- 1Medical Service Dimension, China-Japan Union Hospital of Jilin University, Changchun, China
- 2Department of Hand and Foot Surgery, China-Japan Union Hospital of Jilin University, Changchun, China
- 3Department of Nursing, China-Japan Union Hospital of Jilin University, Changchun, China
Objectives: To present the most recent and comprehensive systematic review and meta-analysis assessing the predictive value of prognostic nutritional index (PNI) for the long-term outcomes of elderly patients with fractures.
Methods: We systematically searched PubMed, Cochrane, Embase and Web of Science up to July, 2025 for studies assessing the predictive value of PNI for the long-term prognosis of elderly patients with fractures. The primary outcome measured was mortality. Odds ratios (ORs) and 95% confidence intervals (CIs) were used for data pooling. Additionally, sensitivity and subgroup analyzes were performed to assess the stability of the results and identify potential sources of heterogeneity. All analyzes were performed using Review Manger 5.4 and STATA 15.1.
Results: Eight studies encompassing 11,576 elderly individuals were included for meta-analysis. The meta-analysis demonstrated that mortality was notably lower in individuals with high PNI compared to those with low PNI (OR: 0.75; 95% CI: 0.66, 0.85; p < 0.0001). Subgroup analysis of mortality based on study design and PNI cut-off showed that the predictive value of PNI for mortality remained significant in prospective studies and those with a cut-off value ≥40. However, this association was not observed in retrospective studies or those with a cut-off below 40.
Conclusion: PNI can effectively predict the long-term mortality in elderly individuals with fractures. Considering the limitations of this article, future large-scale, multicenter prospective cohort studies are still required to evaluate the prognostic value of PNI in senior patients with fractures and its influencing factors.
Systematic review registration: PROSPERO, identifier CRD420251047385.
1 Introduction
Elderly people are more prone to falls and fractures due to decreased coordination, comorbidities, and increased bone fragility (1). Because their recovery ability is not as good as that of young people, fractures can seriously affect the physical and mental functions of elderly patients (2). The health-related quality of life and health status of most elderly patients do not fully return to pre-fracture levels (3). Among them, hip fracture is one of the most common types of fractures in the elderly population, with high disability and mortality rates (4, 5). It is estimated that by 2050, China will fully enter an aging society, and the number of hip fracture cases in China is expected to increase sixfold (6). Approximately 40 to 60% of elderly individuals experience hip fractures, and the mortality rate in the first 30 days after fracture is as high as 8–10%, and one-year mortality rate approaching 20–28% (2, 6). Therefore, exploring the factors influencing poor prognosis in elderly individuals with fractures following surgery is crucial to achieving early prediction and mitigating risk factors to improve patient outcomes.
Multiple studies have found that poor nutritional status plays a significant role in poor prognosis after surgery among senior fracture patients. It can also lead to the occurrence of refeeding syndrome and increase the mortality risk in patients (7–9). Calculated using peripheral blood lymphocyte counts and serum albumin concentrations, the prognostic nutritional index (PNI) is a key indicator of the body’s nutritional and immune status (10, 11). Initially, it was designed to assess the nutritional and immune status of patients undergoing gastrointestinal surgery. Recently, there has been a growing body of research highlighting the prognostic value of PNI in elderly patients with fractures (12–14). Some studies have suggested that PNI levels serve as a reliable indicator for evaluating malnutrition, and low levels of PNI are associated with higher mortality and worse postoperative mobility in elderly patients with fractures, and have important predictive value for long-term poor prognosis (15–17). In addition, PNI was found to be an independent predictor of postoperative intensive care unit requirement in patients with hip fractures (18). However, due to differences in sample size, follow-up time, treatment methods, and fracture sites, there is currently no definite conclusion on whether PNI can effectively predict the long-term prognosis of elderly individuals with fractures.
Although Liu et al. (19) conducted a meta-analysis to assess the role of PNI for postoperative mortality among individuals with hip fracture, they only included 3 original studies and revealed no significant link between PNI levels and mortality in hip fracture patients. After the publication of Liu et al.’s study, numerous new clinical studies have been conducted to assess the long-term prognostic value of PNI in elderly fracture patients, and the conclusions do not support previous studies (15–18, 20–22). Therefore, this study focuses on PNI as an easily measurable peripheral circulation marker. Through systematic literature retrieval and meta-analysis, it expands upon previous meta-analyzes by incorporating the latest research data to further evaluate PNI’s ability to predict the long-term prognosis of elderly individuals with fractures. This study aims to provide updated evidence-based insights for constructing a prognostic prediction model for elderly fracture patients.
2 Methods
2.1 Literature search
Following the PRISMA 2020 statement (Preferred Reporting Items for Systematic Reviews and Meta-Analysis), this meta-analysis was performed and prospectively registered in the PROSPERO database (CRD420251047385). A systematic literature search was conducted across PubMed, Embase, Web of Science, and Cochrane up to July 2025 to collect studies focusing on the prognostic role of PNI in the long-term outcomes of elderly fracture patients. The literature was searched via the following keywords: “prognostic nutritional index,” “PNI,” and “fracture,” etc. The search strategies used in PubMed are outlined below: ((“Fractures, Bone”[Mesh]) OR (((((((((Bone Fracture) OR (Bone Fractures)) OR (Broken Bones)) OR (Broken Bone)) OR (Spiral Fractures)) OR (Spiral Fracture)) OR (Torsion Fractures)) OR (Torsion Fracture)) OR (Fracture))) AND ((prognostic nutritional index[Title/Abstract]) OR (PNI[Title/Abstract])). Furthermore, the reference lists of the selected studies were manually examined. Two authors identified and assessed qualifying articles separately, and any disagreements were addressed by discussion (show in Supplementary Table S1).
2.2 Inclusion and exclusion criteria
The following conditions determined eligibility for articles: (1) the study design was a randomized controlled trial, cohort, or case–control; (2) the studies were conducted in elderly individuals with fractures; (3) the studies assessed the role of PNI in long-term prognosis (at least 3 months after the fracture) of elderly fracture patients; (4) at least one long-term outcome was evaluated, including mortality, refracture, cardiovascular event, etc.; (5) sufficient data to analyze odds ratio (OR). Exclusions included review articles, non-original studies (such as letters, comments, abstracts, corrections, and replies), study protocols, unpublished articles, and studies with inadequate data.
2.3 Data abstraction
Data abstraction was performed independently by two authors, with any differences resolved through discussion with a third author. The following details were extracted from the qualified studies: first author name, published year, study country, study design, types of fractures, sample size, age, gender, BMI, PNI cut-off, and outcomes. In cases of insufficient research data, corresponding authors were contacted to obtain the complete data, if available.
