at: https://www.who.int/es/news-room/factsheets/detail/depression
74. World Health Organization. Ageing and health. (2024). Available online at: https://www.who.int/es/news-room/fact-sheets/detail/ageing-and-health
75. Simancas-Pallares, M, Díaz-Cárdenas, S, Barbosa-Gómez, P, Buendía-Vergara, M, and Arévalo-Tovar, L. Psychometric properties of the World Health Organization general well-being index-5 in partially edentulous patients. Rev Fac Med. (2016) 64:701–5. doi: 10.15446/revfacmed.v64n4.52235
76. Suarez, M, and Alcalá, M. Family APGAR: a tool to detect family dysfunction. Rev Méd Paz. (2014) 20:53–7. Available online at: http://www.scielo.org.bo/scielo.php?script=sci_arttext&pid=S1726-89582014000100010
77. American Educational Research Association. American Psychological Association, & National Council on measurement in education. Standards for educational and psychological testing. Washington, DC: American Educational Research Association. (2014). Availableonline at: https://www.testingstandards.net/uploads/7/6/6/4/76643089/standards_2014edition.pdf.
78. Gadermann, AM, Guhn, M, and Zumbo, BD. Estimating ordinal reliability for Likert-type and ordinal item response data: a conceptual, empirical, and practical guide. Pract Assess Res Eval. (2012) 17:3. doi: 10.7275/n560-j767
79. Jöreskog, KG. On the estimation of polychoric correlations and their asymptotic covariance matrix. Psychometrika. (1994) 59:381–9. doi: 10.1007/BF02296131
80. Viladrich, C, Angulo-Brunet, A, and Doval, E. A journey around alpha and omega to estimate internal consistency reliability. An Psicol. (2017) 33:755–82. doi: 10.6018/analesps.33.3.268401
82. García-Méndez, M, Rivera Aragón, S, and Reyes-Lagunes, I. Parents’ perception of child-rearing. Acta Colombiana Psicol. (2014) 17:133–41. doi: 10.14718/ACP.2014.17.2.14
83. Escobedo, T, Hernández, J, Estebané, V, and Martínez, G. Structural equation models: characteristics, phases, construction, application, and results. Rev Cienc Trabajo. (2016) 18:16–22. Available online at: https://scielo.conicyt.cl/pdf/cyt/v18n55/art04.pdf
84. Rutkowski, L, and Svetina, D. Assessing the hypothesis of measurement invariance in the context of large-scale international surveys. Educ Psychol Meas. (2014) 74:31–57. doi: 10.1177/0013164413498257
85. McDonald, RP. Test theory: A unified treatment. Mahwah, NJ: Lawrence Erlbaum Associates, Inc (1999).
86. Campo-Arias, A, and Oviedo, HC. Psychometric properties of a scale: internal consistency. Rev Salud Pública. (2008) 10:831–9. doi: 10.1590/s0124-00642008000500015
89. Linacre, JM. Optimizing rating scale category effectiveness. J Appl Meas. (2002) 3:85–106. Available online at: https://pubmed.ncbi.nlm.nih.gov/11997586/
90. Pérez, ER, and Medrano, L. Exploratory factor analysis: conceptual and methodological foundations. Rev Argent Cienc Comport. (2010) 2:58–6. doi: 10.32348/1852.4206.v2.n1.15924
91. Svetina, D, Rutkowski, L, and Rutkowski, D. Multiple-group invariance with categorical outcomes using updated guidelines: an illustration using Mplus and the lavaan/semTools packages. Struct Equ Model Multidiscip J. (2019) 27:111–30. doi: 10.1080/10705511.2019.1602776
92. Ferrando, P, and Anguiano-Carrasco, C. Factor analysis as a research technique in psychology. Papeles Psicól. (2010) 31:18–33. Available online at: https://www.redalyc.org/pdf/778/77812441003.pdf
93. Kiliç, S. Cronbach's alpha reliability coefficient. Psychiatry Behav Sci. (2016) 6:47. doi: 10.5455/jmood.20160307122823
94. Hooper, D, Coughlan, J, and Mullen, MR. Structural equation modelling: guidelines for determining model fit. Electron J Bus Res Methods. (2008) 6:53–60. Available online at: https://academic-publishing.org/index.php/ejbrm/article/view/1224
95. Ruiz, M, Pardo, A, and San Martín, R. Structural equation models. Papeles Psicól. (2010) 31:34–45. Available online at: https://www.psychologistpapers.com/English/1794.pdf
96. Hirschfeld, G, and Brachel, R. Improving multiple-group confirmatory factor analysis in R – a tutorial in measurement invariance with continuous and ordinal indicators. Pract Assess Res Eval. (2014) 19:2946. doi: 10.7275/qazy-2946
97. George, D, and Mallery, P. SPSS for windows step by step: A simple guide and reference. 4th ed. Boston, MA: Allyn and Bacon (2003).