2.4 Quality evaluation
The Newcastle-Ottawa Scale (NOS) was used to evaluate the quality of the included cohort studies (23), and studies scoring 7–9 points were deemed high quality (24). Two authors independently reviewed the quality of each study, with any differences addressed through discussion.
2.5 Statistical analysis
The meta-analysis was performed using Review Manager 5.4.1 software. OR and 95% confidence intervals (CIs) were applied for the data synthesis. To evaluate the heterogeneity of each outcome, the chi-squared (χ2) test (Cochran’s Q) and I2 index were employed (25). χ2 p value below 0.1 or I2 value exceeding 50% was considered indicative of high heterogeneity. The random-effects model was then utilized to estimate the overall OR for all outcomes. Additionally, subgroup analyzes were conducted to assess possible confounding factors, provided sufficient data were available. Furthermore, a sensitivity analysis was conducted to assess the impact of each included study on the overall odds ratio (OR) for each outcome. Publication bias was assessed by generating funnel plots using Review Manager 5.4.1 and performing Egger’s regression tests (26) with Stata 15.1 (Stata Corp, College Station, Texas, United States). A p-value < 0.05 was considered indicative of statistically significant publication bias.
3 Results
3.1 Literature retrieval, study characteristics, and baseline
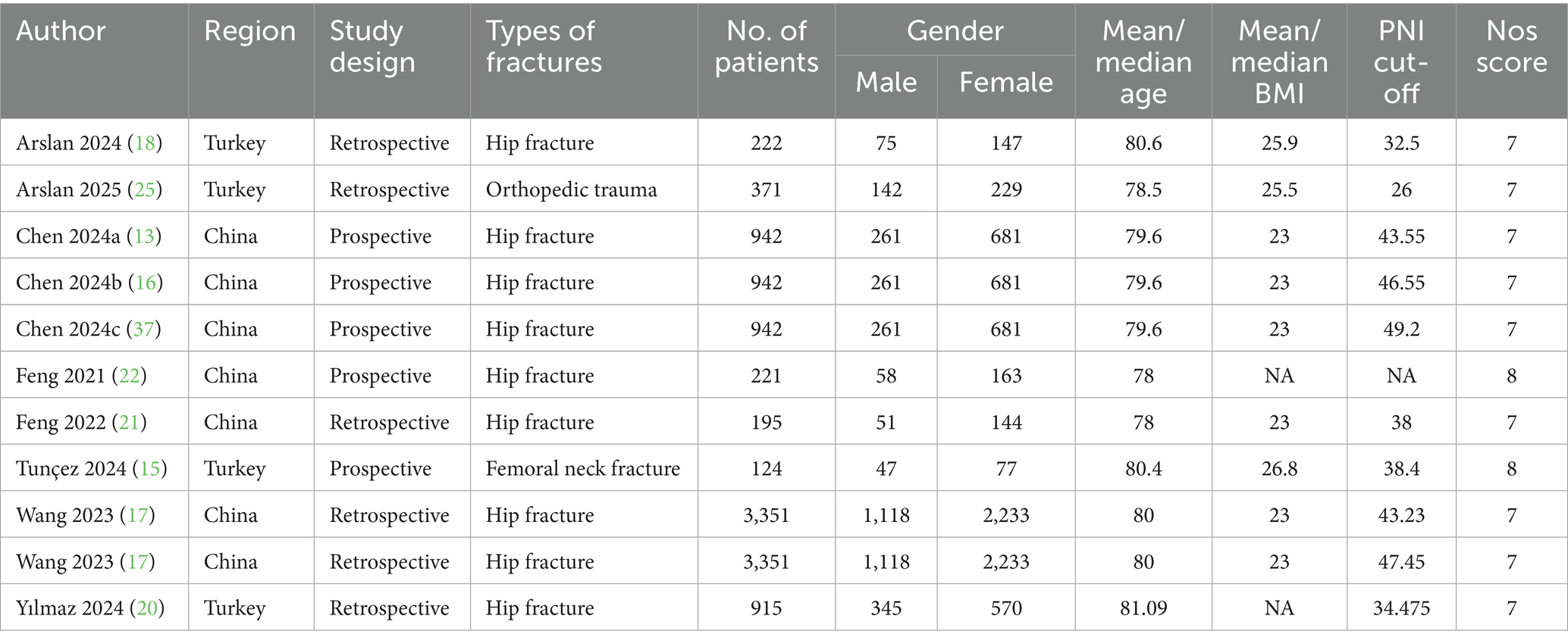
The literature retrieval and selection process is illustrated in the flowchart presented in Figure 1. A total of 199 relevant studies were identified through a systematic literature search across PubMed (n = 50), Embase (n = 46), Web of Science (n = 103), and Cochrane (n = 0). After removing duplicates, 116 titles and abstracts were reviewed. In the end, 8 cohort studies (with 11 comparative groups) comprising 11,576 patients were incorporated into the meta-analysis (15–18, 20–22, 27). The details and quality assessment of each included cohort study are provided in Table 1.
3.2 Mortality
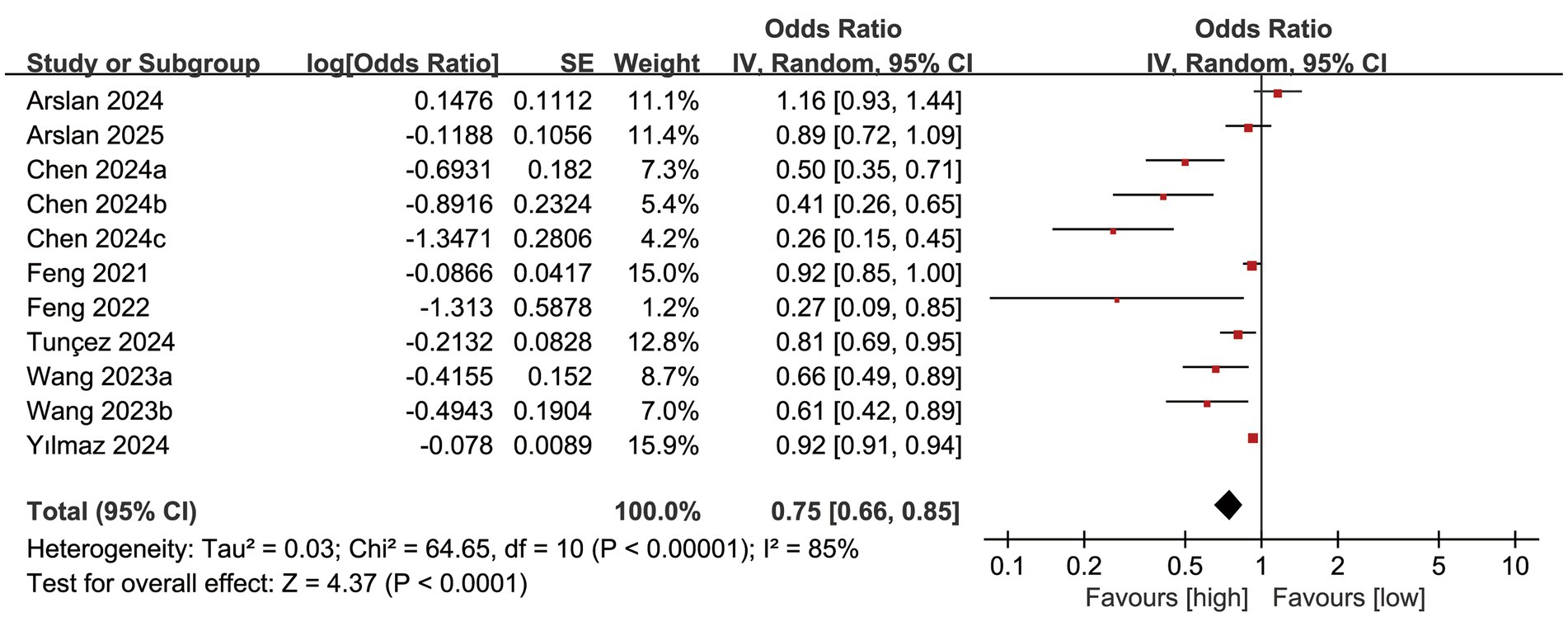
The mortality outcomes were derived from 8 cohort studies, and the meta-analysis indicated a significantly reduced mortality rate in the high PNI group compared to the low PNI group (OR: 0.75; 95% CI: 0.66, 0.85; P <0.0001). Significant heterogeneity was identified (I2 = 85%, P <0.00001) (Figure 2).
3.3 Publication bias and sensitivity analysis
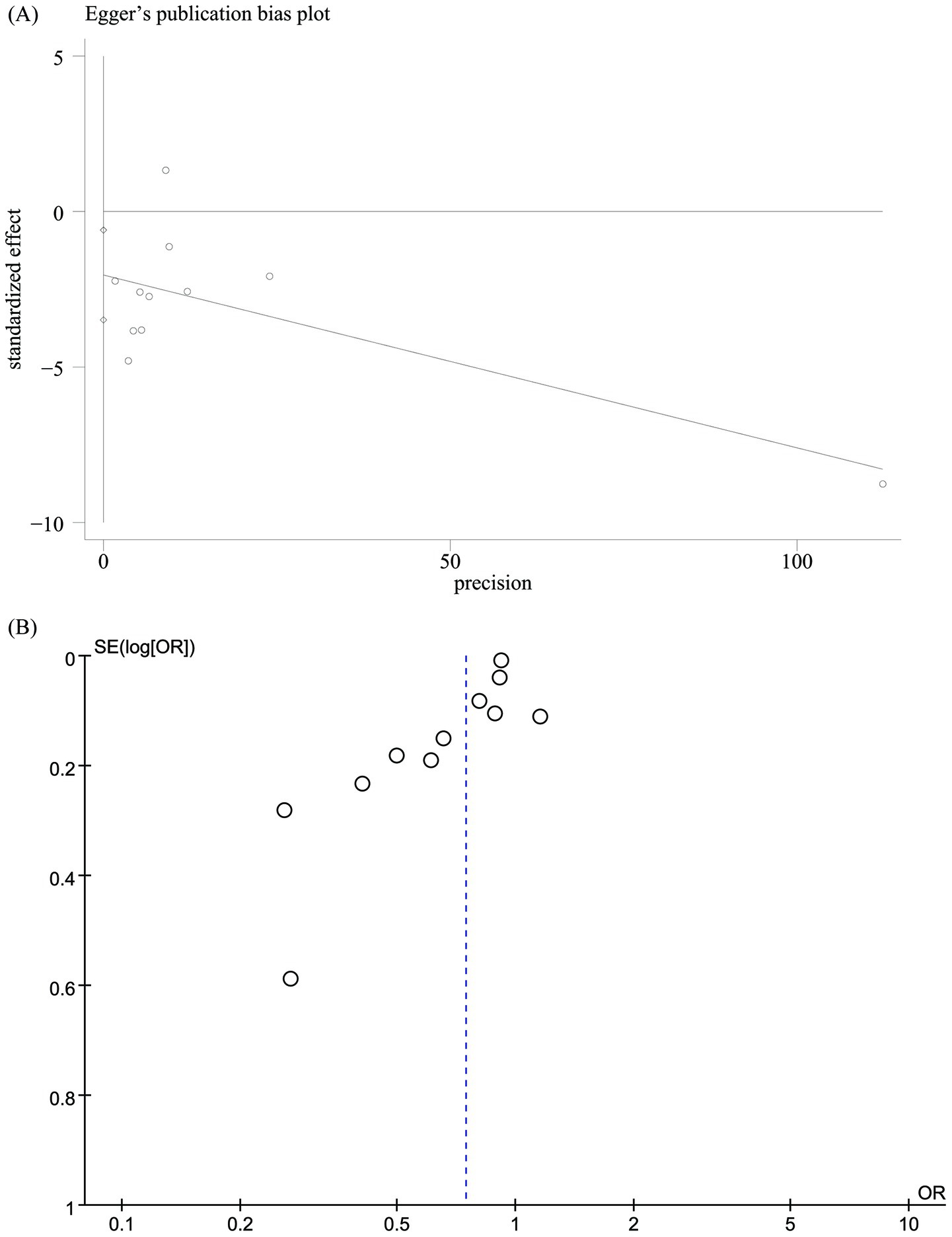
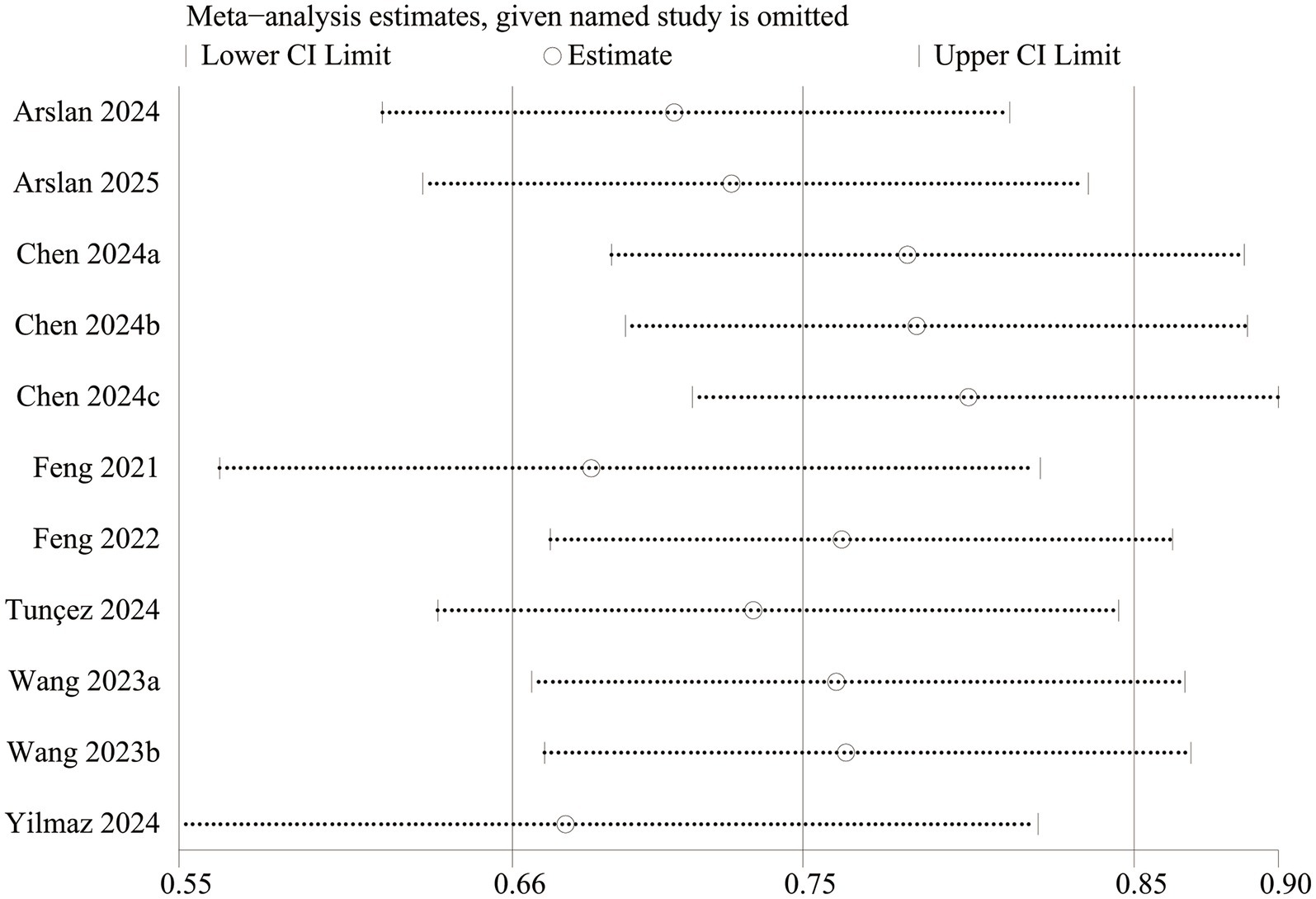
Funnel plots and Egger’s regression tests were used to identify potential publication bias for mortality. Egger’s test (p = 0.012, Figure 3A) and funnel plots (Figure 3B) detected a significant publication bias for mortality. We also performed a sensitivity analysis on the mortality outcomes to assess the influence of each cohort study on the overall OR by sequentially removing studies. The results demonstrated that the total OR remained consistent after the removal of each study for mortality (Figure 4).
3.4 Subgroup analysis
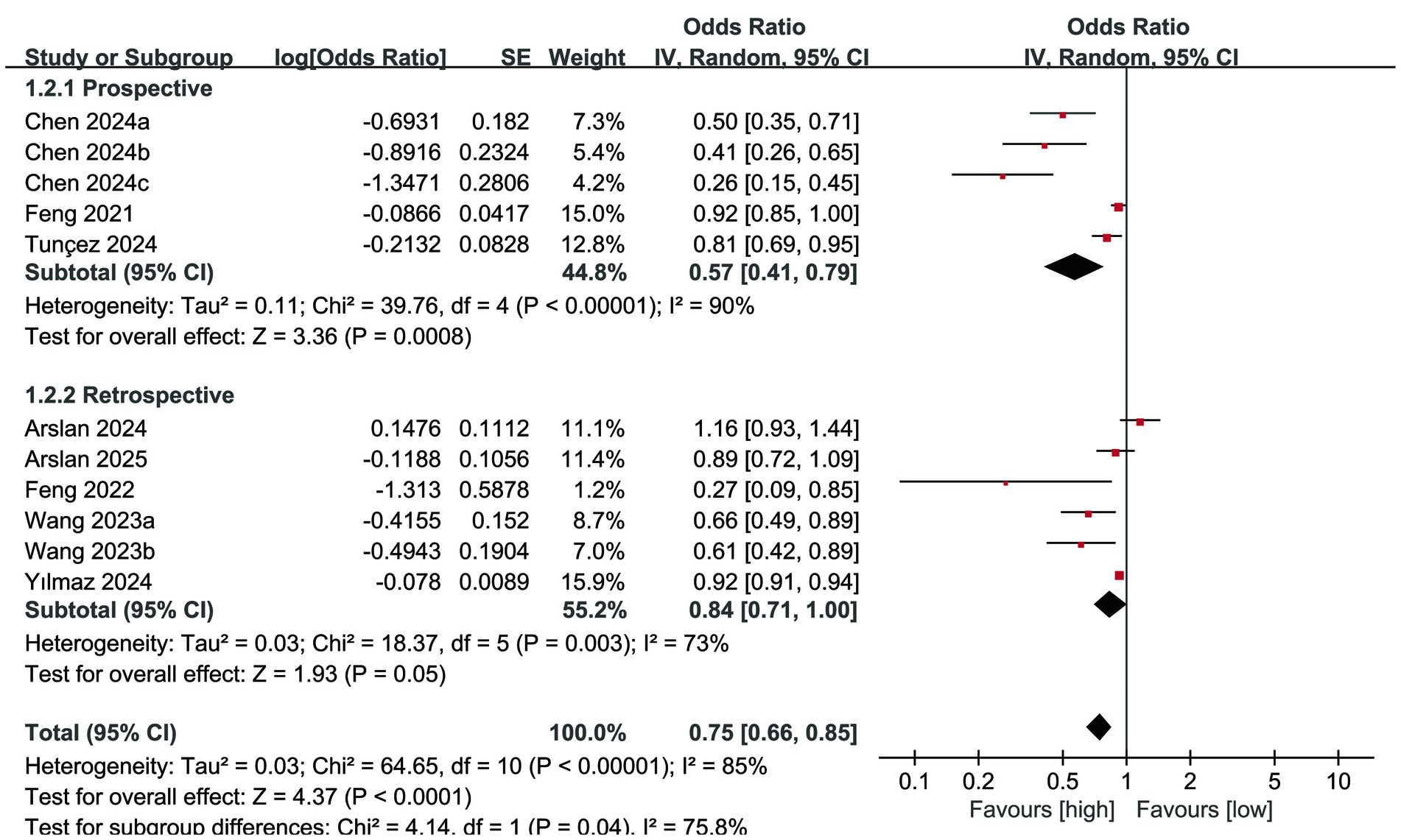
Subgroup analysis of mortality according to study design showed that the predictive value of PNI for mortality continued to be significant in prospective studies (OR: 0.57; 95% CI: 0.41, 0.79; p = 0.0008) but disappeared in retrospective studies (OR: 0.84; 95% CI: 0.71, 1.00; p = 0.05) (Figure 5). At the same time, a decrease in heterogeneity was observed in retrospective studies. Subgroup analysis of mortality according to PNI cut-off values showed that the predictive value of PNI for mortality continued to show significance in studies with a cut-off value ≥ 40 (OR: 0.49; 95% CI: 0.37, 0.65; P <0.00001), but disappeared in studies with a cut-off value < 40 (OR: 0.91; 95% CI: 0.80, 1.04; p = 0.17) (Figure 6). At the same time, a decrease in heterogeneity was observed in both subgroups.