99. Shrestha, N. Factor analysis as a tool for survey analysis. Am J Appl Math Stat. (2021) 9:4–11. doi: 10.12691/ajams-9-1-2
100. Díaz, C, Rodríguez, J, and Rodríguez, R. Subjective well-being, cognitive-affective strategies and family. Int J Dev Educ Psychol. (2018) 3:179–88. doi: 10.17060/ijodaep.2018.n1.v3.1251
101. Lara, L, and González, I. Family functionality and its relationship with subjective well-being in high school students. Latam Rev Latin Cienc Soc Hum. (2023) 4:4544–57. doi: 10.56712/latam.v4i1.311
102. Felsinger, R, Mayer, S, Haidinger, G, and Simon, J. Aging well? Exploring self-reported quality of life in the older Austrian population based on repeated cross-sectional data. J Aging Soc Policy. (2024) 37:654–70. doi: 10.1080/08959420.2024.2423102
103. Dimitrov, D. Factorial invariance tests in the context of construct validation. Meas Eval Couns Dev. (2010) 43:121–49. doi: 10.1177/0748175610373459
104. Yap, SCY, Wortman, J, Anusic, I, Baker, SG, Scherer, LD, Donnellan, MB, et al. The effect of mood on subjective well-being judgments: nine tests of the judgment model. J Pers Soc Psychol. (2017) 113:939–61. doi: 10.1037/pspp0000115
105. Boateng, GO, Neilands, TB, Frongillo, EA, Melgar-Quiñonez, HR, and Young, SL. Best practices for developing and validating scales for health, social, and behavioral research: a primer. Front Public Health. (2018) 6:149. doi: 10.3389/fpubh.2018.00149
106. Peterson, CH, Peterson, NA, and Powell, KG. Cognitive interviewing for item development: validity evidence based on content and response processes. Meas Eval Couns Dev. (2017) 50:217–23. doi: 10.1080/07481756.2017.1339564
108. Instituto de Democracia y Derechos Humanos (Idehpucp). The situation of the elderly population in Peru: findings from an Idehpucp study to improve public policies. (2018). Available online at: https://idehpucp.pucp.edu.pe/notas-informativas/la-situacion-de-la-poblacion-adulta-mayor-en-el-peru-hallazgos-de-una-investigacion-del-idehpucp-para-mejorar-las-politicas-publicas/.
109. Koydemir, S, Sökmez, AB, and Schütz, A. A meta-analysis of the effectiveness of randomized controlled positive psychological interventions on subjective and psychological well-being. Appl Res Qual Life. (2020) 16:1145–85. doi: 10.1007/s11482-019-09788-z
110. Lafont, C, Chah, A, Lemogne, C, Gouraud, C, Fossey-Diaz, V, Orvoen, G, et al. Diagnostic performance of the 4-item geriatric depression scale for depression screening in older patients with cancer: the ELCAPA cohort study. Oncologist. (2021) 26:e983–91. doi: 10.1002/ONCO.13746
111. Lara-Cabrera, M, Betancort, M, Muñoz-Rubilar, A, Bjerkeset, O, and De Las Cuevas, C. Psychometric properties of the WHO-5 well-being index among nurses during the COVID-19 pandemic: a cross-sectional study in three countries. Int J Environ Res Public Health. (2022) 19:10106. doi: 10.3390/ijerph191610106
112. Molina, C, and Ramírez, A. Psychometric properties of the geriatric depression scale: systematic review. Concienc Digit. (2023) 6:89–104. doi: 10.33262/concienciadigital.v6i1.1.2479
113. National Service for the Elderly [SENAMA]. Comprehensive positive aging policy for Chile 2012-2025. (2015). Available online at: https://vifadultomayor.files.wordpress.com/2016/12/senamalibropoliticas_.pdf.
114. Shiva, S, Ajit, B, Nagalakshmi, R, Krishna, P, Palanimuthu, T, and Mathew, V. Geriatric depression and cognitive impairment – an update. Indian J Psychol Med. (2021) 43:286–93. doi: 10.1177/0253717620981556
115. Troncoso Pantoja, C, and Soto-López, N. Family functionality, self-sufficiency, and psychosocial well-being of older adults. Horizonte Méd (Lima). (2018) 18:23–8. doi: 10.24265/horizmed.2018.v18n1.04
116. United Nations (UN). Goal 3: ensure healthy lives and promote well-being for all at all ages. 2030 Agenda for Sustainable Development. (2015).
Keywords: general well-being, family functioning, older adults, psychometric properties, reliability
Citation: del Pilar Díaz Gamarra P, Rosario Quiroz FJ, Alomía ERE, Iparraguirre Yaurivilca NE and Misare Condori MA (2025) Psychometric evidence of the WHO-5 well-being index in a sample of participants from hospitals and older adults care centers in Peru. Front. Public Health. 13:1670429. doi: 10.3389/fpubh.2025.1670429
Edited by:
Víctor Hugo Fernández-Bedoya, Universidad Nacional Mayor de San Marcos, PeruReviewed by:
Inga Iždonaitė-Medžiūnienė, SMK College of Applied Sciences, LithuaniaJohn Ben Prince, Prin LN Welingkar Institute of Management Development and Research–Bengaluru Campus, India
William Alfredo Ortiz-Ochoa, University of Cuenca, Ecuador
Copyright © 2025 del Pilar Díaz Gamarra, Rosario Quiroz, Alomía, Iparraguirre Yaurivilca and Misare Condori. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Patricia del Pilar Díaz Gamarra, Z3BhdHJpY2lhZEB1Y3YuZWR1LnBl
 Patricia del Pilar Díaz Gamarra
Patricia del Pilar Díaz Gamarra Fernando Joel Rosario Quiroz
Fernando Joel Rosario Quiroz Erika Roxana Estrada Alomía
Erika Roxana Estrada Alomía