4 Discussion
Studies have pointed out that elderly patients with fractures have a higher risk of malnutrition during the perioperative period, which will increase the mortality rate of patients. The main reasons are that the elderly have decreased body function, decreased appetite, reduced nutritional intake, and often have chronic diseases, physiological and psychological problems (28). PNI is a commonly used indicator for clinical evaluation of preoperative nutritional status, surgical risk and prognosis of surgery, and has certain value in predicting the prognosis of elderly individuals with fractures. Katsuyama et al. (29) included 1,026 hip fracture patients aged 65 years or older who had undergone surgery. The results showed that PNI was an important predictor of postoperative mortality in individuals with hip fractures, but this conclusion was not supported by all studies (18, 21). Therefore, this article further evaluated the role of PNI in predicting the long-term prognosis of elderly fracture patients, providing up-to-date evidence to inform the creation of a prognosis prediction model for this population.
This study found that PNI was significantly associated with long-term mortality after surgery in senior fracture patients, and the lower the PNI, the higher the mortality rate of the patient. Sensitivity analysis further verified that this result was not significantly affected by a single study, and the evidence was stable and reliable. However, it is worth noting that a significant publication bias was detected in mortality, which could potentially influence the reliability of the findings to some extent. We speculate that regional selection bias may be one of the main causes of publication bias, because the literature included in this study are all studies in Asia, mainly China and Turkey, which also needs to be further resolved by international multicenter studies. In addition, significant heterogeneity is also a problem that cannot be ignored in this study. Based on this, we conducted a subgroup analysis based on the study design and PNI cut-off value, and the results suggested that the significant heterogeneity of mortality can be partially explained by the study design and PNI cut-off value.
Our conclusions do not support the meta-analysis results of Liu et al. (19), which suggested that there is no significant link between PNI and mortality in individuals with hip fractures. It is worth noting that the meta-analysis of Liu et al. only included 3 original studies, which resulted in unavoidable small sample size effects and selection bias. In addition, the study of Liu et al. did not conduct rigorous sensitivity analysis and subgroup analysis, and it is impossible to determine whether its results would be significantly affected by a single study or a certain factor. Therefore, the existing evidence supports that PNI can significantly predict the mortality of elderly patients with fractures, but additional research is required to validate this.
On the other hand, our mortality subgroup analysis according to the study design showed that the prognostic value of PNI for mortality was still relevant in prospective studies, but disappeared in retrospective studies. This differential result does not change the overall quality of this study, because it is well known that the quality of evidence in prospective studies is better than that in retrospective studies. In addition, the subgroup analysis of mortality according to the PNI cut-off value showed that the predictive value of PNI for mortality was still significant in studies with a cut-off value ≥ 40, but disappeared in studies with a cut-off value < 40. However, there is no definite conclusion on the optimal cut-off value of PNI (14, 30). Different studies have different optimal cut-off value confirmation methods (although most of them are through ROC curves), and different fracture populations also have different optimal PNI cut-off values (12, 31, 32). The findings of this study are more inclined to determine the cut off value of PNI above 40 in order to maximize its predictive value, but this result should be validated through additional studies with larger sample sizes.
Elderly patients with fractures are often accompanied by malnutrition, which leads to decreased serum albumin levels and decreased lymphocyte counts (11, 33, 34). Serum albumin plays a crucial role in maintaining plasma osmotic pressure and transporting substances (35–37). Its decreased level can affect the body’s metabolism and immune function (37). As a crucial component of the immune system, a decrease in the number of lymphocytes can lead to decreased immune function and increase the risk of complications such as infection (31, 38). Therefore, PNI can indirectly reflect the patient’s nutritional and immune status by evaluating serum albumin and lymphocyte counts, thereby predicting their postoperative recovery and prognosis (39, 40). In addition, in elderly patients with fractures, disorders of the endocrine system may lead to abnormal metabolism and decreased immune function (41). For example, insulin resistance and decreased growth hormone secretion may lead to decreased protein synthesis and increased decomposition, further aggravating malnutrition (42, 43). As an indicator for evaluating nutritional and immune status, PNI may reflect the regulatory function of the endocrine system to a certain extent. Furthermore, the regulation of the nervous system may be affected in elderly patients with fractures, resulting in a decrease in the body’s ability to regulate nutritional and immune status (44). For example, disorders of the autonomic nervous system may lead to gastrointestinal dysfunction and malnutrition (45, 46). As an indicator for evaluating nutritional and immune status, PNI may reflect the regulatory function of the nervous system to a certain extent.
Nevertheless, it is important to recognize some limitations of this analysis. Owing to the nature of clinical research, a significant portion of the studies included are retrospective cohort studies. As is well-known, confounding factors and risk of bias are the biggest disadvantages of retrospective studies. In addition, the literature analyzed in this meta-analysis predominantly comes from Asia, especially China and Turkey, and lacks data from Europe and the United States. Therefore, the generalizability of these results to other countries is not clear. Lastly, the results of PNI predicting mortality in elderly patients with fractures have obvious heterogeneity and publication bias, which have not been fully explained. Therefore, it is important to be cautious when interpreting the relationship between PNI and mortality in elderly patients with fractures. Despite these limitations, this analysis represents the most recent largest study reporting the prognostic value of PNI in elderly fracture patients. The results underscore the significance of monitoring PNI levels during the clinical management of these patients. Moreover, they highlight the potential of developing a more robust fracture prognosis prediction model incorporating inflammatory markers like PNI, ultimately aiming to enhance patient outcomes and their quality of life.
5 Conclusion
As a clinically accessible, inexpensive, and noninvasive nutritional marker, PNI can effectively predict the long-term mortality of senior fracture patients, and help to identify high-risk individuals with poor prognosis at an early stage and take targeted preventive and treatment measures. Subgroup analysis found that using a PNI cutoff value of 40 or higher provides better predictive value. Considering the limitations of this article, such as significant heterogeneity, publication bias, and regional selection bias, there is still a need for more extensive, multicenter prospective cohort studies to evaluate the prognostic value of PNI in elderly fracture patients and its influencing factors.
Data availability statement
The original contributions presented in the study are included in the article/Supplementary material, further inquiries can be directed to the corresponding author.
Author contributions
BB: Data curation, Conceptualization, Writing – original draft, Writing – review & editing, Investigation, Methodology, Visualization, Formal analysis. XL: Visualization, Validation, Resources, Data curation, Supervision, Conceptualization, Writing – review & editing, Writing – original draft, Software. HL: Project administration, Writing – review & editing, Funding acquisition, Writing – original draft, Resources, Methodology, Investigation.
Funding
The author(s) declare that financial support was received for the research and/or publication of this article. This work was supported by the Norman Bethune Project of Jilin University (2024B10).
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Generative AI statement
The authors declare that no Gen AI was used in the creation of this manuscript.
Publisher’s note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
Supplementary material
The Supplementary material for this article can be found online at: https://www.frontiersin.org/articles/10.3389/fnut.2025.1631128/full#supplementary-material
References
1. Prevot, LB, Bolcato, V, Fozzato, S, Accetta, R, Basile, M, Tronconi, LP, et al. Peri-implant femoral fractures in elderly: morbidity, mortality, treatment options and good practices. Chin J Traumatol. (2024) 9:S1008-1275(24)00173-1. doi: 10.1016/j.cjtee.2024.07.012
2. Alexiou, KI, Roushias, A, Varitimidis, SE, and Malizos, KN. Quality of life and psychological consequences in elderly patients after a hip fracture: a review. Clin Interv Aging. (2018) 13:143–50. doi: 10.2147/CIA.S150067
3. Zhao, H, Wei, P, and Feng, Y. Association between frailty and clinical outcomes and quality of life in older adults following hip fracture surgery: a retrospective cohort study. Anesth Analg. (2022) 134:1035–42. doi: 10.1213/ANE.0000000000005841
4. Pan, WG, Chou, YC, Wu, JL, and Yeh, TT. Impact of hematologic inflammatory markers on the prognosis of geriatric hip fracture: a systematic review and meta-analysis. Eur J Med Res. (2024) 29:609. doi: 10.1186/s40001-024-02211-w
5. Aggarwal, N, Sinha, S, Kumar, A, Kumar, S, Qureshi, OA, and Jameel, J. Predictors of functional outcomes of nonoperatively treated extra-articular distal end radius fractures in older individuals: a prospective clinical study. Hand (NY). (2024) 20:15589447241305421. doi: 10.1177/15589447241305421
6. Chang, S-M, Hou, Z-Y, Hu, S-J, and Du, S-C. Intertrochanteric femur fracture treatment in Asia: what we know and what the world can learn. Orthop Clin North Am. (2020) 51:189–205. doi: 10.1016/j.ocl.2019.11.011
7. Pass, B, Malek, F, Rommelmann, M, Aigner, R, Knauf, T, Eschbach, D, et al. The influence of malnutrition measured by hypalbuminemia and body mass index on the outcome of geriatric patients with a fracture of the proximal femur. Medicina. (2022) 58:1610. doi: 10.3390/medicina58111610
8. Funahashi, H, Morita, D, Iwase, T, and Asamoto, T. Usefulness of nutritional assessment using geriatric nutritional risk index as an independent predictor of 30-day mortality after hip fracture surgery. Orthop Traumatol Surg Res. (2022) 108:103327. doi: 10.1016/j.otsr.2022.103327
9. Fujimoto, Y, Setoguchi, T, Ishidou, Y, and Taniguchi, N. Low geriatric nutritional risk index is a risk factor for death within 1 year following hip fracture. J Orthop Surg. (2022) 30:10225536221103360. doi: 10.1177/10225536221103360
10. Yotsuya, K, Yamazaki, K, Sarukawa, J, Yasuda, T, and Matsuyama, Y. Relationship between the perioperative prognostic nutritional index and postoperative gait function in elderly hip fractures. Osteoporos Sarcopenia. (2024) 10:72–7. doi: 10.1016/j.afos.2024.05.006
11. Mi, X, Jia, Y, Song, Y, Liu, K, Liu, T, Han, D, et al. Preoperative prognostic nutritional index value as a predictive factor for postoperative delirium in older adult patients with hip fractures: a secondary analysis. BMC Geriatr. (2024) 24:21. doi: 10.1186/s12877-023-04629-z
12. Ju, G, and Liu, X. Prognostic nutritional index and modified frailty index, independent risk factors for recompression in elderly patients with osteoporotic vertebral compression fractures. Eur Spine J. (2024) 33:1518–23. doi: 10.1007/s00586-023-08016-5
13. Chen, Y, Bei, M, Liu, G, Zhang, J, Ge, Y, Tan, Z, et al. Prognostic nutritional index (PNI) is an independent predictor for functional outcome after hip fracture in the elderly: a prospective cohort study. Arch Osteoporos. (2024) 19:107. doi: 10.1007/s11657-024-01469-1
14. Rutenberg, TF, Gabarin, R, Kilimnik, V, Daglan, E, Iflah, M, Zach, S, et al. Nutritional and inflammatory indices and the risk of surgical site infection after fragility hip fractures: can routine blood test point to patients at risk? Surg Infect. (2023) 24:645–50. doi: 10.1089/sur.2023.118
15. Tunçez, M, Bulut, T, Süner, U, Önder, Y, and Kazımoğlu, C. Prognostic nutritional index (PNI) is an independent risk factor for the postoperative mortality in geriatric patients undergoing hip arthroplasty for femoral neck fracture? A prospective controlled study. Arch Orthop Trauma Surg. (2024) 144:1289–95. doi: 10.1007/s00402-024-05201-z
16. Chen, Y, Liu, G, Zhang, J, Ge, Y, Tan, Z, Peng, W, et al. Prognostic nutritional index (PNI) as an independent predictor of 3-year postoperative mortality in elderly patients with hip fracture: a post hoc analysis of a prospective cohort study. Orthop Surg. (2024) 16:2761–70. doi: 10.1111/os.14200
17. Wang, Y, Jiang, Y, Luo, Y, Lin, X, Song, M, Li, J, et al. Prognostic nutritional index with postoperative complications and 2-year mortality in hip fracture patients: an observational cohort study. Int J Surg. (2023) 109:3395–406. doi: 10.1097/JS9.0000000000000614
18. Arslan, K, Celik, S, Arslan, HC, Sahin, AS, Genc, Y, and Erturk, C. Predictive value of prognostic nutritional index on postoperative intensive care requirement and mortality in geriatric hip fracture patients. North Clin Istanb. (2024) 11:249–57. doi: 10.14744/nci.2024.60430
19. Liu, N, Lv, L, Jiao, J, Zhang, Y, and Zuo, XL. Association between nutritional indices and mortality after hip fracture: a systematic review and meta-analysis. Eur Rev Med Pharmacol Sci. (2023) 27:2297–304. doi: 10.26355/eurrev_202303_31763
20. Yilmaz, S, Kurt, M, and Dülgeroğlu, TC. Investigation of the predictive value of systemic immune inflammation index (SII) and prognostic nutritional index (PNI) on mortality in patients with endoprosthesis after hip fracture. Medicine. (2024) 103:e38063. doi: 10.1097/MD.0000000000038063
21. Feng, L, Chen, W, Ping, P, Ma, T, Li, Y, Xu, L, et al. Preoperative malnutrition as an independent risk factor for the postoperative mortality in elderly Chinese individuals undergoing hip surgery: a single-center observational study. Ther Adv Chronic Dis. (2022) 13:20406223221102739. doi: 10.1177/20406223221102739
22. Feng, L, Fu, S, Yao, Y, Yuan, W, and Zhao, Y. Age, prognostic nutritional index, and Charlson comorbidity index were independent risk factors for postoperative long-term mortality in Chinese geriatric patients who sustain hip fracture. J Am Med Dir Assoc. (2021) 22:2602–3. doi: 10.1016/j.jamda.2021.08.001
23. Wells, G, Shea, B, O’Connell, D, Peterson, J, Welch, V, Losos, M, et al. The Newcastle-Ottawa scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses (2011). Available online at: http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp (Accessed July 4, 2025).
24. Kim, SR, Kim, K, Lee, SA, Kwon, SO, Lee, JK, Keum, N, et al. Effect of red, processed, and white meat consumption on the risk of gastric Cancer: an overall and dose−Response Meta-analysis. Nutrients. (2019) 11:826. doi: 10.3390/nu11040826
25. Higgins, JP, and Thompson, SG. Quantifying heterogeneity in a meta-analysis. Stat Med. (2002) 21:1539–58. doi: 10.1002/sim.1186
26. Egger, M, Davey Smith, G, Schneider, M, and Minder, C. Bias in meta-analysis detected by a simple, graphical test. BMJ. (1997) 315:629–34. doi: 10.1136/bmj.315.7109.629
27. Arslan, K, and Şahin, AS. Prognostic value of geriatric nutritional risk index and prognostic nutritional index in geriatric orthopedic trauma patients in the surgical intensive care unit. Duzce Med J. (2025) 27:11–6. doi: 10.18678/dtfd.1549923
28. Shigemoto, K, Sawaguchi, T, Horii, T, Goshima, K, Iwai, S, Higashikawa, T, et al. Multidisciplinary care model for geriatric patients with hip fracture in Japan: 5-year experience. Arch Orthop Trauma Surg. (2022) 142:2205–14. doi: 10.1007/s00402-021-03933-w
29. Katsuyama, Y, Horie, N, Yoshii, K, Nakamura, S, Saito, T, and Takahashi, K. Development and validation of a prognostic scoring system for 1-year mortality in older patients with hip fractures. Age Ageing. (2024) 53:afae195. doi: 10.1093/ageing/afae195
30. Zhou, Y, Wang, L, Cao, A, Luo, W, Xu, Z, Sheng, Z, et al. Modified frailty index combined with a prognostic nutritional index for predicting postoperative complications of hip fracture surgery in elderly. J Invest Surg. (2022) 35:1739–46. doi: 10.1080/08941939.2022.2101166
31. Rutenberg, TF, Hershkovitz, A, Jabareen, R, Vitenberg, M, Daglan, E, Iflah, M, et al. Can nutritional and inflammatory indices predict 90-day mortality in fragility hip fracture patients? SICOT J. (2023) 9:30. doi: 10.1051/sicotj/2023029
32. Faust, LM, Lerchenberger, M, Gleich, J, Linhart, C, Keppler, AM, Schmidmaier, R, et al. Predictive value of prognostic nutritional index for early postoperative mobility in elderly patients with Pertrochanteric fracture treated with intramedullary nail Osteosynthesis. J Clin Med. (2023) 12:1792. doi: 10.3390/jcm12051792
33. Tischler, EH, McDermott, JR, Vummidi, S, Mahmoud, SA, Gross, JM, Malik, AN, et al. Is it time to reassess the role of preoperative hypoalbuminemia among geriatric distal femur fracture patients? Arch Orthop Trauma Surg. (2024) 145:66. doi: 10.1007/s00402-024-05725-4
34. Hosokawa, T, Tajika, T, Suto, M, Honda, A, and Chikuda, H. Impact of possible sarcopenia and nutritional status on postoperative quick disabilities of the arm, shoulder, and hand score in geriatric women with distal radius fracture. J Hand Surg Am. (2024) 49:1112–8. doi: 10.1016/j.jhsa.2024.07.007
35. Tang, W, Yao, W, Wang, W, Ding, W, Ni, X, and He, R. Association between admission albumin levels and 30-day readmission after hip fracture surgery in geriatric patients: a propensity score-matched study. BMC Musculoskelet Disord. (2024) 25:234. doi: 10.1186/s12891-024-07336-x
36. Fang, XY, Xu, HW, Chen, H, Zhang, SB, Yi, YY, Ge, XY, et al. The efficacy of nutritional screening indexes in predicting the incidence of osteosarcopenia and major osteoporotic fracture in the elderly. J Bone Miner Metab. (2024) 42:372–81. doi: 10.1007/s00774-024-01514-6
37. Chen, SH, Zhang, BF, and Zhang, YM. The association between prealbumin concentration at admission and mortality in elderly patients with hip fractures: a cohort study. Arch Osteoporos. (2024) 19:27. doi: 10.1007/s11657-024-01384-5
38. Yagi, T, Oshita, Y, Okano, I, Kuroda, T, Ishikawa, K, Nagai, T, et al. Controlling nutritional status score predicts postoperative complications after hip fracture surgery. BMC Geriatr. (2020) 20:243. doi: 10.1186/s12877-020-01643-3
39. Fernández Miró, M, Cabrejo Gavidia, V, Carrascosa Piquer, O, Valero Lanau, J, Toapanta Valencia, M, and Aguado Jodar, A. Malnutrition is associated with postoperative complications in elderly patients undergoing total hip arthroplasty. Endocrinol Diabetes Nutr. (2023) 70:59–66. doi: 10.1016/j.endien.2023.06.003
40. Dias, T, Batista, BB, Chang, R, Noriega, JEA, and Figueiredo, GLP. Evaluation of nutritional status and correlation with postoperative complications in elderly patients submitted to surgical treatment of proximal femoral fractures. Rev Bras Ortop. (2021) 56:104–8. doi: 10.1055/s-0040-1721365
41. Yoel, U, Alkobi Weiss, H, Goldbart, A, Silverman Siris, E, Fisher, DL, Hassan, L, et al. The impact of a fracture liaison service with in-hospital anti-osteoporosis treatment on subsequent hip fracture and mortality rates-a single-center retrospective study. Osteoporos Int. (2024) 36:299–309. doi: 10.1007/s00198-024-07325-9
42. Wei, Z, Gao, X, Wang, J, Wang, Y, Tang, H, Ma, Z, et al. Triglyceride glucose index is associated with vertebral fracture in older adults: a longitudinal study. Endocrine. (2024) 87:1022–30. doi: 10.1007/s12020-024-04136-0
43. Johannesdottir, F, Tedtsen, T, Cooke, LM, Mahar, S, Zhang, M, Nustad, J, et al. Microvascular disease and early diabetes onset are associated with deficits in femoral neck bone density and structure among older adults with longstanding type 1 diabetes. J Bone Miner Res. (2024) 39:1454–63. doi: 10.1093/jbmr/zjae134
44. Titlestad, I, Watne, LO, Caplan, GA, McCann, A, Ueland, PM, Neerland, BE, et al. Impaired glucose utilization in the brain of patients with delirium following hip fracture. Brain. (2024) 147:215–23. doi: 10.1093/brain/awad296
45. Leung, MTY, Turner, JP, Marquina, C, Ilomäki, J, Tran, T, Bykov, K, et al. Gabapentinoids and risk of hip fracture. JAMA Netw Open. (2024) 7:e2444488. doi: 10.1001/jamanetworkopen.2024.44488
Keywords: prognostic nutritional index, elderly, fracture, mortality, meta-analysis
Citation: Bai B, Liu X and Li H (2025) Predictive value of prognostic nutritional index for the long-term prognosis of elderly patients with fracture: a systematic review and meta-analysis. Front. Nutr. 12:1631128. doi: 10.3389/fnut.2025.1631128
Edited by:
Zhiyong Hou, Third Hospital of Hebei Medical University, ChinaReviewed by:
Öztürk Taşkın, Kastamonu University, TürkiyeKadir Arslan, University of Health Sciences, Türkiye
Copyright © 2025 Bai, Liu and Li. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Hong Li, aG9uZ2xpMjAxOEBqbHUuZWR1LmNu; Xilin Liu, bGl1eGlsaW5Aamx1LmVkdS5jbg==
†These authors have contributed equally to this work
 Bing Bai
Bing Bai Xilin Liu
Xilin Liu Hong Li
Hong Li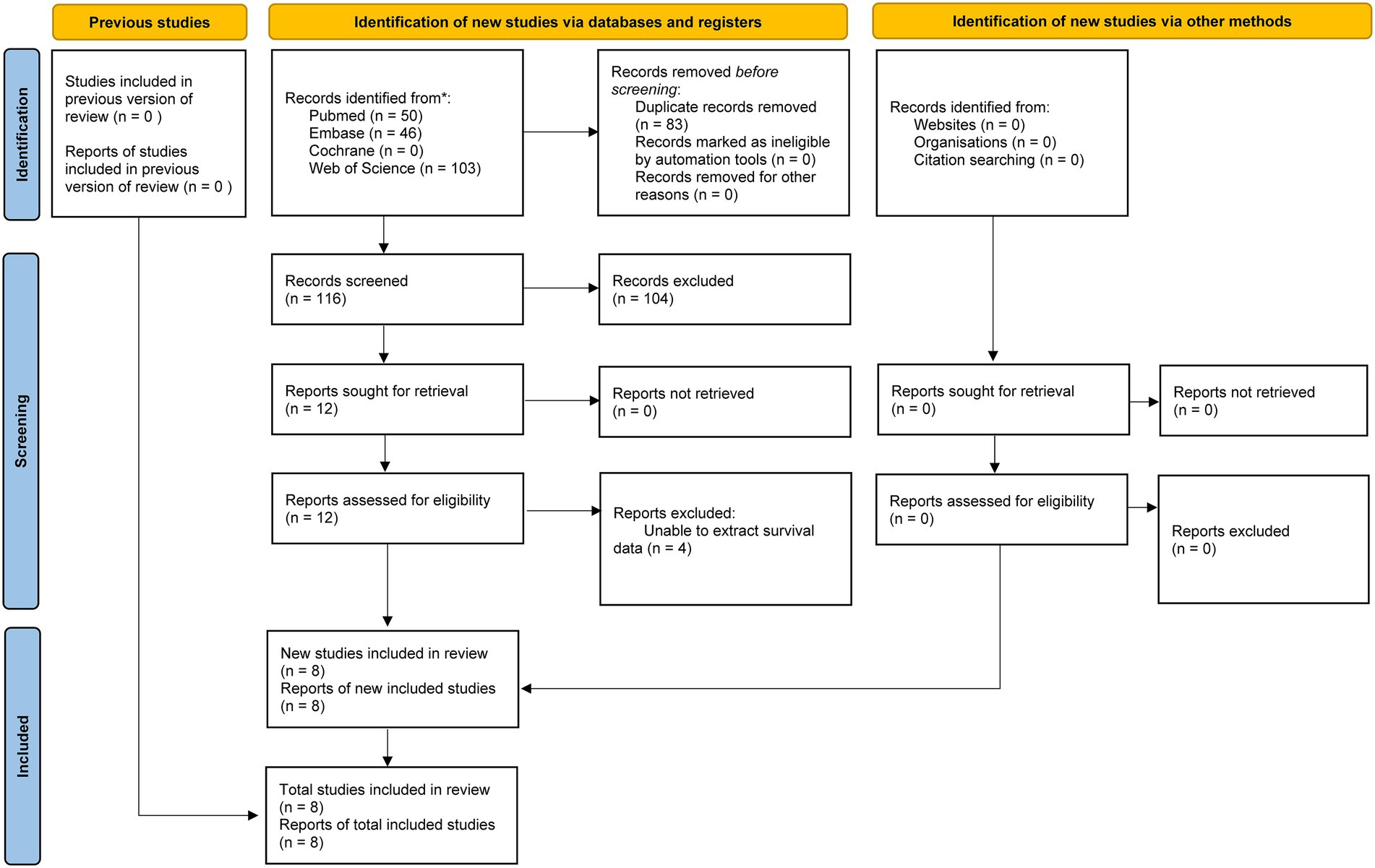
![Forest plot showing odds ratios with confidence intervals for studies grouped by age <40 and ≥40. The first group, <40, has a subtotal odds ratio of 0.91 [0.80, 1.04] with significant heterogeneity. The second group, ≥40, has a subtotal odds ratio of 0.49 [0.37, 0.65]. The overall odds ratio is 0.68 [0.56, 0.82] with high heterogeneity.](https://www.frontiersin.org/files/Articles/1631128/fnut-12-1631128-HTML/image_m/fnut-12-1631128-g006.jpg)